Abstract
Background
Transition from residency to unsupervised practice represents a critical stage in learning and professional identity formation, yet there is a paucity of literature to inform residency curricula and emergency department transition programming for new faculty.
Objective
The objective of this study was to develop consensus-based recommendations to optimize the transition to practice phase of emergency medicine training.
Methods
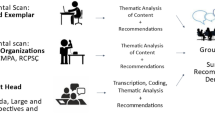
A literature review and results of a survey of emergency medicine (EM) residency program directors informed focus groups of recent (within 5 years) EM graduates. Focus group transcripts were analyzed following conventional content analysis. Preliminary recommendations, based on identified themes, were drafted and presented at the 2022 Canadian Association of Emergency Physicians (CAEP) Academic Symposium on Education. Through a live presentation, symposium attendees representing the Canadian national EM community participated in a facilitated discussion of the recommendations. The authors incorporated this feedback to construct a final set of 14 recommendations, 8 targeted toward residency training programs and 6 specific to department leadership.
Conclusion
The Canadian EM community used a structured process to develop 14 best practice recommendations to enhance the transition to practice phase of residency training as well as the transition period in the career of junior attending physicians.
Abstrait
Arrière-plan
La transition de la résidence à la pratique non supervisée représente une étape cruciale de l’apprentissage et de la formation de l’identité professionnelle, mais il y a peu de documentation pour éclairer les programmes de résidence et les programmes de transition des services d’urgence pour les nouveaux professeurs.
Objectif
L’objectif de cette étude était d’élaborer des recommandations consensuelles pour optimiser la transition vers la pratique de la formation en médecine d’urgence.
Méthodes
Une recension des écrits et les résultats d’un sondage auprès des directeurs des programmes de résidence en médecine d’urgence (GU) ont informé les groupes de discussion des diplômés récents (moins de cinq ans) en GU. Les transcriptions des groupes de discussion ont été analysées à la suite d’une analyse du contenu classique. Des recommandations préliminaires, fondées sur des thèmes déterminés, ont été rédigées et présentées au Symposium universitaire sur l’éducation de 2022 de l’Association canadienne des médecins d’urgence (ACMU). Au moyen d’une présentation en direct, les participants au symposium représentant la communauté nationale canadienne de la GU ont participé à une discussion dirigée sur les recommandations. Les auteurs ont intégré ces commentaires pour élaborer un ensemble final de 14 recommandations, 8 ciblant les programmes de formation en résidence et 6 ciblant le leadership ministériel.
Conclusions
La communauté canadienne de la GU a utilisé un processus structuré pour élaborer 14 recommandations de pratiques exemplaires afin d’améliorer la transition à la phase de pratique de la formation en résidence ainsi que la période de transition dans la carrière des médecins traitants débutants.
Similar content being viewed by others
Data availability
Not applicable.
References
Salib S, Moreno A. Good-bye and good luck: teaching residents the business of medicine after residency. J Grad Med Educ. 2015;7(3):338–40.
Shaffer R, Piro N, Katznelson L, Gephart MH. Practice transition in graduate medical education. Clin Teach. 2017;14(5):344–8.
Holak EJ, Kaslow O, Pagel PS. Facilitating the transition to practice: a weekend retreat curriculum for business-of-medicine education of United States anesthesiology residents. J Anesth. 2010;24(5):807–10.
Schlumbrecht M, Siemon J, Morales G, Huang M, Slomovitz B. Preparation in the business and practice of medicine: perspectives from recent gynecologic oncology graduates and program directors. Gynecol Oncol Res Pract. 2017;4(1):14.
Williams LL. Teaching residents practice-management knowledge and skills: an in vivo experience. Acad Psychiatry. 2009;33(2):135–8.
Westerman M, Teunissen PW, van der Vleuten CPM, Scherpbier AJJA, Siegert CEH, van der Lee N, et al. Understanding the transition from resident to attending physician: a transdisciplinary. Qual Study Acad Med. 2010;85(12):1914–9.
Beckett M. The new consultant survey 2005. Emerg Med J. 2006;23(6):461–3.
Royal College of Physicians and Surgeons of Canada. Competence By Design [Internet]. 2017 [cited 2017 Sep 12]. http://www.royalcollege.ca/rcsite/cbd/competence-by-design-cbd-e. Accessed 15 May 2022
Royal College of Physicians and Surgeons of Canada. Specialty Education Design [Internet]. Royal College of Physicians and Surgeons of Canada. 2018 [cited 2018 Apr 12]. http://www.royalcollege.ca/rcsite/cbd/cbd-specialty-education-design-sed-e. Accessed 15 May 2022
Nath A, Yadav K, Chagnon N, Cheung WJ. Competency based medical education (CBME) in CCFP(EM) programs. CJEM. 2022;24(6):599–605.
Nath A, Cheung WJ, Leppard J, Perry JJ. A novel transition to practice curriculum for CCFP(EM) programs. Can J Emerg Med. 2021;23(3):394–7.
Thomas P, Kern D, Hughes M, Chen B. Curriculum development for medical education: a six-step approach. Baltimore: Johns Hopkins University Press; 2016.
Dillman D. Mail and internet surveys: the tailored design method. 2nd ed. Hoboken: Wiley; 2007.
Hsieh HF, Shannon S. Three approaches to qualitative content analysis. Qual Health Res [Internet]. 2005;15(9):1277–88. https://doi.org/10.1177/1049732305276687.
Dye J, Schatz I, Rosenberg B, Coleman S. Constant comparison method: A kaleidoscope of data. Qual Rep. 2000;4(1):1–10.
Morrow S. Quality and trustworthiness in qualitative research in counseling psychology. J Couns Psychol. 2005;52:250–60.
Thomson B, O’Halloran H, Wu L, Gauthier S, Taylor D. Transition to practice curriculum for general internal medicine physicians: scoping review and Canadian national survey. BMC Med Educ. 2022;22(1):609.
Bennett N, Lockyer J, Mann K, Batty H, LaForet K, Rethans JJ, et al. Hidden curriculum in continuing medical education. J Contin Educ Heal Prof. 2004;24(3):145–52.
Caretta-Weyer H. Transition to practice: a novel life skills curriculum for emergency medicine residents. Western Journal of Emergency Medicine [Internet]. 2018 Nov 19;20(1):100–4. https://escholarship.org/uc/item/9cj711jz. Accessed 15 May 2022
Kennedy TJT, Regehr G, Baker GR, Lingard LA. Progressive independence in clinical training: a tradition worth defending? Acad Med. 2005;80(Supplement):S106–11.
Yardley S, Westerman M, Bartlett M, Walton JM, Smith J, Peile E. The do’s, don’t and don’t knows of supporting transition to more independent practice. Perspect Med Educ. 2018;7(1):8–22.
Royal College of Physicians and Surgeons of Canada. Standards of accreditation for residency programs in Emergency Medicine. Ottawa; 2020.
Sawatsky AP, O’Brien BC, Hafferty FW. Autonomy and developing physicians: Reimagining supervision using self-determination theory. Med Educ. 2022;56(1):56–63.
Yiu S, Yeung M, Cheung W, Frank JR. Stress and conflict from tacit culture forges professional identity in newly graduated independent physicians. Adv Health Sci Educ. 2022. https://doi.org/10.1007/s10459-022-10173-z.
Falvo T, McKniff S, Smolin G, Vega D, Amsterdam JT. The business of emergency medicine: a nonclinical curriculum proposal for emergency medicine residency programs. Acad Emerg Med. 2009;16(9):900–7.
Sanaee L, Glover Takahashi S, Nayer M. Practical solutions for implementation of Transition to Practice curricula in a competency-based medical education model. Can Med Educ J. 2020;11(4):e39–50.
Cogbill TH, Shapiro SB. Transition from training to surgical practice. Surg Clin N Am. 2016;96(1):25–33.
Lister JR, Friedman WA, Murad GJ, Dow J, Lombard GJ. Evaluation of a transition to practice program for neurosurgery residents: creating a safe transition from resident to independent practitioner. J Grad Med Educ. 2010;2(3):366–72.
Landreville J, Cheung W, Frank J, Richardson D. A definition for coaching in medical education. Can Med Educ J. 2019;10(4):109–10.
Mazotti L, O’Brien B, Tong L, Hauer KE. Perceptions of evaluation in longitudinal versus traditional clerkships. Med Educ [Internet]. 2011 May [cited 2014 Sep 30];45(5):464–70. http://www.ncbi.nlm.nih.gov/pubmed/21486322. Accessed 15 May 2022
Teherani A, O’Brien BC, Masters DE, Poncelet AN, Robertson PA, Hauer KE. Burden, responsibility, and reward: preceptor experiences with the continuity of teaching in a longitudinal integrated clerkship. Acad Med [Internet]. 2009 Oct;84(10 Suppl):S50–3. http://www.ncbi.nlm.nih.gov/pubmed/19907386. Accessed 15 May 2022
Ries A, Wingard D, Morgan C, Farrell E, Letter S, Reznik V. Retention of Junior Faculty in Academic Medicine at the University of California, San Diego. Acad Med. 2009;84(1):37–41.
Jackson VA, Palepu A, Szalacha L, Caswell C, Carr PL, Inui T. “Having the right chemistry”: a qualitative study of mentoring in academic medicine. Academic Medicine [Internet]. 2003 Mar;78(3):328–34. http://journals.lww.com/00001888-200303000-00020. Accessed 15 May 2022
Lucas R, Dandar V. Importance of mentoring on workplace engagement of emergency medicine faculty: a multi-institutional study. Western J Emerg Med. 2021;22(3):653–9.
Yeung M, Nuth J, Stiell IG. Mentoring in emergency medicine: the art and the evidence. CJEM. 2010;12(02):143–9.
Yeung M, Cheung WJ, Hebert G, Gee A. P144: “I wasn’t oriented a lot, so I’m essentially learning as I go”: onboarding and transition to practice of new emergency physicians. CJEM. 2019;21(S1):S116.
Calder LA, Mastoras G, Rahimpour M, Sohmer B, Weitzman B, Cwinn AA, et al. Team communication patterns in emergency resuscitation: a mixed methods qualitative analysis. Int J Emerg Med. 2017;10(1):24.
Tallentire VR, Smith SE, Skinner J, Cameron HS. Understanding the behaviour of newly qualified doctors in acute care contexts. Med Educ. 2011;45(10):995–1005.
Ramani S, Könings KD, Ginsburg S, van der Vleuten CPM. Meaningful feedback through a sociocultural lens. Med Teach. 2019;41(12):1342–52.
Cantillon P, Dornan T, de Grave W. Becoming a clinical teacher: identify formation in context. Acad Med. 2019;94(10):1610–8.
Ramani S, Könings KD, Ginsburg S, van der Vleuten CPM. Twelve tips to promote a feedback culture with a growth mind-set: swinging the feedback pendulum from recipes to relationships. Med Teach. 2019;41(6):625–31.
Acknowledgements
The research team would like to thank the Canadian Association of Emergency Physicians for administrative support throughout the research process as well as all participants of the CAEP 2022 Academic Symposium, held in Quebec City, Canada, on May 25, 2022.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest.
Ethical approval
Ethics exemption was granted by the University of Manitoba Bannatyne Campus Research Ethics Board.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
McColl, T., Paterson, Q., Yiu, S. et al. Ready for practice? National recommendations for emergency medicine transition to practice curriculum. Can J Emerg Med 25, 558–567 (2023). https://doi.org/10.1007/s43678-023-00534-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43678-023-00534-x
Keywords
- Medical education
- Transition to practice
- Emergency medicine
- Competency based education
- Competence By Design