Summary
Question of the study
The term ‘sleep attack’ is used in patients with Parkinson's disease (PD) to designate a sudden onset of sleep (SOS) without any prior sleepiness. Clinically, sleep attacks can be distinguished from unintended sleep episodes, i.e. SOS with prior sleepiness. This study aimed to assess the prevalence of SOS and to identify its predictors in patients with sleep-disordered breathing (SDB).
Patients and methods
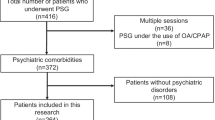
A total of 114 consecutive patients with the clinical suspicion of obstructive sleep apnoea syndrome (OSAS) and a respiratory disturbance index (RDI) of >5/h were examined using a questionnaire and polysomnography (PSG).
Results
Altogether 57.7% reported SOS, with 5.2% of the total population describing exclusively sleep attacks. SOS was observed in both patients with obstructive sleep apnoea-hypopnoea (OSAH) or increased upper airway resistance (UAR). Increased scores on the Epworth Sleepiness Scale (ESS) were the best predictor of SOS. Logistic regression showed a possible association of SOS with a low PLMS index, while no definite effect was observed for other PSG parameters.
Conclusions
Our data show that SDB is frequently associated with SOS. Future studies should address in more detail whether SDB patients with sleep attacks pose an increased accident risk.
Zusammenfassung
Fragestellung
Der Begriff “Schlafattacke” wird bei Parkinson-Patienten verwendet, um ein plötzliches Einschlafen ohne vorherige Müdigkeit zu kennzeichnen. Klinisch können “Schlafattacken” von unbeabsichtigten Schlafepisoden, d. h. einem plötzlichen Einschlafen mit vorheriger Müdigkeit, unterschieden werden. Die vorliegende Studie wurde durchgeführt, um die Prävalenz des plötzlichen Einschlafens und dessen Prädiktoren in Patienten mit schlafbezogenen Atmungsstörungen zu bestimmen.
Patienten und Methodik
114 Patienten mit der klinischen Verdachtsdiagnose eines obstruktiven Schlafapnoe-Syndroms und einem Index schlafbezogener Atmungsstörungen >5/h wurden mittels eines Fragebogens und Poly somnographie (PSG) untersucht.
Ergebnisse
Insgesamt 57,7% berichteten ein plötzliches Einschlafen, wobei 5,2% der Gesamtpopulation ausschließlich “Schlafattacken” angaben. Plötzliches Einschlafen wurde sowohl in Patienten mit einer obstruktiven Schlafapnoe bzw.-hypopnoe als auch in Patienten mit einem erhöhten Widerstand der oberen Atemwege beobachtet. Erhöhte Punktwerte auf der Epworth-Schläfrigkeitsskala stellten den besten Prädiktor für plötzliches Einschalfen dar. Ferner zeigten logistische Regressionen eine mögliche Assoziation von plötzlichem Einschlafen mit einem niedrigen PLMS-Index, während kein eindeutiger Effekt für andere PSG-Parameter gefunden wurde.
Schlussfolgerungen
Unsere Data zeigen, dass schlafbezogene Atmungsstörungen häufig mit plötzlichem Einschlafen verbunden sind. zukünftige Studien sollten detailliert klären, ob Patienten mit “Schlafattacken” eine erhöhtes Unfallrisiko aufweisen.
Similar content being viewed by others
References
Arnulf I, Konofal E, Merino-Andreu M, Houeto JL, Mesnage V, Welter ML, Lacomblez L, Golmard JL, Derenne JP, Agid Y: Parkinson's disease and sleepiness: an integral part of PD. Neurology 58: 1019–1024, 2002.
ASDA. International classification of sleep disorders, revised: diagnostic and coding manual. American Sleep Disorders Association, Rochester, MN, 1997.
Barbe F, Pericas J, Munoz A, Findley L, Anto JM, Agusti AGN, de Lluc Joan M: Automobile accidents in patients with sleep apnea syndrome. Am J Respir Crit Care Med 158: 18–22, 1998.
Bassiri AG, Guilleminault C: Clinical features and evaluation of obstructive sleep apnea-hypopnea syndrome. In: Kryger MH, Roth T, Dement WC (eds): Principles and practice of sleep medicine, Saunders, Philadelphia, pp 869–878, 2000.
Carmona Bernal C, Capote Gil F, Botebol Benhamou G, Garcia Lopez P, Sanchez Armengol A, Castillo Gomez J: Assessment of excessive daytime sleepiness in professional drivers with suspected obstructive sleep apnea syndrome. Arch Bronconeumol 36: 436–440, 2000.
Cassel W, Ploch T, Peter JH, von Wichert P: Risk of accidents in patients with nocturnal respiration disorders. Pneumologie 45(Suppl 1): 271–275, 1991.
Chervin RD: Periodic leg movements and sleepiness in patients evaluated for sleep-disordered breathing. Am J Respir Crit Care Med 164: 1454–1458, 2001.
Chervin RD, Aldrich MS: Characteristics of apneas and hypopneas during sleep and relation to excessive daytime sleepiness. Sleep 21: 799–806, 1998.
Dement W, Rechtschaffen A, Gulevich G: The nature of the narcoleptic sleep attack. Neurology 16: 18–33, 1966.
El-Ad B, Chervin RD: The case of a missing PLM. Sleep 23: 450–451, 2000.
Frucht S, Rogers JD, Greene PE, Gordon MF, Fahn S: Falling asleep at the wheel: motor vehicle mishaps in persons taking pramipexole and ropinirole. Neurology 52: 1908–1910, 1999.
George CF, Smiley A: Sleep apnea and automobile crashes. Sleep 22: 790–795, 1999.
Gottlieb DJ, Yao Q, Redline S, Ali T, Mahowald MW: Does snoring predict sleepiness independently of apnea and hypopnea frequency? Am J Respir Crit Care Med 162: 1512–1517, 2000.
Guilleminault C, Stoohs R, Clerk A, Cetel M, Maistros P: A cause of excessive daytime sleepiness. The upper airway resistance syndrome. Chest 104: 781–787, 1993.
Hishikawa Y, Nanno H, Tachibana M, Furuya E, Koida H, Kaneko Z: The nature of sleep attack and other symptoms of narcolepsy. Electroencephalogr Clin Neurophysiol 24: 1–10, 1968.
Hobson DE, Lang AE, Martin WR, Razmy A, Rivest J, Fleming J: Excessive daytime sleepiness and sudden-onset sleep in Parkinson disease: a survey by the Canadian Movement Disorders Group, JAMA 287: 455–463, 2002.
Homann CN, Wenzel K, Suppan K, Ivanic G, Kriechbaum N, Crevenna R, Ott E: Sleep attacks in patients taking dopamine agonists: review. BMJ 324: 1483–1487, 2002.
Johns MW: A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep 14: 540–545, 1991.
Johns MW: Daytime sleepiness, snoring, and obstructive sleep apnea. The Epworth Sleepiness Scale. Chest 103: 30–36, 1993.
Karadeniz D, Ondze B, Besset A, Billiard M: EEG arousals and awakenings in relation with periodic leg movements during sleep. J Sleep Res 9: 273–277, 2000.
Körner Y, Meindorfner C, Möller JC, Stiasny-Kolster K, Haja D, Cassel W, Oertel WH, Krüger HP: Predictors of sudden onset of sleep. Mov Disord 19: 1298–1305, 2004.
Meindorfner C, Körner Y, Möller JC Stiasny-Kolster K, Oertel WH, Krüger H-P: Driving in Parkinson's disease-mobility, accidents, and sudden onset of sleep at the wheel. Mov Disord: forthcoming.
Noda A, Yagi T, Yokota M, Kayukawa Y, Ohta T, Okada T: Daytime sleepiness and automobile accidents in patients with obstructive sleep apnea syndrome. Psychiatry Clin Neurosci 52: 221–222, 1998.
Ondo WG, Dat Vuong K, Khan H, Atassi F, Kwak C, Jankovic J: Daytime sleepiness and other sleep disorders in Parkinson's disease. Neurology 57: 1392–1396, 2001.
Paus S, Brecht HM, Koster J, Seeger G, Klockgether T, Wüllner U: Sleep attacks, daytime sleepiness, and dopamine agonists in Parkinson's disease. Mov Disord 18: 659–667, 2003.
Penzel T, Hajak G, Hoffmann RM, Lund R, Podszus T, Pollmächer T, Schäfer T, Schulz H, Sonnenschein W, Spieweg I: Empfehlungen zur Durchführung und Auswertung polygraphischer Ableitungen im diagnostischen Schlaflabor. Zeitschr EEG EMG 24: 65–70, 1993.
Punjabi NM, Bandeen-Roche K, Marx JJ, Neubauer DN, Smith PL, Schwartz AR: The association between daytime sleepiness and sleep-disordered breathing in NREM and REM sleep. Sleep 25: 307–314, 2002.
Rechtschaffen A, Kales A: A manual of standardized terminology: techniques and scoring system for sleep stages of human subjects. UCLA Brain Information Service. Los Angeles, 1968.
Roehrs T, Zorick F, Wittig R, Conway W, Roth T: Predictors of objective level of daytime sleepiness in patients with sleep-related breathing disorders. Chest 95: 1202–1206, 1989.
Roth T, Rye DB, Borchert LD, Bartlett C, Bliwise DL, Cantor C, Gorell JM, Hubble JP, Musch B, Olanow CW, Pollak C, Stern MB, Watts RL: Assessment of sleepiness and unintended sleep in Parkinson's disease patients taking dopamine agonists. Sleep Med 4: 275–280, 2003.
Rye DB, Bliwise DL, Dihenia B, Gurecki P: Daytime sleepiness in Parkinson's disease. J Sleep Res 9: 63–69, 2000.
Seneviratne U, Puvanendran K: Excessive daytime sleepiness in obstructive sleep apnea: prevalence, severity, and predictors. Sleep Med 5: 339–343, 2004.
Shiomi T, Arita AT, Sasanabe R, Banno K, Yamakawa H, Hasegawa R, Ozeki K, Okada M, Ito A: Falling asleep while driving and automobile accidents among patients with obstructive sleep apnea-hypopnea syndrome. Psychiatry Clin Neurosci 56: 333–334, 2002.
Teran-Santos J, Jimenez-Gomez A, Cordero-Guevara J: The association between sleep apnea and the risk of traffic accidents. Cooperative Group Burgos-Santander. N Engl J Med 340: 847–851, 1999.
Turkington PM, Sircar M, Allgar V, Elliott MW: Relationship between obstructive sleep apnoea, driving simulator performance, and risk of road traffic accidents. Thorax 56: 800–805, 2001.
Zeman A, Britton T, Douglas N, Hansen A, Hicks J, Howard R, Meredith A, Smith I, Stores G, Wilson S, Zaiwalla Z: Narcolepsy and excessive daytime sleepiness. BMJ 329: 724–728, 2004.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Möller, J.C., Cassel, W., Stiasny-Kolster, K. et al. ‘Sleep attacks’ in patients with sleep-disordered breathing. Somnologie 9, 127–132 (2005). https://doi.org/10.1111/j.1439-054X.2005.00060.x
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1439-054X.2005.00060.x