Abstract
Squamous cell carcinoma represents the second most common type of keratinocyte carcinoma with ultraviolet radiation (UVR) making up the primary risk factor. Oral photoprotection aims to reduce incidence rates through oral intake of photoprotective compounds. Recently, drug repurposing has gained traction as an interesting source of chemoprevention. Because of their reported photoprotective properties, we investigated the potential of bucillamine, carvedilol, metformin, and phenformin as photoprotective compounds following oral intake in UVR-exposed hairless mice. Tumour development was observed in all groups in response to UVR, with only the positive control (Nicotinamide) demonstrating a reduction in tumour incidence (23.8%). No change in tumour development was observed in the four repurposed drug groups compared to the UV control group, whereas nicotinamide significantly reduced carcinogenesis (P = 0.00012). Metformin treatment significantly reduced UVR-induced erythema (P = 0.012), bucillamine and phenformin increased dorsal pigmentation (P = 0.0013, and P = 0.0005), but no other photoprotective effect was observed across the repurposed groups. This study demonstrates that oral supplementation with bucillamine, carvedilol, metformin, or phenformin does not affect UVR-induced carcinogenesis in hairless mice.
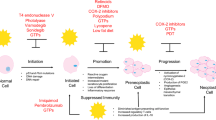
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Drug repurposing is the strategy of reusing drug candidates for treatment options other than their original intention [1]. Drug repurposing is associated with lower risk as trials will build upon previous experiences, including safety data from animal and human studies. Repurposing may also provide a reduction in both the time frame and associated costs during development [2]. Finally, prior knowledge of demonstrated effects and mechanisms of action eases the identification of new disease targets [3].
Cutaneous squamous cell carcinomas (SCCs) are predominantly induced by ultraviolet radiation (UVR) [4]. Incidence rates have risen across the world with further increases predicted in the future [5,6,7]. Classical prevention methods such as sunscreen use have proven insufficient, creating a need for innovation within photoprotection [8]. Oral intake of compounds that counteract the damaging effects of UVR could boost protection against UVR-induced SCCs [9].
Drug repurposing represents an interesting avenue for oral photoprotection. Metformin and phenformin are antidiabetic drugs that function as 5′ AMP-activated protein kinase activators, demonstrating varying degrees of photoprotection. Both topical and gavage-delivered metformin protected against tumour development in hairless mice [10], whereas phenformin reduced 12-O-tetra-decanoylphorbol-13-acetate induced skin tumourigenesis [11]. Topical use of the β-blocker carvedilol, commonly used to treat heart disease, has been shown to inhibit UVR-induced carcinogenesis in hairless mice in two separate studies, demonstrating protection against skin inflammation and cyclobutane pyrimidine dimers [12, 13]. As a final candidate, bucillamine, a cysteine derivate most recently tested as a treatment for COVID-19 [14], has demonstrated photoprotection against UVR-induced cell proliferation, apoptosis, and MAPK signalling following systemic treatment [15, 16].
In the present study, we investigated the potential of drug repurposing in UVR-induced squamous cell carcinoma in hairless mice. With reports of photoprotective effects, we tested whether the observed photoprotection could be translated to oral photoprotection against UVR-induced skin cancer.
2 Materials and methods
2.1 Compounds
Bucillamine, carvedilol, metformin, and phenformin were purchased from Biosynth. Nicotinamide was purchased from Sigma-Aldrich. Once a week, bucillamine was weighed and the powder was placed in seven amber blue-cap bottles stored at − 20 °C. Each morning, the powder of one bottle was solubilised in tap water and transferred to a drinking bottle. Nicotinamide and phenformin were frozen at − 20 °C as aliquots once a week. Each morning, one aliquot was taken out and thawed, diluted in tap water, and transferred to a drinking bottle. Metformin was prepared weekly in aqueous solution. New solution was transferred to a drinking bottle each morning. Carvedilol was added to Altromin 1320 feed (Altromin Spezialfutter GmbH & Co. KG, Lage, Germany) produced every second month. The feed was replaced once a week.
2.2 Animals
All study protocols were approved and carried out under the recommendation and guidelines of the Danish Animal Experiments Inspectorate (permit number: 2021-15-0201-00905) and the local animal welfare committee at Bispebjerg Hospital, Denmark. Female C3.Cg-Hrhr/TifBomTac hairless mice (n = 150, ages 19 to 42 weeks) from Taconic (Ry, Denmark) were used in this study. After acclimatisation for at least 2 weeks, the animals were housed under standard conditions as previously described [17].
2.3 Drug treatments and UVR-induced carcinogenesis
A total of 150 mice were randomised into six groups of 25 mice each. The groups were (i) 20 mg/kg bucillamine [15, 16], (ii) 7.25 mg/kg carvedilolFootnote 1, (iii) 300 mg/kg metformin [10], (iv) 100 mg/kg phenformin [11], (v) 600 mg/kg nicotinamide as a positive control [17], and (vi) no drug treatment, UVR control. All drug treatments were delivered through the drinking water, except for (ii) which was supplemented through the feed. UVR protocol was initiated after the first 2 weeks of drug treatment. All mice were irradiated with UVR 3 times a week with 3.5 standard erythema doses. The UV source has previously been described [17]. To estimate tumour development, tumours reaching 1 mm or above were counted and measured weekly.
2.4 Erythema, pigmentation, and weight
Mice were weighed monthly to monitor health status. UVR-induced erythema was measured once a week for the first 6 weeks of UVR as described previously [17]. In brief, dorsal erythema was measured 30 min after UVR on a scale of no erythema (0), mild erythema (1) to very severe erythema (4). Pigmentation induced by UVR was estimated visually guided by the use of long-wave fluorescent UVA tubes as previously described [17].
2.5 Euthanasia and final measurements
Mice were euthanised using carbon dioxide according to protocol when an endpoint was reached, either (i) one tumour measuring 12 mm in diameter, or (ii) three 4 mm tumours [17]. To ensure the included tumours were squamous cell carcinomas and not benign neoplasms, only tumours measuring 4 mm or above were included in further analysis. Tumour area was calculated with the formula: \({\text{tumour}}\;{\text{area}} =\uppi \cdot \left( {\frac{{{\text{tumour}}\;{\text{length}}}}{2}} \right) \cdot \left( {\frac{{{\text{tumour}}\;{\text{width}}}}{2}} \right)\) [17]. Immediately following euthanasia, the ears of the mouse were removed, six 4 mm punch biopsies collected from the ears and weighed for estimation of oedema formation as previously described [17]. Non-tumour skin was collected and stored at − 80 °C. Sections of 10 µm were prepared and stained with haematoxylin and eosin (HE) to evaluate epidermal thickness.
2.6 Statistical analysis
Statistical analysis was performed using R version 4.1.0 [19]. A Kaplan–Meier survival curve was used to visualise tumour development, and data were analysed with a log-rank test (Mantel–Cox) [20]. Statistical differences between groups were otherwise determined using a Mann–Whitney U test with p-values below 0.05 indicating significance.
3 Results
3.1 Drug treatment toxicity and health status
To ensure safe and tolerable doses, subsections of five mice were treated for 2 weeks with the drug doses in Table 1. Based on previous experience [17], nicotinamide treatment (600 mg/kg) was considered safe and therefore not tested. No change in food or water intake was found during this period (data not shown). To initialise the study, drug treatments were administered to all respective groups for 2 weeks prior to UVR exposure. Following 1 week of treatment, three mice treated with phenformin were found dead. Brief autopsy of the mice did not identify any specific cause and no histology was performed, in part because of the state of the organs. The phenformin dose was reduced from 100 to 75 mg/kg (Table 1), whereafter no further toxicity was demonstrated, indicated by no difference in overall deaths over the course of the study (data not shown). No significant weight loss was observed, but treatment with bucillamine and phenformin significantly increased the percentage weight gain compared to the UV control group (Fig. 1). One mouse from the nicotinamide group was euthanised because of ringtail disease. Following tumour development, three mice in the phenformin group were euthanised because of blood loss due to bleeding from their tumours.
3.2 Effects of drug treatment on murine skin changes
The effects of drug treatment on UVR-induced erythema and pigmentation are shown in Fig. 2. All groups developed erythema in response to the first UVR exposure (Fig. 2A, B), and erythema was decreasingly detectable up to week 6. Metformin treatment significantly reduced erythema expressed as the accumulated score over 6 weeks compared to the UV control (Fig. 3A and Table 2). As shown in Fig. 2C, C3.Cg-Hrhr/TifBomTac mice develop pigmentation in response to UVR. Treatment with bucillamine, phenformin, and the positive control nicotinamide significantly increased pigmentation measured at the end of the study period (week 30; Fig. 3B and Table 2). To evaluate the effects on UVR-induced inflammation, oedema formation measured by ear punch weight was considered. UV control mice had a median ear weight of 3.98 mg, which was not changed by any of the treatments (Table 2). Histological examination of HE-stained skin sections (Fig. 4) revealed no difference in epidermal thickness compared to the UV control group (Table 2).
Effects of drug treatments on UVR-induced skin changes. A Accumulated erythema in response to 6 weeks of UVR, evaluated 30 min after UVR on a scale from 0 (no erythema) to 4 (very severe erythema), and B pigmentation scores at week 30. *, **, and ***p-values < 0.05, 0.01, and 0.001 when compared to the UV control group
3.3 Effects of drug treatment on UVR-induced carcinogenesis
To evaluate the effect of drug treatment on photoprotection, the mice were checked weekly for the development of tumours with diameters of 1 mm or above. The first tumour became visible after 86 days (UV control group) and after 149 days, one mouse from each group had developed at least one tumour (Fig. 5). The median tumour onset was 164 days for the UV control group (Fig. 5B). This was unchanged by all treatment groups except nicotinamide, which delayed tumour onset till 206 days (Table 3). Moreover, the protection provided by nicotinamide resulted in only 76.2% of the mice developing a tumour (Table 3). When no further change in tumour development was observed 1 week after the completion of the second to last group (Metformin), the five remaining nicotinamide-treated mice were euthanised after 262 days in the experiment. The number and sizes of tumours with a diameter of 4 mm or above were similar in all drug-treated groups compared to the UV control (Fig. 5A and Table 3), whereas nicotinamide significantly reduced the median number of tumours from 3 to 1.
4 Discussion
Drug repurposing has become an interesting source of chemoprevention [21]. With the rise in squamous cell carcinoma incidence rates [5,6,7], indicating an increasing need for alternative methods of photoprotection, we wanted to explore the potential of drug repurposing as an avenue for oral photoprotection. Therefore, in this study, we investigated whether four different drugs could reduce UVR-induced carcinogenesis in hairless mice.
Oral supplementation with either bucillamine, carvedilol, metformin, or phenformin did not affect tumour onset or development compared to control treated UVR-exposed hairless mice (Fig. 5 and Table 3), whereas treatment with the positive control, nicotinamide, delayed tumour onset and reduced the number of tumours induced by UVR treatment.
One study has previously reported on the effects of oral metformin on photocarcinogenesis. The authors demonstrated that gavage-delivered metformin resulted in a significant reduction in UVR-induced tumour development [10]. While the same dose was used in both studies (300 mg/kg), there was no change to tumour development in the current study, albeit a significant reduction in erythema (Table 2). The difference in effect may be due to the route of oral delivery. In the present study, mice had ad libitum access to metformin-supplemented drinking water at a concentration that would ensure a dose of 300 mg/kg through their daily water intake. However, in the other study, the entire dose of metformin was delivered through gavage one hour prior to UV radiation. As gavage-delivered compounds reach a higher plasma and tissue concentration than feed supplementation [22], it is possible that metformin did not reach a sufficient level to counteract the damaging effects of UVR in the skin. It may, therefore, be necessary to increase the daily feed dose of metformin to reach a level of photoprotection comparable to what is achieved through gavage delivery.
It is important to note that a cohort study from 2019 reported no reduction in cancer risk in type 2 diabetes patients treated with metformin [23]. This was further supported by the results of a recent retrospective cohort study, which showed that metformin treatment had no effect on the development of new keratinocyte carcinoma lesions [24]. Taken together, these results may suggest that while metformin at a higher dose may prevent UVR-induced skin cancer in mice, it will not be effective as keratinocyte carcinoma prevention in humans.
Topical application of carvedilol has been shown to act photoprotective in two separate studies [12, 13]. To circumvent the need to apply photoprotection, we explored the oral potential of carvedilol but did not observe any protective effect. In humans, oral intake of a 50 mg capsule has a bioavailability of only 24% [25]. The present dose is based on the same human dose, suggesting a similar low level of bioavailability. In a recent study, Shamim et al. reported that topically applied carvedilol had an improved skin-to-plasma ratio compared to oral delivery [13]. Furthermore, the tested dose was more than twice of what is given in the present study (20 mg/kg vs. 7.25 mg/kg), indicating that the mice would have even less carvedilol available in the skin. As higher therapeutic doses would affect the cardiovascular system as reported for mice treated with 20 mg/kg [13], we do not believe carvedilol to be an appropriate candidate for oral photoprotection.
While phenformin did increase dorsal pigmentation (Fig. 3 and Table 2), it had no effect on tumour development (Figs. 5 and 6, and Table 3). Prior to UVR initiation, three mice treated with phenformin were found dead. No change in weight or dietary habits was observed, and following a dose change from 100 to 75 mg/kg, no further toxicity was reported. While phenformin was removed from the market at the end of the 1970s because of lactic acidosis toxicity [26], previous mouse studies have used doses up to 300 mg/kg with no reported toxicity [27, 28]. However, it is possible that the present mouse model, C3.Cg-Hrhr/TifBomTac, is particularly susceptible to lactic acidosis.
Bucillamine was chosen as a drug candidate because of its structural similarity to N-acetylcysteine, which is reported to be photoprotective in both in vitro and mouse models [29,30,31]. There are currently only two other studies reporting on the photoprotective effects of bucillamine [15, 16]. In the current study, we show for the first time that bucillamine treatment does not affect tumour development (Fig. 5 and Table 3), indicating that bucillamine is not an appropriate candidate for oral photoprotection. Although bucillamine did not affect tumour development, bucillamine and phenformin treatment did induce significant increases in weight gain (Fig. 1). While the weight increase in phenformin-treated mice may be explained by a lower starting weight (data not shown), we currently do not know why bucillamine treatment causes weight gain.
There are some technical limitations of the study. Only female mice were used. This was done to optimise housing of the animals as male mice do not allow other males to occupy the same space, creating a need for individual housing. As a result, potential sex-dependent differences were not in the scope of this work and should be explored in a follow-up study. The study included only one concentration of each drug, which may have limited possible findings at higher concentrations. While the applied concentrations were based on observations from other studies [10, 11, 15, 16] and human doses (see Footnote 1), it is possible that gavage delivery is required to reach a higher peak concentration to achieve photoprotection. However, to minimise harm experienced by the mice, this was not done in the current explorative study. Finally, while the drugs according to their data sheets should be stable in their applied solutions, we did not test whether drug activity remained over the 24 h of administration.
In conclusion, oral supplementation with bucillamine, carvedilol, metformin, or phenformin did not affect UVR-induced carcinogenesis in hairless mice. More research is needed to identify relevant candidates for oral photoprotection, and perhaps focus should be put on combining already established compounds in order to increase their photoprotective potential.
Data availability
The datasets generated and analysed during the current study are available from the corresponding author on reasonable request.
Notes
Based on the human therapeutic dose of 50 mg/day [18].
Abbreviations
- SCC:
-
Squamous cell carcinoma
- UVR:
-
Ultraviolet radiation
- HE:
-
Haematoxylin and eosin
References
Ashburn, T. T., & Thor, K. B. (2004). Drug repositioning: Identifying and developing new uses for existing drugs. Nature Reviews Drug Discovery, 3(8), 673–683. https://doi.org/10.1038/nrd1468
Nosengo, N. (2016). Can you teach old drugs new tricks? Nature, 534(7607), 7607. https://doi.org/10.1038/534314a
Smith, S. B., Dampier, W., Tozeren, A., Brown, J. R., & Magid-Slav, M. (2012). Identification of common biological pathways and drug targets across multiple respiratory viruses based on human host gene expression analysis. PLoS ONE, 7(3), e33174. https://doi.org/10.1371/journal.pone.0033174
Kim, Y., & He, Y.-Y. (2014). Ultraviolet radiation-induced non-melanoma skin cancer: Regulation of DNA damage repair and inflammation. Genes & Diseases, 1(2), 188–198. https://doi.org/10.1016/j.gendis.2014.08.005
Birch-Johansen, F., Jensen, A., Mortensen, L., Olesen, A. B., & Kjær, S. K. (2010). Trends in the incidence of nonmelanoma skin cancer in Denmark 1978–2007: Rapid incidence increase among young Danish women. International Journal of Cancer, 127(9), 2190–2198. https://doi.org/10.1002/ijc.25411
Tokez, S., Hollestein, L., Louwman, M., Nijsten, T., & Wakkee, M. (2020). Incidence of multiple vs first cutaneous squamous cell carcinoma on a nationwide scale and estimation of future incidences of cutaneous squamous cell carcinoma. JAMA Dermatology, 156(12), 1–7. https://doi.org/10.1001/jamadermatol.2020.3677
Guo, A., Liu, X., Li, H., Cheng, W., & Song, Y. (2023). The global, regional, national burden of cutaneous squamous cell carcinoma (1990–2019) and predictions to 2035. European Journal of Cancer Care, 2023, e5484597. https://doi.org/10.1155/2023/5484597
Holman, D. M., Berkowitz, Z., Guy, G. P. J., Hawkins, N. A., Saraiya, M., & Watson, M. (2015). Patterns of sunscreen use on the face and other exposed skin among US adults. Journal of the American Academy of Dermatology, 73(1), 83-92.e1. https://doi.org/10.1016/j.jaad.2015.02.1112
Pihl, C., Togsverd-Bo, K., Andersen, F., Haedersdal, M., Bjerring, P., & Lerche, C. M. (2021). Keratinocyte carcinoma and photoprevention: The protective actions of repurposed pharmaceuticals, phytochemicals and vitamins. Cancers, 13(15), 3684. https://doi.org/10.3390/cancers13153684
Wu, C., Qiang, L., Han, W., Ming, M., Viollet, B., & He, Y.-Y. (2013). Role of AMPK in UVB-induced DNA damage repair and growth control. Oncogene, 32(21), 2682–2689. https://doi.org/10.1038/onc.2012.279
Zhou, Q., Kim, S. H., Pérez-Lorenzo, R., Liu, C., Huang, M., Dotto, G. P., Zheng, B., & Wu, X. (2021). Phenformin promotes keratinocyte differentiation via the calcineurin/NFAT pathway. The Journal of Investigative Dermatology, 141(1), 152–163. https://doi.org/10.1016/j.jid.2020.05.114
Huang, K. M., Liang, S., Yeung, S., Oiyemhonlan, E., Cleveland, K. H., Parsa, C., Orlando, R., Meyskens, F. L., Jr., Andresen, B. T., & Huang, Y. (2017). Topically applied carvedilol attenuates solar ultraviolet radiation induced skin carcinogenesis. Cancer Prevention Research, 10(10), 598–606. https://doi.org/10.1158/1940-6207.CAPR-17-0132
Abdullah Shamim, M., Yeung, S., Shahid, A., Chen, M., Wang, J., Desai, P., Parsa, C., Orlando, R., Meyskens, F. L., Jr., Kelly, K. M., Andresen, B. T., & Huang, Y. (2022). Topical carvedilol delivery prevents UV-induced skin cancer with negligible systemic absorption. International Journal of Pharmaceutics, 611, 121302. https://doi.org/10.1016/j.ijpharm.2021.121302
Revive Therapeutics, Ltd. (2023). Multi-center, randomized, double-blind, placebo-controlled study of bucillamine in patients with mild-moderate COVID-19 (clinical trial registration NCT04504734). clinicaltrials.gov. https://clinicaltrials.gov/study/NCT04504734
Anwar, A., Gu, M., Brady, S., Qamar, L., Behbakht, K., Shellman, Y. G., Agarwal, R., Norris, D. A., Horwitz, L. D., & Fujita, M. (2008). Photoprotective effects of bucillamine against UV-induced damage in an SKH-1 hairless mouse model†. Photochemistry and Photobiology, 84(2), 477–483. https://doi.org/10.1111/j.1751-1097.2007.00288.x
Anwar, A., Anwar, H., Yamauchi, T., Tseng, R., Agarwal, R., Horwitz, L. D., Zhai, Z., & Fujita, M. (2020). Bucillamine inhibits UVB-induced MAPK activation and apoptosis in human HaCaT keratinocytes and SKH-1 hairless mouse skin. Photochemistry and Photobiology, 96(4), 870–876. https://doi.org/10.1111/php.13228
Pihl, C., Bendtsen, K. M. S., Jensen, H. E., Andersen, F., Bjerring, P., Haedersdal, M., & Lerche, C. M. (2023). Oral phytochemicals as photoprotectants in UVR exposed hairless mice: A study of hesperidin methyl chalcone, phloroglucinol, and syringic acid. Journal of Photochemistry and Photobiology B: Biology, 246, 112760. https://doi.org/10.1016/j.jphotobiol.2023.112760
Nair, A. B., & Jacob, S. (2016). A simple practice guide for dose conversion between animals and human. Journal of Basic and Clinical Pharmacy, 7(2), 27–31. https://doi.org/10.4103/0976-0105.177703
R Core Team. (2021). R: A language and environment for statistical computing. (3.6.0) [Software]. https://www.R-project.org/
Kassambara, A., Kosinski, M., Biecek, P., Marcin, K., & Przemyslaw, B. (2021). survminer: Drawing survival curves using “ggplot2”. (0.4.9) [Software]. https://CRAN.R-project.org/package=survminer
Siddiqui, S., Deshmukh, A. J., Mudaliar, P., Nalawade, A. J., Iyer, D., & Aich, J. (2022). Drug repurposing: Re-inventing therapies for cancer without re-entering the development pipeline—A review. Journal of the Egyptian National Cancer Institute, 34(1), 33. https://doi.org/10.1186/s43046-022-00137-0
Kapetanovic, I. M., Krishnaraj, R., Martin-Jimenez, T., Yuan, L., van Breemen, R. B., & Lyubimov, A. (2006). Effects of oral dosing paradigms (gavage versus diet) on pharmacokinetics and pharmacodynamics. Chemico-Biological Interactions, 164(1), 68–75. https://doi.org/10.1016/j.cbi.2006.08.019
Farmer, R. E., Ford, D., Mathur, R., Chaturvedi, N., Kaplan, R., Smeeth, L., & Bhaskaran, K. (2019). Metformin use and risk of cancer in patients with type 2 diabetes: A cohort study of primary care records using inverse probability weighting of marginal structural models. International Journal of Epidemiology, 48(2), 527–537. https://doi.org/10.1093/ije/dyz005
Ravishankar, A., Zhang, T., Lindgren, B. R., Farah, R. S., Dong, Z., & Goldfarb, N. I. (2020). The effect of metformin on the risk of recurrent nonmelanoma skin cancers. International Journal of Dermatology, 59(8), e303–e305. https://doi.org/10.1111/ijd.14829
von Möllendorff, E., Reiff, K., & Neugebauer, G. (1987). Pharmacokinetics and bioavailability of carvedilol, a vasodilating beta-blocker. European Journal of Clinical Pharmacology, 33(5), 511–513. https://doi.org/10.1007/BF00544245
Bailey, C. J. (2017). Metformin: Historical overview. Diabetologia, 60(9), 1566–1576. https://doi.org/10.1007/s00125-017-4318-z
Appleyard, M. V. C. L., Murray, K. E., Coates, P. J., Wullschleger, S., Bray, S. E., Kernohan, N. M., Fleming, S., Alessi, D. R., & Thompson, A. M. (2012). Phenformin as prophylaxis and therapy in breast cancer xenografts. British Journal of Cancer, 106(6), 1117–1122. https://doi.org/10.1038/bjc.2012.56
Di Magno, L., Manni, S., Di Pastena, F., Coni, S., Macone, A., Cairoli, S., Sambucci, M., Infante, P., Moretti, M., Petroni, M., Nicoletti, C., Capalbo, C., De Smaele, E., Di Marcotullio, L., Giannini, G., Battistini, L., Goffredo, B. M., Iorio, E., Agostinelli, E., … Canettieri, G. (2020). Phenformin inhibits Hedgehog-dependent tumor growth through a complex I—Independent redox/corepressor module. Cell Reports, 30(6), 1735-1752.e7. https://doi.org/10.1016/j.celrep.2020.01.024
D’Agostini, F., Balansky, R. M., Camoirano, A., & De Flora, S. (2005). Modulation of light-induced skin tumors by N-acetylcysteine and/or ascorbic acid in hairless mice. Carcinogenesis, 26(3), 657–664. https://doi.org/10.1093/carcin/bgi008
Yan, M., Liu, Z., Yang, H., Li, C., Chen, H., Liu, Y., Zhao, M., & Zhu, Y. (2016). Luteolin decreases the UVA-induced autophagy of human skin fibroblasts by scavenging ROS. Molecular Medicine Reports, 14(3), 1986–1992. https://doi.org/10.3892/mmr.2016.5517
Oh, M. C., Piao, M. J., Fernando, P. M. D. J., Han, X., Hewage, S. R. K. M., Park, J. E., Ko, M. S., Jung, U., Kim, I. G., & Hyun, J. W. (2016). Baicalein protects human skin cells against ultraviolet B-induced oxidative stress. Biomolecules & Therapeutics, 24(6), 616. https://doi.org/10.4062/biomolther.2016.022
Acknowledgements
The authors would like to extend their gratitude to Catrine Fischer Goldschmidt and Diana Høeg (Department of Dermatology, Copenhagen University Hospital) for their assistance in animal handling and laboratory support. The study was performed and funded as a part of the Danish Research Center for Skin Cancer (www.researchcenterforskincancer.org), a public-private research partnership between the Private Hospital Molholm, Aalborg University Hospital and Copenhagen University Hospital, Bispebjerg and Frederiksberg, as well as the Skin Cancer INnovation Clinical Academic Group (SCIN CAG), Greater Copenhagen Health Science Partners (GCHSP).
Funding
Open access funding provided by Copenhagen University. Open access funding provided by Copenhagen University.
Author information
Authors and Affiliations
Contributions
Conceptualisation, writing—review and editing: CML, CP, FA, PB, MH; investigation, formal analysis, writing—original draft, visualisation: CP; funding acquisition: FA, PB, MH; resources: CML, MH; supervision: CML.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pihl, C., Bjerring, P., Andersen, F. et al. Oral intake of bucillamine, carvedilol, metformin, or phenformin does not protect against UVR-induced squamous cell carcinomas in hairless mice. Photochem Photobiol Sci 23, 517–526 (2024). https://doi.org/10.1007/s43630-024-00535-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43630-024-00535-4