Abstract
Purpose
This prospective randomized study compares the clinical and radiographic long-term results at least 16 years after total knee arthroplasty (TKA) between a mobile-bearing high flex and a fixed-bearing posterior-stabilized knee.
Methods
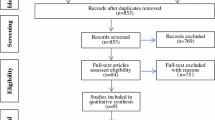
In 2000, we included 60 patients who underwent a TKA. Patients were divided into two groups. At the time of the follow-up after a minimum of 16 years (16.5 years ± 0.6), 16 patients had died for causes unrelated to the operation, 15 were lost to the follow-up. Five patients of the high flex group had a revision. The final evaluation included the hospital for special surgery score (HSS) and radiographs. Using the X-rays and the Knee Society Roentgenographic Evaluation and Scoring System, radiolucent lines and the maximal knee flexion were determined.
Results
No significant differences between the two groups were found. The mean HSS score of LPS group patients was 87.9 (± 10.6) points and that of the high flex group was 93.1 (± 7.4) points. Five patients of the high flex group had undergone a reoperation. One knee was revised for painful mid-flexion instability and the others for symptomatic aseptic loosening of the components.
Conclusion
The long-term follow-up does not show any clear benefits and even a higher incidence of implant loosening using the mobile-bearing high-flex knee.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The high flex total knee arthroplasty (TKA) was developed for patients requiring a deeper flexion up to 150° for reasons of profession, culture and religion. Therefore, the high flex knee (NexGen LPS Flex mobile, Zimmer Inc., Warsaw, USA) was specially designed to prevent increasing wear and to maintain knee stability in comparison to the regular posterior stabilised (PS) knee (NexGen LPS). Therefore, it is a mobile-bearing system that allows an internal and external rotation of 25° each. An additional 2 mm bone cut from the posterior femoral condyles leads to a greater curvature of the posterior condyles. Furthermore, the tibial insert has an anterior cut to avoid patellar tendon impingement during deep flexion. The special design is expected to reduce contact stresses at the different interfaces and decreased polyethylene wear rate. Rotational mobility of the bearing surface might also optimize the tibio-femoral alignment, which could lead to a higher stability and increased anterior knee pain [1]. Wohlrab et al. and Radetzki et al. previously reported the short-, mid- and long-term results (3-month, 3-year, 5-year and 10-year follow-up) of a randomised clinical and radiological study comparing the results after TKA using the NexGen Flex mobile knee versus the NexGen LPS knee [2, 3]. 3- and 5-year postoperatively, there were no significant differences between both groups for the hospital for special surgery score (HSS) either, nor for the radiological results. A clear advantage of the mobile-bearing knee prostheses could not be reflected in the clinical results up to 5 years after surgery. Other studies had even shown a higher complication rate postoperatively using mobile-bearing systems. Ridgeway et al. observed early coronal plane instability and knee pain in 25 cases within 2 years postoperatively [4]. Further, subluxation, dislocation, increasing wear rate and stress shielding were observed [4]. The long-term results after 10 years have shown no clear benefits and even higher incidence of implant loosening of the high flex knee system [2].
The aim of this study was to compare clinical and radiographic long-term results at least 16 years after of TKA using a high flex knee (NexGen Flex mobile) versus a regular PS knee (NexGen LPS). In addition, the study should also evaluate if the high flex knee system will cause additional implant loosening over time.
Materials and Methods
In 2000, we included 60 patients who underwent a TKA in a prospective randomized study. Patients were divided into two groups by following a randomization list, preoperatively. In 30 patients, the NexGen LPS implant (Zimmer Inc., Warsaw, USA) was implanted. The remaining 30 patients received the high flex knee NexGen LPS Flex mobile (Zimmer Inc.). All patients in this study were diagnosed with unilateral degenerative arthritis, had a body mass index (BMI) less than 30, no previous joint infection, a varus deformity of less than 10° or a valgus deformity less than 5°. Preoperatively, we recorded patients’ data (age, gender, height, body weight) as well as the hospital for special surgery score (HSS) [5]. All surgeries were done by two well-trained surgeons. The surgeons were equally familiar with both knee system and their learning curves were completed. The operative procedures were similar in both the groups. In all procedures, a mid-vastus approach was used. The patella was resurfaced and all implants were cemented in all cases. Tourniquet was used in each patient. Drains were removed 48 h after surgery. The rehabilitation program during admission was the same for both the groups and the patients were discharged 5–7 days after surgery.
At the time of the follow-up after a minimum of 16 years (16.5 years ± 0.6), 16 patients (7 in the LPS group, 9 in the high flex group) had died for causes unrelated to the operation. Their preoperative average age was already 72.1 years and, therefore, well over 85 years at the time of the follow-up. Fifteen (8 in the LPS group, 7 in the high flex group) were lost to the follow-up. Five patients of the high flex group had undergone a reoperation of their knee. This left a total of 15 LPS knees and 9 high flex knees for final evaluation including the HSS score and radiographs (AP view in extension and lateral view in maximal flexion). Using the X-rays and the Knee Society Roentgenographic Evaluation and Scoring System [6], radiolucent lines and the maximal knee flexion were determined. Statistical analysis was performed with SPSS 22 software (SPSS Inc., Chicago, USA). Descriptive statistics presented include the mean and standard deviation (SD). A confidence interval of 95% was assumed (significance level p < 0.05). The data were analysed with Student’s t test.
Results
Preoperatively, there were no relevant differences between the two groups. The mean HSS score of LPS group patients was 48.6 (± 8.5) points and that of the high flex group was 54.4 (± 6.3) points. In the subgroups of the HSS score, there were no differences except for the category pain that was less in the high flex group. There were also no relevant differences in the maximal knee flexion between the two groups preoperatively (Table 1).
At the 16-year follow-up, there were no significant differences between the two groups regarding the clinical and radiographic results. The mean HSS score of LPS group patients was 87.9 (± 10.6) points and that of the high flex group was 93.1 (± 7.4) points (p = 0.21). Especially the theoretical advantages of high flex knee systems, namely the range of motion (high flex 14.8, LPS 14.5, p = 0.71), joint stability (high flex 9.6, LPS 9.3, p = 0.59) and function (high flex 21.7, LPS 21.2, p = 0.46) were comparable. In the radiological evaluation, the maximal flexion of the high flex group was 115.7° (± 8.5) and that of the LPS group 113.5 (± 11.1) (p = 0.52) (Table 1).
Using the Knee Society Roentgenographic Evaluation and Scoring System, there was one patient of the LPS group with radiolucent lines smaller than 10 mm in zones 1 and 4 of the tibia in the AP view without clinical symptoms and a HSS score of 91.
Total revision surgeries were performed in 5 knees, all in the high flex group (16.7%). One patient of the high flex group had a painful mid-flexion instability that needed to be revised after 5 years. The mean revision rate due to aseptic loosening was 4 of 30 knees (13.3%) and all were men. Because of symptomatic aseptic loosening of the cemented tibial prosthesis, four high flex knees were revised after 7, 8, 14 and 16 years. In the AP view, tibial radiolucent lines were found just in zone 1 for two knees, zone 1 and 5 in a second knee and another showed a progressive lucency in all zones with dislocation, as described in the Knee Society Roentgenographic Evaluation and Scoring System (Fig. 1). There was no noticed revision in the LPS group.
Discussion
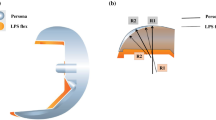
The high flex total knee arthroplasty with a mobile-bearing system was developed to increase the ROM and to optimize the tibio-femoral alignment (Figs. 2, 3). This self-alignment should theoretically decrease the wear rate with a positive effect in preventing early implant loosening. Several studies had shown that these advantages are not reproducible in clinical practice in considering short- and mid-term results [1, 3, 4, 7]. In the presented study, we compared the clinical and radiographic long-term results of the high flex knee (NexGen Flex mobile, Zimmer Inc.) and regular PS knee (NexGen LPS, Zimmer Inc.) after a minimum of 16 years. Wohlrab et al. already reported the short- and mid-term results (3-month, 3-year and 5-year follow-up) of both study groups [3]. Three months postoperatively, there were better results in scores for pain, ROM (122.5° vs. 107.33°), as well as in the overall HSS (87.21 vs. 82.68 points) in the high flex group. 3, 5 and 10 years postoperatively, there were no significant differences between both groups for the hospital for special surgery score (HSS) either, nor for the radiological results [2, 3].
After 16 years, we found no differences between patients with these implant designs with respect to pain, function, range of motion, muscle strength, flexion deformity and instability, as well. The theoretical benefit of high flex knee systems, namely the ROM (113.5 vs. 108.3), joint stability and function were still similar. Choi et al. did also find no significant differences between the two groups regarding postoperative total arc of knee motion, Knee Society score and function score [8]. In the long-term follow-up study after a minimum of 20 years, Kim determined comparable outcomes and survivorship for the high-flexion knee in comparison to a standard knee as well [9]. On the other hand, several studies have reported an improved ROM comparing standard designs with high flex designs within the first two years after surgery [10,11,12,13]. Anyway, the majority of prospective randomized trials showed no significant difference comparing high flex knee system to conventional knee system [3, 14,15,16]. It is assumed that the preselection of patients with at least 90° of flexion and not excessively high BMIs is jointly responsible for the clinical results with respect to function and flexion [16].
Instability and subluxation are typical complications especially with mobile-bearing systems [4, 17]. We just revised one patient of the high flex group for painful mid-flexion instability after 5 years.
It is postulated that mobile-bearing systems could reduce contact stresses at the different interfaces, resulting in a decrease of the wear rate with a positive effect in preventing early implant loosening [18,19,20]. The results of our follow-up after a minimum of 16 years cannot confirm this advantage. Choi et al. also observed a significantly higher revision rate due to aseptic loosening for the high flex knee (4.9%) in comparison to the conventional knee (0.6%) in a large population in the mid-term follow-up [8]. Han et al. reported a 38% aseptic loosening rate in 72 high-flexion knees at a mean follow-up of 32 months as well [21]. Critical stress was noticed at the femoral fixation site at high-flexion angle and lead to early loosening of the femoral component in high-flexion knees [22]. We were not able to confirm this association having more tibial than femoral loosening in our series. Kim et al. had two knees (0.2%) in the high-flexion knee group undergoing a revision of both femoral and tibial components after a mean of 13.2 years. An increased incidence of femoral component loosening in the high-flexion knee group could not be found in that study [23].
The major weakness of this study is the high number of lost patients in each group. All in terms, 15 (8 in the LPS group, 7 in the high flex group) knees (25%) were lost to the final follow-up although an extensive effort in contacting all patients was undertaken. However, it is a quite obvious limitation and inherent difficulty in dealing with long-term studies [4]. In addition, 16 patients died until the 16-year examination. An already old age of these patients at the beginning of the study limits the long-term control. As a consequence, the amount of included patients will have to be increased right from the beginning of long-term follow-ups in the future.
In summary, this prospective, randomized controlled trial demonstrated no benefit to the high flex knee system versus a regular PS knee up to 16 years after surgery. Five patients of the high flex group had to be revised for reasons of instability and aseptic implant loosening. There were no revisions in the LPS group.
The long-term follow-up does not show any clear benefits and even a higher incidence of implant loosening using the high flex knee (NexGen Flex mobile). It must be seriously revaluated and used carefully considering the higher revision rate. Further studies are required to prove long-term adverse effects of high flex knee systems.
Change history
16 August 2021
A Correction to this paper has been published: https://doi.org/10.1007/s43465-021-00449-8
11 March 2022
A Correction to this paper has been published: https://doi.org/10.1007/s43465-022-00615-6
References
Lädermann, A., Lübbeke, A., Stern, R., Riand, N., & Fritschy, D. (2008). Fixed-bearing versus mobile-bearing total knee arthroplasty: a prospective randomised, clinical and radiological study with mid-term results at 7 years. The Knee, 15(3), 206–210.
Radetzki, F., Wienke, A., Mendel, T., Gutteck, N., Delank, K.-S., & Wohlrab, D. (2013). High flex total knee arthroplasty—a prospective, randomized study with results after 10 years. Acta Orthopaedica Belgica, 79(5), 536–540.
Wohlrab, D., Hube, R., Zeh, A., & Hein, W. (2009). Clinical and radiological results of high flex total knee arthroplasty: a 5 year follow-up. Archives of Orthopaedic and Trauma Surgery, 129(1), 21–24.
Ridgeway, S., & Moskal, J. T. (2004). Early instability with mobile-bearing total knee arthroplasty: a series of 25 cases. The Journal of Arthroplasty, 19(6), 686–693.
Insall, J. N., Dorr, L. D., Scott, R. D., & Scott, W. N. (1989). Rationale of the Knee Society clinical rating system. Clinical Orthopaedics and Related Research, 248, 13–14.
Ewald, F. C. (1989). The Knee Society total knee arthroplasty roentgenographic evaluation and scoring system. Clinical Orthopaedics and Related Research, 248, 9–12.
Wohlrab, D., Ditl, J., Herrschelmann, R., Schietsch, U., Hein, W., & Hube, R. (2005). Does the NexGen LPS flex mobile knee prosthesis offer advantages compared to the NexGen LPS?—A comparison of clinical and radiological results. Zeitschrift Fur Orthopadie Und Ihre Grenzgebiete, 143(5), 567–572.
Choi, Y.-J., Lee, K. W., Ha, J.-K., Bae, J.-Y., Lee, S. K., Kim, S.-B., et al. (2018). Comparison of revision rates due to aseptic loosening between high-flex and conventional knee prostheses. Knee Surgery & Related Research, 30(2), 161–166.
Kim, Y.-H., Park, J.-W., & Jang, Y.-S. (2020). 20-year minimum outcomes and survival rate of high-flexion versus standard total knee arthroplasty. The Journal of Arthroplasty.
Bin, S. I., & Nam, T. S. (2007). Early results of high-flex total knee arthroplasty: comparison study at 1 year after surgery. Knee Surgery, Sports Traumatology, Arthroscopy, 15(4), 350–355.
Gupta, S. K., Ranawat, A. S., Shah, V., Zikria, B. A., Zikria, J. F., & Ranawat, C. S. (2006). The P.F.C. sigma RP-F TKA designed for improved performance: A matched-pair study. Orthopedics, 29(9 Suppl), S49–52.
Huang, H.-T., Su, J. Y., & Wang, G.-J. (2005). The early results of high-flex total knee arthroplasty: a minimum of 2 years of follow-up. The Journal of Arthroplasty, 20(5), 674–679.
Weeden, S. H., & Schmidt, R. (2007). A randomized, prospective study of primary total knee components designed for increased flexion. The Journal of Arthroplasty, 22(3), 349–352.
Hamilton, W. G., Sritulanondha, S., & Engh, C. A. (2011). Results of prospective, randomized clinical trials comparing standard and high-flexion posterior-stabilized TKA: a focused review. Orthopedics, 34(9), e500–503.
Kim, Y.-H., Sohn, K.-S., & Kim, J.-S. (2005). Range of motion of standard and high-flexion posterior stabilized total knee prostheses. A prospective, randomized study. The Journal of Bone and Joint Surgery American, 87(7), 1470–1475.
McCalden, R. W., MacDonald, S. J., Bourne, R. B., & Marr, J. T. (2009). A randomized controlled trial comparing “high-flex” vs “standard” posterior cruciate substituting polyethylene tibial inserts in total knee arthroplasty. The Journal of Arthroplasty, 24(6 Suppl), 33–38.
Stiehl, J. B., Hamelynck, K. J., & Voorhorst, P. E. (2006). International multi-centre survivorship analysis of mobile bearing total knee arthroplasty. International Orthopaedics, 30(3), 190–199.
Buechel, F. F., & Pappas, M. J. (1990). Long-term survivorship analysis of cruciate-sparing versus cruciate-sacrificing knee prostheses using meniscal bearings. Clinical Orthopaedics and Related Research, 260, 162–169.
Goodfellow, J., & O’Connor, J. (1978). The mechanics of the knee and prosthesis design. The Journal of Bone and Joint Surgery British, 60-B(3), 358–369.
O’Connor, J. J., & Goodfellow, J. W. (1996). Theory and practice of meniscal knee replacement: Designing against wear. Proceedings of the Institution of Mechanical Engineers Part H, Journal of Engineering in Medicine, 210(3), 217–222.
Han, H. S., Kang, S.-B., & Yoon, K. S. (2007). High incidence of loosening of the femoral component in legacy posterior stabilised-flex total knee replacement. The Journal of Bone and Joint Surgery British, 89(11), 1457–1461.
Zelle, J., Janssen, D., Van Eijden, J., De Waal, M. M., & Verdonschot, N. (2011). Does high-flexion total knee arthroplasty promote early loosening of the femoral component? Journal of Orthopaedic Research: Official Publication of the Orthopaedic Research Society, 29(7), 976–983.
Kim, Y.-H., Park, J.-W., & Kim, J.-S. (2017). Do high-flexion total knee designs increase the risk of femoral component loosening? The Journal of Arthroplasty, 32(6), 1862–1868.
Funding
Open Access funding enabled and organized by Projekt DEAL. The authors confirm that there are no financial and personal relationships with any other people or organisations that could inappropriately influence the content or the statements of the submitted article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The details of affiliation 1 were incorrect and have been corrected.
The original online version of this article was revised due to a retrospective Open Access order.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Radetzki, F., Zeh, A., Delank, KS. et al. The High Flex Total Knee Arthroplasty—Higher Incidence of Aseptic Loosening and No Benefit in Comparison to Conventional Total Knee Arthroplasty: Minimum 16-Years Follow-Up Results. JOIO 55 (Suppl 1), 76–80 (2021). https://doi.org/10.1007/s43465-020-00276-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-020-00276-3