Abstract
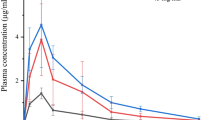
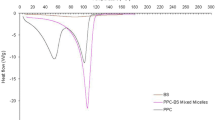
The absorption enhancement and presystemic degradation kinetics of a homologous series of acyclovir 2′-ester prodrugs were investigated in rats using the in situ nasal perfusion technique in the presence of bile salt–fatty acid mixed micells. In vitro incubation studies indicated that nasal perfusate containing a mixed micellar solution generated higher ester-cleaving activity than isotonic phosphate buffer washings. Inhibitor screening and substrate specificity studies demonstrated the enzyme to be most likely carboxylesterase rather than true cholinesterase. The extent of prodrug cleavage by the carboxylesterase appears to correlate well with the substrate li-pophilicity for esters with linear acyl chains. On the other hand, branching of the acyl side chain significantly retards acyclovir pro-drug breakdown. To estimate the nasal epithelial membrane and cytoplasmic damaging effect caused by sodium glycocholate (NaGC)–linoleic acid (15 mM:5 mM) mixed micelles, the release profiles of 5′-nucleotidase (5′-ND), lactate dehydrogenase (LDH), and carboxylesterase in the nasal perfusate were measured as a function of time. The results indicated that the activities of all three enzymes resulting from the mixed micellar solution appeared to be significantly higher than those caused by 15 mM NaGC alone. The apparent nasal absorption rate constants of acyclovir and its butyrate, valerate, pivalate, and hexanoate ester prodrugs in mixed micellar solutions containing an esterase inhibitor (1 mM phenylmethylsulfonyl fluoride) were individually calculated. Without an inhibitor, lengthening of the linear acyl side chain of the prodrug resulted in greatly accelerated degradation coupled with moderate absorption improvement. The solubilities and micellar binding constants of acyclovir prodrugs were also determined. Mixed micelles composed of 15 mM NaGC and 5 mM linoleic acid are incapable of incorporating these esters into the micellar cavity, although NaGC micelle alone can actively solubilize them in a concentration-dependent manner.
Similar content being viewed by others
REFERENCES
Y. W. Chien, K. S. E. Su, and S.-F. Chang. Nasal Systemic Drug Delivery, Marcel Dekker, New York, Basal, 1989, pp. 1–310.
G. S. M. J. E. Duchateau, J. Zuidema, W. M. Albers, and F. W. H. M. Merus. Nasal absorption of alprenolol and metoprolol. Int. J. Pharm. 34:131–136 (1986).
C. H. Huang, R. Kimura, R. Bawarshi, and A. Hussain. Mechanism of nasal absorption of drugs. I. Physicochemical parameters influencing the rate of in situ nasal absorption of drugs in rats. J. Pharm. Sci. 74:60–611 (1985).
C. McMartin, L. E. F. Hutchison, R. Hyde, and G. E. Peters. Analysis of structural requirements for the absorption of drugs and macromolecules from the nasal cavity. J. Pharm. Sci. 76:535–540 (1987).
Z. Shao, G.-B. Park, R. Krishnamoorthy, and A. K. Mitra. The physicochemical properties, plasma enzymatic hydrolysis, and rat nasal absorption of acyclovir and its 2′-ester prodrugs. Pharm. Res. 11:1237–2421 (1994).
S. Hirai, T. Yashiki, T. Matsuzawa, and H. Mima. Absorption of drugs from the nasal mucosa of rat. Int. J. Pharm. 7:317–325 (1981).
G. Land and A. Bye. Simple high-performance liquid chromatographic method for the analysis of 9-(2-hydroxyethoxymethyl)-guanine (acyclovir) in human plasma and urine. J. Chromatogr. 224:51–58 (1981).
J. M. Patel and D. E. Wurster. Catalysis of carbaryl hydrolysis in micellar solutions of cetyltrimethylammonium bromide. Pharm. Res. 8:1155–1158 (1991).
Å. Ljungquist and K.-B. Augustinsson. Purification and properties of two carboxylesterases from rat-liver microsomes. Eur. J. Biochem. 23:303–313 (1971).
S. H. Sterri, B. A. Johnsen, and F. Fonnum. A radiochemical assay method for carboxylesterase, and comparison of enzyme activity towards the substrate methyl [1-14C]butyrate and 4-nitrophenyl butyrate. Biochem. Pharmacol. 34:2779–2785 (1985).
M. S. Bogdanffy, H. W. Randall, and K. T. Morgan. Biochemical quantitation and histochemical localization of carboxylesterase in the nasal passages of the Fischer-344 rat and B6C3F1 mouse. Toxicol. Appl. Pharmacol. 88:183–194 (1987).
P. Tengamnuay and A. K. Mitra. Bile salt-fatty acid mixed micelles as nasal absorption promoters of peptides. I. Effects of ionic strength, adjuvent composition and lipid structure on the nasal absorption of [D-Arg2]kyotorphin. Pharm. Res. 7:127–133 (1990).
P. Tengamnuay and A. K. Mitra. Bile salt-fatty acid mixed micelles as nasal absorption promoters of peptides. II. In vivo nasal absorption of insulin in rats and effects of mixed micelles on the morphological integrity of the nasal mucosa. Pharm. Res. 7:370–375 (1990).
J. A. Faraj, A. A. Hussain, Y. Aramaki, K. Iseki, M. Kagoshima, and L. W. Dittert. Mechanism of nasal absorption of drugs. III. Nasal absorption of leucine enkephalin. J. Pharm. Sci. 79:698–702 (1990).
W. F. Prouty and A. L. Goldberg. Effects of protease inhibitors on protein breakdown in Escherichia coli. J. Biol. Chem. 247:3341–3352 (1972).
M. K. Ghosh and A. K. Mitra. Carboxylic ester hydrolase activity in hairless and athymic nude mouse skin. Pharm. Res. 7:251–255 (1990).
K. Krisch. Carboxylic ester hydrolases. In P. D. Boyer (ed.), The Enzymes, Academic Press, New York and London, 1971, pp. 43–69.
Z. Shao and A. K. Mitra. Nasal membrane and intracellular protein and enzyme release by bile salt-fatty acid mixed micelles: Correlation with facilitated drug transport. Pharm. Res. 9:1184–1189 (1992).
C. H. Huang, R. Kimura, R. Bawarshi-Nassar, and A. Hussain. Mechanism of nasal absorption of drugs. II. Absorption of L-tyrosine and the effect of structural modification on its absorption. J. Pharm. Sci. 74:1298–1301 (1985).
P. D. Miranda, H. C. Krasny, D. A. Page, and G. B. Elion. The disposition of acyclovir in different species. J. Pharmacol. Exp. Ther. 219:309–315 (1981).
E. R. Cooper, E. W. Merritt, and R. L. Smith. Effect of fatty acid and alcohols on the penetration of acyclovir across human skin in vitro. J. Pharm. Sci. 6:688–689 (1985).
M. D. Donovan, G. L. Flynn, and G. L. Amidon. The molecular weight dependence of nasal absorption: The effect of absorption enhancers. Pharm. Res. 7:808–815 (1990).
S. Muranishi. Absorption enhancers. Crit. Rev. Ther. Drug Carr. Syst. 7:1–33 (1990).
W. T. Stott and M. J. McKenna. Hydrolysis of several glycol ether acetates and acrylate esters by nasal mucosal carboxylesterase in vitro. Fund. Appl. Toxicol. 5:399–404 (1985).
S. Hirai, T. Yashiki, and H. Mima. Mechanisms for the enhancement of the nasal absorption of insulin by surfactants. Int. J. Pharm. 9:173–184 (1981).
E. Hayakawa and V. H. L. Lee. Aminopeptidase activity in the jejunal and ileal Peyer's patches of the albino rabbit. Pharm. Res. 9:535–540 (1992).
Y. Li, Z. Shao, and A. K. Mitra. Dissociation of insulin oligomers by bile salt micelles and its effect on α-chymotrypsin-mediated proteolytic degradation. Pharm. Res. 9:864–869 (1992).
K. Kakemi, H. Sezaki, R. Konishi, T. Kimura, and M. Murakami. Effects of bile salts on the gastrointestinal absorption of drugs. I. Chem. Pharm. Bull. 18:275–280 (1970).
F. G. J. Poelma, R. Breäs, and J. J. Tukker. Intestinal absorption of drugs. IV. The influence of taurocholate and L-cysteine on the barrier function of mucus. Int. J. Pharm. 64:161–169 (1990).
S. Choudhury and A. K. Mitra. Effects of hydrophobicity and bile salt micellar entrapment on the nasal transport of β-blockers. Pharm. Res. 9:S-207 (1992).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Shao, Z., Mitra, A.K. Bile Salt–Fatty Acid Mixed Micelles as Nasal Absorption Promoters. III. Effects on Nasal Transport and Enzymatic Degradation of Acyclovir Prodrugs. Pharm Res 11, 243–250 (1994). https://doi.org/10.1023/A:1018955424431
Issue Date:
DOI: https://doi.org/10.1023/A:1018955424431