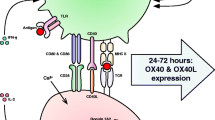
Abstract
A large body of evidence obtained during the last decade has demonstrated that neutrophils suppress T cell proliferation in different models of inflammation and cell interaction. The commonly used method for assessing cell proliferation and proliferation inhibition is measuring [3H]thymidine incorporation into cells. Earlier, we observed inhibition of [3H]thymidine uptake in experiments on neutrophil-mediated regulation of T cell response in tuberculosis immunity. Here, we used different types of proliferating cells to analyze the nature of the soluble “neutrophil factor” by a variety of methods (dialysis, HPLC, mass spectrometry, and NMR) and unambiguously demonstrated that neutrophils do not synthesize a specific factor inhibiting cell proliferation, but secrete high concentrations of extracellular thymidine that competitively inhibit [3H]thymidine incorporation. Although the physiological significance of thymidine secretion by neutrophils remains unknown, this phenomenon should be carefully considered when designing test systems for studying cell–cell interactions.
Similar content being viewed by others
Abbreviations
- APCs:
-
antigen-presenting cells
- CFSE:
-
carboxyfluorescein succinimidyl ester
- 13C-1H-HSQC:
-
heteronuclear single quantum correlation spectroscopy
- DQF-COSY:
-
double-quantum filtered correlation spectroscopy
- MHC:
-
major histocompatibility complex
- PBS:
-
phosphate buffered saline
References
Witko-Sarsat, V., Rieu, P., Descamps-Latscha, B., Lesavre, P., and Halbwachs-Mecarelli, L. (2000) Neutrophils: molecules, functions and pathophysiological aspects, Lab. Invest., 80, 617–653.
Nathan, C. (2006) Neutrophils and immunity: challenges and opportunities, Nat. Rev. Immunol., 6, 173–182.
Kuijpers, T. W., Van den Berg, T. K., and Roos, D. (2009) Phagocyte–Pathogen Interactions (Russel, D. G., and Gordon S., eds.) ASM Press, Washington DC,pp. 3–26.
Quint, J. K., and Wedzicha, J. A. (2007) The neutrophil in chronic obstructive pulmonary disease, J. Allergy Clin. Immunol., 119, 1065–1071.
Eruslanov, E. B., Lyadova, I. V., Kondratieva, T. K., Majorov, K. B., Scheglov, I. V., Orlova, M. O., and Apt, A. S. (2005) Neutrophil responses to Mycobacterium tuberculosis infection in genetically susceptible and resistant mice, Infect. Immun., 73, 1744–1753.
Eum, S. Y., Kong, J. H., Hong, M. S., Lee, Y. J., Kim, J. H., Hwang, S. H., Cho, S. N., Via, L. E., and Barry, C. E., 3rd. (2010) Neutrophils are the predominant infected phagocytic cells in the airways of patients with active pulmonary TB, Chest, 137, 122–128.
Tanaka, D. (2006) Essential role of neutrophils in anti-type II collagen antibody and lipopolysaccharide-induced arthritis, Immunology, 119, 195–202.
Chin, A. C., and Parkos, C. A. (2006) Neutrophil transepithelial migration and epithelial barrier function in IBD: potential targets for inhibiting neutrophil trafficking, Ann. N. Y. Acad. Sci., 1072, 276–287.
Soehnlein, O., Weber, C., and Lindbom, L. (2009) Neutrophil granule proteins tune monocytic cell function, Trends Immunol., 30, 538–546.
Yang, C. W., Strong, B. S. I., Miller, M. J., and Unanue, E. R. (2010) Neutrophils influence the level of antigen presentation during the immune response to protein antigens in adjuvants, J. Immunol., 185, 2927–2934.
Jaeger, B. N., Donadieu, J., Cognet, C., Bernat, C., Ordonez-Rueda, D., Barlogis, V., Mahlaoui, N., Fenis, A., Narni-Mancinelli, E., Beaupain, B., Bellanne-Chantelot, C., Bajenoff, M., Malissen, B., Malissen, M., Vivier, E., and Ugolini, S. (2012) Neutrophil depletion impairs natural killer cell maturation, function, and homeostasis, J. Exp. Med., 209, 565–580.
Kondratieva, T. K., Rubakova, E. I., Linge, I. A., Evstifeev, V. V., Majorov, K. B., and Apt, A. S. (2010) B cells delay neutrophil migration toward the site of stimulus: tardiness critical for effective bacillus Calmette–Guerin vaccination against tuberculosis infection in mice, J. Immunol., 184, 1227–1234.
Kozakiewicz, L., Chen, Y., Xu, J., Wang, Y., DunussiJannopopulos, K., Ou, Q., Flynn, J. L., Porcelli, S. A., Jacobs, W. R., and Chan, J. (2013) B cells regulate neutrophilia during Mycobacterium tuberculosis infection and BCG vaccination by modulating the interleukin-17 response, PLoS Pathog., 9, e1003472.
Yang, D., De la Rosa, G., Tewary, P., and Oppenheim, J. J. (2009) Alarmins link neutrophils and dendritic cells, Trends Immunol., 30, 531–537.
Barquero-Calvo, E., Martirosyan, A., Ordonez-Rueda, D., Arce-Gorvel, V., Alfaro-Alarcon, A., Lepidi, H., Malissen, B., Malissen, M., Gorvel, J. P., and Moreno, E. (2013) Neutrophils exert a suppressive effect on Th1 responses to intracellular pathogen Brucella abortus, PLoS Pathog., 9, e1003167.
Muller, I., Munder, M., Kropf, P., and Hansch, G. M. (2009) Polymorphonuclear neutrophils and T-lymphocytes: strange bedfellows or brothers in arms? Trends Immunol., 30, 522–530.
D’Avila, H., Roque, N. R., Cardoso, R. M., Castro-FariaNeto, H. C., Melo, R. C., and Bozza, P. T. (2008) Neutrophils recruited to the site of Mycobacterium bovis BCG infection undergo apoptosis and modulate lipid body biogenesis and prostaglandin E production by macrophages, Cell. Microbiol., 10, 2589–2604.
Yeremeev, V., Linge, I., Kondratieva, T., and Apt, A. (2015) Neutrophils exacerbate tuberculosis infection in genetically susceptible mice, Tuberculosis (Edinb.), 95, 447–451.
Majorov, K. B., Lyadova, I. V., Kondratieva, T. K., Eruslanov, E. B., Rubakova, E. I., Orlova, M. O., Mischenko, V. V., and Apt, A. S. (2003) Different innate ability of I/St and A/Sn mice to combat virulent Mycobacterium tuberculosis: phenotypes expressed in lung and extrapulmonary macrophages, Infect. Immun., 71, 697–707.
Pichugin, A. V., Khaidukov, S. V., Moroz, A. M., and Apt, A. S. (1998) Capacity of murine T cells to retain long-term responsiveness to mycobacterial antigens is controlled by the H-2 complex, Clin. Exp. Immunol., 111, 316–324.
Nagarai, S., Youn, J. I., and Gabrilovich, D. I. (2013) Reciprocal relationship between myeloid-derived suppressor cells and T-cells, J. Immunol., 191, 17–23.
Biological Magnetic Resonance Data Bank. Thymidine (http://bmrb.wisc.edu/metabolomics/mol_summary/show_data.php?molName=thymidine&id=bmse000244).
Reiter, H. (1979) Effect of thymidine on the survival of mice with EL4 tumors, Cancer Res., 39, 4856–4860.
Lyons, A. B., and Parish, C. R. (1994) Determination of lymphocyte division by flow cytometry, J. Immunol. Methods, 171, 131–137.
Iatropoulos, M. J., and Williams, G. M. (1996) Proliferation markers, Exp. Toxicol. Pathol., 48, 175–181.
Vega-Avila, E., and Pugsley, M. K. (2011) An overview of colorimetric assay methods used to assess survival or proliferation of mammalian cells, Proc. West Pharmacol. Soc., 54, 10–14.
Opitz, H. G., Niethammer, D., Lemke, H., Flad, H. D., and Huget, R. (1975) Inhibition of 3H-thymidine incorporation of lymphocytes by a soluble factor from macrophages, Cell. Immunol., 16, 379–388.
Stadecker, M. J., Calderon, J., Karnovsky, M. L., and Unanue, E. R. (1977) Synthesis and release of thymidine by macrophages, J. Immunol., 119, 1738–1743.
Spilsberg, B., Rise, F., Petersen, D., and Nissen-Meyer, J. (2006) Thymidine secretion by hybridoma and myeloma cells, Biochem. Biophys. Res. Commun., 342, 221–226.
Vorobjeva, N. V., and Pinegin, B. V. (2014) Neutrophil extracellular traps: mechanisms of formation and role in health and disease, Biochemistry (Moscow), 79, 1286–1296.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Original Russian Text © I. A. Linge, E. V. Kondratieva, T. K. Kondratieva, V. A. Makarov, V. I. Polshakov, O. Yu. Savelyev, A. S. Apt, 2016, published in Biokhimiya, 2016, Vol. 81, No. 11, pp. 1530–1539.
Rights and permissions
About this article
Cite this article
Linge, I.A., Kondratieva, E.V., Kondratieva, T.K. et al. “Suppressor factor” of neutrophils: A short story of a long-term misconception. Biochemistry Moscow 81, 1284–1292 (2016). https://doi.org/10.1134/S0006297916110067
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0006297916110067