Abstract
Background/Objectives:
To compare the efficacy and side effects of low-dose vs high-dose iron supplements to correct anaemia in pregnancy.
Subjects/Methods:
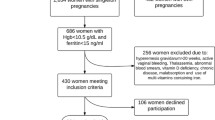
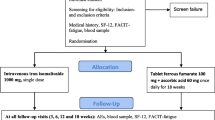
One hundred and eighty women with anaemia (haemoglobin <110 g l−1) in mid-pregnancy. The women were randomly allocated to 20; 40 or 80 mg of iron daily for 8 weeks from mid-pregnancy.
Results:
One hundred and seventy-nine (99%) women completed the trial. At the end of treatment, there was a clear dose–response of increasing mean haemoglobin concentration with iron dose (111±13 g l−1 at 20 mg per day, 114±11 g l−1 at 40 mg per day and 119±12 g l−1 at 80 mg per day, P=0.006). However, the incidence of anaemia did not differ statistically between groups. Compared with women in the 80 mg iron group, the odds ratio of anaemia was 1.9 (95% CI: 0.8, 4.3, P=0.130) and 1.1 (95% CI: 0.5, 2.6, P=0.827), respectively, for women in the 20 mg iron group and the 40 mg iron group. The incidence of gastrointestinal side effects was significantly lower for women in the 20 mg iron group compared with women in the 80 mg iron group; the odds ratio was 0.4 (95% CI: 0.2, 0.8, P=0.014) for nausea, 0.3 (95% CI: 0.2, 0.7, P=0.005) for stomach pain and 0.4 (95% CI: 0.2, 0.9, P=0.023) for vomiting.
Conclusions:
Low-dose iron supplements may be effective at treating anaemia in pregnancy with less gastrointestinal side effects compared with high-dose supplements.

Similar content being viewed by others
References
Cuervo LG, Mahomed K (2003). Treatments for iron deficiency anaemia in pregnancy. Cochrane Database Syst Rev Issue 2, CD 003094.
Department of Health and Aging (DHA) & National Health and Medical Research Council (NHMRC) (2006). Nutrient Reference Values for Australia and New Zealand Including Recommended Dietary Intakes. Commonwealth of Australia: Canberra.
Ekstrom EC, Hyder SM, Chowdhury AM, Chowdhury SA, Lonnerdal B, Habicht JP et al. (2002). Efficacy and trial effectiveness of weekly and daily iron supplementation among pregnant women in rural Bangladesh: disentangling the issues. Am J Clin Nutr 76, 1392–1400.
Enkin M, Keirse M, Halmers I (1995). A Guide to Effective Care in Pregnancy and Childbirth, 2nd edn. Oxford University Press: New York.
Eskeland B, Malterud K, Ulvik RJ, Hunskaar S (1997). Iron supplementation in pregnancy: is less enough? A randomized, placebo controlled trial of low dose iron supplementation with and without heme iron. Acta Obstet Gynecol Scand 76, 822–828.
Garn SM, Ridella SA, Petzold AS, Falkner F (1981). Maternal hematologic levels and pregnancy outcomes. Semin Perinatol 5, 155–162.
Hahn PF, Carothers EL, Darby WJ, Martin M, Sheppard CW, Tenn N et al. (1951). Iron metabolism in human pregnancy as studied with the radioactive isotope, FE59*. Am J Obstet Gynecol 61, 477–486.
Hallberg L, Ryttinger L, Solvell L (1966). Side-effects of oral iron therapy. a double-blind study of different iron compounds in tablet form. Acta Med Scand Suppl 459, 3–10.
Lee JI, Lee JA, Lim HS (2005). Effect of time of initiation and dose of prenatal iron and folic acid supplementation on iron and folate nutriture of Korean women during pregnancy. Am J Clin Nutr 82, 843–849.
Letsky E (1991). The Haematological system. In: Hytten F, Chamberlain G (eds). Clinical Physiology in Obstetrics. Blackwell Scientific Publications: Oxford, UK. pp 39–82.
Mahomed K (2000). Iron supplementation in pregnancy. Cochrane Database Syst Rev Issue 2, CD 000117.
Makrides M, Crowther CA, Gibson RA, Gibson RS, Skeaff CM (2003). Efficacy and tolerability of low-dose iron supplements during pregnancy: a randomized controlled trial. Am J Clin Nutr 78, 145–153.
Milman N, Bergholt T, Eriksen L, Byg KE, Graudal N, Pedersen P et al. (2005). Iron prophylaxis during pregnancy—how much iron is needed? A randomized dose–response study of 20–80 mg ferrous iron daily in pregnant women. Acta Obstet Gynecol Scand 84, 238–247.
Murphy JF, O'Riordan J, Newcombe RG, Coles EC, Pearson JF (1986). Relation of haemoglobin levels in first and second trimesters to outcome of pregnancy. Lancet 1, 992–995.
Pena-Rosas J, Viteri F (2006). Effects of routine oral iron supplementation with or without folic acid for women during pregnancy. Cochrane Database Syst Rev Issue 3, CD004736.
Pena-Rosas JP, Nesheim MC, Garcia-Casal MN, Crompton DW, Sanjur D, Viteri FE et al. (2004). Intermittent iron supplementation regimens are able to maintain safe maternal hemoglobin concentrations during pregnancy in Venezuela. J Nutr 134, 1099–1104.
Reddaiah VP, Raj PP, Ramachandran K, Nath LM, Sood SK, Madan N et al. (1989). Supplementary iron dose in pregnancy anemia prophylaxis. Indian J Pediatr 56, 109–114.
Solomons NW (1986). Competitive interaction of iron and zinc in the diet: consequences for human nutrition. J Nutr 116, 927–935.
Sood SK, Ramachandran K, Mathur M, Gupta K, Ramalingaswamy V, Swarnabai C et al. (1975). W.H.O. sponsored collaborative studies on nutritional anaemia in India. 1. The effects of supplemental oral iron administration to pregnant women. Q J Med 44, 241–258.
Steer P, Alam MA, Wadsworth J, Welch A (1995). Relation between maternal haemoglobin concentration and birth weight in different ethnic groups. BMJ 310, 489–491.
The British Nutrition Foundation (1995). Iron absorption. In: Iron Nutritional and Physiological Significance, the Report of the British Nutrition Foundation's Task Force. Chapman & Hall: London. pp 3–12.
WHO (2001). Iron Deficiency Anaemia: Assessment, Prevention and Control—a Guide for Programme Managers. WHO: Geneva.
Zhou LM, Yang WW, Hua JZ, Deng CQ, Tao X, Stoltzfus RJ (1998). Relation of hemoglobin measured at different times in pregnancy to preterm birth and low birth weight in Shanghai, China. Am J Epidemiol 148, 998–1006.
Zhou SJ, Gibson RA, Crowther CA, Baghurst P, Makrides M (2006). Effect of iron supplementation during pregnancy on the intelligence quotient and behavior of children at 4 y of age: long-term follow-up of a randomized controlled trial. Am J Clin Nutr 83, 1112–1117.
Zhou SJ, Schilling MJ, Makrides M (2005). Evaluation of an iron specific checklist for the assessment of dietary iron intake in pregnant and postpartum women. Nutrition 21, 908–913.
Ziaei S, Norrozi M, Faghihzadeh S, Jafarbegloo E (2007). A randomised placebo-controlled trial to determine the effect of iron supplementation on pregnancy outcome in pregnant women with haemoglobin ⩾13.2 g/dl. BJOG 114, 684–688.
Acknowledgements
This work was supported by funding from the Adelaide Women's & Children's Hospital Research Foundation. MM and RAG were supported by a National Health & Medical Research Council Senior Research Fellowship (ID: 298902 for MM and 250324 for RAG). The iron and placebo tablets used in the trial were manufactured and donated by Soul Pattinson Manufacturing, Kingsgrove, NSW, Australia. The funding organizations had no role in the design and conduct of the study, the analysis and interpretation of the data, or the preparation, review and approval of the manuscript. MM and RAG occasionally provide advice to manufacturers of nutritional supplements. SJZ and CAC have no known conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Contributors: SJZ, MM and RAG designed the study in consultation with CAC. SJZ collected data, did the analysis and wrote the manuscript under the supervision of MM, RAG and CAC. All authors had a role in data interpretation and commented on drafts of the manuscript.
Rights and permissions
About this article
Cite this article
Zhou, S., Gibson, R., Crowther, C. et al. Should we lower the dose of iron when treating anaemia in pregnancy? A randomized dose–response trial. Eur J Clin Nutr 63, 183–190 (2009). https://doi.org/10.1038/sj.ejcn.1602926
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602926
- Springer Nature Limited
Keywords
This article is cited by
-
Providing lipid-based nutrient supplement during pregnancy does not reduce the risk of maternal P falciparum parasitaemia and reproductive tract infections: a randomised controlled trial
BMC Pregnancy and Childbirth (2017)
-
Algorithmus zur Diagnose von Eisenmangelanämie
Wiener Medizinische Wochenschrift (2016)
-
Iron bioavailability from commercially available iron supplements
European Journal of Nutrition (2015)
-
Adapting iron dose supplementation in pregnancy for greater effectiveness on mother and child health: protocol of the ECLIPSES randomized clinical trial
BMC Pregnancy and Childbirth (2014)
-
Accuracy of erythrogram and serum ferritin for the maternal anemia diagnosis (AMA): a phase 3 diagnostic study on prediction of the therapeutic responsiveness to oral iron in pregnancy
BMC Pregnancy and Childbirth (2013)