Abstract
Introduction: Favipiravir and Vitamin C (Vit C) were used together in the treatment of the COVID-19 pandemic. However, the effects of favipiravir on the periodontium are still unknown. Therefore, the aim of this study was to investigate the effects of Favipiravir and Vit C treatment on alveolar bone metabolism. Experimental: Fifty healthy adult male Sprague-Dawley rats (2–3 months old) were randomly divided into five equal groups (n = 10): Control, Favi 20, Favi 100, Favi 20+Vit C, Favi 100+Vit C. Favipiravir (20 mg/kg and 100 mg/kg, i.m.) and Vit C (150 mg/kg/day, oral) were administered to the rats for 14 days. Alveolar bone loss (ABL) and histopathological changes were examined using a light microscope. Immunohistochemistry was used to determine levels of receptor activator of nuclear factor kappa-B ligand (RANKL), caspase-3, bone morphogenic protein 2 (BMP-2) and alkaline phosphatase (ALP) in the bone tissues. Results: Favipiravir increased the levels of RANKL and caspase-3 expression but decreased BMP-2 and ALP levels in a dose-dependent manner. Favi 20+Vit C and Favi 100 +Vit C groups showed decreased RANKL and caspase-3 levels in addition to increased BMP-2 and ALP levels. Conclusion: Favipiravir can cause histopathological damage to the periodontium, but administration of favipiravir combined with Vit C can provide a protective effect against this damage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In December 2019, an epidemic started with symptoms like pneumonia in Wuhan, China, and, expanded to the world and was named coronavirus disease-19 (COVID-19) by the World Health Organization (WHO) [1, 2]. Favipiravir which is a broad-spectrum antiviral drug, is a pyrazine carboxamide derivative and is used for treatment of influenza in Japan [3]. Favipiravir is also used as a potential treatment agent for COVID-19 but clinical studies are still in progress [4]. Active favipiravir competes with purine nucleosides and interferes with viral replication by incorporation into virus RNA, thereby potentially inhibiting the RNA-dependent RNA polymerase (RdRp) of RNA viruses [4]. As a result of animal studies in which dose toxicity was investigated after oral administration of favipiravir, effects such as an increase in liver enzymes (aspartate aminotransferase—AST, alkaline phosphatase—ALP, alanine aminotransferase—ALT, total bilirubin), hepatocyte vacuolization and a decrease in red blood cell (RBC) production were observed [5]. It is also known that favipiravir is teratogenic; therefore, the administration of favipiravir should be avoided in pregnant women [6]. It was reported by clinical and laboratory studies that COVID-19 treatment with favipiravir had fewer adverse effects compared to other antiviral drugs [7].
Vitamin C (Vit C) is an essential antioxidant that participates in the improvement, maintenance, and function of various cell types in the body. Such pharmacological properties of Vit C as antiviral, anti-inflammatory, antioxidant, and immunomodulating effects have also been demonstrated [8]. A recent study demonstrated that intravenous administration of high dose of Vit C for COVID-19 management generates positive results without adverse effects [9]. Both favipiravir and Vit C are among the treatment options for COVID-19 and related studies have been carried out strenuously in many countries [10].
While increasing evidence indicates that there may be an association between COVID-19 infection and periodontitis, maintenance of periodontal health could become an essential factor in preventing its complications, but the effects of favipiravir on alveolar bone are not known. As a result, the purpose of this study was to examine the effects of favipiravir at various doses with or without Vit C supplementation on rat alveolar bone metabolism using such parameters as receptor activator of nuclear factor kappa-B ligand (RANKL), caspase-3, alkaline phosphatase (ALP), and bone morphogenic protein-2 (BMP-2).
Methods
Study design and ethics
The animal experiments were approved by the Animal Experimentation Ethics Committee in Pamukkale University (PAUHDEK-2021/23). The study was carried out following the Basic & Clinical Pharmacology & Toxicology policy for experimental and clinical studies [11]. Fifty healthy adult male Sprague-Dawley rats (2–3 months old) were kept in cages at 22 ± 1°C in 12-hour light/dark cycles. The rats received standard pellet-shaped rodent food and water ad libitum until euthanization. Animals were weighed weekly. Fifty rats were randomly distributed into 5 equal groups (n = 10):
1. Control group: 0.1 mL orally of saline and 0,1 ml intramuscularly (i.m.) of saline.
2. Favi 20 group: 0.1 mL orally of saline and 20mg/kg i.m. of Favipiravir
3. Favi 100 group: 0.1 mlL orally of saline and 100mg/kg i.m. of Favipiravir
4. Favi 20+Vit C group: 20 mg/kg i.m. of Favipiravir and orally 150 mg/kg of Vit C
5. Favi 100+Vit C group: 100 mg/kg i.m. of Favipiravir and orally 150 mg/kg of Vit C
Favipiravir (20 or 100 mg/kg; i.m., T705, Merck) and Vit C (150 mg/kg; L-Ascorbic acid, per os, Merck) were administered to rats for 14 days [12]. At the end of 14 days, all rats were euthanized under anesthesia (80–100 mg/kg of Ketamine; Alfamin, Alfasan IBV and 5–7 mg/kg Xylazine; Alfazin, Alfasan IBV) and samples were collected and stored in 10% formalin at room temperature until analysis.
Histopathological evaluation
Mandibula and maxilla samples were collected and fixed in 10% neutral-buffered formalin for microscopical evaluation. After 3-days of tissue fixation, the samples were decalcified in 0.1 M ethylenediaminetetraacetic acid solution (EDTA) for 2 weeks, and tissues were routinely processed by an automatic tissue processor (Leica ASP300S, Wetzlar, Germany). Then samples were embedded in paraffin and 5 μm serial sections were prepared by a rotary microtome (Leica RM 2155; Leica Microsystems, Wetzlar, Germany) and one serial section was stained with hematoxylin and eosin (HE). Four serial sections were prepared, and two levels of sections were taken from all rats for histopathological and immunohistochemical examinations.
The degree of the alveolar bone loss (ABL) was detected by measuring the distances between the alveolar bone crest (ABC) and cemento-enamel junction (CEJ) at six points in all molar teeth localized in both the maxilla and mandible. Lesioned areas were analyzed in each rat using a light microscope (Olympus CX41, Olympus Corporation, Tokyo, Japan).
Immunohistochemical analysis for RANKL, caspase-3, ALP, and BMP-2
Selected sections were stained to demonstrate the presence of ALP using Anti-ALP antibody (ab224335); BMP2—Anti-BMP2 antibody (ab14933); RANKL—Anti-RANKL antibody (ab216484) and Caspase-3—anti-caspase-3 antibody (ab4051) by the streptavidin-biotin peroxidase technique, according to the manufacturer’s instructions. All antibodies were purchased from Abcam, (Cambridge, UK) and used at a 1/100 dilution. An UltraVision Detection System Anti-Polyvalenti HRP kit (TP-060-HL) (Thermo Shandon Limited, Cheshire, UK) was used for staining with the secondary antibody, and 3,3´-diaminobenzidine was used as the chromogen. For negative controls, antibody dilution solutions were used instead of primary antibodies. The DAB staining step was completed by checking under a microscope to prevent background staining, and then washed twice. All tissue examinations were performed by a specialist pathologist who was blinded to the specimen treatments. All slides were analyzed for immunopositivity by semi-quantitative analysis. For this aim, samples were analyzed by assessing five different areas in each rat. Immunohistochemical staining was scored between 0–3. 0 = negative, 1 = low positive, 2 = positive, and 3 = high positive [13, 14]. The scores obtained were analyzed statistically and tabulated. An automated image analysis system (Olympus CX41, Olympus Corporation, Tokyo, Japan) was used to obtain computer-assisted histomorphometric measurements and immunohistochemical scoring to support the data after conventional microscopic examination. The Database Manual CellSens Life Science Imaging Software System (Olympus Corporation) was used for histomorphological and immunohistochemical analysis. IHC score analyses were performed using Image J 1.46r (National Institutes of Health, Bethesda MD).
IHC optical density scores were calculated using the following formula: IHC optical density score = (Percentage contribution of high positive × 4 + Percentage contribution of positive × 3 + percentage contribution of low positive × 2 + percentage contribution of negative × 4) / 100 [15].
Statistical analysis
Statistical analyses were performed using the SPSS 21.0 program. A one-way analysis of variance post hoc Tukey test was used to reveal significant differences between the groups for comparing the alveolar bone loss (ABL). The Kruskal–Wallis comparison test was used to determine differences between groups in the histopathological and immunohistochemical analyses and p < 0.05 was considered as the level of significance.
Results
Histopathological Findings
No rats were lost during the experimental procedure. Intact gingival epithelium and no alveolar bone loss were observed in the Control group. All other groups showed inflammatory reactions like redness and edema in the gingival tissues and also periodontal ligament, degradation of the alveolar process, and low to partial cement destruction (Fig. 1). ABL was observed in the Favi 100 group compared to the Control group (p > 0.05). The Favi 20, Favi 20+Vit C, and Favi 100+Vit C groups showed the signs of ABL compared to the Control group but the differences were not statistically significant (Fig. 2).
Immunohistochemical Findings
The results of the immunohistochemical examination of BMP-2, one of the precursor markers of bone formation, the Favi 20, and Favi 100 groups revealed decreased immunoreactivity compared to other groups (p < 0.05). The BMP-2 staining in the Vit C applied favipiravir groups approached the levels in the Control group (p > 0.05) (Fig. 3). According to IHC scores, all favipiravir-applied groups revealed decreased BMP-2 activity compared to The Control group (p < 0.05) (Table 1). When the ALP, another important bone formation marker, was examined, decreased immunoactivity was observed in all groups compared to the Control group. Administration of Vit C increased ALP immunoreactivity, with the increase being especially pronounced in the Favi 100+Vit C group (Fig. 4). ALP immunoreactivity was statistically decreased in the Favi 100 group compared to the Control group (Table 1). Caspase-3 plays an important role in the intrinsic and extrinsic pathways of programmed cell death. In this recent study, caspase-3 imunoreactivity was significantly increased in the Favi 20, Favi 100, and Favi 100+Vit C groups compared to the Control group (p < 0.05) whereas the Favi 20+Vit C group showed similar immunostaining (p > 0.05) (Fig. 3, Table 1).
Immunohistochemical examination revealed that both doses of favipiravir increased RANKL immunoreactivity compared to the Control group (p < 0.05) (Fig. 3, Table 1) in a dose-dependent manner. The Favi 100 group showed the highest RANKL levels among the groups. Vit C administration decreased RANKL immunoreactivity, increased by favipiravir, in the Favi 20+Vit C and Favi 100+Vit C groups. Although similar RANKL immunoreactivity wase observed in the alveolar bone border, the affected area was mainly in the periodontal ligament with RANKL -immunopositive cells being mainly localized in the periodontal ligament (Fig. 4). Most of the RANKL immunopositive cells were osteoclasts, osteoblasts, and fibroblasts.
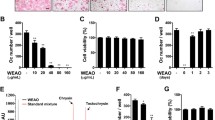
Graphic representation of the levels of immunoreactivity of proteins of interest in the analyzed groups. The data were presented by box and whisker plots, displaying the median, interquartile range, minimum, and maximum. ALP—* p < 0.05, Control vs Favi 20, Favi 100 and, Favi 20+Vit C. BMP-2—* p < 0.05, Control vs Favi 20; ** p < 0.05, Favi 20 vs Favi 20+Vit C and Favi 100+Vit C. Caspase-3—* p < 0.05 Control vs Favi 100 and Favi 100+Vit C; ** p < 0.05 Favi 20+Vit C vs Favi 100. RANKL—* p < 0.05 Control vs Favi 100.
Discussion
In the present study, the effects of favipiravir and favipiravir combined with Vit C, a treatment option for the current pandemic, on the periodontium were investigated in rats by histological and immunohistochemical methods. To the best of our knowledge, this is the first study evaluating the effects of favipiravir, an antiviral agent used in COVID-19 treatment, on the periodontium. Our results showed that high doses of favipiravir caused an increase in caspase-3 and RANKL levels and a reduction in ALP and BMP-2 levels. Administration of Vit C ameliorated favipiravir-induced apoptosis as measured by caspase-3 and RANKL in osteoblasts, with an increase in ALP and BMP-2 levels being observed.
Broad-spectrum antiviral agents are considered as the gold standard in the treatment of viral diseases [12]. Favipiravir, used for COVID-19 infection, is a new antiviral agent that prevents viral transcription and replication and acts as an inhibitor of RNA-dependent RNA polymerase [16]. It should be used in high doses for effective antiviral activity [17]. However, animal studies have shown that its repeated doses have adverse effects on hematopoietic cells, liver function parameters, and hepatocytes. In addition, dose-dependent increases in the serum of the uric acid levels have been detected asymptomatically in humans [18]. Although studies of the effects of antiretroviral treatments and their long-term tolerability continue, the impact of these drugs on bone metabolism has become an important issue. Antiretroviral drugs could affect bone cells directly and indirectly through the changes in the RANK/RANKL system, phosphate metabolism, mitochondrial function, and cytokine production [19]. RANKL released by periosteal cells, osteoblasts, and osteocytes, stimulates osteoclast formation and activity responsible for bone resorption and subsequent binding with RANK. Following the administration of antiretroviral therapy, T lymphocytes become active and trigger bone loss by enhancing the secretion of osteoclastogenic cytokines such as RANKL and TNF [20]. In rats treated with tenofovir, a nucleoside-based antiviral drug, an increase in RANKL-positive cell counts and a decrease in osteoprotegerin levels were detected. In that study, tenofovir was also shown to increase the number of osteoclasts in the bone, reduce bone volume and production, and inhibit bone formation by activating MAPK and NF-kB signaling pathways involved in triggering osteoclastic differentiation [21]. It has been determined that a long-term treatment regimen with lopinavir, also used for COVID-19 management, causes a reduction in bone mineral density [22]. In the current study, 20 mg/kg and 100 mg/kg of favipiravir for 14 days caused an increase in RANKL levels and induced ABL. A previous study reported that the 150 mg/kg Vit C reduces RANKL-induced osteoclastogenesis and associated ABL [23]. Vit C diminishes oxidative stress and inflammation via reduction of NF-κB production [23] and also decreases serum TNF-α and IL-1β levels [24]. Consistent with our study, it has been shown that in a high-cholesterol diet, Vit C reduced the formation of TRAP-positive osteoclasts, with decreased RANKL and NF-κB expression on the alveolar bone surface [25]. According to our results, Vit C could suppress local osteoclast differentiation formed by favipiravir by decreasing RANKL levels on the alveolar bone surface.
Favipiravir is intended as a drug for oral administration with the average doses in humans being reported as 1 600 mg twice a day (followed by 600 mg twice a day) for 10–14 days [26–28]. However, in animal studies, it is understood that the effective dose is much higher. The effectiveness of high doses may be due to the high favipiravir EC50 pharmacokinetics of the drug [18, 29]. In a clinical study evaluating the favipiravir usage in Ebola-infected patients, the dosages used in patients were 6000 mg on day 0, followed by 1200 mg BID for 9 days. The median trough concentrations of favipiravir in serum on days 2 and 4 were 46.1 and 25.9 µg/mL, respectively. In hamsters treated with a high dose (approximately 1400 µg/kg/day), the mean trough concentration is 29.9 µg/mL [30]. However, further studies are needed to determine the most effective and non-cytotoxic dose in terms of favipiravir plasma concentrations in patients infected with SARS-CoV-2. In a recent study, the effectiveness of favipiravir was researched with (18.75, 37.5, and 75 mg/day TID). The treatment of SARS-CoV-2 infected hamsters with different high doses of favipiravir resulted in reduced histopathological damages in the lungs dose-dependently, although some toxicity was noticed, especially with the dose of 75 mg/day TID [29]. The efficacy of administration of favipiravir intraperitoneally or orally twice daily (loading dose of 900 and 1200 mg/kg/day, respectively, followed by 600 and 1000 mg/kg/day) was evaluated in hamsters highly infected with the virus (2 × 106 TCID50). Regardless of the dose regimen, pulmonary histopathological disorders regressed and no toxicity was observed with favipiravir treatment [31].
Caspases belong to a proteolytic enzyme family, involved in inflammation and the apoptotic signaling pathway [32]. While caspase-3 has a stimulatory effect in the early phase of RANKL-induced osteoclast differentiation, activation of caspase-3 plays an inhibitory role at later stages of RANKL-induced osteoclast differentiation [33, 34]. Enhanced caspase-3 levels were detected after antiviral treatments and it was reported that this increase could be used to predict the effectiveness of antiviral therapy [33, 35]. In an in vitro study performed with favipiravir on human neuronal progenitor cells, human dermal fibroblasts, human lung adenocarcinoma cells, and Vero cells infected by Asian ZIKV, a significant increase was observed in Bcl-2 mRNA expression levels, while Bax mRNA expression levels were decreased [36]. In the above referenced study, favipiravir seems to have reduced apoptosis in virus-infected tissues. In our study, rats were not infected with SARS-CoV-2. Although this is seen as a limitation, it was done to fully observe the effects of favipiravir in the periodontium of healthy rats. According to our results, favipiravir provides an increase in caspase-3 immunoexpression in a dose-dependent manner. Vit C has been shown in numerous studies to inhibit oxidative stress and apoptosis [37, 38]. We have also found that caspase-3 levels were diminished in Vit C-treated rats. These data suggest that Vit C could attenuate the cellular toxicity developed by favipiravir and therefore may serve as a targeted intervention for apoptosis.
BMP-2, released from many cells such as osteoblasts and osteocytes, is an important growth factor involved in bone remodeling and hemostasis. It regulates osteoblast differentiation by triggering the release of transcription factors specific to osteoblasts [39]. On the other hand, ALP is an enzyme situated in osteoblasts and involved in mineralization of newly formed bone [40]. In an animal model, it was shown that tenofovir exposure results in a reduction of ALP levels [41]. Also, it has been reported that enhanced plasma ALP levels following tenofovir administration testify to the impairment of bone mineralization [42]. In our study we also observed a decrease in BMP-2 and ALP levels following favipiravir treatment. These results suggest that favipiravir deteriorates formation of new bones. Vit C plays a crucial role in determining the life cycle as well as proliferation of osteoblasts. Studies have shown that addition of Vit C to osteoblast-like cells encourages the initial deposition of the extracellular matrix of collagen [8]. Vit C exerts a favorable impact on trabecular bone formation by affecting bone matrix gene release in osteoblasts [8]. It has been reported that Vit C is an essential antioxidant for bone homeostasis by regulating osteoblastic and osteoclastic activity in osteoporosis models [43]. In addition, Vit C has been described to prevent the reduction in bone mineral volume in postmenopausal women [44]. There is a report that orally applied Vit C supplementation in rats inhibited the expression of osteoclastogenesis-related factors such as RANK, RANKL, as well as cathepsin K and induced BMP-2 gene release [45]. Several studies have shown that BMP-2 release is increased [46] and ALP-specific genes are induced in osteoblast-like cells treated with Vit C [47]. In the present study, Vit C administration suppressed the favipiravir-induced changes in expression in ALP and BMP-2 and prevented ABL in rat alveolar bones.
Conclusion
In conclusion, our findings showed that two doses of systemic favipiravir administration for 14 days in a rat model increase osteoblast apoptosis and RANKL induced osteoclastogenesis in a dose-dependent manner and decrease BMP-2 and ALP immunoreactivity. Concomitant use of Vit C with favipiravir reversed these adverse effects on alveolar bone metabolism. Further investigation of the mechanism of combined action of Favipiravir and Vit C on specific cytokines that accelerate alveolar bone resorption or formation will be of undeniable value.
Change history
29 June 2022
An Erratum to this paper has been published: https://doi.org/10.1134/S0022093022030280
References
WHO (2020) WHO Director-General’s Remarks at the Media Briefing on 2019-nCoV on 11 February 2020. https://www.who.int/dg/speeches/detail/who-director-general-s-remarks-at-the-media-briefing-on-2019-ncov-on-11-february-2020
Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, Zhao X, Huang B, Shi W, Lu R, Niu P, Zhan F, Ma X, Wang D, Xu W, Wu G, Gao GF, Tan W, China Novel Coronavirus I, Research T (2020) A Novel Coronavirus from Patients with Pneumonia in China, 2019. N Engl J Med 382 (8):727–733. https://doi.org/10.1056/NEJMoa2001017
Furuta Y, Komeno T, Nakamura T (2017) Favipiravir (T-705), a broad spectrum inhibitor of viral RNA polymerase. Proc Jpn Acad Ser B Phys Biol Sci 93 (7):449–463. https://doi.org/10.2183/pjab.93.027
Du YX, Chen XP (2020) Favipiravir: Pharmacokinetics and Concerns About Clinical Trials for 2019-nCoV Infection. Clin Pharmacol Ther 108 (2):242–247. https://doi.org/10.1002/cpt.1844
Ghasemnejad-Berenji M, Pashapour S (2021) Favipiravir and COVID-19: A Simplified Summary. Drug Res (Stuttg) 71 (3):166–170. https://doi.org/10.1055/a-1296-7935
Delang L, Abdelnabi R, Neyts J (2018) Favipiravir as a potential countermeasure against neglected and emerging RNA viruses. Antiviral Res 153:85–94. https://doi.org/10.1016/j.antiviral.2018.03.003
Cai Q, Yang M, Liu D, Chen J, Shu D, Xia J, Liao X, Gu Y, Cai Q, Yang Y, Shen C, Li X, Peng L, Huang D, Zhang J, Zhang S, Wang F, Liu J, Chen L, Chen S, Wang Z, Zhang Z, Cao R, Zhong W, Liu Y, Liu L (2020) Experimental Treatment with Favipiravir for COVID-19: An Open-Label Control Study. Engineering (Beijing) 6 (10):1192–1198. https://doi.org/10.1016/j.eng.2020.03.007
Aghajanian P, Hall S, Wongworawat MD, Mohan S (2015) The Roles and Mechanisms of Actions of Vitamin C in Bone: New Developments. J Bone Miner Res 30 (11):1945–1955. https://doi.org/10.1002/jbmr.2709
Abobaker A, Alzwi A, Alraied AHA (2020) Overview of the possible role of vitamin C in management of COVID-19. Pharmacol Rep 72 (6):1517–1528. https://doi.org/10.1007/s43440-020-00176-1
Wu R, Wang L, Kuo HD, Shannar A, Peter R, Chou PJ, Li S, Hudlikar R, Liu X, Liu Z, Poiani GJ, Amorosa L, Brunetti L, Kong AN (2020) An Update on Current Therapeutic Drugs Treating COVID-19. Curr Pharmacol Rep 6:1–15. https://doi.org/10.1007/s40495-020-00216-7
Tveden-Nyborg P, Bergmann TK, Jessen N, Simonsen U, Lykkesfeldt J (2021) BCPT policy for experimental and clinical studies. Basic Clin Pharmacol Toxicol 128 (1):4–8. https://doi.org/10.1111/bcpt.13492
Caroline AL, Powell DS, Bethel LM, Oury TD, Reed DS, Hartman AL (2014) Broad spectrum antiviral activity of favipiravir (T-705): protection from highly lethal inhalational Rift Valley Fever. PLoS Negl Trop Dis 8 (4):e2790. https://doi.org/10.1371/journal.pntd.0002790
Lektemur Alpan A, Kizildag A, Ozdede M, Karakan NC, Ozmen O (2020) The effects of taxifolin on alveolar bone in experimental periodontitis in rats. Arch Oral Biol 117:104823. https://doi.org/10.1016/j.archoralbio.2020.104823
Lektemur Alpan A, Calisir M, Kizildag A, Ozdede M, Ozmen O (2020) Effects of a Glycogen Synthase Kinase 3 Inhibitor Tideglusib on Bone Regeneration With Calvarial Defects. J Craniofac Surg 31 (5):1477–1482. https://doi.org/10.1097/SCS.0000000000006326
Seyed Jafari SM, Hunger RE (2017) IHC Optical Density Score: A New Practical Method for Quantitative Immunohistochemistry Image Analysis. Appl Immunohistochem Mol Morphol 25 (1):e12–e13. https://doi.org/10.1097/PAI.0000000000000370
Lagocka R, Dziedziejko V, Klos P, Pawlik A (2021) Favipiravir in Therapy of Viral Infections. J Clin Med 10 (2):273. https://doi.org/10.3390/jcm10020273
Hashemian SM, Farhadi T, Velayati AA (2020) A review on favipiravir: the properties, function, and usefulness to treat COVID-19. Expert Rev Anti Infect Ther 19(8):1–9. https://doi.org/10.1080/14787210.2021.1866545
Madelain V, Nguyen TH, Olivo A, de Lamballerie X, Guedj J, Taburet AM, Mentre F (2016) Ebola Virus Infection: Review of the Pharmacokinetic and Pharmacodynamic Properties of Drugs Considered for Testing in Human Efficacy Trials. Clin Pharmacokinet 55 (8):907–923. https://doi.org/10.1007/s40262-015-0364-1
Borderi M, Gibellini D, Vescini F, De Crignis E, Cimatti L, Biagetti C, Tampellini L, Re MC (2009) Metabolic bone disease in HIV infection. AIDS 23 (11):1297–1310. https://doi.org/10.1097/QAD.0b013e32832ce85a
Weitzmann MN, Ofotokun I (2016) Physiological and pathophysiological bone turnover—role of the immune system. Nat Rev Endocrinol 12 (9):518–532. https://doi.org/10.1038/nrendo.2016.91
Conesa-Buendia FM, Llamas-Granda P, Larranaga-Vera A, Wilder T, Largo R, Herrero-Beaumont G, Cronstein B, Mediero A (2019) Tenofovir Causes Bone Loss via Decreased Bone Formation and Increased Bone Resorption, Which Can Be Counteracted by Dipyridamole in Mice. J Bone Miner Res 34 (5):923–938. https://doi.org/10.1002/jbmr.3665
Brown TT, McComsey GA, King MS, Qaqish RB, Bernstein BM, da Silva BA (2009) Loss of bone mineral density after antiretroviral therapy initiation, independent of antiretroviral regimen. J Acquir Immune Defic Syndr 51 (5):554–561. https://doi.org/10.1097/QAI.0b013e3181adce44
Chen Y, Luo G, Yuan J, Wang Y, Yang X, Wang X, Li G, Liu Z, Zhong N (2014) Vitamin C mitigates oxidative stress and tumor necrosis factor-alpha in severe community-acquired pneumonia and LPS-induced macrophages. Mediators Inflamm 2014:426740. https://doi.org/10.1155/2014/426740
Erol N, Saglam L, Saglam YS, Erol HS, Altun S, Aktas MS, Halici MB (2019) The Protection Potential of Antioxidant Vitamins Against Acute Respiratory Distress Syndrome: a Rat Trial. Inflammation 42 (5):1585–1594. https://doi.org/10.1007/s10753-019-01020-2
Sanbe T, Tomofuji T, Ekuni D, Azuma T, Irie K, Tamaki N, Yamamoto T, Morita M (2009) Vitamin C intake inhibits serum lipid peroxidation and osteoclast differentiation on alveolar bone in rats fed on a high-cholesterol diet. Arch Oral Biol 54 (3):235–240. https://doi.org/10.1016/j.archoralbio.2008.11.001
Karatas EAL, Kilic PE, Dogru A, Ozaslan E (2021) Early onset favipiravir saves lives. Research Square. https://doi.org/10.21203/rs.3.rs-142868/v1 (Preprint).
Dabbous HM, Abd-Elsalam S, El-Sayed MH, Sherief AF, Ebeid FFS, El Ghafar MSA, Soliman S, Elbahnasawy M, Badawi R, Tageldin MA (2021) Efficacy of favipiravir in COVID-19 treatment: a multi-center randomized study. Arch Virol 166 (3):949–954. https://doi.org/10.1007/s00705-021-04956-9.
Tam DNT QT, Luu NM, Turnage M, Tran L, Tawfik GM, Minh LHN, Huy NT, Iiyama T, Kita K, Hirayama K (2021) Favipiravir and its potentials in COVID-19 pandemic: An update. Asian Pacific Journal of Tropical Medicine 14 (10):433–439. https://doi.org/10.4103/1995-7645.329005
Driouich JS, Cochin M, Lingas G, Moureau G, Touret F, Petit PR, Piorkowski G, Barthelemy K, Laprie C, Coutard B, Guedj J, de Lamballerie X, Solas C, Nougairede A (2021) Favipiravir antiviral efficacy against SARS-CoV-2 in a hamster model. Nat Commun 12 (1):1735. https://doi.org/10.1038/s41467-021-21992-w
Sissoko D, Laouenan C, Folkesson E, M’Lebing AB, Beavogui AH, Baize S, Camara AM, Maes P, Shepherd S, Danel C, Carazo S, Conde MN, Gala JL, Colin G, Savini H, Bore JA, Le Marcis F, Koundouno FR, Petitjean F, Lamah MC, Diederich S, Tounkara A, Poelart G, Berbain E, Dindart JM, Duraffour S, Lefevre A, Leno T, Peyrouset O, Irenge L, Bangoura N, Palich R, Hinzmann J, Kraus A, Barry TS, Berette S, Bongono A, Camara MS, Chanfreau Munoz V, Doumbouya L, Souley H, Kighoma PM, Koundouno FR, Rene L, Loua CM, Massala V, Moumouni K, Provost C, Samake N, Sekou C, Soumah A, Arnould I, Komano MS, Gustin L, Berutto C, Camara D, Camara FS, Colpaert J, Delamou L, Jansson L, Kourouma E, Loua M, Malme K, Manfrin E, Maomou A, Milinouno A, Ombelet S, Sidiboun AY, Verreckt I, Yombouno P, Bocquin A, Carbonnelle C, Carmoi T, Frange P, Mely S, Nguyen VK, Pannetier D, Taburet AM, Treluyer JM, Kolie J, Moh R, Gonzalez MC, Kuisma E, Liedigk B, Ngabo D, Rudolf M, Thom R, Kerber R, Gabriel M, Di Caro A, Wolfel R, Badir J, Bentahir M, Deccache Y, Dumont C, Durant JF, El Bakkouri K, Gasasira Uwamahoro M, Smits B, Toufik N, Van Cauwenberghe S, Ezzedine K, D’Ortenzio E, Pizarro L, Etienne A, Guedj J, Fizet A, Barte de Sainte Fare E, Murgue B, Tran-Minh T, Rapp C, Piguet P, Poncin M, Draguez B, Allaford Duverger T, Barbe S, Baret G, Defourny I, Carroll M, Raoul H, Augier A, Eholie SP, Yazdanpanah Y, Levy-Marchal C, Antierrens A, Van Herp M, Gunther S, de Lamballerie X, Keita S, Mentre F, Anglaret X, Malvy D, Group JS (2016) Experimental Treatment with Favipiravir for Ebola Virus Disease (the JIKI Trial): A Historically Controlled, Single-Arm Proof-of-Concept Trial in Guinea. PLoS Med 13 (3):e1001967. https://doi.org/10.1371/journal.pmed.1001967
Kaptein SJF, Jacobs S, Langendries L, Seldeslachts L, Ter Horst S, Liesenborghs L, Hens B, Vergote V, Heylen E, Barthelemy K, Maas E, De Keyzer C, Bervoets L, Rymenants J, Van Buyten T, Zhang X, Abdelnabi R, Pang J, Williams R, Thibaut HJ, Dallmeier K, Boudewijns R, Wouters J, Augustijns P, Verougstraete N, Cawthorne C, Breuer J, Solas C, Weynand B, Annaert P, Spriet I, Vande Velde G, Neyts J, Rocha-Pereira J, Delang L (2020) Favipiravir at high doses has potent antiviral activity in SARS-CoV-2-infected hamsters, whereas hydroxychloroquine lacks activity. Proc Natl Acad Sci U S A 117 (43):26955–26965. https://doi.org/10.1073/pnas.2014441117
Shalini S, Dorstyn L, Dawar S, Kumar S (2015) Old, new and emerging functions of caspases. Cell Death Differ 22 (4):526–539. https://doi.org/10.1038/cdd.2014.216
Szymczyk KH, Freeman TA, Adams CS, Srinivas V, Steinbeck MJ (2006) Active caspase-3 is required for osteoclast differentiation. J Cell Physiol 209 (3):836–844. https://doi.org/10.1002/jcp.20770
Katao Y, Shishido M, Inami K, Matsumoto N, Sawai H (2014) An inhibitory role for caspase-3 at the late stage of RANKL-induced osteoclast differentiation in RAW264 cells and mouse bone marrow macrophages. Cell Biol Int 38 (6):723–728. https://doi.org/10.1002/cbin.10263
Shaimerdenova M, Karapina O, Mektepbayeva D, Alibek K, Akilbekova D (2017) The effects of antiviral treatment on breast cancer cell line. Infect Agent Cancer 12:18. https://doi.org/10.1186/s13027-017-0128-7
Kim JA, Seong RK, Kumar M, Shin OS (2018) Favipiravir and Ribavirin Inhibit Replication of Asian and African Strains of Zika Virus in Different Cell Models. Viruses 10 (2):72. https://doi.org/10.3390/v10020072
Guaiquil VH, Vera JC, Golde DW (2001) Mechanism of vitamin C inhibition of cell death induced by oxidative stress in glutathione-depleted HL-60 cells. J Biol Chem 276 (44):40955–40961. https://doi.org/10.1074/jbc.M106878200
Hanada Y, Iomori A, Ishii R, Gohda E, Tai A (2014) Protection of free radical-induced cytotoxicity by 2-O-alpha-D-glucopyranosyl-L-ascorbic acid in human dermal fibroblasts. Biosci Biotechnol Biochem 78 (2):301–306. https://doi.org/10.1080/09168451.2014.882756
Halloran D, Durbano HW, Nohe A (2020) Bone Morphogenetic Protein-2 in Development and Bone Homeostasis. J Dev Biol 8 (3):19. https://doi.org/10.3390/jdb8030019
Kim SH, Shin KH, Moon SH, Jang J, Kim HS, Suh JS, Yang WI (2017) Reassessment of alkaline phosphatase as serum tumor marker with high specificity in osteosarcoma. Cancer Med 6 (6):1311–1322. https://doi.org/10.1002/cam4.1022
Carnovali M, Banfi G, Mora S, Mariotti M (2016) Tenofovir and bone: age-dependent effects in a zebrafish animal model. Antivir Ther 21 (7):587–594. https://doi.org/10.3851/IMP3048
Kim-Chang JJ, Wilson L, Chan C, Fischer B, Venturi G, Goodenow MM, Aldrovandi G, Weber TJ, Sleasman JW, Adolescent Medicine Trials Network for HIVAI (2019) Tenofovir Has Minimal Effect on Biomarkers of Bone Health in Youth with HIV Receiving Initial Antiretroviral Therapy. AIDS Res Hum Retroviruses 35 (8):746–754. https://doi.org/10.1089/AID.2018.0270
Malmir H, Shab-Bidar S, Djafarian K (2018) Vitamin C intake in relation to bone mineral density and risk of hip fracture and osteoporosis: a systematic review and meta-analysis of observational studies. Br J Nutr 119 (8):847–858. https://doi.org/10.1017/S0007114518000430
Morton DJ, Barrett-Connor EL, Schneider DL (2001) Vitamin C supplement use and bone mineral density in postmenopausal women. J Bone Miner Res 16 (1):135–140. https://doi.org/10.1359/jbmr.2001.16.1.135
Choi HK, Kim GJ, Yoo HS, Song DH, Chung KH, Lee KJ, Koo YT, An JH (2019) Vitamin C Activates Osteoblastogenesis and Inhibits Osteoclastogenesis via Wnt/beta-Catenin/ATF4 Signaling Pathways. Nutrients 11 (3):506. https://doi.org/10.3390/nu11030506
Valenti MT, Zanatta M, Donatelli L, Viviano G, Cavallini C, Scupoli MT, Dalle Carbonare L (2014) Ascorbic acid induces either differentiation or apoptosis in MG-63 osteosarcoma lineage. Anticancer Res 34 (4):1617–1627.
Franceschi RT, Young J (1990) Regulation of alkaline phosphatase by 1,25-dihydroxyvitamin D3 and ascorbic acid in bone-derived cells. J Bone Miner Res 5 (11):1157–1167. https://doi.org/10.1002/jbmr.5650051111
Author information
Authors and Affiliations
Contributions
Conceptualization, ALA and GTC; methodology, ALA, GTC, ÖÖ, MFD, and YŞ; formal analysis, ALA; investigation, ALA, GTC, MFD and YŞ; resources, ÖÖ; writing—original draft, ALA, and ÖÖ; writing—review & editing, ALA, ÖÖ, YŞ and GTC.
Corresponding author
Ethics declarations
Declaration of Conflicting Interests
The authors declare that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Lektemur Alpan, A., Torumtay Cin, G., Özmen, Ö. et al. Evaluation of the Effects of Favipiravir Combined with Vitamin C on Alveolar Bone in Rats. J Evol Biochem Phys 58, 430–440 (2022). https://doi.org/10.1134/S0022093022020119
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0022093022020119