Abstract
OBJECTIVE: This pilot study's aim was to establish feasibility of a protocol for delayed cord clamping (DCC) versus immediate cord clamping (ICC) at preterm birth and to examine its effects on initial blood pressure and other outcomes.
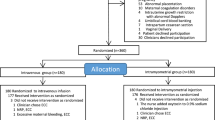
STUDY DESIGN: A randomized controlled trial recruited 32 infants between 24 and 32 weeks. Immediately before delivery, mothers were randomized to ICC (cord clamped at 5 to 10 seconds) or DCC (30- to 45-second delay in cord clamping) groups.
RESULTS: Intention-to-treat analyses revealed that the DCC group were more likely to have higher initial mean blood pressures (adjusted OR 3.4) and less likely to be discharged on oxygen (adjusted OR 8.6). DCC group infants had higher initial glucose levels (ICC=36 mg/dl, DCC=73.1 mg/dl; p=0.02).
CONCLUSION: The research design is feasible. The immediate benefit of improved blood pressure was confirmed and other findings deserve consideration for further study.

Similar content being viewed by others
References
Kinmond S, Aitchison TC, Holland BM, et al. Umbilical cord clamping and preterm infants: a randomized trial. BMJ 1993;306:172–175.
McDonnell M, Henderson-Smart DJ . Delayed umbilical cord clamping in preterm infants: a feasibility study. J Paediatr Child Health 1997;33:308–310.
Narendra A, Beckett C, Aitchison T, et al. Is it possible to promote placental transfusion (PTFx) at preterm delivery? Pediatr Res 1998;44:454 (Abstract).
Nelle M, Fischer S, Conze S, Beedgen B, Grischke EM, Linderkamp O . Effects of late cord clamping on circulation in prematures (VLBWI). Pediatr Res 1998;44:454 (Abstract).
Rabe H, Wacker A, Hulskamp G, Hornig-Franz I, Jorch G . Late cord clamping benefits extrauterine adaptation. Pediatr Res 1998;44:454 (Abstract).
Rabe H, Wacker A, Hulskamp G, et al. A randomised controlled trial of delayed cord clamping in very low birth weight preterm infants. Eur J Pediatr 2000;159(10):775–777.
Ibrahim HM, Krouskop RW, Lewis DF, Dhanireddy R . Placental transfusion: umbilical cord clamping and preterm infants. J Perinatol 2000;20:351–354.
Yao AC, Moinian M, Lind J . Distribution of blood between the infant and the placenta after birth. Lancet 1969;7626(2):871–873.
Waldrop CAJ, Holland BM . The roles and vital importance of placental blood to the newborn infant. J Perinat Med 1995;23:139–143.
World Medical Association Recommendations Guiding Physicians in Biomedical Research: Declaration of Helsinki. http://www.wma.net//policy/17-c_e.html.
Richardson DK, Corcoran JD, Escobar GJ, Lee SK . SNAP-II and SNAPPE-II: simplified newborn illness severity and mortality risk scores. J Pediatr 2001;138(1):92–100.
Ebbutt A, Frith L . Practical issues in equivalence trials. Stat Med 1998;17:1691–1701.
Friedman L, Furberg C, DeMets D . Fundamentals of Clinical Trials. 3rd ed. New York: Springer; 1998.
Lindner W, Vobeck S, Hummler H, Pohlandt F . Delivery room management of extremely low birth weigth infants spontaneous breathing or intubation? Pediatrics 1999;103(5):961–967.
Oh W, Lind J, Gessner IH . Circulatory and respiratory adaptation to early and late cord clamping in newborn infants. Acta Paediatr Scand 1966;55:17–25.
Tsuru A, Mizuguchi M, Takashima S . Cystic leukomalacia in the cerebellar folia of premature infants. Acta Neuropathol (Berl) 1995;94(4):400–402.
Arroe M, Peitersen B . Retinopathy of prematurity: review of a seven-year period in a Danish neonatal intensive care unit. Acta Pediatr 1994;83(5):501–505.
Murphy D, Hope P, Johnson A . Neonatal risk factors for cerebral palsy in very preterm babies: case control study. BMJ 1997;314(7078):404–408.
Polin R, Fox W . Fetal and Neonatal Physiology. 2nd ed. Philadelphia: WB Saunders Company; 1998.
Dixon LR . The complete blood count: physiologic basis and clinical usage. J Perinat Neonatal Nurs 1997;11(3):1–18.
Callahan DJ, Engle MJ, Volpe JJ . Hypoxic injury to developing glial cells: protective effect of high glucose. Pediatr Res 1990;27(2):186–190.
Jaykka S . Capillary erection and the structural appearance of fetal and neonatal lungs. Acta Paediatr 1958;47:484–500.
Porges SW . Vagal tone: a physiologic marker of stress vulnerability. Pediatrics 1992;90(3):498–504.
Mercer JS, Skovgaard R . Neonatal transitional physiology: a new paradigm. J Perinat Neonatal Nurs 2002;15(4):56–75.
Clark R, Slutsky A, Gertsmann D . Lung protective strategies of ventilation in the neonate: what are they? Pediatrics 2000;105(1):112–114.
Jones JG, Holland BM, Hudson IR, Wardrop CA . Total circulating red cells versus haematocrit as the primary descriptor of oxygen transport by the blood. Br J Haematol 1990;76(2):288–294.
Wardrop CAJ, Holland BM, Jones JG . Consensus on red cell transfusion. BMJ 1995;311:962–963.
Author information
Authors and Affiliations
Additional information
Statistical Consultation: Walter Heber, M.Sc., Research Statistician, Division of Research, Department of Obstetrics and Gynecology, Women and Infants Hospital, Providence, Rhode Island.
Funding sources: Sigma Theta Tau, Epsilon Chapter; University of Rhode Island Foundation and College of Nursing
Rights and permissions
About this article
Cite this article
Mercer, J., McGrath, M., Hensman, A. et al. Immediate and Delayed Cord Clamping in Infants Born Between 24 and 32 Weeks: A Pilot Randomized Controlled Trial. J Perinatol 23, 466–472 (2003). https://doi.org/10.1038/sj.jp.7210970
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7210970
- Springer Nature America, Inc.
This article is cited by
-
Antenatal and perinatal factors influencing neonatal blood pressure: a systematic review
Journal of Perinatology (2021)
-
Early versus delayed umbilical cord clamping on maternal and neonatal outcomes
Archives of Gynecology and Obstetrics (2019)
-
Timing of umbilical cord clamping among infants born at 22 through 27 weeks’ gestation
Journal of Perinatology (2016)
-
A physiologic approach to cord clamping: Clinical issues
Maternal Health, Neonatology and Perinatology (2015)
-
Early versus delayed umbilical cord clamping in infants with congenital heart disease: a pilot, randomized, controlled trial
Journal of Perinatology (2015)