Abstract
This systematic review and meta-analysis aimed to examine the association between maternal education and completion of childhood vaccination among aged 12–23 months children in Ethiopia. Systematic review and meta-analysis. PubMed-Medline, EMBASE, SCOPUS, Global Health, and Google Scholar were searched for articles published from January 2010 to January 2020. The data extraction was reported based on the PRISMA guideline (Preferred Reporting Items for Systematic Reviews and Meta-Analysis) guidelines. We performed the I2 test and a funnel plot to assess heterogeneity and check for publication bias. We assessed 841 studies for eligibility, of which 43 studies were included in the qualitative synthesis, and 28 studies were fully accessed for meta-analysis. The overall pooled effect of this systematic review and meta-analysis demonstrated a positive association between maternal education and completion of childhood vaccination. Having a primary level of maternal education was correlated with a 1.87 times higher likelihood (95% CI 1.76–1.98) of completing childhood vaccination compared to having no education. Furthermore, attending secondary education and above was associated with a 3.47 times higher likelihood (95% CI 3.18–3.78) of completing childhood vaccination compared to having no education. This systematic review and meta-analysis study revealed that as the level of maternal education increases, the completion of childhood vaccination accelerates. Therefore, investment in maternal education should be prioritized as an intervention. Empowering mothers through education can contribute to the reduction and prevention of vaccine-preventable diseases and associated risks.
Similar content being viewed by others
Introduction
“All individuals and communities have to enjoy lives free from vaccine-preventable diseases”1. Every year vaccination saves millions of lives2. It is a fruitful, cost-effective health intervention, and with proven strategies that make it accessible to even the most hard-to-reach and vulnerable populations1,2.
Globally, vaccination prevents 2–3 million deaths each year2. In 2018, worldwide vaccination coverage for three doses of the Pentavalent vaccine was 86%1. In Africa vaccination coverage was 76% in 20153.
According to the Ethiopian Minister of Health EPI (Expanded Program Immunization) guideline, all basic vaccination coverage is having vaccinated BCG (bacillus Calmette-Guérin), Pentavalent, Polio, and Measles. In Ethiopia four out of every ten children had received basic vaccination. Based on the mini Ethiopian Demographic Health Survey (EDHS) 2019, the basic vaccination coverage had reached 43%4.
Around 19.4 million infants have not received basic vaccination Worldwide2. One in five children had not had access to vaccination in Africa5. Ethiopia is one of the top ten countries carrying the 60% world burden of unvaccinated infants2.
Vaccine-preventable diseases have been reduced drastically due to the implementation of vaccination programs in Africa5. However, vaccination coverage still has not reached the target yet. This is due to many different factors such as low health education, limited access to healthcare, and inequity in access to immunization services3,6.
In Ethiopia also, different studies showed that vaccination coverage is affected by different factors. Based on those studies, antenatal care (ANC) visits, women’s decision-making autonomy, the number of under-five children in the household, the mother’s education, and proximity to the health facility, and residence were increasingly associated with the completion of vaccination7,8,9,10.
Regarding those different studies done in Ethiopia, maternal education was the most commonly mentioned factor4,8, 11,12,13. However, there was inconsistency, and didn’t confirm whether it was a factor or not. Needs systematic review and meta-analysis for the confirmation of the association between maternal education and complete childhood vaccination must be conducted. This systematic review and meta-analysis aimed to examine the association between maternal education and completion of childhood vaccination among aged 12–23 months children in Ethiopia. The findings of this study will help policymakers, programmers, researchers, and other stakeholders to be certain and take a lesson on the issue.
Methods
This study was carried out in strict compliance with systematic review and Meta-analysis with PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-analysis) guidelines14.
Patient and public involvement
No patients or the public were involved in this review.
Search strategy
Using relevant Medical Subject Headings (MeSH) terms, a final search strategy was developed. Searches were conducted on 05 February 2020 on PubMed-Medline, EMBASE, SCOPUS, Global Health, and Google Scholar for articles published from January 2010 to January 2020 using different searching terms as shown in Table 1. Unpublished papers are also searched from different online sites such as Google. We considered reviewing articles with full PDF texts of relevant studies accessed. We also tried to contact the authors of relevant studies for missing information (Tables 1 and 2).
Selection criteria
We considered our review of all quantitative observational studies (cross-sectional, case-control, and cohort studies). The authors (Aregawi and Kisanet) screened all the titles and abstracts identified through database searches. We excluded all papers that did not fulfill the inclusion criteria. Disagreements were resolved using discussion and consensus. Papers with full text were then retrieved. We used PRISMA (preferred reporting items for systematic reviews and meta-analysis) guidelines14. Studies were eligible if: they were conducted in Ethiopia and included maternal education as a determinant of the childhood vaccination coverage in children aged 12–23 months, had full text, published from January 2010 to January 2020, written in English, and done with observational study designs. A study was excluded if: not have parameters, studies with the specific vaccines, and vaccines out of childhood vaccination.
Quality criteria
Based on the Ethiopian Minister of Health, complete vaccination means if the child took 1 dose of BCG, 3 doses of polio, 3 doses of pentavalent, 3 doses of PCV, and 1 dose of measles. We did a critical appraisal for all eligible studies to include in the meta-analysis.
Data extraction
Data were extracted from the eligible articles based on their study characteristics; including publication information (author and year of publication), study region, setting, design, period, sample size, children’s age, maternal education parameter, and vaccine types. The number of children per maternal education level, the number of children fully vaccinated per maternal education level, and the percentage of children fully vaccinated per maternal education level were extracted for data analysis. Data were sorted into the nine regional states and 2 self-administrative cities.
Risk of bias
Papers were assessed for quality and risk of bias using an adapted version of the certified “Quality Assessment Tool for Quantitative Studies” by the Effective Public Health Practice Project15,16,17. Each study was also assessed and done critical appraisal using the checklist “The Joanna Briggs Institute Critical Appraisal tools for use in JBI Systematic Reviews” according to the criteria for inclusion, describing study subjects and study setting, measuring exposure validly and reliably, identifying of confounding factor, utilizing standard criteria to measure the objective, strategies to deal with confounding, measuring outcome validly and reliably, and using appropriate statistical analysis. The articles were rated its quality as “strong”, “moderate” or “weak”18,19.
Summary measures and synthesis of results
For the meta-analysis, the independent variable maternal education variable was categorized under three categories classified as “Have no formal education/illiterate”, “primary education” and “secondary and/or higher education”. We excluded papers from the meta-analysis if they had only two categories of maternal education level (“educated and non-educated” or “illiterate and literate”), had no clear categories, and had no values for their categories.
A pooled odds ratio was determined using an Influential analysis (Fixed effect model) and random-effects model using the classified categories from each included paper20,21 as large heterogeneity was anticipated considering the differences in study characteristics, such as varied sample size, region, and settings. The analysis was performed in the R statistical software R Studio version 3.622.
Sub-category analysis was also conducted for each region of the country. The reason why we used the years between 2010 and 2020 was, that the Ethiopian Health Sector Transformation Plan introduced new policy Phase-I in 2010–2015 and phase-II from 2015 to 202023.
Forest plots were created for the “primary education” and “secondary and/or higher education” separately taking “have no education/illiterate” as a reference for both categories. And also determined the individual study odds ratios and 95% Confidence Intervals, pooled estimate, and the I2-value for testing the heterogeneity24,25.
Publication bias
Graphically using funnel plots and statistically egger tests were also conducted for both categories independently using R studio statistical software 3.6 version to assess for publication bias of the included papers26,27.
Results
Study selection
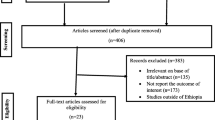
Out of 16,273 papers, 43 studies met the eligibility criteria for the qualitative synthesis of this systematic review, and 28 articles fulfilled the criteria for quantitative synthesis of meta-analysis (Fig. 1).
The main eligibility criteria for excluding the 841 papers were that they were conducted outside of Ethiopia and were irrelevant to the topic. We excluded the maternal education variable, which was classified into three categories: “illiterate/literate,” “educated/not-educated,” and “no education and primary/secondary and above,” or “primary/secondary.” Articles that had three classifications for maternal education (No education, primary education, and secondary and above) were included in the meta-analysis synthesis.
Study range and characteristics
The authors independently assessed the quality of the articles using the global score critical appraisal checklist. Twenty-one articles were rated as moderate quality, seven articles were rated as strong quality, and fifteen articles were rated as weak quality. Articles with weak quality scores were excluded from the meta-analysis (Table 3).
Among the twenty-eight articles included in the meta-analysis, the total number of children was 32,361. The sample size ranged from 248 to 8905 children, with a mean ± SD of 8905 ± 1781. (Table 4) In this study, 6503 mothers (31.4%) who had no educational status fully vaccinated their children. Among mothers with primary education, 3698 (49.6%) fully vaccinated their children. Mothers with a secondary and above level of education had fully vaccinated 2675 children (69%) (Table 4).
Data extraction and meta-analysis
The meta-analysis was conducted separately for both “primary education” and “secondary and above level of education,” with “no education” as the reference. We performed forest plots and funnel plots for both models using R-studio statistical software.
The meta-analysis revealed that children whose mothers had primary education had 1.866 times higher odds (95% CI 1.76–1.98) of receiving full childhood vaccination compared to those whose mothers had no education. Although the effect (OR) of 4 studies showed a negative association with completing vaccination (less than 1), the effect of the remaining 24 studies resulted in an OR greater than 1 (positive effect of having primary education). This resulted in a range of effects from 0.35 (0.18–0.68) to 23.19 (15.17–35.43). The effect size varied significantly among studies, with an overall I-squared value of 89.5% (p < 0.001), indicating a high level of heterogeneity among the studies (Fig. 8).
Secondly, the odds of full childhood vaccination were 3.47 times (95% CI 3.18–3.78) higher in children whose mothers had secondary education and above, compared to those whose mothers had no education. Although the effect (OR) of 4 studies showed a negative association with completing vaccination (less than 1), the effect of the remaining 24 studies resulted in an OR greater than 1 (positive effect of having primary education). This resulted in a range of effects from 0.35 (0.07–0.1.67) to 11.29 (4.73–26.9). The effect size varied significantly between studies, with an overall I-squared value of 89.8% (p < 0.001). This also indicates a high level of heterogeneity among the studies (Fig. 9).
In addition to this, the l’abbe plot showed that most of the studies were located at the top right and above the line, indicating a positive effect of maternal education on completing childhood vaccination (Figs. 9 and 10). We also conducted a funnel plot to observe publication bias, which revealed slight asymmetry among the studies. This bias may be attributed to variations in sample size. It reports Egger’s test for the primary school, t = − 0.61, df = 26, p-value = 0.5468, bias estimate: − 0.9537, SE = 1.5620; where as for the secondary school and above, t = − 1.38, df = 26, p-value = 0.0948, bias estimate: − 1.1428, and SE = 1.6395 (Fig. 9).
Sub-group analysis in regions
In the subgroup analysis, we only conducted for three regions: Oromia, Amhara, and South Ethiopia. The subgroup analysis of these regions revealed that the overall effect size was highest in the Oromia region. In this region, the odds of full childhood vaccination were 2.06 times (95% CI 1.71–2.49) higher if the mother had primary education compared to mothers with no education (Fig. 2). Additionally, the odds of full childhood vaccination were 2.84 times (95% CI 2.1–2.3.84) higher if the mother had secondary education compared to mothers with no education (Fig. 3). All studies within the Oromia region subgroup were significant, although the funnel plot indicated some slight asymmetry among the studies (Fig. 2).
The overall effect for the south region was an increased odds of 1.41 (95% CI 1.2–1.65) for completion of childhood vaccination with primary education, and an increased odds of 2.3 (95% CI 1.79–2.96) for completion of childhood vaccination with secondary and above maternal education. There were three statistically insignificant studies in the South Ethiopia subgroup. The funnel plot indicated the presence of publication bias (Figs. 4 and 5).
In the Amhara region subgroup, the association between having primary education and completing child vaccination yielded statistically insignificant results and showed low heterogeneity, with odds of 1.56 (95% CI 1.25–1.95) and a heterogeneity test I2 of 45% (Fig. 6). The overall effect for the Amhara region indicated an increased odds ratio of 1.52 (95% CI 1.25–1.86) for the completion of childhood vaccination when mothers had secondary education or above (Fig. 7). Within this subgroup, two studies were statistically insignificant about maternal education at the secondary level and above and its impact on full child vaccination (Figs. 6 and 7).
Discussion
The study aimed to examine the association between maternal education and completion of childhood vaccination among aged 12–23 months children in Ethiopia. Based on this systematic review and meta-analysis, the overall pooled effect indicates a positive association between maternal education and the completion of childhood vaccination. The primary finding of this meta-analysis is that having primary school maternal education is correlated with a 1.87 times higher likelihood (95% CI 1.76–1.98) of completing childhood vaccination compared to having no education. Additionally, the pooled effect of having a secondary and above level of education is 3.47 times higher (95% CI 3.18–3.78) than having no education. These findings suggest that as maternal education status increases, the likelihood of their children being fully vaccinated also increases. The systematic review also reveals that the percentage of children who are fully vaccinated increases progressively as the maternal education level goes from “no education” to “primary education” to “secondary and above level of education.” This highlights the importance of maternal education in ensuring the completion of childhood vaccination. Educated mothers are more likely to be aware of vaccine-preventable diseases, understand the benefits of vaccination, and ensure the timely completion of vaccinations for their children. Literature from different regions and periods also supports these assumptions50,51,52,53,54. Conversely, mothers with no education may have poor knowledge about their child’s vaccination, childcare, and overall health. Maternal education plays a crucial role in fostering a positive attitude and perception towards child health12,55,56,57,58.
The meta-analysis also examines the effect of maternal education on completing childhood vaccination across different regions of the country through subgroup analysis. While a positive association is observed in the Oromia, Amhara, and South Ethiopia regions, the strength of the effect varies across these regions. This variation may be attributed to factors such as sample size, maternal age, household income, location, accessibility to education, distance to health facilities, living standards, and other unestimated factors.
Strengths and limitations of the study
This systematic review and meta-analysis confirmed that there is a positive association between maternal education and completion of childhood vaccination in Ethiopia using R-studio statistical software.
However, this study used studies written in English only and this could potentially lead to language bias. We also included studies that had a free full PDF only, and this might have some limitations in generalization even though the authors were contacted for the raw data. We also didn’t make subgroup analyses using study year, sample size, and other variables; this is because of the problem related to the distribution of the studies with those variables (Figs. 8, 9, 10).
Conclusion
This systematic review and meta-analysis study revealed that as the maternal level of education increases the completeness of childhood vaccination accelerates. And then, investment in maternal education should be the prioritized intervention because it empowers the mother and this will help in reducing and preventing the vaccine-preventable diseases and associated risks.
Data and materials availability
All the data supporting the findings is contained within the manuscript, when there is in need the data set used for the present study’s conclusion can be accessible from the corresponding author upon reasonable request.
References
World Health Organization. Immunization, Vaccines and Biologicals. (2019).
World Health Organization. Immunization Coverage. (2019).
Mihigo, R. et al. Challenges of immunization in the African region. Pan Afr. Med. J. 27(Suppl 3), 12 (2017).
Ethiopia, C. S. A. Mini Ethiopian Demographic Health Survey. (Addis Ababa, 2019).
Addis Declaration on Immunization. Accessed 2020.
Brownwright, T. K., Dodson, Z. M. & van Panhuis, W. G. Spatial clustering of measles vaccination coverage among children in sub-Saharan Africa. BMC Public Health 17(1), 957 (2017).
Tefera, Y. A. et al. Predictors and barriers to full vaccination among children in Ethiopia. Vaccines 6(2), 22 (2018).
Wado, Y. D., Afework, M. F. & Hindin, M. J. Childhood vaccination in rural southwestern Ethiopia: The nexus with demographic factors and women’s autonomy. Pan Afr. Med. J. 17(Suppl 1), 9 (2014).
Yenit, M., Assegid, S. & Abrha, H. Factors associated with incomplete childhood vaccination among children 12–23 months of age in Machakel Woreda, East Gojjam Zone: A case-control study. J. Pregnancy Child Health 2(4), 180 (2015).
Tesfaye, T. D., Temesgen, W. A. & Kasa, A. S. Vaccination coverage and associated factors among children aged 12–23 months in Northwest Ethiopia. Hum. Vaccines Immunother. 14(10), 2348–2354 (2018).
Workina, A., Seid, S. & Moga, T. T. Reason for incomplete vaccination and associated factors among children aged 12–23 months in Serbo Town, Jimma Zone, Oromia Region, Southwest Ethiopia. Adv. Res. J. Multi-Discipl. Discov. I 32(14), 79–84 (2018).
Tesfaye, F. et al. Predictors of Immunization defaulting among children age 12–23 months in Hawassa Zuria district of Southern Ethiopia. Int. J. Public Health Sci. 3(3), 185–193 (2014).
Tessema, F. et al. Child vaccination coverage and dropout rates in pastoral and semi-pastoral regions in Ethiopia: CORE group polio project implementation areas. Ethiop. J. Health Dev. 33 (2019).
Asar, S. et al. PRISMA; preferred reporting items for systematic reviews and meta-analyses. J. Rafsanjan Univ. Med. Sci. 15(1), 68–80 (2016).
EPHPP, P. Quality assessment tool for quantitative studies. Hamilton: The effective public health practice project. URL: http://www.ephpp.ca/PDF/Quality%20Assessment. 20 (2010).
Methods, N. C. C. F. & Tools. A quality assessment tool for quantitative studies. (McMaster University Hamilton, 2008).
Thomas, H., Ciliska, D. & Dobbins, M. Quality assessment tool for quantitative studies (Effective Public Health Practice Project McMaster University, 2003).
Porritt, K., Gomersall, J. & Lockwood, C. JBI’s systematic reviews: Study selection and critical appraisal. AJN Am. J. Nurs. 114(6), 47–52 (2014).
Institute, J. B. The Joanna Briggs institute critical appraisal tools for use in JBI systematic reviews checklist for analytical cross-sectional studies. North Adelaide, Austr. Joanna Briggs Inst. (2017).
Hedges, L. V. & Vevea, J. L. Fixed-and random-effects models in meta-analysis. Psychol. Methods 3(4), 486 (1998).
Harris, R. J. et al. Metan: fixed-and random-effects meta-analysis. Stata J. 8(1), 3–28 (2008).
Gandrud, C. Reproducible research with R and R studio (CRC Press, 2013).
Health, F. D. R. O. E. M. O. HSTP health sector transformation plan 2015/16–2019/20 (2008‐2012 EFY). Federal Democratic Republic of Ethiopia Ministry of Health (2015).
Thorlund, K. et al. Evolution of heterogeneity (I2) estimates and their 95% confidence intervals in large meta-analyses. PloS One 7(7), e39471 (2012).
Pathak, M. et al. Which is the preferred measure of heterogeneity in meta-analysis and why? A revisit. Biostat. Biom. Open Access J. 1, 1–7 (2017).
Duval, S. & Tweedie, R. Trim and fill: a simple funnel-plot–based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56(2), 455–463 (2000).
Sterne, J. A. C., Becker, B. J. & Egger, M. The funnel plot. In Publication bias in meta‐analysis: Prevention, assessment and adjustments (eds Rothstein, H. R. et al.) 73–98 (Wiley, 2005). https://doi.org/10.1002/0470870168.ch5.
Bogale, T. Assessment of incomplete vaccination and associated risk factors among children under one year at Guder hospital, West Shoa zone, Oromia regional state, Ethiopia. Assessment 45 (2017).
Negussie, A. et al. Factors associated with incomplete childhood immunization in Arbegona district, southern Ethiopia: A case-control study. BMC Public Health 16(1), 27 (2015).
Yismaw, A. E. et al. Incomplete childhood vaccination and associated factors among children aged 12–23 months in Gondar city administration, Northwest, Ethiopia 2018. BMC Res. Notes 12(1), 241 (2019).
Asfaw, A. G. et al. Determinants of default to full completion of immunization among children aged 12 to 23 months in south Ethiopia: Unmatched case-control study. Pan Afr. Med. J. 23(1) (2016).
Gualu, T. & Dilie, A. Vaccination coverage and associated factors among children aged 12–23 months in Debre Markos Town, Amhara regional state, Ethiopia. Adv. Public Health 2017, 1–6 (2017).
Tamirat, K. S. & Sisay, M. M. Full immunization coverage and its associated factors among children aged 12–23 months in Ethiopia: Further analysis from the 2016 Ethiopia demographic and health survey. BMC Public Health 19(1), 1019 (2019).
Yenit, M. K., Gelaw, Y. A. & Shiferaw, A. M. Mothers’ health service utilization and attitude were the main predictors of incomplete childhood vaccination in east-central Ethiopia: A case-control study. Arch. Public Health 76(1), 14 (2018).
Lakew, Y., Bekele, A. & Biadgilign, S. Factors influencing full immunization coverage among 12–23 months of age children in Ethiopia: evidence from the national demographic and health survey in 2011. BMC Public Health 15(1), 728 (2015).
Hailu, S. et al. Low immunization coverage in Wonago district, southern Ethiopia: A community-based cross-sectional study. PloS one 14(7), e0220144 (2019).
Wassihun, B. Determinants of incomplete immunization among children age 12–23 months in Southwest, Ethiopia: Case control study.
Roy, S. G. Risk factors for childhood immunization incompletion in Ethiopia. (2010).
Birhane, M. G. N., Mekonnen, M. & Jember, A. A community-based assessment of the immunization coverage and the associated factors of children aged 12–23 months at Gondar Town, Northwest Ethiopia. (2015).
Lake, M. W. et al. Factors for low routine immunization performance: a community-based cross-sectional study in Dessie town, south Wollo zone, Ethiopia, 2014. Adv. Appl.Sci. 1(1), 7–17 (2016).
Girmay, A. & Dadi, A. F. Full immunization coverage and associated factors among children aged 12–23 months in hard-to-reach areas of Ethiopia. Int. J. Pediatr. 2019, 1–8 (2019).
Mohammed, R. T. Assessment of factors associated with incomplete immunization among children aged 12–23 months in Ethiopia. (2016).
Kassahun, M. B., Biks, G. A. & Teferra, A. S. Level of immunization coverage and associated factors among children aged 12–23 months in Lay Armachiho District, North Gondar Zone, Northwest Ethiopia: A community-based cross-sectional study. BMC Res. Notes 8(1), 239 (2015).
Mesfin, M. Incomplete vaccination and associated factors among children aged 12–23 months in Yirgalem Town, South Ethiopia. (Addis Abeba Universty, 2015).
Mekonnen, A. G., Bayleyegn, A. D. & Ayele, E. T. Immunization coverage of 12–23 months old children and its associated factors in Minjar-Shenkora district, Ethiopia: A community-based study. BMC Pediatr. 19(1), 198 (2019).
Geweniger, A. & Abbas, K. M. Childhood vaccination coverage and equity impact in Ethiopia by socioeconomic, geographic, maternal and child characteristics. Vaccine 38(20), 3627–3638 (2020).
Hagos, M. G. et al. Magnitude and associated factors of delayed immunization among children aged 11–23 months in Edagahamus town, Tigray, Ethiopia. (2018).
Legesse, E. & Dechasa, W. An assessment of child immunization coverage and its determinants in Sinana District, Southeast Ethiopia. BMC Pediatr. 15(1), 31 (2015).
Regassa, N., Bird, Y. & Moraros, J. Preference in the use of full childhood immunizations in Ethiopia: The role of maternal health services. Patient Prefer. Adher. 13, 91 (2019).
Zewdie, T. Maternal knowledge, involvement and integrative early child development programs in Ethiopia. Ethiop. J. Educ. 22(1), 57–84 (2002).
Huang, K.-Y. et al. Maternal knowledge of child development and quality of parenting among White, African-American and Hispanic mothers. J. Appl. Dev. Psychol. 26(2), 149–170 (2005).
Reich, S. What do mothers know? Maternal knowledge of child development. Infant Ment. Health J. Off. Publ. World Assoc. Infant Ment. Health 26(2), 143–156 (2005).
Sundaram, M. S., Sekar, M. & Subburaj, A. Women empowerment: Role of education. Int. J. Manag. Soc. Sci. 2(12), 76–85 (2014).
McMillin, S. E. et al. The role of maternal knowledge of child development in predicting risk for child maltreatment. Clin. Pediatr. 55(4), 374–376 (2016).
Ojobo, J. A. Education: A catalyst for women empowerment in Nigeria. Ethiop. J. Educ. Sci. 4(1) (2008).
Murphy-Graham, E. And when she comes home? Education and women’s empowerment in intimate relationships. Int. J. Educ. Dev. 30(3), 320–331 (2010).
Murtaza, K. F. Women empowerment through higher education in Gilgit-Baltistan. Int. J. Acad. Res. Bus. Soc. Sci. 2(9), 343 (2012).
Upadhyay, U. D. & Karasek, D. Women’s empowerment and ideal family size: an examination of DHS empowerment measures in Sub-Saharan Africa. Int. Perspect. Sex. Reprod. Health 38, 78–89 (2012).
Author information
Authors and Affiliations
Contributions
AG is the first author who conceptualized the study, screened articles, performed data extraction, and critical appraisal, performed statistical analysis of the data sets, and was a major contributor in writing the manuscript. KT screened articles and performed data extraction, critical appraisal, review, and editing of the manuscript. Both authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Gebreyesus, A., Tesfay, K. Effect of maternal education on completing childhood vaccination in Ethiopia: systematic review and meta-analysis. Sci Rep 14, 17453 (2024). https://doi.org/10.1038/s41598-024-68182-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-68182-4
- Springer Nature Limited