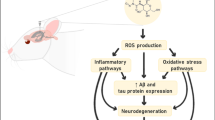
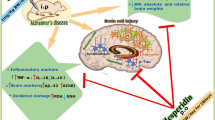
Abstract
Glutamate antibodies intranasally administered to Wistar rats at a dose of 300 μg/kg reduced the elevated levels of expression of Aifml, Casp3, and Parp1 genes in the prefrontal cortex and Aifml and Casp3 genes in the hippocampus on the third day after administration of the β-amyloid fragment Aβ25–35 into the Meynert nuclei of the brain. Changes in Aifm1, Bax, Casp3, and Parp1 gene expression were not found in the hypothalamus, and changes in Bax gene expression were not found in the brain structures studied. The discovered features of gene expression in the prefrontal cortex and hippocampus are considered in terms of development of various cell-death programs, which are modulated by glutamate antibodies.
Similar content being viewed by others
References
Acute Neuronal Injury: The Role of Excitotoxic Programmed Cell Death Mechanisms, Fujikawa, D.G., Ed., New York: Springer, 2010.
Ayala-Grosso, C., Ng, G., Roy, S., and Robertson, G.S., Caspase-cleaved amyloid precursor protein in Alzheimer’s disease, Brain Pathol., 2002, vol. 12, no. 4, pp. 430–441.
Benilova, I., Karran, E., and De Strooper, B., The toxic Aβ oligomer and Alzheimer’s disease: an emperor in need of clothes, Nat. Neurosci., 2012, vol. 15, no. 3, pp. 349–357.
Cheung, E.C., Melanson-Drapeau, L., Cregan, S.P., et al., Apoptosis-inducing factor is a key factor in neuronal cell death propagated by BAX-dependent and BAX-independent mechanisms, J. Neurosci., 2005, vol. 25, no. 6, pp. 1324–1334.
Cregan, S.P., Dawson, V.L., and Slack, R.S., Role of AIF in caspase-dependent and caspase-independent cell death, Oncogene, 2004, vol. 23, no. 16, pp. 2785–2796.
Evseev, V.A., Antitela k neiromediatoram v mekhanizmakh neiroimmunopatologii (Antibodies to the Neurotransmitters in the Mechanisms of Neuroimmunopathology), Moscow: Izd. Ross. Akad. Med. Nauk, 2007.
Evseev, V.A., Vetrile, L.A., Smirnova, V.S., et al., Autoantibodies against glutamate, gamma-aminobutyric acid, and norepinephrine in mechanisms of neuropathic pain syndrome, Bull. Exp. Biol. Med., 2008, vol. 145, no. 5, pp. 584–587.
Evseev, V.A., Vetrile, L.A., and Zakharova, I.A., Involvement of autoantibodies to neurotransmitters in mechanisms of stress reaction in rats, Bull. Exp. Biol. Med., 2010, vol. 149, no. 5, pp. 687–690.
Giovannelli, L., Casamenti, F., Scali, C., et al., Differential effects of amyloid peptides beta-(1–40) and beta-(25–35) injections into the rat nucleus basalis, Neuroscience, 1995, vol. 66, no. 4, pp. 781–792.
Gorbatov, V.Yu., Trekova, N.A., Fomina, V.G., and Davydova, T.V., Antiamnestic effects of antibodies to glutamate in experimental Alzheimer’s disease, Bull. Exp. Biol. Med., 2010, vol. 150, no. 7, pp. 23–25.
Gritti, I., Mainville, L., Mancia, M., and Jones, B.E., GABAergic and other noncholinergic basal forebrain neurons, together with cholinergic neurons, project to the mesocortex and isocortex in the rat, J. Comp. Neurol., 1997, vol. 383, no. 2, pp. 163–177.
Gruden, M.A., Storozheva, Z.I., Sewell, R.D.E., et al., Distinct functional brain regional integration of Casp3, Ascl1 and S100a6 gene expression in spatial memory, Behav. Brain Res., 2013, vol. 252, pp. 230–238.
Gulyaeva, N.V., “Apoptotic” mechanisms in normal brain plasticity: caspase-3 and long-term potentiation, Zh. Vyssh. Nervn. Deyat., 2004, vol. 54, no. 4, pp. 437–447.
Hardy, J. and Higgins, G.A., Alzheimer’s disease: the amyloid cascade hypothesis, Science, 1992, vol. 256, no. 5054, pp. 184–185.
Harkany, T., O’Mahony, S., Kelly, J.P., et al., Beta-amyloid(Phe(SO3H)24)25–35 in rat nucleus basalis induces behavioral dysfunctions, impairs learning and memory and disrupts cortical cholinergic innervation, Behav. Brain. Res., 1998, vol. 90, no. 2, pp. 133–145.
Harkany, T., Abrahám, I., Timmerman, W., et al., Betaamyloid neurotoxicity is mediated by a glutamate-triggered excitotoxic cascade in rat nucleus basalis, Eur. J. Neurosci., 2000, vol. 12, no. 8, pp. 2735–2745.
Jellinger, K.A. and Stadelmann, C., Problems of cell death in neurodegeneration and Alzheimer’s disease, J. Alzheimer’s Dis., 2001, vol. 3, no. 1, pp. 31–40.
Jimenez, S., Baglietto-Vargas, D., Caballero, C., et al., Inflammatory response in the hippocampus of PS-1M146L/APP751SL mouse model of Alzheimer’s disease: age-dependent switch in the microglial phenotype from alternative to classic, J. Neurosci., 2008, vol. 28, no. 45, pp. 11650–11661.
Kauppinen, T.M., Suh, S.W., Higashi, Y., et al., Poly(ADP-ribose)polymerase-1 modulates microglial responses to amyloid β, J. Neuroinflammat., 2011, vol. 8, p. 152. doi: 10.1186/1742-2094-8-152
Kermer, P., Liman, J., Weishaupt, J.H., and Bähr, M., Neuronal apoptosis in neurodegenerative disease: from basic research to clinical application, Neurodegener. Dis., 2004, vol. 1, no. 1, pp. 9–19.
Kolobov, V.V., Fomina, V.G., and Davydova, T.V., Antibodies to glutamate reduce the neurotoxic effects of Aβ25–35 in prefrontal cortex cell transcriptome, Dokl. Akad. Nauk, 2012a, vol. 447, no. 3, pp. 277–279.
Kolobov, V.V., Davydova, T.V., Zakharova, I.A., et al., Glutamate antibodies repress expression of Dffb gene in brain of rats in experimental Alzheimer’s disease, Mol. Biol. (Moscow), 2012b, vol. 46, no. 5, pp. 678–686.
Kolobov, V.V., Zakharova, I.A., Fomina, V.G., et al., Effect of antibodies to glutamate on caspase-3 activity in brain structures of rats with experimental Alzheimer’s disease, Bull. Exp. Biol. Med., 2013a, vol. 154, no. 10, pp. 425–427.
Kolobov, V.V., Fomina, V.G., Gorbatov, V.Yu., and Davydova, T.V., Comparison of the effects of glutamate antibodies on neuronal caspase-3 activity and memory disorders in rats caused by the administration of Aβ25–35 into the Meynert nucleus, Patol. Fiziol. Eksp. Ter., 2013b, no. 1, pp. 27–32.
Krantic, S., Mechawar, N., Reix, S., and Quirion, R., Molecular basis of programmed cell death involved in neurodegeneration, Trends Neurosci., 2005, vol. 28, no. 12, pp. 670–676.
Kubo, T., Nishimura, S., Kumagae, Y., and Kaneko, I., In vivo conversion of racemized beta-amyloid ([D-Ser26]Aβ1–40) to truncated and toxic fragments ([D-Ser26]Aβ25–35/40) and fragment presence in the brains of Alzheimer’s patients, J. Neurosci. Res., 2002, vol. 70, no. 3, pp. 474–483.
Livak, K.J. and Schmittgen, T.D., Analysis of relative gene expression data using real-time quantitative PCR and the 2-ΔΔC(T) method, Methods, 2001, vol. 25, no. 4, pp. 402–408.
Lorenzo, H.K. and Susin, S.A., Therapeutic potential of AIF-mediated caspase-independent programmed cell death, Drug Resist. Updat., 2007, vol. 10, no. 6, pp. 235–255.
Miller, T.M., Moulder, K.L., Knudson, C.M., et al., BAX deletion further orders the cell death pathway in cerebellar granule cells and suggests a caspase-independent pathway to cell death, J. Cell Biol., 1997, vol. 139, no. 1, pp. 205–217.
Parson, C.G., Stöffler, A., and Danysz, W., Memantine: a NMDA receptor antagonist that improves memory by restoration of homeostasis in the glutamatergic system—too little activation is bad, too much is even more, Neuropharmacology, 2007, vol. 53, no. 6, pp. 699–723.
Paxinos, G. and Watson, C., The Rat Brain in Stereotaxic Coordinates, Amsterdam: Elsevier Acad. Press, 2007.
Pike, C.J., Walencewicz-Wasserman, A.J., Kosmoski, J., et al., Structure-activity analyses of beta-amyloid peptides: contributions of the beta 25–35 region to aggregation and neurotoxicity, J. Neurochem., 1995, vol. 64, no. 1, pp. 253–265.
Reix, S., Mechawar, N., Susin, S.A., et al., Expression of cortical and hippocampal apoptosis-inducing factor (AIF) in aging and in Alzheimer’s disease, Neurobiol. Aging, 2007, vol. 28, no. 3, pp. 351–356.
Revett, T.J., Baker, G.B., Jhamandas, J., and Kar, S., Glutamate system, amyloid β peptides and tau protein: functional interrelationships and relevance to Alzheimer’s disease pathology, J. Psychiatry Neurosci., 2013, vol. 38, no. 3, pp. 6–23.
Sorokina, S.Yu., Kuptsov, V.N., Urban, Yu.N., et al., Data-bases as instruments for analysis of large-scale data sets of interactions between molecular biological objects, Biol. Bull. (Moscow), 2013, vol. 40, no. 3, pp. 233–242.
Stepanichev, M.Yu., Zdobnova, I.M., Zarubenko, I.I., et al., Amyloid-beta-(25–35)-induced memory impairments correlate with cell loss in rat hippocampus, Physiol. Behav., 2004, vol. 80, no. 5, pp. 647–655.
Tang, Y., Scott, D.A., Das, U., et al., Early and selective impairments in axonal transport kinetics of synaptic cargoes induced by soluble amyloid β-protein oligomers, Traffic, 2012, vol. 13, no. 5, pp. 681–693.
Walsh, D.M., Klyubin, I., Fadeeva, J.V., et al., Naturally secreted oligomers of amyloid beta protein potently inhibit hippocampal long-term potentiation in vivo, Nature, 2002, vol. 416, no. 6880, pp. 535–539.
Walsh, D.M. and Selkoe, D.J., Aβ oligomers—a decade of discovery, J. Neurochem., 2007, no. 5, pp. 1172–1184.
Wang, Y., Kim, N.S., Li, X., et al., Calpain activation is not required for AIF translocation in parp-1-dependent cell death (parthanatos), J. Neurochem., 2009, vol. 110, no. 2, pp. 687–696.
Yu, S.W., Andrabi, S.A., Wang, H., et al., Apoptosis-inducing factor mediates poly(ADP-ribose) (PAR) polymer-induced cell death, Proc. Natl. Acad. Sci. USA, 2006, vol. 103, no. 48, pp. 18314–18319.
Yuan, J., Lipinski, M., and Degterev, A., Diversity in the mechanisms of neuronal cell death, Neuron, 2003, vol. 40, no. 2, pp. 401–413.
Zhang, X., Chen, J., Graham, S.H., et al., Intranuclear localization of apoptosis-inducing factor (AIF) and large scale DNA fragmentation after traumatic brain injury in rats and in neuronal cultures exposed to peroxynitrite, J. Neurochem., 2002, vol. 82, no. 1, pp. 181–191.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original Russian Text © V.V. Kolobov, T.V. Davydova, V.G. Fomina, 2014, published in Izvestiya Akademii Nauk, Seriya Biologicheskaya, 2014, No. 2, pp. 133–141.
Rights and permissions
About this article
Cite this article
Kolobov, V.V., Davydova, T.V. & Fomina, V.G. Protective action of glutamate antibodies on increased expression of genes of programmed death of rat brain cells induced by injection of a β-amyloid fragment (25–35). Biol Bull Russ Acad Sci 41, 118–125 (2014). https://doi.org/10.1134/S1062359014020034
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S1062359014020034