Abstract
Human milk contains SARS-CoV-2-specific antibodies after COVID-19 vaccination. These milk antibodies decrease several months post-vaccination. Whether booster immunization restores human milk antibody levels, potentially offering prolonged passive immunity for the infant, remains unknown. In this prospective follow-up study, we investigated the longitudinal SARS-CoV-2-specific antibody response in human milk of 26 lactating women who received a COVID-19 booster dose of an mRNA-based vaccine. Moreover, we evaluated whether the booster-induced human milk antibody response differs for participants who received a similar or different vaccine type in their primary vaccination series. All participants (100%) who received a homologous booster vaccination showed SARS-CoV-2-specific immunoglobulin A (IgA) and immunoglobulin G (IgG) in their milk. Heterologous booster vaccination resulted in milk conversion for 9 (69%) and 13 (100%) participants for IgA and IgG respectively. Findings of this study indicate that both homologous and heterologous boosting schedules have the potential to enhance SARS-CoV-2-specific IgA and IgG in human milk.
Similar content being viewed by others
Introduction
Infants account for the highest proportion of hospitalized children due to severe coronavirus disease 2019 (COVID-19)1,2. In the first months of life, infants mainly rely on passive immunity derived from their mother to protect them from respiratory infections3, including infection with the severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2). Human milk offers passive immunity to the breastfed infant through the transfer of disease-specific antibodies, mostly immunoglobulin A (IgA)4.
Maternal vaccination against COVID-19 can induce neutralizing SARS-CoV-2-specific human milk antibodies, which likely offer protection to the breastfed infant5,6. Vaccine-induced antibodies against SARS-CoV-2 in serum wane after several months, consequently leading to the occurrence of breakthrough infections7. A similar decrease was observed for specific human milk antibodies6, which may also entail waning protection for the breastfed infant. Booster vaccination can lead to restored immune protection against SARS-CoV-2 by boosting neutralizing antibody titers in serum8. Whether booster immunization also leads to restored human milk antibody levels, potentially offering prolonged passive immunity for the infant, remains unknown.
In this prospective cohort study, we demonstrate the longitudinal SARS-CoV-2-specific antibody response in human milk of lactating women receiving a COVID-19 booster dose of an mRNA-based vaccine. These findings indicate that both homologous and heterologous boosting schedules enhance SARS-CoV-2-specific IgA and IgG in milk of lactating women.
Results
Of the 26 lactating women participating in this follow-up study, 13 (50%) received homologous booster vaccination after completing a COVID-19 vaccination regimen with an mRNA-based vaccine, namely BNT162b2 (n = 4) or mRNA-1273 (n = 9). The other 13 participants (50%) received heterologous booster vaccination after they had previously completed a vaccination regimen with a vector-based vaccine, namely AZD1222 (n = 8) or Ad26.COV2.S (n = 5). For the booster dose, all participants received the BNT162b2 vaccine, except for one participant who received a booster dose of the mRNA-1273 vaccine (Fig. 1).
Characteristics of participants prior to the first COVID-19 vaccination are shown in Table 1. At the start of the initial study, before vaccination, participants had been breastfeeding for a mean time of 6.6 months (SD, 4.5), and this was similar between the two groups. None of the participants reported a PCR-confirmed SARS-CoV-2 infection prior to vaccination. Participants with specific antibodies targeting the spike protein of SARS-CoV-2 in their serum prior to their first vaccination were excluded from the analysis.
The mean time to booster vaccination after the first vaccine dose was 285 days (full range, 230–366 days) in the homologous group and 266 days (full range, 214–319 days) in the heterologous group. In total, 199 human milk samples were analyzed.
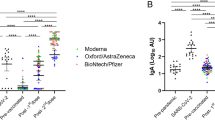
Prior to the administration of the booster dose, mean IgA antibodies in milk were similar for both groups (95% CI of mean 0.08–0.54; p = 0.25, n = 22 samples). All participants who received homologous booster vaccination showed detectable levels of SARS-CoV-2-specific IgA in their milk at one time point at least (Fig. 2a). Detectable IgA was sustained in the milk of 12 out of 13 participants until the end of the follow-up period. In the heterologous booster vaccination group, 9 out of 13 participants had detectable IgA in their milk during the follow-up period at one time point at least. All participants (100%) had detectable levels of SARS-CoV-2-specific IgG after both homologous and heterologous booster vaccination (Fig. 2b and Supplementary Data 1).
Antibody responses in human milk before and after homologous and heterologous booster vaccination are shown in box-and-whisker plots of SARS-CoV-2-specific immunoglobulin A (a) and immunoglobulin G (b). Blue dots (y) represent participants who received an mRNA-based vaccine for their primary series: two doses of mRNA-1273 (blue-filled dots) or BNT162b2 (transparent dots, blue border). Red dots (z) represent participants who received an adenoviral vector-based vaccine as primary series: two doses of AZD1222 (red-filled dots) or a single dose of Ad26.COV2.S (transparent dots, red border). For each group, n = 13 biologically independent samples except for the following days in the heterologous booster group prior to booster dose (n = 12) and after 3 days (n = 11), and in the homologous booster group prior to booster dose (n = 10), after 7 days (n = 11), and 15 days (n = 12). All scatter plots in this figure represent the mean of measurements in duplicate per participant. Analyzed samples were collected before (Pre-BD), and 3 days (3d), 5 days (5d), 7 days (7d), 9 days (9d), 11 days (11d), 13 days (13d), and 15 days (15d) after administration of an mRNA-vaccine booster dose (BD). Boxes indicate the 25th percentile, median (horizontal bar), mean (“+”), and 75th percentile; whiskers, minimum and maximum ranges; OD450nm, optical density 450 nm. Cutoff values are indicated with dashed lines. Source data are provided in the Supplementary Data 1 file.
There was no difference in the elicited antibody response following booster vaccination between participants who received AZD1222 or Ad26.COV2.S as a vector-based vaccine for their primary vaccine series.
Homologous and heterologous booster vaccination induced a similar change in IgA and IgG antibodies in human milk during the follow-up period, defined as AUCI (Fig. 3, Supplementary Data 1, and Table 2). Participants who received homologous booster vaccination had overall higher levels of SARS-CoV-2-specific IgA and IgG in their human milk (AUCG, AUCPP, and AUCNet) than those who received heterologous booster vaccination, due to overall higher pre-booster levels.
Antibody response in human milk of 26 lactating women vaccinated against COVID-19. SARS-CoV-2-specific immunoglobulin A (a) and immunoglobulin G (b) in human milk were measured using an ELISA with the SARS-CoV-2 spike protein. Participants either received a primary series with an mRNA vaccine (2 × mRNA-1273 or 2 × BNT162b2), subsequently following a homologous boosting schedule (n = 13), or a vector-based vaccine (2 × AZD1222 or 1 × Ad26.COV2.S) and thus following a heterologous boosting schedule (n = 13). The left part of both graphs (from pre-1D to 2D2wk), is already described in our previous study10. The time between the first dose and booster dose in the homologous group was, on average, 338 days (BNT162b2) and 262 days (mRNA-1273), and in the heterologous group, 234 days (Ad26.COV2.S) and 285 days (AZD1222). Analyzed samples were collected prior to a vaccine dose, 3 days, 5 days, 7 days, 9 days, 11 days, 13 days, and 15 days after a vaccine dose. 1D, first vaccine dose; 2D, second vaccine dose; BD, mRNA-vaccine booster vaccine; Pre, one day prior to; 1wk, one week after; 2wk, two weeks after vaccine dose. Data points represent the mean of all measurements per group; the shaded area around the mean represents the standard deviation. Cutoff values are indicated with dashed lines. OD450nm, optical density 450 nm. Source data are provided in the Supplementary Data 1 file.
Both mean IgA and IgG antibodies detected in human milk increased significantly after 15 days following vaccination. However, mean IgA levels in milk stagnated between 7 and 15 days following vaccination, even showing a moderate decline, while a gradual increase in mean IgG antibodies in milk was observed from pre-booster to day 7 and day 7 to day 15.
Discussion
Booster doses against COVID-19 are currently being administered because of the decline in efficacy of the primary vaccination series due to the waning of SARS-CoV-2-specific antibodies9. Consistent with findings in serum, a decline in human milk antibodies several months after a primary COVID-19 vaccination was observed10. In the current study, after booster vaccination with an mRNA-based vaccine, an increase in SARS-CoV-2-specific antibodies in human milk was observed. Interestingly, booster vaccination led to a comparable increase in human milk antibodies from participants who received a primary series of an mRNA-based vaccine (homologous booster vaccination group) to those who completed a primary series with a vector-based vaccine (heterologous booster vaccination group). However, because participants in the homologous booster vaccination group started from higher pre-booster levels, the total amount of SARS-CoV-2-specific antibodies in their milk over the study period after booster vaccination was higher.
We observed a steady increase in human milk IgG after booster vaccination, while the IgA response was moderate and of greater inter-individual variation. This difference could be explained by the fact that COVID-19 vaccines are intradermally administered, mostly triggering a systemic immune response (IgG).
In addition, IgG appeared earlier than IgA in human milk after booster vaccination, and IgG continued to increase steadily, whereas IgA showed a moderate increase which stagnated after only several days and started to decline thereafter. The diverse dynamics of IgA and IgG responses could be attributed to their different immune functions. IgA is the principal antibody in mucosal immunity and serves as the first line of defense, whereas IgG, the most abundant antibody type in serum, predominantly plays a role during the secondary immune response and is maintained for several months11. Similar observations have been described by other researchers studying the humoral response to natural SARS-CoV-2 infection and to different COVID-19 vaccines12,13.
Currently, trials supporting recommendations for booster vaccinations in lactating women are lacking. In one study, an increase in specific IgG and IgA levels in milk was observed after administration of a BNT162b2 booster vaccination in 12 lactating women who had received a primary series of BNT162b214. Moreover, heterologous vaccination schedules in lactating women have not been studied, even though many lactating women received heterologous booster vaccination because vector-based vaccines for women below 60 years of age were no longer used in the Netherlands due to reports of severe thrombosis. Our study adds that the administration of an mRNA-based booster vaccination induces a significant antibody response in human milk independent of the initial vaccine type.
Although previous data on human milk is lacking, findings from a randomized controlled trial also show that both homologous and heterologous booster vaccinations induce a sufficient systemic antibody response and that these booster-induced antibodies in serum have the capacity to neutralize SARS-CoV-215.
Timing of sampling and freeze-thaw cycles are suggested to affect human milk composition16, but it is unclear whether this also affects IgA. Human milk antibodies have been found to be relatively stable during freeze-thaw cycles, though contradictory observations have been reported17. In the current study, all of the collected samples of milk were thawed once. Despite clear instructions to participants on milk sample collection, personal variation in collection and time between collection and storage in the freezer cannot be ruled out since there was no supervision during sample collection. Also, we cannot completely rule out a SARS-CoV-2 infection in between vaccine doses as we did not verify the absence of anti-nucleocapsid antibodies; only the absence of anti-spike protein antibodies was verified prior to vaccination. Therefore, we cannot draw conclusions from comparisons on an individual level, but solely on a group level. Interpretation of our results may also be limited due to our small sample size. But as we only included participants who had already participated in our previous study, this allowed us to demonstrate the longitudinal antibody response following their primary series and booster vaccination. In the current study, we did not collect infant samples. Transmission of vaccine-induced antibodies against SARS-CoV-2 to the breastfed infant has been previously described18. Large sample-sized studies are needed to confirm the transfer and immunological protection of human milk antibodies for breastfed infants against SARS-CoV-2 infection.
In summary, our current findings demonstrate the potential of mRNA-based booster vaccination to enhance SARS-CoV-2-specific immunoglobulin A and immunoglobulin G in human milk. Based on our results, we support recommendations on mRNA-vaccine booster doses in lactating women and suggest that both homologous and heterologous boosting induce specific antibodies against SARS-CoV-2 in human milk, which likely protect the breastfed infant.
Methods
Study design
To investigate the longitudinal antibody response against SARS-CoV-2 in human milk after COVID-19 booster vaccination, we conducted a prospective cohort follow-up study of previously fully vaccinated individuals who participated in our original vaccination study10.
To assess whether the human milk antibody response against COVID-19 differs after homologous and heterologous booster vaccination, participants were divided into two cohorts based on the type of vaccine they received for their primary vaccination series, and human milk samples from both groups were collected longitudinally following booster vaccination.
Ethical considerations
This study was conducted in accordance with the declaration of Helsinki and the ICH GCP Guidelines and complied with the Regulation on Medical Research Involving Human Subjects. The study protocol was approved by the Ethics Committee of the Amsterdam University Medical Center. We have obtained written informed consent from all participants.
Population and setting
The current study is a follow-up of our previous vaccination study10. All lactating individuals in the Netherlands receiving a vaccination against COVID-19 were eligible to participate. Participants of the initial vaccination study who were still lactating and were going to receive a booster dose of a COVID-19 vaccine could register to participate in the current prospective follow-up study.
Recruitment of participants for the original study was done through several social media platforms and registration for participation in the current follow-up study was requested from participants who had consented to be contacted for possible further research.
Study groups
The first study group consisted of participants who received an mRNA-based vaccine, namely BNT162b2 or mRNA-1273, both for their primary vaccination series and for their booster vaccination (homologous booster vaccination group). The second study group consisted of lactating women who completed a primary series of an adenoviral vector-based COVID-19 vaccine which included either two doses of the AZD1222/Vaxzevria vaccine or a single dose of the Ad26.COV2.S vaccine, and for their booster vaccination, they received an mRNA-based vaccine (heterologous booster vaccination group).
Sample collection
Over a period of 16 days, participants collected eight human milk samples: one sample before and a sample on days 3, 5, 7, 9, 11, 13, and 15 after booster vaccination. All samples were collected in a standardized way. Participants were instructed to empty one breast completely before the first feeding moment, either manually or with an electric breast pump, mix the milk (so that fore- and hindmilk were mixed), and subsequently store 5 ml in the freezer until collection by one of the researchers during the home visit at the end of the follow-up period. Human milk samples were collected in sterile polypropylene tubes. During transport to the study site, milk samples were placed on dry ice and at the study site, samples were stored at −80 °C up until analysis.
Antibody analysis in human milk
SARS-CoV-2-specific IgA and IgG antibodies in human milk were determined using an enzyme-linked immunosorbent assay with the SARS-CoV-2 spike protein. A more detailed description was also reported in our previous study19 as follows:
Soluble prefusion-stabilized S-protein of SARS-CoV-2 was generated. This protein was immobilized on a 96-well plate (Greiner, Kremsmünster, Austria) at 5 µg/mL in 0.1 M NaHCO3 overnight, followed by a 1-h blocking step with 1% casein PBS (Thermo Scientific, Waltham, MA, USA). Human milk was diluted 1:5 in 1% casein PBS and incubated on the S-protein coated plates for 2 h to allow binding. Antibody binding was measured in the human milk samples using 1:3000 diluted HRP-labeled goat anti-human IgG (Jackson Immunoresearch, West Grove, PA, USA) and 1:3000 diluted HRP-labeled goat anti-human IgA (Biolegend, San Diego, CA, USA) in casein. Healthy controls were used (of our previous study) to determine cutoff values defined as the mean plus two times the standard deviation. Sensitivity was 68% for IgA and 96% for IgG in human milk. Specificity was 99% for both IgA and IgG in human milk. All samples of human milk were analyzed as one batch at the same time. Milk samples were considered positive at an optical density 450-nm cutoff value of 0.5 for IgA in human milk (sensitivity, 68%; specificity, 99%) and 0.2 for IgG in human milk (sensitivity, 96%; specificity, 99%). All biologically independent samples were assayed in duplicate.
Statistics and reproducibility
Characteristics of participants and their infants were compared between study groups, IBM SPSS Statistics for macOS (Version 29) was used. Discrete variables are denoted by the observed number and percentages within a study group, and continuous variables are presented by mean and standard deviation after testing for normality.
Human milk antibody dynamics following COVID-19 vaccination are displayed using Graphpad Prism 9.1.0 for macOS. To assess the total antibody response after booster vaccination, we determined the area under the curve with respect to ground (AUCG), with respect to increase from mean pre-booster level (AUCI), and the area under the curve with respect to the cutoff: both the area of positive peaks (AUCPP) and the net area which subtracts the area of peaks below the cutoff (AUCNet), as described in ref. 20. The AUCs were calculated for the human milk antibody response up to 15 days after the administration of the booster dose. The mean AUCs with standard errors of the mean (SEM) and degrees of freedom (df) for both study groups were compared using an unpaired-sampled t-test, with a significance level set at a p value <0.05. GraphPad Prism version 9.1.0 for macOS was used to determine and compare the AUCs.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
Data supporting the findings of this study are included in Supplementary Data 1.
References
Hobbs, C. V. et al. Frequency, characteristics and complications of COVID-19 in hospitalized infants. Pediatr. Infect. Dis. J. 41, e81–e86 (2022).
Nachega, J. B. et al. Assessment of clinical outcomes among children and adolescents hospitalized with COVID-19 in 6 sub-Saharan African countries. JAMA Pediatr. 176, e216436 (2022).
Bachrach, V. R. G., Schwarz, E. & Bachrach, L. R. Breastfeeding and the risk of hospitalization for respiratory disease in infancy: a meta-analysis. Arch. Pediatr. Adolesc. Med. 157, 237–243 (2003).
Goldman, A. S., Chheda, S. & Garofalo, R. Evolution of immunologic functions of the mammary gland and the postnatal development of immunity. Pediatr. Res. 43, 155–162 (1998).
Collier, A. Y. et al. Immunogenicity of COVID-19 mRNA vaccines in pregnant and lactating women. J. Am. Med. Assoc. 325, 2370–2380 (2021).
Young, B. E. et al. Association of human milk antibody induction, persistence, and neutralizing capacity with SARS-CoV-2 infection vs mRNA vaccination. JAMA Pediatr. 176, 159–168 (2022).
Bates, T. A. et al. Antibody response and variant cross-neutralization after SARS-CoV-2 breakthrough infection. J. Am. Med. Assoc. 327, 179–181 (2022).
European Centre for Disease Prevention and Control. Interim Public Health Considerations for the Provision of Additional COVID-19 Vaccine Doses (ECDC, 2021).
Goldberg, Y. et al. Waning immunity after the BNT162b2 vaccine in Israel. N. Engl. J. Med. 385, e85 (2021).
Juncker, H. G. et al. Comparing the human milk antibody response after vaccination with four COVID-19 vaccines: a prospective, longitudinal cohort study in the Netherlands. EClinicalMedicine 47, 101393 (2022).
Krammer, F. SARS-CoV-2 vaccines in development. Nature 586, 516–527 (2020).
Wisnewski, A. V., Campillo Luna, J. & Redlich, C. A. Human IgG and IgA responses to COVID-19 mRNA vaccines. PLoS ONE 16, e0249499 (2021).
Sterlin, D. et al. IgA dominates the early neutralizing antibody response to SARS-CoV-2. Sci. Transl. Med. 13, eabd2223 (2021).
Henle, A. M. Increase in SARS-CoV-2 RBD-specific IgA and IgG antibodies in human milk from lactating women following the COVID-19 booster vaccination. J. Hum. Lact. https://doi.org/10.1177/08903344221134631 (2022).
Munro, A. P. S. et al. Safety and immunogenicity of seven COVID-19 vaccines as a third dose (booster) following two doses of ChAdOx1 nCov-19 or BNT162b2 in the UK (COV-BOOST): a blinded, multicentre, randomised, controlled, phase 2 trial. Lancet 398, 2258–2276 (2021).
Dingess, K. A. et al. Optimization of a human milk–directed quantitative sIgA ELISA method substantiated by mass spectrometry. Anal. Bioanal. Chem. 413, 5037–5049 (2021).
Rastawicki, W., Smietanska, K., Rokosz, N. & Jagielski, M. Effect of multiple freeze-thaw cycles on detection of IgA, IgG and IgM antibodies to selected bacterial antigens. Med. Dosw. Mikrobiol. 64, 79–85 (2012).
Narayanaswamy, V. et al. Neutralizing antibodies and cytokines in breast milk after coronavirus disease 2019 (COVID-19) mRNA vaccination. Obstet. Gynecol. 139, 181–191 (2022).
van Keulen, B. A.-O. et al. Human milk from previously COVID-19-infected mothers: the effect of pasteurization on specific antibodies and neutralization capacity. Nutrients 13, 1645 (2021).
Pruessner, J. C., Kirschbaum, C., Meinlschmid, G. & Hellhammer, D. H. Two formulas for computation of the area under the curve represent measures of total hormone concentration versus time-dependent change. Psychoneuroendocrinology 28, 916–931 (2003).
Acknowledgements
This research was funded by Stichting Steun Emma Kinderziekenhuis. M.J.v.G. acknowledges the Amsterdam Infection and Immunity Institute for funding this work under the COVID-19 Grant Number (24175).
Author information
Authors and Affiliations
Contributions
Conceptualization: S.J.M., H.G.J., B.J.v.K., and J.B.v.G. Investigation: S.J.M., H.G.J., E.J.M.R., M.J.v.G., and B.J.v.K. Visualization: S.J.M., H.G.J., and B.J.v.K. Funding acquisition: H.G.J., J.B.v.G., M.J.v.G., and B.J.v.K. Project administration: S.J.M., H.G.J., E.J.M.R., and B.J.v.K., Supervision: A.K., J.B.v.G., and B.J.v.K. Writing—original draft: S.J.M., H.G.J., and B.J.v.K. Writing—review & editing: S.J.M., H.G.J., E.J.M.R., A.K., J.B.v.G., M.J.v.G., and B.J.v.K. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Biology thanks Yarden Golan and the other, anonymous, reviewers for their contribution to the peer review of this work. Primary Handling Editor: Zhijuan Qiu.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mulleners, S.J., Juncker, H.G., Ruhé, E.J.M. et al. Comparing the SARS-CoV-2-specific antibody response in human milk after homologous and heterologous booster vaccinations. Commun Biol 6, 100 (2023). https://doi.org/10.1038/s42003-023-04455-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s42003-023-04455-4
- Springer Nature Limited