Abstract
Study Design
Retrospective clinical cohort study.
Objective
To compare the long-term complications and outcomes scores of primary and revision surgeries for adult spinal deformity of patients treated with long fusions to the sacrum.
Summary of Background Data
Long fusions in patients with adult spinal deformity are fraught with complications and the need for reoperation that can significantly impact patient health-related quality of life.
Methods
Data from 134 consecutive patients who underwent spinal fusion from the thoracic spine to the sacropelvis and had a minimum of 5-year follow-up were analyzed. Patients were classified as primary surgery (PS) and index revision (IR) surgery; they were then subdivided based on whether they returned to the operating room (RTO) or not (NRTO). RTO complications were classified as 1) infection, 2) neurologic, 3) fusion status, 4) implants, and 5) global alignment and stratified as <6 months, <2 years, and >2 years. Final Scoliosis Research Society Patient Questionnaire (SRS 22r) and Oswestry Disability Index (ODI) scores were compared between subgroups.
Results
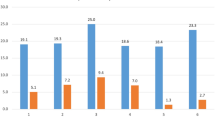
Seventy-one PS and 63 IR were included in the analysis. Mean age at surgery was 54.9 years (30–78), mean follow-up 5.8 years (4.9–12.8). RTO rates were 21.1% and 34.9%, respectively, for PS and IR (p =.16). 43.8% of patients requiring reoperation did so on multiple occasions. Fifty PS and 41 IR cases had complete SRS 22 and ODI scores. Final SRS 22 total scores were 3.74 and 3.41 (p =.02) for the respective groups. ODI scores were 25.4% and 34.0% (p =.02).
Conclusions
Both groups had a significant number of revision surgeries performed by 5 years of follow-up. Unplanned reoperation significantly affected ODI and SRS 22 outcomes scores in the individual domains of pain, function, and overall satisfaction as well as total score at the 5-year follow-up regardless of PS or IR status. Overall, the PS group had improved outcomes when compared to the IR group.
Similar content being viewed by others
References
Dick J, Boachie-Adjei O, Wilson M. One-stage versus two-stage anterior and posterior spinal reconstruction in adults. Comparison of outcomes including nutritional status, complications rates, hospital costs, and other factors. Spine (Phila Pa 1976) 1992;17:S310–6.
Edwards 2nd CC, Bridwell KH, Patel A, et al. Long adult deformity fusions to L5 and the sacrum. A matched cohort analysis. Spine (Phila Pa 1976) 2004;29:1996–2005.
Weistroffer JK, Perra JH, Lonstein JE, et al. Complications in long fusions to the sacrum for adult scoliosis: minimum five-year analysis of fifty patients. Spine (Phila Pa 1976) 2008;33:1478–83.
Pichelmann MA, Lenke LG, Bridwell KH, et al. Revision rates following primary adult spinal deformity surgery: six hundred forty-three consecutive patients followed-up to twenty-two years postoperative. Spine (Phila Pa 1976) 2010;35:219–26.
Baron EM, Albert TJ. Medical complications of surgical treatment of adult spinal deformity and how to avoid them. Spine (Phila Pa 1976) 2006;31:S106–18.
Cho SK, Bridwell KH, Lenke LG, et al. Major complications in revision adult deformity surgery: risk factors and clinical outcomes with 2- to 7-year follow-up. Spine (Phila Pa 1976) 2012;37:489–500.
Sansur CA, Smith JS, Coe JD, et al. Scoliosis research society morbidity and mortality of adult scoliosis surgery. Spine (Phila Pa 1976) 2011;36:E3–7.
Smith JS, Sansur CA, Donaldson 3rd WF, et al. Short-term morbidity and mortality associated with correction of thoracolumbar fixed sagittal plane deformity: a report from the Scoliosis Research Society morbidity and mortality committee. Spine (Phila Pa 1976) 2011;36:958–64.
Howe CR, Agel J, Lee MJ, et al. The morbidity and mortality of fusions from the thoracic spine to the pelvis in the adult population. Spine (Phila Pa 1976) 2011;36:1397–401.
Glassman SD, Hamill CL, Bridwell KH, et al. The impact of perioperative complications on clinical outcome in adult deformity surgery. Spine (Phila Pa 1976) 2007;32:2764–70.
Schwab FJ, Lafage V, Farcy JP, et al. Predicting outcome and complications in the surgical treatment of adult scoliosis. Spine (Phila Pa 1976) 2008;33:2243–7.
Smith JS, Shaffrey CI, Glassman SD, et al. Risk-benefit assessment of surgery for adult scoliosis: an analysis based on patient age. Spine (Phila Pa 1976) 2011;36:817–24.
Glassman SD, Berven S, Kostuik J, et al. Nonsurgical resource utilization in adult spinal deformity. Spine (Phila Pa 1976) 2006;31:941–7.
Schwab F, Dubey A, Gamez L, et al. Adult scoliosis: prevalence, SF- 36, and nutritional parameters in an elderly volunteer population. Spine (Phila Pa 1976) 2005;30:1082–5.
Bridwell KH, Berven S, Edwards 2nd C, et al. The problems and limitations of applying evidence-based medicine to primary surgical treatment of adult spinal deformity. Spine (Phila Pa 1976) 2007;32:S135–9.
Li G, Passias P, Kozanek M, et al. Adult scoliosis in patients over sixty-five years of age: outcomes of operative versus nonoperative treatment at a minimum two-year follow-up. Spine (Phila Pa 1976) 2009;34:2165–70.
Ploumis A, Liu H, Mehbod AA, et al. A correlation of radiographic and functional measurements in adult degenerative scoliosis. Spine (Phila Pa 1976) 2009;34:1581–4.
Zimmerman RM, Mohamed AS, Skolasky RL, et al. Functional outcomes and complications after primary spinal surgery for scoliosis in adults aged forty years or older: a prospective study with minimum two-year follow-up. Spine (Phila Pa 1976) 2010;35:1861–6.
Bradford DS, Tay BK, Hu SS. Adult scoliosis: surgical indications, operative management, complications, and outcomes. Spine (Phila Pa 1976) 1999;24:2617–29.
Bess S, Boachie-Adjei O, Burton D, et al. Pain and disability determine treatment modality for older patients with adult scoliosis, while deformity guides treatment for younger patients. Spine (Phila Pa 1976) 2009;34:2186–90.
Pekmezci M, Berven SH, Hu SS, et al. The factors that play a role in the decision-making process of adult deformity patients. Spine (Phila Pa 1976) 2009;34:813–7.
Schwab F, Farcy JP, Bridwell K, et al. A clinical impact classification of scoliosis in the adult. Spine (Phila Pa 1976) 2006;31:2109–14.
Kostuik JP, Hall BB. Spinal fusions to the sacrum in adults with scoliosis. Spine (Phila Pa 1976) 1983;8:489–500.
Emami A, Deviren V, Berven S, et al. Outcome and complications of long fusions to the sacrum in adult spine deformity: Luque-Galveston, combined iliac and sacral screws, and sacral fixation. Spine (Phila Pa 1976) 2002;27:776–86.
Lapp MA, Bridwell KH, Lenke LG, et al. Long-term complications in adult spinal deformity patients having combined surgery: a comparison of primary to revision patients. Spine (Phila Pa 1976) 2001;26:973–83.
Haher TR, Gorup JM, Shin TM, et al. Results of the Scoliosis Research Society instrument for evaluation of surgical outcome in adolescent idiopathic scoliosis. A multicenter study of 244 patients. Spine (Phila Pa 1976) 1999;24:1435–40.
Asher MA, Lai SM, Glattes RC, et al. Refinement of the SRS-22 Health-Related Quality of Life questionnaire Function domain. Spine (Phila Pa 1976) 2006;31:593–7.
Berven S, Deviren V, Demir-Deviren S, et al. Studies in the modified Scoliosis Research Society outcomes instrument in adults: validation, reliability, and discriminatory capacity. Spine (Phila Pa 1976) 2003;28:2164–9; discussion 2169.
Bridwell KH, Cats-Baril W, Harrast J, et al. The validity of the SRS-22 instrument in an adult spinal deformity population compared with the Oswestry and SF-12: a study of response distribution, concurrent validity, internal consistency, and reliability. Spine (Phila Pa 1976) 2005;30:455–61.
Baldus C, Bridwell K, Harrast J, et al. The Scoliosis Research Society health-related quality of life (SRS-30) age-gender normative data: an analysis of 1346 adult subjects unaffected by scoliosis. Spine (Phila Pa 1976) 2011;36:1154–62.
Bridwell KH, Berven S, Glassman S, et al. Is the SRS-22 instrument responsive to change in adult scoliosis patients having primary spinal deformity surgery? Spine (Phila Pa 1976) 2007;32:2220–5.
Fairbank JC, Pynsent PB. The Oswestry Disability Index. Spine (Phila Pa 1976) 2000;25:2940–52; discussion 2952.
Author information
Authors and Affiliations
Corresponding author
Additional information
HSS - IRB Research Registry 23-032.
No funding was received for the conduction of this study.
Rights and permissions
About this article
Cite this article
Faloon, M.J., Essig, D., Cho, W. et al. Unplanned Reoperations Affect Long-Term Outcomes in Adult Spinal Deformity Patients Undergoing Long Fusions to the Sacrum. Spine Deform 3, 367–371 (2015). https://doi.org/10.1016/j.jspd.2015.02.005
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2015.02.005