Abstract
Immune privileges of cancer stem cells is a well-known and widely studied problem, as presence of such cells in tumors is associated with refractoriness, recurrence, and metastasis. Accumulating evidence also suggests presence of immune privileges in non-pathological stem cells in addition to their other defense mechanisms against damaging factors. This similarity between pathological and normal stem cells raises the question of why stem cells have such a potentially dangerous property. Regulation of vital processes of autoimmunity control and regeneration realized through interactions between immune cells, stem cells, and their microenvironment are reviewed in this work as causes of formation of the stem cell immune privilege. Deep mutual integration between regulations of stem and immune cells is noted. Considering diversity and complexity of mutual regulation of stem cells, their microenvironment, and immune system, I suggest the term “stem system”.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Advances in surgical techniques and, in particular, transplantation techniques have led to the need of animal models for taining purposes. This led, naturally, to detection of rejection reactions of allogeneic grafts and discovery of immune privileges. For example, the first references on immune privileges date back to the late 19th century [1, 2], when an ophthalmologist observed that the mouse skin graft planted in the anterior chamber of a dog’s eye showed longer survival. In his work, Shirai showed engraftment of cancer cells planted from a third-party donor into brain as opposed to rejection when planted in other tissues [3]. Another work [4] showed that transplantation of a fragment of autologous spleen into brain together with tumour cells leads to the death of the latter. It was also shown that prior immunisation of recipient leads to rejection of skin graft in the mouse brain [5]. Transplantations are still providing an important link allowing in vivo study of details of immune privileges during interaction of complex systems of the organism, complementing the methods of modern molecular biology and bioinformatics.
Initially, the main hypothesis explaining formation of immune privileges in organs was assumption of existence of a region isolated from immune cells. However, the demonstrated migration of peripheral immune cells across the intact blood-brain barrier and active regulation of macrophages and lymphocytes by neurons and glia [6] have forced researchers to reconsider the view of immunoprivilege as a property of the organ area isolated from immune system. Moreover, the brain territory can be distinguished as a special immune territory [7]. It is also widely known that disruption of the integrity of one eye can trigger an immune response and attack in the contralateral eye [8]. In addition to barrier mechanisms, special attention is paid to microenvironment inside the eye, as well as to participation of immune cells and, in particular, regulatory T-lymphocytes (T-regs) as key factors in formation of the immunoprivileged territory of the eye [9, 10]. Current evidence suggests that CD8 and CD4 T-reg subpopulations both in the anterior chamber of the eye itself and in the spleen are involved in the formation of immune privilege in the eye [10]. For placenta and fetus, one theory of their immunoprivilege is also associated with the layer of T-regs expressing factors HO-1, LIF, TGF-β, and IL-10 [11]. Immunogenicity of the autologous semen shown in pig [12] also implies that testes are immunoprivileged. The mechanisms of immune privileges in testes include both cellular barriers built by Sertoli cells [13] and cytokine regulatory mechanisms that suppress immune response [14, 15]. Melanocytes are able to migrate into hair follicles, where they are not subjects to destruction by the immune system in the heterotypic transplantation [16]. This allows hair follicles to be classified as immunoprivileged regions of the body [16, 17]. Mechanisms of immune privileges are also found in articular cartilage [18-20].
The use of immune privilege mechanisms by tumors is of particular interest [21-24]. Immunosuppressive tumor microenvironment can vary considerably, exploiting a broad spectrum of regulation involving expression of signalling cytokines, metabolic alteration of microenvironment, immune checkpoints on cancer cells, and involvement of immune cells polarised as anti-inflammatory [23, 25-28]. While the mechanisms studied and the amount of literature data on them vary widely, a complete review of the mechanisms for which involvement in the formation of immune privileges in cancer has been demonstrated requires separate consideration.
The accumulated experimental data allow to identify a wide range of both mechanisms of immune privileges and areas of the organism with immune privileges that are not limited to barrier organs. The strength of immune privileges is not an absolute concept and can vary greatly depending on many factors [29, 30]. Depending on the strength of immune privileges, intermediate terms can be distinguished. For example, immune evasion reflects the ability to temporarily avoid immune response, which is manifested in a relatively longer survival of allogeneic grafts, but inability to avoid immune response completely [31].
IMMUNE PRIVILEGES OF STEM CELLS
Earlier studies demonstrate evasion of stem cells from the cytotoxic action of immune cells for the hematopoietic stem cells [32], embryonic stem cells [33], and further for the mesenchymal [34] and neural stem cells [35]. It was shown in the studies that the decreased expression of major histocompatibility complex (MHC) molecules removes surveillance from the cytotoxic CD8+ lymphocytes, and that natural killer (NK) cells do not attack stem cells regardless of MHC expression.
Recent work [36] demonstrates immune privileges as an intrinsic property of the stem cells considered in this work. The work used transgenic mice expressing green fluorescent protein (GFP) in the LGR5+ stem cells and CD8+ cytotoxic T lymphocytes with the T-cell receptor affinity to GFP peptides in the composition of the MHC I complex, which destroy the GFP-producing cells in vivo. The authors did a thorough work and showed that it is possible to isolate subpopulations of stem cells that are not subject to immune surveillance in the hair follicles and muscle, but not in the gut, ovaries, or breast. The quiescent state has been highlighted as a defining property of the stem cell subpopulations that escape immune surveillance. Expression of the major histocompatibility complex class I (MHC I) and β2-microglobulin (B2m) is reduced in the resting stem cells. They also showed a significant decrease in the expression of receptors and transcription factors Irf3, Irf5, Stat1, and Stat3 that respond to inflammation. The authors showed that this stem cell subpopulation does not activate effector T cells and is not affected by the immune system, but that these properties are lost when the stimuli activate proliferation of the resting stem cell. Absence or significant reduction of MHC I on the cell surface should lead to NKs activation and destruction of such cells, which was not observed in the described work. This implies existence of other mechanisms protecting resting stem cells from immunity.
Based on the results presented above [36], of particular interest are the long-repopulating hematopoietic stem cells (HSCs), which rarely divide and mainly remain in a quiescent state [37]. Immunogenicity of the total mass of allogeneic bone marrow cells is not in doubt [31, 38], but this does not exclude the possibility of the presence of minor cell populations that are immunoprivileged. Thus, in the work on mice it was shown that the niche CD150high T-regs are involved in formation of immune privileges of the allogeneic HSCs [39]. At the same time, the authors show participation of the niche T-regs in protecting HSCs from oxidative stress and keeping them in a resting state by means of adenosine generated by the CD39 receptors on the T-reg surface. However, the authors do not consider the stem cell dormancy and immune privilege as the cause and effect.
Subpopulation of mesenchymal stem cells (MSCs), which serve as a source of stroma both in the bone marrow and in organs and tissues throughout the body, is also of considerable interest due to their immunosuppressive activity and their tendency to be dormant in vivo [40, 41]. Opinions of the reaserchers on the immune privileges of mesenchymal cells (MCs) differ significantly. Despite the background and demonstration of the significant immunomodulatory potential [34], MCs and MSCs have been classified as cells lacking immune privileges [31, 42-45]. However, works demonstrating immune privileges of the resting stem cells [36, 39], including cancer cells [46, 47], lead to the opposite conclusion accepting association of the mesenchymal cell phenotype with immune privileges [48]. In our recent work, we have shown the immune privileges of MSCs [49]. We used a model of ectopic hematopoiesis taking the transgenic Nestin-GFP mice expressing GFP in stem cells under control of the nestin promoter as a bone marrow donor, and placing the graft under the kidney capsule of isogenic wild-type mice with a complete uncompromised immune system. Immune privileges have also been reported for the multilineage differentiating stress-enduring (MUSEs), identified as an SSEA-3+ subpopulation of MCs [50]. Allogeneic and xenogeneic MUSEs injected intravenously into rabbits without immune suppression have been shown to survive for several weeks [51]. Despite the differences in approaches to phenotyping subpopulations, similarities in the functional characteristics of SSEA-3+ MUSEs and NES-GFP+ MSCs [40, 49, 50] suggest that they represent one common subpopulation. According to the literature, MUSEs express nestin [52]. Previously, based on our results and the literature data, we pointed out the relationship between the nestin expression and population of the immunoprivileged cells [49]. Such nestin-expressing stem cells are found in various parts of the adult organism and organs of various embryonic origins: both exemplified by the immunoprivileged cells we have studied, in particular MSCs, and other immunoprivileged stem cells such as the muscle stem cells and hair follicle stem cells [49], as well as stem cells from other immunoprivileged territories: testis [53], cartilage [54], brain [55], and retina [56]. The question of nestin involvement in the mechanisms of immune privileges was not directly addressed in our work, as well as the question of immune privilege mechanisms in general [49].
Nestin is a type VI intermediate filament [57], which is known as a stem cell marker [57]. Along with other intermediate filaments, nestin participates in a number of key signalling pathways for both normal and cancer stem cells [58]. Increased nestin expression has been identified as a negative prognostic factor for a number of cancers of epithelial, mesenchymal, and neural origin: colorectal cancer, hepatocellular carcinoma, various cancers of the central nervous system, non-small cell lung cancer, breast cancer, melanoma, and multiple myeloma [59]. Moreover, nestin is associated with the immature tumour phenotype and cancer stem cells (CSCs) [60]. Nestin overexpression is associated with a more aggressive course and metastasis of the tumours and their refractoriness to therapy [61]. The question whether nestin is a direct regulator in the processes of immune privilege formation or is only a passive marker associated with stemness regulation remains open.
Additional arguments about the commonality of stem cells of different tissues come from the works devoted to adult pluripotent stem cells [62-65]. Such pluripotent cells have an eventful history of their study using different protocols and are referred to in the literature under different names MAPC/spore-like cell/STAP/MUSE/VSEL [62]. VSELs are very small embryo-like stem cells and are positioned as precursors of tissue-specific stem cells. Such cells have been shown to participate in the reparative processes: their number and release into peripheral blood increase under the action of tissue damage factors. MUSEs demonstrate the ability to cross-differentiate between the directions of germinal sheets [52, 66]. Thus, for the small subpopulation of MCs, which can be found in connective tissues of almost all organs, the authors demonstrated the ability of the cells to differentiate in all three directions of germ layers, their self-maintenance, and their migration to the areas of damage [52]. It has been shown that such stem cells migrate into tissues during embryogenesis, do not directly participate in the tissue formation, and remain quiescent in the adult organism [64, 67-70]. At the same time, such stem cells are resistant to radiation and chemotherapeutic effects [71-73]. In the experiments on allogeneic and xenogeneic transplantations of MUSEs, it has been shown that they have immune privileges [50, 51]. Thus, we can generalise that subpopulations of the stem cells of different organs and tissues of the adult organism have many common functions and characteristics. It is unlikely that many different and independent mechanisms have evolutionarily emerged for the same functions, but a rigorous test of this hypothesis is necessary.
The resting state of stem cells is identified as a key characteristic, regulation of which is performed by multiple mechanisms and is associated with the functions of self-maintenance, differentiation, and activation in response to damage [65, 74-79]. Disruption of regulation of the stem cells resting state is often accompanied by their depletion and is associated with the degenerative pathologies and aging [80-83]. Thus, association of the stem cell dormancy with immune privileges [36] and, moreover, participation of T-regs in the maintenance of dormancy [39] indicate deep integration of immune privilege mechanisms into stem cell regulation.
STEM SYSTEM
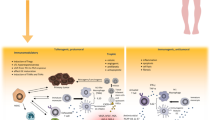
The functions and characteristics of stem cells described above are largely determined endogenously by epigenetic marks, metabolic products, internal signalling cascades, RNA interference and other cellular mechanisms [58, 84-86]. At the same time, stem cell and its environment constitute a complex system of their mutual regulation [87, 88]. From the practical point of view, separation of stem cells from their niche is problematic due to disruption of cellular regulation [36, 63, 89-92]. Culturing of the isolated stem cell subpopulation requires special solutions [93]. For example, culturing techniques aimed at keeping muscle stem cells quiescent have been demonstrated to be effective in increasing subsequent therapeutic effects in mice [94]. These methods involve local regulation of stem cells through a niche that includes a matrix and a special growth medium. Metabolic products contribute significantly to the regulation of stem cells and their environment [39, 95]. Ligand–receptor intercellular contacts and nanotubes, which provide direct exchange of cytoplasmic contents, also play an important role in the regulation of stem cells and their environment [96-99]. In addition to stem cell progeny, immune and other stem cell niche cells play an important role in stem cell maintenance [39, 100, 101]. Microvesicles secreted by MSCs, which contain both a membrane repertoire of receptors and ligands capable of interacting at the cell surface and an internal content with its intracellular diversity of signalling molecules, are capable of interacting with targets elsewhere in the body [102-104]. The example of muscle stem cells demonstrates their transition to the state of readiness to respond to damage in another part of the body, and for VSELs their exit into the peripheral blood [69, 105]. The above examples mention only a small part of the studied mechanisms, while demonstrating existence of a complex network of regulation related to stem cell functions (Fig. 1). Terminologically, it is appropriate to speak about the existence of a stem system responsible for regulation of its cellular and other components. This system fulfils the function of supporting cellular composition of organs of an adult organism, reacts with reparative response in a case of damage, and co-regulates with immune system (Fig. 1). The term “stem system” will allow a more accurate reflection of the structure of the object of study, which should have a favourable effect on the overall preception. At the same time, separation of the concepts of stem cell and stem cell niche is of fundamental importance in understanding their functioning. Schemes of experiments capable of distinguishing contribution of the individual cells or their subpopulations can offer a fundamentally new perspective on the object of study [49, 65, 88]. So, for example, MC abbreviation provides better distinction from MSC abbreviation. We identified such distinction as the key point that allowed us to show immune privileges of the mesenchymal stem cells among the general population of mesenchymal cells lacking immune privileges [49].
Schematic representation of the idea of generalising stem cells, their microenvironment, and their regulatory mechanisms into a stem system. The dotted lines separate the areas of interactions, marked in the right part. The centre captions indicate the main elements involved in the interactions, including both cells and various non-cellular components. The arrows in the left part indicate the processes occurring between the highlighted regions of interaction.
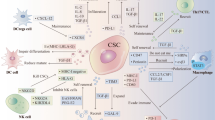
Generalisation of stem cell features in an organism and recognition of immune privileges as the base property of stem cell subpopulations gives a new perspective on the processes of oncogenesis. CSCs are known to be associated with refractoriness to therapy, metastasis, and recurrence [106, 107]. The literature demonstrates systemic similarities between the CSCs and normal stem cells, manifested as deep quiescent state, ability to migrate and differentiate, hypoxia resistance, self-maintenance, and nestin expression [49, 57, 58, 60, 64, 66, 106]. Immune system is able to exert suppressive effects on cancer cells and inhibit cancer development [108, 109]. Presence of immune privileges in CSCs as stem cells confers meaningful advantages to pathological cells, as demonstrated in experiments [46, 110]. As shown in our work with non-pathological stem cells [49], long-term survival of the cancer stem cells and preservation of their functions to give metastasis when the immune system is suppressed has been demonstrated [46]. As for non-pathological stem cells, studies have highlighted the role of T-regs and the resting state of CSCs in formation of the CSC immune privileges [46, 47, 110, 111]. Thus, cancer cells may gain a range of stem cell-specific advantages, including immune privileges, through a shift to the stem state rather than independent sequential accumulation (Fig. 2).
A separate risk factor associated with immune privileges is the possibility of sheltering infectious pathogens from the action of the immune system [112]. Infection of stem cells and their niches leads to disruption of stem system functions manifested as clinical pathologies in the form of fibroses, impaired hematopoiesis, bone and cartilage disorders, and damage to barrier functions in brain vessels [112].
Existence of such potentially dangerous mechanism as stem cell immune privileges must be evolutionarily balanced by the equally significant reasons in order not to be rejected in the evolutionary process. Control of autoimmunity is a suitable significant reason. In addition to the central control mechanisms of autoimmunity, peripheral control mechanisms exist in the body [113, 114]. The main peripheral control executors are considered to be T-reg, but involvement of other immune control mechanisms has also been noted. Immune privileges of stem cells may be part of such mechanisms [29] (Fig. 3). This assumption is supported by the fact that during the inflammatory process, MSCs do not simply evade the action of immune cells, but become activated by secreting chemokines that attract immune cells [115, 116]. Involvement of stem cells in the process of peripheral control of immunity may be due to the high value of such cells and the need to protect them. Also, peripheral control may be necessary in addition to the central control, especially for the complex, long-lived organisms that could accumulate mutational differences in the genome of peripheral tissues and in the central immune system during life time [117].
In addition to autoimmune control, interaction between the stem system and the immune system is essential at the site of injury [118]. Properly orchestrated activation of repair and inflammatory programmes is an important biological regulation [102, 119, 120]. Interplay between these functions seems even more compelling for the evolutionary equilibrium, and it may utilise the same mechanisms as the control of autoimmunity (Fig. 4).
Participation of immune system in regulation of stem system has been noted not only in active pathological processes, but also in the norm with participation of T-regs and macrophages. Existence of the tissue T-regs with expression profile and transcriptome similar to that of stem cells has been demonstrated [120]. T-regs has been shown to be involved in the tissue repair, maintenance of stem cell resting state, and differentiation [39, 121, 122]. For the T-regs resident in hair follicle stem cell niches, JAG1 signal expression has been shown, demonstrating involvement of the Notch signal transduction in both immune and stem cell regulation [123-126]. For macrophages, their role in the repair processes of various tissues has been shown, and their dysfunction leads to dysregulation of stem cell differentiation and fibrosis [119, 127, 128]. Macrophages also support MSCs by reducing oxidative stress through recycling of depolarised mitochondria [101]. Involvement of immune cells in stem cell maintenance in normal cells demonstrates the depth of mutual integration between the stem and immune systems.
In turn, stem cells, along with immunosuppressive effects, are able to stimulate the inflammatory response. In particular, the MSCs activated by inflammatory signals release chemokines that attract immune cells to the area of damage, where stem cells could modulate their further activity [115, 116]. The hormone procalcitonin produced by MSCs is one of the best and earliest markers of various groups of infectious diseases [112, 129]. Procalcitonin levels are significantly elevated well before the C-reactive protein levels rise, which is utilised in intensive care units. MSCs also express functional Toll-like receptors (TLRs) that activate migration, differentiation, cytokine and chemokine secretion in response to the pathogen-associated ligands [130]. It has been shown that such MSCs, depending on environmental signals, can lose their ability to inhibit T lymphocytes by disrupting the Notch signalling pathway through activation of TLR3 and TLR4 [131]. Moreover, a set of genes specifically activated in the stem cells confer intrinsic protection against viral infections [86]. Thus, MSCs have a complex pattern of behaviour and can both block immune response and actively participate in it.
The presented examples of mutual regulation of the stem and immune systems are not exhaustive. For example, the effect of hypoxia, which often follows injury, has been noted to both suppress immunity and maintain stem cells [95, 111, 132]. Also, adenosine plays an important role in the regulation of both systems [133]. Moreover, various cells, including stem cell progeny or dendritic cells, are involved in the regulatory mechanisms [88, 134]. As can be seen from the literature review, stem cell immune privileges are due to recruitment of T lymphocytes from circulating blood, their reprogramming, resting state, and other mechanisms that simultaneously regulate both immune response and stem cell maintenance. Thus, the immune privileges of stem cells are deeply integrated into regulation of stem system, which, as already noted, is regulated by a variety of mechanisms acting both by intercellular contact and through systemic and local mechanisms involving immune and other cells as intermediates, forming the complex system discussed in the review (Fig. 1). Detailed consideration of the mechanisms deserves a separate analysis, and the most studied mechanisms may be the subject of separate reviews.
An important conclusion is that there is a close and complex relationship between the stem and the immune systems. Understanding the mechanisms of this relationship would allow application of complex approaches in the translational medicine and in the already existing therapies. The use of mesenchymal cells and their products to suppress autoimmune pathologies could be such example [50, 103, 135]. In transplantology, mesenchymal cells and their non-cellular products can be used for prevention and treatment of the graft-versus-host reactions [115, 136]. Another example is the stimulation of stem niches and their mechanisms of peripheral defence against autoimmunity instead of general immunosuppression, which could be accompanied by complications of the infection [137]. Experiments in mice with T-regs carrying an artificial chimeric antigenic receptor against a given MHC I show potential in combating graft rejection [138]. Inflammatory processes play a key role in triggering regeneration, but their exsessive activity slows down regeneration [133]. Understanding the mechanisms of immune regulation of regeneration processes may offer tools for therapeutic control over the immune system and new solutions for regenerative medicine [133, 139, 140]. Considering that the presence of immune privileges in the norm is the result of a complex coregulation of different mechanisms, in the case of cancer it may be necessary to inhibit different signalling pathways on a patient-specific basis to achieve greater efficacy of personalised therapy [27, 141, 142].
Integration of a new mechanism into the system creates a potential breakdown point. For each mechanism, there are reasons fot its existence that outweigh the risks associated with it, otherwise it would be rejected by natural selection. Such deep integration of the stem system and the immune system means there is evolutionary necessity and complex fine-tuned regulation. As can be seen from the review, fundamental importance of the immune privileges of non-pathological stem cells and especially of MSCs cannot be overemphasized. Indeed, MSCs are distributed throughout the body and show a strong contribution to immune regulation [67, 102, 103, 115, 116]. Interaction between the stem and the immune systems plays an important role in various aspects of damage regeneration and control of autoimmunity [17, 39, 66, 101, 103, 119, 122]. The immunoregulatory properties of MSCs have been utilised in the supportive transplantation therapy, and regenerative potential of MSCs has been used in the regenerative medicine [66, 102, 104, 115, 136]. Also, immune privileges may be involved in the development of cancer and infectious diseases [46, 47, 110, 112]. Thus, the issue considered in this review addresses a wide range of medical problems including those not discussed in this review.
CONCLUSIONS
Association of immune privileges with the basic property of resting stem cells offers a perspective on regulation of autoimmunity, infectious diseases, regenerative medicine, transplantation, and oncology. Thus, in a number of cases, stemness of cancer cells could provide a range of benefits, including protection from immunity. This insight may prove important for treatment of cancer cases complicated by the presence of CSCs. Studies of the stem cell-immune cell interactions suggest existence of a complex network of mutual regulation, disruption of which could lead to cancer, autoimmune pathologies, organ tissue dysfunction, and accelerated aging. Based on the presence of a complex network of stem cell regulation, I propose to use the term “stem system”, which includes both regulation of stem cells themselves and their microenvironment, and mechanisms of their interaction with the immune system. The term “stem system” provides more accurate description of the structure of the object of study, which will have a favourable effect on the overall perception. The study of the mechanisms of regulation of the stem and the immune systems opens wide opportunities for research, the results of which would provide better understanding of their biological nature and application of the findings in medicine.
Abbreviations
- CSCs:
-
cancer stem cells
- GFP:
-
green fluorescent protein
- HSCs:
-
hematopoietic stem cells
- MCs:
-
mesenchymal cells
- MHC:
-
major histocompatibility complex
- MSCs:
-
mesenchymal stem cells
- MUSEs:
-
multilineage differentiating stress-enduring cells
- T-regs:
-
regulatory T lymphocytes
References
Van Dooremaal, J. C. (1873) The development of living tissue transplanted to foreign soil [in German], Arch. Ophthalmol., 19, 358-373.
Niederkorn, J. Y. (2006) See no evil, hear no evil, do no evil: the lessons of immune privilege, Nat. Immunol., 7, 354-359, https://doi.org/10.1038/NI1328.
Shirai, Y. (1921) On the transplantation of the rat sarcoma in adult heterogeneous animals, Japan Med. World, 1, 14-15.
Murphy, J. B., and Sturm, E. (1923) Conditions determining the transplantability of tissues in the brain, J. Exp. Med., 38, 183-197, https://doi.org/10.1084/jem.38.2.183.
Medawar, P. B. (1948) Immunity to homologous grafted skin; the fate of skin homografts, Br. J. Exp. Pathol., 29, 58-69.
Carson, M. J., Doose, J. M., Melchior, B., Schmid, C. D., and Ploix, C. C. (2006) CNS immune privilege: hiding in plain sight, Immunol. Rev., 213, 48-65, https://doi.org/10.1111/j.1600-065X.2006.00441.x.
Negi, N., and Das, B. K. (2018) CNS: not an immunoprivilaged site anymore but a virtual secondary lymphoid organ, Int. Rev. Immunol., 37, 57-68, https://doi.org/10.1080/08830185.2017.1357719.
Chang, G. C., and Young, L. H. (2011) Sympathetic ophthalmia, Semin. Ophthalmol., 26, 316-320, https://doi.org/10.3109/08820538.2011.588658.
Hori, J., Yamaguchi, T., Keino, H., Hamrah, P., and Maruyama, K. (2019) Immune privilege in corneal transplantation, Prog. Retin. Eye Res., 72, 100758, https://doi.org/10.1016/j.preteyeres.2019.04.002.
Keino, H., Horie, S., and Sugita, S. (2018) Immune privilege and eye-derived T-regulatory cells, J. Immunol. Res., 2018, 1679197, https://doi.org/10.1155/2018/1679197.
Zenclussen, A. C., Schumacher, A., Zenclussen, M. L., Wafula, P., and Volk, H. D. (2007) Immunology of pregnancy: cellular mechanisms allowing fetal survival within the maternal uterus, Expert Rev. Mol. Med., 9, 1-14, https://doi.org/10.1017/S1462399407000294.
Katsh, S. (1957) In vitro demonstration of uterine anaphylaxis in guinea pigs sensitized with homologous testis or sperm, Nature, 180, 1047-1048, https://doi.org/10.1038/1801047a0.
Kaur, G., Thompson, L. A., and Dufour, J. M. (2014) Sertoli cells – immunological sentinels of spermatogenesis, Semin. Cell Dev. Biol., 30, 36-44, https://doi.org/10.1016/j.semcdb.2014.02.011.
Kern, S., Robertson, S. A., Mau, V. J., and Maddocks, S. (1995) Cytokine Secretion by macrophages in the rat testis, Biol. Reprod., 53, 1407-1416, https://doi.org/10.1095/biolreprod53.6.1407.
O’Bryan, M. K., Gerdprasert, O., Nikolic-Paterson, D. J., Meinhardt, A., Muir, J. A., Foulds, L. M., Phillips, D. J., De Kretser, D. M., and Hedger, M. P. (2005) Cytokine profiles in the testes of rats treated with lipopolysaccharide reveal localized suppression of inflammatory responses, Am. J. Physiol. Regul. Integr. Comp. Physiol., 288, 1744-1755, https://doi.org/10.1152/ajpregu.00651.2004.
Billingham, R. E., and Silvers, W. K. (1971) A biologist’s reflections on dermatology, J. Invest. Dermatol., 57, 227-240, https://doi.org/10.1111/1523-1747.ep12261543.
Paus, R., Bulfone-Paus, S., and Bertolini, M. (2018) Hair follicle immune privilege revisited: the key to alopecia areata management, J. Invest. Dermatol. Symp. Proc., 19, 12-17, https://doi.org/10.1016/j.jisp.2017.10.014.
Sun, Z., Zhang, M., Zhao, X. H., Liu, Z. H., Gao, Y., Samartzis, D., Wang, H. Q., and Luo, Z. J. (2013) Immune cascades in human intervertebral disc: the pros and cons, Int. J. Clin. Exp. Pathol., 6, 1009-1014.
Fujihara, Y., Takato, T., and Hoshi, K. (2014) Macrophage-inducing FasL on chondrocytes forms immune privilege in cartilage tissue engineering, enhancing in vivo regeneration, Stem Cells, 32, 1208-1219, https://doi.org/10.1002/stem.1636.
Sun, Z., Liu, B., and Luo, Z. J. (2020) The immune privilege of the intervertebral disc: implications for intervertebral disc degeneration treatment, Int. J. Med. Sci., 17, 685-692, https://doi.org/10.7150/ijms.42238.
Joyce, J. A., and Fearon, D. T. (2015) T cell exclusion, immune privilege, and the tumor microenvironment, Science, 348, 74-80, https://doi.org/10.1126/science.aaa6204.
Chen, D. S., and Mellman, I. (2013) Oncology meets immunology: the cancer-immunity cycle, Immunity, 39, 1-10, https://doi.org/10.1016/j.immuni.2013.07.012.
Kalavska, K., Kucerova, L., Schmidtova, S., Chovanec, M., and Mego, M. (2020) Cancer stem cell niche and immune-active tumor microenvironment in testicular germ cell tumors, Adv. Exp. Med. Biol., 1226, 111-121, https://doi.org/10.1007/978-3-030-36214-0_9.
Nguyen, P. H. D., Wasser, M., Tan, C. T., Lim, C. J., Lai, H. L. H., Seow, J. J. W., DasGupta, R., Phua, C. Z. J., Ma, S., Yang, J., Suthen, S. D., Tam, W. L., Lim, T. K. H., Yeong, J., Leow, W. Q., Pang, Y. H., Soon, G., Loh, T. J., Wan, W. K., Chan, C. Y., Cheow, P. C., Toh, H. C., Kow, A., Dan, Y. Y., Kam, J. H., Iyer, S., Madhavan, K., Chung, A., Bonney, G. K., Goh, B. K. P., Fu, N., Yu, V. C., Zhai, W., Albani, S., Chow, P. K. H., and Chew, V. (2022) Trajectory of immune evasion and cancer progression in hepatocellular carcinoma, Nat. Commun., 13, 1441, https://doi.org/10.1038/S41467-022-29122-W.
Duan, Q., Zhang, H., Zheng, J., and Zhang, L. (2020) Turning cold into hot: firing up the tumor microenvironment, Trends Cancer, 6, 605-618, https://doi.org/10.1016/J.TRECAN.2020.02.022.
Lim, A. R., Rathmell, W. K., and Rathmell, J. C. (2020) The tumor microenvironment as a metabolic barrier to effector T cells and immunotherapy, eLife, 9, 1-13, https://doi.org/10.7554/ELIFE.55185.
Li, B., Chan, H. L., and Chen, P. (2019) Immune checkpoint inhibitors: basics and challenges, Curr. Med. Chem., 26, 3009-3025, https://doi.org/10.2174/0929867324666170804143706.
Xia, L., Oyang, L., Lin, J., Tan, S., Han, Y., Wu, N., Yi, P., Tang, L., Pan, Q., Rao, S., Liang, J., Tang, Y., Su, M., Luo, X., Yang, Y., Shi, Y., Wang, H., Zhou, Y., and Liao, Q. (2021) The cancer metabolic reprogramming and immune response, Mol. Cancer, 20, 28, https://doi.org/10.1186/S12943-021-01316-8.
Ichiryu, N., and Fairchild, P. J. (2013) Immune privilege of stem cells, Methods Mol. Biol., 1029, 1-16, https://doi.org/10.1007/978-1-62703-478-4_1.
Agudo, J. (2021) Immune privilege of skin stem cells: what do we know and what can we learn? Exp. Dermatol., 30, 522-528, https://doi.org/10.1111/EXD.14221.
Ankrum, J. A., Ong, J. F., and Karp, J. M. (2014) Mesenchymal stem cells: immune evasive, not immune privileged, Nat. Biotechnol., 32, 252-260, https://doi.org/10.1038/nbt.2816.
Aguila, H. L., and Weissman, I. L. (1996) Hematopoietic stem cells are not direct cytotoxic targets of natural killer cells, Blood, 87, 1225-1231, https://doi.org/10.1182/BLOOD.V87.4.1225.BLOODJOURNAL8741225.
Drukker, M., Katz, G., Urbach, A., Schuldiner, M., Markel, G., Itskovitz-Eldor, J., Reubinoff, B., Mandelboim, O., and Benvenisty, N. (2002) Characterization of the expression of MHC proteins in human embryonic stem cells, Proc. Natl. Acad. Sci. USA, 99, 9864-9869, https://doi.org/10.1073/PNAS.142298299.
Rasmusson, I., Ringdén, O., Sundberg, B., and Le Blanc, K. (2003) Mesenchymal stem cells inhibit the formation of cytotoxic T lymphocytes, but not activated cytotoxic T lymphocytes or natural killer cells, Transplantation, 76, 1208-1213, https://doi.org/10.1097/01.TP.0000082540.43730.80.
Mammolenti, M., Gajavelli, S., Tsoulfas, P., and Levy, R. (2004) Absence of major histocompatibility complex class I on neural stem cells does not permit natural killer cell killing and prevents recognition by alloreactive cytotoxic T lymphocytes in vitro, Stem Cells, 22, 1101-1110, https://doi.org/10.1634/STEMCELLS.22-6-1101.
Agudo, J., Park, E. S., Rose, S. A., Alibo, E., Sweeney, R., Dhainaut, M., Kobayashi, K. S., Sachidanandam, R., Baccarini, A., Merad, M., and Brown, B. D. (2018) Quiescent tissue stem cells evade immune surveillance, Immunity, 48, 271-285, https://doi.org/10.1016/j.immuni.2018.02.001.
Bernitz, J. M., Kim, H. S., MacArthur, B., Sieburg, H., and Moore, K. (2016) Hematopoietic stem cells count and remember self-renewal divisions, Cell, 167, 1296-1309, https://doi.org/10.1016/j.cell.2016.10.022.
Fürst, D., Neuchel, C., Tsamadou, C., Schrezenmeier, H., and Mytilineos, J. (2019) HLA matching in unrelated stem cell transplantation up to date, Transfus. Med. Hemother., 46, 326-336, https://doi.org/10.1159/000502263.
Hirata, Y., Furuhashi, K., Ishii, H., Li, H. W., Pinho, S., Ding, L., Robson, S. C., Frenette, P. S., and Fujisaki, J. (2018) CD150 high bone marrow Tregs maintain hematopoietic stem cell quiescence and immune privilege via adenosine, Cell Stem Cell, 22, 445-453, https://doi.org/10.1016/j.stem.2018.01.017.
Méndez-Ferrer, S., Michurina, T. V., Ferraro, F., Mazloom, A. R., Macarthur, B. D., Lira, S. A., Scadden, D. T., Ma’ayan, A., Enikolopov, G. N., and Frenette, P. S. (2010) Mesenchymal and haematopoietic stem cells form a unique bone marrow niche, Nature, 466, 829-834, https://doi.org/10.1038/nature09262.
Naji, A., Eitoku, M., Favier, B., Deschaseaux, F., Rouas-Freiss, N., and Suganuma, N. (2019) Biological functions of mesenchymal stem cells and clinical implications, Cell. Mol. Life Sci., 76, 3323-3348, https://doi.org/10.1007/S00018-019-03125-1.
Zangi, L., Margalit, R., Reich-Zeliger, S., Bachar-Lustig, E., Beilhack, A., Negrin, R., and Reisner, Y. (2009) Direct imaging of immune rejection and memory induction by allogeneic mesenchymal stromal cells, Stem Cells, 27, 2865-2874, https://doi.org/10.1002/stem.217.
Miura, Y., Yoshioka, S., Yao, H., Takaori-Kondo, A., Maekawa, T., and Ichinohe, T. (2013) Chimerism of bone marrow mesenchymal stem/stromal cells in allogeneic hematopoietic cell transplantation: is it clinically relevant? Chimerism, 4, 78-83, https://doi.org/10.4161/chim.25609.
Badillo, A. T., Beggs, K. J., Javazon, E. H., Tebbets, J. C., and Flake, A. W. (2007) Murine bone marrow stromal progenitor cells elicit an in vivo cellular and humoral alloimmune response, Biol. Blood Marrow Transplant., 13, 412-422, https://doi.org/10.1016/j.bbmt.2006.12.447.
Berglund, A. K., Fortier, L. A., Antczak, D. F., and Schnabel, L. V. (2017) Immunoprivileged no more: measuring the immunogenicity of allogeneic adult mesenchymal stem cells, Stem Cell Res. Ther., 8, 288, https://doi.org/10.1186/s13287-017-0742-8.
Malladi, S., MacAlinao, D. G., Jin, X., He, L., Basnet, H., Zou, Y., De Stanchina, E., and Massagué, J. (2016) Metastatic latency and immune evasion through autocrine inhibition of WNT, Cell, 165, 45, https://doi.org/10.1016/J.CELL.2016.02.025.
Galassi, C., Musella, M., Manduca, N., Maccafeo, E., and Sistigu, A. (2021) The immune privilege of cancer stem cells: a key to understanding tumor immune escape and therapy failure, Cells, 10, 2361, https://doi.org/10.3390/CELLS10092361.
Babaei, G., Aziz, S. G. G., and Jaghi, N. Z. Z. (2021) EMT, cancer stem cells and autophagy; the three main axes of metastasis, Biomed. Pharmacother., 133, 110909, https://doi.org/10.1016/J.BIOPHA.2020.110909.
Karpenko, D., Kapranov, N., and Bigildeev, A. (2022) Nestin-GFP transgene labels immunoprivileged bone marrow mesenchymal stem cells in the model of ectopic foci formation, Front. Cell Dev. Biol., 10, 993056, https://doi.org/10.3389/FCELL.2022.993056.
Kuroda, Y., Oguma, Y., Hall, K., and Dezawa, M. (2022) Endogenous reparative pluripotent muse cells with a unique immune privilege system: hint at a new strategy for controlling acute and chronic inflammation, Front. Pharmacol., 13, 1027961, https://doi.org/10.3389/FPHAR.2022.1027961.
Yamada, Y., Wakao, S., Kushida, Y., Minatoguchi, S., Mikami, A., Higashi, K., Baba, S., Shigemoto, T., Kuroda, Y., Kanamori, H., Amin, M., Kawasaki, M., Nishigaki, K., Taoka, M., Isobe, T., Muramatsu, C., Dezawa, M., and Minatoguchi, S. (2018) S1P-S1PR2 axis mediates homing of muse cells into damaged heart for long-lasting tissue repair and functional recovery after acute myocardial infarction, Circ. Res., 122, 1069-1083, https://doi.org/10.1161/CIRCRESAHA.117.311648.
Li, H., Wei, J., Liu, X., Zhang, P., and Lin, J. (2022) Muse Cells: ushering in a new era of stem cell-based therapy for stroke, Stem Cell Res. Ther., 13, 421, https://doi.org/10.1186/S13287-022-03126-1.
Jiang, M. H., Cai, B., Tuo, Y., Wang, J., Zang, Z. J., Tu, X., Gao, Y., Su, Z., Li, W., Li, G., Zhang, M., Jiao, J., Wan, Z., Deng, C., Lahn, B. T., and Xiang, A. P. (2014) Characterization of nestin-positive stem leydig cells as a potential source for the treatment of testicular leydig cell dysfunction, Cell Res., 24, 1466-1485, https://doi.org/10.1038/CR.2014.149.
Jaramillo-Rangel, G., Chávez-Briones, M. D. L., Ancer-Arellano, A., and Ortega-Martínez, M. (2021) Nestin-expressing cells in the lung: the bad and the good parts, Cells, 10, 3413, https://doi.org/10.3390/CELLS10123413.
Li, L., Mignone, J., Yang, M., Matic, M., Penman, S., Enikolopov, G., and Hoffman, R. M. (2003) Nestin expression in hair follicle sheath progenitor cells, Proc. Natl. Acad. Sci. USA, 100, 9958-9961, https://doi.org/10.1073/PNAS.1733025100.
Bhatia, B., Singhal, S., Lawrence, J. M., Khaw, P. T., and Limb, G. A. (2009) Distribution of Müller stem cells within the neural retina: evidence for the existence of a ciliary margin-like zone in the adult human eye, Exp. Eye Res., 89, 373-382, https://doi.org/10.1016/J.EXER.2009.04.005.
Bernal, A., and Arranz, L. (2018) Nestin-expressing progenitor cells: function, identity and therapeutic implications, Cell. Mol. Life Sci., 75, 2177-2195, https://doi.org/10.1007/S00018-018-2794-Z.
Sharma, P., Alsharif, S., Fallatah, A., and Chung, B. M. (2019) Intermediate filaments as effectors of cancer development and metastasis: a focus on keratins, vimentin, and nestin, Cells, 8, 497, https://doi.org/10.3390/CELLS8050497.
Szymańska-Chabowska, A., Świątkowski, F., Jankowska-Polańska, B., Mazur, G., and Chabowski, M. (2021) Nestin expression as a diagnostic and prognostic marker in colorectal cancer and other tumors, Clin. Med. Insights Oncol., 15, https://doi.org/10.1177/11795549211038256.
Neradil, J., and Veselska, R. (2015) Nestin as a marker of cancer stem cells, Cancer Sci., 106, 803-811, https://doi.org/10.1111/CAS.12691.
Ishiwata, T., Matsuda, Y., and Naito, Z. (2011) Nestin in gastrointestinal and other cancers: effects on cells and tumor angiogenesis, World J. Gastroenterol., 17, 409-418, https://doi.org/10.3748/WJG.V17.I4.409.
Bhartiya, D. (2017) Pluripotent stem cells in adult tissues: struggling to be acknowledged over two decades, Stem Cell. Rev. Rep., 13, 713-724, https://doi.org/10.1007/S12015-017-9756-Y.
Ratajczak, M. Z., Ratajczak, J., and Kucia, M. (2019) Very small embryonic-like stem cells (VSELs), Circ. Res., 124, 208-210, https://doi.org/10.1161/CIRCRESAHA.118.314287.
Ratajczak, M. Z., Ratajczak, J., Suszynska, M., Miller, D. M., Kucia, M., and Shin, D. M. (2017) A novel view of the adult stem cell compartment from the perspective of a quiescent population of very small embryonic-like stem cells, Circ. Res., 120, 166-178, https://doi.org/10.1161/CIRCRESAHA.116.309362.
Bhartiya, D., Jha, N., Tripathi, A., and Tripathi, A. (2023) Very small embryonic-like stem cells have the potential to win the three-front war on tissue damage, cancer, and aging, Front. Cell. Dev. Biol., 10, 1061022, https://doi.org/10.3389/FCELL.2022.1061022.
Dezawa, M. (2016) Muse cells provide the pluripotency of mesenchymal stem cells: direct contribution of muse cells to tissue regeneration, Cell Transplant., 25, 849-861, https://doi.org/10.3727/096368916X690881.
Isern, J., García-García, A., Martín, A. M., Arranz, L., Martín-Pérez, D., Torroja, C., Sánchez-Cabo, F., and Méndez-Ferrer, S. (2014) The neural crest is a source of mesenchymal stem cells with specialized hematopoietic stem cell niche function, eLife, 3, 03696, https://doi.org/10.7554/ELIFE.03696.
Gleiberman, A. S., Michurina, T., Encinas, J. M., Roig, J. L., Krasnov, P., Balordi, F., Fishell, G., Rosenfeld, M. G., and Enikolopov, G. (2008) Genetic approaches identify adult pituitary stem cells, Proc. Natl. Acad. Sci. USA, 105, 6332, https://doi.org/10.1073/PNAS.0801644105.
Dumont, N. A., Wang, Y. X., and Rudnicki, M. A. (2015) Intrinsic and extrinsic mechanisms regulating satellite cell function, Development, 142, 1572-1581, https://doi.org/10.1242/DEV.114223.
Neo, W. H., Lie-A-Ling, M., Fadlullah, M. Z. H., and Lacaud, G. (2021) Contributions of embryonic HSC-independent hematopoiesis to organogenesis and the adult hematopoietic system, Front. Cell Dev. Biol., 9, 631699, https://doi.org/10.3389/FCELL.2021.631699.
Shaikh, A., Bhartiya, D., Kapoor, S., and Nimkar, H. (2016) Delineating the effects of 5-fluorouracil and follicle-stimulating hormone on mouse bone marrow stem/progenitor cells, Stem Cell Res. Ther., 7, 59, https://doi.org/10.1186/S13287-016-0311-6.
Anand, S., Bhartiya, D., Sriraman, K., and Mallick, A. (2016) Underlying mechanisms that restore spermatogenesis on transplanting healthy niche cells in busulphan treated mouse testis, Stem Cell Rev. Rep., 12, 682-697, https://doi.org/10.1007/S12015-016-9685-1.
Ratajczak, J., Wysoczynski, M., Zuba-Surma, E., Wan, W., Kucia, M., Yoder, M. C., and Ratajczak, M. Z. (2011) Adult murine bone marrow-derived very small embryonic-like stem cells differentiate into the hematopoietic lineage after coculture over OP9 stromal cells, Exp. Hematol., 39, 225-237, https://doi.org/10.1016/J.EXPHEM.2010.10.007.
Sousa-Victor, P., García-Prat, L., and Muñoz-Cánoves, P. (2021) Control of satellite cell function in muscle regeneration and its disruption in ageing, Nat. Rev. Mol. Cell Biol., 23, 204-226, https://doi.org/10.1038/s41580-021-00421-2.
Chen, Z., Guo, Q., Song, G., and Hou, Y. (2022) Molecular regulation of hematopoietic stem cell quiescence, Cell. Mol. Life Sci., 79, 218, https://doi.org/10.1007/S00018-022-04200-W.
Cavallucci, V., Fidaleo, M., and Pani, G. (2016) Neural stem cells and nutrients: poised between quiescence and exhaustion, Trends Endocrinol. Metab., 27, 756-769, https://doi.org/10.1016/J.TEM.2016.06.007.
Ancel, S., Stuelsatz, P., and Feige, J. N. (2021) Muscle stem cell quiescence: controlling stemness by staying asleep, Trends Cell Biol., 31, 556-568, https://doi.org/10.1016/J.TCB.2021.02.006.
Ayyaz, A., Kumar, S., Sangiorgi, B., Ghoshal, B., Gosio, J., Ouladan, S., Fink, M., Barutcu, S., Trcka, D., Shen, J., Chan, K., Wrana, J. L., and Gregorieff, A. (2019) Single-cell transcriptomes of the regenerating intestine reveal a revival stem cell, Nature, 569, 121-125, https://doi.org/10.1038/S41586-019-1154-Y.
Dias, I. B., Bouma, H. R., and Henning, R. H. (2021) Unraveling the big sleep: molecular aspects of stem cell dormancy and hibernation, Front. Physiol., 12, 624950, https://doi.org/10.3389/FPHYS.2021.624950.
Ibrayeva, A., Bay, M., Pu, E., Jörg, D. J., Peng, L., Jun, H., Zhang, N., Aaron, D., Lin, C., Resler, G., Hidalgo, A., Jang, M. H., Simons, B. D., and Bonaguidi, M. A. (2021) Early stem cell aging in the mature brain, Cell Stem Cell, 28, 955-966, https://doi.org/10.1016/J.STEM.2021.03.018.
Choi, K., Park, S. H., Park, S. Y., and Yoon, S. K. (2022) The stem cell quiescence and niche signaling is disturbed in the hair follicle of the hairpoor mouse, an MUHH model mouse, Stem Cell Res. Ther., 13, 211, https://doi.org/10.1186/S13287-022-02898-W.
Chakkalakal, J. V., Jones, K. M., Basson, M. A., and Brack, A. S. (2012) The aged niche disrupts muscle stem cell quiescence, Nature, 490, 355-360, https://doi.org/10.1038/NATURE11438.
Singh, S., Jakubison, B., and Keller, J. R. (2020) Protection of hematopoietic stem cells from stress-induced exhaustion and aging, Curr. Opin. Hematol., 27, 225-231, https://doi.org/10.1097/MOH.0000000000000586.
Zhang, Z., Zhuang, L., and Lin, C. P. (2019) Roles of microRNAs in establishing and modulating stem cell potential, Int. J. Mol. Sci., 20, 3643, https://doi.org/10.3390/IJMS20153643.
Ren, R., Ocampo, A., Liu, G. H., and Izpisua Belmonte, J. C. (2017) Regulation of stem cell aging by metabolism and epigenetics, Cell Metab., 26, 460-474, https://doi.org/10.1016/J.CMET.2017.07.019.
Wu, X., Dao Thi, V. L., Huang, Y., Billerbeck, E., Saha, D., Hoffmann, H. H., Wang, Y., Silva, L. A. V., Sarbanes, S., Sun, T., Andrus, L., Yu, Y., Quirk, C., Li, M., MacDonald, M. R., Schneider, W. M., An, X., Rosenberg, B. R., and Rice, C. M. (2018) Intrinsic immunity shapes viral resistance of stem cells, Cell, 172, 423-438, https://doi.org/10.1016/J.CELL.2017.11.018.
Fuchs, E., and Blau, H. M. (2020) Tissue stem cells: architects of their niches, Cell Stem Cell, 27, 532-556, https://doi.org/10.1016/J.STEM.2020.09.011.
Cancedda, R., and Mastrogiacomo, M. (2023) Transit Amplifying Cells (TACs): a still not fully understood cell population, Front. Bioeng. Biotechnol., 11, 1189225, https://doi.org/10.3389/FBIOE.2023.1189225.
Chertkov, J. L., Drize, N. J., and Gurevitch, O. A. (1983) Hemopoietic stromal precursors in long-term culture of bone marrow: II. Significance of initial packing for creating a hemopoietic microenvironment and maintaining stromal precursors in the culture, Exp. Hematol., 11, 243-248.
Nie, Y., Han, Y.-C., and Zou, Y.-R. (2008) CXCR4 is required for the quiescence of primitive hematopoietic cells, J. Exp. Med., 205, 777-783, https://doi.org/10.1084/jem.20072513.
Greenbaum, A., Hsu, Y. M. S., Day, R. B., Schuettpelz, L. G., Christopher, M. J., Borgerding, J. N., Nagasawa, T., and Link, D. C. (2013) CXCL12 in early mesenchymal progenitors is required for haematopoietic stem-cell maintenance, Nature, 495, 227-230, https://doi.org/10.1038/nature11926.
Boyd, A. L., Campbell, C. J. V., Hopkins, C. I., Fiebig-Comyn, A., Russell, J., Ulemek, J., Foley, R., Leber, B., Xenocostas, A., Collins, T. J., and Bhatia, M. (2014) Niche displacement of human leukemic stem cells uniquely allows their competitive replacement with healthy HSPCs, J. Exp. Med., 211, 1925-1935, https://doi.org/10.1084/jem.20140131.
Lahlil, R., Scrofani, M., Barbet, R., Tancredi, C., Aries, A., and Hénon, P. (2018) VSELs maintain their pluripotency and competence to differentiate after enhanced ex vivo expansion, Stem Cell Rev. Rep., 14, 510-524, https://doi.org/10.1007/S12015-018-9821-1.
Quarta, M., Brett, J. O., DiMarco, R., De Morree, A., Boutet, S. C., Chacon, R., Gibbons, M. C., Garcia, V. A., Su, J., Shrager, J. B., Heilshorn, S., and Rando, T. A. (2016) An artificial niche preserves the quiescence of muscle stem cells and enhances their therapeutic efficacy, Nat. Biotechnol., 34, 752-759, https://doi.org/10.1038/nbt.3576.
Elashry, M. I., Kinde, M., Klymiuk, M. C., Eldaey, A., Wenisch, S., and Arnhold, S. (2022) The effect of hypoxia on myogenic differentiation and multipotency of the skeletal muscle-derived stem cells in mice, Stem Cell Res. Ther., 13, 56, https://doi.org/10.1186/S13287-022-02730-5.
Kann, A. P., Hung, M., and Krauss, R. S. (2021) Cell-cell contact and signaling in the muscle stem cell niche, Curr. Opin. Cell. Biol., 73, 78-83, https://doi.org/10.1016/J.CEB.2021.06.003.
Zamfirescu, A. M., Yatsenko, A. S., and Shcherbata, H. R. (2022) Notch signaling sculpts the stem cell niche, Front. Cell. Dev. Biol., 10, 1027222, https://doi.org/10.3389/FCELL.2022.1027222.
Whitehead, J., Zhang, J., Harvestine, J. N., Kothambawala, A., Liu, G. Yu, and Leach, J. K. (2020) Tunneling nanotubes mediate the expression of senescence markers in mesenchymal stem/stromal cell spheroids, Stem Cells, 38, 80-89, https://doi.org/10.1002/STEM.3056.
Jackson, M. V., Morrison, T. J., Doherty, D. F., McAuley, D. F., Matthay, M. A., Kissenpfennig, A., O’Kane, C. M., and Krasnodembskaya, A. D. (2016) Mitochondrial transfer via tunneling nanotubes is an important mechanism by which mesenchymal stem cells enhance macrophage phagocytosis in the in vitro and in vivo models of ARDS, Stem Cells, 34, 2210-2223, https://doi.org/10.1002/STEM.2372.
Yamazaki, S., Ema, H., Karlsson, G., Yamaguchi, T., Miyoshi, H., Shioda, S., Taketo, M. M., Karlsson, S., Iwama, A., and Nakauchi, H. (2011) Nonmyelinating schwann cells maintain hematopoietic stem cell hibernation in the bone marrow niche, Cell, 147, 1146-1158, https://doi.org/10.1016/J.CELL.2011.09.053.
Phinney, D. G., Di Giuseppe, M., Njah, J., Sala, E., Shiva, S., St Croix, C. M., Stolz, D. B., Watkins, S. C., Di, Y. P., Leikauf, G. D., Kolls, J., Riches, D. W. H., Deiuliis, G., Kaminski, N., Boregowda, S. V., McKenna, D. H., and Ortiz, L. A. (2015) Mesenchymal stem cells use extracellular vesicles to outsource mitophagy and shuttle microRNAs, Nat. Commun., 6, 8472, https://doi.org/10.1038/NCOMMS9472.
Toh, W. S., Zhang, B. I. N., Lai, R. C., and Lim, S. K. (2018) Immune regulatory targets of mesenchymal stromal cell exosomes/small extracellular vesicles in tissue regeneration, Cytotherapy, 20, 1419-1426, https://doi.org/10.1016/J.JCYT.2018.09.008.
Kahmini, F. R., and Shahgaldi, S. (2021) Therapeutic potential of mesenchymal stem cell-derived extracellular vesicles as novel cell-free therapy for treatment of autoimmune disorders, Exp. Mol. Pathol., 118, 104566, https://doi.org/10.1016/J.YEXMP.2020.104566.
Nakazaki, M., Lankford, K. L., Yamamoto, H., Mae, Y., and Kocsis, J. D. (2023) Human mesenchymal stem-derived extracellular vesicles improve body growth and motor function following severe spinal cord injury in rat, Clin. Transl. Med., 13, 1284, https://doi.org/10.1002/CTM2.1284.
Ratajczak, M. Z., Liu, R., Marlicz, W., Blogowski, W., Starzynska, T., Wojakowski, W., and Zuba-Surma, E. (2011) Identification of very small embryonic/epiblast-like stem cells (VSELS) circulating in peripheral blood during organ/tissue injuries, Methods Cell Biol., 103, 31-54, https://doi.org/10.1016/B978-0-12-385493-3.00003-6.
Barbato, L., Bocchetti, M., Di Biase, A., and Regad, T. (2019) Cancer stem cells and targeting strategies, Cells, 8, 926, https://doi.org/10.3390/CELLS8080926.
Mantovani, A., Marchesi, F., Malesci, A., Laghi, L., and Allavena, P. (2017) Tumour-associated macrophages as treatment targets in oncology, Nat. Rev. Clin. Oncol., 14, 399-416, https://doi.org/10.1038/NRCLINONC.2016.217.
Rollan, M. P., Cabrera, R., and Schwartz, R. A. (2022) Current knowledge of immunosuppression as a risk factor for skin cancer development, Crit. Rev. Oncol. Hematol., 177, 103754, https://doi.org/10.1016/J.CRITREVONC.2022.103754.
Dugué, P. A., Rebolj, M., Garred, P., and Lynge, E. (2013) Immunosuppression and risk of cervical cancer, Expert Rev. Anticancer Ther., 13, 29-42, https://doi.org/10.1586/ERA.12.159.
You, Y., Li, Y., Li, M., Lei, M., Wu, M., Qu, Y., Yuan, Y., Chen, T., and Jiang, H. (2018) Ovarian cancer stem cells promote tumour immune privilege and invasion via CCL5 and regulatory T cells, Clin. Exp. Immunol., 191, 60-73, https://doi.org/10.1111/CEI.13044.
Baldominos, P., Barbera-Mourelle, A., Barreiro, O., Huang, Y., Wight, A., Cho, J. W., Zhao, X., Estivill, G., Adam, I., Sanchez, X., McCarthy, S., Schaller, J., Khan, Z., Ruzo, A., Pastorello, R., Richardson, E. T., Dillon, D., Montero-Llopis, P., Barroso-Sousa, R., Forman, J., Shukla, S. A., Tolaney, S. M., Mittendorf, E. A., von Andrian, U. H., Wucherpfennig, K. W., Hemberg, M., and Agudo, J. (2022) Quiescent cancer cells resist T cell attack by forming an immunosuppressive niche, Cell, 185, 1694-1708, https://doi.org/10.1016/J.CELL.2022.03.033.
Lebeau, G., Ah-Pine, F., Daniel, M., Bedoui, Y., Vagner, D., Frumence, E., and Gasque, P. (2022) Perivascular mesenchymal stem/stromal cells, an immune privileged niche for viruses? Int. J. Mol. Sci., 23, 8038, https://doi.org/10.3390/IJMS23148038.
Theofilopoulos, A. N., Kono, D. H., and Baccala, R. (2017) The Multiple pathways to autoimmunity, Nat. Immunol., 18, 716-724, https://doi.org/10.1038/NI.3731.
Legoux, F. P., Lim, J. B., Cauley, A. W., Dikiy, S., Ertelt, J., Mariani, T. J., Sparwasser, T., Way, S. S., and Moon, J. J. (2015) CD4+ T cell tolerance to tissue-restricted self antigens is mediated by antigen-specific regulatory T Cells rather than deletion, Immunity, 43, 896-908, https://doi.org/10.1016/J.IMMUNI.2015.10.011.
Sergeant, E., Buysse, M., Devos, T., and Sprangers, B. (2021) Multipotent mesenchymal stromal cells in kidney transplant recipients: the next big thing? Blood Rev., 45, 100718, https://doi.org/10.1016/J.BLRE.2020.100718.
López-García, L., and Castro-Manrreza, M. E. (2021) TNF-α and IFN-γ participate in improving the immunoregulatory capacity of mesenchymal stem/stromal cells: importance of cell-cell contact and extracellular vesicles, Int. J. Mol. Sci., 22, 9531, https://doi.org/10.3390/IJMS22179531.
Blokzijl, F., De Ligt, J., Jager, M., Sasselli, V., Roerink, S., Sasaki, N., Huch, M., Boymans, S., Kuijk, E., Prins, P., Nijman, I. J., Martincorena, I., Mokry, M., Wiegerinck, C. L., Middendorp, S., Sato, T., Schwank, G., Nieuwenhuis, E. E. S., Verstegen, M. M. A., Van Der Laan, L. J. W., De Jonge, J., Ijzermans, J. N. M., Vries, R. G., Van De Wetering, M., Stratton, M. R., Clevers, H., Cuppen, E., and Van Boxtel, R. (2016) Tissue-specific mutation accumulation in human adult stem cells during life, Nature, 538, 260-264, https://doi.org/10.1038/NATURE19768.
Cooke, J. P. (2019) Inflammation and its role in regeneration and repair, Circ. Res., 124, 1166-1168, https://doi.org/10.1161/CIRCRESAHA.118.314669.
Vannella, K. M., and Wynn, T. A. (2017) Mechanisms of organ injury and repair by macrophages, Annu. Rev. Physiol., 79, 593-617, https://doi.org/10.1146/ANNUREV-PHYSIOL-022516-034356.
Zhang, R., Xu, K., Shao, Y., Sun, Y., Saredy, J., Cutler, E., Yao, T., Liu, M., Liu, L., Drummer IV, C., Lu, Y., Saaoud, F., Ni, D., Wang, J., Li, Y., Li, R., Jiang, X., Wang, H., and Yang, X. (2021) Tissue Treg secretomes and transcription factors shared with stem cells contribute to a Treg niche to maintain Treg-ness with 80% innate immune pathways, and functions of immunosuppression and tissue repair, Front. Immunol., 11, 632239, https://doi.org/10.3389/FIMMU.2020.632239.
Cho, I., Lui, P. P., and Ali, N. (2020) Treg regulation of the epithelial stem cell lineage, J. Immunol. Regen. Med., 8, 100028, https://doi.org/10.1016/J.REGEN.2020.100028.
Li, J., Tan, J., Martino, M. M., and Lui, K. O. (2018) Regulatory T-cells: potential regulator of tissue repair and regeneration, Front. Immunol., 9, 585, https://doi.org/10.3389/FIMMU.2018.00585.
Liu, J., Sato, C., Cerletti, M., and Wagers, A. (2010) Notch signaling in the regulation of stem cell self-renewal and differentiation, Curr. Top. Dev. Biol., 92, 367-409, https://doi.org/10.1016/S0070-2153(10)92012-7.
Ali, N., Zirak, B., Rodriguez, R. S., Pauli, M. L., Truong, H. A., Lai, K., Ahn, R., Corbin, K., Lowe, M. M., Scharschmidt, T. C., Taravati, K., Tan, M. R., Ricardo-Gonzalez, R. R., Nosbaum, A., Bertolini, M., Liao, W., Nestle, F. O., Paus, R., Cotsarelis, G., Abbas, A. K., and Rosenblum, M. D. (2017) Regulatory T cells in skin facilitate epithelial stem cell differentiation, Cell, 169, 1119-1129, https://doi.org/10.1016/J.CELL.2017.05.002.
Golub, R. (2021) The Notch signaling pathway involvement in innate lymphoid cell biology, Biomed. J., 44, 133-143, https://doi.org/10.1016/J.BJ.2020.12.004.
Meng, J., Jiang, Y.-Zhou, Zhao, S., Tao, Y., Zhang, T., Wang, X., Zhang, Y., Sun, K., Yuan, M., Chen, J., Wei, Y., Lan, X., Chen, M., David, C. J., Chang, Z., Guo, X., Pan, D., Chen, M., Shao, Z. M., Kang, Y., and Zheng, H. (2022) Tumor-derived Jagged1 promotes cancer progression through immune evasion, Cell Rep., 38, 110492, https://doi.org/10.1016/J.CELREP.2022.110492.
Chazaud, B. (2020) Inflammation and skeletal muscle regeneration: leave it to the macrophages!, Trends Immunol., 41, 481-492, https://doi.org/10.1016/J.IT.2020.04.006.
Oishi, Y., and Manabe, I. (2018) Macrophages in inflammation, repair and regeneration, Int. Immunol., 30, 511-528, https://doi.org/10.1093/INTIMM/DXY054.
Velissaris, D., Zareifopoulos, N., Lagadinou, M., Platanaki, C., Tsiotsios, K., Stavridis, E. L., Kasartzian, D. I., Pierrakos, C., and Karamouzos, V. (2021) Procalcitonin and sepsis in the emergency department: an update, Eur. Rev. Med. Pharmacol. Sci., 25, 466-479, https://doi.org/10.26355/EURREV_202101_24416.
Lombardo, E., and Delarosa, O. (2010) Modulation of adult mesenchymal stem cells activity by toll-like receptors: implications on therapeutic potential, Mediators Inflamm., 2010, 865601, https://doi.org/10.1155/2010/865601.
Raicevic, G., Rouas, R., Najar, M., Stordeur, P., Id Boufker, H., Bron, D., Martiat, P., Goldman, M., Nevessignsky, M. T., and Lagneaux, L. (2010) Inflammation modifies the pattern and the function of Toll-like receptors expressed by human mesenchymal stromal cells, Hum. Immunol., 71, 235-244, https://doi.org/10.1016/J.HUMIMM.2009.12.005.
Wu, Q., You, L., Nepovimova, E., Heger, Z., Wu, W., Kuca, K., and Adam, V. (2022) Hypoxia-inducible factors: master regulators of hypoxic tumor immune escape, J. Hematol. Oncol., 15, 77, https://doi.org/10.1186/S13045-022-01292-6.
Newman, H., Shih, Y. V., and Varghese, S. (2021) Resolution of inflammation in bone regeneration: from understandings to therapeutic applications, Biomaterials, 277, 121114, https://doi.org/10.1016/J.BIOMATERIALS.2021.121114.
Song, X., Zhang, Y., Zhang, L., Song, W., and Shi, L. (2018) Hypoxia enhances indoleamine 2,3-dioxygenase production in dendritic cells, Oncotarget, 9, 11572-11580, https://doi.org/10.18632/ONCOTARGET.24098.
Matheakakis, A., Batsali, A., Papadaki, H. A., and Pontikoglou, C. G. (2021) Therapeutic implications of mesenchymal stromal cells and their extracellular vesicles in autoimmune diseases: from biology to clinical applications, Int. J. Mol. Sci., 22, 10132, https://doi.org/10.3390/IJMS221810132.
Petinati, N., Kapranov, N., Davydova, Y., Bigildeev, A., Pshenichnikova, O., Karpenko, D., Drize, N., Kuzmina, L., Parovichnikova, E., and Savchenko, V. (2020) Immunophenotypic characteristics of multipotent mesenchymal stromal cells that affect the efficacy of their use in the prevention of acute graft vs host disease, World J. Stem Cells, 12, 1377-1395, https://doi.org/10.4252/WJSC.V12.I11.1377.
Ara, T., and Hashimoto, D. (2021) Novel insights into the mechanism of GVHD-induced tissue damage, Front. Immunol., 12, 713631, https://doi.org/10.3389/fimmu.2021.713631.
Proics, E., David, M., Mojibian, M., Speck, M., Lounnas-Mourey, N., Govehovitch, A., Baghdadi, W., Desnouveaux, J., Bastian, H., Freschi, L., Privat, G., Pouzet, C., Grossi, M., Heimendinger, P., Abel, T., Fenard, D., Levings, M. K., Meyer, F., and Dumont, C. (2023) Preclinical assessment of antigen-specific chimeric antigen receptor regulatory t cells for use in solid organ transplantation, Gene Ther., 30, 309-322, https://doi.org/10.1038/S41434-022-00358-X.
Alanazi, R. F., Alhwity, B. S., Almahlawi, R. M., Alatawi, B. D., Albalawi, S. A., Albalawi, R. A., Albalawi, A. A., Abdel-Maksoud, M. S., and Elsherbiny, N. (2023) Multilineage differentiating stress enduring (Muse) cells: a new era of stem cell-based therapy, Cells, 12, 1676, https://doi.org/10.3390/CELLS12131676.
Kushioka, J., Chow, S. K. H., Toya, M., Tsubosaka, M., Shen, H., Gao, Q., Li, X., Zhang, N., and Goodman, S. B. (2023) Bone regeneration in inflammation with aging and cell-based immunomodulatory therapy, Inflamm. Regen., 43, 29, https://doi.org/10.1186/S41232-023-00279-1.
Akhbariyoon, H., Azizpour, Y., Esfahani, M. F., Firoozabad, M. S. M., Rad, M. R., Esfahani, K. S., Khoshavi, N., Karimi, N., Shirinisaz, A., Abedi, F., Rad, M. R., and Sharifi, P. (2021) Immune checkpoint inhibition for the treatment of cancers: an update and critical review of ongoing clinical trials, Clin. Immunol., 232, 108873, https://doi.org/10.1016/J.CLIM.2021.108873.
Kong, X. (2020) Discovery of new immune checkpoints: family grows up, Adv. Exp. Med. Biol., 1248, 61-82, https://doi.org/10.1007/978-981-15-3266-5_4.
Acknowledgments
The author would like to thank Alexey Bigildeev, Head of the Laboratory of Epigenetic Regulation of Hematopoiesis, NMRC Hematology, for critical reading of the work.
Funding
The research was financially supported by the Russian Science Foundation (grant no. 22-25-00459, https://rscf.ru/project/22-25-00459/ [in Russian]).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The author declares no conflict of interest in financial or any other sphere. This article does not describe any studies involving humans or animals performed by the author.
Rights and permissions
Open access. This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit https://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Karpenko, D.V. Immune Privileges as a Result of Mutual Regulation of Immune and Stem Systems. Biochemistry Moscow 88, 1818–1831 (2023). https://doi.org/10.1134/S0006297923110123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0006297923110123