Abstract
This study aimed to compare the prevalence of somnolence and hypersomnolence between a higher education student and non-student sample. Hershner and Chervin [Hershner in Nat sci sleep 10.2147/NSS.S62907, 2014] defined somnolence as lapses into drowsiness, consequently leading to the inability to maintain alertness. This definition aligns with the American Academy of Sleep Medicine's (AASM) definition [Berry in Am Acad Sleep Med 176:2012, 2012]. Hypersomnolence differs from this, as suggested by Lammers et al. [Lammers in Sleep Med Rev 52, 101306, 2020], and refers to the experience of excessive daytime sleepiness. It is commonly observed that individuals enrolled in higher education courses often experience somnolence and hypersomnolence; however, it is currently unclear whether this is more prevalent in students compared to the general population. An online survey was administered to 202 participants measuring somnolence, hypersomnolence, sleep quality, sleep efficiency, sleep disturbance, sleep duration, circadian preference, and daytime dysfunction. 94 participants were non-students, and 108 were enrolled in higher education. Significant differences were found between student and non-student samples for somnolence but not for hypersomnolence. Furthermore, within the non-student sample a multiple linear regression demonstrated that hypersomnolence was predicted by daytime dysfunction. The results suggest that there are differences in the predictors of somnolence and hypersomnolence between a student and non-student sample. Consequently, this study highlights that students experience hypersomnolence and somnolence differently to their non-student counterparts. Thus, warranting the need for further investigating within this unique population.
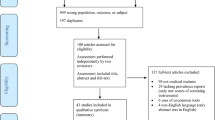
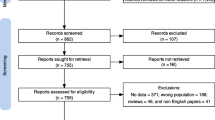
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Individuals enrolled in higher education courses are often reported as experiencing somnolence and hypersomnolence [1], however, it is currently unclear whether this differs from the general population. Chervin and Hershner [2] defined somnolence as lapses into drowsiness, consequently leading to the inability to maintain wakefulness. This definition aligns with the American Academy of Sleep Medicine's (AASM) definition [3]. Conversely, hypersomnolence differs from this, as suggested by Lammers et al. [4], and refers to the experience of excessive daytime sleepiness. The following study investigates whether students perceive their somnolence and hypersomnolence to impact their lives more significantly than their general population counterparts.
Somnolence is a public health crisis, with the European Research Society investigating predictors that leave individuals vulnerable to somnolence [5]. Somnolence is a multidimensional state [6] frequently reported among the general population and has been demonstrated to impact safety and productivity [7, 8]. There are two ways to define somnolence: by examining physiological characteristics or by self-reported measures [9]. Within this study, introspective somnolence will be the focus, using self-report measures. Introspective somnolence refers to the self-reported and perceived experience of somnolence that individuals may be exposed to, due to health or behavioural origins such as bedtime procrastination or chronic sleep restriction [10]. The experience of somnolence can become intrusive to everyday life when the ability to maintain wakefulness cannot be sustained [11]. Somnolence often occurs alongside other sleep complaints. For example, sleep disturbance is commonly experienced alongside somnolence [12, 13] and is frequently observed in literature within a higher education environment [14,15,16,17]. However, sleep disturbance and somnolence are frequently viewed in these studies as a symptom of a depressive state, not as their own phenomenon.
Kim and Young [18] demonstrate that somnolence is a frequent issue that is also identified within the general population. However, risk factors such as being male, overweight, and frequent alcohol use can also increase the risk of experiencing somnolence further [19]. These factors may leave some populations more vulnerable to somnolence than others, including those suffering from sleep-disordered breathing [20], sleep disorder patients [21], older populations [22], and those with sleep co-morbidities [23]. Further identification is required to determine whether this is consistent for all vulnerable populations.
Increasing in severity, growing levels of somnolence in the population has led to the investigation of hypersomnolence [24]. However, as demonstrated by Perez Carbonell et al. [11], hypersomnolence frequently remains underdiagnosed as the experience, and treatment, tends to be subjective to the individual. Over recent years, various populations have been identified as at a higher risk of experiencing hypersomnolence, such as public transport drivers [25], shift workers [26], and finally those within higher education [27].
Higher education students have been highlighted as a vulnerable population for hypersomnolence by Hershner and Chervin [2] who identified somnolence as a significant problem for higher education students within the USA. Further, Alves et al. [28] demonstrated the prevalence of hypersomnolence among adolescents within education, attributing this effect to long and short sleep duration. However, this study did not highlight important individual factors in their student population, such as the potential differences in circadian preference. Circadian preference may significantly impact educational samples performance, and wellbeing, as ever-changing schedules result in students being forced to act against their natural preference [29]. Equally, Marta et al. [30] associates the link of sleep deprivation, insomnia, and somnolence within academic performance, identifying the trend that those suffering from sleep disturbances have lower academic performance. Dagnew [31] once again demonstrates the prevalence of hypersomnolence among higher education students. However, Dagnew [31] also stresses the requirement for further research investigating the contributing factors that make students more vulnerable to the effects of hypersomnolence. Dagnew [31] furthers this by suggesting that until some indication of what might make students more likely to suffer from hypersomnolence, our ability to put into place preventative strategies still needs to be improved.
As outlined, recent studies have shown that somnolence is a common experience in the general population, and has an increased prevalence among students [14,15,16,17]. Yet, to our knowledge, no studies compare whether there is a difference between these populations. This study will further the work of Hershner and Chervin [2] by identifying the differences in somnolence and hypersomnolence between a student and non-student sample in the United Kingdom. In addition, key sleep parameters related to and potentially predicting somnolence within a student sample will also be examined, such as circadian preference and sleep disturbance.
2 Methodology
Participants. G*Power (version 3.1.9.2) [32] was used to calculate the required sample size. The effect size (0.3), α error probability (0.05), and statistical power (1-β err prob = 0.95), were pre-set and left untouched. The G*Power calculation demonstrated non-centrally parameter λ of 25.2000000, critical t of 2.0644393, and df of 75. Therefore, the overall sample size per group required was 84. Participants were screened and excluded if they reported a diagnosed sleep or neurological disorder before the study took place. Exclusion criteria also included individuals who identified as having an intake of stimulants, hypnotics, benzodiazepines and/or antidepressants different from their habitual daily intake.
Data from 202 participants were collected online. 94 were non-students and 108 were currently enrolled in higher education. Further demographic information is provided in Table 1, age distribution for each sample is provided in Fig. 1, and employment, education, and qualification status are presented in Table 2.
Design. An independent measures design was employed. Within this study, participants were split into student and non-student groups to determine the difference in somnolence, hypersomnolence and sleep quality.
Materials. Four sleep scales were used in this study, the Epworth Sleepiness Scale, ESS [33], Stanford Sleepiness Scale, SSS [34], the Pittsburgh Sleep Quality Index, PSQI [35] and the Morningness Eveningness Questionnaire, MEQ [36]. Details of these scales are provided in Table 3.
Procedure. Ethical approval was granted by the University of Suffolk Ethics Committee on 29/07/21 (RETH20/070). Participants were presented with an appropriate information sheet and consent form, outlining the purpose of the project and the potential risks involved with the survey. All participants were asked to complete the following scales in a counterbalanced order: the Epworth Sleepiness Scale, ESS [33], Stanford Sleepiness Scale, SSS [34] Pittsburgh Sleep Quality Index, PSQI [35] and the Morningness and Eveningness Questionnaire, MEQ [36]. Participants were also asked to provide demographic information such as age, gender, and whether they were currently enrolled in higher education.
Data Analysis. Hypersomnolence was obtained from the Epworth Sleepiness Scale, ESS [33], somnolence was acquired from the Stanford Sleepiness Scale, SSS [34], sleep quality and sleep parameters were derived from the Pittsburgh Sleep Quality Index, PSQI [35], and descriptive statistics were also recorded for both the student and non-student samples. To determine the differences between those currently enrolled in higher education institutions (students) and those not currently enrolled in higher education (non-students) t-tests were performed for sleep quality (PSQI), somnolence (SSS), and hypersomnolence (ESS), as well as circadian preference (MEQ). Finally, to determine the individual contributing factors of somnolence (SSS) and hypersomnolence (ESS) multiple linear regression analyses were performed with global sleep quality, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, sleep latency and circadian preference as predictor variables. Predictor variables were obtained from the PSQI, with circadian preference being obtained from the MEQ.
3 Results
Sleep parameters were compared between students and non-students with each mean and standard deviation listed in Table 4 below.
Global Sleep Quality. Mean scores for global sleep quality, sleep efficiency, daytime dysfunction, sleep disturbance and sleep duration for the student and non-student samples are shown in Table 4. The significance level was adjusted using the Bonferroni correction to control for multiple comparisons. The adjusted alpha level was set at 0.01. There were no significant findings for the independent samples t-tests with Bonferroni corrections for global sleep quality (t(200) = 0.907, p = 0.365), sleep efficiency (t(200) = 0.809, p = 0.419), daytime dysfunction (t(200) = 0.129, p = 0.897), sleep disturbance (t(200) = 0.720, p = 0.473), or sleep duration (t(200) = 0.342, p = 0.029) between the students and non-student samples.
Circadian Preference. Mean scores for circadian preference are shown in Table 4. An independent samples t-test for circadian preference between students (M = 49.51, SD = 11.37) and non-students (M = 51.23, SD = 11.82) was not significant, t(200) = 1.04, p = 0.294, demonstrating that there was no significant difference between the students and non-students samples.
Somnolence (SSS). Mean scores for somnolence using the SSS scores are shown in Table 4. An independent samples t-test for somnolence between students (M = 3.49, SD = 1.53) and non-students (M = 3.04, SD = 1.26) was significant, t(200) = 2.22, p = 0.027, demonstrating that students had significantly higher levels of somnolence than the non-student sample.
Hypersomnolence (ESS). Mean scores for hypersomnolence using the ESS scores are shown in Table 4, and the distribution of ESS scores are displayed in Fig. 2 below. There was no significant finding for the independent samples t-tests for hypersomnolence (t(200) = 1.73, p = 0.085) between students (M = 6.86, SD = 4.00) and non-students (M = 7.86, SD = 4.19), demonstrating that there was no significant difference between the students and non-students samples.
Predicting somnolence (SSS) in the student sample. A simultaneous multiple linear regression was used to investigate whether global sleep quality, circadian preference, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency predicted somnolence within the student sample. The correlation matrix indicates that somnolence correlates with global sleep quality and daytime dysfunction within the student sample (see Table 5).
Overall, the multiple linear regression model was significant, F(7, 99) = 2.24, p < 0.05, R2 = 0.140, with 14% of the variance in somnolence being explained by circadian preference, global sleep quality, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency. However, circadian preference (β = 0.071, p = 0.475), global sleep quality (β = 0.346, p = 0.566), sleep efficiency (β = -0.104, p = 0.684), sleep medication (β = -0.099, p = 0.539), sleep disturbance (β = 0.057, p = 0.724), daytime dysfunction (β = 0.184, p = 0.402), sleep duration (β = -0.188, p = 0.311), and sleep latency (β = 0.042, p = 0.851) were not significant predictors of somnolence in the student sample.
Predicting hypersomnolence (ESS) in the student sample. A simultaneous multiple linear regression was used to investigate whether global sleep quality, circadian preference, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency predicted hypersomnolence within the student sample. The correlation matrix indicates that hypersomnolence correlates with global sleep quality, daytime dysfunction, and sleep disturbance in the student sample (see Table 6).
Overall, the multiple linear regression model was significant, F(7, 99) = 2.65, p < 0.005, R2 = 0.179, with 17.9% of the variance in hypersomnolence being explained by circadian preference, global sleep quality, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration and sleep latency. However, circadian preference (β = -031, p = 0.753), global sleep quality (β = 0.065, p = 0.912), sleep efficiency (β = 0.025, p = 0.919), sleep medication (β = -0.099, p = 0.539), sleep disturbance (β = 0.194, p = 0.223), daytime dysfunction (β = 0.321, p = 0.135), sleep duration (β = -0.188, p = 0.311), and sleep latency (β = − 0.137, p = 0.532) were not significant predictors of hypersomnolence in the student sample.
Predicting somnolence (SSS) in the non-student sample. A simultaneous multiple linear regression was used to investigate whether global sleep quality, circadian preference, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency predicted somnolence within the non-student sample. The correlation matrix indicates that somnolence correlates with global sleep quality, daytime dysfunction, and sleep latency within the non-student sample (see Table 7).
Overall, the multiple linear regression model was significant, F(8, 85) = 4.67, p < 0.01, R2 = 0.306, with 30.6% of the variance in somnolence being explained by circadian preference, global sleep quality, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency. However, circadian preference (β = 0.043, p = 0.640), global sleep quality (β = 0.738, p = 0.181), sleep efficiency (β = − 0.479, p = 0.038), sleep medication (β = − 0.357, p = 0.041), sleep disturbance (β = 0.097, p = 0.543), daytime dysfunction (β = 0.196, p = 0.288), sleep duration (β = -0.138, p = 0.516), and sleep latency (β = − 0.018, p = 0.942) were not significant predictors of somnolence in the non-student sample.
Predicting hypersomnolence (ESS) in the non-student sample. A simultaneous multiple linear regression was used to investigate whether global sleep quality, circadian preference, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration, and sleep latency predicted hypersomnolence within the non-student sample. The correlation matrix indicates that hypersomnolence only correlates with daytime dysfunction in the non-student sample (see Table 8).
Overall, the regression model was significant, F(8, 85) = 2.20, p < 0.035, R2 = 0.172, with 17.2% of the variance in hypersomnolence being explained by circadian preference, global sleep quality, sleep efficiency, daytime dysfunction, sleep medication, sleep disturbance, sleep duration and sleep latency. Daytime dysfunction significantly predicted hypersomnolence in the non-student sample, (β = 0.324, p = 0.003), demonstrating that as hypersomnolence increases so does daytime dysfunction within the non-student sample. However, circadian preference (β = 0.049, p = 0.628), global sleep quality (β = − 0.673, p = 0.263), sleep efficiency (β = 0.025, p = 0.919), sleep medication (β = 0.202, p = 0.287), sleep disturbance (β = 0.151, p = 0.386), sleep duration (β = 0.324, p = 0.164), and sleep latency (β = 0.023, p = 0.93) were not significant predictors of hypersomnolence in the non-student sample.
4 Discussion
This study identified that higher education students experience somnolence (SSS) in a distinctive way to their non-higher education enrolled counterparts. In summary, significant differences were found within somnolence but not facets of sleep quality or hypersomnolence (ESS) between the student and non-student sample. Additionally, daytime dysfunction predicted hypersomnolence, but only within the non-student sample, and not within the student sample.
We suggest no differences between global sleep quality, sleep efficiency, sleep disturbance, or sleep latency between a student and non-student population. Although our results do not indicate that students have a particularly high sleep quality, they do indicate that student’s sleep quality are similar to the general population. There was no significant difference found in sleep duration between students and non-students, however, non-students did report a lower number of hours sleep than the student sample, on average. This contrasts with research such as Lund et al. [16] who highlight insufficient sleep within a large student sample. Witkowski et al. [39] demonstrated how chronic sleep restriction can occur within a student population, with sleep duration decreasing through the duration of an academic semester. Therefore, it could be suggested that academic stress contributes to reduced sleep duration alongside the progression of their academic career and the lack of significance in this finding, could be indicative of variability in the sample. Further evidence from Liguori et al. [40] also demonstrates similar results, suggesting that sleep duration can increase or decrease depending on the semester schedule. Thus, demonstrating that although sleep duration may seem, on average, standard in a student population, there is a significant level of variability in these results. Therefore, examining hypersomnolence and somnolence may be more accurate in investigating sleep health in a student population.
Conversely, as our results highlighted that students have a higher sleep duration than the general population, longer sleep duration could indicate the presence of sleep inertia [41,42,43], which could contribute to our findings of daytime dysfunction, somnolence, and hypersomnolence. Sleep extension and, therefore, sleep inertia may occur due to increased sleep time due to circadian preference. Similarly, Onyper et al. [44] further investigated the impact of late class times on academic performance within a university sample. This research [44] found that later class times reduced the experience of daytime somnolence and reduced sleep disruption. However, this effect was also paired with increased alcohol use, which was suggested to impact academic attainment more significantly than the influence of somnolence. Yet, the findings of the current study demonstrated that circadian preference was not related to somnolence or hypersomnolence. Nevertheless, circadian preference was correlated with daytime dysfunction. This may indicate that students are using interventions such as sleep extension, alcohol, or stimulant use, as a method to accommodate for this incongruency. This is supported by Stock et al. [45] who demonstrated sleep extension increases students' academic performance and health indicators, such as systolic blood pressure. The current study suggests that students have a higher sleep duration than the non-student sample, likely to promote these physical requirements, as Stock et al. [45] suggested. This study contributes to the circadian preference and education debate highlighting that circadian preference may not be as maladaptive to higher education as previously thought.
Additionally, our results suggested a significant difference between students and non-students for somnolence, reporting that students have higher levels of somnolence than non-students in the UK. This finding is supported by evidence by Hershner and Chervin [2] who identify somnolence as a significant problem within higher education in the USA. This could be explained by unique determinants that apply to the student population, such as academic stress [46,47,48]. This academic stress may also be more extreme for medical courses, which may explain hypersomnolence being frequently reported among students in the medical field [27, 49, 50]. Furthermore, this result could also be due to the transitional phase of life that students experience, as identified by Brooman & Darwent [50]. This transitional period during higher education has previously been linked to sleep parameters such as sleep hygiene [51]. Poor sleep hygiene is a factor found within higher education across many studies [52,53,54,55]. Brown et al. [51] suggests that higher education students have inconsistent sleep schedules, unsatisfied physical needs, such as thirst or hunger before sleep, noisy sleep environments, and academic stress, all of which are factors that may contribute to sleep quality and somnolence. Although sleep hygiene was not investigated in the current study, our student sample demonstrated high levels of sleep duration and somnolence. Yet, sleep latency was not identified as a significant predictor of somnolence, suggesting that inconsistent sleep did not contribute to student somnolence in this study.
Although, previous research has suggested that hypersomnolence is common within a student population [2], no research to the best of our knowledge compared this finding to the general population. Within this study comparisons between a student and non-student sample, suggested no significant difference in levels of hypersomnolence. However, the average hypersomnolence levels for both groups were below the cut-offs for clinical hypersomnolence (< 11) [56]. Nonetheless, the focus of this study remained primarily on non-clinical levels of hypersomnolence. Therefore, further research would benefit from investigating these relationships within a clinical population.
Several limitations apply to this study. As identified by Boyes et al. [56], there are gender differences in the reporting of hypersomnolence; within the current study 84% of the sample (173/204) identified as female. Female participants are less likely to score highly within hypersomnolence or complain of somnolence symptoms, therefore it is likely that this has impacted our findings. Further research into this area, should attempt to balance the gender distribution within their sample to continue the investigation into this difference, as identified by Boyes et al. [56]. However, our research still offers important insights into the female student population and their self-reported somnolence. Within this study, age was unable to be controlled due to the unbalanced range in our sample. Moving forward, research into the area would benefit from separating and investigating different ages in isolation, for example, young and mature students. Although circadian preference showed no significant results in this study, it would be beneficial to control the time of day when future studies are completed. This in turn may be able to mediate the effects of wakefulness. Finally, this study focused on hypersomnolence and somnolence, it would be beneficial in future research to examine the longitudinal effects of sleepiness as students’ progress within education. Finally, this study focuses purely on the perceptions of somnolence, and the degree to which someone perceives themselves to be experiencing somnolence. Future research could therefore highlight how this may impact manifest sleepiness, as well as, how this would impact behavioural aspects such as one’s ability to maintain attention.
To summarise, this paper identified no significant differences between the sleep health structure of students and non-students, more specifically, in the form of sleep disruption, quality, latency, and efficiency, as well as daytime dysfunction. Despite finding no significant difference in sleep duration, on further examination, students did report higher sleep duration, than their non-student counterparts, which could lead to higher risks of comorbidities and mortality [57, 58]. Interestingly, a significant difference was found in somnolence between students and non-students. We suggest that this could be caused by factors such as academic stress, as well as the transition students experience within education. Furthermore, we did not find a significant difference in hypersomnolence between our student and non-student sample. In contrast to what was previously assumed, our finding suggest that students may not in fact be at a higher risk of hypersomnolence. Nevertheless our regression models highlight variation in the contributing factors of somnolence and hypersomnolence between students and non-students. Thus, highlighting the need for further examination of somnolence and hypersomnolence in a student population.
Data availability
Upon publication the data and materials for this study will be made available on the OSF profile for the lead author.
Code availability
Not applicable.
References
Dunn, C., Goodman, O., & Szklo-Coxe, M. (2022). Sleep duration, sleep quality, excessive daytime sleepiness, and chronotype in university students in India: a systematic review. J Health Soc Sci. 7(1).
Hershner SD, Chervin RD. Causes and consequences of sleepiness among college students. Nature Sci Sleep. 2014. https://doi.org/10.2147/NSS.S62907.
Berry RB, Brooks R, Gamaldo CE, Harding SM, Marcus C, Vaughn BV. The AASM manual for the scoring of sleep and associated events rules, terminology and technical specifications, darien, illinois. Am Acad Sleep Med. 2012;176:2012.
Lammers GJ, Bassetti CL, Dolenc-Groselj L, Jennum PJ, Kallweit U, Khatami R, Dauvilliers Y. Diagnosis of central disorders of hypersomnolence: a reappraisal by European experts. Sleep Med Rev. 2020;52:101306.
Bonsignore MR. Adaptive responses to chronic intermittent hypoxia: contributions from the European sleep apnoea database (ESADA) Cohort. J Physiol. 2023. https://doi.org/10.1113/JP284108.
Cluydts R, De Valck E, Verstraeten E, Theys P. Daytime sleepiness and its evaluation. Sleep Med Rev. 2002;6(2):83–96.
Al Shareef SM. Occupational outcomes associated with sleep quality and excessive daytime sleepiness: results from a national survey. Nat Sci Sleep. 2020. https://doi.org/10.2147/NSS.S271154.
Ferguson SA, Appleton SL, Reynolds AC, Gill TK, Taylor AW, McEvoy RD, Adams RJ. Making errors at work due to sleepiness or sleep problems is not confined to non-standard work hours: results of the 2016 sleep health foundation national survey. Chronobiol Int. 2019;36(6):758–69.
Pilcher JJ, Schoeling SE, Prosansky CM. Self-report sleep habits as predictors of subjective sleepiness. Behav Med. 2000;25(4):161–8.
Baiardi S, Mondini S. Inside the clinical evaluation of sleepiness: subjective and objective tools. Sleep Breathing. 2020;24:369–77.
Pérez-Carbonell L, Mignot E, Leschziner G, Dauvilliers Y. Understanding and approaching excessive daytime sleepiness. Lancet. 2022;400(10357):1033–46.
Happe S. Excessive daytime sleepiness and sleep disturbances in patients with neurological diseases: epidemiology and management. Drugs. 2003;63:2725–37.
Malakouti SK, Foroughan M, Nojomi M, Ghalebandi MF, Zandi T. Sleep patterns, sleep disturbances and sleepiness in retired Iranian elders. Int J Geriatr Psychiatry. 2009;24(11):1201–8.
Deng J, Zhou F, Hou W, Silver Z, Wong CY, Chang O, Huang E. The prevalence of depressive symptoms, anxiety symptoms and sleep disturbance in higher education students during the COVID-19 pandemic: a systematic review and meta-analysis. Psychiatry Res. 2021;301:113863.
Harvey AG, Gregory AM, Bird C. The role of cognitive processes in sleep disturbance: a comparison of Japanese and English university students. Behav Cogn Psychother. 2002;30(3):259–70.
Lund HG, Reider BD, Whiting AB, Prichard JR. Sleep patterns and predictors of disturbed sleep in a large population of college students. J Adolesc Health. 2010;46(2):124–32.
Nyer M, Farabaugh A, Fehling K, Soskin D, Holt D, Papakostas GI, Mischoulon D. Relationship between sleep disturbance and depression, anxiety, and functioning in college students. J Am Coll Health. 2013;61(2):96–103.
Kim H, Young T. Subjective daytime sleepiness: dimensions and correlates in the general population. Sleep. 2005;28(5):625–34.
Bonsignore MR, Randerath W, Schiza S, Verbraecken J, Elliott MW, Riha R, McNicholas WT. European respiratory society statement on sleep apnoea, sleepiness and driving risk. Eur Respir J. 2021. https://doi.org/10.1183/13993003.01272-2020.
Karimi M, Hedner J, Häbel H, Nerman O, Grote L. Sleep apnea-related risk of motor vehicle accidents is reduced by continuous positive airway pressure: Swedish traffic accident registry data. Sleep. 2015;38(3):341–9.
Flemons WW, Tsai W. Quality of life consequences of sleep-disordered breathing. J Allergy Clin Immunol. 1997;99(2):S750–6.
Hays JC, Blazer DG, Foley DJ. Risk of napping: excessive daytime sleepiness and mortality in an older community population. J Am Geriatr Soc. 1996;44(6):693–8.
Duss SB, Bauer-Gambelli SA, Bernasconi C, Dekkers MP, Gorban-Peric C, Kuen D, Bassetti CL. Frequency and evolution of sleep-wake disturbances after ischemic stroke: a 2-year prospective study of 437 patients. Sleep Med. 2023;101:244–51.
Kolla BP, He JP, Mansukhani MP, Kotagal S, Frye MA, Merikangas KR. Prevalence and correlates of hypersomnolence symptoms in US teens. J Am Acad Child Adolesc Psychiatr. 2019;58(7):712–20.
Charlton JL, Di Stefano M, Dimech-Betancourt B, Aburumman M, Osborne R, Peiris S, Koppel S. What is the motor vehicle crash risk for drivers with a sleep disorder? Trans Res Part F Traffic Psychol Behav. 2022;90:229–42.
Chen S, Wu H, Sun M, Wei Q, Zhang Q. Effects of shift work schedules, compensatory sleep, and work–family conflict on fatigue of shift-working nurses in Chinese intensive care units. Nursing Critical Care. 2023. https://doi.org/10.1111/nicc.12909.
Rodrigues H, Cobucci R, Oliveira A, Cabral JV, Medeiros L, Gurgel K, Gonçalves AK. Burnout syndrome among medical residents: a systematic review and meta-analysis. PloS ONE. 2018;13(11):e0206840.
Alves FR, de Souza EA, de França Ferreira LG, Neto JDOV, de Bruin VMS, de Bruin PFC. Sleep duration and daytime sleepiness in a large sample of Brazilian high school adolescents. Sleep Med. 2020;66:207–15.
Zerbini G, Merrow M. Time to learn: How chronotype impacts education. PsyCh journal. 2017;6(4):263–76.
Marta OFD, Kuo SY, Bloomfield J, Lee HC, Ruhyanudin F, Poynor MY, Chiu HY. Gender differences in the relationships between sleep disturbances and academic performance among nursing students: a cross-sectional study. Nurse Edu Today. 2020;85:104270.
Dagnew B, Andualem Z, Dagne H. Excessive daytime sleepiness and its predictors among medical and health science students of University of Gondar, Northwest Ethiopia: institution-based cross-sectional study. Health Qual Life Outcomes. 2020;18:1–7.
Faul F, Erdfelder E, Buchner A, Lang AG. Statistical power analyses using G* Power 3.1: tests for correlation and regression analyses. Behav Res Methods. 2009;41(4):1149–60.
Johns MW. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 1991;14(6):540–5.
Hoddes E, Zarcone V, Dement W. Stanford sleepiness scale. Enzyklopädie der Schlafmedizin. 1972;1184(1).
Buysse DJ, Reynolds CF III, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatr Res. 1989;28(2):193–213.
Horne JA, Ostberg O. A self-assessment questionnaire to determine morningness-eveningness in human circadian rhythms. Int J Chronobiol. 1976;4(2):97–110.
Johns MW. Reliability and factor analysis of the Epworth sleepiness scale. Sleep. 1992;15(4):376–81.
Mollayeva T, Thurairajah P, Burton K, Mollayeva S, Shapiro CM, Colantonio A. The Pittsburgh sleep quality index as a screening tool for sleep dysfunction in clinical and non-clinical samples: a systematic review and meta-analysis. Sleep Med Rev. 2016;25:52–73.
Witkowski S, Trujillo LT, Sherman SM, Carter P, Matthews MD, Schnyer DM. An examination of the association between chronic sleep restriction and electrocortical arousal in college students. Clin Neurophysiol. 2015;126(3):549–57.
Liguori G, Schuna J Jr, Mozumdar A. Semester long changes in sleep duration for college students. Coll Stud J. 2011;45(3):481–93.
Carciofo R. Morning affect or sleep inertia? Comparing the constructs and their measurement. Chronobiol Int. 2023;40(4):458–72.
Patterson PD, Okerman TS, Roach DG, Hilditch CJ, Weaver MD, Patterson CG, Weiss LS. Are short duration naps better than long duration naps for mitigating sleep inertia? Brief report of a randomized crossover trial of simulated night shift work. Prehospital Emergency Care. 2023. https://doi.org/10.1080/10903127.2023.2227696.
McCauley M, McCauley P, Kalachev L, Van Dongen H. 0190 Propensity for sleep inertia during sleep and its manifestation after awakening in a dynamic biomathematical fatigue model. Sleep. 2023;46(1):A84–A84.
Onyper SV, Thacher PV, Gilbert JW, Gradess SG. Class start times, sleep, and academic performance in college: a path analysis. Chronobiol Int. 2012;29(3):318–35.
Stock AA, Lee S, Nahmod NG, Chang AM. Effects of sleep extension on sleep duration, sleepiness, and blood pressure in college students. Sleep Health. 2020;6(1):32–9.
Waqas A, Khan S, Sharif W, Khalid U, Ali A. Association of academic stress with sleeping difficulties in medical students of a Pakistani medical school: a cross sectional survey. PeerJ. 2015;3:e840.
Khan A, Sriyanto S, Baranovich DL, Tahir LM, Panatik SA, Sasmoko S, Jabor MK. The relationship between positive mental health, academic stress and suicide ideation among Malaysian adolescents residing in Johor Bahru. Curr Psychol. 2022;42(18):15718–26.
Yousif MA, Arbab AH, Yousef BA. Perceived academic stress, causes, and coping strategies among undergraduate pharmacy students during the COVID-19 pandemic. Adv Med Edu Pract. 2022. https://doi.org/10.2147/AMEP.S350562.
Rodrigues RND, Viegas CA, Abreu e Silva AA, Tavares P. Daytime sleepiness and academic performance in medical students. Arquivos de Neuro-Psiquiatria. 2002;60:6–11.
Bagrowski B, Gutowska J. Sleep quality and the level of perceived stress in medical students. Roczniki Psychol. 2022;25(1):87–98.
Brown FC, Buboltz WC Jr, Soper B. Relationship of sleep hygiene awareness, sleep hygiene practices, and sleep quality in university students. Behav Med. 2002;28(1):33–8.
Forquer LM, Johnson CM. Continuous white noise to reduce sleep latency and night wakings in college students. Sleep Hypnosis. 2007;9(2):60.
Gellis LA, Park A, Stotsky MT, Taylor DJ. Associations between sleep hygiene and insomnia severity in college students: cross-sectional and prospective analyses. Behav Ther. 2014. https://doi.org/10.1016/j.beth.2014.05.002.
Beha Peach H, Gaultney JF, Gray DD. Sleep hygiene and sleep quality as predictors of positive and negative dimensions of mental health in college students. Cogent Psychol. 2016;3(1):1168768.
Peltz JS, Rogge RD. The indirect effects of sleep hygiene and environmental factors on depressive symptoms in college students. Sleep Health. 2016;2(2):159–66.
Trimmel K, Żebrowska M, Böck M, Stefanic A, Mayer D, Klösch G, Seidel S. Wanted: a better cut-off value for the Epworth sleepiness scale. Wiener Klinische Wochenschrift. 2018;130:349–55.
Heslop P, Smith GD, Metcalfe C, Macleod J, Hart C. Sleep duration and mortality: the effect of short or long sleep duration on cardiovascular and all-cause mortality in working men and women. Sleep Med. 2002;3(4):305–14.
Gallicchio L, Kalesan B. Sleep duration and mortality: a systematic review and meta-analysis. J Sleep Res. 2009;18(2):148–58.
Funding
The present work was funded by the University of Suffolk. There are no relevant financial or non-financial interests to disclose.
Author information
Authors and Affiliations
Contributions
AM managed the project, KB conceived the theoretical work, undertook all the experimental work and AM and KB drafted the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was conducted in accordance with the British Psychological Society code of Ethics and approved by the University of Sufolk Ethics Committee (Approval Reference RETH20/070 on 29 July 2021). Informed consent was obtained from all participants involved in the study.
Clinical trial
The current study did not use clinical trials.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Burrows, K., Millett, A. Higher education enrollment as a risk factor for somnolence and hypersomnolence. Discov Psychol 4, 45 (2024). https://doi.org/10.1007/s44202-024-00141-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44202-024-00141-6