Abstract
Background
Unnecessary caesarean births may be affected by physician factors, such as preferences, incentives and convenience. Delivery during office hours can be a valuable proxy for measuring such effects.
Objective
To determine the effect of office hours on the decision for caesarean delivery by assessing the odds of caesarean during office hours compared to out-of-office hours.
Search strategy
We searched CINAHL, ClinicalTrials.gov, The Cochrane Library, PubMed, Scopus and Web of Science from the beginning of records through August 2021.
Data collection and analysis
Search results were screened by three researchers. First, we selected studies that reported odds ratios of caesareans, or data allowing their calculation, for office and out-of-office hours. We extracted data on the study population, study design, data sources, setting, type of caesarean section, statistical analysis, and outcome measures. For groups reporting the same outcome, we performed a standard inverse-variance random-effects meta-analysis, which enabled us to calculate the overall odds ratios for each group. For groups reporting varying outcomes, we performed descriptive analysis.
Main results
Meta-analysis of weekday vs weekend for any caesarean section showed higher odds of caesarean during weekdays in adjusted analysis 1.40 (95%CI 1.13, 1.72 from 1,952,691 births). A similar effect was observed in the weekday vs Sunday comparison (1.39, 95%CI 1.10, 1.75, 150,932 births). A lower effect was observed for emergency CS, with a slight increase in adjusted analysis (1.06, 95%CI 0.90, 1.26, 2,622,772 births) and a slightly higher increase in unadjusted analysis (1.15, 95%CI 1.03, 1.29, 12,591,485 births). Similar trends were observed in subgroup analyses and descriptive synthesis of studies examining other office hours outcomes.
Conclusions
Delivery during office hours is associated with higher odds for overall caesarean sections and little to no effect for emergency caesarean. Non-clinical factors associated with office hours may influence the decision to deliver by caesarean section. Further detailed investigation of the “office hours effect” in delivery care is necessary and could lead to improvements in care systems.
Funding
The authors received no direct funding for this study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Since its introduction in medical practice, delivery by caesarean section (CS) has been associated with improved outcomes for mothers and infants [1]. While rates of 10-15% have been suggested as optimal, [2, 3] rates continue to surge in many countries beyond these widely accepted thresholds. In 2015, the global CS rate was estimated to be 21.1%,[4] with 2018 estimates of up to 17 million unnecessary CS [4]. Caesarean birth rates vary considerably between countries, with rates as low as 5% and as high as 58% [4, 5]. Like any other medical intervention, CS can have short and long term risks for mother and child [6]. Various studies have associated caesarean sections with an increased risk for stillbirth in subsequent childbirths, [7] placenta accreta spectrum, [8, 9] or diabetes development in childhood [10]. Moreover, overuse of caesarean sections is expensive, potentially wasting hospital resources and physician time [11,12,13,14].
The association of CS with health system factors has been investigated, and various factors appear to influence CS rates, including country-level factors [4, 12, 15, 16] such as cultural preferences, insurance systems, payment practices; [4, 17,18,19] hospital-level characteristics, such as for-profit or teaching status [17, 19,20,21] and micro-level factors, i.e. factors related to physician, [22] patient and clinical units [17, 23]. It has also been suggested that the delivery time may be associated with variation in CS rates [23, 24]. While this variation may result from the natural delivery cycle, [24,25,26] studies suggest health system factors may also be responsible [23, 24]. If we consider Wennberg types of care, CS, when clinically indicated, can be considered effective care, [27] important for the health of delivering mothers and their newborns. Nevertheless, it could also fall into the domain of preference and supply sensitive care when used without clear clinical indications.
In a hypothetical natural cycle of delivery, the CS rates should be the same within a given population or show only minor variation by time of day. However, in reality, higher CS rates are often observed during office hours (working days or hours). This effect may relate to physician and patient preferences or availability of maternity services, or a mixture of both. For example, CS overuse may reflect physician convenience, [23, 24, 28] i.e., it is easier to perform a CS during office hours. CS overuse during office hours may also reflect resource availability to perform operative work, or stronger incentives that are enacted via hospital strategies and arrangements, [28,29,30] and/or physicians’ incentives, [31] to perform more CS. Other factors may be relevant, including patient preferences, [32] manipulation of timing, [33] or physician practice style, which can be influenced by training and education [34]. We have included a conceptual framework for how office hours may influence CS rates (Additional file 1). Another critical hypothesis related to Wennberg types of care is that the office hours effect should be more prominent if clinical indications are not clear and less prominent if clinical indicators are unambiguous, i.e., when CS is the most effective or safest choice of care. For example, when there is an emergency during birth, i.e. foetal malposition or dystocia, there is little room for variation in clinical decision-making -- an emergency CS is often required. In cases where there are no medical indications for performing CS, some physicians may be more prone to perform one due to the influence of preference or supply factors, while others may be more bound to clinical criteria resulting in considerable variation in CS use. To explore this “office hours effect” and underlying factors at greater depths, we examined the relationship between time of delivery and CS through a systematic review of the relevant literature. This work sheds light on the effect of non-clinical factors on CS rates which could help address the overuse of CS in delivery care.
Materials and methods
The study was modelled after our previous meta-analyses [18, 19, 21, 22, 35] and was also designed to adhere to existing guidelines: the Preferred Reporting Items for Systematic Reviews (PRISMA),[36, 37] Conducting Systematic Reviews and Meta-Analyses of Observational Studies of Aetiology (COSMOS-E) [38] and Meta-analysis Of Observational Studies in Epidemiology (MOOSE) guidelines [39]. Prior to study initiation, the protocol was submitted to Prospero (CRD42020158434).
Search strategy and study inclusion criteria
We searched six databases: CINAHL, ClinicalTrials.gov, The Cochrane Library, PubMed, Scopus and Web of Science. We also augmented this with a manual search of the references of included studies. Our search strategy (available in the Additional file 1) was designed to obtain the broadest possible cross-section of data and was last updated in August 2021. Studies were excluded only to remove duplicate data. Exclusion criteria based on year of publication, country or language were not applied. We included studies that reported any, i.e. overall, or emergency CS by day of week or time of the day. The primary outcome was the odds ratio (OR) of CS by delivery time. Studies not reporting odd ratios but with information that allowed their calculation were also included. The suitability of studies for inclusion was assessed by independent reviewers (AL, GB, KG) by screening titles and abstracts followed by a full-text review. Any disagreements between reviewers were resolved by discussion or consultation with a senior reviewer (IH).
Data extraction
Data extraction from included studies was performed independently by three researchers (AL, GB and KG) and reviewed by a senior researcher (IH). A data extraction spreadsheet was designed to include the independent variable information, OR and confidence limits, sample size, covariates used for statistical adjustment, data on the study population and other characteristics of the included studies. We assessed all studies for risk of bias across six domains according to the Quality in Prognosis Studies (QUIPS) protocol [40]. Each study was assigned a risk of bias (low, medium or high) within six domains – study participation, study attrition, prognostic factor measurement, outcome measurement, study confounding, and statistical analysis and reporting.
Data analysis
The primary outcomes of interest were odds ratios and rates of CS. We report separate effect estimates for “any” or “emergency” CS. This distinction is critical as “any” CS rate includes planned CS, likely to be performed during office hours [41]. If CS occurred during labour, it would be considered an emergency CS, whereas if CS occurred without labour, it would be considered a planned CS. Using these types of CS outcomes was necessary to examine our study hypothesis. Any CS would show office hours effects likely caused by preference and supply factors. On the other hand, emergency CS, because it should be based solely on medical indications, should not be associated with office hours effects. However, observed effects may reflect practice patterns in dealing with medical indications for CS.
The primary variable of interest was time of delivery (office hours compared to out-of-office hours) as a proxy variable indicating preference and supply effects. The included studies examined the effect of office hours on CS using a variety of comparisons for the time of the day. For this reason, we assigned the effect estimates reported by studies to different groups: day vs night, evening vs night, day and evening vs night, day vs evening, weekday vs weekend, weekday vs Sunday, and office hours vs out-of-office hours, where ‘office hours’ denotes working hours during weekdays. The time classification of day, evening or night was not identical among the studies. As a result, we performed two types of analysis. First, we have performed a meta-analysis for studies where comparison groups matched (i.e. weekday vs weekend and weekday vs Sunday). We then performed a descriptive analysis without estimating an overall effect for other groups that did not report comparable delivery time comparisons. The analysis (meta-analysis or descriptive analysis) was performed for each comparison group separately.
We performed the meta-analysis for adjusted and crude estimates. Standard inverse-variance random-effects meta-analysis was used to obtain an overall OR. An overall OR lower than 1 denotes a decreased likelihood of CS during office hours. The heterogeneity of studies was determined using τ2. Values of 0.04, 0.16 and 0.36 represent low, moderate and high heterogeneity between studies [42]. For adjusted estimates, we conducted subgroup analysis by country, study design, CS rate, period of data collection, population by Robson groups and criteria, inclusion in the sample of women with existing conditions, type of data used and the domains of (QUIPS) risk of bias. Robson identifies ten groups using the onset of labour, presentation of foetus, previous CS, number of neonates and gestational age as criteria for classification [43]. We chose Robson groups and criteria because it is a well-known and easy to interpret metric valuable for identifying the risk for birth outcomes and the overuse of CS. In analysis, we use Robson groups and criteria because many studies do not report data by Robson groups, or report them for multiple groups. Having additional analysis by Robson criteria can somewhat compensate for this. In addition, as a measure of potential risk for CS, we have used an additional variable of whether women with existing conditions were included in the study sample.
Descriptive analysis was carried out for comparisons of: day vs night, evening vs night, day and evening vs night, day vs evening and office hours vs out-of-office hours. This included a presentation of effect estimates in a forest plot without meta-analysis. Together with effect estimates for each study, we present information on the country, sample size, study design, period of data collection, CS rate (if available), population by Robson group, source population, the inclusion of women with existing conditions in the study sample, and inclusion of births with conditions developed during delivery. The source population variable distinguishes if the sample was a sample of any risk cases or high-risk cases such as dystocia, gestational diabetes (GDM) and existing diabetes (GDM*) or second stage of labour malposition. The other two variables reported if the study sample included or excluded the women with existing conditions or conditions developed during pregnancy, both useful indicators for the inclusion of a higher risk population in the study sample.
Finally, we have graphically represented CS rates for office hours and out-of-office hours for outcomes (Any or Emergency CS) and comparisons (office hour categories).
Statistical analysis was carried out using STATA, release V.17 BE (StataCorp).
Results
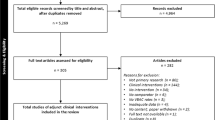
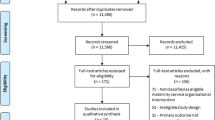
We identified 5935 records; 420 from CINAHL, 45 from ClinicalTrials.gov, 1193 from The Cochrane Library, 1923 from PubMed, 563 from Scopus, 1748 from Web of Science; and 43 from manual search (Fig. 1). We removed 932 duplicates. The remaining 5003 records were screened for eligibility by review of titles and abstracts, of which 3970 were excluded based on their focus on other medications or surgeries. The remaining 1033 articles were screened in full text. We removed studies which did not report shift (941), overlapping populations (1) and other irrelevant studies (39). We were finally left with 52 articles (53 studies), from which 29 studies were suitable for quantitative synthesis (meta-analysis) and 37 studies were suitable to be included in descriptive analysis [23, 24, 28, 31, 33, 34, 41, 44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89].
Characteristics of included studies are presented in Additional file 1. Studies were analysed with a focus on the circumstances surrounding delivery, type of CS, and the types of pregnancy according to the Robson Classification [90]. These studies were carried out in a diverse range of countries, with the population size of studies ranging from 266 to 8.62 million births, during the years 1982 to 2019 with most of them using hospital data. Study populations and variables used for statistical adjustment varied considerably.
Risk of bias of included studies
Confounding was the main source of bias for studies that reported any CS. Eight out of 32 studies had a moderate risk of bias, while 17 studies had a high risk of bias from confounding. Apart from a moderate risk of bias concerning study participation for three studies, all other studies had a low risk of bias across all remaining QUIPS domains. Similarly, studies across all domains had a low risk of bias except for confounding for emergency CS. In this domain, out of 22 reporting emergency CS, one study had a moderate risk of bias, and 15 had a high risk of bias.
Any caesarean section
Any CS was examined using 32 studies reported in 31 articles.
Meta-analysis
Figure 2 presents meta-analyses for the adjusted ORs of any CS, comparing weekdays with weekends (7 studies, 1,952,691 births) and weekdays with Sundays (5 studies, 150,932). We found that the odds of CS were 1.40 (95%CI 1.13, 1.72) during weekdays as compared to weekends and 1.39 (95%CI 1.10, 1.75) during weekdays as compared to Sundays, with low heterogeneity between studies (τ2 = 0.072, τ2 = 0.041).
Figure 3 displays the unadjusted analysis for weekday vs weekend analysis. Across 11 studies (3,610,230 births), we observed a higher OR for weekdays (1.41 95%CI 0.91, 2.18), with high heterogeneity among studies (τ2 = 0.539). Notably, one study by Palmer et al. showed lower odds of any caesarean during weekdays (0.52, 95%CI 0.52, 0.53), while all other studies reported higher odds of CS on weekdays. In the unadjusted analysis of 6 studies (24,192 births), comparing weekdays with Sundays, we found higher odds of any caesarean section on weekdays (1.44, 95%CI 1.24, 1.68) with no heterogeneity between studies (τ2 = 0.016).
Subgroup analysis of adjusted effect estimates
For weekdays and weekends comparison (Additional file 1), the higher odds during weekdays were present in all subgroups, including groups indicating clinical risk or other study characteristics. Tests for interaction across all subgroups were negative. Subgroup effect estimates ranged from 1.15 to 1.72. For example, the OR of CS in Robson groups 1 to 5 was 1.27 (95%CI 0.73, 2.21), for studies reporting data for all Robson groups, the OR was 1.47 (95%CI 1.36, 1.60), and for studies reporting data for multiple Robson groups, the OR was 1.38 (95%CI 1.16, 1.64). Studies with CS rates below or equal to 19% had an OR of 1.40 (95%CI 1.25, 1.57), those with rates of 20-40% the OR was 1.51 (95%CI 1.38, 1.66), and studies with CS rates over 40% the OR was 1.72 (95%CI 1.27, 2.35). In subgroup analysis for weekdays vs Sundays comparison, we also observed higher odds for CS, except for Mexico, studies reporting period before and after 2000, and studies not reporting CS rates. Subgroup effect estimates ranged from 0.71 to 2.05. Tests for interaction were positive for country (p for interaction = 0.001), period of data collection (p for interaction = 0.004) and CS rate (p for interaction = 0.003) (Additional file 1).
Descriptive analysis
Studies showed higher odds of CS during the days as compared to nights in all studies reporting adjusted estimates, with values ranging from 1.07 (95%CI 1.03, 1.12) [53] to 3.45 (95%CI 1.95, 6.09) [31] (Additional file 1). Studies also showed higher odds of CS during the evenings than during night shifts. Effect sizes varied from 1.40 (95%CI 0.48, 4.06) [59] to 4.65 (95%CI 3.13, 6.92) [65]. Single studies for day vs evening comparison (1.35, 95%CI 1.22, 1.49) [34] and office vs out-of-office hours comparison (2.36, 95%CI 1.37, 4.06), [23] again showed higher odds in daytime and office hours respectively. In the crude estimates, we observed similar trends. All included studies in a day vs night, evening vs night, day and evening vs night, and office vs out-of-office hours comparisons reported higher odds of CS during the day and/or evening, and office hours. Only one study reported a lower OR in the day vs evening comparison (Additional file 1) [80].
Emergency caesarean
Emergency CS was examined using 22 studies reported in the same number of articles.
Meta-analysis
There was a small difference in the odds of emergency CS on weekdays vs weekends comparison across four studies (2,622,772 births), with an overall odds ratio of 1.06 (95%CI 0.90, 1.26) and no relevant heterogeneity between studies (τ2 = 0.029, Fig. 4). The odds ratios varied between 0.89 (95%CI 0.78, 1.02) [86] to 1.37 (95%CI 1.33, 1.41) [58]. Only one study (8908 births) reported weekdays vs Sundays and showed higher odds during weekdays at 1.13 (95%CI 0.98, 1.31) [33]. In the analysis of unadjusted estimates from 8 studies (12,591,485 births), we found higher odds of CS on weekdays as compared to weekends (1.15, 95%CI 1.03, 1.29) with no relevant heterogeneity between studies (τ2 = 0.023, Fig. 5).
Subgroup analysis
There was considerable variation between pooled effect estimates among different subgroups for weekday vs weekend comparison. There was a positive test for interaction for the subgroups of women with existing conditions, birth registry data, and claims data. Pooled effect estimates ranged from 0.89 (95%CI 0.78, 1.02) to 1.37 (95%CI 1.33, 1.41). For example, in studies excluding women with existing conditions, the OR of CS was 1.37 (95%CI 1.33, 1.41), while the odds reported in studies including women with existing conditions the OR was 1.00 (0.97, 1.04). For studies with CS rates below or equal to 19% the OR was 1.17 (95%CI 0.86, 1.59) and with studies reporting rates of 20-40% the OR was 0.97 (95%CI 0.85, 1.10, Additional file 1).
Descriptive analysis
Adjusted ORs for day vs night comparison varied considerably in effect sizes. A study reported lower rates of emergency CS during the day (0.67, 95%CI 0.60, 0.75) [55]. Higher odds during daytime were reported by Sebastião and co-workers (1.19, 95%CI 1.16, 1.22) [81]. Higher odds were also reported for evenings compared to nights (1.50 95%CI 1.46, 1.54) [81] and office compared to out-of-office hours (1.06, 95%CI 1.02, 1.11) [23]. Trends were similar for unadjusted estimates.
CS rates analysis
Any caesarean
All studies showed higher CS rates during daytime compared to night. In addition, higher rates of CS during the day or weekday were observed for almost all studies in the day vs evening, weekday vs weekend comparison and all the studies in weekdays vs Sunday comparisons (Additional file 1). The CS rate was also considerably higher for office hours in a single study comparing office with out-of-office hours.
Emergency caesarean
We found a negligible difference between office and out-of-office hours comparisons for emergency CS rates. CS rates were often very close to each other and even lower during office hours.
Discussion
All meta-analyses reveal that women are more likely to undergo a caesarean delivery during office hours for any CS outcome, which is consistent with individual studies included in the descriptive analysis. The results of our meta-analysis for emergency CS show a small effect in adjusted, crude and subgroup analysis. Descriptive analysis of individual papers in other group comparisons shows variation in effect estimates below and above value 1.
Strengths and limitations
The major strengths of our meta-analysis include a broad literature search, screening and data extraction performed by multiple reviewers, an exploration of study characteristics as a potential source of variation between studies, and quality assessment using the QUIPS tool. We were able to include many studies with a large number of births. Most of the studies included in the meta-analysis used data from after 2000. Having more recent data is more beneficial for current discussions on CS rates. To consider the effect of medical risk for CS, we classified pregnancies according to Robson criteria and other clinical risk criteria, which were then used in subgroup analysis. The use of such clinical criteria enabled the assessment of the risk of pregnancy for study population with unambiguous and widely accepted categories. The challenge with Robson criteria was that most of the study populations belonged to multiple Robson groups, making it difficult to utilise fully such classification in subgroup analysis. The potential risk of bias in our review lies in the use of effect estimates that lacked control for known confounders. Many studies included in the review reported a moderate or high risk of bias for the confounding domain. The included papers also varied in terms of study designs. Using studies with different study designs can lead to biases associated with design features such as participant selection, sampling and data measurement. For this reason, we also examined and reported the study design in subgroup analysis. Variation in the study definitions of office hours was another major challenge which was solved with the organization of studies in different subgroups and performing only a descriptive analysis for studies that reported varying times.
Interpretation of the findings
Our analysis shows that regardless of clinical risk and other factors we examined, the odds for any CS were higher during office hours. This apparent CS overuse during office hours may be explained by preference and supply influences [23, 24, 28,29,30,31, 33, 59, 60, 62, 85, 91]. “Office hours effect” is likely a manifestation of many factors such as application of clinical guidelines, medical practice style, and induction to speed up the delivery process, as examples of preference-related factors. Financial incentives, availability of resources and other support are examples of supply-related factors that can contribute to such “effect” as well. Even factors such as patient behaviour, preferences [23, 46, 92] or convenience [24, 93,94,95] and strategies of clinicians to reduce complications and to avoid litigation can intermingle in the process [64, 96,97,98,99,100,101]. In contrast, the analysis shows negligible effect sizes for emergency CS indicating that when CS is the effective care option, the decision for CS is little affected by office hours. The variation in effect estimates for emergency CS during office hours in different studies may be an effect of inappropriate care, practice patterns among clinicians or medical reasons [23, 24, 28, 29, 31]. As a result, in any interpretation of the “time effect” on CS, we must consider the proxy nature of office hours as a variable which represents many of the above-highlighted effects.
Implications for health policy and clinical practice
Close to a third of primary caesarean deliveries in low-risk women could be avoided by altering the current maternity care practices [24, 98, 99]. The results of this study could help in the first step of avoiding unnecessary CS and improvement of systems of maternity care, that is, in understanding of how health system factors influence delivery care. More specifically, this study contributes to understanding of the role of preference and supply factors related to the “office hours effect” in the CS decisions. This review may also encourage review of clinical practice differences during office and out-of-office hours among clinicians, hospitals, regions and countries. The examination of the underlying causes behind the “office hours effect” will help identify real causes of this CS variation and direct remedies for addressing it. For example, physician preferences may be remedied with a consistent application of clinical guidelines and review of clinical decision making. Overuse due to financial incentives can be addressed with a review and change of payment mechanisms.
Implications for research
This review also provides information for the design of future studies and reviews of clinical decision making related to office hours effect on CS. In quantitative studies, we recommend that the effect of office hours be examined by level of patient risk, such as Robson groups or criteria, women with pre-existing conditions and conditions developed during pregnancy, i.e. material and/or foetal complications. This approach will limit confounding and provide greater clinical meaning to the analytical outcomes. Qualitative methods could also be useful in the examination of the “office hours effect”. Qualitative studies at the country, regional, or hospital level could help to distinguish the effects of specific underlying factors, only hinted in the existing research.
Conclusion
Delivery during office hours is associated with higher odds for caesarean sections overall and, to a lesser extent, for emergency caesarean. This review can enhance our understanding of non-clinical factors that influence caesarean rates, in particular the timing of caesareans. This review should encourage review and improvements in delivery care and support research that examines the underlying causes and outcomes of the “office hours effect” on caesarean section rates.
Availability of data and materials
All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf and declare: no support from any organization for the submitted work; no financial relationships with any organizations that might have an interest in the submitted work in the previous 3 years; no other relationships or activities that could appear to have influenced the submitted work. All authors had full access to all of the data (including statistical reports and tables) in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
References
Villar J, Carroli G, Zavaleta N, Donner A, Wojdyla D, Faundes A et al (2007) Maternal and neonatal individual risks and benefits associated with caesarean delivery: multicentre prospective study. BMJ 335(7628):1025. https://doi.org/10.1136/bmj.39363.706956.55 PubMed PMID: 17977819Epub 10/30
APPROPRIATE TECHNOLOGY FOR BIRTH (1985) Lancet 326(8452):436–437. https://doi.org/10.1016/S0140-6736(85)92750-3
Betrán AP, Ye J, Moller AB, Zhang J, Gülmezoglu AM, Torloni MR (2016) The increasing trend in caesarean section rates: global, regional and National Estimates: 1990-2014. PLoS One 11(2):e0148343. https://doi.org/10.1371/journal.pone.0148343 PubMed PMID: 26849801; PubMed Central PMCID: Pmc4743929. Epub 2016/02/06
Hoxha I, Fink G (2021) Caesarean sections and health financing: a global analysis. BMJ Open 11(5):e044383. https://doi.org/10.1136/bmjopen-2020-044383
Betran AP, Ye J, Moller A-B, Souza JP, Zhang J (2021) Trends and projections of caesarean section rates: global and regional estimates. BMJ Glob Health 6(6):e005671. https://doi.org/10.1136/bmjgh-2021-005671
Gregory KD, Jackson S, Korst L, Fridman M (2012) Cesarean versus vaginal delivery: whose risks? Whose benefits? Am J Perinatol 29(1):7–18. https://doi.org/10.1055/s-0031-1285829 PubMed PMID: 21833896. Epub 2011/08/13
Smith GC, Pell JP, Dobbie R (2003) Caesarean section and risk of unexplained stillbirth in subsequent pregnancy. Lancet (London, England) 362(9398):1779–1784. https://doi.org/10.1016/s0140-6736(03)14896-9 PubMed PMID: 14654315. Epub 2003/12/05
Cahill AG, Beigi R, Heine RP, Silver RM, Wax JR (2018) Placenta Accreta Spectrum. Am J Obstet Gynecol 219(6):B2–b16. https://doi.org/10.1016/j.ajog.2018.09.042 PubMed PMID: 30471891. Epub 2018/11/26
Renz-Polster H, David MR, Buist AS, Vollmer WM, O'Connor EA, Frazier EA et al (2005) Caesarean section delivery and the risk of allergic disorders in childhood. Clin Exp Allergy : J British Soc Allergy Clin Immunol 35(11):1466–1472. https://doi.org/10.1111/j.1365-2222.2005.02356.x PubMed PMID: 16297144. Epub 2005/11/22.
Cardwell CR, Stene LC, Joner G, Cinek O, Svensson J, Goldacre MJ et al (2008) Caesarean section is associated with an increased risk of childhood-onset type 1 diabetes mellitus: a meta-analysis of observational studies. Diabetologia. 51(5):726–735. https://doi.org/10.1007/s00125-008-0941-z PubMed PMID: 18292986. Epub 2008/02/23.
Entringer AP, Pinto M, Gomes M (2018) Cost-effectiveness analysis of natural birth and elective C-section in supplemental health. Rev Saude Publica 52:91. https://doi.org/10.11606/s1518-8787.2018052000373 PubMed PMID: 30484479; PubMed Central PMCID: Pmc6280622. Epub 2018/11/30.
Gibbons L, Belizán J, Lauer J, Betrán A, Merialdi M, Althabe F (2010) The global numbers and costs of additionally needed and unnecessary caesarean sections performed per year: overuse as a barrier to universal coverage HEALTH SYSTEMS FINANCING. World Health Report 2010:30
Saini V, Brownlee S, Elshaug AG, Glasziou P, Heath I (2017) Addressing overuse and underuse around the world. Lancet (London, England) 390(10090):105–107. https://doi.org/10.1016/s0140-6736(16)32573-9 PubMed PMID: 28077230. Epub 2017/01/13.
Berwick DM (2017) Avoiding overuse-the next quality frontier. Lancet (London, England) 390(10090):102–104. https://doi.org/10.1016/s0140-6736(16)32570-3 PubMed PMID: 28077229. Epub 2017/01/13.
Porreco RP, Thorp JA (1996) The cesarean birth epidemic: trends, causes, and solutions. Am J Obstet Gynecol 175(2):369–374. https://doi.org/10.1016/s0002-9378(96)70148-5 PubMed PMID: 8765255. Epub 1996/08/01.
Betran AP, Torloni MR, Zhang JJ, Gulmezoglu AM (2016) WHO statement on caesarean section rates. Bjog. 123(5):667–670. https://doi.org/10.1111/1471-0528.13526 PubMed PMID: 26681211; PubMed Central PMCID: PMC5034743. Epub 2015/12/19.
Hoxha I, Busato A, Luta X (2016) Medical practice variations in reproductive, obstetric, and gynecological care. In: Johnson A, Stukel TA (eds) Medical practice variations. Springer US, Boston, MA, pp 141–160
Hoxha I, Syrogiannouli L, Braha M, Goodman DC, da Costa BR, Juni P (2017) Caesarean sections and private insurance: systematic review and meta-analysis. BMJ Open 7(8):e016600. https://doi.org/10.1136/bmjopen-2017-016600 PubMed PMID: 28827257; PubMed Central PMCID: PMC5629699. Epub 2017/08/23.
Hoxha I, Syrogiannouli L, Luta X, Tal K, Goodman DC, da Costa BR et al (2017) Caesarean sections and for-profit status of hospitals: systematic review and meta-analysis. BMJ Open 7(2):e013670. https://doi.org/10.1136/bmjopen-2016-013670 PubMed PMID: 28213600; PubMed Central PMCID: Pmc5318567. Epub 2017/02/19.
Stafford RS (1991) The impact of nonclinical factors on repeat cesarean section. Jama. 265(1):59–63 Epub 1991/01/02. PubMed PMID: 1984126
Hoxha I, Zhubi E, Grezda K, Kryeziu B, Bunjaku J, Sadiku F et al (2021) Caesarean sections in teaching hospitals: systematic review and meta-analysis of hospitals in 22 countries. BMJ Open 11(1):e042076. https://doi.org/10.1136/bmjopen-2020-042076
Hoxha I, Sadiku F, Lama A, Bunjaku G, Agahi R, Statovci J et al (2020) Cesarean delivery and gender of delivering physicians: a systematic review and Meta-analysis. Obstet Gynecol 136(6):1170–1178. https://doi.org/10.1097/aog.0000000000004172 PubMed PMID: 00006250-202012000-00016
Hoxha I, Fejza A, Aliu M, Juni P, Goodman DC (2019) Health system factors and caesarean sections in Kosovo: a cross-sectional study. BMJ Open 9(4):e026702. https://doi.org/10.1136/bmjopen-2018-026702 PubMed PMID: 30975683; PubMed Central PMCID: PMC6500236. Epub 2019/04/13.
Clark SL, Perlin JB, Fraker S, Bush J, Meyers JA, Frye DR et al (2014) Association of obstetric intervention with temporal patterns of childbirth. Obstet Gynecol 124(5):873–880. https://doi.org/10.1097/aog.0000000000000485 PubMed PMID: 25437713. Epub 2014/12/02.
Bernis C, Varea C (2012) Hour of birth and birth assistance: from a primate to a medicalized pattern? American journal of human biology : the official journal of the Human Biology Council 24(1):14–21. https://doi.org/10.1002/ajhb.21228 PubMed PMID: 22121066. Epub 2011/11/29.
Mancuso PJ, Alexander JM, McIntire DD, Davis E, Burke G, Leveno KJ (2004) Timing of birth after spontaneous onset of labor. Obstet Gynecol 103(4):653–656. https://doi.org/10.1097/01.aog.0000118309.70035.63 PubMed PMID: 15051554. Epub 2004/03/31
Wennberg JE (2010) Tracking medicine: a Researcher's quest to understand health care. Oxford University Press
Grytten J, Skau I, Sorensen R (2011) Do expert patients get better treatment than others? Agency discrimination and statistical discrimination in obstetrics. J Health Econ 30(1):163–180. https://doi.org/10.1016/j.jhealeco.2010.10.004 PubMed PMID: 21095034
Grytten J, Monkerud L, Hagen TP, Sorensen R, Eskild A, Skau I (2011) The impact of hospital revenue on the increase in caesarean sections in Norway. A panel data analysis of hospitals 1976-2005. BMC Health Serv Res 11:267. https://doi.org/10.1186/1472-6963-11-267 PubMed PMID: 21992174; PubMed Central PMCID: PMC3210106. Epub 2011/10/14.
Faúndes A, Cecatti JG (1993) Which policy for caesarian sections in Brazil? An analysis of trends and consequences. Health Policy Plan 8(1):33–42
Mossialos E, Allin S, Karras K, Davaki K (2005) An investigation of Caesarean sections in three Greek hospitals: the impact of financial incentives and convenience. Eur J Pub Health 15(3):288–295. https://doi.org/10.1093/eurpub/cki002 PubMed PMID: 15923214. Epub 05/27.
Evans MI, Richardson DA, Sholl JS, Johnson BA (1984) Cesarean section. Assessment of the convenience factor. J Reprod Med 29(9):670–676 Epub 1984/09/01. PubMed PMID: 6541697
Fabbri D, Monfardini C, Castaldini I, Protonotari A (2016) Cesarean section and the manipulation of exact delivery time. Health Policy 120(7):780–789. https://doi.org/10.1016/j.healthpol.2016.05.001 PubMed PMID: 27263061. Epub 2016/06/06.
Burns LR, Geller SE, Wholey DR (1995) The effect of physician factors on the cesarean section decision. Med Care 33(4):365–382 Epub 1995/04/01. PubMed PMID: 7731278
Hoxha I, Braha M, Syrogiannouli L, Goodman DC, Jüni P (2019) Caesarean section in uninsured women in the USA: systematic review and meta-analysis. BMJ Open 9((3):e025356-e. https://doi.org/10.1136/bmjopen-2018-025356 PubMed PMID: 30833323
Moher D, Liberati A, Tetzlaff J, Altman DG, The PG (2009) Preferred reporting items for systematic reviews and Meta-analyses: The PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 372:n71. https://doi.org/10.1136/bmj.n71
Dekkers OM, Vandenbroucke JP, Cevallos M, Renehan AG, Altman DG, Egger M (2019) COSMOS-E: guidance on conducting systematic reviews and meta-analyses of observational studies of etiology. PLoS Med 16(2):e1002742. https://doi.org/10.1371/journal.pmed.1002742
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA. 283(15):2008–2012. https://doi.org/10.1001/jama.283.15.2008 PubMed PMID: 10789670. Epub 2000/05/02.
Hayden JA, van der Windt DA, Cartwright JL, Cote P, Bombardier C (2013) Assessing bias in studies of prognostic factors. Ann Intern Med 158(4):280–286. https://doi.org/10.7326/0003-4819-158-4-201302190-00009 PubMed PMID: 23420236
Wehberg S, Guldberg R, Gradel KO, Kesmodel US, Munk L, Andersson CB et al (2018) Risk factors and between-hospital variation of caesarean section in Denmark: a cohort study. BMJ Open 8(2):e019120. https://doi.org/10.1136/bmjopen-2017-019120 PubMed PMID: 29440158; PubMed Central PMCID: PMC5829888. Epub 2018/02/15.
da Costa BR, Juni P (2014) Systematic reviews and meta-analyses of randomized trials: principles and pitfalls. Eur Heart J 35(47):3336–3345. https://doi.org/10.1093/eurheartj/ehu424 PubMed PMID: 25416325
Robson MS (2001) Classification of caesarean sections. Fetal Matern Med Rev 12(1):23–39. Epub 2001/01/17. https://doi.org/10.1017/S0965539501000122
Aiken AR, Aiken CE, Alberry MS, Brockelsby JC, Scott JG (2015) Management of fetal malposition in the second stage of labor: a propensity score analysis. Am J Obstet Gynecol 212(3):355.e1–355.e7. https://doi.org/10.1016/j.ajog.2014.10.023
Bailit JL, Landon MB, Thom E, Rouse DJ, Spong CY, Varner MW et al (2006) The MFMU cesarean registry: impact of time of day on cesarean complications. Am J Obstet Gynecol 195(4):1132–1137 PubMed PMID: 106211278. Corporate author: US National Institute of Child Health and Human Development. Maternal-fetal medicine units network. Language: English. Entry date: 20070112. Revision date: 20150711. Publication Type: Journal Article
Barros AJD, Santos IS, Matijasevich A, Domingues MR, Silveira M, Barros FC et al (2011) Patterns of deliveries in a Brazilian birth cohort: almost universal cesarean sections for the better-off. Rev Saude Publica 45(4):635–643. https://doi.org/10.1590/s0034-89102011005000039 PubMed PMID: WOS:000292934600001
Bell EF, Hansen NI, Morriss FH Jr, Stoll BJ, Ambalavanan N, Gould JB et al (2010) Impact of timing of birth and resident duty-hour restrictions on outcomes for small preterm infants. Pediatrics. 126(2):222–231. https://doi.org/10.1542/peds.2010-0456 PubMed PMID: 20643715; PubMed Central PMCID: 2924191
Bertollini R, DiLallo D, Spadea T, Perucci C (1992) Cesarean section rates in Italy by hospital payment mode: an analysis based on birth certificates. Am J Public Health 82(2):257–261 Epub 1992/02/01. PubMed PMID: 1739159
Bommarito KM, Gross GA, Willers DM, Fraser VJ, Olsen MA (2016) The effect of clinical Chorioamnionitis on cesarean delivery in the United States. Health Serv Res 51(5):1879–1895. https://doi.org/10.1111/1475-6773.12447 PubMed PMID: WOS:000384752600009
Brookfield KF, O'Malley K, El-Sayed YY, Blumenfeld YJ, Butwick AJ (2016) Does Time of Delivery Influence the Risk of Neonatal Morbidity? Am J Perinatol 33(5):502–509. https://doi.org/10.1055/s-0035-1567891 PubMed PMID: 26595143. Epub 11/23.
Busowski JD, Chez RA, Goldfain VM (1997) The effect of a resident night team on cesarean delivery. Am J Perinatol 14(4):177–180. https://doi.org/10.1055/s-2007-994122 PubMed PMID: 9259923
Butler K, Ramphul M, Dunney C, Farren M, McSweeney A, McNamara K et al (2014) A prospective cohort study of the morbidity associated with operative vaginal deliveries performed by day and at night. BMJ Open 4(10):e006291–e00629e. https://doi.org/10.1136/bmjopen-2014-006291 PubMed PMID: 25354825
Caceres IA, Arcaya M, Declercq E, Belanoff CM, Janakiraman V, Cohen B et al (2013) Hospital differences in cesarean deliveries in Massachusetts (US) 2004–2006: the case against case-mix artifact. PLoS One 8(3)
Campero L, Hernandez B, Osborne J, Morales S, Ludlow T, Munoz C (2004) Support from a prenatal instructor during childbirth is associated with reduced rates of caesarean section in a Mexican study. Midwifery. 20(4):312–323. https://doi.org/10.1016/j.midw.2004.04.002 PubMed PMID: 15571880. Epub 2004/12/02.
Campillo-Artero C, Serra-Burriel M, Calvo-Perez A (2018) Predictive modeling of emergency cesarean delivery. PLoS One 13(1):e0191248. https://doi.org/10.1371/journal.pone.0191248 PubMed PMID: 29360875; PubMed Central PMCID: PMC5779661. Epub 2018/01/24.
Caughey AB, Urato AC, Lee KA, Thiet MP, Washington AE, Laros RK (2008) Time of delivery and neonatal morbidity and mortality. Am J Obstet Gynecol 199(5). https://doi.org/10.1016/j.ajog.2008.03.046 PubMed PMID: WOS:000260585800019
de Almeida S, Bettiol H, Barbieri MA, da Silva AAM, Ribeiro VS (2008) Significant differences in cesarean section rates between a private and a public hospital in Brazil. Cadernos De Saude Publica 24(12):2909–2918. https://doi.org/10.1590/s0102-311x2008001200020 PubMed PMID: WOS:000262995900020
Del Carmen GA, Stapleton S, Qadan M, Del Carmen MG, Chang D (2020) Does the day of the week predict a cesarean section? A Statewide Analysis J Surg Res 245:288–294. https://doi.org/10.1016/j.jss.2019.07.027 PubMed PMID: 31421375
D'Orsi E, Chor D, Giffin K, Angulo-Tuesta A, Barbosa GP, Gama Ade S et al (2006) Factors associated with cesarean sections in a public hospital in Rio de Janeiro. Brazil Cad Saude Publica 22(10):2067–2078 Epub 2006/09/05. PubMed PMID: 16951878
Eze P, Lawani LO, Ukaegbe CI, Anozie OB, Iyoke CA (2019) Association between time of delivery and poor perinatal outcomes -an evaluation of deliveries in a tertiary hospital, south-East Nigeria. PLoS One 14(6):e0217943. https://doi.org/10.1371/journal.pone.0217943 PubMed PMID: 31181101; PubMed Central PMCID: 6557521
Frank-Wolf M, Tovbin J, Wiener Y, Neeman O, Kurzweil Y, Maymon R (2017) Is there a correlation between time of delivery and newborn cord pH? J Maternal-fetal & Neonatal Medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet 30(13):1637–1640. https://doi.org/10.1080/14767058.2016.1220526 PubMed PMID: 27491639
Fraser W, Usher RH, McLean FH, Bossenberry C, Thomson ME, Kramer MS et al (1987) Temporal variation in rates of cesarean section for dystocia: does “convenience” play a role? Am J Obstet Gynecol 156(2):300–304. https://doi.org/10.1016/0002-9378(87)90272-9
Freitas PF, Fernandes TM. Association between institutional factors, birth care profile, and cesarean section rates in Santa Catarina. ' 2016;19(3):525-538. https://doi.org/10.1590/1980-5497201600030005. PubMed PMID: 27849268. Epub 2016/11/17.
Goldstick O, Weissman A, Drugan A (2003) The circadian rhythm of "urgent" operative deliveries. Isr Med Assoc J 5(8):564–566 PubMed PMID: 12929294
Gomes UA, Silva AA, Bettiol H, Barbieri MA (1999) Risk factors for the increasing caesarean section rate in Southeast Brazil: a comparison of two birth cohorts, 1978-1979 and 1994. Int J Epidemiol 28(4):687–694. https://doi.org/10.1093/ije/28.4.687 PubMed PMID: 10480697
Gould JB, Qin C, Marks AR, Chavez G (2003) Neonatal mortality in weekend vs weekday births. Jama 289(22):2958–2962. https://doi.org/10.1001/jama.289.22.2958 PubMed PMID: 12799403
Hall ML, Alexander CH (1982) Fetal monitoring in a community hospital: analysis of health maintenance organization, fee-for-service, and clinic populations. Am J Obstet Gynecol 143(3):277–285. https://doi.org/10.1016/0002-9378(82)90817-1 PubMed PMID: 7081346. Epub 1982/06/01.
Kalogiannidis I, Margioula-Siarkou C, Petousis S, Goutzioulis M, Prapas N, Agorastos T (2011) Infant births during the internal night are at increased risk for operative delivery and NICU admission. Arch Gynecol Obstet 284(1):65–71. https://doi.org/10.1007/s00404-010-1602-2 PubMed PMID: 20652279
Knight HE, van der Meulen JH, Gurol-Urganci I, Smith GC, Kiran A, Thornton S et al (2016) Birth "out-of-hours": an evaluation of obstetric practice and outcome according to the presence of senior obstetricians on the labour Ward. PLoS Med 13(4):e1002000–e100200e. https://doi.org/10.1371/journal.pmed.1002000 PubMed PMID: 27093698
Kopec-Godlewska K, Pac A, Rozanska A, Wojkowska-Mach J (2018) Is Vaginal Birth without an Episiotomy a Rarity in the 21st Century? Cross-Sectional Studies in Southern Poland. Int J Environ Res Public Health 15(11). https://doi.org/10.3390/ijerph15112462 PubMed PMID: 30400584; PubMed Central PMCID: PMC6266457. Epub 2018/11/08.
Lee SK, Lee DS, Andrews WL, Baboolal R, Pendray M, Stewart S et al (2003) Higher mortality rates among inborn infants admitted to neonatal intensive care units at night. J Pediatr 143(5):592–597. https://doi.org/10.1067/s0022-3476(03)00367-6 PubMed PMID: 14615728
Librero J, Peiró S, Calderón SM (2000) Inter-hospital variations in caesarean sections. A risk adjusted comparison in the Valencia public hospitals. J Epidemiol Community Health 54(8):631–636. https://doi.org/10.1136/jech.54.8.631 PubMed PMID: 10890876
Liu L, Miller E, Yee L (2019) Association between time of day and performance, indications, and outcomes of obstetric interventions among nulliparous women delivering at term. J Perinatol 39:1–6. https://doi.org/10.1038/s41372-019-0353-6
Marquez-Calderon S, Ruiz-Ramos M, Juarez S, Lopez JL (2011) Caesarean Delivery in Andalusia, Spain. Relationship with Social, Clinical and Health Services Factors (2007-2009). Revista Espanola De Salud Publica 85(2):205–215. https://doi.org/10.1590/s1135-57272011000200008 PubMed PMID: WOS:000294121000008
Mgaya A, Hinju J, Kidanto H (2017) Is time of birth a predictor of adverse perinatal outcome? A hospital-based cross-sectional study in a low-resource setting, Tanzania. BMC Pregnancy Childbirth 17(1):184. https://doi.org/10.1186/s12884-017-1358-9 PubMed PMID: 28606111
Mitler LK, Rizzo JA, Horwitz SM (2000) Physician gender and cesarean sections. J Clin Epidemiol 53(10):1030–1035. https://doi.org/10.1016/s0895-4356(00)00221-3 PubMed PMID: 11027936
Osava RH, da Silva FMB, Tuesta EF, de Oliveira S (2011) do Amaral MCE. Cesarean sections in a birth center. Rev Saude Publica 45(6) PubMed PMID: WOS:000297802600006
Palmer WL, Bottle A, Aylin P (2015) Association between day of delivery and obstetric outcomes: observational study. BMJ. 351:h5774. https://doi.org/10.1136/bmj.h5774
Phillips RN, Thornton J, Gleicher N (1982) Physician bias in cesarean sections. Jama. 248(9):1082–1084 Epub 1982/09/03. PubMed PMID: 7109201
Saraiva JM, Gouveia HG, Goncalves AC (2017) Factors associated with cesarean sections in a high complexity university hospital in southern Brazil. Rev Gaucha Enferm 38(3):e69141. https://doi.org/10.1590/1983-1447.2017.03.69141 PubMed PMID: 29641683
Sebastião YV, Womack L, Vamos CA, Louis JM, Olaoye F, Caragan T et al (2016) Hospital variation in cesarean delivery rates: Contribution of individual and hospital factors in Florida. Am J Obstet Gynecol 214(1):123.e1–123e18. https://doi.org/10.1016/j.ajog.2015.08.027 PubMed Central PMCID: 26292046
Suzuki S, Nakai M, Hiraizumi Y, Satomi M (2010) Time of delivery and perinatal outcome. Journal of Nippon Medical School = Nippon Ika Daigaku zasshi 77(5):277–281. https://doi.org/10.1272/jnms.77.277 PubMed PMID: 21060241
Stivanello E, Rucci P, Lenzi J, Fantini MP (2014) Determinants of cesarean delivery: a classification tree analysis. BMC Pregnancy Childbirth 14:215. https://doi.org/10.1186/1471-2393-14-215 PubMed PMID: 24973937
Tamim H, El-Chemaly SY, Nassar AH, Aaraj AM, Campbell OM, Kaddour AA et al (2007) Cesarean delivery among nulliparous women in Beirut: assessing predictors in nine hospitals. Birth. 34(1):14–20. https://doi.org/10.1111/j.1523-536X.2006.00141.x PubMed PMID: 17324173; PubMed Central PMCID: 1913632
Woodhead N, Lindow S (2012) Time of birth and delivery outcomes: a retrospective cohort study. J Obstet Gynaecol 32(4):335–337. https://doi.org/10.3109/01443615.2012.664586 PubMed PMID: 22519475
Zbiri S, Rozenberg P, Goffinet F, Milcent C (2018) Cesarean delivery rate and staffing levels of the maternity unit. PLoS One 13(11):e0207379–e020737e. https://doi.org/10.1371/journal.pone.0207379 PubMed PMID: 30485335
Mirabal-Beltran R, Strobino DM (2020) Birth mode after primary cesarean among Hispanic and non-Hispanic women at one U.S. Institution Women's Health Issues 30(1):7–15. https://doi.org/10.1016/j.whi.2019.09.001
Takegata M, Ronsmans C, Nguyen HAT, Kitamura N, Iwasaki C, Toizumi M et al (2020) Socio-demographic factors of cesarean births in Nha Trang city. Vietnam: a community-based survey Trop Med Health 48:57. https://doi.org/10.1186/s41182-020-00239-2 PubMed PMID: 32669947; PubMed Central PMCID: PMC7350841. Epub 2020/07/17
Gould JB, Qin C, Chavez G (2005) Time of birth and the risk of neonatal death. Obstet Gynecol 106(2):352–358. https://doi.org/10.1097/01.AOG.0000168627.33566.3c PubMed PMID: 00006250-200508000-00023
Robson M, Murphy M, Byrne F (2015) Quality assurance: The 10-group classification system (Robson classification), induction of labor, and cesarean delivery. Int J Gynecol Obstet 131(S1):S23–SS7. https://doi.org/10.1016/j.ijgo.2015.04.026
Phadungkiatwattana P, Tongsakul N (2011) Analyzing the impact of private service on the cesarean section rate in public hospital Thailand. Arch Gynecol Obstet 284(6):1375–1379. https://doi.org/10.1007/s00404-011-1867-0 PubMed PMID: 21359844. Epub 02/27.
Barros FC, Vaughan JP, Victora CG (1986) Why so many caesarean sections? The need for a further policy change in Brazil. Health Policy Plan 1(1):19–29 Epub 1986/02/09. PubMed PMID: 10283013
Campo-Engelstein L, Howland LE, Parker WM, Burcher P (2015) Scheduling the stork: media portrayals of Women's and Physicians' reasons for elective cesarean delivery. Birth. 42(2):181–188. https://doi.org/10.1111/birt.12161 PubMed PMID: 25881794. Epub 2015/04/18.
Loewenstein G, Asch DA, Volpp KG (2013) Behavioral economics holds potential to deliver better results for patients, insurers, and employers. Health affairs (Project Hope) 32(7):1244–1250. https://doi.org/10.1377/hlthaff.2012.1163 PubMed PMID: 23836740. Epub 2013/07/10.
Volpp KG, Asch DA, Galvin R, Loewenstein G (2011) Redesigning employee health incentives — lessons from behavioral economics. N Engl J Med 365(5):388–390. https://doi.org/10.1056/NEJMp1105966
Boerma T, Ronsmans C, Melesse DY, Barros AJD, Barros FC, Juan L et al (2018) Global epidemiology of use of and disparities in caesarean sections. Lancet. 392(10155):1341–1348. https://doi.org/10.1016/s0140-6736(18)31928-7 PubMed PMID: 30322584. Epub 2018/10/17.
Berkowitz GS, Fiarman GS, Mojica MA, Bauman J, de Regt RH (1989) Effect of physician characteristics on the cesarean birth rate. Am J Obstet Gynecol 161(1):146–149. https://doi.org/10.1016/0002-9378(89)90252-4
Iriye BK, Huang WH, Condon J, Hancock L, Hancock JK, Ghamsary M et al (2013) Implementation of a laborist program and evaluation of the effect upon cesarean delivery. Am J Obstet Gynecol 209(3):251.e1–251.e6. https://doi.org/10.1016/j.ajog.2013.06.040 PubMed PMID: 23904102. Epub 2013/08/02.
Clark SL (2009) Sleep deprivation: implications for obstetric practice in the United States. Am J Obstet Gynecol 201(2):136.e1–136.e4. https://doi.org/10.1016/j.ajog.2009.01.013 PubMed PMID: 19344882. Epub 2009/04/07.
Savage W, Francome C (2007) British consultants' attitudes to caesareans. J Obstet Gynaecol 27(4):354–359. https://doi.org/10.1080/01443610701327354 PubMed PMID: 17654184. Epub 2007/07/27.
Bettes BA, Coleman VH, Zinberg S, Spong CY, Portnoy B, DeVoto E et al (2007) Cesarean delivery on maternal request: obstetrician-gynecologists' knowledge, perception, and practice patterns. Obstet Gynecol 109(1):57–66. https://doi.org/10.1097/01.AOG.0000249608.11864.b6 PubMed PMID: 17197588. Epub 2007/01/02.
Acknowledgments
We thank Altina Bimbashi, Dorentina Kuqi, Melisa Uka and Vesa Osmani for the graphic design of the figures and Altina Bimbashi and Dorentina Kuqi for technical assistance with data.
Funding
We report no financial, personal, political, intellectual or religious interests relevant to this work.
Our study used data from existing studies, rather than data directly from human or animal subjects, and thus did not require ethics board approval.
No funding was received to perform this study.
Author information
Authors and Affiliations
Contributions
IH conceived and designed the study. IH, AL, GB, KG performed the screening of studies, data extraction and preparation. IH and AL performed quality assessment of the studies. IH has analysed the data. IH, AL and RA drafted the paper, and PB and DG contributed to the interpretation of the results and editing the paper. The paper was critically reviewed and approved by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors report no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hoxha, I., Lama, A., Bunjaku, G. et al. Office hours and caesarean section: systematic review and Meta-analysis. Res Health Serv Reg 1, 4 (2022). https://doi.org/10.1007/s43999-022-00002-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43999-022-00002-6