Abstract
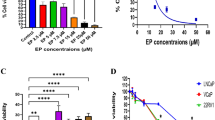
Overexpression of peroxisome proliferator activator receptor γ (PPARγ) has been implicated in many types of cancer including cervical cancer. Radiation therapy remains the main nonsurgical modality for the treatment of cervical cancer. The present study reports the impact of pharmacological inhibition of PPARγ in enhancing the radiosensitization of cervical cancer cells in vitro. Three cervical cancer cell lines (HeLa, SiHa, and Me180) were treated with a PPARγ inhibitor, T0070907, and/or radiation. The changes in protein, cell cycle, DNA content, apoptosis, and cell survival were analyzed. The PPARγ is differentially expressed in cervical cancer cells with maximum expression in ME180 cells. T0070907 has significantly decreased the tubulin levels in a time-dependent manner in ME180 cells. The decrease in the tubulin levels after T0070907 in ME180 and SiHa cells was associated with significant increase in the cells at the G2/M phase. The changes in the tubulin and G2/M phase were not evident in HeLa cells. T0070907 reduced the protein levels of PPARγ; however, PPARγ silencing had no effect on the α-tubulin level in ME180 cells suggesting the PPARγ-dependent and -independent actions of T0070907. To ascertain the impact of synergistic effect of T0070907 and radiation, HeLa and ME180 cells were pretreated with T0070907 and subjected to radiation (4 Gy). Annexin V-fluorescein isothiocyanate analysis revealed increased apoptosis in cells treated with radiation and T0070907 when compared to control and individual treatment. In addition, T0070907 pretreatment enhanced radiation-induced tetraploidization reinforcing the additive effect of T0070907. Confocal analysis of tubulin confirmed the onset of mitotic catastrophe in cells treated with T0070907 and radiation. These results strongly suggest the radiosensitizing effects of T0070907 through G2/M arrest and mitotic catastrophe.
Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61(2):69–90.
Woodman CB, Collins SI, Young LS. The natural history of cervical HPV infection: unresolved issues. Nat Rev Cancer. 2007;7(1):11–22.
Martelli ML, Iuliano R, Le Pera I, et al. Inhibitory effects of peroxisome proliferator-activated receptor gamma on thyroid carcinoma cell growth. J Clin Endocrinol Metab. 2002;87(10):4728–4735.
Panigrahy D, Shen LQ, Kieran MW, Kaipainen A. Therapeutic potential of thiazolidinediones as anticancer agents. Expert Opin Investig Drugs. 2003;12(12):1925–1937.
Han S, Inoue H, Flowers LC, Sidell N. Control of COX-2 gene expression through peroxisome proliferator-activated receptor gamma in human cervical cancer cells. Clin Cancer Res. 2003; 9(12):4627–4635.
Posch MG, Zang C, Mueller W, Lass U, von Deimling A, Elstner E. Somatic mutations in peroxisome proliferator-activated receptor-gamma are rare events in human cancer cells. Med Sci Monit. 2004;10(8):BR250–BR254.
Lefebvre AM, Chen I, Desreumaux P, et al. Activation of the peroxisome proliferator-activated receptor gamma promotes the development of colon tumors in C57BL/6J-APCMin/+ mice. Nat Med. 1998;4(9): 1053–1057.
Saez E, Tontonoz P, Nelson MC, et al. Activators of the nuclear receptor PPARgamma enhance colon polypformation. Nat Med. 1998;4(9):1058–1061.
Kristiansen G, Jacob J, Buckendahl AC, et al. Peroxisome proliferator-activated receptor gamma is highly expressed in pancreatic cancer and is associated with shorter overall survival times. Clin Cancer Res. 2006;12(21):6444–6451.
Schaefer KL, Takahashi H, Morales VM, et al. PPARgamma inhibitors reduce tubulin protein levels by a PPARgamma, PPARdelta and proteasome-independent mechanism, resulting in cell cycle arrest, apoptosis and reduced metastasis of colorectal carcinoma cells. Int J Cancer. 2007;120(3):702–713.
Lee G, Elwood F, McNally J, et al. T0070907, a selective ligand for peroxisome proliferator-activated receptor gamma, functions as an antagonist of biochemical and cellular activities. J Biol Chem. 2002;277(22):19649–19657.
Nakajima A, Tomimoto A, Fujita K, et al. Inhibition of peroxisome proliferator-activated receptor gamma activity suppresses pancreatic cancer cell motility. Cancer Sci. 2008;99(10):1892–900.
Takahashi H, Fujita K, Fujisawa T, et al. Inhibition of peroxisome proliferator-activated receptor gamma activity in esophageal carcinoma cells results in a drastic decrease of invasive properties. Cancer Sci. 2006;97(9):854–860.
Burton JD, Goldenberg DM, Blumenthal RD. Potential of peroxisome proliferator-activated receptor gamma antagonist compounds as therapeutic agents for a wide range of cancer types. PPAR Res. 2008;2008:494161.
Kim KR, Choi HN, Lee HJ, et al. A peroxisome proliferator-activated receptor gamma antagonist induces vimentin cleavage and inhibits invasion in high-grade hepatocellular carcinoma. Oncol Rep. 2007;18(4):825–832.
Hall EJ, Giaccia AJ. Radiosensitivity and cell age in the mitotic cycle. In: Lippincott Williams and Wilkins, eds. Radiobiology for the Radiologist. 7th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2011:54–66.
Tsao MS, Earp HS, Grisham JW. Gradation of carcinogen-induced capacity for anchorage-independent growth in cultured rat liver epithelial cells. Cancer Res. 1985;45(9):4428–4432.
Landsverk KS, Lyng H, Stokke T. The response of malignant B lymphocytes to ionizing radiation: cell cycle arrest, apoptosis and protection against the cytotoxic effects of the mitotic inhibitor nocodazole. Radiat Res. 2004;162(4):405–415.
Pines J, Hunter T. Human cyclin A is adenovirus E1A-associated protein p60 and behaves differently from cyclin B. Nature. 1990; 346(6286):760–763.
Innocente SA, Abrahamson JL, Cogswell JP, Lee JM. p53 regulates a G2 checkpoint through cyclin B1. Proc Natl Acad Sci U S A. 1999;96(5):2147–2152.
Niméus-Malmström E, Koliadi A, Ahlin C, et al. Cyclin B1 is a prognostic proliferation marker with a high reproducibility in a population-based lymph node negative breast cancer cohort. Int J Cancer. 2010;127(4):961–967.
Kosacka M, Korzeniewska A, Jankowska R. The evaluation of prognostic value of cyclin B1 expression in patients with resected non-small-cell lung cancer stage I-IIIA–preliminary report [in Polish]. Pol Merkur Lekarski. 2010;28(164):117–121.
Weaver BA, Cleveland DW. Decoding the links between mitosis, cancer, and chemotherapy: The mitotic checkpoint, adaptation, and cell death. Cancer Cell. 2005;8(1):7–12.
Yamada HY, Gorbsky GJ. Spindle checkpoint function and cellular sensitivity to antimitotic drugs. Mol Cancer Ther. 2006;5(12): 2963–2969.
Eriksson D, Joniani HM, Sheikholvaezin A, et al. Combined low dose radio- and radioimmunotherapy of experimental HeLa Hep 2 tumours. Eur J Nucl Med Mol Imaging. 2003;30(6):895–906.
Eriksson D, Löfroth PO, Johansson L, Riklund KA, Stigbrand T. Cell cycle disturbances and mitotic catastrophes in HeLa Hep2 cells following 2.5 to 10 Gy of ionizing radiation. Clin Cancer Res. 2007;13(18 pt 2):5501s-5508s.
Castedo M, Kroemer G. Mitotic catastrophe: a special case of apoptosis [in French]. J Soc Biol. 2004;198(2):97–103.
Erenpreisa J, Kalejs M, Ianzini F, et al. Segregation of genomes in polyploid tumour cells following mitotic catastrophe. Cell Biol Int. 2005;29(12):1005–1011.
Roninson IB, Broude EV, Chang BD. If not apoptosis, then what? Treatment-induced senescence and mitotic catastrophe in tumor cells. Drug Resist Updat. 2001;4(5):303–313.
Rieder CL, Maiato H. Stuck in division or passing through: what happens when cells cannot satisfy the spindle assembly checkpoint. Dev Cell. 2004;7(5):637–651.
Kerr JF, Wyllie AH, Currie AR. Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer. 1972;26(4):239–257.
Ferri KF, Kroemer G. Organelle-specific initiation of cell death pathways. Nat Cell Biol. 2001;3(11):E255–E263.
Brenner C, Kroemer G. Apoptosis. Mitochondria–the death signal integrators. Science. 2000; 289(5482):1150–1151.
Ravagnan L, Roumier T, Kroemer G. Mitochondria, the killer organelles and their weapons. J Cell Physiol. 2002;192(2):131–137.
Castedo M, Perfettini JL, Roumier T, Andreau K, Medema R, Kroemer G. Cell death by mitotic catastrophe: a molecular definition. Oncogene. 2004;23(16):2825–2837.
Xiao Z, Chen Z, Gunasekera AH, et al. Chk1 mediates S and G2 arrests through Cdc25A degradation in response to DNA-damaging agents. J Biol Chem. 2003;278(24):21767–2173.
Ashwell S, Zabludoff S. DNA damage detection and repair pathways—recent advances with inhibitors of checkpoint kinases in cancer therapy. Clin Cancer Res. 2008;14(13):4032–4037.
Burton JD, Castillo ME, Goldenberg DM, Blumenthal RD. Peroxisome proliferator-activated receptor-gamma antagonists exhibit potent antiproliferative effects versus many hematopoietic and epithelial cancer cell lines. Anticancer Drugs. 2007;18(5):525–534.
Kim KY, Kim SS, Cheon HG. Differential anti-proliferative actions of peroxisome proliferator-activated receptor-gamma agonists in MCF-7 breast cancer cells. Biochem Pharmacol. 2006;72(5):530–540.
Tachibana K, Yamasaki D, Ishimoto K, Doi T. The role of PPARs in cancer. PPAR Res. 2008;2008:102737.
Lea MA, Sura M, Desbordes C. Inhibition of cell proliferation by potential peroxisome proliferator-activated receptor (PPAR) gamma agonists and antagonists. Anticancer Res. 2004;24(5A): 2765–2771.
Zaytseva YY, Wallis NK, Southard RC, Kilgore MW. The PPARgamma antagonist T0070907 suppresses breast cancer cell proliferation and motility via both PPARgamma-dependent and -independent mechanisms. Anticancer Res. 2011;31(3):813–823.
Kumala S, Niemiec P, Widel M, Hancock R, Rzeszowska-Wolny J. Apoptosis and clonogenic survival in three tumour cell lines exposed to gamma rays or chemical genotoxic agents. Cell Mol Biol Lett. 2003;8(3):655–665.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
An, Z., Muthusami, S., Yu, JR. et al. T0070907, a PPAR γ Inhibitor, Induced G2/M Arrest Enhances the Effect of Radiation in Human Cervical Cancer Cells Through Mitotic Catastrophe. Reprod. Sci. 21, 1352–1361 (2014). https://doi.org/10.1177/1933719114525265
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719114525265