Abstract
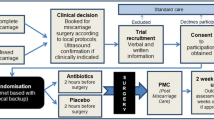
We did a double-blind, randomized, placebo-controlled study to assess the incidence of infectious complications and the protective effect of antibiotic administration during operative hysteroscopic procedures in an office setting. A total of 1046 consecutively enrolled women with intrauterine lesions were randomly allocated to the reference group (523 patients administered with 1 g of cefazolin intramuscularly) and the study group (523 patients administered with 10 mL of isotonic sodium chloride solution), and treated in office setting by operative hysteroscopy for endometrial polypectomy, uterine septa, submucosal myomas, and intrauterine adhesions. The primary outcome measure was the computation of difference between groups in postsurgical infectious complications occurring in the 5 days after the procedures. The time spent in performing the various procedures did not differ significantly (P > .05) between the groups. With respect to the overall rate of postsurgical infection, we found that 12 (1.15%) of 1046 patients referred with symptoms related to infective complications, 7 (1.3% of 523 women) in the study—untreated—group and 5 (1.0% of 523 women) in the reference group. Such incidences did not differ significantly between the groups (P > .05). Antibiotics were prescribed in all cases of postsurgical infection and the infective process resolved in few days. None of these patients developed serious infections with adnexal involvement, as confirmed by clinical and ultrasounds evaluation. The results of the current study would support the American College of Obstetricians and Gynecologists recommendation not to prescribe routine antibiotic administration in the case of hysteroscopic surgery.
Similar content being viewed by others
References
Bettocchi S, Nappi L, Ceci O, Selvaggi L. What does ‘‘diagnostic hysteroscopy’’ mean today? The role of the new techniques. Curr Opin Obstet Gynecol. 2003;15(4):303–308.
Bettocchi S, Nappi L, Ceci O, Selvaggi L. Office hysteroscopy. Obstet Gynecol Clin North Am. 2004;31(3):641–654.
Bettocchi S, Ceci O, Di Venere R, et al. Advanced operative office hysteroscopy without anaesthesia: analysis of 501 cases treated with a 5 Fr. bipolar electrode. Hum Reprod. 2002;17(9): 2435–2438.
Thinkhamrop J, Laopaiboon M, Lumbiganon P. Prophylactic antibiotics for transcervical intrauterine procedures. Cochrane Database Syst Rev. 2007;(3):CD005637.
Su HY, Ding DC, Chen DC, Lu MF, Liu JY, Chang FY. Prospective randomized comparison of single-dose versus 1-day cefazolin for prophylaxis in gynecologic surgery. Acta Obstet Gynecol Scand. 2005;84(4):384–389.
The American College of Obstetricians and Gynecologists. Antibiotic prophylaxis for gynaecologic procedures. Obstet Gynecol. 2009;13(5):1180–1189.
Aydeniz B, Gruber IV, Schauf B, Kurek R, Meyer A, Wallwiener D. A multicenter survey of complications associated with 21,676 operative hysteroscopies. Eur J Obstet Gynecol Reprod Biol. 2002;104(2):160–164.
Jansen FW, Vredevoogd CB, van Ulzen K, Hermans J, Trimbos JB, Trimbos-Kemper TC. Complications of hysteroscopy: a prospective, multicenter study. Obstet Gynecol. 2000;96(2): 266–270.
Munro MG. Complications of hysteroscopic and uterine resectoscopic surgery. Obstet Gynecol Clin North Am. 2010; 37(3):399–425.
Pocok SJ, Simon R. Sequential assignment with balancing for prognostic factors in the controlled clinical trial. Biometrics. 1975;31(3):103–215.
Bettocchi S, Ceci O, Nappi L, Pontrelli G, Pinto L, Vicino M. Office hysteroscopic metroplasty: three ‘‘diagnostic criteria’’ to differentiate between septate and bicornuate uteri. J Minim Invasive Gynecol. 2007;14(3):324–332.
Di Spiezio Sardo A, Mazzon I, Bramante S, et al. Hysteroscopic myomectomy: a comprehensive review of surgical techniques. Hum Reprod Update. 2008;14(2):101–119.
Mittendorf R, Aronson MP, Berry RE, et al. Avoiding serious infections associated with abdominal hysterectomy: a meta-analysis of antibiotic prophylaxis. Am J Obstet Gynecol. 1993;169(5):1119–1124.
American College of Obstetricians and Gynecologists. ACOG practice bulletin number 47, October 2003: prophylactic antibiotics in labor and delivery. Obstet Gynecol. 2003;102(4): 875–882.
Chelmow D, Ruehli MS, Huang E. Prophylactic use of antibiotics for non labouring patients undergoing caesarean delivery with intact membranes: a meta-analysis. Am J Obstet Gynecol. 2001; 184(4):656–661.
Hopkins L, Smaill FM. Withdrawn: antibiotic prophylaxis regimens and drugs for cesarean section. Cochrane Database Syst Rev. 2012;1:CD001136.
Thinkhamrop J, Laopaiboon M, Lumbiganon P. Prophylactic antibiotics for transcervical intrauterine procedures. Cochrane Database Syst Rev. 2007;(3):CD005637.
Kasius JC, Broekmans FJ, Fauser BC, Devroey P, Fatemi HM. Antibiotic prophylaxis for hysteroscopy evaluation of the uterine cavity. Fertil Steril. 2011;95(2):792–794.
Agostini A, Cravello L, Shojai R, Ronda I, Roger V, Blanc B. Postoperative infection and surgical hysteroscopy. Fertil Steril. 2002;77(4):766–768.
Bhattacharya S, Parkin DE, Reid TMS, Abramovich DR, Mollison J, Kitchener HC. A prospective randomised study of the effects of prophylactic antibiotics on the incidence of bacteraemia following hysteroscopic surgery. Eur J Obstet Gynecol Reprod Biol. 1995;63(1):37–40.
Idsoe O, Guthe T, Willcox RR, de Weck AL. Nature and extent of penicillin side-reactions, with particular reference to fatalities from anaphylactic shock. Bull World Health Organ. 1968;38(2):159–188.
Soderstrom RM. Distending the uterus: what medium is best? Clin Obstet Gynecol. 1992;35(2):225–228.
Baker VL, Adamson GD. Intrauterine pressure and uterine distention. J Am Assoc Gynecol Laparosc. 1996;3(suppl 4):S3.
Bassil S, Nissole M, Donnez J. Complications of endoscopic surgery in gynaecology. Gynaecol Endosc. 1993;2:195–197.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nappi, L., Di Spiezio Sardo, A., Spinelli, M. et al. A Multicenter, Double-Blind, Randomized, Placebo-Controlled Study to Assess Whether Antibiotic Administration Should Be Recommended During Office Operative Hysteroscopy. Reprod. Sci. 20, 755–761 (2013). https://doi.org/10.1177/1933719112466308
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719112466308