Abstract
The present study was performed to explore the role of galanin and galanin receptor 2 in nociceptive modulation in anterior cingulate cortex (ACC) of normal rats and rats with mononeuropathy. Intra-ACC injection of galanin induced significant increases in hindpaw withdrawal latencies (HWLs) to thermal and mechanical stimulations in both normal rats and rats with mononeuropathy, the increased HWLs were attenuated significantly by intra-ACC injection of galanin receptor 2 antagonist M871, indicating an involvement of galanin receptor 2 in nociceptive modulation in ACC. Interestingly, the galanin-induced HWL was significant higher in rats with mononeuropathy than that in normal rats tested by Randall Selitto test. Furthermore, both the galanin mRNA expression and galanin content increased significantly in ACC in rats with mononeuropathy than that in normal rats. Moreover, both the mRNA levels of galanin receptor 2 and the content of galanin receptor 2 in ACC increased significantly in rats with mononeuropathy than that in normal rats. These results found that galanin induced antinociception in ACC in both normal rats and rats with mononeuropathy. And there may be plastic changes in the expression of galanin and galanin receptor 2 in rats with mononeuropathy, as well as in the galanin-induced antinociception.
Similar content being viewed by others
Introduction
The neuropeptide galanin, with 29 amino acids (30 in humans), is firstly isolated from porcine intestine1. It is well known that galanin is widely distributed in the central nervous system and peripheral nervous system2. There are three subtypes of galanin receptor (Gal R1, Gal R2 and Gal R3) and they belong to the family of G-protein coupled receptors3,4,5. Many studies have reported that galanin and its receptors are involved in many physiological functions and pathological processions4,6,7,8. Previous studies have demonstrated that galanin and galanin receptors play important roles in the transmission and/or modulation of nociception of the central nervous system, at spinal cord levels7,9, as well as in the brain, such as hypothalamic arcuate nucleus, nucleus accumbens, periaqueductal grey, and the central nucleus of amygdala10,11,12,13,14,15,16,17,18,19. Wang and her colleagues demonstrated that administration of galanin into periaqueductal grey induced significant antinociceptive effects in intact rats and rats with mononeuropathy16,20. Jin et al. reported that galanin induced antinociceptive effects in the central nucleus of amygdala of rats, and opioid receptors were involved in the galanin-induced antinociception14. Sun and his colleagues reported that intra-arcuate nucleus of hypothalamus administration of galanin induced significant antinociceptive effects in rats15. Recently, many studies have demonstrated that galanin receptor 2 (Gal R2) is involved in the modulation of neuropathic pain in the central nervous system19,21,22,23.
The anterior cingulate cortex (ACC) is one of the important structures of the brain24,25,26. Recently, many studies demonstrated that ACC is involved in the nociceptive modulation in the brain25,26,27,28,29,30,31,32. Neuropathic pain is one of common clinic pain13,16,33. Recently, many studies demonstrated that ACC is involved in the persistent neuropathic pain25,28,31. Activation of the ACC is associated with reduced pain behavior produced by unilateral spinal nerve injury in rats34. Study from Zhuo’s laboratory found that protein kinase M zeta (PKMζ) maintains pain-induced persistent changes in the mouse ACC, and microinjection of the selective PKMζ inhibitor into ACC blocked behavioral sensitization in mouse with peripheral nerve injury28.
The present study was performed to explore the role of galanin in nociceptive modulation in ACC of normal rats and rats with mononeuropathy, and further to explore the plastic changes in the expression of galanin and galanin receptor 2 in ACC in rats with mononeuropathy.
Results
Antinociceptive effects induced by intra-ACC administration of galanin in normal rats
To determine the influence of galanin on nociceptive modulation in ACC of normal rats, five groups of rats received intra-ACC injection of 0.1 (n = 7), 0.5 (n = 8), 1 (n = 9) or 2 nmol (n = 8) of galanin, or 1 μl of 0.9% saline as a control (n = 10). The results are shown in Fig. 1.
As shown in Fig. 1, the hindpaw withdrawal latencies (HWLs) to thermal and mechanical stimulations increased significantly in a dose-dependent manner after intra-ACC injection of 0.1 nmol of galanin (Hot-plate Test: Fleft/left = 84.27, P < 0.001; Fright/right = 98.05, P < 0.001; Randall Selitto Test: Fleft/left = 193.10, P < 0.001; Fright/right = 57.21, P < 0.001), 0.5 nmol of galanin (Hot-plate Test: Fleft/left = 797.30, P < 0.001; Fright/right = 834.90, P < 0.001; Randall Selitto Test: Fleft/left = 84.59, P < 0.001; Fright/right = 60.43, P < 0.001), 1 nmol of galanin (Hot-plate Test: Fleft/left = 414.10, P < 0.001; Fright/right = 394.90, P < 0.001; Randall Selitto Test: Fleft/left = 387.20, P < 0.001; Fright/right = 179.40, P < 0.001) and 2 nmol of galanin (Hot-plate Test: Fleft/left = 915.90, P < 0.001; Fright/right = 582.30, P < 0.001; Randall Selitto Test: Fleft/left = 418.60, P < 0.001; Fright/right = 684.20, P < 0.001) compared with the control group. The results demonstrated that intra-ACC injection of galanin induced significant antinociceptive effects in normal rats.
At the end of the experiments, the location of the tip of the injection needle was verified and the injection points are shown in Fig. 1E. Only the results obtained from nociceptive tests that the tips of the injection needle are within the ACC are used for statistical analysis.
Influences of intra-ACC injection of the galanin receptor 2 antagonist M871 on the galanin-induced antinociception in normal rats
To determine the involvement of galanin receptor 2 in galanin-induced antinociception in ACC of normal rats, four groups of rats received intra-ACC injection of 1 nmol of galanin, followed 5 min later by intra-ACC injection of 0.1 (n = 9), 0.5 (n = 9) or 1 nmol (n = 8) of the selective galanin receptor 2 antagonist M871, or 1 μl of 0.9% saline as a control (n = 7).
As shown in Fig. 2, compared with the control group, there were no significant influences on galanin-induced increases in HWLs after intra-ACC injection of 0.1 nmol of M871 (Hot-plate Test: Dunnett test, P = 0.13; Dunnett test, P = 0.85; Randall Selitto Test: Dunnett test, P = 0.41; Dunnett test, P = 0.99. One-way ANOVA, followed Dunnett multiple comparison test). The galanin-induced increases in HWLs were significantly attenuated after intra-ACC injection of 0.5 nmol of M871 (Hot-plate Test: Dunnett test, P < 0.001; Dunnett test, P < 0.001; Randall Selitto Test: Dunnett test, P < 0.001; Dunnett test, P < 0.001) and 1 nmol of M871 (Hot-plate Test: Dunnett test, P < 0.001; Dunnett test, P < 0.001; Randall Selitto Test: Dunnett test, P < 0.001; Dunnett test, P < 0.001) compared with the control group.
Another group of rats (n = 7) received intra-ACC injection of 1 μl of 0.9% saline, followed 5 min later by intra-ACC injection of 1 nmol of M871. The results demonstrated that there are no marked influences on the HWLs to thermal and mechanical stimulation after intra-ACC administration of the selective galanin receptor 2 antagonist M871, as shown in Fig. 2. These results indicate that galanin receptor 2 is involved in the galanin-induced antinociception in the ACC of normal rats.
Antinociceptive effects induced by intra-ACC administration of galanin in rats with mononeuropathy
In order to determine the influence of galanin on neuropathic pain, four groups of rats with sciatic nerve ligation received intra-ACC injection of 0.1 (n = 8), 0.5 (n = 8), or 1 nmol (n = 8) of galanin, or 1 μl of 0.9% saline as a control (n = 8), the results are shown in Fig. 3.
There were no significant increases in the HWLs to thermal and mechanical stimulations after intra-ACC injection of 0.1 nmol of galanin (Hot-plate Test: Fleft/left = 4.32, P = 0.06; Fright/right = 2.54, P = 0.13; Randall Selitto Test: Fleft/left = 0.08, P = 0.77; Fright/right = 3.21, P = 0.10) compared with control group in rats with mononeuropathy. The HWLs to thermal and mechanical stimulations increased significantly after intra-ACC injection of 0.5 nmol of galanin (Hot-plate Test: Fleft/left = 162.50, P < 0.001; Fright/right = 286.00, P < 0.001; Randall Selitto Test: Fleft/left = 85.52, P < 0.001; Fright/right = 161.90, P < 0.001), or 1 nmol of galanin (Hot-plate Test: Fleft/left = 410.80, P < 0.001; Fright/right = 292.60, P < 0.001; Randall Selitto Test: Fleft/left = 176.30, P < 0.001; Fright/right = 226.40, P < 0.001) compared with the control group in rats with mononeuropathy. The results demonstrated that intra-ACC injection of galanin induced significant antinociceptive effects in rats with mononeuropathy.
Influences of intra-ACC injection of the galanin receptor 2 antagonist M871 on the galanin-induced antinociception in rats with mononeuropathy
Two groups of rats with mononeuropathy received intra-ACC injection of 1 nmol of galanin, followed 5 min later by intra-ACC injection of 1 nmol (n = 8) of the selective galanin receptor 2 antagonist M871, or 1 μl of 0.9% saline as a control (n = 7), the results are shown in Fig. 4.
After intra-ACC injection of 1 nmol of galanin, the HWL of rats with mononeuropathy increased markedly. The galanin-induced increases in HWLs were significantly attenuated after intra-ACC injection of 1 nmol of M871 (Hot-plate Test: tleft/left = 5.69, P < 0.001; tright/right = 7.92, P < 0.001; Randall Selitto Test: tleft/left = 8.98, P < 0.001; tright/right = 10.31, P < 0.001) compared with the control group.
Another group of rats with mononeuropathy (n = 8) received intra-ACC injection of 1 μl of 0.9% saline, followed 5 min later by intra-ACC injection of 1 nmol of M871, there were no marked influences on the HWLs to thermal and mechanical stimulation after intra-ACC administration of the selective galanin receptor 2 antagonist M871 in rats with mononeuropathy, as shown in Fig. 4.
Comparison of the basal HWL and the galanin-induced antinociception in normal rats and rats with mononeuropathic pain
The basal HWL in normal rats and rats with neuropathic pain are shown in Fig. 5. There were significant decreases in HWL to noxious thermal and mechanical stimulation in rats with neuropathic pain compared with normal rats (Hot-plate Test: tleft/left = 6.38, P < 0.001; Randall Selitto Test: tleft/left = 21.53, P < 0.001).
Figure 6 shows the changes in antinociceptive effects induced by intra-ACC injection of galanin in rats with neuropathic pain compared with that in normal rats. There was significant increase in HWL to noxious mechanical stimulation (Randall Selitto Test: t = 6.46, P < 0.001) in rats with neuropathic pain compared with normal rats as shown in Fig. 6B, well there was no significant increase in HWL to noxious thermal stimulation (Hot-plate Test: t = 0.29, P = 0.77) as shown in Fig. 6A.
Comparison of the mRNA levels of galanin and the content of galanin in ACC of normal rats and rats with mononeuropathic pain
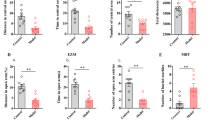
The galanin mRNA levels in ACC in normal rats and in rats with mononeuropathy were tested by real-time PCR (RT-PCR) and the results are shown in Fig. 7A. There was a significant increase in the mRNA level of galanin in ACC in rats with mononeuropathy than that in normal rats (t = 3.88, P < 0.01). The results indicate that the expression of galanin in ACC increased in rats with neuropathic pain.
We further determined the influence of sciatic nerve ligation-induce mononeuropathy on the content of galanin in ACC. The contents of galanin in ACC in normal rats and rats with mononeuropathy were tested by western blot and the results are shown in Fig. 7B and C. There was a significant increase in the content of galanin in ACC in rats with mononeuropathy (t = 6.83, P < 0.001) than that in normal rats.
The above results indicate that there may be increased changes of galanin expression in ACC induced by neuropathic pain in rats with sciatic nerve ligation.
Comparison of the mRNA levels and the content of galanin receptor 2 in ACC in normal rats and rats with mononeuropathic pain
Our results have demonstrated that galanin receptor 2 is involved in the galanin-induced antinociception in the ACC in normal rats and rats with mononeuropathy. Here we try to find the changes of galanin receptor 2 induced by neuropathic pain in rats with sciatic nerve ligation. The mRNA levels of galanin receptor 2 in ACC and the content of galanin receptor 2 in ACC were determined by RT-PCR and western blot, and the results are shown in Fig. 8.
As shown in Fig. 8A, there was a significant increase in the mRNA level of galanin receptor 2 (t = 9.77, P < 0.001) in ACC in rats with mononeuropathy than that in normal rats tested by RT-PCR. The results indicate that the expression of galanin receptor 2 increased in ACC in rats with neuropathic pain.
Figure 8B and C show the changes of galanin receptor 2 content in ACC in rats with neuropathic pain. There was a significant increase in the content of galanin receptor 2 in ACC of rats with mononeuropathy (t = 5.80, P < 0.001) than that in normal rats tested by western blot. The above results indicate that there may be plastic changes in the expression of galanin receptor 2 in ACC in rats with mononeuropathy.
Discussion
The present study demonstrated that administration of galanin into ACC induced significant increases in HWLs to noxious thermal and mechanical stimulations in normal rats and rats with mononeuropathy, indicate that galanin is involved in pain modulation in ACC in both normal rats and rats with mononeuropathy. Consistent with our findings, administration of galanin to the midbrain periaqueductal grey induced significant antinociceptive effects in intact rats and rats with mononeuropathy16,20. Jin and his colleagues reported that galanin induced antinociceptive effects in the central nucleus of amygdala of rats, and opioid receptors are involved in the galanin-induced antinociception14.
There are few reports related to the roles of galanin receptor 2 in the brain in pain modulation. Some studies showed that there were no marked differences in pain related behaviors between the mice lacking galanin receptor 2 and WT mice35. Interestingly, while mice with an absence of galanin receptor 2 gene transcription displayed significant deficits in pain behavior in neuropathic and inflammatory pain models36. Recent studies have demonstrated that galanin receptor 2 is involved in neuropathic pain5,21,23. Hulse and his collogues reported that the high level of endogenous galanin in injured primary afferents activate peripheral galanin receptor 2, which leads to an increase in c-fibre mechanical activation thresholds and a marked reduction in evoked and ongoing nociceptive responses21. Recently, Zhang and her colleagues reported that galanin receptor 2 is involved in the galanin-induced antinociceptive effects in the periaqueductal grey of rats19. As galanin receptor 2 may play an important role in nociceptive modulation in the central nervous system, the present study was further to explore the role of galanin receptor 2 in pain modulation in ACC of rats and found that the selective galanin receptor 2 antagonist M871 attenuated the galanin-induced antinociceptive effects in ACC, suggesting that galanin receptor 2 is involved in the galanin-induced antinociceptive effects in ACC in both normal rats and rats with mononeuropathy.
Recently, studies demonstrated that ACC is involved in the modulation of nociception25,31,37. Activation of the ACC is associated with reduced pain behavior produced by unilateral spinal nerve injury in rats34. The ACC is also reported to be involved in the persistent neuropathic pain31,38,39. The nerve cells in ACC responded to noxious stimuli and were activated during pain tested by electrophysiological methods40. In the present study, we found that intra-ACC injection of galanin induced dose-dependent increases in the latencies of hindpaw withdrawal to noxious thermal and mechanical stimulations in rats, suggesting that galanin induces antinociceptive effects in the ACC.
Chronic pain induced plasticity in central nervous system has been paid more and more attention. Recently Zhuo and his colleagues reviewed the synaptic plasticity in the anterior cingulate cortex in acute and chronic pain. In this review, they discussed that ACC activation contributes to chronic pain states and describe several forms of synaptic plasticity that may underlie the effect, in particular, one form of long-term potentiation (LTP) in the ACC sustains the affective component of the pain state41. In the present study, we found that both the galanin mRNA expression and galanin content increased significantly in ACC in rats with mononeuropathy than that in normal rats. Moreover, both the mRNA level of galanin receptor 2 and the content of galanin receptor 2 in ACC increased significantly in rats with mononeuropathy than that in normal rats. Combining the behavioral tests with these results indicate that there may be plasticity in the expression of galanin and galanin receptor 2 in rats with mononeuropathy, as well as in the galanin-induced antinociception.
Taken together, the present study found for the first time that galanin induces antinociception in ACC in both normal rats and rats with mononeuropathy. And there may be plastic changes in the expression of galanin and galanin receptor 2 in rats with mononeuropathy, as well as in the galanin-induced antinociception.
Methods
Chemicals
Solutions for intra-ACC administration were prepared with sterilized saline, each with a volume of 1 μl containing: (1) 0.1, 0.5, 1, or 2 nmol of galanin (rat galanin, 1–29 amino acids, Tocris, UK); (2) 0.1, 0.5, or 1 nmol of M871 (selective galanin receptor 2 antagonist; Tocris, UK).
Animal preparation
All experiments were carried out on freely moving male Sprague–Dawley rats weighing 220 to 260 g (Experimental Animal Center of Luye Pharmaceutical Company, Yantai, China). The rats were housed in cages with free access to food and water, and maintained in a room temperature of 20 ± 2 °C with a normal day/night cycle. All experiments were performed according to the guidelines of the International Association for the Study of Pain42 and The Guidelines for the Care and Use of Laboratory Animals of Yantai University. Our experiments were approved by Laboratory Animal Ethics Committee of Yantai University and the authorization number is 20140901-01. And every effort was made to minimize both the animal suffering and the number of animals used.
Nociceptive tests
Rats were accustomed to the test condition for 3 days before the experiment to minimize the stress induced by handling and measurements. The hindpaw withdrawal latencies (HWLs) during thermal and mechanical stimulation were measured as described previously14,15,43. Briefly, the entire ventral surface of the rat hindpaw was placed manually on a hot plate (YLS-6B Intelligent Heat Panel Instrument, Jinan Yiyan Science & Technology Development Co., Ltd., Jinan, China), which was maintained at a temperature of 52 ± 0.2 °C. The time to hindpaw withdrawal was measured in seconds and referred to as the HWL to thermal stimulation. The Randall Selitto Test (Ugo Basile, Type 7200, Italy) was used to assess the HWL to mechanical stimulation. A wedge-shaped pusher at a loading rate of 30 g/s was applied to the dorsal surface of the hindpaw. The latency required to initiate the withdrawal response was assessed and expressed in seconds. Before intra-ACC injection, the HWLs were tested three times and regarded as the basal HWLs. The HWLs recorded during subsequent experiments were expressed as percentage changes of the basal level for each rat (% changes of the HWL). Each rat was tested by both types of stimulation. Every measurement of the HWL to both thermal and mechanical stimulation was finished within 1–2 min. A cut-off limit of 15s was set up to avoid tissue damage.
Surgical procedures and intra-ACC injection
Rats were anaesthetized by intraperitoneal injection of pentobarbital sodium (50 mg/kg, Xudong Chemical Factory, Beijing, China) and mounted on stereotaxic frame, a stainless steel guide cannula of 0.8 mm outer diameter was directed to the ACC (1.6 mm anterior to Bregma; 0.7 mm lateral to midline; 2.0 mm ventral to the surface of skull) according to Paxinos and Watson44, and was fixed to the skull by dental acrylic. There were more than 3 days for rats to recover from the operation. On the day of experiment, a stainless steel needle with 0.4 mm outer diameter was directly inserted into the guide cannula with 1.5 mm beyond the tip of the latter. One microliter of solution was thereafter infused into the ACC over 1 min. The injection needle was left in the site for 1 min after each injection before removal.
The rat model of mononeuropathy
The mononeuropathy model was produced as previously reported13,43. Animals were anaesthetized by intraperitoneal injection of pentobarbital sodium (50 mg/kg) and 8–10 mm of the left common sciatic nerve was exposed at the level of the mid-high. Four loose ligatures were placed around the dissected nerve at 1.0–1.5 mm intervals. The ligations were carefully manipulated so that the nerve was barely constricted, and the skin incision was closed with silk sutures and animals allowed to recover.
RT-PCR
Normal rats (n = 3, as a control) and rats with sciatic nerve ligation 10 days after surgery (n = 3) received injection of over dose of 10% trichloroacetaldehyde monohydrate and the brain was removed immediately. The regions of the ACC were dissected on ice and the total RNA was isolated with UNIQ-10 Column Trizol Total RNA Extraction Kit (Sangon Biotech, Shanghai, China) following the instruction. Total RNA was firstly reverse-transcribed using AMV First Strand cDNA Synthesis Kit (Sangon Biotech, Shanghai, China), and the RT-PCRs were performed using StepOne™ Real-Time PCR System and software (Thermo Fisher Scientific, USA). Sequences of primers for the experiments were rat galanin: sense 5′-CACATGCCATTGACAACCAC-3′ and antisense 5′-AACTCCATTATAGTGCGGACG-3′; rat galanin receptor 2: sense 5′-GCCGCCATCGGGCTCATCTG-3′ and antisense 5′-GTCGAGGTGCGCTCCATGCT-3′); rat GAPDH: sense 5′-GACCACCCAGCCCAGCAAGG-3′and antisense 5′-TCCCCAGGCCCCTCCTGTTG-3′. The unigene expression levels were calculated with the 2(-delta delta C (T)) method45.
Western Blot
The normal rats (n = 3, as a control) and rats with sciatic nerve ligation 10 days after surgery (n = 3) received injection of over dose of 10% trichloroacetaldehyde monohydrate and the brain was removed immediately. The regions of the ACC were dissected on ice and then frozen at −80 °C. Total protein was extracted following our published protocol46, briefly the ACC samples homogenized in RIPA lysis buffer (Beyotime Institute of Biotechnology, Shanghai, China), the total protein was extracted and the whole protein extracts (80 μg) of ACC samples were subject to western blot assay. After transferred to PVDF membranes (Millipore, MA, USA), the membranes were incubated in blocking solution and then incubated with the polyclonal goat anti-galanin antibody (SAB2501407, Sigma–Aldrich, St. Louis, MO, USA), polyclonal rabbit anti-Gal R2 antibody (ab203072, Abcam, Cambridge, UK), beta-actin antibody (Beyotime Institute of Biotechnology, Shanghai, China) at 4 °C overnight. The membranes were washed with TBST and then probed with HRP-conjugated donkey anti-goat secondary antibody (Beyotime Institute of Biotechnology, Shanghai, China), HRP-conjugated goat anti-rabbit secondary antibody (Beyotime Institute of Biotechnology, Shanghai, China), HRP-conjugated goat anti-mouse secondary antibody (Beyotime Institute of Biotechnology, Shanghai, China). The brands were visualized by enhanced chemiluminescence (ECL) detection reagents (Beyotime Institute of Biotechnology, Shanghai, China) and imaged using ImageQuant LAS 4000 (GE Healthcare Bio-Sciences AB, Tokyo, Japan) automatically and quantified using ImageQuant software (GE Healthcare Bio-Sciences AB, Tokyo, Japan).
Statistical analysis
At the end of the experiments, the location of the tip of the injection needle was verified and the injection points were in ACC of rats. Only the results obtained from nociceptive tests that the tips of the injection needle are within the ACC are used for statistical analysis. Data from the experiment were expressed as mean ± S.E.M. Statistical difference between groups was determined by Two-way analysis of variance (ANOVA) for repeated measurements (Fleft/left is the F value of the two groups: the left HWL of one group compared with the left HWL of another group), One-way ANOVA followed Dunnett multiple comparison test or by Student’s t test (two-tailed). *P < 0.05, **P < 0.01 and ***P < 0.001 were considered as significant differences.
Additional Information
How to cite this article: Zhang, M.-L. et al. Involvement of galanin and galanin receptor 2 in nociceptive modulation in anterior cingulate cortex of normal rats and rats with mononeuropathy. Sci. Rep. 7, 45930; doi: 10.1038/srep45930 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Tatemoto, K., Rokaeus, A., Jornvall, H., Mcdonald, T. J. & Mutt, V. Galanin—a novel biologically active peptide from porcine intestine. FEBS Letters. 164, 124–128 (1983).
Melander, T., Hokfelt, T. & Rokaeus, A. Distribution of galanin-like immunoreactivity in the rat central nervous system. J. Comp. Neurol. 248, 475–517 (1986).
Branchek, T. A., Smith, K. E., Gerald, C. & Walker, M. W. Galanin receptor subtypes. Trends Pharmacol. Sci. 21, 109–117 (2000).
Lang, R., Gundlach, A. & Kofler, B. The galanin peptide family: receptor pharmacology, pleiotropic biological actions, and implications in health and disease. Pharmacol. Ther. 115, 177–207 (2007).
Mitsukawa, K., Lu, X. & Bartfai, T. Galanin, galanin receptors and drug targets. Cell. Mol. Life Sci. 65, 1796–1805 (2008).
Cheng, Y. & Yu, L.-C. Galanin protects amyloid-β-induced neurotoxicity on hippocampal neurons in rats. J. Alzheimer’s Dis. 20, 1143–1157 (2010).
Hokfelt, T. & Tatemoto, K. Galanin–25 years with a multitalented neuropeptide. Cell Mol. Life Sci. 65, 1793–1795 (2008).
Walton, K. M., Chin, J. E., Duplantier, A. J. & Mather, R. J. Galanin function in the central nervous system. Curr. Opin. Drug Disc. 9, 560–570 (2006).
Xu, X. et al. Effects of exogenous galanin on neuropathicpain state and change of galanin and its receptors in DRG and SDH after sciatic nerve-pinch injury in rat. PLoS One 7, e37621 (2012).
Amorim, D. et al. A role of supraspinal galanin in behavioural hyperalgesia in the rat. PLoS One 9, e113077 (2014).
Amorim, D. et al. Galanin-mediated behavioural hyperalgesia from the dorsomedial nucleus of the hypothalamus involves two independent descending pronociceptive pathways. PLoS One 10, e0142919 (2015).
Fu, L. B., Wang, X. B., Shi, J., Wu, X. & Yu, L.-C. Antinociceptive effects of intracerebroventricular injection of the galanin receptor 1 agonist M 617 in rats. Neurosci. Lett. 491, 174–176 (2011).
Gu, X. L., Sun, Y. G. & Yu, L.-C. Involvement of galanin in nociceptive regulation in the arcuate nucleus of hypothalamus in rats with mononeuropathy. Behav Brain Res. 179, 331–335 (2007).
Jin, W. Y., Liu, Z., Liu, D. & Yu, L.-C. Antinociceptive effects of galanin in the central nucleus of amygdala of rats, an involvement of opioid receptors. Brain Res. 1320, 16–21 (2010).
Sun, Y., Gu, X., Lundeberg, T. & Yu, L.-C. An antinociceptive role of galanin in the arcuate nucleus of hypothalamus in intact rats and rats with inflammation. Pain 106, 143–150 (2003).
Wang, D., Lundeberg, T. & Yu, L.-C. Antinociceptive Role of galanin in periaqueductal grey of rats with experimentally induced monomononeuropathy. Neuroscience 96, 767–771 (2000).
Wu, X. & Yu, L.-C. Alternation of galanin in nociceptive modulation in the central nervous system of rats during morphine tolerance: a behavioral and immunohistochemical study. Brain Res. 1086, 85–91 (2006).
Xu, S. L., Li, J., Zhang, J. J. & Yu, L. C. Antinociceptive effects of galanin in the nucleus accumbens of rats. Neurosci. Lett. 520, 43–46 (2012).
Zhang, X. Y., Zhang, Y. M., Zhang, M. L. & Yu, L. C. Involvement of galanin receptor 2 and CaMKII in galanin-induced antinociception in periaqueductal grey of rats. Neurosci. Lett. 604, 124–127 (2015).
Wang, D., Ye, H., Yu, L.-C. & Lundeberg, T. Intra-periaqueductal grey injection of galanin increases the nociceptive response latency in rats, an effect reversed by naloxone. Brain Res. 834, 152–154 (1999).
Hulse, R. P., Wynick, D. & Donaldson, L. F. Activation of the galanin receptor 2 in the periphery reverses nerve injury-induced allodynia. Mol. Pain 7, 26 (2011).
Hulse, R. P., Donaldson, L. F. & Wynick, D. Peripheral galanin receptor 2 as a target for the modulation of pain. Pain Res. Treat. 2012, 545386(2012).
Metcalf, C. S. et al. Analgesic properties of a peripherally acting and GalR2 receptor–preferring galanin analog in inflammatory, neuropathic, and acute pain models. J. Pharmacol. Exp. Ther. 352, 185–193 (2015).
Devinsky, O., Morrell, M. J. & Vogt, B. A. Contributions of anterior cingulate cortex to behaviour. Brain 118, 279–306 (1995).
Shen, F.-Y. et al. Alleviation of neuropathic pain by regulating T-type calcium channels in rat anterior cingulated cortex. Mol. Pain 11, 7, doi: 10.1186/s12990-015-0008-3 (2015).
Zhuo, M. Contribution of synaptic plasticity in the insular cortex to chronic pain. Neuroscience 338, 220–229 (2016).
Gu, L. et al. Pain inhibition by optogenetic activation of specific anterior cingulate cortical neurons. PLoS ONE 10, e0117746, doi: 10.1371 (2015).
Li, X. Y. et al. Alleviating neuropathic pain hypersensitivity by inhibiting PKMzeta in the anterior cingulate cortex. Science 330, 1400–1404 (2010).
Lu, B. et al. Inhibition of mammalian target of rapamycin activation in the rostral anterior cingulate cortex attenuates pain-related aversion in rats. Behav. Brain Res. 310, 51–58 (2016).
Lieberman, M. D. & Eisenberger, N. I. The dorsal anterior cingulate cortex is selective for pain: Results from large-scale reverse inference. PANS. 112, 15250–15255 (2015).
Xu, H. et al. Presynaptic and postsynaptic amplifications of neuropathic pain in the anterior cingulated cortex. J. Neurosci. 28, 7445–7453 (2008).
Zhuo, M. Multiple PKCε-dependent mechanisms mediating mechanical hyperalgesia. Pain 150, 17–21 (2010).
Brian, C. et al. Diabetic mononeuropathy: Clinical manifestations and current treatments. Lancet Neurol. 11, 521–534 (2012).
LaBuda, C. J. & Fuchs, P. N. Attenuation of negative pain affect produced by unilateral spinal nerve injury in the rat following anterior cingulate cortex activation. Neuroscience 136, 311–322 (2005).
Shi, T. J. et al. Sensory neuronal phenotype in galanin receptor 2 knockout mice: focus on dorsal root ganglion neuron development and pain behaviour. Eur. J. Neurosci. 23, 627–36 (2006).
Hobson, S. A., Holmes, F. E., Kerr, N. C., Pope, R. J. & Wynick, D. Mice deficient for galanin receptor 2 have decreased neurite outgrowth from adult sensory neurons and impaired pain-like behaviour. J. Neurochem. 99, 1000–1010 (2006).
Zhuo, M. Molecular mechanisms of pain in the anterior cingulate cortex. J. Neurosci. Res. 84, 927–933 (2006).
Widerström-Noga, E. et al. Metabolite concentrations in the anterior cingulate cortex predict high neuropathic pain impact after spinal cord injury. Pain 154, 204–212 (2013).
Zhang, L. et al. Brain-derived neurotrophic factor (BDNF) in the rostral anterior cingulate cortex (rACC) contributes to neuropathic spontaneous pain-related aversion via NR2B receptors. Brain Res. Bull. 127, 56–65 (2016).
Yamamura, H. et al. Morphological and electrophysiological properties of ACC nociceptive neurons in rats. Brain Res. 735, 83–92 (1996).
Bliss, T. V., Collingridge, G. L., Kaang, B. K. & Zhuo, M. Synaptic plasticity in the anterior cingulate cortex in acute and chronic pain. Nat. Rev. Neurosci. 17, 485–96 (2016).
Zimmermann, M. Ethical guidelines for investigations of experimental pain in conscious animals. Pain 16, 109–10 (1983).
Bian, H. & Yu, L. C. Intra-nucleus accumbens administration of the calcium/calmodulin-dependent protein kinase II inhibitor AIP induced antinociception in rats with monomononeuropathy. Neurosci. Lett. 599, 129–132 (2015).
Paxinos, G. & Watson, C. The rat brain in stereotaxic coordinates, fourth ed., (Academic Press, Sydney 1998).
Livak, K. J. & Schmittgen, T. D. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-delta delta C (T)) method. Methods. 25, 402–408 (2001).
Li, M. et al. Oral administration of escin inhibits acute inflammation and reduces intestinal mucosal injury in animal models. EVID-BASED COMPL ALT 2015, Article ID 503617, 9 pages (2015).
Acknowledgements
The study is supported by grants from Foundation of Collaborative Innovation Center of Advanced Drug Delivery System and Biotech Drugs in Universities of Shandong (Yantai University), the Graduate Innovation Foundation of Yantai University and the National Natural Science Foundation of China (NSFC 30870802, 81171043).
Author information
Authors and Affiliations
Contributions
Meng-Lin Zhang completed the whole experiments. Hong-Bo Wang edited the manuscript, Feng-Hua Fu and Long-Chuan Yu designed the experiments and edited the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zhang, ML., Wang, HB., Fu, FH. et al. Involvement of galanin and galanin receptor 2 in nociceptive modulation in anterior cingulate cortex of normal rats and rats with mononeuropathy. Sci Rep 7, 45930 (2017). https://doi.org/10.1038/srep45930
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep45930
- Springer Nature Limited
This article is cited by
-
The activation of galanin receptor 2 plays an antinociceptive effect in nucleus accumbens of rats with neuropathic pain
The Journal of Physiological Sciences (2021)
-
Involvement of galanin and galanin receptor 1 in nociceptive modulation in the central nucleus of amygdala in normal and neuropathic rats
Scientific Reports (2017)