Abstract
The Sustainable Development Goals (SDGs) represent global action to address the challenges that impact society and nations, are inclusive, equitable, integrated, interdependent and people-centric. Some of the key SDG targets address societal issues, that include education, economic and health lags, particularly in low- and middle-income and African countries. The nexus of society, education, the economy and health, is therefore discussed and interrelated to provide perspectives on advancing development and sustainability. Being socioeconomically disadvantaged impacts access to quality education and health, limits economic activity and diminishes sustainability. Many people live in impoverished countries due to ailing economies with high unemployment. These global and pervasive challenges persist and limit the potential of people and nations. Sustainable advancement requires empowered well-educated people who contribute to economic growth and have access to quality healthcare who can contribute to greater development and sustainability. Therefore a social-education-economy-health nexus is contextualized that aligns with the SDGs and converges to support growth and sustainability, and realize social, education, economic and health value. Education, training and skilling that are relevant to address socioeconomic and health challenges are critical for development and sustainability. Strengthening the social-education-economy-health nexus will advance development and sustainability. Investment in low- and middle-income and African countries, through public–private-philanthropy partnerships to fund social, economic, education and health initiatives, will foster development and sustainability.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
1 Introduction
Advanced societies, quality education, robust economies and good health (physical, mental and well-being) are integral for development and sustainability at individual and national levels. The social determinants of health straddles society (people and community), education (access, quality and attainment), the economy (growth and stability, closely linked to employment), healthcare (access and quality), and living conditions (neighborhoods and infrastructure including access to basic services), which impact people’s health, well-being and quality of life. Insufficient water supplies, poor sanitation and poor hygiene, contribute to morbidity and mortality, particularly in low- and middle-income countries (LMICs) and young children [1, 2]. Food insecurity is associated with psychosocial dysfunction in children, socio-familial problems and poor health and well-being [3], and household income, which relies on employment, is a determinant for accessing food [4]. Society, education, the economy and health are interlinked and progress across these and related dimensions drive development and sustainability (Fig. 1). Quality education, economic growth and accessible quality healthcare empowers society to foster and advance development and sustainability. These inter-related elements reinforce each other to enable and enhance advancement.
At an individual level, society, education, the economy and health are shaped by income, education attainment, employment rates, and community safety and support, to enable and expand choices such as purchasing healthy food, determining type of housing, transport modes and access to healthcare. Empowered communities can contribute to better health access and services [5]. At a national level, healthy and well-educated citizens, who are suitably employed (relevantly skilled in alignment with their country’s development needs) advance their country’s economy and development. This reflects the social-education-economy-health nexus that is foundational to enable development and drive sustainability.
In LMICs and in Africa, particularly sub-Saharan Africa (SSA), the social-education-economy-health nexus requires strengthening to build resilience towards greater sustainability. Socially, people need access and opportunity to safe housing and communities; adequate infrastructure; education, training and skilling; quality preventative and treatment services; and employment that is aligned to personal and community economic growth. Educationally, suitable and higher levels of education and skills should be attained and align with economic growth. Economically, people need to be suitably employed for sector growth and to support the economy. For health and well-being, people who are more educated often secure better employment, are more health aware and may adopt healthier lifestyles. Healthier educated people can make more informed decisions, although this is dependent on lifestyle choices and personal will, and with less morbidity and mortality, economies grow and develop. An empowered society, with decent education levels who are employed in a growing economy, and have access to quality health benefit, and confer benefits, for development and sustainability. The social-education-economy-health nexus will be discussed in the context of LMICs and African (SSA) countries.
The global Sustainable Development Goals (SDGs) focus on advancing development and are particularly relevant for LMIC and African countries. The 17 SDGs are a shared agenda for peace and prosperity for people and the planet, with a call for global partnerships to advance society [6]. The goals focus on eradicating poverty (SDG 1) and hunger (SDG 2), promoting good health and well-being (SDG 3), providing quality education (SDG 4), addressing gender equality (SDG 5), providing clean water and sanitation (SDG 6), affordable and clean energy (SDG 7), and decent work and economic growth (SDG 8), building industry, innovation and infrastructure (SDG 9), reducing inequality (SDG 10), creating sustainable cities and communities (SDG 11), promoting responsible consumption and production (SDG 12), taking action against climate change (SDG 13), conserving life below water (SDG 14), and on land (SDG 15), promoting peace, justice and strong institutions (SDG 16), and strengthening partnerships for development and sustainability (SDG 17) [6]. Eradicating poverty and reducing inequality are aligned with improving education, enhancing economic growth and better health and well-being [6]. Some of these SDGs address societal issues, that encompasses education, economic and health lags, particularly in low and middle-income and African countries. These global and pervasive challenges persist and limit the potential of people and nations. Advancing society, education, the economy and health also requires collaborative partnerships. Low- and middle-income and African countries should support domestic implementation of all the SDGs, through North–South, South-South and triangular cooperation (North–South-South or North–North-South) to promote equitable partnerships (SDG 17). The social-education-economy-health nexus and sustainability will also be discussed in the context of the relevant SDGs. First a snapshot of challenges in LMICs and Africa will be presented; perspectives on society, education, the economy and health will be discused; followed by unpacking the social-education-economic-health nexus and the transitions towards development and sustainability.
2 Snapshot of the developmental challenges in low- and middle-income and African countries
Apart from war, that displaces people and uproots communities, and health outbreaks, such as Ebola and cholera that collapse health systems and diminish health outcomes, several African countries are affected by worsening climate change. More recently, the Covid-19 pandemic has wreaked havoc on global health, economies and education, which was particularly devastating in low- and middle-income and African countries. Health services were disrupted with Covid-19 cases triaged, somewhat limiting access for other patients [7,8,9]. Governments and people experienced a loss of income by lockdowns, trade restrictions and loss of livelihoods. Schools and universities were temporarily closed due to several waves of the Covid-19 pandemic. In some SSA and low- and middle-income countries, the disruptions in education, economies and health services were exacerbated by the inability to absorb these shocks due to the fragility in systems that were already under strain. Worsening and more intense storms, flooding, heat waves and droughts affect food security leading to famine and water scarcity. There was a recent locust plague, the worst in decades, that spread throughout Eastern Africa. These adverse socio-economic and environmental factors strain individuals, and this hardship does not bode well for their health and well-being, particularly those with pre-existing diseases and who are vulnerable such as the poor, disabled, children, mothers and the elderly. Disasters also constrain access to health services and education that disrupts society and the economy. The mental and emotional burden of war, food and water insecurity and limited access to health, education and social services is distressing. These are some of the experiences that people encounter. Empowering people to handle stresses and disruptions will equip them to make informed health decisions and cope better during adversity.
3 Societal, education, economic and health drivers of development and sustainability
One way to link society, education, the economy and health is through poverty. In low- and middle-income and African countries, there is a high prevalence of stunting, which is associated with poor health outcomes and reflects inequality [10]. There is extreme poverty in ~ 250 million children who are at risk for not reaching their developmental potential as a ~ third of preschool children do not meet basic cognitive or socioemotional development milestones, with stunting in ~ 17% [11]. These developmental deficits constrain education and economic opportunities in adulthood, which perpetuates an intergenerational cycle of poverty [11] and may result in ~ 25% less in potential annual income earned [12]. The Socio-demographic Index (SDI) measures development status and is calculated with indicators on fertility, income and education in people ≥ 15 years [13]. Using the SDI, in 2015, there were high deaths in children and adolescents in South Asia, Western SSA, Eastern SSA, North Africa, the Middle East and central SSA, and although children and adolescent mortality decreased in all SDI quintiles, there was an increase in inequality [13]. Thus despite better health outcomes, inequality exacerbated which may contribute to poverty and diminish education and economic potential. Social enterprises, i.e. sustainable ventures that apply business principles for positive impact, can help to alleviate poverty and provide care to the most vulnerable people, which in turn improves health, well-being and quality of life [14, 15].
Health enables and is an outcome of development and sustainability [16] and is integrated and interdependent on the other SDGs [16,17,18] that operate in an ecosystem [18], which links health to society, education, the economy and other related SDGs to drive development and sustainability. Empowered societies, quality education, growing economies and quality and accessible healthcare are the foundational elements for advancing development and sustainability. Each driver of development and sustainability is contextualized to the relevant SDGs, then related to the other drivers (i.e. in the social-education-economy-health nexus).
3.1 Empowered society
Countries need to focus on social vulnerabilities such as school life expectancy, unemployment and labor market discouragement [19] to empower society (people and communities). Variations in risk factors, morbidity and mortality, inter- and intra-country, are influenced by the social and physical milieus, and the associated structural policies [20]. Poverty disempowers people, stagnates nations, and amplifies inequality [21]. In relation to the SDGs, to empower society, eradicating poverty (SDG 1) and hunger (SDG 2), promoting gender equality (SDG 5) and reducing inequalities (SDG 10) are some of the key determinants. Providing clean water and sanitation (SDG 6) and improving access to clean energy (SDG 7), taking climate action (SDG 13) and enhancing peace and justice (SDG 16), through continental and global partnerships (SDG 17), are also necessary to empower society. In relation to the nexus, societal empowerment is also realized by quality lifelong education (SDG 4), decent jobs provision and economic growth (SDG 8), and access to good health services (SDG 3). Further, reducing inequality by non-discriminatory empowerment and promoting social, economic and political inclusion to ensure equal opportunities (SDG 10) will drive societal empowerment, and is supported by access to affordable housing and transport and safe public spaces (SDG 11). In addition, mitigating the morbidity, mortality and economic losses due to disasters will help protect poor and vulnerable people (SDG 11). LMIC and African citizens can be further empowered by responsible and efficient use of natural resources (SDG 12), reducing food waste and loss during production (SDG 12), and strengthening resilience and capacity to climate-related hazards and natural disasters, supported by increasing awareness on climate change (SDG 13). Regulating the harvesting of fish, and ending overfishing and destructive fishing practices to restore fish stocks will help to improve food security (SDG 14), whereas improving access to marine resources and markets (SDG 14) will contribute to greater economic activity. Conserving, restoring and the sustainable utilization of water ecosystems concomitant with combatting deforestation (SDG 15) to restore degraded land, can preserve biodiversity and limit the destructive impact of invasive species on water and land ecosystems (SDG 15). This is linked to sustainable agricultural practices for food security and access to clean water. Eradicating violence and related mortalities, eliminating corruption and implementing effective, accountable and transparent governance with non-discriminatory policies and legislation will enhance development and sustainability (SDG 16). An empowered society therefore contributes to achieving positive education, economic and health outcomes, and other dimensions to enable development and sustainability.
3.2 Quality education
Inequalities in education, which is pervasive in low- and middle-income and African countries, need to be addressed for societies to realize better health and well-being and to foster greater economic activity and development; thus education equality (i.e. improving education quality) translates into greater equality in health and well-being, and economic activity (productivity) [22]. There were vast improvements in education from 1970 to 2018 in SSA and South Asia, but also greater increases in education inequality (Western SSA countries had the most inequality in 2018) [22]. However, in these regions, access to and quality of education still lags relative to high income countries (HICs). Poor education can perpetuate inequality across generations [23]. Intergenerational and individual sociodemographic factors shape educational opportunities and trajectories that contribute to educational attainment [23]. Thus quality, relevant education is important to sustain the health and related sectors and for development and sustainability. Quality education and health are integral to individual and population well-being and contribute to better societies [23] to sustain economic growth [18]. Citizens should have access and opportunities for relevant, frequent and structured education, thereby applying their knowledge for the development and sustainability of their neighborhoods, communities (districts or municipalities), provinces (states), countries, regions and continents. This feeds into greater economic empowerment and activity to benefit countries, and ultimately, continents prosper. Health service delivery is dependent on a skilled workforce employed by the health sector and supporting sectors and factors that directly and indirectly contribute to development and sustainability such as open trade, supporting and enabling infrastructure, good governance and quality education.
Education can create better health awareness to make healthcare more accessible [19], and to augment health promotion to help prevent or delay the onset of diseases, that relieves health systems and reduces the costs of health service delivery. People with tertiary education tend to be healthier, have higher states of well-being and longer lifespans relative to less educated peers, that influences their perspectives on child vaccination and mortality, vaccine enrollment and life expectancy [19]. This may be attributed to greater health awareness and access to healthcare. Investing in education yields increased productivity [24], improves individuals’ reasoning, effectiveness, skills and knowledge and an array of abilities to benefit health [25] and grow economies.
Quality and relevant education is a lever for breaking the poverty cycle [26, 27] and can be achieved through empowered, well-trained and supported teachers to drive universal primary and secondary education [28], and through the fair provision of quality education in rural and urban areas, across regions and districts, and between and within schools. Quality education equips people with skills and knowledge (such as self-control, learned effectiveness and problem solving) to improve their health [29] and enhances human capital [19] that charts a path for countries’ towards financial security, stable employment and an empowered society [30]. Countries that implement policies to improve education also benefit from healthy behavior [19] e.g. reduced smoking, drinking, and unhealthy food intake that improves health outcomes e.g. reduced prevalence of non-communicable diseases. Further, education influences the potential years of life lost i.e. the years lost due to premature deaths [19] as greater health awareness helps to lessen the burden of disease. Education equips people with general health skills and knowledge for greater awareness of healthy behaviors and preventive care [19]. This contributes to greater individual ownership of health and healthier people, that adopt health promotion and disease prevention strategies, and thus require less health services thereby relieving health systems and saving countries money.
3.3 Growing economy
To understand the disparities in health resourcing, some socioeconomic perpectives should be considered. Globally, countries’ economies are classified into four income groups viz. high, upper-middle, lower-middle, and low [31] income countries. According to income, 31 (14.3%) countries are low income, 107 (49.3%) are middle income, and 79 (36.4%) are high income countries. There are 217 countries, of which 138 (63.6%) are classified as LMICs, 55 (25.3%) are in Africa and 48 are in SSA (22.1%). Within LMICs, African countries constitute 40% (SSA countries constitute 35%) and other LMICs (non-African countries) account for 60% of the countries.
SSA has a population of 1.079 billion [32]. In 2018, the gross domestic product (GDP) in SSA was $1.699 trillion whereas in the Middle East and North Africa (MENA) the GDP was ~ $3.3 trillion; (the global GDP was $85 trillion, and $31 trillion in LMICs) [32]. Further, in SSA, gross national income (GNI) per capita was $1 506 in 2018 (compared to global GNI of $11 097; $3 968 in MENA; and $4 837 in LMICs) [32]. This reflects the economic lag in SSA that constrains development and sustainability. Further, Northern Africa (as part of MENA excluding HICs), is a more advanced regional ecomony than SSA that translates into better health resourcing [5]. This also translates into better health outcomes evident as life expectancy was 73 years in Northern Africa compared to 60 years in SSA (in 2017, with global life expectancy of 72 years and LMIC life expectancy of 70 years) [32]. Health resourcing in SSA should therefore be contextualized against lagging economic and development constraints relative to Northern Africa, LMICs and globally.
Economic growth and development are achieved through infrastructural investments, providing employment, delivering quality education and skills, to build human capital, enhance productivity, and foster innovation [33]. Robust economies that can absorb shocks and grow steadily are critical for enabling quality health delivery and sustainability. Vulnerable countries, with excessive morbidities and early and excessive mortalities, experience devasting consequences on economies, which is exacerbated in poverty stricken African countries. Pervasive income inequality, inter- and intra-country, and great disparities in access to resources were evident during the Covid-19 pandemic [9]. Achieving the SDGs are somewhat constrained by economic policies that perpetuate the challenges that adversely impact societies’ health and well-being [9]. Economic evidence should focus on interventions where policy makers, supporting stakeholders and the health sector collaborate [34] to reduce disease burdens to improve health systems and services. Some emerging economies have reformed their health systems for more equitable access and better quality of healthcare [35] to advance their development and sustainability.
In low- and middle-income and African countries, providing infrastructure to enable economic growth, health and well-being through affordable and equitable access (SDG 9), and by promoting small, medium and micro enterprises (SMMEs) by increasing their access to financial services and integrating them into supply chains for access to markets (SDG 9) links industry, innovation and infrastructure to the society-education-economic-health nexus. Enhancing global macroeconomic stability, policy coordination and coherence, through continental and global partnerships, will advance sustainable development (SDG 17). This can be supported by encouraging and promoting robust public–private-philanthropy partnerships, building capacity and scaling up effective initiatives to advance development and sustainability. Strengthening domestic resource mobilization and revenue (SDG 17) can help low- and middle-income and African countries to realize process and cost efficiencies.
Low- and middle-income and African countries should regulate the number of youths becoming unemployed, not attending schools and not being skilled or trained to enhance school life expectancy [19] as these factors contribute to lost economic activity that exacerbate poverty and inequality. By targeted promotions that convey the value of developing skills and becoming employed, countries can lower the rate of people not in employment or education and training [19], and thereby combat school dropouts, youth unemployment and labor market discouragement [19]. Growing economies are therefore dependent on relevant and high rates of employment that is enabled by access and opportunity to quality education.
3.4 Quality and accessible healthcare
Primary healthcare can serve to refer people for access to other services such as social and judicial protection services for vulnerable people [36, 37] and adult education [38], which contributes to poverty alleviation, access to education, gender equality, and addresses inequalities to promote justice [39]. Health and poverty are strongly linked; nutrition and hunger relate to poverty and are key determinants of primary healthcare [39]. Quality education and adequate and productive employment (provision for jobs) are key for enabling good health and well-being [40] and for greater economic activity and to sustain economic growth [18]. Reducing morbidity and mortality improves the economic outlook (i.e. absenteeism and lost productivity decreases, thereby freeing up health services as citizens are healthier); therefore countries should prioritize health promotion and disease prevention [21, 41]. The health sector creates and supports jobs, offers job security and provides decent jobs [42]. Further, the health sector is essential for stable and functional economies by determining the economic performance and stability of a country; enhancing economic performance in other sectors, by generating employment from purchasing goods and services; by reducing social exclusion (aligned to universal health coverage and limiting out-of-pocket payments for access to healthcare) [42], and providing employment for women.
The Covid-19 pandemic linked health and the economy, and their convergence for influencing development and sustainability [35]. Establishing and developing resilient health systems in countries is critical for global health security [35] and is dependent on adequate health resourcing (personnel and infrastructure) and agile, resilient health systems that can respond to fluctuating and intense health services demands. Health workers include professional, skilled and non-skilled people who make health systems functional [43] and deliver healthcare to serve population health needs and support economic growth [44,45,46]. In 2006, SSA had ~ 11% of the global population, ~ 24% of the disease burden with ~ 67% of the HIV/AIDS burden, and only ~ 3% of the global health workforce [47]. In 2016, SSA had ~ 20.9% of the global disease burden with only ~ 4.5% of the global health workforce [48, 49]. This demonstrates the inadequate health worker resourcing and distribution, in the poorest region in the world (46 of the 55 African countries are in SSA), to tackle a persistently high burden of disease.
In Africa, the countries that were best resourced for doctors and nurses barely met the global threshold (4.45 doctors and nurses per 1 000); further, variable healthcare quality would constrain service delivery [5]. Having sufficient health workers is necessary to align with the disease burden, and knowledge, skills and training are levers for delivering quality care [5]. Sufficient and regular training that is relevant, supported by knowledge generation and the transferring of skills and mentoring, are necessary to enhance and equip the health workforce to be responsive to population health needs [18].
Another key consideration for health worker resourcing is the net migratory health worker outflow to HICs. With globalization, LMIC health workers are more mobile and connected to take up employment in HICs [50]. Health worker migration exacerbates the strain on the already overstretched health systems of the source countries, and erodes the source countries’ investments in health training [51] and skills development. In the globalized healthcare market, HICs recruit and import qualified health workers from LMICs [50]. Nine source countries in SSA (viz. Ethiopia, Kenya, Malawi, Nigeria, South Africa, Uganda, Tanzania, Zambia and Zimbabwe) lost ~ $2 billion due to educating doctors who then migrated to major destination countries viz. the USA, UK, Australia and Canada [52]. The health worker shortages are then further exacerbated in LMICs (for the benefit of HICs), therefore increasing global inequities [50] and severely constraining the ability and potential of LMICs to advance and even provide decent healthcare. In essence, the already impoverished LMICs, particularly SSA countries, are subsidizing health worker resourcing in HICs through training and skilling health workers in LMICs for later export, integration and benefication for HICs’ health systems. This is a hard dilemna that requires urgent redress. As African health worker migration erodes the diminishing African health workforce, the dedicated health workers who strive to make Africa better should be incentivized and motivated to continue to help improve continental health outcomes [53]. Aligned continental, regional and national initiatives should be implemented to retain, attract and skill African health workers and to provide improving and enabling working environments. Training African health workers for export erodes health service delivery, development and sustainability at a great loss for the continent and its citizens.
For investors in LMIC and African health, developing the health workforce is imperative during the course of their operations. Universities in HICs should consider opening satellite campuses to train doctors, nurses and allied health workers, in collaboration with resident universities and health and allied departments. This can also be supported by partnering with other HIC univerisities and attracting donor investment to train health workers thereby contributing to better health for LMIC and Africans citizens. This presents a humanitarian initiative, a business development opportunity and a contribution to positive social-education-economy-health impact. More nurses should be trained to replenish the health workforce, and in the interim, other health workers could be trained to deliver certain non-essential clinical services. Other initiatives are to improve health facility efficiencies such as improving partient record keeping, and reducing waiting times and stock-outs. This will require investment in lifelong (continous) learning and skilling, to increase enrolment and capacity at universities and colleges. Private education and healthcare (e.g. hospitals) providers could also help to deliver some of the training and skilling for nurses and allied health workers through public–private-philanthropy partnerships. This is an opportunity for globally recognized HIC universities to provide faculty and run accredited courses to help increase the nursing (and allied health worker) densities in and LMIC and African countries. More public–private-philanthropy partnerships should be established to drive LMIC and African development and sustainability. Smart health investments, such as investments in digital health, health security and artificial intelligence, that enable development and sustainability will enhance social stability while contributing to economic growth [35].
3.5 Value creation for development and sustainability
Where the society-education-economy-health nexus converges to support development and sustainability, social, education, economic and health value are realized. The social value is that diseases affecting those who are poorest, most vulnernable and living in highly unequal societies are prioritized with greater access to quality healthcare. The education value is that quality and relevant training and skilling are implemented, to address the disease burden, and enable greater economic activity. The economic value is that investments, public–private-philanthropy partnerships, shared knowledge, resources and processes, and cost efficiencies advance economic progress that enable and realize better basic and health services for the benefit of people. Further, infrastructure is established for the benefit of future generations. The health value is that high disease morbidities and mortalities are addressed, which concomitant with disease prevention and improved management (treatment), leads to better health outcomes, effectiveness and efficiencies that ultimately enhance economic activity. The collective value created contributes to poverty alleviation and greater equality.
Table 1 presents the social-education-economy-health nexus, the main objectives, the relevant SDGs and key initiatives for development and sustainability. Socioeconomic determinants of health are intertwined. Quality education enables societal, economic and health progress. Societal empowerment, by eliminating poverty and reducing inequality, requires the implementation of social protection initiatives to protect the poorest and most vulnerable by uplifting them from poverty (Table 1). This can be achieved by better access to basic services, through maintenance and investment in infrastructure to provide decent water and sanitation. People become more empowered through adopting sustainable agricultural practices and responsible consumption practices for better food security towards ending hunger. Countries should strive to provide nutritious food throughout seasons and to ensure that citizens, particularly the most vulnerable, are adequately nourished. Enhancing water use efficiency and protecting water ecosystems to avoid water scarcity for people, livestock and crops are critical. Other levers for social empowerment are enhancing awareness and resilience to climate change, empowering women to participate in the economy and improving their access to education. Improving access to clean energy and growing the renewable energy sector creates employment while reducing the carbon footprint.
To realize educational attainment, by providing quality primary and secondary education to support increased enrolment for tertiary education, and enhancing literacy and numeracy rates are critical, and should be supported by an enabling environment for learning, knowledge sharing and upskilling, that is reinforced by adequately trained teachers and lecturers to continuously improve teaching and learning (Table 1). Creating sustainable institutions, that are carbon neutral, and provide quality relevant education that encompasses knowledge, training and skills that are transferable to the employment sectors are important for development and sustainability. Linking education, skills and training to the employment demands will grow the economy. There should be targeted enrolment for science, technology, engineering, mathematics and medicine (STEMM), with support for entrepreneurship and innovation, and training and skilling of artisans, technicians and technologists related to sector specific needs to advance development and sustainability.
Economic growth, that provides decent jobs aligned to the local, provincial and national economies, requires greater economic productivity through increasing the employment rates, adopting and harnessing technology and diversifying the economy (Table 1). Increasing the number of youth in education, training, skilling or employment is necessary for economic growth. Further, the protection of workers’ rights is important, as workers are valued, as is enabling equitable access to employment by promoting diversity, equality and inclusion. Preserving and responsibly harnessing biodiversity will help to retain resource richness and can enhance economic growth by adding value to materials e.g. mineral beneficiation and growing the services sector. SMMEs and the informal sector help drive the economies in low- and middle-income and African countries and are largely unregulated. Creating enabling environments for SMME owners, that employ local people, uplifts that community. Better access to markets and support are key for enabling greater economic access and activity. Focusing on the informal sector by implementing practices to facilitate business is necessary as is including people to supply value chains. Further, upskilling the most vulnerable people enables better employment prospects and economic activity, and helps to address poverty and inequality.
Better health access and quality services, focused on reducing morbidity and mortality for the most prevalent diseases, can be achieved by training and upskilling health workers to better equip them to address the disease burden (Table 1). This requires improving access to quality care by providing a standard package of care customized to people’s health needs. Maintaining and investing in infrastructure and applying technology for greater efficiencies improves health services. Promoting health in communities increases health awareness and relieves health systems. Implementing task shifting and sharing contributes to process and cost efficiencies in the delivery of healthcare, and it is important to keep health workers motivated as they contribute to the betterment of society. Enhancing surveillance and implementing artificial intelligence to reveal health trends and patterns better prepares health workers to address the disease burden and supports pandemic preparedness. Also, enabling and supporting health innovation of products, i.e. getting products to market, for the prevention, diagnosis and treatment of diseases, helps to upskill people, creates employment and contributes to the economy while improving health. Further, streamlining process and cost efficiencies to optimize resource allocation enables better and more optimal delivery of health services.
Continental public–private-philanthropy investments and partnerships to empower people, grow the economy, enhance attainment and quality of education, and enhance access to quality health services will advance development and sustainability. For universal health coverage to be realized, all people are to have access to health, without financial hardship, through a motivated and qualified workforce who utilize sufficient infrastructure to deliver health services, to create a healthier society (less morbidity and mortality), who will contribute to greater economic growth. An empowered, relevantly educated society, that is suitably employed in alignment with economic development, further advances economic development and contributes to better health outcomes, towards greater national development and sustainability.
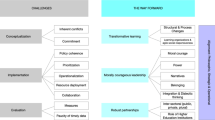
Figure 2 unpacks the transitions towards development and sustainability. Addressing poverty and inequality by improving access to education, jobs and health empowers and advances society. Enhancing pre-, primary, secondary, technical and tertiary education, that is aligned to the economic and health needs of a country, localized per province and city, drives development and sustainability. This will yield quality education outcomes and suitably qualified and skilled workers who can access decent employment thereby contributing to greater economic activity and growth. Better educated and suitably qualified or skilled people can make better health decisions and should enjoy better access to healthcare that translates into better health outcomes. Collectively, well educated, economically active, healthier people will elevate society, education, the economy and health, thereby preserving and advancing development and sustainability.
4 Conclusion
Despite socioeconomic challenges, LMIC and African citizens need to be further empowered through quality education to contribute to their countries’ economies and to support quality health access and delivery. Long-term training and investment are required to implement programs to develop and grow the LMIC and African health workforce. Investment in African countries and LMICs, through public–private-philanthropy partnerships to fund social, economic, education and health initiatives, is imperative to address existing and limit further socioeconomic, education and health lags, thereby advancing development and sustainability.
References
GBD Diarrhoeal Diseases Collaborators. Estimates of global, regional, and national morbidity, mortality, and aetiologies of diarrhoeal diseases: a systematic analysis for the global burden of disease study 2015. Lancet Infect Dis. 2017;17:909–48. https://doi.org/10.1016/S1473-3099(17)30276-1.
Wolf J, Hunter PR, Freeman MC, Cumming O, Clasen T, Bartram J, Higgins JPT, Johnston R, Medlicott K, Boisson S, et al. Impact of drinking water, sanitation and handwashing with soap on childhood diarrhoeal disease: updated meta-analysis and meta-regression. Trop Med Int Health. 2018;23:508–25. https://doi.org/10.1111/tmi.13051.
Chinnakali P, Upadhyay RP, Shokeen D, Singh K, Kaur M, Singh AK, Goswami A, Yadav K, Pandav CS. Prevalence of household-level food insecurity and its determinants in an urban resettlement colony in North India. J Health Popul Nutr. 2014;32:227–36.
Dharmaraju N, Mauleshbhai SS, Arulappan N, Thomas B, Marconi DS, Paul SS, Mohan VR. Household food security in an urban slum: determinants and trends. J Family Med Prim Care. 2018;7:819–22. https://doi.org/10.4103/jfmpc.jfmpc_185_17.
Cerf ME. Quintile distribution of health resourcing in Africa. Cogent Med. 2021;8:1. https://doi.org/10.1080/2331205x.2021.1997161.
United Nations. Sustainable development. 2022. https://sdgs.un.org/goals. Accessed 24 May 2022.
Kawade A, Gore M, Lele P, Chavan U, Pinnock H, Smith P, Juvekar S, Cunningham S, Khan F, Simpson C, et al. Interplaying role of healthcare activist and homemaker: a mixed-methods exploration of the workload of community health workers (accredited social health activists) in India. Hum Resour Health. 2021;19:7. https://doi.org/10.1186/s12960-020-00546-z.
Cerf ME. Healthy lifestyles and noncommunicable diseases: nutrition, the life-course, and health promotion. Lifestyle Med. 2021;2:e31.https://doi.org/10.1002/lim2.31.
Lencucha R, Kulenova A, Thow AM. Framing policy objectives in the Sustainable Development Goals: hierarchy, balance, or transformation? Global Health. 2023;19:5. https://doi.org/10.1186/s12992-023-00909-w.
de Onis M, Branca F. Childhood stunting: a global perspective. Matern Child Nutr. 2016;12 Suppl 1:12–26. https://doi.org/10.1111/mcn.12231
Black MM, Walker SP, Fernald LCH, Andersen CT, DiGirolamo AM, Lu C, McCoy DC, Fink G, Shawar YR, Shiffman J, et al. Early childhood development coming of age: science through the life course. Lancet. 2017;389:77–90. https://doi.org/10.1016/S0140-6736(16)31389-7
Richter LM, Daelmans B, Lombardi J, Heymann J, Boo FL, Behrman JR, Lu C, Lucas JE, Perez-Escamilla R, Dua T, et al. Investing in the foundation of sustainable development: pathways to scale up for early childhood development. Lancet. 2017;389:103–118. https://doi.org/10.1016/S0140-6736(16)31698-1.
Global Burden of Disease Child and Adolescent Health Collaboration. Child and adolescent health from 1990 to 2015: findings from the global burden of diseases, injuries, and risk factors 2015 study. JAMA Pediatr. 2017;171:573–92. https://doi.org/10.1001/jamapediatrics.2017.0250.
Drayton W, Brown C, Hillhouse K. Integrating social entrepreneurs into the “health for all” formula. Bull World Health Organ. 2006;84:591. https://doi.org/10.2471/blt.06.033928.
Maji A, Itodo DA. Exploring the potentials of social enterprises for poverty alleviation in Nigeria and Cameroon in the 21st century. Eur J Business Manag. 2016;8:10–14.
Menne B, Aragon de Leon E, Bekker M, Mirzikashvili N, Morton S, Shriwise A, Tomson G, Vracko P, Wippel C. Health and well-being for all: an approach to accelerating progress to achieve the Sustainable Development Goals (SDGs) in countries in the WHO European region. Eur J Public Health. 2020;30:i3-i9. https://doi.org/10.1093/eurpub/ckaa026.
GBD 2015 SDG Collaborators. Measuring the health-related Sustainable Development Goals in 188 countries: a baseline analysis from the Global Burden of Disease Study 2015. Lancet. 2016;388:1813–50. https://doi.org/10.1016/S0140-6736(16)31467-2
Cerf ME. Sustainable Development Goal integration, interdependence, and implementation: the environment–economic–health nexus and universal health coverage. Global Chall. 2019;3:1900021. https://doi.org/10.1002/gch2.201900021.
Raghupathi V, Raghupathi W. The influence of education on health: an empirical assessment of OECD countries for the period 1995–2015. Arch Public Health. 2020;78:20. https://doi.org/10.1186/s13690-020-00402-5.
Zimmerman EB, Woolf SH, Haley A. Understanding the relationship between education and health: a review of the evidence and an examination of community perspectives. In: Kaplan RM, Spittel ML, David DH, editors. Population health: behavioral and social science insights. Rockville, MD: National Institutes of Health; 2015. pp. 347–84.
Cerf ME. The Sustainable Development Goals: contextualizing Africa’s economic and health landscape. Global Chall. 2018;2:1800014. https://doi.org/10.1002/gch2.201800014.
Friedman J, York H, Graetz N, Woyczynski L, Whisnant J, Hay SI, Gakidou E. Measuring and forecasting progress towards the education-related SDG targets. Nature. 2020;580:636–9. https://doi.org/10.1038/s41586-020-2198-8.
Zajacova A, Lawrence EM. The relationship between education and health: reducing disparities through a contextual approach. Annu Rev Public Health. 2018;39:273–289. https://doi.org/10.1146/annurev-publhealth-031816-044628.
Caire G. [Review of human capital, a theoretical and empirical analysis with special reference to education, by Becker GS]. Rev Écon. 1967;18:132–133. https://doi.org/10.2307/3499575.
Mirowsky J, Ross CE. Education, social status, and health. New York: Aldine Transaction; 2003.
Herrmann B, Rundshagen V. Paradigm shift to implement SDG 2 (end hunger): a humanistic management lens on the education of future leaders. Int J Manag Educ. 2020;18:100368. https://doi.org/10.1016/j.ijme.2020.100368.
Nakidien T, Singh M, Sayed Y. Teachers and teacher education: limitations and possibilities of attaining SDG 4 in South Africa. Educ Sci. 2021;11:66. https://doi.org/10.3390/educsci11020066.
Unterhalter E. The many meanings of quality education: politics of targets and indicators in SDG4. Glob Policy. 2019;10:39–51. https://doi.org/10.1111/1758-5899.12591.
Mirowsky J, Ross CE. Education, learned effectiveness and health. Lond Rev Educ. 2005;3:205–20. https://doi.org/10.1080/14748460500372366.
Baker D. The schooled society: the educational transformation of global culture. Redwood City CA: Stanford University Press; 2014.
World Bank Data Team. 2019. New country classifications by income level: 2019–2020. http://blogs.worldbank.org/opendata/new-country-classifications-income-level-2019-2020. Accessed 21 Nov 2019.
World Bank Bank. Data. 2023. https://data.worldbank.org/region/sub-saharan-africa?view=chart. Accessed 21 Mar 2023.
Scott AJ. The longevity economy. Lancet Healthy Longev. 2021;2:828-35. https://doi.org/10.1016/S2666-7568(21)00250-6.
World Health Organization. The economics of the social determinants of health and health inequalities: a resource book. 2013. https://apps.who.int/iris/handle/10665/84213. Accessed 22 Mar 2023.
Kitamura N, Abbas K, Nathwani D. Public health and social measures to mitigate the health and economic impact of the COVID-19 pandemic in Turkey, Egypt, Ukraine, Kazakhstan, and Poland during 2020–2021: situational analysis. BMC Public Health. 2022;22:991. https://doi.org/10.1186/s12889-022-13411-6.
Adams J, White M, Moffatt S, Howel D, Mackintosh J. A systematic review of the health, social and financial impacts of welfare rights advice delivered in healthcare settings. BMC Public Health. 2006;6:81. https://doi.org/10.1186/1471-2458-6-81.
Baldwin SB, Eisenman DP, Sayles JN, Ryan G, Chuang KS. Identification of human trafficking victims in health care settings. Health Hum Rights. 2011;13:E36–49.
Ferguson HB, Bovaird S, Mueller MP. The impact of poverty on educational outcomes for children. Paediatr Child Health. 2007;12:701–6. https://doi.org/10.1093/pch/12.8.701.
Hone T, Macinko J, Millett C. Revisiting Alma-Ata: what is the role of primary health care in achieving the Sustainable Development Goals? Lancet. 2018;392:1461–72. https://doi.org/10.1016/S0140-6736(18)31829-4.
Marmot M. Social determinants of health inequalities. Lancet. 2005;365:1099–104. https://doi.org/10.1016/S0140-6736(05)71146-6.
Kieny MP, Bekedam H, Dovlo D, Fitzgerald J, Habicht J, Harrison G, Kluge H, Lin V, Menabde N, Mirza Z, et al. Strengthening health systems for universal health coverage and sustainable development. Bull World Health Org. 2017;95:537–9. https://doi.org/10.2471/BLT.16.187476
Boyce T, Brown C. Economic and social impacts and benefits of health systems: report. World Health Organization. Regional Office for Europe. 2019. https://apps.who.int/iris/handle/10665/329683. Accessed 22 Mar 2023.
Bhatnagar A, Scott K, Govender V, George A. Pushing the boundaries of research on human resources for health: fresh approaches to understanding health worker motivation. WHO South East Asia J Public Health. 2018;7:13–17. https://doi.org/10.4103/2224-3151.228422
World Health Organization. Global strategy on human resources for health: workforce 2030. Geneva: World Health Organization; 2016.
World Health Organization/Global Health Workforce Alliance. Human resources for health: foundation for universal health coverage and the post-2015 development agenda. Report of the third global forum on human resources for health, (Nov 2013) Recife Brazil. Geneva: World Health Organization; 2014.
World Health Organization. High-level commission on health employment and economic growth: report of the expert group. Geneva: World Health Organization; 2016. https://apps.who.int/iris/handle/10665/250040.
World Health Organization. The world health report: 2006: working together for health. Geneva: World Health Organization; 2006. https://apps.who.int/iris/handle/10665/43432.
GBD 2016 DALYs and HALE Collaborators. Global, regional, and national disability-adjusted life-years (DALYs) for 333 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390:1260–344. https://doi.org/10.1016/S0140-6736(17)32130-X.
World Health Organization. The Global Health Observatory. Global Health Workforce statistics database. 2023. https://www.who.int/data/gho/data/themes/topics/health-workforce. Accessed 5 Apr 2023.
Aluttis C, Bishaw T, Frank MW. The workforce for health in a globalized context—global shortages and international migration. Glob Health Action. 2014;7:23611. https://doi.org/10.3402/gha.v7.23611.
Oladeji BD, Gureje O. Brain drain: a challenge to global mental health. BJPsych Int. 2016;13:61–3. https://doi.org/10.1192/s2056474000001240.
Mills EJ, Kanters S, Hagopian A, Bansback N, Nachega J, Alberton M, Au-Yeung CG, Mtambo A, Bourgeault IL, Luboga S, et al. The financial cost of doctors emigrating from sub-Saharan Africa: human capital analysis. BMJ. 2011;343:d7031. https://doi.org/10.1136/bmj.d7031.
Cerf ME. Health worker resourcing to meet universal health coverage in Africa. Int J Healthc Manag. 2019;14:789–96. https://doi.org/10.1080/20479700.2019.1693711.
Author information
Authors and Affiliations
Contributions
MC wrote the manuscript, prepared the figures and table, and reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cerf, M.E. The social-education-economy-health nexus, development and sustainability: perspectives from low- and middle-income and African countries. Discov Sustain 4, 37 (2023). https://doi.org/10.1007/s43621-023-00153-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43621-023-00153-7