Abstract
The global trend of advanced aging comes at the cost of amplified onset of age-related diseases. Dementia is a common multifactorial age-related neurodegenerative disorder, which manifests with progressive declines in cognitive functioning and ability to perform activities of daily living. As polices discourage institutionalized care, family members act as primary caregivers and endure increased vulnerability to physical and mental health problems secondary to care-related changes in life routine and relationships. Targeting clinically significant distress at earlier stages through valid brief measures may promote caregivers’ wellbeing and dementia care continuity/quality. This study aimed to determine the optimal cutoff score of the Depression Anxiety Stress Scale 8-items (DASS-8) in a convenience sample of 571 European caregivers (Mean age = 53 ± 12 years, Italian = 74.4%, Swiss = 25.6%) through three methods. K-means clustering classified the sample into high- and low-distress clusters based on DASS-8 score of 19. Receiver operator curve (ROC) analysis using 48 and 7 cutoffs of the Zarit Burden Interview (ZBI) and the Three-Item University of California, Los Angeles, Loneliness Scale-version 3 (UCLALS3), revealed two DASS-8 cutoffs (12.5 and 14.5, area under the curve (AUC) = 0.85 and 0.92, p values < .001, 95% CI 0.82–0.88 and 0.89 to 0.94, sensitivity = 0.81 and 0.78, specificity = 0.76 and 0.89, Youden index = 0.57 and 0.67, respectively). Decision modeling produced two DASS-8 cutoffs (9.5 and 14.5) for predicting low and high caregiving burden and loneliness, respectively. According to the median of all DASS-8 cutoffs (14.5) the prevalence of mental distress was 50.8%. Distress correlated with key mental problems such as burnout and loneliness—in path analysis, DASS-8 scores were predicted by the ZBI, UCLALS3, care dependency, and receiving help with care, especially among older, female, and spouse caregivers. Further diagnostic workup should follow to confirm psycho-pathogenicity among caregivers with DASS-8 scores above 14.5. Investigations of the DASS-8 in other countries/populations may confirm the validity of this cutoff score.
Similar content being viewed by others
Introduction
By 2050, the global populations aged 65 and 80 years, in order, are expected to double and triple1,2. This unprecedented increase in life expectancy comes at the cost of amplified onset of age-related physical and mental disorders, with increasing trends toward the use of institutionalized care3. Dementia is a common age-related neurodegenerative disease, in which patients display progressive declines in cognitive functions and ability to perform activities of daily living. Because of increased risk factors (e.g., aging, lifestyle, loneliness, pollution, etc.), dementia incidence has considerably increased, and it is expected to reach 1.7 million cases in the UK by 20401,4. Older adults benefiting from nursing homes witness a twofold increase in mortality relative to counterparts living in the community2. Therefore, policy makers’ top priority is to promote older people’ s capacity to live in the community and receive advanced health care services at home3.
Dementia care is primarily provided by family members, with more than 41 million Americans acting as informal caregivers5. Dementia family caregivers struggle with the deteriorating and demanding disease of their relatives6. Physical, psychological, relational, and financial burdens endured by caregivers put them at an increased risk for psychopathology7,8,9. Around two thirds dementia caregivers experience anxiety and depression symptoms10,11. Emotional difficulties in this population are associated with numerous challenges including behavioral symptoms, long duration of being caregivers, financial constraints, lack of knowledge, communication difficulties, lack of public awareness, concerns about the selection of care facilities, providing care and decision-making, and death with dignity9,11,12. Mental distress in dementia caregivers is associated with greater levels of care burden, poor health-related quality of life, and lower resilience10,13.
Caregiving burden and distress symptoms are at their highest among those facing high-care demand10,13,14, with increased vulnerability to social isolation and loneliness among individuals spending more time in caregiving activities15,16. Loneliness is a threatening chronic source of stress, which depletes physiological buffer mechanisms such as the internal antioxidant system, resulting in accelerated oxidative and inflammatory signaling (e.g., increased production of H2O2, interleukin-6, and tumor necrosis factor-alpha)16,17. Free radicals and inflammatory cytokines trigger generalized cellular degeneration, resulting in cognitive decline, pain, fatigue, depression, anxiety, and multiple physical health problems5,17.
Physical and mental problems potentiate caregiving burden and loneliness as caregivers attempt to meet their own life responsibilities and struggle with changes in daily routine associated with prolonged caregiving5,15. Despite the enormous challenges they encounter, up to 43% of family caregivers display resilience—high levels of psychological well-being noted by ability to resist and adapt to adversities (high caregiving demands) through a range of personal strengths/assets and environmental resources), eventually leading to positive outcomes13. Particularly, positive aspects of caregiving may buffer the effect of behavioral bother on caregivers’ symptoms of depression and anxiety18. Indeed, activities focused on enhancing the coping resources of caregivers by interrupting the vicious cycle of distress/burden/loneliness (e.g., support groups) may improve their quality of life and mental wellbeing, reduce loneliness, and boost their ability to provide better care for their patients12,16,19. Thus, identifying caregivers with greater proneness to distress is pivotal for interventions that target caregiver's own intra-psychic resources, coping, and resilience to be more effective in lowering psychiatric comorbidity, which may have implications for dementia care quality and continuity10.
Using a sample of students, Lovibond and Lovibond developed the Depression Anxiety Stress Scale (DASS, 1995) as a 42-item, three-dimensional measure of three interrelated negative emotional states (depression, anxiety and tension/stress), which comprise the tripartite model of distress20. Despite its high reliability and concurrent validity (correlating with parallel measures e.g., Beck Depression Inventory and Beck Anxiety Inventory)20,21,22, investigations in clinical and nonclinical samples revealed structural issues with the DASS. Aiming to produce a cleaner factor structure and smaller inter-factor correlations, scale developers generated the DASS-21 by reducing the number of items by half20. Taking advantage of its small number of items, this short form has been frequently used in research and clinical practice to identify people with common mental disorders (anxiety and/or depression)20,21,23. Meta-analyses generally support the original three-factor structure of both DASS measures, but bifactor models show superior fit in most studies—suggesting presence of an overall negative emotion factor, denoting that a unidimensional score of the DASS may account for the overlap between depression and anxiety23,24. Additionally, the DASS-21 records inconsistent results on core psychometric properties, including invariance across genders, responsiveness, and ceiling effects23,25,26, especially when used among adolescents and children. Indeed, Rasch analysis shows that the DASS-21 features disordered categories with multiple redundant items that assess traits at analogous levels among youth27,28.
Poor response rate is common among people with mental problems29,30. Therefore, shorter scales may be favorable for eliciting higher response rates in large-scale screening31,32. Accordingly, several researchers attempted to develop briefer versions to overcome the structural shortcomings of the DASS-21 (e.g., 18-, 17-, 14-, 13-, 12-, and 9-item DASS)21,22,33,34,35, with a model developed especially for young groups, the DASS-Youth28. Studies replicating these shortened models are lacking, which limits the practicality of their use in research or clinical settings.
The DASS-8 has been introduced in the early period of the COVID-19 pandemic by a group of Arab and Japanese researchers during the testing of various structures of the DASS-21 and its shortened versions in three samples: individuals suspected of or diagnosed with COVID-19 in quarantine facilities, psychiatric outpatients, and community-dwelling adults. Items retained were those demonstrating the highest frequency of occurrence and greatest values of item-total correlations. The DASS-8 retained the three-dimensional structure of the parent DASS-21 but expressed best fit and invariance across age and gender groups26. However, the inherently unique nature of distress during the early stage of the pandemic may render scale capacity for symptom detection inaccurate in subsequent stages as well as in the general population. Accordingly, the DASS-8 was further investigated in studies comprising samples collected before the pandemic from Gana, Australia, the UK, the US, as well as samples collected during the peak of the pandemic from Italy and Switzerland36,37,38. It expressed psychometric adequacy relative to the parent scale and a 12-item form of the DASS-21 (DASS-12) regarding its factor structure, measurement invariance, convergent validity, criterion validity, discriminant validity, and reliability26,36,37,38. Principally, it differentiated women with pelvic pain and caregivers with significant levels of mental distress from those with low distress36,37. Despite its relative novelty, the DASS-8 and its subscales have been used as criterion variables in many studies recruiting patient and healthy populations. They predicted decreased sexual satisfaction in women with endometriosis39, decreased academic achievement in university student40, psychotic-like experiences41 and reduced resilience in adolescents42 as well as disordered eating43, cyber-victimization, severe insomnia44, internal shame45, irritable temperament, feeling less valued by others, perceived dark future46,47, expressive suppression, low cognitive reappraisal, poor social support48, and self-perceived temporal perspectives (the past negative, present fatalistic, present hedonistic dimensions)49 in community-dwelling adults. DASS-8 scores also mediated the effect of exposure to media violence on all subtypes of aggression50 as well as the effect of mature religiosity on problem-focused disengagement at all levels of social support51.
Although all the DASS measures are not diagnostic26,38, people with high DASS scores embrace high risk of psychiatric morbidity, which may be ascertained in sophisticated clinician-facilitated diagnostic investigations. Hence, statistically determined DASS cutoff scores may improve the practicality of applying these symptom measures in clinical settings to highlight the presence of clinically meaningful anxiety and/or depression23. While the total score of the DASS measures demonstrates good convergent validity as a screener of distress23,25,27,45, lack of established cutoff scores for identifying populations with clinically significant levels of depression/anxiety is a major flaw associated with these measures23,25. The developers suggested that the total subscale scores, which range from 0 to 42 can reflect a range of conventional symptom severity from normal (below 9, 7, and 14) to severe (above 27, 19, and 33), for the symptoms of depression, anxiety, and stress, respectively52,53. Nonetheless, cutoffs of the DASS are used inconsistently: Lee et al. used only two cutoffs (normal and ≥ mild) 53, Cao et al. used scores ≥ 5, ≥ 4, and ≥ 8 to flag clinical depression, anxiety, and stress, respectively52,54 while cutoffs ≥ 1 of the three subscales were used to predict common mental disorders in post-partum women in Malawi55—a low score that commonly occurs in people with no mental problems despite high sensitivity and specificity reported in that study. Studies investigating cutoffs of the total scale are also inconsistent. In Vietnamese women with mood disorders, the DASS-21 and combinations of its subscales (anxiety with stress or anxiety with depression) better predicted mixed mood disorders without differentiating anxiety from depressive disorders at cutoffs ranging between 24 and 3456. Cutoffs of 32, 9, 7, and 14 were reported for the DASS-21 and its subscales in Chinese patients with traumatic brain injury57. Especially, DASS-21 cutoffs varied by gender; 14 and 17 cutoffs were reported for differentiating male and female adolescents with clinical distress27. DASS-21 scores ≥ 10 indicated that the prevalence of postpartum depression in women with breast cancer was 23%: 3% lower than that revealed by Structured Clinical Interview for DSM-IV (SCID) criteria and Beck Depression Inventory58. Research documents significant discrepancies in the prevalence of clinically significant mood disorders according to the cutoff of the DASS-21 and the DASS-Youth version, suggesting a need to alter cutoffs of the DASS-2128. Moreover, sensitivity analysis indicates that most items on the anxiety dimension are not significant in identifying the presence of anxiety disorders as portrayed by SCID in patients with brain injury57 or women with mixed mood disorders56. Likewise, co-calibration of the anxiety dimension against similar measures (Hospital Anxiety and Depression-Anxiety subscale and Generalized Anxiety Disorder scale-7) in a sample of cancer patients uncovered variations in the intensity of anxiety symptoms on the three measures (the DASS-anxiety subscale had a cutoff of 3 with unacceptable values of fit indices)59. Exploratory bifactor structure of the DASS-21 (Jennrich and Bentler vs Schmid–Leiman) showed weak factorial validity of the anxiety and stress subscales22,60, prompting the researchers to report only cutoffs of the DASS-21 (at a score of 16) and the depression subscale (two or more cutoffs) for detecting mood disorders60. Wide support for the bifactor structure of the DASS measures, with a general distress factor accounting for most of the variance and trivial contribution of its dimensions, implies that scale total scores reflect a unidimensional factor of negative emotions, which accounts for the overlap between depression and anxiety22,23,24. In line, theoretical backgrounds widely accepted for the treatment of mood disorders postulate that a superordinate temperamental trait of negative affect exists in both anxiety and depression, while lack of positive affect distinguishes unipolar depression from anxiety disorders60. Therefore, a well-validated, meaningful single cutoff of briefer versions of the DASS measure may support effective screening of psychological distress in large populations23,24,28, given their support for higher response rates22. To our knowledge, none of the shortened versions of the DASS-21 has been subjected to statistical investigations of its cutoffs except for the DASS-861. Nonetheless, data were outdated (collected nine years before the study), and all predictors were examined by self-reported single-item questions, necessitating further validation of its cutoff62,63,64,65. Consequently, this study aimed to investigate cutoffs of the DASS-8 among dementia family caregivers basing its diagnostic potentials on predictors of caregiving burden and loneliness—common psychological problems closely associated with mental distress. Given the ominous effects of caregiving burden and loneliness, the resulting cutoff scores may be helpful for identifying caregivers vulnerable to psychiatric morbidity and in need of clinical help.
For a single measure, arbitrary cutoffs may result from arbitrary statistical methodologies, ranging from measures of variable distribution (e.g., means and medians) to machine learning models63. Clustering, an unsupervised multi-step learning technique, divides data into distinct groups with a high degree of inter-group similarity based on uncovered characteristics. In the initial stages, it detects and generates groups through a sequential approach, which pre-clusters cases and/or variables according to a distance measure that defines dense regions in the analyzed attribute-space. Then, it uses a probabilistic approach to statistically select and merge pre-clusters stepwise until the optimal subgroup model is determined, resulting in few non-overlapping groups62,64,66. Receiver operating characteristic (ROC) curve analysis is a valuable computational method, which aids in evaluating and comparing the diagnostic or prognostic accuracies of quantitative tests by determining clinically relevant cutoff scores—when a specific outcome has two possible endpoints, it classifies people as ‘‘positive’’ for this outcome63,64. ROC curve visualizes the diagnostic/prognostic possibilities of respective measures prior to categorization. It plots all potential cutoffs of binary tests that can be made from the continuously distributed values, with each value generating a point on a curve that stars at coordinates X0;Y0, goes vertically up the Y-axis and then horizontally across to coordinates X1;Y163. The relationship between true and false positives is displayed, with true positivity (sensitivity) plotted against false positivity (1-specificity) for a chosen clinically relevant binary outcome on the curve65. Accurate cutoffs are noted by deviation of the ROC curve closer to the ‘‘optimal’’ upper-left handed corner, with larger area under the ROC curve (AUC)60,63,65. The diagnostic performance of a test variable is decided based on values of the AUC, sensitivity, specificity, and Youden index (J: (sensitivity + specificity) – 1)65. They should be closer to 1 in ideal tests, with a narrow 95% confidence interval (CI) for AUC values, which are persistently < 0.05. On the contrary, ROC curves run diagonally and have low fit indices in equally random tests, which comprise variables with no diagnostic/prognostic values63,64. Decision trees are machine learning techniques that set tree-like models that classify data into categories according to the target variables by exploring hidden patterns within the data. The model is inversely created with the root at the top with many branches downwards determined by a series of splits (internal nodes) based on conditions defined for the predictor variables. Branches, which end with child nodes (leaves), determine a decision. Criteria for the stop of tree growth may be chosen as either the longest path length from the root to a child node or by selecting a minimum number of training inputs for each child node62,64. The DASS-8 was tested through the three techniques in the current analysis.
Material and methods
Study design, participants, and procedure
This cross-sectional instrumental study comprised a convenience sample of 571 dementia family caregivers (mean age = 53 ± 12, range = 24–89 years) from northern Italy (74.4%) and southern Switzerland (25.6%). Caregivers were primarily females (n = 466, 81.6%) and adult children of care recipients (n = 410, 71.8%). Half the caregivers were employed (part-time or full time: n = 283, 49.6%), and most caregivers attained upper secondary education (n = 322, 56.4%). Care recipients had primarily Alzheimer’s disease (n = 316, 55.3%) and were dependent for activities of activities of daily living (ADL; n = 455, 79.7%). More details on the characteristics of the participants are available elsewhere36,67. Data were collected between May 25th and June 25th, 2020, through an online survey conducted via RedCap. The participants signed a digital informed consent before completing the test battery.
Measures
The questionnaire administered to the participants was in the Italian language, and it contained questions about their sociodemographic characteristics (e.g., age, gender, education, etc.), relationship with care recipients (adult children or spouses), receiving help with caregiving (yes or no e.g., from another family member, neighbor, or a paid caregiver), type of dementia, and the level of care recipient dependency for ADL (autonomous or not autonomous). The test battery comprised three measures:
-
1.
The Depression Anxiety Stress Scale-8 (DASS-8) comprises 8 items in three subscales, which capture depression, anxiety, and stress symptoms. The stress subscale comprises two items “e.g., I was using a lot of my mental energy” while each of the depression and anxiety subscales comprises three items “e.g., I felt that I had nothing to look forward” and “e.g., I felt close to panic”, respectively. The respondents rate the frequency of endorsing the items of the DASS-8 over the past week on a scale of four response categories ranging from 0 (did not apply to me at all) to 3 (applied to me very much or most of the time). Our respondents were instructed to rate their symptoms over the last month for better detection of their distress during the peak of the COVID-19 pandemic (the time of data collection)67. The total scores of the DASS-8 and its depression, anxiety, and stress subscales range between 0 (all the measures) and 24, 9, 9, and 6, respectively26,38. Its reliability in this study is excellent (coefficient alpha = 0.93).
-
2.
The Zarit Burden Interview (ZBI)68 comprises 22 items, which capture caregiving burnout: adverse effects of caring for a patient with dementia on caregivers’ physical and mental health, quality of life, relationships, and finance14. Example items include “feel strained, feel angry, social life suffering, financial stress, health affected, and lack privacy”. Respondents rate the frequency of endorsing items of the ZBI on a five-point Likert scale ranging from 0 (never) to 4 (nearly always). The total scores of the ZBI range between 0 and 88. Higher scores reflect greater burden68,69. Its reliability in this study is excellent (coefficient alpha = 0.94).
-
3.
The Three-Item Loneliness Scale is a brief measure, which has been developed as a refinement of the University of California, Los Angeles, Loneliness Scale-version (UCLALS), herein referred to as UCLALS368,70. It comprises three items “e.g., how often do you feel that you lack companionship”. Items are rated on a three-point scale ranging from 1 (hardly ever) to 3 (often). The total scores of the UCLALS3 range between 3 and 9. Higher scores indicate greater loneliness70. Its reliability in this study is very good (coefficient alpha = 0.87).
Statistical analysis
Quartile scores of the DASS-8 were calculated to determine its initial cutoff scores. In K-means clustering analysis, the participants were located into non-overlapping clusters based on the scores of the DASS-8 and its subscales37. Decision tree and ROC analyses were conducted using the continuous scores of the DASS-8 to predict caregiving burden and loneliness, which were both used as categorical variables. ZBI categories were created based on the cutoff (48) reported for predicting depression and anxiety among family caregivers of patients with schizophrenia71. Because we found no cutoff score of the UCLALS3, we created its categorical form using the median (7), which can be acceptable for setting thresholds that reflect variable distribution65. This method does not eliminate uncertainty in time-to-event endpoints of the outcome of interest63 unlike advanced techniques (e.g., ROC analysis and decision trees), which employ optimal separation between groups concerning some outcomes. However, it was not possible to use these techniques to examine the UCLALS3 because of lack of predictor variables required for these tests62,63, which also fall beyond the scope of this study. In ROC analysis, DASS-8 cutoffs were selected based on fit indices discussed above64,71,72. In decision tree analysis, we employed the classification and regression (CRT) growing method with the validation method of random assignment of cases into training and test samples (70 and 30% of cases, respectively)64. The test sample acts as a source of prior probabilities of group membership. Prior probabilities are estimates of the overall relative frequency for each category of the dependent variable prior to knowing anything about the values of the independent (predictor) variables. They aid in minimizing tree growth caused by data in samples that are not representative of the entire population73.
Apart from cutoff score analyses, a general path model was used to investigate whether the DASS-8 can reflect burnout and distress. Predictors in the model comprised the ZBI, UCLALS3, and sociodemographic characteristics of the respondents. We trimmed nonsignificant paths. Model fit was considered good based on a non-significant χ2, along with discrepancy divided by degree of freedom (CMIN/DF) < 3, Comparative Fit Index (CFI) and Tucker–Lewis Index (TLI) > 0.95, standardized root-mean-square residual (SRMR), and root mean square error of approximation (RMSEA) < 0.0674,75. The analyses were performed in IBM SPSS Statistics (version 28) and IBM Amos Statistics (version 24). Significance was considered at a probability < 0.05 in two-tailed tests.
Ethics approval and consent to participate
The study was conducted according to the Declaration of Helsinki. The protocol for data collection has been approved by the Italian and Swiss Cantonal ethics committee67, and no further ethical approval was obtained because the study does not fall within the scope of Art 2 and Art 3 of the law on human research. The dataset generated is shared under the terms of Creative Common License (CC BY 4.0)76. Accordingly, no ethical approval was attained for the current secondary analysis.
Results
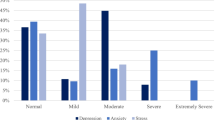
The mean scores of the DASS-8, ZBI, and UCLALS3 were 13.6 ± 6.9, 54.3 ± 18.3, and 6.8 ± 2.1, respectively. The quartile scores of the DASS-8 were 8.0, 15.0, and 19.0. Clustering analysis classified caregivers into two clusters reflecting low (n = 271) and high (n = 300) levels of distress. Cutoff scores of the DASS-8, depression, anxiety, and stress subscales that were used to locate the participants into clusters were 19.0, 7.0, 7.0, and 5.0, respectively (Fig. 1). ANOVA test shows that the differences between clusters were significantly maximized (F(212) = 536.83, 246.19, 316.57, and 227.89; all p values < 0.001).
Based on the ZBI cutoff, ROC-curve criteria (AUC = 0.85, SE = 0.02, p < 0.001, 95% CI 0.82 to 0.88, sensitivity = 0.81, specificity = 0.76, Youden index = 0.57) show that DASS-8 cutoff of 12.5 can discriminate caregivers with high and low caregiving burden. Based on the UCLALS3 cutoff, ROC-curve criteria (AUC = 0.91, SE = 0.01, p < 0.001, 95% CI 0.89 to 0.94, sensitivity = 0.78, specificity = 0.89, Youden index = 0.67) show that DASS-8 cutoff of 14.5 can discriminate caregivers with high and low loneliness (Fig. 2).
Receiver-operating characteristic (ROC) curve using the scores of the Depression Anxiety Stress Scale 8 (DASS-8) to classify dementia family caregivers according to their levels of caregiving burden (Zarit Burden Interview (ZBI), a) and loneliness (University of California, Los Angeles, Loneliness Scale-version 3 (UCLALS3), b).
Decision tree analysis indicated that 9.5 DASS-8 cutoff may distinguish between caregivers with high and low burden (Fig. 3a,b). However, higher cutoffs (16.5 and 19) demonstrated a greater probability of prediction. Consistent with ROC analysis, decision modeling indicated that 14.5 DASS-8 cutoff may efficiently predict loneliness (Fig. 3c,d). However, the probability of prediction was greater at higher scores (e.g., 18.5 and 21.5).
To determine a single optimal cutoff score of the DASS-8, cutoffs obtained from all analyses were ordered ascendingly (9.5, 12.5, 14.5, 14.5, 15.0, 19.0). The value in the middle was chosen (14.5) as an optimal cutoff in this sample.
The path model expressed excellent fit (χ2 = 11.89, df = 11, p = 0.3, CMIN/DF = 1.08, CFI = 0.999, TLI = 0.998, RMSEA = 0.012, RMSEA 95% CI 0.000 to 0.046, SRMR = 0.026). It predicted 71% of the variance in psychological distress. Because non-significant paths were trimmed, all direct relations in Fig. 4 are significant. Loneliness and caregiving burden predicted 51 and 47% of the variance in the DASS-8, respectively (p values < 0.001). Loneliness predicted 51% of the variance in caregiving burden, and it expressed an indirect effect on distress through caregiving burden (β = 0.238, 95% CI 0.204 to 0.278, p = 0.011).
Path analysis model predicting scores of the Depression Anxiety Stress Scale 8 (DASS-8) based on the continuous scores of the Zarit Burden Interview (ZBI), the University of California, Los Angeles, Loneliness Scale-version 3 (UCLALS3), and the sociodemographic characteristics of dementia family caregivers.
Age directly predicted loneliness and caregiving burden (p = 0.001 and 0.020). While its direct effect on distress was negative (p = 0.036), it expressed a positive indirect effect on distress through caregiving burden (β = 0.120, 95% CI 0.057 to 0.173, p = 0.012). Gender was a strong direct predictor of loneliness and caregiving burden (both p values = 0.004). Mann Whitney U test revealed greater levels of loneliness (U = 17,952.0, z = − 4.21, p < 0.001) and caregiving burden (U = 15,431.5, z = -5.81, p < 0.001) among females. Although gender had no direct effect on distress, it exerted significant positive indirect effects on distress through loneliness (β = 0.131, 95% CI 0.086 to 0.185, p = 0.012) and caregiving burden (β = 0.059, 95% CI 0.031 to 0.086, p = 0.020). Receiving help with caregiving negatively predicted caregiving burden and loneliness (p values < 0.001). It positively predicted distress (p = 0.034), but its indirect effects on caregiving burden and distress were negative (β = − 0.107 and − 0.228, 95% CI − 0.140 to − 0.068 and − 0.281 to − 0.161, p values = 0.012).
ADL dependency negatively predicted caregiving burden and loneliness (Fig. 4, p = 0.048 and 0.002) without a direct effect on distress. It exerted significant indirect effects on distress (β = − 0.120, 95% CI − 0.189 to − 0.066, p = 0.006) and caregiving burden (β = − 0.062, 95% CI − 0.106 to − 0.029, p = 0.008). Distress scores were significantly greater among those caring for ADL-dependent patients compared with those who cared for ADL-autonomous patients36. Caregivers’ relationship with care recipients negatively predicted caregiving burden (Fig. 4, p = 0.019). Spouses had greater caregiving burden (U = 17,172.5, z = − 4.81, p = 0.001) and loneliness scores (U = 18,013.5, z = − 4.31, p = 0.001) compared with adult-children. However, distress scores were significantly greater among adult children relative to spouses36.
Discussion
Caring for demanding, chronic conditions such as dementia can deplete caregivers’ emotional resources, resulting in poor mental and physical health10,13. Quick screening for distress may be a cost-effective method for early detection and treatment of psycho-pathogenicity among caregivers7,8,16. In practice, cutoffs of continuous measures represent a straightforward method for classifying individuals as “positive or high risk” and “negative or low risk” for specific conditions. A single study testing DASS-8 cutoffs revealed an array of scores, which predicted miscellaneous outcomes in women with chronic pelvic pain61. To provide unbiased, statistically-established optimal cutoff of the DASS-8, the current study comes in concordance with calls for testing measures using several robust strategies62,63,64 in different independent datasets (herein dementia caregivers) to minimize risk bias and type-I error65. Many cutoffs of the DASS-8 emerged in our analyses (clustering, ROC analysis, and decision tree). Referring to the literature64,65, a single optimal cutoff was defined by choosing the median of all the resulting cutoffs. Accordingly, caregivers with DASS-8 scores above 14.5 should undergo advanced investigations for psychiatric problems.
Previous research has examined cutoffs of the DASS-21 in different populations. Given the dearth of studies investigating cutoffs of the DASS-8, herein, we take advantage of the fact that AUC values as general calculations of the global diagnostic accuracy of measures may aid in general comparisons of two or more diagnostic tests60. Our values of AUC, Youden index, sensitivity, and specificity indices show comparable or even greater global diagnostic accuracy of the cutoff of the DASS-8 relative to the parent scale—suggesting that not too many false-negative or false positive cases may emerge at a DASS-8 cutoff of 14.5. For example, DASS-21 cutoffs of 10, 16, and 34 (AUC values = 0.81, 0.67, and 0.81) predicted mental health problems in Arab women with breast cancer58, healthy students from the USA60, and women with mood disorders from rural Vietnam56, respectively. In this sense, our results supplement existing knowledge, which may employ the cutoff of the DASS-21 as a beneficial component of an actuarial decision-making strategy within the context of stepped healthcare delivery system—by defining individuals in need for additional psychiatric evaluations60.
Unlike previously reported cutoff scores for the DASS-8, clustering analysis defining groups based on solo differences in the DASS-8 and its subscales, in the absence of external predictor variables, distinguished two clusters of caregivers based on a DASS-8 score of 19. This score corresponds to the third quartile score of the DASS-8. However, different cutoffs appeared in tests using burnout and loneliness as outcome measures. These scores are consistent with previously recorded cutoffs of the DASS-8. Particularly, ROC analysis revealed significant burnout and loneliness at DASS-8 cutoffs of 12.5 and 14.5 with AUC values of 0.85 and 0.92, respectively. The same DASS-8 cutoffs, in order, previously predicted intake of over-the-counter medicine and high vs low distress in women with pelvic pain61. The present values of AUC and Youden index were greater in the model predicting loneliness—denoting greater diagnostic potentials of the DASS-8 14.5 than 12.5 cutoff64. This score was closer to the median of the DASS-8 (15.0). Median scores represent a plain high vs low distress threshold65. Indeed, the median of the DASS-21 successfully differentiated women diagnosed with depression or anxiety disorders from healthy counterparts56. Decision tree modeling shows that the DASS-8 at a score of 9.5 may discriminate people with high and low caregiving burden. The same DASS-8 score predicted self-reported psychiatric comorbidity in women with chronic pelvic pain61. Interestingly, decision tree and ROC analyses predicting loneliness produced DASS-8 cutoffs with similar values, implying robust applicability of the finally defined cutoff64. Given greater diagnostic accuracy of the narrow range of the DASS-8 cutoffs seen in the present and previous investigations relative to the considerably wide range of cutoffs (10 to 34) of the DASS-21, the DASS-8 may be more acceptable as a simple measure of distress symptoms.
It is worth mentioning that the probability of prediction in both decision tree models increased at higher scores (16.5 and 19 for burnout; 18.5 and 21.5 for loneliness). Evidently, those higher scores were closer to the score produced in clustering analysis and the third DASS-8 quartile score. Thus, they may correspond to higher degrees of severity (severe or extremely severe distress). Similarly, scores below the first quartile may reflect normal/mild distress63. However, this is not the scope of this study, which aims to determine an optimal cutoff: a single diagnostic score that can distinguish subjects as high and low on the measurement at hand without interest in defining different degrees of severity (e.g., low, mild, moderate, high, severe/extremely severe)64. Further investigations may examine multiple levels of distress captured by the DASS-8.
The DASS-8 is a brief measure, which can be easily self-applied to elicit a greater response rate. Its ability to predict higher loneliness and caregiving burden signifies that higher DASS-8 scores may also reflect greater loneliness and burnout, even without measuring these outcomes directly. To test this hypothesis, we ran a path model to see if DASS-8 scores reflect the distressing psychological experiences of loneliness and caregiving burden among dementia caregivers. As expected, greater distress appeared as an outcome of higher scores of loneliness and caregiving burden. The model included caregivers’ sociodemographic characteristics, which operated interweavingly to affect loneliness, burnout, and distress. Not surprisingly, care recipients’ ADL dependency was a source of greater caregivers’ distress. Meanwhile, receiving help with caregiving was associated with a significant direct and indirect reduction in caregiving burden along with a direct increase and indirect decrease in distress scores. Group comparisons revealed greater loneliness (U = 27,758.5, z = − 6.18, p = 0.001) and lower caregiving burden (U = 24,140.5, z = − 7.93, p = 0.001) among those who received help than those who did not. Given the mediating role of caregiving burden and loneliness on the effect of receiving help on distress, it seems that lonely caregivers’ tendency to seek assistance with caregiving may reduce their burden and indirectly reduce their distress, but it does not totally free them from mental distress. This might be attributed to doing more effort to secure the availability of an alternative caregiver during COVID-19’s periods of lockdowns, which witnessed extensive social isolation, global economic recession, dramatic loss of employment, and rise in prices36,77. The cost of respite care, which on average exceeds one quarter of the income of family caregivers, is another documented source of distress9. Likewise, depression in caregivers of people with Alzheimer's disease is associated with increased numbers of caregivers11. Same as in caregivers of people with Alzheimer's disease, being a spouse was associated with greater loneliness and burnout11. Possibly because of their advanced age, spouses had extended duration of caregiving (r = 0.257, p < 0.001), which is further associated with caregiving burden, loneliness, and distress (r = 0.350, 0.290, and 0.393; p values < 0.001). This coincides with higher levels of loneliness and burnout among older participants (Fig. 4). In line, caregivers of people with Alzheimer's disease who were caregivers for longer durations displayed elevated levels of caregiving burden and anxiety11. Loneliness expressed a significant indirect positive effect through caregiving on distress. Research suggests a bidirectional relationship between loneliness and negative emotional conditions (major depression and generalized anxiety disorders, sadness, and stress)78,79. However, longitudinal data show that elevated levels of loneliness predict more severe symptoms of social anxiety and depression over time78,79. Taken together, our findings imply that younger caregivers (who were predominantly middle-aged) are less prone to distress as a function of their own capacity to provide care more efficiently and keep themselves less lonely than older counterparts. In support, research reports higher caregiving burden and loneliness in older adults relative to middle-aged caregivers15. Although gender had no direct effect on distress, females displayed greater caregiving burden and loneliness. Gender indirectly increased distress through caregiving burden and loneliness. In summary, high distress scores reflect greater loneliness, caregiving burden, ADL-dependency, being involved in care for relatively long durations, and greater need for help with caregiving, especially among older, female, and spouse caregivers. These specific groups of caregivers have been previously reported to struggle with higher levels of distress7,80,81,82. Thanks to its brevity, use of the DASS-8 for frequent screening may allow practitioners to be more specific and effective in detecting caregiver distress, especially within groups with identified risk for burden and loneliness.
One merit of this study is analyzing publicly accessible data through robust techniques (ROC analysis and decision modeling) to determine an optimal cutoff of the DASS-8 that may effectively predict critical mental health-related problems (caregiving burden and loneliness) in a highly vulnerable population. Decision tree analysis employed a validation method: 70 and 30% of the participants were simultaneously located into training and test samples, which permits accounting for variations related to the data in the samples64. Our study has clinical and research implications. The results show that distress in dementia caregivers is a direct and indirect function of loneliness and caregiving burden, along with their interaction with a variety of demographic and clinical variables. Therefore, higher DASS-8 scores (14.5 and above) may reflect loneliness, burnout, ADL-dependency, and need for help with caregiving, especially among female, older, and spouse caregivers who represent targets for the detection and treatment of psychiatric morbidities. The results should be interpreted with caution, because the study has limitations. Online surveying, convenience sampling, and cross-sectional design entail risks for selection and reporting bias. Because comorbidities are associated with lowered resilience and increased proneness to psycho-pathogenicity77, our respondents should have been screened for mental problems (e.g., mixed mood disorders) through clinician-based interviews or through other measures of distress, depression, and anxiety to validate the cutoff scores. However, this was not possible since the analyses used a public dataset. Accordingly, lack of assessment of the history of mental and physical illness in the sample may confound the results. Alternatively, the analysis involved already available measures of closely linked constructs (burnout and loneliness)5,15, which may lend some support to the credibility of our results, albeit they are still not doubt-free. Moreover, loneliness and burnout were included in path model as observed variables. Assuming absence of measurement error does not provide closer-to-reality results as when latent variables are tested. Additionally, the direction of relations revealed in path analysis may not reflect the reality given the cross-sectional nature of the data. Data were collected during the peak of the COVID-19 from a border area involving north Italy and south Switzerland. In the meantime, our variables (e.g., loneliness and distress) occur at greater rates in individualistic cultures (e.g., Europe), which focus primary on individuals' interests rather than group norms and social connections15,38. Therefore, data and characteristics of our subjects may diverge from those found in other areas and time points. The questionnaires were addressed in Italian assuming that all the respondents could fluently speak Italian, but this assumption was not proved by inquiring about the level of fluency. Consequently, further examinations in populations from different cultural backgrounds may ensure the reliability of the reported cutoffs.
Conclusion
Different statistical methods indicate usefulness of the DASS-8 at a score of 14.5 for predicting high burnout and loneliness among dementia caregivers. Referring caregivers with higher DASS-8 score, especially females, elderly, and spouses, for advanced assessment and treatment of psychiatric comorbidities may promote their wellbeing and care continuity. Replications of the study in other countries may confirm the findings.
Data availability
The dataset supporting the conclusions of this article is available in Zenodo repository, [https://zenodo.org/record/4748652#.YdbwiWhBw2w]76, and also the datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Chen, Y. et al. Dementia incidence trend in England and Wales, 2002–19, and projection for dementia burden to 2040: Analysis of data from the English Longitudinal Study of Ageing. Lancet Public Health 8, e859–e867. https://doi.org/10.1016/s2468-2667(23)00214-1 (2023).
Boucaud-Maitre, D. et al. Comparison of mortality and hospitalizations of older adults living in residential care facilities versus nursing homes or the community. A systematic review. PLoS ONE 18, e0286527. https://doi.org/10.1371/journal.pone.0286527 (2023).
Chang, M. et al. Trends in the use of home care services among Norwegians 70+ and projections towards 2050: The HUNT study 1995–2017. Scand. J. Caring Sci. 37, 752–765. https://doi.org/10.1111/scs.13158 (2023).
Ali, A. M. & Kunugi, H. Royal jelly as an intelligent anti-aging—a focus on cognitive aging and Alzheimer’s disease: A review. Antioxidants 9, E937. https://doi.org/10.3390/antiox9100937 (2020).
Perez, S. G., Nuccio, A. G. & Stripling, A. M. A rapid review of the detrimental impact of loneliness and social isolation in caregivers of older adults. Am. J. Geriatr. Psychiatry 29, S122–S123. https://doi.org/10.1016/j.jagp.2021.01.117 (2021).
Borelli, W. V. et al. Neuropsychiatric symptoms in patients with dementia associated with increased psychological distress in caregivers during the COVID-19 pandemic. J. Alzheimers Dis. 80, 1705–1712. https://doi.org/10.3233/jad-201513 (2021).
Wawrziczny, E., Duprez, C. & Antoine, P. Predictors of caregiver distress among spouses, adult children living with the person with dementia, and adult children not living with the person with dementia. Psychogeriatrics 20, 594–601. https://doi.org/10.1111/psyg.12553 (2020).
Cohen, G., Russo, M. J., Campos, J. A. & Allegri, R. F. Living with dementia: increased level of caregiver stress in times of COVID-19. Int. Psychogeriatr. 32, 1377–1381. https://doi.org/10.1017/s1041610220001593 (2020).
Mage, S. et al. “I Lay Awake at Night”: Latino family caregivers’ experiences covering out-of-pocket costs when caring for someone living with dementia. Gerontologist 64, gnad011. https://doi.org/10.1093/geront/gnad011 (2023).
Durán-Gómez, N. et al. Understanding resilience factors among caregivers of people with Alzheimer’s disease in Spain. Psychol. Res. Behav. Manag. 13, 1011–1025. https://doi.org/10.2147/prbm.s274758 (2020).
Lou, Q. et al. Comprehensive analysis of patient and caregiver predictors for caregiver burden, anxiety and depression in Alzheimer’s disease. J. Clin. Nurs. 24, 2668–2678. https://doi.org/10.1111/jocn.12870 (2015).
Han, S. et al. Adapting the resilience framework for family caregivers of hospice patients with dementia. Am. J. Alzheimers Dis. Other Demen. 34, 399–411. https://doi.org/10.1177/1533317519862095 (2019).
Joling, K. J. et al. Factors of resilience in informal caregivers of people with dementia from integrative international data analysis. Dement. Geriatr. Cogn. Disord. 42, 198–214. https://doi.org/10.1159/000449131 (2016).
Khatatbeh, H., Al-Dwaikat, T., Alfatafta, H., Ali, A. M. & Pakai, A. Burnout, quality of life and perceived patient adverse events among paediatric nurses during the COVID-19 pandemic. J. Clin. Nurs. https://doi.org/10.1111/jocn.16540 (2022).
Barreto, M. et al. Loneliness around the world: Age, gender, and cultural differences in loneliness. Pers. Individ. Diff. 169, 110066. https://doi.org/10.1016/j.paid.2020.110066 (2021).
Velloze, I. G., Jester, D. J., Jeste, D. V. & Mausbach, B. T. Interventions to reduce loneliness in caregivers: An integrative review of the literature. Psychiatry Res. 311, 114508. https://doi.org/10.1016/j.psychres.2022.114508 (2022).
Pourriyahi, H., Yazdanpanah, N., Saghazadeh, A. & Rezaei, N. Loneliness: An immunometabolic syndrome. Int. J. Environ. Res. Public Health 18, 12162 (2021).
Cheng, S.-T. Positive aspects of caregiving attenuate the relationship between behavioral bother and anxiety and depressive symptoms in dementia family caregivers. Geriatr. Gerontol. Int. 23, 366–370. https://doi.org/10.1111/ggi.14581 (2023).
McRae, C. et al. Predictors of loneliness in caregivers of persons with Parkinson’s disease. Parkinsonism Relat. Disord. 15, 554–557. https://doi.org/10.1016/j.parkreldis.2009.01.007 (2009).
Lovibond, S. H. & Lovibond, P. F. Depression Anxiety Stress Scales (DASS–21, DASS–42) [Database record]. APA PsycTests. https://doi.org/10.1037/t01004-000 (1995).
Ali, A. M. & Green, J. Factor structure of the depression anxiety stress Scale-21 (DASS-21): Unidimensionality of the Arabic version among Egyptian drug users. Subst. Abuse Treat. Prev. Policy 14, 40. https://doi.org/10.1186/s13011-019-0226-1 (2019).
Osman, A. et al. The Depression Anxiety Stress Scales-21 (DASS-21): Further examination of dimensions, scale reliability, and correlates. J. Clin. Psychol. 68, 1322–1338. https://doi.org/10.1002/jclp.21908 (2012).
Lee, J., Lee, E. H. & Moon, S. H. Systematic review of the measurement properties of the Depression Anxiety Stress Scales-21 by applying updated COSMIN methodology. Qual. Life Res. 28, 2325–2339. https://doi.org/10.1007/s11136-019-02177-x (2019).
Yeung, A. Y., Yuliawati, L. & Cheung, S.-H. A systematic review and meta-analytic factor analysis of the depression anxiety stress scales. Clin. Psychol. Sci. Pract. 27, e12362. https://doi.org/10.1111/cpsp.12362 (2020).
Page, A. C., Hooke, G. R. & Morrison, D. L. Psychometric properties of the Depression Anxiety Stress Scales (DASS) in depressed clinical samples. Br. J. Clin. Psychol. 46, 283–297. https://doi.org/10.1348/014466506x158996 (2007).
Ali, A. M., Alkhamees, A. A., Hori, H., Kim, Y. & Kunugi, H. The Depression Anxiety Stress Scale 21: Development and validation of the Depression Anxiety Stress Scale 8-item in psychiatric patients and the general public for easier mental health measurement in a post-COVID-19 world. Int. J. Environ. Res. Public Health 18, 10142. https://doi.org/10.3390/ijerph181910142 (2021).
Evans, L., Haeberlein, K., Chang, A. & Handal, P. An evaluation of the convergent validity of and preliminary cutoff scores for the DASS-21 total score as a measure of distress in adolescents. Curr. Psychol. 41, 4283–4290. https://doi.org/10.1007/s12144-020-00937-4 (2022).
Cao, C.-H. et al. Evaluating the psychometric properties of the Chinese Depression Anxiety Stress Scale for Youth (DASS-Y) and DASS-21. Child Adolesc. Psychiatry Ment. Health 17, 106. https://doi.org/10.1186/s13034-023-00655-2 (2023).
Butterworth, P., Watson, N. & Wooden, M. Trends in the prevalence of psychological distress over time: Comparing results from longitudinal and repeated cross-sectional surveys. Front. Psychiatry 11, 595696. https://doi.org/10.3389/fpsyt.2020.595696 (2020).
Long, A. C. et al. Understanding response rates to surveys about family members’ psychological symptoms after patients’ critical illness. J. Pain Symptom Manag. 54, 96–104. https://doi.org/10.1016/j.jpainsymman.2017.02.019 (2017).
Cheah, J.-H., Sarstedt, M., Ringle, C. M., Ramayah, T. & Ting, H. Convergent validity assessment of formatively measured constructs in PLS-SEM. Int. J. Contemp. Hosp. Manag. 30, 3192–3210. https://doi.org/10.1108/IJCHM-10-2017-0649 (2018).
Mund, M. et al. Would the real loneliness please stand up? The validity of loneliness scores and the reliability of single-item scores. Assessment https://doi.org/10.1177/10731911221077227 (2022).
Wise, F. M., Harris, D. W. & Olver, J. H. The DASS-14: Improving the construct validity and reliability of the depression, anxiety, and stress scale in a cohort of health professionals. J. Allied Health 46, e85–e90 (2017).
Oei, T. P. S., Sawang, S., Goh, Y. W. & Mukhtar, F. Using the Depression Anxiety Stress Scale 21 (DASS-21) across cultures. Int. J. Psychol. https://doi.org/10.1080/00207594.2012.755535 (2013).
Lee, E. H. et al. The 21-item and 12-item versions of the Depression Anxiety Stress Scales: Psychometric evaluation in a Korean population. Asian Nurs. Res. (Korean Soc. Nurs. Sci.) 13, 30–37. https://doi.org/10.1016/j.anr.2018.11.006 (2019).
Ali, A. M. et al. Psychometric evaluation of the depression anxiety stress scale 8-items (DASS-8)/DASS-12/DASS-21 among family caregivers of patients with dementia. Front. Public Health 10, 1012311. https://doi.org/10.3389/fpubh.2022.1012311 (2022).
Ali, A. M. et al. Psychometric evaluation of the Depression Anxiety Stress Scale 8 among women with chronic non-cancer pelvic pain. Sci. Rep. 12, 20693. https://doi.org/10.1038/s41598-022-15005-z (2022).
Ali, A. M., Hori, H., Kim, Y. & Kunugi, H. The Depression Anxiety Stress Scale 8-items expresses robust psychometric properties as an ideal shorter version of the Depression Anxiety Stress Scale 21 among healthy respondents from three continents. Front. Psychol. 13, 799769. https://doi.org/10.3389/fpsyg.2022.799769 (2022).
Kfoury, M., Barakat, H., Hallit, S. & Saliba, S. Association between endometriosis and sexual satisfaction among a sample of Lebanese women. BMC Womens Health 23, 164. https://doi.org/10.1186/s12905-023-02323-1 (2023).
Hammoudi Halat, D. et al. Exploring the effects of health behaviors and mental health on students’ academic achievement: A cross-sectional study on Lebanese university students. BMC Public Health 23, 1228. https://doi.org/10.1186/s12889-023-16184-8 (2023).
Fekih-Romdhane, F. et al. Validation of the Arabic version of the Psychotic-Like Experiences Questionnaire for Children (PLEQ-C) in a community sample of children and adolescents aged 12–18 years. Int. J. Ment. Health Addict. https://doi.org/10.1007/s11469-023-01133-8 (2023).
Chaaya, R. et al. Validation of the Arabic version of the resilience scale for adolescents (READ). BMC Psychiatry 23, 713. https://doi.org/10.1186/s12888-023-05219-4 (2023).
Fekih-Romdhane, F. et al. Psychometric properties of an Arabic translation of the Nine Item Avoidant/Restrictive Food Intake Disorder Screen (NIAS) in a community sample of adults. J. Eat. Disord. 11, 143. https://doi.org/10.1186/s40337-023-00874-0 (2023).
Fekih-Romdhane, F. et al. Insomnia and distress as mediators on the relationship from cyber-victimization to self-reported psychotic experiences: A binational study from Tunisia and Lebanon. BMC Psychiatry 23, 524. https://doi.org/10.1186/s12888-023-05019-w (2023).
Fekih-Romdhane, F. et al. Psychometric properties of an Arabic translation of the external and internal shame scale (EISS). BMC Psychiatry 23, 242. https://doi.org/10.1186/s12888-023-04729-5 (2023).
Awad, E., Malaeb, D., Fekih-Romdhane, F., Hallit, S. & Obeid, S. The moderating effect of psychological distress in the association between temperaments and dark future among young adults. BMC Psychiatry 24, 18. https://doi.org/10.1186/s12888-023-05486-1 (2024).
Liu, W. et al. The General mattering scale, the anti-mattering scale, and the fear of not mattering inventory: Psychometric properties and links with distress and hope among Chinese university students. Psychol. Res. Behav. Manag. 16, 4445–4459. https://doi.org/10.2147/PRBM.S430455 (2023).
Karam, J.-M. et al. The moderating effect of emotion regulation in the association between social support and religiosity and psychological distress in adults. BMC Psychol. 11, 120. https://doi.org/10.1186/s40359-023-01160-z (2023).
Fekih-Romdhane, F. et al. Psychometric properties of an Arabic translation of the briefest version of the Zimbardo time perspective inventory (ZTPI-15). BMC Psychiatry 23, 338. https://doi.org/10.1186/s12888-023-04815-8 (2023).
Chabbouh, A. et al. Examining correlates of aggression and mediating effect of psychological distress between exposure to media violence and aggression in Lebanese adults. BMC Psychol. 11, 191. https://doi.org/10.1186/s40359-023-01232-0 (2023).
Mahfoud, D., Fawaz, M., Obeid, S. & Hallit, S. The co-moderating effect of social support and religiosity in the association between psychological distress and coping strategies in a sample of Lebanese adults. BMC Psychol. 11, 61. https://doi.org/10.1186/s40359-023-01102-9 (2023).
Lovibond, P. F. & Lovibond, S. H. Manual for the Depression Anxiety Stress Scales 2nd edn. (Psychology Foundation, 1995).
Lee, J.-Y., Yoo, Y. S. & Song, Y. Sex differences in depression, anxiety, stress, and mindfulness among patients with percutaneous coronary intervention. SAGE Open 13, 21582440231167120. https://doi.org/10.1177/21582440231167121 (2023).
Cao, C.-H. et al. Psychometric evaluation of the depression, anxiety, and stress scale-21 (DASS-21) among Chinese primary and middle school teachers. BMC Psychol. 11, 209. https://doi.org/10.1186/s40359-023-01242-y (2023).
Moya, E. et al. Reliability and validity of depression anxiety stress scale (DASS)-21 in screening for common mental disorders among postpartum women in Malawi. BMC Psychiatry 22, 352. https://doi.org/10.1186/s12888-022-03994-0 (2022).
Tran, T. D., Tran, T. & Fisher, J. Validation of the depression anxiety stress scales (DASS) 21 as a screening instrument for depression and anxiety in a rural community-based cohort of northern Vietnamese women. BMC Psychiatry https://doi.org/10.1186/1471-244X-13-24 (2013).
Dahm, J., Wong, D. & Ponsford, J. Validity of the Depression Anxiety Stress Scales in assessing depression and anxiety following traumatic brain injury. J. Affect. Disord. 151, 392–396. https://doi.org/10.1016/j.jad.2013.06.011 (2013).
Bener, A., Alsulaiman, R., Doodson, L. & El Ayoubi, H. Comparison of reliability and validity of the breast cancer depression anxiety stress scales (DASS-21) with the Beck Depression Inventory-(BDI-II) and Hospital Anxiety and Depression Scale (HADS). Int. J. Behav. Res. Psychol. 4, 197–203. https://doi.org/10.19070/2332-3000-1600035 (2016).
Clover, K. et al. Apples to apples? Comparison of the measurement properties of hospital anxiety and depression-anxiety subscale (HADS-A), depression, anxiety and stress scale-anxiety subscale (DASS-A), and generalised anxiety disorder (GAD-7) scale in an oncology setting using Rasch analysis and diagnostic accuracy statistics. Curr. Psychol. 41, 4592–4601. https://doi.org/10.1007/s12144-020-00906-x (2022).
Chin, E. G., Buchanan, E. M., Ebesutani, C. & Young, J. Depression, anxiety, and stress: How should clinicians interpret the total and subscale scores of the 21-item depression, anxiety, and stress scales?. Psychol. Rep. 122, 1550–1575. https://doi.org/10.1177/0033294118783508 (2019).
Ali, A. M. et al. Cut-off scores of the Depression Anxiety Stress Scale-8: Implications for improving the management of chronic pain. J. Clin. Nurs. https://doi.org/10.1111/jocn.16878 (2023).
Neamțu, B. M. et al. A decision-tree approach to assist in forecasting the outcomes of the neonatal brain injury. Int. J. Environ. Res. Public Health 18, 4807 (2021).
Tzankov, A. et al. Prognostic immunophenotypic biomarker studies in diffuse large B cell lymphoma with special emphasis on rational determination of cut-off scores. Leuk. Lymphoma 51, 199–212. https://doi.org/10.3109/10428190903370338 (2010).
Yu, Y. et al. Determining a cutoff score for the family burden interview schedule using three statistical methods. BMC Med. Res. Methodol. 19, 93. https://doi.org/10.1186/s12874-019-0734-8 (2019).
Tustumi, F. Choosing the most appropriate cut-point for continuous variables. Rev. Col. Bras. Cir 49, e20223346. https://doi.org/10.1590/0100-6991e-20223346-en (2022).
Benassi, M. et al. Using two-step cluster analysis and latent class cluster analysis to classify the cognitive heterogeneity of cross-diagnostic psychiatric inpatients. Front. Psychol. 11, 1085. https://doi.org/10.3389/fpsyg.2020.01085 (2020).
Messina, A., Lattanzi, M., Albanese, E. & Fiordelli, M. Caregivers of people with dementia and mental health during COVID-19: findings from a cross-sectional study. BMC Geriatr. https://doi.org/10.21203/rs.3.rs-966605/v1 (2022).
Chattat, R. et al. The Italian version of the Zarit Burden interview: A validation study. Int. Psychogeriatr. 23, 797–805. https://doi.org/10.1017/s1041610210002218 (2011).
Bédard, M. et al. The Zarit Burden Interview: A new short version and screening version. Gerontologist 41, 652–657. https://doi.org/10.1093/geront/41.5.652 (2001).
Hughes, M. E., Waite, L. J., Hawkley, L. C. & Cacioppo, J. T. A short scale for measuring loneliness in large surveys: Results from two population-based studies. Res. Aging 26, 655–672. https://doi.org/10.1177/0164027504268574 (2004).
Yu, Y. et al. Cutoff of the Zarit Burden Interview in predicting depression and anxiety. Qual. Life Res. 28, 2525–2533. https://doi.org/10.1007/s11136-019-02208-7 (2019).
Naemi, A., Schmidt, T., Mansourvar, M., Ebrahimi, A. & Wiil, U. K. Quantifying the impact of addressing data challenges in prediction of length of stay. BMC Med. Inform. Decis. Mak. 21, 298. https://doi.org/10.1186/s12911-021-01660-1 (2021).
IBM. Chapter 1. Decision Trees in IBM SPSS Decision Trees 28. Retreived July 7, 2022. https://www.ibm.com/docs/en/SSLVMB_28.0.0/pdf/IBM_SPSS_Decision_Trees.pdf (2022).
Ali, A. M. et al. The Nine-Item Internet Gaming Disorder Scale (IGDS9-SF): Its psychometric properties among Sri Lankan students and measurement invariance across Sri Lanka, Turkey, Australia, and the USA. Healthcare 10, 490. https://doi.org/10.3390/healthcare10030490 (2022).
Ali, A. M. et al. The Arabic version of the impact of event scale–revised: Psychometric evaluation in psychiatric patients and the general public within the context of COVID-19 outbreak and quarantine as collective traumatic events. J. Pers. Med. 12, 681. https://doi.org/10.3390/jpm12050681 (2022).
Messina, A. Caregivers of people with dementia and mental health during COVID-19: Findings from a cross-sectional study. Zenodo Version 1, https://doi.org/10.5281/zenodo.4748651 (2021).
Ali, A. M., Alkhamees, A. A., Elhay, E. S. A., Taha, S. M. & Hendawy, A. O. COVID-19-related psychological trauma and psychological distress among community-dwelling psychiatric patients: People struck by depression and sleep disorders endure the greatest burden. Front. Public Health https://doi.org/10.3389/fpubh.2021.799812 (2022).
Eres, R., Lim, M. H. & Bates, G. Loneliness and social anxiety in young adults: The moderating and mediating roles of emotion dysregulation, depression and social isolation risk. Psychol. Psychother. Theory Res. Pract. 96, 793–810. https://doi.org/10.1111/papt.12469 (2023).
Steen, O. D., Ori, A. P. S., Wardenaar, K. J. & van Loo, H. M. Loneliness associates strongly with anxiety and depression during the COVID pandemic, especially in men and younger adults. Sci. Rep. 12, 9517. https://doi.org/10.1038/s41598-022-13049-9 (2022).
Isik, A. T., Soysal, P., Solmi, M. & Veronese, N. Bidirectional relationship between caregiver burden and neuropsychiatric symptoms in patients with Alzheimer’s disease: A narrative review. Int. J. Geriatr. Psychiatry 34, 1326–1334. https://doi.org/10.1002/gps.4965 (2019).
Lee, M., Ryoo, J. H., Campbell, C., Hollen, P. J. & Williams, I. C. Exploring the challenges of medical/nursing tasks in home care experienced by caregivers of older adults with dementia: An integrative review. J. Clin. Nurs. 28, 4177–4189. https://doi.org/10.1111/jocn.15007 (2019).
Stall, N. M. et al. Association of informal caregiver distress with health outcomes of community-dwelling dementia care recipients: A systematic review. J. Am. Geriatr. Soc. 67, 609–617. https://doi.org/10.1111/jgs.15690 (2019).
Acknowledgements
The Researchers would like to thank the Deanship of Graduate Studies and Scientific Research at Qassim University for financial support (QU-APC-2024-9/1).
Author information
Authors and Affiliations
Contributions
AMA, AAA, and SAA conceptualized the study and designed the methodology. TNA and HK cleaned the data. AMA and SAA analyzed and interpreted the data. TNA, AAA, SH, and HK wrote the initial draft of the manuscript. AMA, SH, and SAA edited and revised the final draft. All authors have critically revised and approved the final draft of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ali, A.M., Alkhamees, A.A., Hallit, S. et al. The Depression Anxiety Stress Scale 8: investigating its cutoff scores in relevance to loneliness and burnout among dementia family caregivers. Sci Rep 14, 13075 (2024). https://doi.org/10.1038/s41598-024-60127-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-60127-1
- Springer Nature Limited