Abstract
Objective
A multitude of factors promotes inflammation in the reproductive tract leading to preterm birth. Macrophages peak in the cervix prior to birth and their numbers are increased by the cytokine granulocyte-macrophage colony-stimulating factor (GM-CSF). We hypothesize GM-CSF is produced from multiple sites in the genital tract and is a key mediator in preterm birth.
Study Design
Ectocervical, endocervical, and amniotic fluid mesenchymal stem cells were treated with lipopolysaccharide (LPS), and the concentration and expression of GM-CSF was measured. Pregnant CD-1 mice on gestational day 17 received LPS and an intravenous injection of either anti-mouse GM-CSF or control antibody. After 6 hours, the preterm birth rate was recorded.
Results
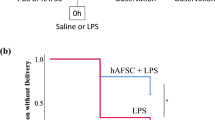
Treatment with LPS increased the GM-CSF concentration and messenger RNA expression after 24 hours in all 3 cell lines (P <.01). Mice treated with LPS and the GM-CSF antibody had a preterm birth rate of 25%, compared to a 66.7% preterm birth rate in controls, within 6 hours (P <.05, χ2). Treatment with the anti-mouse GM-CSF antibody decreased the concentration of GM-CSF in the mouse serum (P <.01) but did not alter the number of macrophages or collagen content in the cervix.
Conclusion
These studies demonstrate that GM-CSF is produced from multiple sites in the genital tract and that treatment with an antibody to GM-CSF prevents preterm birth. Curiously, the anti-mouse GM-CSF antibody did not decrease the number of macrophages in the cervix. Further research is needed to determine whether antibodies to GM-CSF can be utilized as a therapeutic agent to prevent preterm birth.
Similar content being viewed by others
References
Goldenbertg R, Culhane J, Iams J, Romero R. Epidemiology and causes of preterm birth. Lancet. 2008;371(9606):75–84.
Blencowe H, Cousens S, Oestergaard M, et al. National, regional and worldwide estimates of preterm birth. Lancet. 2012;379(9832):2162–2172.
Romero R, Dey S, Fisher S. Preterm labor: one syndrome, many causes. Science. 2014;345(6198):760–765.
Kemp W, Saito M, Newnham JP, Nitsos I, Okamura K, Kallapur SG. Preterm birth, infection, and inflammation advances from the study of animal models. Reprod Sci. 2010;17(7):619–628.
Huang WC, Sala-Newby GB, Susana A, Johnson JL, Newby AC. Classical macrophage activation up-regulates several matrix metalloproteinases through mitogen activated protein kinases and nuclear factor-kappaB. PLoS One. 2012;7(8):e42507.
Vadillo-Ortega F, Hernandez A, Gonzalez-Avila G, Bermejo L, Iwata K, Strauss J. Increased matrix metalloproteinase activity and reduced tissue inhibitor of metalloproteinases-1 levels in amniotic fluids from pregnancies complicated by premature rupture of membranes. Am J Obstet Gynecol. 1996;174(4):1371–1376.
Athayde N, Edwin SS, Romero R, et al. A role for matrix metalloproteinase-9 in spontaneous rupture of the fetal membranes. Am J Obstet Gynecol. 1998;179(5):1248–1253.
Xu P, Alfaidy N, Challis JR. Expression of matrix metalloproteinase (MMP)-2 and MMP-9 in human placenta and fetal membranes in relation to preterm and term labor. J Clin Endocrinol Metab. 2002;87(3):1353–1361.
Gomez-Lopez N, StLouis D, Lehr M, Sanchez-Rodriguez E, Arenas-Hernandez M. Immune cells in term and preterm labor. Cell Mol Immunol. 2014;11(6):571–581.
Yellon S, Dobyns A, Beck H, Kurtzman J, Garfield R, Kirby M. Loss of progesterone receptor-mediated actions induce preterm cellular and structural remodeling of the cervix and premature birth. PLoS One. 2013;8(12):e81340.
Kirby M, Heuerman A, Custer M, et al. Progesterone receptor-mediated actions regulate remodeling of the cervix in preparation for preterm parturition. Reprod Sci. 2016;23(11):1473–1483.
Yellon S. Contributions to the dynamics of cervix remodeling prior to term and preterm birth. Biol Reprod. 2017;96(1):13–23.
Cetean S, Căinap C, Constantin A, et al. The importance of the granulocyte-colony stimulating factor in oncology. Clujul Med. 2015;88(4):468–472.
Shi Y, Liu C, Roberts A, et al. Granulocyte-macrophage colony-stimulating factor (GM-CSF) and T-cell responses: what we do and don’t know. Cell Res. 2006;16(2):126–133.
Curry AE, Thorsen P, Drews C, et al. First-trimester maternal plasma cytokine levels, pre-pregnancy body mass index, and spontaneous preterm delivery. Acta Obstet Gynecol Scand. 2009;88(3):332–342.
Chandiramani M, Seed P, Orsi N, et al. Limited relationship between cervico-vaginal fluid cytokine profiles and cervical shortening in women at high risk of spontaneous preterm birth. PLoS One. 2012;7(12):e52412.
Basraon S, Menon R, Makhlouf M, et al. Can statins reduce the inflammatory response associated with preterm birth in an animal model? Am J Obstet Gynecol. 2012;207(3):224.e1–227.e1.
Phermthai T, Odglun Y, Julavijitphong S, et al. A novel method to derive amniotic fluid stem cells for therapeutic purposes. BMC Cell Biol. 2010;11:79. doi:https://doi.org/10.1186/1471-2121-11-79
Elovitz MA, Wang Z, Chien EK, Rychlik DF, Phillippe M. A new model for inflammation-induced preterm birth: the role of platelet-activating factor and toll-like receptor-4. Am J Pathol. 2003;163(5):2103–2111.
Kirby M, Heuerman A, Custer M et al. Progesterone receptor-mediated actions regulate remodeling of the cervix in preparation for preterm parturition. Reprod Sci. 2016;23(11):1473–1483.
Nold C, Maubert M, Anton L, Yellon S, Elovitz M. Prevention of preterm birth by progestational agents: what are the molecular mechanisms? Am J Obstet Gynecol. 2013;208(3):223.e1–223.e7.
Nold C, Anton L, Brown A, Elovitz M. Inflammation promotes a cytokine response and disrupts the cervical epithelial barrier: a possible mechanism of premature cervical remodeling and preterm birth. Am J Obstet Gynecol. 2012;206(3):208.e1–208.e7.
Bastek J, Gómez L, Elovitz M. The role of inflammation and infection in preterm birth. Clin Perinatol. 2011;38(3):385–406.
Menon R, Fortunato S. Infection and the role of inflammation in preterm premature rupture of the membranes. Best Pract Res Clin Obstet Gynaecol. 2007;21(3):467–478.
Basraon S, Costantine M, Saade G, Menon R. The effect of simvastatin on infection-induced inflammatory response of human fetal membranes. Am J Reprod Immunol. 2015;74(1):54–61.
Gonzalez J, Pedroni S, Girardi G. Statins prevent cervical remodeling, myometrial contractions and preterm labor through a mechanism that involves hemoxygenase-1 and complement inhibition. Mol Hum Reprod. 2014;20(6):579–589.
Shynlova O, Dorogin A, Li Y, Lye S. Inhibition of infection-mediated preterm birth by administration of broad spectrum chemokine inhibitor in mice. J Cell Mol Med. 2014;18(9):1816–1829.
Arango Duque G, Descoteaux A. Macrophage cytokines: involvement in immunity and infectious diseases. Front Immunol. 2014;5:491.
Gonzalez JM, Romero R, Girardi G. Comparison of the mechanisms responsible for cervical remodeling in preterm and term labor. J Reprod Immunol. 2013;97(1):112–119.
Gonzalez J, Franzke C, Yang F, Romero R, Girardi G. Complement activation triggers metalloproteinases release inducing cervical remodeling and preterm birth in mice. Am J Pathol. 2011;179(2):838–849.
Yellon S, Ebner CA, Elovitz M. Medroxyprogesterone acetate modulates remodeling, immune cell census, and nerve fibers in the cervix of a mouse model for inflammation-induced preterm birth. Reprod Sci. 2009;16(3):257–264.
Parisi L, Gini E, Baci D, et al. Macrophage polarization in chronic inflammatory diseases: killers or builders? J Immunol Res. 2018;2018:8917804.
Dos Anjos Cassado A. F4/80 as a major macrophage marker: the case of the peritoneum and spleen. Results Probl Cell Differ. 2017;62:161–179.
Wang Y, Weng Y, Shi Y, Xia X, Wang S, Duan H. Expression and functional analysis of Toll-like receptor 4 in human cervical carcinoma. J Membr Biol. 2014;247(7):591–599.
Schioppo T, Ingegnoli F. Current perspective on rituximab in rheumatic diseases. Drug Des Devel Ther. 2017;11:2891–2904.
Marin-Acevedo J, Soyano A, Dholaria B, Knutson K, Lou Y. Cancer immunotherapy beyond immune checkpoint inhibitors. J Hematol Oncol. 2018;11(1):8.
McGinty L, Kolesar J. Dinutuximab for maintenance therapy in pediatric neuroblastoma. Am J Health Syst Pharm. 2017;74(8):563–567.
Shiomi A, Usui T, Mimori T. GM-CSF as a therapeutic target in autoimmune diseases. Inflamm Regen. 2016;36:8.
Elovitz M, Mrinalini C. Animal models of preterm birth. Trends Endocrinol Metab. 2004;15(10):479–487.
Mitchell B, Taggart M. Are animal models relevant to key aspects of human parturition? Am J Physiol Regul Integr Comp Physiol. 2009;297(3):R525–R545.
Liggins G. Premature delivery of foetal lambs infused with glucocorticoids. J Endocrinol. 1969;45(4):515–523.
Author information
Authors and Affiliations
Corresponding author
Additional information
Authors’ Note
This research was conducted at the University of Connecticut School of Medicine in Farmington, Connecticut, and Loma Linda University in Loma Linda, California.
Rights and permissions
About this article
Cite this article
Nold, C., Stone, J., O’Hara, K. et al. Block of Granulocyte-Macrophage Colony-Stimulating Factor Prevents Inflammation-Induced Preterm Birth in a Mouse Model for Parturition. Reprod. Sci. 26, 551–559 (2019). https://doi.org/10.1177/1933719118804420
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719118804420