Abstract
Heme oxygenase-1 (HO-1), an inducible stress protein, confers cytoprotection against oxidative stress in vitro and in vivo. In addition to its physiological role in heme degradation, HO-1 may influence a number of cellular processes, including growth, inflammation, and apoptosis. By virtue of anti-inflammatory effects, HO-1 limits tissue damage in response to proinflammatory stimuli and prevents allograft rejection after transplantation. The transcriptional upregulation of HO-1 responds to many agents, such as hypoxia, bacterial lipopolysaccharide, and reactive oxygen/nitrogen species. HO-1 and its constitutively expressed isozyme, heme oxygenase-2, catalyze the rate-limiting step in the conversion of heme to its metabolites, bilirubin IXα, ferrous iron, and carbon monoxide (CO). The mechanisms by which HO-1 provides protection most likely involve its enzymatic reaction products. Remarkably, administration of CO at low concentrations can substitute for HO-1 with respect to anti-inflammatory and anti-apoptotic effects, suggesting a role for CO as a key mediator of HO-1 function. Chronic, low-level, exogenous exposure to CO from cigarette smoking contributes to the importance of CO in pulmonary medicine. The implications of the HO-1/CO system in pulmonary diseases will be discussed in this review, with an emphasis on inflammatory states.
Similar content being viewed by others
Introduction
The heme oxygenase-1/carbon monoxide (HO-1/CO) system has recently seen an explosion of research interest due to its newly discovered physiological effects. This metabolic pathway, first characterized by Tenhunen et al. [1, 2], has only recently revealed its surprising cytoprotective properties [3, 4]. Research in HO-1/CO now embraces the entire field of medicine where reactive oxygen/nitrogen species, inflammation, growth control, and apoptosis represent important pathophysiological mechanisms [3–6]. Indeed, the number of publications in recent years concerning HO-1 has increased exponentially, while the list of diseases and physiological responses associated with changes in HO-1 continues to expand [5].
Until now, relatively few studies have addressed the role of HO-1/CO in pulmonary medicine. Several investigators have focused on the diagnostic application of the HO-1/CO system, by measuring exhaled CO (E-CO) in various pathological pulmonary conditions, such as asthma or chronic obstructive pulmonary disease (COPD) [7]. In another experimental approach, investigators have examined the expression of HO-1 in lung tissue from healthy or diseased subjects [8, 9]. This review will highlight the actions of HO-1/CO in the context of pulmonary diseases (Fig. 1), emphasizing potential protective effects against inflammation, allergic reactions, oxidative stress, endotoxin shock, apoptosis, and tumor/cell growth [10–17].
Role of heme oxygenase and carbon monoxide in lung diseases. Heme oxygenase (HO) generates biliverdin IXα, ferrous iron, and carbon monoxide (CO) from the oxidation of heme. Exhaled CO reflects active heme metabolism. Inflammation, oxidative stress, and apoptosis represent an axis of disease, against which both endogenous HO activity and exogenous CO exert protective effects. CO may inhibit both inflammation and apoptosis. The toxicological properties of CO imply increased pro-oxidant activity; however, the pro-oxidant/and antioxidant consequences of CO in the physiological range remain unclear. The bile pigments biliverdin IXα and bilirubin IXα have demonstrated antioxidant properties, though their prospective roles in modulation of inflammation and apoptosis are currently under investigation. Iron (Fe) released from HO activity returns to a transient chelatable pool, where it may potentially promote oxidative stress and apoptosis. Induction of ferritin synthesis and sequestration of the released iron into ferritin may represent one possible detoxification pathway that limits the potential of iron in pro-apoptotic and pro-oxidative processes.
Review
Heme oxygenase-1
Heme oxygenase (HO, EC 1.14.99.3) catalyzes the first and rate-limiting step in heme degradation. In the HO reaction, the oxidation of heme generates equimolar ferrous iron, biliverdin IXα, and CO. NAD(P)H:biliverdin reductase subsequently converts bilverdin IXα into bilirubin IXα [1]. The bile pigments generated during heme degradation have antioxidant properties [18, 19]. The liberated heme iron undergoes detoxification either by extracellular efflux or by sequestration into ferritin, an intracellular iron-storage molecule with potential cytoprotective function [20–23]. Of the three known isoforms of HO (HO-1, HO-2, and HO-3), only HO-1 responds to xenobiotic induction [24–27]. Constitutively expressed in many tissues, HO-2 occurs at high levels in nervous and vascular tissues, and may respond to regulation by glucocorticoids [25, 28, 29]. HO-1 and HO-2 differ in genetic origin, in primary structure, in molecular weight, and in their substrate and kinetic parameters [25, 26]. HO-3 displays a high sequence homology with HO-2 but has little enzymatic activity [27]. This review will focus on the inducible, HO-1, form.
In addition to the physiological substrate heme, HO-1 responds to induction by a wide variety of stimuli associated with oxidative stress. Such inducing agents include hypoxia, hyperoxia, cytokines, nitric oxide (NO), heavy metals, ultraviolet-A (320–380 nm) radiation, heat shock, shear stress, hydrogen peroxide, and thiol (-SH)-reactive substances [3]. The multiplicity of toxic inducers suggest that HO-1 may function as a critical cytoprotective molecule [3, 4]. Many studies have suggested that HO-1 acts as an inducible defense against oxidative stress, in models of inflammation, ischemia-reperfusion, hypoxia, and hyperoxia-mediated injury (reviewed in [3]). The mechanisms by which HO-1 can mediate cytoprotection are still poorly understood. All three products of the HO reaction potentially participate in cellular defense, of which the gaseous molecule CO has recently received the most attention [30, 31]. The administration of CO at low concentrations can compensate for the protective effects of HO-1 in the presence of competitive inhibitors of HO-1 activity [32–34]. While HO-1 gene transfer confers protection against oxidative stress in a number of systems, clearly not all studies support a beneficial role for HO-1 expression. Cell-culture studies have suggested that the protective effects of HO-1 overexpression fall within a critical range, such that the excess production of HO-1 or HO-2 may be counterprotective due to a transient excess of reactive iron generated during active heme metabolism [35, 36]. Thus, an important caveat of comparative studies on the therapeutic effects of CO administration versus HO-1 gene delivery arises from the fact that the latter approach, in addition to producing CO, may have profound effects on intracellular iron metabolism.
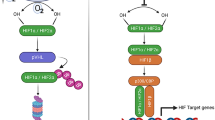
HO-1 expression is primarily regulated at the transcriptional level. Genetic analyses have revealed two enhancer sequences (E1, E2) in the murine HO-1 gene located at -4 kb (E1) and -10 kbp (E2) of the transcriptional start site [37, 38]. These enhancers mediate the induction of HO-1 by many agents, including heavy metals, phorbol esters, endotoxin, oxidants, and heme. E1 and E2 contain repeated stress-responsive elements, which consist of overlapping binding sites for transcription factors including activator protein-1 (AP-1), v-Maf oncoprotein, and the cap'n'collar/basic-leucine zipper family of proteins (CNC-bZIP), of which Nrf2 (NF-E2-related factor) may play a critical role in HO-1 transcription [39]. The promoter region of HO-1 also contains potential binding sites for nuclear factor κB (NF-κB), though the functional significance of these are not clear [40]. Both NF-κB and AP-1 have been identified as regulatory elements responsive to oxidative cellular stress [40, 41]. In response to hyperoxic stress, AP-1 factors mediated the induction of HO-1 in cooperation with signal-transducer and activator of transcription (STAT) proteins [41]. Furthermore, a distinct hypoxia-response element (HRE), which mediates the HO-1 response to hypoxia, represents a binding site for the hypoxia-inducible factor-1 (HIF-1) [42].
Carbon monoxide
The toxic properties of CO are well known in the field of pulmonary medicine. This invisible, odorless gas still claims many victims each year by accidental exposure. CO evolves from the combustion of organic materials and is present in smoke and automobile exhaust. The toxic actions of CO relate to its high affinity for hemoglobin (240-fold greater than that of O2). CO replaces O2 rapidly from hemoglobin, causing tissue hypoxia [43–45]. At high concentrations, other mechanisms of CO-induced toxicity may include apoptosis, lipid peroxidation, and inhibition of drug metabolism and respiratory enzyme functions [44].
Only recently has it become known that, at very low concentrations, CO participates in many physiological reactions. Where a CO exposure of 10,000 parts per million (ppm) (1% by volume CO in air) is toxic, 100–250 ppm (one hundredth to one fortieth as much) will stimulate the physiological effects without apparent toxicity [4]. The majority of endogenous CO production originates from active heme metabolism (>86%), though a portion may be produced in lipid peroxidation and drug metabolism reactions [46]. Cigarette smoking, still practiced by many lung patients, represents a major source of chronic low-level exposure to CO. Inhaled CO initially targets alveolar macrophages and respiratory epithelial cells.
The exact mechanisms by which CO acts at the molecular level remain incompletely understood. CO potentially exerts its physiological effects by influencing at least three known pathways (Fig. 2). By complexation with the heme moiety of the enzyme, CO activates soluble guanylate cyclase (sGC), stimulating the production of cyclic 3':5'-guanosine monophosphate (cGMP) [47]. The sGC/cGMP pathway mediates the effects of CO on vascular relaxation, smooth muscle cell relaxation, bronchodilation, neurotransmission, and the inhibition of platelet aggregation, coagulation, and smooth muscle proliferation [48–51]. Furthermore, CO may cause vascular relaxation by directly activating calcium-dependent potassium channels [52–54]. CO potentially influences other intracellular signal transduction pathways. The mitogen-activated protein kinase (MAPK) pathways, which transduce oxidative stress and inflammatory signaling (i.e. response to lipopolysaccharide), may represent an important target of CO action [32, 34, 55, 56]. An anti-apoptotic effect of CO and its relation to MAPK has recently been described. The overexpression of HO-1 or the exogenous administration of CO prevented tumor necrosis factor α (TNF-α)-induced apoptosis in murine fibroblasts [57]. In endothelial cells, the anti-apoptotic effect of CO depended on the modulation of the p38 (38 kilodalton protein) MAPK pathway [34]. The role of the remaining heme metabolites, (i.e. Fe and biliverdin IXα) in the modulation of apoptosis is currently being investigated and is beyond the scope of this review. Recent studies have reported a potent anti-inflammatory effect of CO, involving the inhibition of proinflammatory cytokine production after endotoxin stimulation, dependent on the modulation of p38 MAPK [32]. The clinical relevance of p38 MAPK lies in the possibility of modulating this pathway in various clinical conditions to downregulate the inflammatory response [58].
Possible mechanism(s) of carbon monoxide action. Endogenous carbon monoxide (CO) arises principally as a product of heme metabolism, from the action of heme oxygenase enzymes, although a portion may arise from environmental sources such as pharmacological administration or accidental exposure, or other endogenous processes such as drug and lipid metabolism. The vasoregulatory properties of CO, including its effects on cellular proliferation, platelet aggregation, and vasodilation, have been largely ascribed to the stimulation of guanylate cyclase by direct heme binding, leading to the generation of cyclic GMP. The anti-inflammatory properties of CO are associated with the downregulation of proinflammatory cytokine production, dependent on the selective modulation of mitogen-activated protein kinase (MAPK), such as the 38 kilodalton protein (p38MAPK). In addition to these two mechanisms, CO may potentially interact with any hemoprotein target, though the functional consequences of these interactions with respect to cellular signaling remain poorly understood.
Involvement of HO-1 and CO in lung disease
Oxidative stress arising from an imbalance between oxidants and antioxidants plays a central role in the pathogenesis of airway disease [59]. In lung tissue, HO-1 expression may occur in respiratory epithelial cells, fibroblasts, endothelial cells, and to a large extent in alveolar macrophages [41, 60, 61]. HO-1 induction in these tissues, in vitro and in vivo, responds to common causes of oxidative stress to the airways, including hyperoxia, hypoxia, endotoxemia, heavy metal exposure, bleomycin, diesel exhaust particles, and allergen exposure [4, 41, 61]. Induction of HO-1 or administration of CO can protect cells from these stressful stimuli [10, 41]. In one of the experiments that best illustrate the protective role of CO in vivo, rats were exposed to hyperoxia (>98% O2) in the absence or presence of CO at low concentration (250 ppm). The CO-treated rats showed increased survival and a diminished inflammatory response to the hyperoxia [11]. As demonstrated in a model of endotoxin-induced inflammation, the protection afforded by CO most likely resulted from the downregulated synthesis of proinflammatory cytokines (i.e. TNF-α, IL-1β) and the upregulation of the anti-inflammatory cytokine interleukin-10 (IL-10) [32]. Furthermore, increases in exhaled CO (E-CO) have been reported in a number of pathological pulmonary conditions, such as unstable asthma, COPD, and infectious lung disease; these increases may reflect increased endogenous HO-1 activity [7]. Elevated carboxyhemoglobin (Hb-CO) levels have also been reported in these same diseases in nonsmoking subjects, where both the E-CO and Hb-CO levels decrease to normal levels in response to therapy [62].
E-CO in humans originates primarily from both systemic heme metabolism, which produces CO in various tissues, and localized (lung) heme metabolism, as a result of the combined action of inducible HO-1 and constitutive HO-2 enzymatic activity. Endogenously produced or inspired CO is eliminated exclusively by respiration [63]. Elevation of E-CO may also reflect an increase in exogenous sources such as smoking or air pollution. In addition to changes in environmental factors, elevations of E-CO in lung diseases may reflect an increase in blood Hb-CO levels in response to systemic inflammation, as well as an increase in pulmonary HO-1 expression in response to local inflammation [9, 62, 64].
The diagnostic value of measuring E-CO remains controversial due to many conflicting reports (i.e. some reports indicate differences in E-CO measurements between disease activity and controls, and some reports do not). The possible explanations for these discrepancies include large differences in patient populations and in the methods used for measuring E-CO, and undefined corrections for background levels of CO. Furthermore, remarkable differences arise between studies in the magnitude of the E-CO levels in the control groups as well as in treated or untreated asthma patients. When active or passive smoking occurs, or in the presence of high background levels of CO, the measurement of E-CO is not particularly useful for monitoring airway inflammation. In patients who smoke, E-CO can be used only to confirm the smoking habit [65, 66]. Comparable to the beginning era of measurements of exhaled NO, a standardization in techniques and agreement on background correction should be reached for E-CO measurements, to allow proper conclusions to be drawn in this area of investigation.
Asthma and allergy
Asthma, a form of allergic lung disease, features an accumulation of inflammatory cells and mucus in the airways, associated with bronchoconstriction and a generalized airflow limitation. Inflammation, a key component of asthma, involves multiple cells and mediators where an imbalance in oxidants/antioxidants contributes to cell damage. Several pathways associated with oxidative stress may participate in asthma. For example, the redox-sensitive transcription factors NF-κB and AP-1 control the expression of proinflammatory mediators [59, 67–69].
In light of the potential protective effects of HO-1/CO on inflammatory processes, the study of HO-1 in asthma has gained popularity. In a mouse model of asthma, HO-1 expression increased in lung tissue in response to ovalbumin aerosol challenge, indicating a role for HO-1 in asthma [70]. In a similar model of aeroallergen-induced asthma in ovalbumin-sensitized mice, exposure to a CO atmosphere resulted in a marked attenuation of eosinophil content in bronchoalveolar lavage fluid (BALF) and downregulation of the proinflammatory cytokine IL-5 [10]. This experiment showed that exogenous CO can inhibit asthmatic responses to allergens in mice.
Recent human studies have revealed higher HO-1 expression in the alveolar macrophages and higher E-CO in untreated asthmatic patients than in healthy nonsmoking controls [71, 72]. Patients with exacerbations of asthma and patients who were withdrawn from inhaled steroids showed higher E-CO levels than steroid-treated asthmatics or healthy controls [73]. Higher levels of E-CO may also occur in children with persistent asthma than in healthy controls [74]. E-CO levels may correlate with functional parameters such as peak expiratory flow rate. A low rate in asthma exacerbations correlated with high E-CO, whereas normalization of the rate with oral glucocorticoid treatment resulted in a reduction of E-CO [75]. Furthermore, increased E-CO was associated with greater expression of HO-1 in airway alveolar macrophages obtained by induced sputum in untreated asthmatic patients than in controls. These asthma patients also showed higher bilirubin levels in the induced sputum, indicating higher HO activity [71]. Furthermore, patients with asthma show an increased Hb-CO level at the time of exacerbation, with values decreasing to control levels after oral glucocorticoid treatment [62]. In human asthmatics, E-CO and airway eosinophil counts decreased in response to a one-month treatment with inhaled corticosteroids [73]. In direct contrast to such studies promoting E-CO as a useful noninvasive tool for monitoring airway inflammation, other studies reported no difference in E-CO levels of asthma patients versus healthy controls, or between patients with stable and unstable asthma. In one such report, no further change in E-CO occurred in asthma patients after a one-month treatment of inhaled corticosteroids, despite observed decreases in airway eosinophil content and bronchial responsiveness to metacholine [76]. A recent study accentuates this finding in asthma excerbations, where no decrease in E-CO of children with asthma could be detected after oral prednisolone treatment [77]. In human allergic responses, results on elevation of E-CO are also inconclusive. A clear elevation of E-CO after allergen exposure occurred in patients with asthma during the late response, and during the early response immediately after the inhalation [78]. However, another report showed that no elevation of E-CO occurred in allergen-induced asthma within 48 hours after allergen challenge [79]. Finally, increases in E-CO were measured in allergic rhinitis, correlating with seasonal changes in exposure to allergen (pollen) [80].
Chronic obstructive pulmonary disease
Airway inflammation plays an important role in the development of COPD, characterized by the presence of macrophages, neutrophils, and inflammatory mediators such as proteinases, oxidants, and cytokines. Furthermore, the inflammatory consequences of chronic microbiological infections may contribute to the progression of the disease. The current paradigm for the pathogenesis of COPD involves imbalances in protease/antiprotease activities and antioxidant/pro-oxidant status. Proteases with tissue-degrading capacity, (i.e. elastases and matrix metalloproteinases), when insufficiently inhibited by antiproteases, can induce tissue damage leading to emphysema. Oxidants that supersede cellular antioxidant defenses can furthermore inactivate antiproteases, cause direct injury to lung tissue, and interfere with the repair of the extracellular matrix. Smoking plays an important role in both hypotheses. Cigarette smoke will act primarily on alveolar macrophages and epithelial cells, which react to this oxidative stress by producing proinflammatory cytokines and chemokines and releasing growth factors. Nevertheless, smoking cannot be the only factor in the development of COPD, since only 15–20% of smokers develop the disease [81, 82].
Exposure to reactive oxygen species (from cigarette smoke or chronic infections) and an imbalance in oxidant/antioxidant status are the main risk factors for the development of COPD. To defend against oxidative stress, cells and tissues contain endogenous antioxidant defense systems, which include millimolar concentrations of the tripeptide glutathione (GSH). A close relation exists between GSH concentration and HO-1, whereby depletion of GSH augments the transcriptional regulation of HO-1 by oxidants, suggesting that the HO-1/CO system acts as a secondary defense against oxidative stress [83–86]. Accumulating clinical evidence suggests that HO-1/CO may also play an important part in COPD. Alveolar macrophages, which produce a strong HO-1 response to stimuli, may represent the main source of CO production in the airways [60, 64]. Patients with COPD have displayed higher E-CO than healthy nonsmoking controls [87]. Furthermore, much higher levels of HO-1 have been observed in the airways of smokers than in nonsmokers [64]. Among subjects who formerly smoked, patients with COPD have lower HO-1 expression in alveolar macrophages than healthy subjects [88]. A microsatellite polymorphism that is linked with the development of COPD may occur in the promoter region of HO-1, resulting in a lower production of HO-1 in people who have the polymorphism. Thus, a genetically dependent downregulation of HO-1 expression may arise in subpopulations, possibly linked to increased susceptibility to oxidative stress [89–91]. Future studies on both genetic predisposition and possible therapeutic modalities will reveal the involvement of the HO-1/CO system in COPD.
Cystic fibrosis
Cystic fibrosis (CF) involves a deposition of hyperviscous mucus in the airways associated with pulmonary dysfunction and pancreatic insufficiency, which may be accompanied by chronic microbiological infections. E-CO readings were higher in untreated versus oral-steroid-treated CF patients [92]. Furthermore, E-CO increased in patients during exacerbations of CF, correlating to deterioration of the forced expiratory volume in one second (FEV1), with normalization of the E-CO levels after treatment [93]. E-CO levels may correlate with exhaled ethane, a product of lipid peroxidation that serves as an indirect marker of oxidative stress. Both E-CO and exhaled ethane were higher in steroid-treated and untreated CF patients than in healthy controls [94]. E-CO was higher in children with CF than in control patients. In addition to the inflammatory and oxidative stress responses to continuous infectious pressure in these patients, E-CO may possibly respond to hypoxia. E-CO increased further in CF children following an exercise test, and correlated with the degree of oxyhemoglobin desaturation, a finding suggestive of an increased HO-1 expression in CF patients during hypoxic states induced by exercise [95].
Infectious lung disease
In patients with pneumonia, higher Hb-CO levels can be measured at the onset of illness, with values decreasing to control levels after antibiotic treatment [62]. E-CO levels were reported to be higher in lower-respiratory-tract infections and bronchiectasis, with normalization after antibiotic treatment [96, 97]. Furthermore, E-CO levels in upper-respiratory-tract infections were higher than in healthy controls [74, 80]. The relationship between higher measured E-CO in these infectious states and higher Hb-CO levels cannot be concluded from these studies.
Interstitial lung disease
The role of HO-1 in the development of interstitial lung disease remains undetermined. Comparative immunohistochemical analysis has revealed that lung tissue of control subjects, patients with sarcoidosis, usual interstitial pneumonia, and desquamative interstitial pneumonia, all showed a high expression of HO-1 in the alveolar macrophages but a weak expression in the fibrotic areas [98]. The antiproliferative properties of HO-1 suggest a possible beneficial role in limiting fibrosis; however, this hypothesis is complicated by a newly discovered relation between IL-10 and HO-1. IL-10 produced by bronchial epithelial cells promotes the growth and proliferation of lung fibroblasts [99]. HO-1 expression and CO treatment have been shown to increase the production of IL-10 in macrophages following proinflammatory stimuli [32]. Conversely, IL-10 induces HO-1 production, which is apparently required for the anti-inflammatory action of IL-10 [100].
A recent report clearly shows the suppression of bleomycin-induced pulmonary fibrosis by adenovirus-mediated HO-1 gene transfer and overexpression in C57BL/6 mice, involving the inhibition of apoptotic cell death [101]. Overall, more research is needed to elucidate the mechanisms of HO-1 in interstitial lung disease and its possible therapeutic implications.
Lung cancer
HO-1 action may be of great importance in solid tumors, an environment that fosters hypoxia, oxidative stress, and neovascularization. HO-1 may have both pro- and antagonistic effects on tumor growth and survival. HO-1 and CO cause growth arrest in cell-culture systems and thus may represent a potential therapeutic modality in modulating tumor growth [16]. The overexpression of HO-1 or administration of CO in mesothelioma and adenocarcinoma mouse models resulted in improved survival (>90%) as well as reduction in tumor size (>50%) [17]. Furthermore, HO-1 expression in oral squamous cell carcinomas can be useful in identifying patients at low risk of lymph node metastasis. High expression of HO-1 was detected in groups without lymph node metastasis in this report [102]. In contrast to growth arrest, HO-1 may protect solid tumors from oxidative stress and hypoxia, possibly by promoting neovascularization. In one study, zinc protoporphyrin, a competitive inhibitor of HO-1 enzyme activity, suppressed tumor growth [103].
Pulmonary vascular disease
CO may represent a critical mediator of the body's adaptive response to hypoxia, a common feature in pulmonary vascular disease [104]. Since CO can modulate vascular tone by inducing cGMP and large, calcium-dependent potassium channels, HO-1 and CO probably play important roles in pulmonary vascular diseases [54]. A NO-mediated HO-1 induction occurred in the hepatopulmonary syndrome during cirrhosis, associated with enhancement of vascular relaxation [105]. In portopulmonary hypertension, elevated levels of cGMP and inducible nitric oxide synthase (iNOS) expression in the vascular endothelium, and HO-1 expression in macrophages and bronchial epithelium have been described [106]. In transgenic mice models, ho-1 -/-and ho-1 +/+ mice did not differ in their development of pulmonary hypertension following chronic hypoxia treatment, despite the development of right ventricular dilation and right myocardial infarction in ho-1 -/- mice [107]. The preinduction of HO-1 protein with chemical inducers, however, prevented the development of pulmonary hypertension in the rat lung as a consequence of chronic hypoxia treatment [108]. Transgenic mice overexpressing HO-1 in the lung were resistant to hypoxia-induced inflammation and hypertension [109]. Further research is needed to elucidate the potential role of HO-1 and CO in primary human lung vascular diseases such as primary pulmonary hypertension.
Hyperoxic lung injury and acute respiratory distress syndrome
Supplemental oxygen therapy is often used clinically in the treatment of respiratory failure. Exposure to high oxygen tension (hyperoxia) may cause acute and chronic lung injury, by inducing an extensive inflammatory response in the lung that degrades the alveolar-capillary barrier, leading to impaired gas exchange and pulmonary edema [110, 111]. Hyperoxia-induced lung injury causes symptoms in rodents that resemble human acute respiratory distress syndrome [112].
Hyperoxia induced HO-1 expression in adult rats but apparently not in neonatal rats, in which the expression and activities of HO-1 and HO-2 are developmentally upregulated during the prenatal and early postnatal period [113].
Both HO-1 and HO-2 potentially influence pulmonary adaptation to high O2 levels. In one example, the adenoviral-mediated gene transfer of HO-1 into rat lungs protected against the development of lung apoptosis and inflammation during hyperoxia [114]. In vitro studies showed that the overexpression of HO-1 in lung epithelial cells or rat fetal lung cells caused growth arrest and conferred resistance against hyperoxia-induced cell death [15, 16]. An oxygen-tolerant variant of hamster fibroblasts that moderately overexpressed HO-1 in comparison with the parent line resisted oxygen toxicity in vitro. The treatment of this oxygen-tolerant strain with HO-1 antisense oligonucleotides reduced the resistance to hyperoxia. In contrast, additional, vector-mediated, HO-1 expression did not further increase oxygen tolerance in this model [115].
In vivo studies with gene-deleted mouse strains have provided much information on the roles of HO-1 and HO-2 in oxygen tolerance. Dennery et al. demonstrated that heme oxygenase-2 knockout mice (ho-2-/-) were more sensitive to the lethal effects of hyperoxia than wild-type mice [116]. In addition to the absence of HO-2 expression, however, the mice displayed a compensatory increase in HO-1 protein expression, and higher total lung HO activity. Thus, in this model, the combination of HO-2 deletion and HO-1 overexpression resulted in a hyperoxia-sensitive phenotype. Recent studies of Dennery et al. have shown that HO-1- deleted (ho-1-/-) mice were more resistant to the lethal effects of hyperoxia than the corresponding wild type [117]. The hyperoxia resistance observed in the ho-1-/- strain could be reversed by the reintroduction of HO-1 by adenoviral-mediated gene transfer [117]. In contrast, mouse embryo fibroblasts derived from ho-1-/- mice showed increased sensitivity to the toxic effects of hemin and H2O2 and generated more intracellular reactive oxygen species in response to these agents [118]. Both ho-1-/- and ho-2-/- strains were anemic, yet displayed abnormal accumulations of tissue iron. Specifically, ho-1-/- accumulated nonheme iron in the kidney and liver and had decreased total iron content in the lung, while ho-2-/- mice accumulated total lung iron in the absence of a compensatory increase in ferritin levels [116, 119]. The mechanism(s) by which HO-1 or HO-2 deletions result in accumulation of tissue iron remain unclear. These studies, taken together, have indicated that animals deficient in either HO-1 and HO-2 display altered sensitivity to oxidative stress conditions. Aberrations in the distribution of intra- and extra-cellular iron, may underlie in part, the differential sensitivity observed [116, 117].
Otterbein et al. have shown that exogenous CO, through anti-inflammatory action, may protect the lung in a rat model of hyperoxia-induced lung injury. The presence of CO (250 ppm) prolonged the survival of rats in a hyperoxic (>95% O2) environment, and inhibited the appearance of markers of hyperoxia-induced lung injury (i.e. hemorrhage, fibrin deposition, edema, airway protein accumulation, and BALF neutrophil influx) [11]. Furthermore, in a mouse model, CO inhibited the expression of proinflammatory cytokines (TNF-α, IL-1β, and IL-6) in mice induced by the hyperoxia treatment. Using gene-deleted mice, Otterbein and colleagues also observed that the protection afforded by CO in this model, similar to a lipopolysaccharide-induced model of lung injury, depended on the p38 MAPK pathway (Otterbein et al., unpublished observation, as reviewed in [3]).
In direct contrast to these studies, the group of Piantadosi and colleagues reported no significant difference in the hyperoxia tolerance of rats at CO doses between 50 and 500 ppm [120]. In their model, CO did not alter the accumulation of fluid in the airway. Furthermore, CO, when applied in combination with hyperoxia, increased the activity of myeloperoxidase, a marker of airway neutrophil influx. This study also suggested that inhalation of CO (50–500 ppm) did not alter the expression of HO-1 or other antioxidant enzymes such as Manganese superoxide dismutase (MnSOD) in vivo[120]. Furthermore, Piantadosi and colleagues were able to induce oxygen tolerance in rats and HO-1 expression with hemoglobin treatment, but this tolerance also occurred in the presence of HO inhibitors, thereby not supporting a role for HO activity in oxygen tolerance [121]. Although no consensus has been reached as to the protective role of CO inhalation and/or HO-1 induction in hyperoxic lung injury, human studies will be required to show if CO will supersede NO in providing a significant therapeutic benefit in the context of severe lung diseases [122]. While antioxidant therapies have been examined, until now no human studies exist on the role of HO-1 and CO in acute respiratory distress syndrome (ARDS) and bronchopulmonary dysplasia [123].
Lung transplantation
Lung transplantation is the ultimate and often last therapeutic option for several end-stage lung diseases. After lung transplantation, there remains an ongoing hazardous situation in which both acute and chronic graft failure, as well as complications of the toxic immunosuppressive regimen used (i.e. severe bacterial, fungal, and viral infections; renal failure; and Epstein-Barr-virus-related lymphomas), determine the outcome [124]. The development of chronic graft failure, obliterative bronchiolitis (OB), determines the overall outcome after lung transplantation. OB, which may develop during the first months after transplantation, is the main cause of morbidity and death following the first half-year after transplantation, despite therapeutic intervention. Once OB has developed, retransplantation remains the only therapeutic option available [124, 125]. Little is known about the pathophysiological background of OB. The possible determinants of developing OB include ongoing immunological allograft response, HLADR mismatch, cytomegalovirus infection, acute rejection episodes, organ-ischemia time, and recipient age [125]. OB patients displayed elevated neutrophil counts in the BALF, and evidence of increased oxidant activity, such as increased methionine oxidation in BALF protein and decreases in the ratio of GSH to oxidized glutathione (GSSG) in epithelial lining fluid. [126, 127].
So far, only very limited research data are available on the possible role for HO-1 in allograft rejection after lung transplantation. Higher HO-1 expression has been detected in alveolar macrophages from lung tissue in lung transplant recipients with either acute or chronic graft failure than in stable recipients [128]. The protective role of HO-1 against allograft rejection has been shown in other transplantation models, in which solid organ transplantation typically benefits from HO-1 modulation. A higher expression of protective genes such as HO-1 has been observed in episodes of acute renal allograft rejection [129]. Furthermore, the induction of HO-1 alleviates graft-versus-host disease [130]. Adenoviral-HO-1 gene therapy resulted in remarkable protection against rejection in rat liver transplants [131]. The upregulation of HO-1 protected pancreatic islet cells from Fas-mediated apoptosis in a dose-dependent fashion, supporting an anti-apoptotic function of HO-1 [132, 133]. HO-1 may confer protection in the early phase after transplantation by inducing Th2-dependent cytokines such as IL-4 and IL-10, while suppressing interferon-γ and IL-2 production, as demonstrated in a rat liver allograft model [134].
Beneficial effects of HO-1 modulation have also been described in xenotransplantation models, in which HO-1 gene expression appears functionally associated with xenograft survival [135]. In a mouse-to-rat heart transplant model, the effects of HO-1 upregulation could be mimicked by CO administration, suggesting that HO-derived CO suppressed the graft rejection [136]. The authors proposed that CO suppressed graft rejection by inhibition of platelet aggregation, a process that facilitates vascular thrombosis and myocardial infarction.
HO-1 may also contribute to ischemic preconditioning, a process of acquired cellular protection against ischemia/reperfusion injury, as observed in guinea pig transplanted lungs [137]. HO-1 overexpression provided potent protection against cold ischemia/reperfusion injury in a rat model through an anti-apoptotic pathway [138, 139]. The induction of HO-1 in rats undergoing liver transplantation with cobalt-protoporphyrin or adenoviral-HO-1 gene therapy resulted in protection against ischemia/reperfusion injury and improved survival after transplantation, possibly by suppression of Th1-cytokine production and decreased apoptosis after reperfusion [140, 141]. Until now, no reports have addressed E-CO measurements in lung transplantation, where it is possible that differences in E-CO will be found in patients with acute and chronic allograft rejection.
Conclusion and future implications
The evolution of CO in exhaled breath may serve as a general marker and diagnostic indicator of inflammatory disease states of the lung, though more research will be required to verify its reliability. Increases in exhaled CO presumably reflect changes in systemic and airway heme metabolic activity from the action of HO enzymes. Evidence from numerous in vitro and animal studies indicates that HO-1 provides a protective function in many, if not all, diseases that involve inflammation and oxidative stress. Thus, the exploitation of HO-1 for therapeutic gain could be achieved through the modulation of HO-1 enzyme activity or its up- and downstream regulatory factors, either by gene transfer, pharmacological inducers, or direct application of CO by gas administration or chemical delivery [142–145]. The CO-releasing molecules (transition metal carbonyls) developed by Motterlini et al. [144] show promise in the pharmacological delivery of CO for therapeutic applications in vascular and immune regulation. The CO-releasing molecules have been shown to limit hypertension in vivo and promote vasorelaxation in isolated heart and aortic rings [144].
Ultimately, the challenge remains in applying the therapeutic potentials of HO-1 to the treatment of human diseases. In vivo models of transplantation have shown that HO-1 gene therapy protects against allograft rejection [129, 134]. Given the toxic therapy that every transplant patient receives, especially after lung transplantation, the field of transplantation medicine may bring the first frontier for human applications of HO-1 gene therapy or exogenous CO administration. The potential use of inhalation CO as a clinical therapeutic in inflammatory lung diseases has also appeared on the horizon. In one promising study, an inhalation dose of 1500 ppm CO at the rate of 20 times per day for a week produced no cardiovascular side effects [146]. Cigarette smoking and CO inhalation at identical intervals produced comparable Hb-CO levels of approximately 5%. The question of whether or not CO can be used as an inhalation therapy will soon be replaced by questions of "how much, how long, and how often?" The fear of administering CO must be weighed against the severe toxicity of the immunosuppressive agents in current use, and the often negative outcome of solid organ transplantation.
Abbreviations
- AP-1:
-
activator protein-1
- BALF:
-
bronchoalveolar lavage fluid
- CF:
-
cystic fibrosis
- cGMP:
-
cyclic 3':5'-guanosine monophosphate
- CO:
-
carbon monoxide
- COPD:
-
chronic obstructive pulmonary disease
- E-CO:
-
exhaled carbon monoxide
- GSH:
-
glutathione, reduced form
- Hb-CO:
-
carboxyhemoglobin
- HO-1:
-
heme oxygenase-1
- IL:
-
interleukin
- kb:
-
kilobase
- MAPK:
-
mitogen-activated protein kinase
- NF-κB:
-
nuclear factor κB
- NO:
-
nitric oxide
- OB:
-
obliterative bronchiolitis
- p38:
-
38 kilodalton protein
- ppm:
-
parts per million
- sGC:
-
soluble guanylate cyclase
- TNF-α:
-
tumor necrosis factor α
References
Tenhunen R, Marver H, Schmid R: Microsomal heme oxygenase, characterization of the enzyme. J Biol Chem 1969, 244:6388–6394.
Tenhunen R, Marver HS, Schmid R: The enzymatic conversion of heme to bilirubin by microsomal heme oxygenase. Proc Natl Acad Sci USA 1968, 61:748–755.
Ryter S, Otterbein LE, Morse D, Choi AM: Heme oxygenase/carbon monoxide signaling pathways: regulation and functional significance. Mol Cell Biochem 2002, 234–235:249–263.
Otterbein LE, Choi AM: Heme oxygenase: colors of defence against cellular stress. Am J Physiol Lung Cell Mol Physiol 2000, 279:L1029-L1037.
Morse D, Choi AM: Heme oxygenase-1. The "emerging molecule" has arrived. Am J Respir Cell Mol Biol 2002, 27:8–16.
Willis D, Moore AR, Frederick R, Willoughby DA: Heme oxygenase: a novel target for the modulation of the inflammatory response. Nat Med 1996, 2:87–90.
Horvath I, MacNee W, Kelly FJ, Dekhuijzen PN, Phillips M, Doring G, Choi AM, Yamaya M, Bach FH, Willis D, Donnelly LE, Chung KF, Barnes PJ: "Haemoxygenase-1 induction and exhaled markers of oxidative stress in lung diseases", summary of the ERS Research Seminar in Budapest, Hungary, September, 1999. Eur Respir J 2001, 18:420–430.
Lim S, Groneberg D, Fischer A, Oates T, Caramori G, Mattos W, Adcock I, Barnes PJ, Chung KF: Expression of heme oxygenase isoenzymes 1 and 2 in normal and asthmatic airways: effect of inhaled corticosteroids. Am J Respir Crit Care Med 2000, 162:1912–1908.
Donnelly LE, Barnes PJ: Expression of heme oxygenase in human airway epithelial cells. Am J Respir Cell Mol Biol 2001, 24:295–303.
Chapman JT, Otterbein LE, Elias JA, Choi AM: Carbon monoxide attenuates aeroallergen-induced inflammation in mice. Am J Physiol Lung Cell Mol Physiol 2001, 281:L209-L216.
Otterbein LE, Mantell LL, Choi AM: Carbon monoxide provides protection against hyperoxic lung injury. Am J Physiol 1999, 276:L688-L694.
Yachie A, Niida Y, Wada T, Igarashi N, Kaneda H, Toma T, Ohta K, Kasahara Y, Koizumi S: Oxidative stress causes enhanced endothelial cell injury in human heme oxygenase-1 deficiency. J Clin Invest 1999, 103:129–135.
Inoue S, Suzuki M, Nagashima Y, Suzuki S, Hashiba T, Tsuburai T, Ikehara K, Matsuse T, Ishigatsubo Y: Transfer of heme oxygenase 1 cDNA by a replication-deficient adenovirus enhances interleukin-10 production from alveolar macrophages that attenuates lipopolysaccharide-induced acute lung injury in mice. Hum Gene Ther 2001, 12:967–979.
Otterbein L, Sylvester SL, Choi AM: Hemoglobin provides protection against lethal endotoxemia in rats: the role of heme oxygenase-1. Am J Respir Cell Mol Biol 1995, 13:595–601.
Otterbein LE, Lee PJ, Chin BY, Petrache I, Camhi SL, Alam J, Choi AM: Protective effects of heme oxygenase-1 in acute lung injury. Chest 1999, 116:61S-63S.
Lee PJ, Alam J, Wiegand GW, Choi AM: Overexpression of heme oxygenase-1 in human pulmonary epithelial cells results in cell growth arrest and increased resistance to hyperoxia. Proc Natl Acad Sci USA 1996, 93:10393–10398.
Otterbein LE, Choi AMK: Carbon monoxide at low concentrations causes growth arrest and modulates tumor growth in mice [abstract]. Am J Respir Crit Care Med 2001, 163:A476.
Stocker R, Yamamoto Y, McDonagh AF, Glazer AN, Ames BN: Bilirubin is an antioxidant of possible physiological importance. Science 1987, 235:1043–1046.
Yesilkaya A, Altinayak R, Korgun DK: The antioxidant effect of free bilirubin on cumene-hydroperoxide treated human leukocytes. Gen Pharmacol 2000, 35:17–20.
Ferris CD, Jaffrey SR, Sawa A, Takahashi M, Brady SD, Barrow RK, Tysoe SA, Wolosker H, Baranano DE, Dore S, Poss KD, Snyder SH: Haem oxygenase-1 prevents cell death by regulating cellular iron. Nat Cell Biol 1999, 1:152–157.
Vile GF, Tyrrell RM: Oxidative stress resulting from ultraviolet A irradiation of human skin fibroblasts leads to a heme oxygenase-dependent increase in ferritin. J Biol Chem 1993, 268:14678–14681.
Vile GF, Basu-Modak S, Waltner C, Tyrrell RM: Heme oxygenase-1 mediates an adaptive response to oxidative stress in human skin fibroblasts. Proc Natl Acad Sci USA 1994, 91:2607–2610.
Oberle S, Schwartz P, Abate A, Schroder H: The antioxidant defense protein ferritin is a novel and specific target for pentaerithrityl tetranitrate in endothelial cells. Biochem Biophys Res Commun 1999, 261:28–34.
Cruse I, Maines MD: Evidence suggesting that the two forms of heme oxygenase are products of different genes. J Biol Chem 1988, 263:3348–3353.
Maines MD: Heme Oxygenase: Clinical Applications and Functions.Boca Raton, FL: CRC Press 1992.
Maines MD, Trakshel GM, Kutty RK: Characterization of two constitutive forms of rat liver microsomal heme oxygenase. Only one molecular species of the enzyme is inducible. J Biol Chem 1986, 261:411–419.
McCoubrey WK Jr, Huang TJ, Maines MD: Isolation and characterization of a cDNA from the rat brain that encodes hemoprotein heme oxygenase-3. Eur J Biochem 1997, 247:725–732.
Zakhary R, Gaine SP, Dinerman JL, Ruat M, Flavahan NA, Snyder SH: Heme oxygenase 2: endothelial and neuronal localization and role in endothelium-dependent relaxation. Proc Natl Acad Sci USA 1996, 93:795–798.
Raju VS, McCoubrey WK Jr, Maines MD: Regulation of heme oxygenase-2 by glucocorticoids in neonatal rat brain: characterization of a functional glucocorticoid response element. Biochim Biophys Acta 1997, 1351:89–104.
Townsend CL, Maynard R: Changing views on carbon monoxide. Clin Exp Allergy 2002, 32:172–174.
Thiemermann C: Inhaled CO: deadly gas or novel therapeutic? Nat Med 2001, 7:534–535.
Otterbein LE, Bach FH, Alam J, Soares M, Tao Lu H, Wysk M, Davis RJ, Flavell RA, Choi AM: Carbon monoxide has anti-inflammatory effects involving the mitogen-activated protein kinase pathway. Nat Med 2000, 6:422–428.
Sato K, Balla J, Otterbein L, Smith RN, Brouard S, Lin Y, Csizmadia E, Sevigny J, Robson SC, Vercellotti G, Choi AM, Bach FH, Soares MP: Carbon monoxide generated by heme oxygenase-1 suppresses the rejection of mouse-to-rat cardiac transplants. J Immunol 2001, 166:4185–4194.
Brouard S, Otterbein LE, Anrather J, Tobiasch E, Bach FH, Choi AM, Soares MP: Carbon monoxide generated by heme oxygenase-1 suppresses endothelial cell apoptosis. J Exp Med 2000, 192:1015–1026.
Suttner DM, Sridhar K, Lee CS, Tomura T, Hansen TN, Dennery PA: Protective effects of transient HO-1 overexpression on susceptibility to oxygen toxicity in lung cells. Am J Physiol 1999, 276:L443-L451.
Kvam E, Hejmadi V, Ryter S, Pourzand C, Tyrrell RM: Heme oxygenase activity causes transient hypersensitivity to oxidative ultraviolet a radiation that depends on release of iron from heme. Free Radic Biol Med 2000, 28:1191–1196.
Alam J: Multiple elements within the 5' distal enhancer of the mouse heme oxygenase-1 gene mediate induction by heavy metals. J Biol Chem 1994, 269:25049–25056.
Alam J, Camhi S, Choi AM: Identification of a second region upstream of the mouse heme oxygenase-1 gene that functions as a basal level and inducer-dependent transcription enhancer. J Biol Chem 1995, 270:11977–11984.
Choi AM, Alam J: Heme oxygenase-1: function, regulation, and implication of a novel stress-inducible protein in oxidant-induced lung injury. Am J Respir Cell Mol Biol 1996, 15:9–19.
Lavrovsky Y, Schwartzman ML, Levere RD, Kappas A, Abraham NG: Identification of binding sites for transcription factors NF-kappa B and AP-2 in the promoter region of the human heme oxygenase 1 gene. Proc Natl Acad Sci USA 1994, 91:5987–5991.
Lee PJ, Camhi SL, Chin BY, Alam J, Choi AM: AP-1 and STAT mediate hyperoxia-induced gene transcription of heme oxygenase-1. Am J Physiol Lung Cell Mol Physiol 2000, 279:L175-L182.
Lee PJ, Jiang BH, Chin BY, Iyer NV, Alam J, Semenza GL, Choi AM: Hypoxia-inducible factor-1 mediates transcriptional activation of the heme oxygenase-1 gene in response to hypoxia. J Biol Chem 1997, 272:5375–5381.
Walker E, Hay A: Carbon monoxide poisoning. BMJ 1999, 319:1082–1083.
Weaver LK: Carbon monoxide poisoning. Crit Care Clin 1999, 15:297–317.
Piantadosi CA: Carbon monoxide poisoning. N Engl J Med 2002, 347:1054–1055.
Vremen HJ, Wong RJ, Stevenson DK: Carbon monoxide in breath, blood, and other tissues. In Carbon Monoxide Toxicity (Edited by: Penney DG). Boca Raton, FL: CRC Press 2000, 19–60.
Duckers HJ, Boehm M, True AL, Yet SF, San H, Park JL, Clinton Webb R, Lee ME, Nabel GJ, Nabel EG: Heme oxygenase-1 protects against vascular constriction and proliferation. Nat Med 2001, 7:693–698.
Cardell LO, Ueki IF, Stjarne P, Agusti C, Takeyama K, Linden A, Nadel JA: Bronchodilatation in vivo by carbon monoxide, a cyclic GMP related messenger. Br J Pharmacol 1998, 124:1065–1068.
Kinhult J, Uddman R, Cardell LO: The induction of carbon monoxide-mediated airway relaxation by PACAP 38 in isolated guinea pig airways. Lung 2001, 179:1–8.
Fujita T, Toda K, Karimova A, Yan SF, Naka Y, Yet SF, Pinsky DJ: Paradoxical rescue from ischemic lung injury by inhaled carbon monoxide driven by derepression of fibrinolysis. Nat Med 2001, 7:598–604.
Morita T, Mitsialis SA, Koike H, Liu Y, Kourembanas S: Carbon monoxide controls the proliferation of hypoxic vascular smooth muscle cells. J Biol Chem 1997, 272:32804–32809.
Koehler RC, Traystman RJ: Cerebrovascular effects of carbon monoxide. Antioxid Redox Signal 2002, 4:279–290.
Ingi T, Cheng J, Ronnett GV: Carbon monoxide: an endogenous modulator of the nitric oxide-cyclic GMP signaling system. Neuron 1996, 16:835–842.
Wang R, Wang Z, Wu L: Carbon monoxide-induced vasorelaxation and the underlying mechanisms. Br J Pharmacol 1997, 121:927–934.
Kyriakis JM, Avruch J: Sounding the alarm: protein kinase cascades activated by stress and inflammation. J Biol Chem 1996, 271:24313–24316.
Nick JA, Avdi NJ, Young SK, McDonald PP, Billstrom MA, Henson PM, Johnson GL, Worthen GS: An intracellular signaling pathway linking lipopolysaccharide stimulation to cellular responses of the human neutrophil: the p38 MAP kinase cascade and its functional significance. Chest 1999, 116:54S-55S.
Petrache I, Otterbein LE, Alam J, Wiegand GW, Choi AM: Heme oxygenase-1 inhibits TNF-α-induced apoptosis in cultured fibroblasts. Am J Physiol Lung Cell Mol Physiol 2000, 278:L312-L319.
Hele DJ: Meeting report. New approaches to the modulation of inflammatory processes in airway disease models: ATS May 18–23, San Francisco. Respir Res 2001, 2:E003.
Rahman I, Morrison D, Donaldson K, MacNee W: Systemic oxidative stress in asthma, COPD, and smokers. Am J Respir Crit Care Med 1996, 154:1055–1060.
Donnelly LE, Barnes PJ: Expression of heme oxygenase in human airway epithelial cells. Am J Respir Cell Mol Biol 2001, 24:295–303.
Li N, Venkatesan MI, Miguel A, Kaplan R, Gujuluva C, Alam J, Nel A: Induction of heme oxygenase-1 expression in macrophages by diesel exhaust particle chemicals and quinones via the antioxidant-responsive element. Immunol 2000, 165:3393–3401.
Yasuda H, Yamaya M, Yanai M, Ohrui T, Sasaki H: Increased blood carboxyhaemoglobin concentrations in inflammatory pulmonary diseases. Thorax 2002, 57:779–783.
Wagner JA, Horvath SM, Dahms TE: Carbon monoxide elimination. Respir Physiol 1975, 23:41–47.
Maestrelli P, El Messlemani AH, De Fina O, Nowicki Y, Saetta M, Mapp C, Fabbri LM: Increased expression of heme oxygenase (HO)-1 in alveolar spaces and HO-2 in alveolar walls of smokers. Am J Respir Crit Care Med 2001, 164:1508–1513.
Middleton ET, Morice AH: Breath carbon monoxide as an indication of smoking habit. Chest 2000, 117:758–763.
Jarvis MJ, Russell MA, Saloojee Y: Expired air carbon monoxide: a simple breath test of tobacco smoke intake. Br Med J 1980, 281:484–485.
Donaldson K, Gilmour MI, MacNee W: Asthma and PM10. Respir Res 2000, 1:12–15.
MacNee W: Oxidative stress and lung inflammation in airways disease. Eur J Pharmacol 2001, 429:195–207.
O'byrne PM, Postma DS: The many faces of airway inflammation. Asthma and chronic obstructive pulmonary disease. Am J Respir Crit Care Med 1999, 159:S41-S63.
Kitada O, Kodama T, Kuribayashi K, Ihaku D, Fujita M, Matsuyama T, Sugita M: Heme oxygenase-1 protein induction in a mouse model of asthma. Clin Exp Allergy 2001, 31:1470–1477.
Horvath I, Donnelly LE, Kiss A, Paredi P, Kharitonov SA, Barnes PJ: Raised levels of exhaled carbon monoxide are associated with an increased expression of heme oxygenase-1 in airway macrophages in asthma: a new marker of oxidative stress. Thorax 1998, 53:668–672.
Harju T, Soini Y, Paakko R, Kinnula VL: Up-regulation of heme oxygenase-I in alveolar macrophages of newly diagnosed asthmatics. Respir Med 2002, 96:418–423.
Zayasu K, Sekizawa K, Okinaga S, Yamaya M, Ohrui T, Sasaki : Increased carbon monoxide in exhaled air of asthmatic patients. Am J Respir Crit Care Med 1997, 156:1140–1143.
Uasuf CG, Jatakanon A, James A, Kharitonov SA, Wilson NM, Barnes PJ: Exhaled carbon monoxide in childhood asthma. J Pediatr 1999, 135:569–574.
Yamaya M, Sekizawa K, Ishizuka S, Monma M, Sasaki H, Yamara M: Exhaled carbon monoxide levels during treatment of acute asthma. Eur Respir J 1999, 13:757–760.
Lim S, Groneberg D, Fischer A, Oates T, Caramori G, Mattos W, Adcock I, Barnes PJ, Chung KF: Expression of heme oxygenase isoenzymes 1 and 2 in normal and asthmatic airways: effect of inhaled corticosteroids. Am J Respir Crit Care Med 2000, 162:1912–1918.
Zanconato S, Scollo M, Zaramella C, Landi L, Zacchello F, Baraldi E: Exhaled carbon monoxide levels after a course of oral prednisone in children with asthma exacerbation. J Allergy Clin Immunol 2002, 109:440–445.
Paredi P, Leckie MJ, Horvath I, Allegra L, Kharitonov SA, Barnes PJ: Changes in exhaled carbon monoxide and nitric oxide levels following allergen challenge in patients with asthma. Eur Respir J 1999, 13:48–52.
Khatri SB, Ozkan M, McCarthy K, Laskowski D, Hammel J, Dweik RA, Erzurum SC: Alterations in exhaled gas profile during allergen-induced asthmatic response. Am J Respir Crit Care Med 2001, 164:1844–1848.
Andersson JA, Uddman R, Cardell LO: Increased carbon monoxide levels in the nasal airways of subjects with a history of seasonal allergic rhinitis and in patients with upper respiratory tract infection. Clin Exp Allergy 2002, 32:224–227.
Rutgers SR, Timens W, Kauffman HF, Postma DS: Markers of active airway inflammation and remodelling in chronic obstructive pulmonary disease. Clin Exp Allergy 2001, 31:193–205.
Croxton TL, Weinmann GG, Senior RM, Hoidal JR: Future research directions in COPD. Am J Respir Crit Care Med 2002, 165:838–844.
Lautier D, Luscher P, Tyrrell RM: Endogenous glutathione levels modulate both constitutive and UVA radiation/hydrogen peroxide inducible expression of the human heme oxygenase gene. Carcinogenesis 1992, 13:227–232.
Rahman I, MacNee W: Oxidative stress and regulation of glutathione in lung inflammation. Eur Respir J 2000, 16:534–554.
Ewing JF, Maines MD: Glutathione depletion induces heme oxygenase-1 (HSP32) mRNA and protein in rat brain. J Neurochem 1993, 60:1512–1519.
Horikawa S, Yoneya , Nagashima Y, Hagiwara K, Ozasa H: Prior induction of HO-1 with glutathione depletor ameliorates the renal ischemia and reperfusion in the rat. FEBS Lett 2002, 510:221–224.
Montuschi P, Kharitonov SA, Barnes PJ: Exhaled carbon monoxide and nitric oxide in COPD. Chest 2001, 120:496–501.
Slebos DJ, Kauffman HF, Rutgers SR, Dijkhuizen B, van Haelst PL, Choi AMK, Koeter GH, Postma DS: Haemoxygenase-1 expression in broncho-alveolar lavage fluid alveolar macrophages is diminished in patients with COPD abstract. Eur Respir J 2002, Suppl 38:404s.
Yamada N, Yamaya M, Okinaga S, Nakayama K, Sekizawa K, Shibahara S, Sasaki H: Microsatellite polymorphism in the heme oxygenase-1 gene promoter is associated with susceptibility to emphysema. Am J Hum Genet 2000, 66:187–195.
Koyama H, Geddes DM: Genes, oxidative stress, and the risk of COPD. Thorax 1998, 53:S10-S14.
Lomas DA, Silverman EK: The genetics of chronic obstructive pulmonary disease. Respir Res 2001, 2:20–26.
Paredi P, Shah PL, Montuschi P, Sullivan P, Hodson ME, Kharitonov SA, Barnes PJ: Increased carbon monoxide in exhaled air of patients with cystic fibrosis. Thorax 1999, 54:917–920.
Antuni JD, Kharitonov SA, Hughes D, Hodson ME, Barnes PJ: Increase in exhaled CO during exacerbations of cystic fibrosis. Thorax 2000, 55:138–142.
Paredi P, Kharitonov SA, Leak D, Shah PL, Cramer D, Hodson ME, Barnes PJ: Exhaled ethane is elevated in cystic fibrosis and correlates with carbon monoxide levels and airway obstruction. Am J Respir Crit Care Med 2000, 16:1247–1251.
Horvath I, Borka P, Apor P, Kollai M: Exhaled carbon monoxide concentration increases after exercise in children with cystic fibrosis. Acta Physiol Hung 1999, 86:237–244.
Biernacki WA, Kharitonov SA, Barnes PJ: Exhaled carbon monoxide in patients with lower respiratory tract infection. Respir Med 2001, 95:1003–1005.
Horvath I, Loukides S, Wodehouse T, Kharitonov SA, Cole PJ, Barnes PJ: Increased levels of CO in bronchiectasis: a new marker of oxidative stress. Thorax 1998, 53:867–870.
Lakari E, Pylkas P, Pietarinen-Runtti P, Paakko P, Soini Y, Kinnula VL: Expression and regulation of hemeoxygenase 1 in healthy human lung and interstitial lung disorders. Hum Pathol 2001, 32:1257–1263.
Dosanjh A, Morris RE, Wan B: Bronchial epithelial cell-derived cytokine IL-10 and lung fibroblast proliferation. Transplant Proc 2001, 33:352–354.
Lee TS, Chau LY: Heme oxygenase-1 mediates the anti-inflammatory effect of interleukin-10 in mice. Nat Med 2002, 8:240–246.
Tsuburai T, Suzuki M, Nagashima Y, Suzuki S, Inoue S, Hasiba T, Ueda A, Ikehara K, Matsuse T, Ishigatsubo Y: Adenovirus-mediated transfer and overexpression of heme oxygenase 1 cDNA in lung prevents bleomycin-induced pulmonary fibrosis via a Fas-Fas ligand-independent pathway. Hum Gene Ther 2002, 13:1945–1960.
Tsuji MH, Yanagawa T, Iwasa S, Tabuchi K, Onizawa K, Bannai S, Toyooka H, Yoshida H: Heme oxygenase-1 expression in oral squamous cell carcinoma as involved in lymph node metastasis. Cancer Lett 1999, 138:53–59.
Doi K, Akaike T, Fujii S, Tanaka S, Ikebe N, Beppu T, Shibahara S, Ogawa M, Maeda H: Induction of haem oxygenase-1 nitric oxide and ischaemia in experimental solid tumours and implications for tumour growth. Br J Cancer 1999, 80:1945–1954.
Kourembanas S: Hypoxia and carbon monoxide in the vasculature. Antioxid Redox Signal 2002, 4:291–299.
Carter EP, Hartsfield CL, Miyazono M, Jakkula M, Morris KG Jr, McMurtry IF: Regulation of heme oxygenase-1 by nitric oxide during hepatopulmonary syndrome. Am J Physiol Lung Cell Mol Physiol 2002, 283:L346-L353.
Schroeder RA, Ewing CA, Sitzmann JV, Kuo PC: Pulmonary expression of iNOS and HO-1 protein is upregulated in a rat model of prehepatic portal hypertension. Dig Dis Sci 2000, 45:2405–2410.
Yet SF, Perrella MA, Layne MD, Hsieh CM, Maemura K, Kobzik L, Wiesel P, Christou H, Kourembanas S, Lee ME: Hypoxia induces severe right ventricular dilatation and infarction in heme oxygenase-1 null mice. J Clin Invest 1999, 103:R23-R29.
Christou H, Morita T, Hsieh CM, Koike H, Arkonac B, Perrella MA, Kourembanas S: Prevention of hypoxia-induced pulmonary hypertension by enhancement of endogenous heme oxygenase-1 in the rat. Circ Res 2000, 86:1224–1229.
Minamino T, Christou H, Hsieh CM, Liu Y, Dhawan V, Abraham NG, Perrella MA, Mitsialis SA, Kourembanas S: Targeted expression of heme oxygenase-1 prevents the pulmonary inflammatory and vascular responses to hypoxia. Proc Natl Acad Sci US A 2001, 98:8798–8803.
Robbins CG, Horowitz S, Merritt TA, Kheiter A, Tierney J, Narula P, Davis JM: Recombinant human superoxide dismutase reduces lung injury caused by inhaled nitric oxide and hyperoxia. Am J Physiol 1997, 272:L903-L907.
Davis JM, Robbins CG, Anderson T, Sahgal N, Genen L, Tierney J, Horowitz S: The effects of hyperoxia, mechanical ventilation, and dexamethasone on pulmonary antioxidant enzyme activity in the newborn piglet. Pediatr Pulmonol 1995, 20:107–111.
Clark JM, Lambertson CJ: Pulmonary oxygen toxicity: a review. Pharmacol Rev 1971, 23:37–133.
Dennery PA, Lee CS, Ford BS, Weng Y-H, Yang G, Rodgers PA: Developmental expression of heme oxygenase in the rat lung. Pediatric Res 2003, 53:42–47.
Otterbein LE, Kolls JK, Mantell LL, Cook JL, Alam J, Choi AMK: Exogenous administration of heme oxygenase-1 by gene transfer provides protection against hyperoxia-induced lung injury. J Clin Invest 1999, 103:1047–1054.
Dennery PA, Sridhar KJ, Lee CS, Wong HE, Shokoohi V, Rodgers P, Spitz DR: Heme oxygenase-mediated resistance to oxygen toxicity in hamster fibroblasts. J Biol Chem 1997, 272:14937–14943.
Dennery PA, Spitz DR, Yang G, Tatarov A, Lee CS, Shegog ML, Poss KD: Oxygen toxicity and iron accumulation in the lungs of mice lacking heme oxygenase-2. J Clin Invest 1998, 101:1001–1011.
Dennery PA, Visner G, Weng Y-H, Nguyen X, Lu F, Zander D, Yang G: Resistance to hyperoxia with heme oxygenase-1 disruption: role of iron. Free Radic Biol Med 2003, 34:124–133.
Poss KD, Tonegawa S: Reduced stress defense in heme oxygenase-1 deficient cells. Proc Natl Acad Sci USA 1997, 94:10925–10930.
Poss KD, Tonegawa S: Heme oxygenase-1 is required for mammalian iron reutilization. Proc Natl Acad Sci USA 1997, 94:10919–10924.
Clayton CE, Carraway MS, Suliman HB, Thalmann ED, Thalmann KN, Schmechel DE, Piantadosi CA: Inhaled carbon monoxide and hyperoxic lung injury in rats. Am J Physiol Lung Cell Mol Physiol 2001, 281:L949-L957.
Taylor JL, Carraway MS, Piantadosi CA: Lung-specific induction of heme oxygenase-1 and hyperoxic lung injury. Am J Physiol 1998, 274:L582-L590.
Sokol J, Jacobs SE, Bohn D: Inhaled nitric oxide for acute hypoxemic respiratory failure in children and adults. Cochrane Database Syst Rev 2003, 1:CD002787.
Evans HE, Rosenfeld W, Jhaveri R, Concepcion L, Zabaleta I: Oxidant-mediated lung disease in newborn infants. J Free Radic Biol Med 1986, 2:369–372.
Hosenpud JD, Bennett LE, Keck BM, Boucek MM, Novick RJ: The registry of the international society for heart and lung transplantation: seventeenth official report. J Heart Lung Transplant 2000, 19:909–931.
Estenne M, Hertz MI: Bronchiolitis obliterans after human lung transplantation. Am J Respir Crit Care Med 2002, 166:440–444.
Hirsch J, Elssner A, Mazur G, Maier KL, Bittmann I, Behr J, Schwaiblmair M, Reichenspurner H, Furst H, Briegel J, Vogelmeier C: Bronchiolitis obliterans syndrome after (heart-)lung transplantation. Impaired antiprotease defense and increased oxidant activity. Am J Respir Crit Care Med 1999, 160:1640–1646.
Behr J, Maier K, Braun B, Schwaiblmair M, Vogelmeier C: Evidence for oxidative stress in bronchiolitis obliterans syndrome after lung and heart-lung transplantation. Transplantation 2000, 69:1856–1860.
Lu F, Zander DS, Visner GA: Increased expression of heme oxygenase-1 in human lung transplantation. J Heart Lung Transplant 2002, 21:1120–1126.
Avihingsanon Y, Ma N, Csizmadia E, Wang C, Pavlakis M, Giraldo M, Strom TB, Soares MP, Ferran C: Expression of protective genes in human renal allografts: a regulatory response to injury associated with graft rejection. Transplantation 2002, 73:1079–1085.
Woo J, Iyer S, Mori N, Buelow R: Alleviation of graft-versus-host disease after conditioning with cobalt-protoporphyrin, an inducer of HO-1. Transplantation 2000, 69:623–633.
Ke B, Buelow R, Shen XD, Melinek J, Amersi F, Gao F, Ritter T, Volk HD, Busuttil RW, Kupiec-Weglinski JW: Heme oxygenase-1 gene transfer prevents CD95/Fas ligand-mediated apoptosis and improves liver allograft survival via carbon monoxide signaling pathway. Hum Gene Ther 2002, 13:1189–1199.
Pileggi A, Molano RD, Berney T, Cattan P, Vizzardelli C, Oliver R, Fraker C, Ricordi C, Pastori RL, Bach FH, Inverardi L: Heme oxygenase-1 induction in islet cells results in protection from apoptosis and improved in vivo function after transplantation. Diabetes 2001, 50:1983–1991.
Tobiasch E, Gunther L, Bach FH: Heme oxygenase-1 protects pancreatic beta cells from apoptosis caused by various stimuli. J Invest Med 2001, 49:566–571.
Ke B, Shen XD, Melinek J, Gao F, Ritter T, Volk HD, Busuttil RW, Kupiec-Weglinski JW: Heme oxygenase-1 gene therapy: a novel immunomodulatory approach in liver allograft recipients? Transplant Proc 2001, 33:581–582.
Soares MP, Lin Y, Anrather J, Csizmadia E, Takigami K, Sato K, Grey ST, Colvin RB, Choi AM, Poss KD, Bach FH: Expression of heme oxygenase-1 can determine cardiac xenograft survival. Nat Med 1998, 4:1073–1077.
Sato K, Balla J, Otterbein L, Smith RN, Brouard S, Lin Y, Csizmadia E, Sevigny J, Robson SC, Vercellotti G, Choi AM, Bach FH, Soares MP: Carbon monoxide generated by heme oxygenase-1 suppresses the rejection of mouse-to-rat cardiac transplants. J Immunol 2001, 166:4185–4194.
Soncul H, Oz E, Kalaycioglu S: Role of ischemic preconditioning on ischemia-reperfusion injury of the lung. Chest 1999, 115:1672–1677.
Katori M, Anselmo DM, Busuttil RW, Kupiec-Weglinski JW: A novel strategy against ischemia and reperfusion injury: cytoprotection with heme oxygenase system. Transplant Immunol 2002, 9:227–233.
Katori M, Buelow R, Ke B, Ma J, Coito AJ, Iyer S, Southard D, Busuttil RW, Kupiec-Weglinski JW: Heme oxygenase-1 overexpression protects rat hearts from cold ischemia/reperfusion injury via an anti-apoptotic pathway. Transplantation 2002, 73:287–292.
Amersi F, Buelow R, Kato H, Ke B, Coito AJ, Shen XD, Zhao D, Zaky J, Melinek J, Lassman CR, Kolls JK, Alam J, Ritter T, Volk HD, Farmer DG, Ghobrial RM, Busuttil RW, Kupiec-Weglinski JW: Upregulation of heme oxygenase-1 protects genetically fat Zucker rat livers from ischemia/reperfusion injury. J Clin Invest 1999, 104:1631–1639.
Kato H, Amersi F, Buelow R, Melinek J, Coito AJ, Ke B, Busuttil RW, Kupiec-Weglinski JW: Heme oxygenase-1 overexpression protects rat livers from ischemia/reperfusion injury with extended cold preservation. Am J Transplant 2001, 1:121–128.
Immenschuh S, Ramadori G: Gene regulation of HO-1 as a therapeutic target. Biochem Pharmacol 2000, 60:1121–1128.
Melo LG, Agrawal R, Zhang L, Rezvani M, Mangi AA, Ehsan A, Griese DP, Dell'Acqua G, Mann MJ, Oyama J, Yet SF, Layne MD, Perrella MA, Dzau VJ: Gene therapy strategy for long-term myocardial protection using adeno-associated virus-mediated delivery of heme oxygenase gene. Circulation 2002, 105:602–607.
Motterlini R, Clark JE, Foresti R, Sarathchandra P, Mann BE, Green CJ: Carbon monoxide-releasing molecules: characterization of biochemical and vascular activities. Circ Res 2002, 90:E17-E24.
Underwood DC, Osborn RR, Bochnowicz S, Webb EF, Rieman DJ, Lee JC, Romanic AM, Adams JL, Hay DW, Griswold DE: SB 23 a p38 MAPK inhibitor, reduces neutrophilia, inflammatory cytokines, MMP-9, and fibrosis in lung. Am J Physiol Lung Cell Mol Physiol 9063, 279:L895-L902.
Zevin S, Saunders S, Gourlay SG, Jacob P, Benowtitz NL: Cardiovascular effects of carbon monoxide and cigarette smoking. J Am Col Cardiol 2001, 38:1633–1638.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Slebos, DJ., Ryter, S.W. & Choi, A.M. Heme oxygenase-1 and carbon monoxide in pulmonary medicine. Respir Res 4, 7 (2003). https://doi.org/10.1186/1465-9921-4-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1465-9921-4-7