Abstract
Cognitive impairment is a key feature of schizophrenia (SZ) and determines functional outcome. Nonetheless, molecular signatures in neuronal tissues that associate with deficits are not well understood. We conducted nasal biopsy to obtain olfactory epithelium from patients with SZ and control subjects. The neural layers from the biopsied epithelium were enriched by laser-captured microdissection. We then performed an unbiased microarray expression study and implemented a systematic neuropsychological assessment on the same participants. The differentially regulated genes in SZ were further filtered based on correlation with neuropsychological traits. This strategy identified the SMAD 5 gene, and real-time quantitative PCR analysis also supports downregulation of the SMAD pathway in SZ. The SMAD pathway has been important in multiple tissues, including the role for neurodevelopment and bone formation. Here the involvement of the pathway in adult brain function is suggested. This exploratory study establishes a strategy to better identify neuronal molecular signatures that are potentially associated with mental illness and cognitive deficits. We propose that the SMAD pathway may be a novel target in addressing cognitive deficit of SZ in future studies.
Similar content being viewed by others
Introduction
Although operational diagnostic systems such as the Diagnostic and Statistical Manual of Mental Disorders (DSM) may increase the reliability of diagnoses,1 they do little to aid our understanding of the biological basis of psychiatric conditions. For example, cognitive impairment is a key feature of schizophrenia (SZ) and a predictor of functional outcome in patients:2, 3, 4 nonetheless, molecular cascades that specifically underlie cognitive deficit in SZ are not yet well understood. It is likely that the current DSM-based classification of SZ alone is insufficient for providing an accurate framework for studying molecular signatures underlying cognitive impairment.
A perpetual challenge to uncovering molecular mechanisms in psychiatric disorders is the difficulty of obtaining central nervous system tissues and cells from live patients that are likely to underlie clinical features.5, 6, 7 Post-mortem brains are valuable resources for studying molecular signatures; however, these do not reliably provide molecular information associated with the onset or course of cognitive impairment in living subjects. There is a critical need for reliable and representative biological samples that can be collected longitudinally. Blood is frequently used because of its ease of repeated collection; however, we have previously shown that the gene expression profile of lymphocytes and lymphoblasts (LBs) derived from peripheral blood is dissimilar to that of fetal and adult brain.8 Several groups have proposed that the olfactory epithelium (OE), which contains olfactory receptor neurons, may be a good surrogate to address this question.8, 9, 10, 11 In particular, we have reported a method to enrich neuronal cells from the biopsied epithelium using laser-captured microdissection (LCM) to study molecular signatures relevant to neurons.12, 13
Deficits in olfaction are known in several neuropsychiatric conditions, including SZ, Parkinson’s disease and Alzheimer’s disease, which likely associate with cellular or molecular dysregulation in the OE.9, 11, 14 In SZ, olfactory dysfunction is associated with negative and cognitive symptoms.15, 16, 17 Furthermore, the OE contains cells of neuronal lineage at multiple stages of maturity.18, 19 This provides a unique opportunity to investigate aspects of neurodevelopment, which may have been derailed early in life in SZ.
In the present study, we aimed to establish a strategy to uncover molecular signatures that reflect changes in neuronal cells and are associated with cognitive impairment in SZ. This exploratory study addressed the question using a unique, multilayered approach to discover molecular candidates, taking correlation with behavioral dimensions into consideration. We examined molecular expression profiles in the olfactory neuronal layers in parallel with systematic neuropsychological assessments on the same participants. We used correlation between differentially expressed genes and neuropsychological traits as an additional filter following correction for multiple testing. On the basis of this exploratory strategy, we propose that the SMAD pathway may be an interesting target in studying cognitive deficits related to SZ.
Materials and methods
Subject recruitment and clinical assessment
Patients with chronic SZ were recruited from outpatient clinics in the Johns Hopkins Schizophrenia Center. Diagnosis was determined according to the DSM-IV.20 Normal control subjects were recruited from the general population through flyers posted at Johns Hopkins Medicine and an ad hoc advertisement in a local magazine. Participants were matched for age, sex, race, education and smoking status. All subjects were administered the Structured Clinical Interview for DSM-IV Axis I Disorders-Clinician Version,21 and SZ patients were assessed with the Scales for the Assessment of Positive and Negative Symptoms.22 Subjects were excluded from the study if they had a history of traumatic brain injury with loss of consciousness for >1 h, a history of drug abuse within 6 months of the study, a history of drug dependence within 12 months of the study or a history of untreated major medical illnesses. The study was conducted under approval of the Johns Hopkins Institutional Review Board (Protocol #NA_00037204: AS is the PI of this protocol), and all the subjects gave written consent for their participation.
Nasal biopsy and LCM of OE from subjects
OE tissues were obtained with nasal biopsy under local anesthesia to the nasal cavity. The biopsy procedure was performed under endoscopic control and used either a small curette or biting forceps for tissue removal. To avoid trauma to the cribriform plate, the biopsies were usually taken from the upper nasal septum. The tissue was removed from either the front or the back of the olfactory cleft, or both. Four to six pieces of tissue (5 mm3) were removed from each nostril. The neuronal OE layers were enriched and purified using LCM. Detailed methods for this procedure have been reported previously by our group12, 13 and can be viewed at the following URL: http://www.jove.com/video/51853/. As described previously, successful enrichment of neuronal cells using this method is evidenced by substantially higher expression of olfactory marker protein, a specific olfactory receptor neuronal marker, and beta tubulin III in the microdissected tissue relative to that of the whole OE sample.13
Neuropsychological assessment
Neuropsychological assessments were conducted for 16 SZ patients and 15 control subjects (demographic data are shown in Table 1) according to a methodology published by our group.16, 23, 24 Participants completed tests from the Calibrated Neuropsychological Normative System and the Hopkins Adult Reading Test (HART) to estimate premorbid IQ based on the HART. The six-factor domain includes the following: (i) (psychomotor) processing speed, (Trail Making Test–part A, Trail Making Test–part B and Grooved Pegboard Test); (ii) attention/working memory (Brief Test of Attention–Letter, Brief Test of Attention–Number and Conners’ Continuous Performance Test hit reaction time s.e.); (iii) verbal learning/memory, (Hopkins Verbal Learning Test-Revised–Learning and Hopkins Verbal Learning Test–Delayed Recall); (iv) visual learning/memory (Brief Visuospatial Memory Test-Revised–Learning and Brief Visuospatial Memory Test-Revised–Delayed Recall); (v) ideational fluency (letter, category and design tests); and (vi) executive functioning (Modified Wisconsin Card Sorting Test–category sorts and Modified Wisconsin Card Sorting Test–errors).24 The neuropsychological test scores in each domain have acceptable internal homogeneity, as shown in our previous study.23 The six factors capture the fundamental domains of cognitive functioning typically disrupted in SZ and the composite score is defined as the mean of the six-factor scores.24, 25
LBs from human subjects
Peripheral blood samples were collected from all subjects who underwent nasal biopsy and neuropsychological assessments (except for one SZ patient from whom we had OE but could not obtain blood). Lymphocytes were obtained from the peripheral blood, followed by incubation at 37 °C for 20–25 days to generate LBs according to a published protocol.26 As the LBs were derived from subjects who also underwent nasal biopsy, all of the LB samples were 'paired' with their respective OE tissue. Therefore, they are hereafter referred to as the 'paired' LBs (15 patients with SZ and 15 control subjects).
In addition, LBs were generated from peripheral blood of an independent cohort consisting of 16 patients with SZ and 18 control subjects using the method described above. These LBs are hereafter referred to as the 'non-paired' LBs to distinguish them from the 'paired' LBs (see Table 1).
Microarray analysis
We used a published protocol from our group.14 Briefly, total RNA was isolated from the neural layers of OE or paired/non-paired LBs from patients with SZ and control subjects using the RNeasy Mini Kit (Qiagen) according to manufacturer’s instructions. The RNA was of high quality, with an RNA integrity number score of 10, which was assessed using a Bioanalyzer RNA 6000 Nano Chip (Agilent Technologies). Fragmented biotin-labeled cRNAs were hybridized to Affymetrix U133 Plus2.0 according to the manufacturer’s protocol. Data analysis was performed using the Partek Genomics Suite software (version 6.5, Partek) and R (http://www.r-project.org/, version 3.1.1) with Bioconductor packages (http://www.bioconductor.org/). Raw intensities were normalized using the GC-Robust Multi-array Average. For differential gene expression analysis, one-way analysis of variance (ANOVA) was used to test the mean differences between two groups. The ANOVA P-values were adjusted using the Benjamini–Hochberg procedure to control the false discovery rate (FDR).27 The raw data (CEL files) are deposited in the Gene Expression Omnibus archive at the National Center for Biotechnology Information (GSE73129: http://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE73129). To the best of our knowledge, this is the first report of microarray data for the paired and non-paired LBs, and the first report of the OE microarray data set analyzed in the present configuration of 16 SZ and 15 control subjects. The OE data have been reported previously in different configurations.13, 28
We examined expression patterns of co-regulated genes in the OE microarray data based on publicly available gene co-regulation networks.29 Raw data for the networks were downloaded from the Gene Expression Omnibus (accession id: GSE12526) and were processed to calculate the all-to-all correlation matrix as per the paper.29 A correlation coefficient cutoff of 0.75 re-constructed the networks consisting of 1645 correlations (that is, co-regulations) among 206 genes within a large set of human cell lines (N=295). Likewise, co-regulated gene pairs of the OE microarray data from only control subjects were also defined.
We compared the differentially expressed transcripts from the OE microarray to the genes identified by the Psychiatric Genomics Consortium as being associated with the 108 SZ-associated genetic loci.30 The 348 unique genes listed in the paper’s 'Supplementary Table 3: Bioinformatic summary data for 108 genome-wide significant loci' were used to identify the 727 corresponding Affymetrix Human Genome U133 Plus 2.0 probe set IDs using Biomart (www.ensembl.org/biomart). A hypergeometric distribution was used to calculate whether the number of overlapping probe sets was beyond chance levels.
Correlation analysis of neuropsychology test scores and OE molecular expression
In order to identify genes that may be associated with deficits in cognitive function in SZ, we filtered the differentially expressed genes in OE based on their correlation with neuropsychology test scores (the six-factor scores and composite score) from the SZ patients. The analysis was limited to SZ patients as we were interested in genes that specifically correlate with cognitive function in the disease state rather than cognition in general. The scores from SZ patients were normalized as Z-scores with adjustment for sex and years of education. Briefly, each raw score was regressed against sex and years of education in a linear model, yielding the expected score taking sex and years of education into consideration. The residual value was calculated using the expected score (residual value=actual score−expected score). The mean and the standard deviation (s.d.) of the residual values were used for calculating Z-scores [Z=(residual value−mean residual value)/s.d.]. Spearman’s rank correlation analysis was performed to examine the relationship between differentially expressed genes and neuropsychology test Z-scores. P-values for the correlation tests were computed by permutation testing (N=1 000 000). R (http://www.r-project.org/, version 3.1.1) was used for correlation analysis.
Real-time quantitative PCR data analysis
To validate the microarray data, gene expression was quantified using real-time quantitative polymerase chain reaction (qPCR) with a TaqMan Gene Expression Assay and ABI PRISM 7900HT Sequence Detection System (Applied Biosystems, Foster City, CA, USA) as per the manufacturer’s instructions. Primers and probes were purchased from Life Technology (Carlsbad, CA, USA) [assay ID: SMAD1, Hs00195432_m1; SMAD3, Hs00706299_s1; SMAD5, Hs00289739_s1; SMAD specific E3 ubiquitin protein ligase 1 (SMURF1), Hs00410929_m1]. Human glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as an internal control, and measurement of the threshold cycle (Ct) was performed in triplicate. Data were collected and analyzed with the Sequence Detector Software version 2.2 (Applied Biosystems) and the standard curve method. Relative gene expression was calculated as the ratio of the genes to the internal control (GAPDH). Outliers were determined as any data point more than 1.5 interquartile ranges below the first quartile or above the third quartile.
Linear regression analysis
For evaluating the effects of antipsychotic medication on gene expression profiles, we converted daily doses of antipsychotics at the time of the biopsy to chlorpromazine equivalents.31 Then, we conducted linear regression analysis for gene expression levels detected by qPCR using the chlorpromazine equivalents as a covariate. Linear regression was also used to evaluate the effect of smoking (using the number of packs of cigarettes smoked per day as an independent variable) on gene expression levels in the qPCR experiments, and on the neuropsychological assessment scores.
Results
To investigate which genes or gene groups in neuronal cells are related to cognitive function in SZ, we designed the present study as follows (scheme shown in Figure 1).
Study design. Microarray analysis using olfactory epithelium (OE) tissue and neuropsychological assessments were conducted in the same participants. Following differential gene expression analysis (false discovery rate (FDR) <0.05), correlation of gene expression with neuropsychological test scores was used as a filter to select candidate genes for validation with quantitative real-time PCR (qPCR). To determine whether genes identified using OE would also be significantly different in lymphoblasts (LBs), we conducted microarray differential gene expression analysis in 'paired' and 'non-paired' samples.
The demographics of the participants and clinical assessment
Sixteen patients with chronic SZ and fifteen normal control subjects participated in the neuropsychological testing and OE biopsy. Their demographic data and neuropsychological scores are shown in Table 1. The participants were matched for age (SZ, 39.8±11.3 years; control, 41.8±10.8 years; P=0.60), sex (SZ, 12 males and 4 females; control, 11 males and 4 females; P=0.77) and race (SZ, 6 Caucasian and 10 African-American; control, 6 Caucasian and 9 African-American; P=0.92). Years of education (SZ, 12.0±2.6; control, 13.4±2.6; P=0.16) and current smoking status (SZ, 9 yes and 7 no; control, 3 yes and 12 no; P=0.07) did not differ significantly. The cognitive assessments consist of six domains and the composite score. Among the six domains, there was a significant difference in performance across neurocognitive tests, with patients’ performance being worse than healthy controls for processing speed, attention/working memory and ideational fluency (P=0.02, 0.04 and 0.004, respectively). The composite score was also significantly lower in patients (P=0.03). These differences remained significant even after adjusting for smoking status by linear regression analysis (data not shown). Patients underwent the Scales for the Assessment of Negative and Positive Symptom tests, with the mean scores being 6.6±4.1 and 3.8±3.6, respectively.
Gene expression changes in SZ from LCM-enriched neural layers of OE
Following LCM, relative expression levels of the neuronal marker olfactory marker protein (OMP) were analyzed in a subset of control samples to confirm consistency of enrichment with previous studies (Supplementary Figure 1). Microarray analysis was performed on microdissected tissue from the same subjects who underwent the neuropsychological assessments. We identified 2574 transcripts that were differently expressed between SZ and control in olfactory neuronal tissues enriched by LCM FDR <0.05. The differentially expressed gene list, ordered by fold change, is available as Supplementary Table 1.
As validation of the OE microarray data, we examined the co-regulated genes in the OE tissues by comparing with those in the publicly available co-regulation networks consisting of 1645 gene–gene correlations (that is, co-regulations; |Pearson’s coefficient|⩾0.75) within a large set of human cell lines (immortalized B cells from 295 normal individuals).29 The co-regulated genes of the OE tissues, which were defined as above, were significantly over-represented in the co-regulation networks (82/1645=4.98%, P=2.92 × 10−41; calculated by using hypergeometric distribution), suggesting that co-regulation patterns of the OE microarray data are shared, at least in part, with those within the human cell lines. In addition, we examined the relationship of the differentially expressed genes in the OE tissues with the co-regulation networks and found that few of the differential gene pairs exist on the co-regulation networks (3/1645<1%; P≈1.00).
Forty-eight genes were overlapped between the probe sets associated with the 108 SZ-associated genetic loci30 and our 2574 differentially expressed OE transcripts (48/727=6.6%, P=0.0148; calculated by using hypergeometric distribution; Supplementary Table 1). None of the 17 genes correlated with neuropsychological test scores (described below) were represented in the overlap.
Correlation between neuropsychological domain scores and gene expression
In order to narrow down from the 2574 differentially expressed genes (FDR<0.05) to those that may be specifically associated with cognitive function in SZ patients, we calculated Spearman’s rank correlations between genes and patient neuropsychology test scores (composite and factor scores for individual domains). For this filtering method we used a cutoff of P<0.01, which narrowed our list of candidate genes to 17 (Table 2). As scores for the composite, processing speed, attention/working memory and ideational fluency domains were significantly lower in SZ patients compared with control, we focused on the genes that correlated with these four domains (SMAD5, PABPC4L, RBM28, RAB4A, ERO1LB, CCL11, CD69, LINC01004, COA3, CBFA2T2). Two genes, SMAD family member 5 (SMAD5) and poly(A) binding protein, cytoplasmic 4-like (PABPC4L), positively correlated with the composite score, which is the most representative of the neuropsychological assessment scores. SMAD5 was also positively correlated with the processing speed score. Although its function is not well understood, a rare copy number variation in the PABPC4L gene was found in a treatment-resistant depression cohort in a recent study.32
qPCR validation in OE and cross-validation in LB microarray
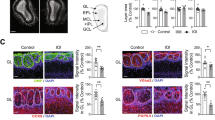
As the SMAD5 gene is located at chromosome 5q31.1, a suggested risk locus for SZ,33, 34 and has a role in neurodevelopment,35 we further explored expression of molecules in the SMAD pathway. The OE microarray demonstrated a downregulation of representative molecules from the SMAD pathway, such as SMAD1, SMAD5 (both FDR<0.05), SMAD3 and SMURF1, in SZ patients compared with controls. qPCR confirmed that SMAD1, SMAD3 and SMAD5 were differentially expressed in OE (P<0.05; Figure 2).
Gene expression level of SMAD pathway-related genes in the olfactory epithelium (OE) neuronal layer. The mRNA expression level of SMAD pathway-related genes using quantitative real-time polymerase chain reaction (qPCR). The qPCR analysis confirmed downregulation of SMAD1, SMAD3 and SMAD5 in schizophrenia (SZ). Expression levels were normalized to glyceraldehyde-3-phosphate dehydrogenase (GAPDH) expression. Results are shown as mean±s.e.m. Statistical analysis was conducted with Welch's t-test. *P<0.05.
Exposure to tobacco smoke has been shown to change the binding activity of transcription factors, including SMAD3/4, in human lung cells.36 As olfactory epithelia, like lung tissue, would be directly exposed to cigarette smoke, the SMAD pathway in olfactory epithelia might be affected by cigarette smoke. To evaluate the relationship between SMAD gene expression and smoking, we conducted linear regression analysis involving SMAD gene expression (qPCR) as a dependent variable and the number of packs of cigarettes smoked per day as an independent variable. None of the SMAD genes showed a significant relationship with the number of packs smoked (P>0.05; data not shown).
We next asked whether OE neuronal tissues might have unique advantages as brain surrogates. Thus, we examined gene expression in blood cells from the same subjects to determine whether the same molecular signature (for example, downregulation of SMAD5) was also observed in peripheral cells. As described in the Materials and methods section, we used both 'paired' and 'non-paired' LBs. Strikingly, none of the 17 genes identified in OE tissue using the combined strategy of FDR cutoff and correlation with neuropsychology test scores were differentially expressed at FDR<0.05 between patients and controls in either the 'paired' or 'non-paired' LB data sets (Table 3). This result suggests that there is little overlap in the differential gene expression characteristics of OE and LB cells, supporting the utility of OE samples over peripheral cell samples in the analysis of brain-related changes.
Discussion
This study aimed to develop a unique strategy for identifying neuronal changes associated with cognitive impairment in SZ at the molecular level. Cognitive deficits in SZ are intrinsic to the disorder, rather than being medication-induced. A meta-analysis of cognitive performance in antipsychotic-naive SZ patients has revealed impairments in processing speed and working memory.37 Furthermore, our research design, obtaining neuronal information from living patients, allows us to longitudinally track changes in gene expression that may be associated with changes in cognitive function, which is not possible using post-mortem brain tissue. We propose that the SMAD pathway may be an important target in studying cognitive deficits in SZ.
SMAD proteins are intracellular mediators in the bone morphogenic protein and transforming growth factor-beta (TGF-β) signaling pathways and are important in regulating neurodevelopment; SMAD2 and 3 are downstream of TGF-β receptors, whereas SMAD1, 5 and 8 are primarily substrates for the bone morphogenic protein receptors.38, 39 Dysregulation of SMAD genes reportedly affect oligodendrogenesis,40 axon development and regeneration,40 growth and maintenance of midbrain dopaminergic neurons,41 as well as differentiation, maintenance and protection of basal forebrain cholinergic neurons.42, 43, 44, 45, 46, 47 Cholinergic neurons are thought to influence diverse cognitive tasks including attention, learning and memory. There is growing evidence for the dysfunction of cholinergic systems in SZ and related disorders.48, 49 The SMADs are also critical for bone formation and intriguingly, bone function may be important for stability of brain function; in addition to being a structural organ, the bone functions as an endocrine organ by secreting osteocalcin, which has been suggested to have a direct role in memory and mood.50, 51 There have been several reports that include an alteration in the molecular cascade in various mental conditions,34, 52, 53, 54, 55 and the present study defines its implication in the cognition associated with SZ.
There is precedence for applying a multifaceted approach to explore biomarkers for mental illnesses. For example, the convergent functional genomics approach aims to increase the sensitivity and specificity of biomarkers by integrating data from animal models, genetics, gene expression studies in post-mortem brain and blood samples.56, 57, 58, 59, 60, 61 We feel that our approach of combining expression data from different human cell types, and filtering them based on correlation with a behavioral trait of interest, is complementary to the convergent functional genomics approach, and may be particularly informative in a translational psychiatry setting.
This exploratory study has some limitations. Although the two groups (SZ and control) are matched by age, race, sex, years of education and smoking status, we cannot exclude differences due to other confounding factors, such as the effects of long-term medication and diet. Note, as far as daily dose of antipsychotic medication at the time of biopsy is used as a covariate, linear regression analysis indicates that antipsychotic medication had no significant effect on gene expression levels (Supplementary Table 2). However, future studies with medication-naive patients would be informative. Although the current data suggest the SMAD pathway as a novel target in studying cognitive deficits in SZ, we fully acknowledge that the sample size of the present study is relatively small. Further studies with larger sample sizes are warranted.
Our unique approach of combining the analysis of two observations from the same subjects, microarray from LCM-processed OE neuronal tissues and neuropsychological assessment, allowed us to identify potentially important new gene associations. Of note, our results showed that the neuronal OE tissues provide unique molecular information that could not be obtained from blood cells (immortalized LBs) in the present data set, including the molecules of the SMAD pathway (Table 3). This failure is partly because the process for immortalization leads to the loss of state information in the fresh blood. It is also possible that blood studies may need larger sample size. However, this does not diminish the significance and utility of blood cells in molecular profiling in mental disorders: indeed, there is successful precedence in using blood cells for the profiling.53, 54, 55, 56, 57, 58, 59, 60, 61 At least within the present study, we can say that the neuronal OE tissues may be good for academic purposes and understanding the biology of illness, whereas the blood, in particular fresh blood, is advantageous for repeated routine monitoring and clinical practice. Thus, although negative in LBs, it may be an important future effort to study the SMAD pathway in the fresh whole blood together with neurocognition.
The present experimental strategy with OE neuronal tissues may be useful in translational psychiatry, particularly in studies that look for molecular signatures that reflect the 'state' at the time of biopsy. Although recent advances in stem cell biology, such as induced pluripotent stem cells, have given us the ability to generate neurons and glia from patients, these cells can capture only 'trait' changes.12, 62, 63 An ongoing challenge in translational psychiatry is to capture treatment-associated 'state' alterations in neuronal molecular markers that correlate with specific features in mental illness. For example, it is very important to understand molecular mechanisms underlying treatment response, or resistance to lithium, or neuroleptics. Although such application is beyond the scope of this study, our experimental strategy can be used to address this question—conducting biopsies before and after the treatment and comparing molecular and clinical changes in response to the treatment at the level of the individual.
Additionally with the maturation of next-generation sequencing technologies, it is becoming easier to obtain reliable transcriptomic data from small amounts of starting material. Beyond studies for treatment response to current medications, we anticipate that this experimental system can also be effectively utilized to identify new drug targets by connecting molecular/biological effects and clinical outcomes. The utility of this system will be further improved by the development of a platform for protein assays in future studies.
Accession codes
References
Maj M . Report on the implementation of the WPA Action Plan 2008-2011. World Psychiatry 2011; 10: 161–164.
Keefe RS, Eesley CE, Poe MP . Defining a cognitive function decrement in schizophrenia. Biol Psychiatry 2005; 57: 688–691.
Sponheim SR, Jung RE, Seidman LJ, Mesholam-Gately RI, Manoach DS, O'Leary DS et al. Cognitive deficits in recent-onset and chronic schizophrenia. J Psychiatr Res 2010; 44: 421–428.
Tamminga CA, Buchanan RW, Gold JM . The role of negative symptoms and cognitive dysfunction in schizophrenia outcome. Int Clin Psychopharmacol 1998; 13 (Suppl 3): S21–S26.
Gamo NJ, Sawa A . Human stem cells and surrogate tissues for basic and translational study of mental disorders. Biol Psychiatry 2014; 75: 918–919.
Brennand KJ, Simone A, Tran N, Gage FH . Modeling psychiatric disorders at the cellular and network levels. Mol Psychiatry 2012; 17: 1239–1253.
Wilson AM, Sawa A. Human cell models for schizophrenia. In: Silverstein SM, Moghaddam B, Wykes T (eds). Schizophrenia: Evolution and Synthesis. The MIT Press: Cambridge, MA, USA, 2013, pp 167–182.
Horiuchi Y, Kano S, Ishizuka K, Cascella NG, Ishii S, Talbot CC Jr et al. Olfactory cells via nasal biopsy reflect the developing brain in gene expression profiles: utility and limitation of the surrogate tissues in research for brain disorders. Neurosci Res 2013; 77: 247–250.
Cascella NG, Takaki M, Lin S, Sawa A . Neurodevelopmental involvement in schizophrenia: the olfactory epithelium as an alternative model for research. J Neurochem 2007; 102: 587–594.
Mackay-Sim A, Feron F, Cochrane J, Bassingthwaighte L, Bayliss C, Davies W et al. Autologous olfactory ensheathing cell transplantation in human paraplegia: a 3-year clinical trial. Brain 2008; 131: 2376–2386.
Borgmann-Winter K, Willard SL, Sinclair D, Mirza N, Turetsky B, Berretta S et al. Translational potential of olfactory mucosa for the study of neuropsychiatric illness. Transl Psychiatry 2015; 5: e527.
Narayan S, McLean C, Sawa A, Lin SY, Rai N, Hipolito MS et al. Olfactory neurons obtained through nasal biopsy combined with laser-capturemicrodissection: a potential approach to study treatment response in mental disorders. J Vis Exp 2014.
Tajinda K, Ishizuka K, Colantuoni C, Morita M, Winicki J, Le C et al. Neuronal biomarkers from patients with mental illnesses: a novel method through nasal biopsy combined with laser-captured microdissection. Mol Psychiatry 2010; 15: 231–232.
Kano S, Colantuoni C, Han F, Zhou Z, Yuan Q, Wilson A et al. Genome-wide profiling of multiple histone methylations in olfactory cells: further implications for cellular susceptibility to oxidative stress in schizophrenia. Mol Psychiatry 2013; 18: 740–742.
Cieslak K, Walsh-Messinger J, Stanford A, Vaez-Azizi L, Antonius D, Harkavy-Friedman J et al. Olfactory performance segregates effects of anhedonia and anxiety on social function in patients with schizophrenia. J Psychiatry Neurosci 2015; 40: 387–393.
Ishizuka K, Tajinda K, Colantuoni C, Morita M, Winicki J, Le C et al. Negative symptoms of schizophrenia correlate with impairment on the University of Pennsylvania smell identification test. Neurosci Res 2010; 66: 106–110.
Kastner A, Malzahn D, Begemann M, Hilmes C, Bickeboller H, Ehrenreich H . Odor naming and interpretation performance in 881 schizophrenia subjects: association with clinical parameters. BMC Psychiatry 2013; 13: 218.
Leung CT, Coulombe PA, Reed RR . Contribution of olfactory neural stem cells to tissue maintenance and regeneration. Nat Neurosci 2007; 10: 720–726.
Schwob JE . Neural regeneration and the peripheral olfactory system. Anat Rec 2002; 269: 33–49.
American Psychiatric Association, American Psychiatric Association Task Force on DSM-IV. Diagnostic and Statistical Manual of Mental Disorders: DSM-IV. 4th edn, American Psychiatric Association: Washington, DC, USA, 1994 xxvii, 886p.
First MB, Spitzer RL, Gibbon M, Williams JBW . Structured Clinical Interview for DSM-IV Axis I Disorders - Clinical Version (SCID-CV). American Psychiatric Press: Washington, DC, USA, 1997.
Andreasen NC, Olsen S . Negative v positive schizophrenia. Definition and validation. Arch Gen Psychiatry 1982; 39: 789–794.
Schretlen DJ, Cascella NG, Meyer SM, Kingery LR, Testa SM, Munro CA et al. Neuropsychological functioning in bipolar disorder and schizophrenia. Biol Psychiatry 2007; 62: 179–186.
Schretlen DJ, Pena J, Aretouli E, Orue I, Cascella NG, Pearlson GD et al. Confirmatory factor analysis reveals a latent cognitive structure common to bipolar disorder, schizophrenia, and normal controls. Bipolar Disord 2013; 15: 422–433.
Nuechterlein KH, Barch DM, Gold JM, Goldberg TE, Green MF, Heaton RK . Identification of separable cognitive factors in schizophrenia. Schizophr Res 2004; 72: 29–39.
Sawa A, Wiegand GW, Cooper J, Margolis RL, Sharp AH, Lawler JF Jr et al. Increased apoptosis of Huntington disease lymphoblasts associated with repeat length-dependent mitochondrial depolarization. Nat Med 1999; 5: 1194–1198.
Benjamini Y, Hochberg Y . Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Series B Stat Methodol 1995; 57: 289–300.
Toritsuka M, Kimoto S, Muraki K, Landek-Salgado MA, Yoshida A, Yamamoto N et al. Deficits in microRNA-mediated Cxcr4/Cxcl12 signaling in neurodevelopmental deficits in a 22q11 deletion syndrome mouse model. Proc Natl Acad Sci USA 2013; 110: 17552–17557.
Nayak RR, Kearns M, Spielman RS, Cheung VG . Coexpression network based on natural variation in human gene expression reveals gene interactions and functions. Genome Res 2009; 19: 1953–1962.
Schizophrenia Working Group of the Psychiatric Genomics C. Biological insights from 108 schizophrenia-associated genetic loci. Nature 2014; 511: 421–427.
Andreasen NC, Pressler M, Nopoulos P, Miller D, Ho BC . Antipsychotic dose equivalents and dose-years: a standardized method for comparing exposure to different drugs. Biol Psychiatry 2010; 67: 255–262.
O'Dushlaine C, Ripke S, Ruderfer DM, Hamilton SP, Fava M, Iosifescu DV et al. Rare copy number variation in treatment-resistant major depressive disorder. Biol Psychiatry 2014; 76: 536–541.
Sklar P, Pato MT, Kirby A, Petryshen TL, Medeiros H, Carvalho C et al. Genome-wide scan in Portuguese Island families identifies 5q31-5q35 as a susceptibility locus for schizophrenia and psychosis. Mol Psychiatry 2004; 9: 213–218.
Zaharieva I, Georgieva L, Nikolov I, Kirov G, Owen MJ, O'Donovan MC et al. Association study in the 5q31-32 linkage region for schizophrenia using pooled DNA genotyping. BMC Psychiatry 2008; 8: 11.
Rios I, Alvarez-Rodriguez R, Marti E, Pons S . Bmp2 antagonizes sonic hedgehog-mediated proliferation of cerebellar granule neurones through Smad5 signalling. Development 2004; 131: 3159–3168.
Zhao J, Harper R, Barchowsky A, Di YP . Identification of multiple MAPK-mediated transcription factors regulated by tobacco smoke in airway epithelial cells. Am J Physiol Lung Cell Mol Physiol 2007; 293: L480–L490.
Fatouros-Bergman H, Cervenka S, Flyckt L, Edman G, Farde L . Meta-analysis of cognitive performance in drug-naive patients with schizophrenia. Schizophr Res 2014; 158: 156–162.
Derynck R, Zhang YE . Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature 2003; 425: 577–584.
Massague J, Seoane J, Wotton D . Smad transcription factors. Genes Dev 2005; 19: 2783–2810.
Nicolay DJ, Doucette JR, Nazarali AJ . Transcriptional control of oligodendrogenesis. Glia 2007; 55: 1287–1299.
Hegarty SV, Collins LM, Gavin AM, Roche SL, Wyatt SL, Sullivan AM et al. Canonical BMP-Smad signalling promotes neurite growth in rat midbrain dopaminergic neurons. Neuromolecular Med 2014; 16: 473–489.
Lopez-Coviella I, Berse B, Krauss R, Thies RS, Blusztajn JK . Induction and maintenance of the neuronal cholinergic phenotype in the central nervous system by BMP-9. Science 2000; 289: 313–316.
Lopez-Coviella I, Mellott TJ, Schnitzler AC, Blusztajn JK . BMP9 protects septal neurons from axotomy-evoked loss of cholinergic phenotype. PLoS One 2011; 6: e21166.
Lopez-Coviella I, Mellott TM, Kovacheva VP, Berse B, Slack BE, Zemelko V et al. Developmental pattern of expression of BMP receptors and Smads and activation of Smad1 and Smad5 by BMP9 in mouse basal forebrain. Brain Res 2006; 1088: 49–56.
Nonner D, Barrett EF, Kaplan P, Barrett JN . Bone morphogenetic proteins (BMP6 and BMP7) enhance the protective effect of neurotrophins on cultured septal cholinergic neurons during hypoglycemia. J Neurochem 2001; 77: 691–699.
Nonner D, Panickar K, Barrett EF, Barrett JN . Bone morphogenetic proteins and neurotrophins provide complementary protection of septal cholinergic function during phosphatase inhibitor-induced stress. J Neurochem 2004; 91: 77–87.
Schnitzler AC, Mellott TJ, Lopez-Coviella I, Tallini YN, Kotlikoff MI, Follettie MT et al. BMP9 (bone morphogenetic protein 9) induces NGF as an autocrine/paracrine cholinergic trophic factor in developing basal forebrain neurons. J Neurosci 2010; 30: 8221–8228.
Dean B, Scarr E . Possible involvement of muscarinic receptors in psychiatric disorders: a focus on schizophrenia and mood disorders. Curr Mol Med 2015; 15: 253–264.
Higley MJ, Picciotto MR . Neuromodulation by acetylcholine: examples from schizophrenia and depression. Curr Opin Neurobiol 2014; 29: 88–95.
Karsenty G, Ferron M . The contribution of bone to whole-organism physiology. Nature 2012; 481: 314–320.
Oury F, Khrimian L, Denny CA, Gardin A, Chamouni A, Goeden N et al. Maternal and offspring pools of osteocalcin influence brain development and functions. Cell 2013; 155: 228–241.
Toyooka K, Usui M, Washiyama K, Kumanishi T, Takahashi Y . Gene expression profiles in the brain from phencyclidine-treated mouse by using DNA microarray. Ann N Y Acad Sci 2002; 965: 10–20.
Beech RD, Lowthert L, Leffert JJ, Mason PN, Taylor MM, Umlauf S et al. Increased peripheral blood expression of electron transport chain genes in bipolar depression. Bipolar Disord 2010; 12: 813–824.
Beech RD, Qu J, Leffert JJ, Lin A, Hong KA, Hansen J et al. Altered expression of cytokine signaling pathway genes in peripheral blood cells of alcohol dependent subjects: preliminary findings. Alcohol Clin Exp Res 2012; 36: 1487–1496.
Levey DF, Niculescu EM, Le-Niculescu H, Dainton HL, Phalen PL, Ladd TB et al. Towards understanding and predicting suicidality in women: biomarkers and clinical risk assessment. Mol Psychiatry 2016; 21: 768–785.
Le-Niculescu H, Levey DF, Ayalew M, Palmer L, Gavrin LM, Jain N et al. Discovery and validation of blood biomarkers for suicidality. Mol Psychiatry 2013; 18: 1249–1264.
Levey DF, Le-Niculescu H, Frank J, Ayalew M, Jain N, Kirlin B et al. Genetic risk prediction and neurobiological understanding of alcoholism. Transl Psychiatry 2014; 4: e391.
Ayalew M, Le-Niculescu H, Levey DF, Jain N, Changala B, Patel SD et al. Convergent functional genomics of schizophrenia: from comprehensive understanding to genetic risk prediction. Mol Psychiatry 2012; 17: 887–905.
Le-Niculescu H, Balaraman Y, Patel SD, Ayalew M, Gupta J, Kuczenski R et al. Convergent functional genomics of anxiety disorders: translational identification of genes, biomarkers, pathways and mechanisms. Transl Psychiatry 2011; 1: e9.
Kurian SM, Le-Niculescu H, Patel SD, Bertram D, Davis J, Dike C et al. Identification of blood biomarkers for psychosis using convergent functional genomics. Mol Psychiatry 2011; 16: 37–58.
Niculescu AB, Le-Niculescu H . Convergent functional genomics: what we have learned and can learn about genes, pathways, and mechanisms. Neuropsychopharmacology 2010; 35: 355–356.
Brennand KJ, Landek-Salgado MA, Sawa A . Modeling heterogeneous patients with a clinical diagnosis of schizophrenia with induced pluripotent stem cells. Biol Psychiatry 2014; 75: 936–944.
Merkle FT, Eggan K . Modeling human disease with pluripotent stem cells: from genome association to function. Cell Stem Cell 2013; 12: 656–668.
Acknowledgements
We thank Dr Nao J Gamo for critical reading of the manuscript. This work was supported by the National Institute of Mental Health MH-084018, MH-094268 Silvio O Conte center, MH-069853 (AS), MH-085226 (AS), MH-088753 (AS), MH-092443 (AS), MH-105660 (AS and KI), as well as foundation grants from Stanley (AS), S-R (AS), RUSK (AS), NARSAD (KI and AS), and Maryland Stem Cell Research Fund (KI, AS and YH). Funding from Astellas Pharm was also used for the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Translational Psychiatry website
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Horiuchi, Y., Kondo, M., Okada, K. et al. Molecular signatures associated with cognitive deficits in schizophrenia: a study of biopsied olfactory neural epithelium. Transl Psychiatry 6, e915 (2016). https://doi.org/10.1038/tp.2016.154
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2016.154
- Springer Nature Limited
This article is cited by
-
RNAseq analysis of olfactory neuroepithelium cytological samples in individuals with Down syndrome compared to euploid controls: a pilot study
Neurological Sciences (2023)
-
Sex-specific involvement of the Notch–JAG pathway in social recognition
Translational Psychiatry (2022)
-
Expression Analysis of Ermin and Listerin E3 Ubiquitin Protein Ligase 1 Genes in the Periphery of Patients with Schizophrenia
Journal of Molecular Neuroscience (2022)
-
Transcriptional profile of pyramidal neurons in chronic schizophrenia reveals lamina-specific dysfunction of neuronal immunity
Molecular Psychiatry (2021)
-
Olfactory deficits in individuals at risk for psychosis and patients with schizophrenia: relationship with socio-cognitive functions and symptom severity
European Archives of Psychiatry and Clinical Neuroscience (2018)