Abstract
Background
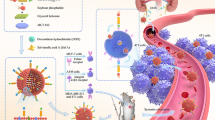
Traditional small-molecule chemotherapeutics usually do not distinguish tumors from healthy tissues. However, nanotechnology creates nanocarriers that selectively deliver drugs to their site of action. This work is the next step in the development of the quantum dot−β−cyclodextrin−folic acid (QD−β−CD−FA) platform for targeted and selected delivery of C−2028 unsymmetrical bisacridine in cancer therapy.
Methods
Herein, we report an initial biological evaluation (using flow cytometry and light microscopy) as well as cell migration analysis of QD−β−CD(C−2028)−FA nanoconjugate and its components in the selected human lung and prostate cancer cells, as well as against their respective normal cells.
Results
C−2028 compound induced apoptosis, which was much stronger in cancer cells compared to normal cells. Conjugation of C−2028 with QDgreen increased cellular senescence, while the introduction of FA to the conjugate significantly decreased this process. C−2028 nanoencapsulation also reduced cell migration. Importantly, QDgreen and QDgreen−β−CD−FA themselves did not induce any toxic responses in studied cells.
Conclusions
In conclusion, the results demonstrate the high potential of a novel folic acid-targeted receptor quantum dot−β−cyclodextrin carrier (QDgreen−β−CD−FA) for drug delivery in cancer treatment. Nanoplatforms increased the amount of delivered compounds and demonstrated high suitability.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancers or malignant neoplasms are still a leading cause of morbidity and mortality worldwide [1, 2]. The conventional strategies in cancer treatment involve surgical resection of the solid localized tumors, radiotherapy with X-rays, and chemotherapy used as a single treatment or in combination [3,4,5,6]. Although all of them are the most recommended, they are often not enough to provide an effective cure and/or protection from this devastating disease. Chemotherapy, which generally uses small-molecule compounds to kill fast-growing cancer cells and/or delay their growth, is one of the most common methods of treatment for blood-related cancers and solid metastatic tumors [7]. However, the development of a potent anticancer drug is a highly complex and multi-factorial process that faces many difficulties. Drug low water solubility, rapid metabolic decomposition, and aggregation could reduce its bioavailability [8, 9]. An important factor that limits drug clinical application is its non-selective action, which consists of toxicity to all rapidly proliferating cells– both cancer and normal cells [6, 10, 11]. This may lead to some serious adverse effects (e.g., side effects and multidrug resistance) or even cause the patient’s death [12].
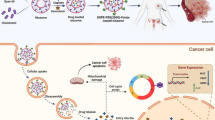
The urgent need to obtain a ‘smart’ drug that can distinguish tumors from normal tissues, so it is transported to exactly the right place of action, raises progress in nanotechnology [12]. In recent years, nanoscale technology has provided a wide spectrum of opportunities to design and develop multi-functional devices that can target, diagnose, and treat cancers with high efficiency [13]. One example of such innovative strategies is nanoparticle-based platforms for the targeted delivery and release of drugs, proteins, peptides, or nucleic acids [11, 14, 15]. Nanoparticles (NPs) present in these systems include but are not limited to micelles, liposomes, dendrimers, carbon nanotubes, magnetic NPs, and quantum dots (QDs) [16]. They are usually designed or chosen based on their size and characteristics according to the pathophysiology of the tumors. Compared to traditional anticancer drugs, NP-based drug carriers have specific advantages, such as increased stability and biocompatibility, enhanced permeability, and retention effect [17, 18]. The improvement of drug bioavailability in tumor tissue is achieved by exploiting the differences between the normal physiological environment and the tumor microenvironment (TME) [19, 20]. The unique properties of TME, which are closely related to the occurrence and development of tumors, include acidity, hypoxia, excessive reactive oxygen species, and high glutathione concentration as well as overexpression of specific enzymes and receptors. Hence, TME-stimuli-responsive systems, such as pH-responsive, hypoxia-responsive, redox-sensitive, or targeting molecule-conjugated nanocarriers, are gaining more attention [19,20,21]. Active targeting of neoplastic cells in the latter can be realized through direct interactions between ligands on the surface of NPs and receptors overexpressed on the surface of cancer cells [12]. In view of this, promising tumor targets are folic acid (FA) receptors (FRs) as their expression is often enhanced on the surface of 40% of solid tumors, but negligible in the majority of healthy tissues [22]. Folic acid-drug delivery systems can enter tumor cells through receptor-mediated endocytosis which allows internalized NPs to successfully release drug molecules [23]. In this way, it improves the drug’s therapeutic efficacy while protecting normal cells from cytotoxicity. Other docking sites for precise targeting of anticancer chemotherapeutics include receptors for transferrin (TfR) [24, 25], G-proteins (GPCRs) [26], or epidermal growth factor (EGFR) [27].
Considering the above, we previously constructed the quantum dots−β−cyclodextrin−folic acid (QD− β−CD−FA) vehicles as a platform for improved unsymmetrical bisacridine (UA) delivery and controllable drug release in various human cancer cells [28,29,30,31]. It was fully structurally and morphologically characterized [28, 30, 31]. The details can also be found in the Supplementary information. In this multi-component system, we applied quaternary QDs (Ag−In−Zn−S nanocrystals) decorated with β−CD which was the main skeleton for drug encapsulation. QDs represent a promising avenue for the design and engineering of versatile drug nanocarriers. A combination of unique physical, chemical, and optical properties enables the study of QD interactions with biological systems through real-time monitoring of NP biodistribution, intracellular uptake, controlled drug release, and long-term nanocarrier fate. Therefore, QDs have a significant impact on the further development of life sciences, including their applications in bio-imaging, diagnostics, and biosensing [32, 33]. CDs are amphiphilic cyclic oligosaccharides. Due to their unique internal cavity, CDs are regarded to be an efficient and accessible unit for the construction of drug delivery systems. They are characterized by high stability, good biocompatibility, low immunogenicity, negligible toxicity, and modifiability. In addition, CDs can circumvent the limitations of NPs, such as low encapsulation efficiency and drug loading [34]. FA was used as a self-navigating molecule to specifically bind to FRs. C−2028 was selected as a model compound from a novel class of patented anticancer drug candidates - UAs - developed in our research team. These acridine analogs, in non-conjugated form, exhibited high cytotoxic activity against a lot of tumor cells in vitro (e.g., human breast, prostate, pancreatic, colon, and lung cancers) as well as demonstrated high antitumor efficacy against several types of human cancer xenografts in nude mice, including pancreatic, colorectal, and lung cancers [35]. So far, we have shown that the application of QDs and FA successfully increased the cellular uptake of the studied C−2028 compound, especially in lung H460 and prostate Du-145 cell lines with no change in the cytotoxic activity of this chemotherapeutic. Then, we demonstrated the mechanism of internalization of QD−β−CD(C−2028)−FA vehicles in all cell types studied. We achieved the drug release profile at an intracellular level and proved pH-dependent drug release from its nanoconjugates in the noncellular system.
The current work is the next step in the development of the QD−β−CD−FA platform for the efficient targeted delivery and release of UA drugs in cancer cells. Herein, we report an initial biological evaluation, the cell cycle progression, including induction of apoptosis, and cellular senescence as well as analysis of cell migration of our nanosystem for potential application in the treatment of lung and prostate cancers in humans. The biological response of QD−β−CD(C−2028)−FA and each of its components alone was assessed in vitro against human lung (H460) and prostate (Du-145 and LNCaP) cancer cells as well as against their respective (MRC-5 and PNT1A) normal cells.
Materials and methods
Materials
1-Ethyl-3-(3-dimethylaminopropyl)carbodiimide hydrochloride (EDC×HCl; product cat. no. E6383), 4-dimethylaminopyridine (DMAP; product cat. no. 8.51055), acetone (product cat. no. 179,124), diethyl ether (product cat. no. 673,811), dimethyl sulfoxide (DMSO; product cat. no. D8418), folic acid (FA; product cat. no. 1.03984), hydrochloric acid (HCl; product cat. no. 258,148), methanol (MeOH; product cat. no. 34,860), penicillin (product cat. no. P3032), phenol (product cat. no. 8.43984), streptomycin (product cat. no. S9137), trichloromethane (CHCl3; product cat. no. 366,927), X-gal (5-bromo-4-chloro-3-indolyl-β-D-galactosidase; product cat. no. B4252), and β−cyclodextrin (β−CD; product cat. no. C4805) were all purchased from Sigma-Aldrich (Merck KGa, Darmstadt, Germany). All used reagents and chemicals were of the highest purity available and used as received. Ultrapure water (conductivity 0.056 µS·cm− 1) was used to prepare all aqueous solutions (Milli-Q® IQ 7005 Water Purification System, Merck KGa).
C−2028 compound (9-{N-[(imidazo[4,5,1-de]-acridin-6-on-5-yl)aminopropyl]-N-methylaminopropylamino}-1’-nitroacridine), QDgreen, QDgreen−β−CD−FA, QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA vehicles were synthesized in-house. The materials required for their synthesis, as well as the structural evidence for all these compounds, were provided in the Supplementary information (Figures S1–S7).
Methods
Preparation of C−2028: 9-{N-[(imidazo[4,5,1-de]-acridin-6-on-5-yl)aminopropyl]-N-methylaminopropylamino}-1’-nitroacridine×1.5 HCl
A mixture of derivative 5-{3-[N-(3-aminopropyl)-N-methylamino]propylamino}-imidazo[4,5,1-de]-acridin-6-one×2 HCl (0.001 mol), 5 mL phenol, and 9-phenoxy-1-nitroacridine (0.001 mol) was stirred at 90 °C for 24 h. After cooling, the reaction mixture was dissolved in methanol (MeOH) (~ 10 mL), poured into diethyl ether (~ 100 mL), and then stirred for 0.5 h. The precipitate was filtered off, washed with diethyl ether, and then with acetone. The product was dissolved in MeOH and a small quantity of silica gel was added and the solvent was evaporated. The remainder was loaded onto a dry chromatography column. The initial eluent was CHCl3 and then CHCl3/MeOH at a ratio of (15:1, 10:1 v/v), CHCl3/MeOH/NH3 (10:1:0.1 v/v); yield 45%, m.p. 207–209 °C. Procedures of the synthesis of derivatives: 5-{3-[N-(3-aminopropyl)-N-methylamino]propylamino}-imidazo[4,5,1-de]-acridin-6-one×2 HCl and 1-{3-[N-(3-aminopropyl)-N-methylamino]propylamino}-4-nitro-9(10 H)-acridone×2 HCl were described in the Supplementary information.
Elemental analysis: C34H34N7O3Cl1,5 × 2 H2O; electrospray ionization mass spectrometry (ESI-MS) C34H31N7O3 [M + 1]+ 586.258. ESI-MS analyses were performed on an Agilent 6500 Series Accurate-Mass Quadrupole-Time of Flight (Q-TOF) mass spectrometer (Agilent Technologies, Santa Clara, CA, USA). The system was controlled by Agilent MassHunter Workstation software (Agilent Technologies). ESI-MS spectrum for C−2028 was presented in Figure S1.
1H NMR (Me2SO-d6 + TFA) δ: 9.79 (s, 1H, N10CH); 9.70 (br.s, 1H, N1HCH2); 8.43 (d, J = 8.3 Hz, 1H, Ar-H); 8.37–8.41 (m, 1H, Ar-H); 8.36 (d, J = 7.8 Hz, 1H, Ar-H); 8.20 (d, J = 7.3 Hz, 1H, Ar-H); 8.08 (d, J = 8.8 Hz, 1H, Ar-H); 7.99–8.02 (m, 2 H, Ar-H); 7.92–7.99 (m, 2 H, Ar-H); 7.82 (d, J = 8.8 Hz, 1H, Ar-H); 7.63 (t, J = 7.6 Hz, 1H, Ar-H); 7.58 (t, J = 7.3 Hz, 1H, Ar-H); 7.01 (d, J = 9.3 Hz, 1H, C2); 3.58–3.63 (m, 2 H, CH2N9’H) 3.48–3.56 (m, 2 H, CH2N5H); 2.91–3.27 (m, 4 H, CH2NCH3CH2); 2.75 (s, 3 H, NCH3); 1.90–2.22 (m, 4 H, CH2CH2CH2N9’H; N5HCH2CH2CH2). 1H NMR spectra for C−2028 were presented in Figure S2.
Preparation of Ag1.0In1.2Zn5.6S9.4 nanocrystals (QDgreen)
The alloyed Ag−In−Zn−S quantum dots were prepared through the injection of sulfur dissolved in oleylamine (S/OLA) into a mixture of silver nitrate (AgNO3), indium (III) chloride (InCl3), zinc stearate, and 1-dodecanothiol (DDT) dissolved in 1-octadecene (ODE). This procedure allows for obtaining alloyed Ag−In−Zn−S quantum dots smoothly varying in composition via strict control of the precursor molar ratios. To stabilize the synthesized Ag−In−Zn−S quantum dots in a water solution, the initial hydrophobic ligands (stearic acid and 1-aminooctadecane) were exchanged for hydrophilic ligands: 11-mercaptoundecanoic acid (MUA). The quantum dots before and after (QDgreen) ligands exchange were spherical. Their diameter, as determined from transmission electron microscopy (TEM) images, were 3.2 ± 0.4 nm and 3.1 ± 0.6 nm respectively (Figure S3). In the obtained quantum dots (QDgreen), the inorganic core content (Ag1.0In1.2Zn5.6S9.4) was determined based on energy-dispersive X-ray spectroscopy (EDS) data (Figure S4). Hydrophilic quantum dots were labeled (QDgreen) due to their green luminescence (λmax = 576 nm, Figure S5).
Preparation of QDgreen−β−CD−FA
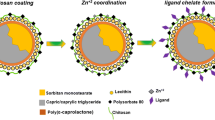
The synthesis of the QD−β−CD−FA was performed according to the literature procedure [30]. In brief, in the first step, the QD−β−CD was synthesized using the formation of ester bonds between primary hydroxyl groups from β−CD and carboxyl functionalities on the surface of the QD. Then, using the formation of ester linkages between primary hydroxyl groups from β−CD and carboxyl functionalities of FA the QD−β−CD−FA nanoconjugate was formed.
Preparation of QDgreen−C−2028 and QDgreen− β−CD(C−2028)− FA
The two conjugates QDgreen−C−2028 and QDgreen− β−CD(C−2028)−FA were formed by non-covalent interactions. To attach the C−2028 molecules to the QDgreen nanocrystals modified with 11-mercaptoundecanoic acid, the mixture of QDgreen (2 mg·mL−1) and C−2028 (0.8 mM) in 0.02 M phosphate buffer pH 7.4 was first sonicated in a water bath for ca. 15 min and then stirred overnight in a ThermoMixer at room temperature. The as-obtained solution was dialyzed twice against 0.02 M PBS buffer pH 7.4 to remove unbound C−2028 molecules.
In turn, the formation of the QDgreen−β−CD(C−2028)−FA nanoconjugate took advantage of the properties of forming inclusion complexes in which the host is β−cyclodextrin while the guest is a potential anticancer drug (C−2028). The procedure for forming such a complex is very simple and involves preparing a mixture of QDgreen− β−CD−FA hybrid (1.0 mg·mL− 1) and C−2028 (300 µM), which was incubated overnight at room temperature. The unreacted mixture components were removed through a dialysis process against ultrapure water.
Cell culture
Three cancer cell lines and two normal cell lines were used to perform experiments in this work. The human non-small-cell lung cancer (H460), human prostate cancer (Du-145 and LNCaP), and human fetal lung fibroblasts (MRC-5) cell lines were purchased from the American Type Culture Collection (ATCC, USA). The human prostate PNT1A cell line was kindly provided by Prof. Jędrzej Antosiewicz from the Medical University of Gdańsk (Gdańsk, Poland). H460, LNCaP, and PNT1A cells were cultured in RPMI 1640 medium (Sigma-Aldrich, USA, product cat. no. R0883). Du-145 and MRC-5 cells were grown in an EMEM medium (Eagle’s Minimal Essential Medium, Sigma-Aldrich, USA, product cat. no. M2279). Both media were supplemented with 10% FBS (fetal bovine serum; Biowest, USA, product cat. no. S1520), 100 units·mL− 1 of penicillin (Sigma-Aldrich, Israel, product cat. no. P3032), and 100 µg·mL− 1 of streptomycin (Sigma-Aldrich, China, product cat. no. S9137). MRC-5 cells were cultured in an EMEM medium containing only 10% FBS without antibiotics. All cells grew were incubated in a humidified atmosphere and 5% CO2 at 37 °C according to the standard procedures.
Concentrations of the compounds in the experiments
The cytotoxic activity of all studied compounds against H460, Du-124, LNCaP, MRC-5, and PNT1A cells was examined previously by MTT assay [30]. In order to treat cells with the same concentration of the C−2028 compound, regardless of the form of its administration (unconjugated or conjugated form), corresponding to the estimated IC80 value for C−2028 alone following 72 h of incubation with cancer cells was chosen. The concentrations used in the experiments for C−2028, β−CD(C−2028), QDgreen−C−2028, and QDgreen−β− CD(C−2028)−FA nanoconjugates were 0.035 µM for H460 and MRC-5, 0.024 µM for Du-145, and 0.133 µM for LNCaP and PNT1A cell lines, respectively. The concentrations of different forms of nanoplatform (QDgreen, β −CD, and QDgreen−β−CD−FA), corresponding to the IC80 value of unbound C − 2028 compound in the nanoconjugates, were 1.2 µg·mL− 1 for H460 and MRC-5, 0.8 µg·mL− 1 for Du-145, and 4.4 µg·mL− 1 for LNCaP and PNT1A cell lines, respectively.
Cell cycle analysis
The PI/RNase Staining Kit (BD Pharmingen, Franklin Lakes, NJ, USA, product cat. no. 550,825) was used for DNA content analysis in accordance with the manufacturer’s recommendations. Briefly, the cells were seeded onto tissue culture plates and allowed to adhere overnight. After treatment the cells with QDgreen, QDgreen− β− CD− FA, C−2028, QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA for 24, 72, and 144 h at IC80 value, cells were harvested from the plates by incubation with a solution of trypsin, washed twice with PBS, fixed in ice-cold 80% ethanol, and stored overnight at − 20 °C. After centrifugation, the cells were stained with PI/RNase staining buffer (500 µL) at room temperature in the dark for 15 min and analyzed by flow cytometry (Accuri™ C6; Becton Dickinson, USA). The data were analyzed using BD Accuri™ C6 Software Version 1.0.264.21. Cell cycle analysis was performed at least three times.
Annexin V/propidium iodide (PI) binding assay
The FITC Annexin V Apoptosis Detection Kit I (BD Pharmingen, product cat. no. 556,547) was used to detect apoptosis, according to the manufacturer’s recommendations. In short, the cells were seeded onto tissue culture plates and allowed to adhere overnight. After treatment of the cells with compounds for the time indicated at IC80 value, cells were harvested from the plates by incubation with a solution of trypsin and washed twice with cold PBS. Next, the cells were resuspended in staining buffer (100 µL 1× binding buffer, 5 µL FITC Annexin V, and 5 µL propidium iodide (PI)) and incubated at room temperature in the dark for 15 min. The cells were then treated with 300 µL of 1× binding buffer and analyzed by flow cytometry as above. The analysis was performed at least three times and then included in the statistical analysis.
Senescence-associated β-galactosidase activity assay
Determination of cellular senescence required the use of pH 6.0-dependent β-galactosidase expression as a marker. H460, Du-145, and LNCaP cells were seeded at a plate with coverslips for 72 and 144 h of incubation, respectively, and incubated overnight. After treatment with QDgreen, β−CD, QDgreen−β−CD−FA, C− 2028, β −CD(C−2028), QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA for 72 and 144 h of incubation, cells were washed three times with PBS and then Fixative Solution (consisting of 0.2% glutaraldehyde and 2% formaldehyde in PBS) was added for 5 min. The cells were then washed three times with PBS and stained with a Staining Solution containing 1 mg·mL− 1 of X-gal. After incubation for 12–16 h at 37 °C, the cells were washed twice with PBS and observed by light microscope (Olympus BX60, Tokyo, Japan) using the Nomarski interference contrast at 200× magnification. The experiment was performed three times. For each repetition, 3–4 photos were taken and then included in the statistical analysis.
Wound healing migration assay
To analyze cell mobility, H460, and Du-145 cancer cells were seeded in a culture-insert (Ibidi culture-insert 2 well; Ibidi GmbH, Martinsried, Germany) at a density of 3 × 104 cells per well. After allowing the cells to attach overnight, the culture-insert medium was removed and the cells were washed with RPMI or EMEM (for H460 or Du-145, respectively) to remove non-adherent cells. Then, the cells were incubated in a fresh medium containing QDgreen, QDgreen−β−CD−FA, C−2028, QDgreen−C−2028, and QDgreen− β−CD(C−2028)−FA at 0.25 IC80 value in an imaging chamber (cellVivo incubation system; Olympus, Tokyo, Japan) at 37 °C with 5% CO2. Images were captured every 6 h for 72 h under 100× magnification using a fluorescence microscope (IX83 Inverted Microscope; Olympus, Tokyo, Japan) connected to an XC50 digital color camera (Olympus, Tokyo, Japan). The experiment was performed three times. For each repetition, 2–3 photos were taken and then included in the statistical analysis. The percentage of wound closure was quantified with ImageJ software.
Statistical analysis
The data from all experiments were analyzed using the Kruskal−Wallis test for non-parametric data and Dunn’s test for post-hoc analysis. The results were presented as a median with a 95% confidence interval (CI), where a value of p ≤ 0.05 was considered significant. When the results were significant, Dunn’s test for post-hoc analysis was performed to check the influence of conjugation with the C−2028 compound. * p ≤ 0.05; ** p ≤ 0.01; *** p ≤ 0.01, **** p ≤ 0.0001 were considered as significant. The GraphPad Prism 8 (GraphPad Software Inc., USA) was used to perform statistical analysis.
Results and discussion
QDgreen−β−CD(C−2028)−FA nanoconjugate used in this study was synthesized according to the procedure described in the Materials and methods section as well as in the Supplementary information. Fourier-transform infrared (FTIR) spectroscopy and TEM measurements were performed to confirm the introduction of C−2028 into the QDgreen−β−CD−FA conjugate and onto the QDgreen surface. The representative FTIR spectra and TEM images are presented in Figure S6 and Figure S7 in the Supplementary information, respectively. The amount of loaded compound was determined based on UV-vis measurements of the C−2028 solutions before and after its interaction with QDgreen and QDgreen−β−CD−FA nanoconjugates. It was found that the amount of C−2028 was ca. 19.0 mg and 6.16 mg per 1 g of QDgreen and QDgreen−β−CD−FA, respectively. The physical parameters of the synthesized nanoconjugate are presented in Table 1.
Cell cycle analysis
C−2028 alone and its nanoconjugates were evaluated for their antiproliferative activity against three human cancer cell lines: H460, Du-145, and LNCaP, as well as two normal cell lines: MRC-5 and PNT1A. The details were presented in our previous paper [30] and in the Materials and methods section. Confocal images confirmed superior penetration as well as drug delivery in cancer cells treated with nanoconjugates [30, 31]. Therefore, the next step of our study was the biological evaluation of a novel folic acid-targeted receptor quantum dot−β− cyclodextrin carrier for unsymmetrical bisacridine (C−2028) in the treatment of human lung and prostate cancers. First, we evaluated cell cycle progression anomalies. It is known that cell apoptosis and cycle arrest are therapeutic targets for many chemotherapeutics [36, 37]. Many drugs have been shown to induce apoptosis and G2/M phase arrest [38, 39]. The impacts of C−2028 alone and its nanoconjugates (QDgreen−C−2028 and QDgreen−β−CD(C−2028)−FA) on the cell cycle progression of lung and prostate cancer and normal cells were measured by flow cytometry. As shown in Fig. 1 and Table S1 a–e, treatment of cancer cells with the C−2028 alone and its nanoconjugates resulted in a time-dependent increase in the population of hypodiploid cells (sub-G1 fraction), which represents apoptosis. This tendency was much higher in the case of cancer cells compared to normal cells, in which there was no obvious difference in control cells (untreated) and treated with compounds and their nanoconjugates (Table 2). Therefore, studied compounds are more toxic to cancer cells. The highest size of the sub-G1 population was observed in the case of prostate LNCaP cancer cells treated with the C−2028 compound (about 82%). Conjugation of this compound with nanoparticles decreased significantly in this population in the case of cancer cells, especially in LNCaP cells treated with QDgreen−β−CD(C−2028)−FA (82% vs. 57%). This dependence was higher in nanoconjugates with folic acid (QDgreen−β−CD(C−2028)−FA). In turn, the population of the G2/M phase in cells treated with the C−2028 compound remained at a similar level to control cells (untreated), except in LNCaP cells after 72 h of incubation, where the population size significantly decreased (16.2% for control vs. 6.8% for C−2028) and in MRC-5 cells, where the population size increased (17% vs. 23.9%, respectively). Conjugation of the C−2028 with nanoparticles may increase the size of the G2/M population. This tendency was observed mostly in the case of LNCaP and Du-145 cancer cell lines treated with conjugates with folic acid (QDgreen−β−CD(C−2028)−FA). In rest cell lines, especially in normal cell lines, there is no significant difference in the size of G2/M population cells treated with the C−2028 compound and its nanoconjugates. The G1 phase was the highest in all cell lines in the case of untreated cells (control). Treatment of cells with the C−2028 alone and its nanoconjugates resulted in a time-dependent decrease in the population of the G1 phase. This tendency was the highest in the case of cancer LNCaP cell lines. Conjugation of the C−2028 compound with QDs significantly increased the size of this population in the case of H460 cells (43.6% for C−2028 vs. 64.1% for QDgreen−C−2028) and LNCaP (22.6% for C−2028 vs. 37.6% for QDgreen−β−CD(C−2028)−FA). In turn, in normal MRC-5 cells treated with QDgreen−β−CD(C−2028)−FA the size of the G1 phase was lower than in cells treated with C−2028 alone (48.8% vs. 62.6%, respectively). Importantly, nanoparticles alone (QDgreen and QDgreen−β−CD−FA) did not cause any changes in the cell cycle progression of the studied cancer H460, Du-145, and LNCaP cells, as well as normal MRC-5 and PNT1A cells (Fig. 1, Figure S8, and Table S1 a–e). Consequently, they are good carriers for transporting tested compounds.
Cell cycle analysis of H460, Du-145, LNCaP, MRC-5, and PNT1A cells. (A) Representative plots of cells treated with C−2028, QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA. (B) Graphs represent the median of the percentage in the sub-G1, G1, and G2/M phases of the cell cycle in the studied cell lines with a 95% confidence interval (CI), where *p ≤ 0.05; **p ≤ 0.01 indicates statistically significant differences between the studied phases of cells incubated with C−2028 alone and its nanoconjugates. Statistical analysis was performed using the Kruskal–Wallis test for non-parametric data and Dunn’s test as a post-hoc test
Induction of apoptosis
The presence of the sub-G1 population in cancer cell lines treated with the C−2028 compound and its nanoconjugates (Fig. 1) prompted us to evaluate its apoptotic effects studied by flow cytometry. Figure 2A illustrates the dot plots of Annexin-V/propidium iodide staining of apoptotic cells. The C−2028 compound induced time-dependent apoptotic cell death in cancer cell lines, which is the strongest in the case of Du-145 cell lines (69.1%; Fig. 2, Figure S9, and Table S2 a–e). In the case of MRC-5 normal cells treated with C−2028, no obvious difference in the size of the late apoptosis cell population (A+/PI+) was observed (2.5% for control and 5.4% for C−2028). In contrast, in the second normal cell line - PNT1A, this was 4.0% vs. 23.8%, respectively. Conjugation of the C−2028 compound with nanoparticles decreased the late apoptosis cell population of all studied cancer cells (Table 3). This tendency was stronger in the case of QDgreen−C−2028 nanoconjugates (without folic acid in nanoconjugates). Interestingly, in the case of normal cell lines, the biological response was cell-line dependent. In normal human prostatic cell line PNT1A, the conjugation with nanoparticles increased the size of the population of late apoptosis cells (23.8% for C−2028, 44.9% for QDgreen−C−2028, and 50.3% for QDgreen−β−CD(C−2028)−FA). In this cell line, the use of FA in the conjugates increased the number of apoptotic cells in the population. In contrast, in the human fetal lung fibroblast cell line MRC-5, the size of the late apoptosis cells population was lower than 6% irrespective of the form of chemotherapeutic (alone or conjugated) − 5.4%, 4.9%, and 2.3% respectively. What is important, cancer, as well as normal cells treated with nanoparticles alone (QDgreen and QDgreen−β−CD−FA), were viable and not undergoing apoptosis, which is consistent with cell cycle progression studies.
Flow cytometry analysis of phosphatidylserine externalization by Annexin V/propidium iodide (PI) assay in H460, Du-145, LNCaP, MRC-5, and PNT1A cells. (A) Representative plots of the studied cell lines treated with C−2028, QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA after treatment for 24, 72, and 144 h. (B) Graphs represent the median of the percentage of late apoptotic cells (A+/PI+) with a 95% confidence interval (CI). Statistical analysis between the fraction of late apoptotic cells incubated with C−2028 alone and its nanoconjugates was performed using the Kruskal–Wallis test for non-parametric data and Dunn’s test as a post-hoc test. The bottom left quadrant represents live cells (Annexin V negative, PI negative); the bottom right quadrant– early apoptotic cells (Annexin V positive, PI negative); the top right quadrant– late apoptotic cells (Annexin V positive, PI positive); top left quadrant– primary necrotic cells (Annexin V negative, PI positive)
Induction of cellular senescence
The C−2028 compound and its nanoconjugates induced apoptosis in studied cancer cell lines. However, this process concerns only part of the cancer cell population. Therefore, in the next part of our study senescence-associated-β-galactosidase (SA-β-gal) activity and morphological features (flattened cell shape and enlargement with abundant granulation) were evaluated as markers of senescence using bright-field microscopy (Fig. 3 and Figure S10). The typical blue color resulting from the metabolic activity of the SA-β-gal substrate was observed in two cell lines: H460 and LNCaP. In contrast, only a few percent of SA-β-gal positive cells in the population were observed in the Du-145 cancer cell line. In the case of H460 cells, the number of SA-β-gal positive cells was increased following prolonged incubation times (up to 144 h). The results show an increase for SA-β-gal positive cells after treatment with QDgreen−C−2028 (Table 4). Interestingly, the use of FA in this nanoconjugate (QDgreen−β−CD(C−2028)−FA) substantially decreased the senescence process to almost 3% (50.5% for C−2028, 74.2% for QDgreen−C−2028, and 2.7% for QDgreen−β−CD(C−2028)−FA). For LNCaP cells, the SA-β-gal positive cells remained at similar levels after 72 and 144 h of incubation. In this cell line, the number of SA-β-gal positive cells was similar for C−2028 and its nanoconjugates. A slight decrease in the number of senescent cells was detected only in the case of QDgreen−β−CD(C−2028)−FA nanoconjugates. In the prostate Du-145 cell line, only a few SA-β-gal positive cells were detected. The percentage of senescent cells never exceeded 4%. The conjugation of the C−2028 compounds has not changed biological response, however, even in this case the use of FA in nanoconjugates decreased the amount of SA-β-gal positive cells (4.0% for C−2028, 2.6% for QDgreen−C−2028, and 0.6% for QDgreen−β− CD(C−2028)−FA). In all of the studied cell lines treated with nanoconjugate containing folic acid as a linker (QDgreen−β−CD(C−2028)−FA), the reduction of the senescence process was observed, especially in the case of H460 cells (50.1% vs. 2.7% for C−2028 alone and QDgreen−β−CD(C−2028)−FA, respectively). Zhang X. et al. showed FA as a vitamin to oppose telomere dysfunction, as well as the associated senescence phenotype induced by sleep deprivation [40]. Therefore, that can be the reason for the reduced number of senescent cells after treatment with QDgreen−β−CD(C−2028)−FA nanoconjugates. Furthermore, nanoparticles alone (QDgreen, β−CD, and QDgreen−β−CD−FA) did not induce senescence in all of the studied cancer cells after 144 h of incubation, which is consistent with the above results (Figure S10).
Cellular senescence of H460, Du-145, and LNCaP cancer cells following treatment with C−2028, β−CD(C−2028), QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA for the time indicated. Senescence-associated (SA) β-galactosidase (β-gal) activities were assessed by X-gal staining using a light microscope. (A) Representative images of the studied cells. (B) Graphs represent the median of the percentage of SA-β-gal positive cells with a 95% confidence interval (CI), where *p ≤ 0.05; **p ≤ 0.01; ***p ≤ 0.01, ****p ≤ 0.0001 indicate statistically significant differences between the studied phases of cells incubated with C−2028 alone and its nanoconjugates. Statistical analysis was performed using the Kruskal–Wallis test for non-parametric data and Dunn’s test as a post-hoc test. The scale bar is 50 μm
Wound healing migration assay
The next step of our study was to evaluate the anti-migratory potential of the studied nanoconjugates, thus, the wound healing migration assay was performed on H460 and Du-145 cancer cell lines. As shown in Fig. 4, cells treated with nanoplatforms (QDgreen and QDgreen−β−CD−FA) gradually repopulated the wound area in a time-dependent manner in both cancer cell lines. This area was getting smaller slightly faster in the case of cells treated with nanoparticles, compared to the control group. In contrast, the C−2028 compound significantly reduced the migration of cells (Table 5). Conjugation of C−2028 with nanoparticles in prostate Du-145 cancer cells further enhanced this effect, which was stronger in the case of QDgreen−C−2028. This effect was retained during the entire exposure time, with the highest difference during 24–48 h compared to that in the control. In the case of the lung H460 cancer cell line, the weak migratory effect was observed. These cells tended to grow in layers, which was observed mostly in the case of the control group and cells treated with nanoplatforms. However, in the case of the C−2028 compound and its nanoconjugates decrease in the rate of cell migration was observed. It is important to note that the concentrations of all studied compounds were slightly cytotoxic which were 0.25 of IC80 values. This may suggest that the observed anti-migratory properties of C−2028 and its nanoconjugates were not affected by their cytotoxic effect.
Analysis of cell migration by in vitro wound healing migration assay of H460 and Du-145 cancer cells following treatment with QDgreen, QDgreen−β−CD−FA, C−2028, QDgreen−C−2028, and QDgreen−β−CD(C−2028)−FA. (A) Time-lapse microscopy representative images after culture insert removal. (B) Graphs represent the differences between wound area (% of 0 h) cells incubated with C−2028 alone and its nanoconjugates with a 95% confidence interval (CI). Statistical analysis between the fraction of late apoptotic cells incubated with C−2028 alone and its nanoconjugates was performed. The scale bar is 200 μm
Conclusions and future considerations
To conclude, anticancer drug delivery carriers with a controllable drug release have desirable advantages in efficiency, selectivity, safety, tolerance, and side effects. In this study, we presented that the anticancer C−2028 compound alone and its nanoconjugates induced time-dependent apoptosis, mostly in cancer cells. However, the linkage of this compound with nanoplatforms (QDgreen and QDgreen−β−CD−FA) decreased the number of late apoptotic cells in cancer cell lines. In the case of normal cell lines, the biological response was cell-line dependent. The apoptotic cells, after treatment with C−2028 and its nanoconjugates were observed in the PNT1A cell line, in contrast to the MRC-5 cell line. Similar results for normal cell lines were observed in cell cycle studies. The C−2028 compound and its nanoconjugates did not induce apoptosis (sub-G1 population) in the normal MRC-5 cell line, in contrast to the PNT1-A cell line. Unsymmetrical bisacridine and its nanoconjugates induced cellular senescence, depending on the cell line. This process was observed in cancer H460 and LNCaP cell lines in opposition to the Du-145 cancer cell line. Moreover, the senescence process can be also dependent on the composition of nanoconjugates, especially in the case of H460 cancer cells. The strongest effect was observed in cells treated with QDgreen−C−2028 nanoconjugates, while only a few percent of SA-β-gal positive cells after treatment with QDgreen−β−CD(C−2028)−FA nanoconjugates were detected. The wound healing migration assay showed that the C−2028 compound significantly reduced the migration of cells. Conjugation of C−2028 with nanoparticles further enhanced this effect, especially in the case of QDgreen−C−2028 in prostate Du-145 cancer cells. Nanoplatforms alone (QDgreen and QDgreen−β−CD−FA) did not affect the processes of apoptosis and senescence in all of the studied cancer and normal cells. In summary, the described results demonstrate the high potential of a novel folic acid-targeted receptor quantum dot−β−cyclodextrin carrier (QDgreen−β−CD−FA) for drug delivery in cancer treatment.
The results obtained so far will be used to develop further nanoconjugates. In the future, we would like to test different targeting linkers (e.g., transferrin) that would allow for the selective delivery of drugs to cancer cells. We also plan to perform in vivo experiments for QDgreen−β−CD(C−2028)−FA nanoconjugates and new platforms to verify the performance of the proposed drug delivery system in a physiological environment.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- C−2028:
-
9-{N-[(imidazo[4,5,1-de]-acridin-6-on-5-yl)aminopropyl]-N-methylaminopropylamino}-1’-nitroacridine
- FA:
-
Folic acid
- FRs:
-
Folic acid receptors
- FTIR:
-
Fourier-transform infrared spectroscopy
- NPs:
-
Nanoparticles
- QDs:
-
Quantum dots, Ag−In−Zn−S nanocrystals
- QD−β−CD−FA:
-
Quantum dots−β−cyclodextrin−folic acid (nanoplatforms)
- SA-β-gal:
-
Senescence-associated-β-galactosidase
- TEM:
-
Transmission electron microscopy
- TME:
-
Tumor microenvironment
- UA:
-
Unsymmetrical bisacridine
- X-gal:
-
5-Bromo-4-chloro-3-indolyl-β-D-galactosidase
- β−CD:
-
β−Cyclodextrin
References
Sung H, Ferlay C, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2020;71:209–49. https://doi.org/10.3322/caac.21660
Chhikara BS, Parang K. Global cancer statistics 2022: the trends projection analysis. Chem Biol Lett. 2023;10:451.
Arruebo M, Vilaboa N, Sáez-Gutierrez B, Lambea J, Tres A, Valladares M, et al. Assessment of the evolution of cancer treatment therapies. Cancers. 2022;3:3279–330. https://doi.org/10.3390/cancers3033279.
Kamran SC, D’Amico AV. Radiation therapy for prostate cancer. Hematol Oncol Clin North Am. 2020;34:45–69. https://doi.org/10.3322/caac.21250.
Kumar L, Harish P, Malik PS, Khurana S. Chemotherapy and targeted therapy in the management of cervical cancer. Curr Probl Cancer. 2028;42:120–8. https://doi.org/10.1016/j.currproblcancer.2018.01.016.
Debela DT, Muzazu SG, Heraro KD, Ndalama MT, Mesele BW, Haile DC, et al. New approaches and procedures for cancer treatment: current perspectives. SAGE Open Med. 2021;9:1–10. https://doi.org/10.1177/20503121211034366.
Skeel RT, Khleif SN. Handbook of cancer chemotherapy. 8th ed. Philadelphia (PA): Lippincott Williams & Wilkins; 2011.
Narvekar M, Xue HY, Eoh JY, Wong HL. Nanocarrier for poorly water-soluble anticancer drugs-barriers of translation and solutions. AAPS PharmSciTech. 2014;15:822–33. https://doi.org/10.1208/s12249-014-0107-x.
Damle MA, Shetty VG, Jakhade AP, Kaul-Ghanekar R, Chikate RC. Bi-functional nature of nanoceria: pro-drug and drug-carrier potentiality towards receptor-mediated targeting of doxorubicin. New J Chem. 2020;44:17013–26. https://doi.org/10.1039/D0NJ02895A.
Mondal J, Panigrahi AK, Khuda-Bukhsh AR. Conventional chemotherapy: problems and scope for combined therapies with certain herbal products and dietary supplements. Austin J Mol Cell Biol. 2014;1:10.
Senapati S, Mahanta AK, Kumar S, Maiti P. Controlled drug delivery vehicles for cancer treatment and their performance. Signal Transduct Target Ther. 2013;3:7. https://doi.org/10.1038/s41392-017-0004-3.
Yao Y, Zhou Y, Liu L, Xu Y, Chen Q, Wang Y, et al. Nanoparticle-based drug delivery in cancer therapy and its role in overcoming drug resistance. Front Mol Biosci. 2020;7:193. https://doi.org/10.3389/fmolb.2020.00193.
Jin C, Wang K, Oppong-Gyebi A, Hu J. Application of nanotechnology in cancer diagnosis and therapy - a mini-review. Int J Med Sci. 2020;17:2964–73. https://doi.org/10.7150/ijms.49801.
Singh R, Lillard JW Jr. Nanoparticle-based targeted drug delivery. Exp Mol Pathol. 2009;86:215–23. https://doi.org/10.1016/j.yexmp.2008.12.004.
Bahrami B, Hojjat-Farsangi M, Mohammadi H, Anvari E, Ghalamfarsa G, Yousefi M, et al. Nanoparticles and targeted drug delivery in cancer therapy. Immunol Lett. 2017;190:64–83. https://doi.org/10.1016/j.imlet.2017.07.015.
Dadwal A, Baldi A, Kumar Narang R. Nanoparticles as carriers for drug delivery in cancer. Artif Cells Nanomed Biotechnol. 2018;46:295–305. https://doi.org/10.1080/21691401.2018.1457039.
Blanco E, Shen H, Ferrari M. Principles of nanoparticle design for overcoming biological barriers to drug delivery. Nat Biotechnol. 2015;33:941–51. https://doi.org/10.1038/nbt.3330.
Shi J, Kantoff PW, Wooster R, Farokhzad OC. Cancer nanomedicine: progress, challenges and opportunities. Nat Rev Cancer. 2017;17:20–37. https://doi.org/10.1038/nrc.2016.108.
Thomas RG, Surendran SP, Jeong YY. Tumor microenvironment-stimuli responsive nanoparticles for anticancer therapy. Front Mol Biosci. 2020;7:610533. https://doi.org/10.3389/fmolb.2020.610533.
Zhou W, Jia Y, Liu Y, Chen Y, Zhao P. Tumor microenvironment-based stimuli-responsive nanoparticles for controlled release of drugs in cancer therapy. Pharmaceutics. 2022;14:2346. https://doi.org/10.3390/pharmaceutics14112346.
Ruttala HB, Ramasamy T, Madeshwaran T, Hiep TT, Kandasamy U, Oh KT, et al. Emerging potential of stimulus-responsive nanosized anticancer drug delivery systems for systemic applications. Arch Pharm Res. 2018;41:111–29. https://doi.org/10.1007/s12272-017-0995-x.
Low PS, Kularatne SA. Folate-targeted therapeutic and imaging agents for cancer. Curr Opin Chem Biol. 2009;13:256–62. https://doi.org/10.1016/j.cbpa.2009.03.022.
Farokhzad OC, Langer R. Impact of nanotechnology on drug delivery. ACS Nano. 2009;3:16–20. https://doi.org/10.1021/nn900002m.
Liu L, Wei Y, Zhai S, Chen Q, Xing D. Dihydroartemisinin and transferrin dual-dressed nano-graphene oxide for a pH-triggered chemotherapy. Biomaterials. 2015;62:35–46. https://doi.org/10.1016/j.biomaterials.2015.05.036.
Santi M, Maccari G, Mereghetti P, Voliani V, Rocchiccioli S, Ucciferri N, et al. Rational design of a transferrin-binding peptide sequence tailored to targeted nanoparticle internalization. Bioconjug Chem. 2017;28:471–80. https://doi.org/10.1021/acs.bioconjchem.6b00611.
Kübler E, Albrecht H. Large set data mining reveals overexpressed GPCRs in prostate and breast cancer: potential for active targeting with engineered anti-cancer nanomedicines. Oncotarget. 2018;9:24882–97. https://doi.org/10.18632/oncotarget.2542.
Sigismund S, Avanzato D, Lanzetti L. Emerging functions of the EGFR in cancer. Mol Oncol. 2018;12:3–20. https://doi.org/10.1002/1878-0261.1215.
Pilch J, Matysiak-Brynda E, Kowalczyk A, Bujak P, Mazerska Z, Nowicka AM, et al. New unsymmetrical bisacridine derivatives noncovalently attached to quaternary quantum d.ots improve cancer therapy by enhancing cytotoxicity toward cancer cells and protecting normal cells. ACS Appl Mater Interfaces. 2020;12:17276–89. https://doi.org/10.1021/acsami.0c02621.
Pilch J, Kowalik P, Bujak P, Nowicka AM, Augustin E. Quantum dots as a good carriers of unsymmetrical bisacridines for modulating cellular uptake and the biological response in lung and colon cancer cells. Nanomaterials. 2021;11:462. https://doi.org/10.3390/nano11020462.
Pilch J, Kowalik P, Kowalczyk A, Bujak P, Kasprzak A, Paluszkiewicz E, et al. Foliate-targeting quantum dots-cyclodextrin nanocarrier for efficient delivery of unsymmetrical bisacridines to lung and prostate cancer cells. Int J Mol Sci. 2022;23:1261. https://doi.org/10.3390/ijms2303126.
Pilch J, Potęga A, Kowalczyk A, Kasprzak A, Kowalik P, Bujak P, et al. pH-responsive drug delivery nanoplatforms as smart carriers of unsymmetrical bisacridines for targeted cancer therapy. Pharmaceutics. 2023;15:201. https://doi.org/10.3390/pharmaceutics15010201.
Probst CE, Zrazhevskiy P, Bagalkot V, Gao X. Quantum dots as a platform for nanoparticle drug delivery vehicle design. Adv Drug Deliv Rev. 2013;65:703–18. https://doi.org/10.1016/j.addr.2012.09.036.
Zhao MX, Zhu BJ. The research and applications of quantum dots as nano-carriers for targeted drug delivery and cancer therapy. Nanoscale Res Lett. 2016;11:207. https://doi.org/10.1186/s11671-016-1394-9.
Xing C, Zheng X, Deng T, Zeng L, Liu X, Chi X. The role of cyclodextrin in the construction of nanoplatforms: from structure, function and application perspectives. Pharmaceutics. 2023;15:1536. https://doi.org/10.3390/pharmaceutics15051536.
Paluszkiewicz E, Horowska B, Borowa-Mazgaj B, Peszyńska-Sularz G, Paradziej-Łukowicz J, Augustin E, et al. Design, synthesis and high antitumor potential of new unsymmetrical bisacridine derivatives towards human solid tumors, specifically pancreatic cancers and their unique ability to stabilize DNA G quadruplexes. Eur J Med Chem. 2020;204:112599. https://doi.org/10.1016/j.ejmech.2020.112599.
Pfeffer CM, Singh ATK. Apoptosis: a target for anticancer therapy. Int J Mol Sci. 2018;19:448. https://doi.org/10.3390/ijms19020448.
Evan GI, Vousden KH. Proliferation, cell cycle and apoptosis in cancer. Nature. 2001;411:342–8. https://doi.org/10.1038/35077213.
Skwarska A, Augustin E, Konopa. Sequential induction of mitotic catastrophe followed by apoptosis in human leukemia MOLT4 cells by imidazoacridinone C-1311. Apoptosis. 2007;12:2245–57. https://doi.org/10.1007/s10495-007-0144-y.
Skwarska A, Augustin E, Beffinger M, Wojtczyk A, Konicz S, Laskowska K, et al. Targeting of FLT3-ITD kinase contributes to high selectivity of imidazoacridinone C-1311 against FLT3-activated leukemia cells. Biochem Pharmacol. 2015;95:238–52. https://doi.org/10.1016/j.bcp.2015.04.006.
Zhang X, Wang Y, Zhao R, Hu X, Zhang B, Lv X, et al. Folic acid supplementation suppresses sleep deprivation-induced telomere dysfunction and senescence-associated secretory phenotype (SASP). Oxid Med Cell Longev. 2019;4569614. https://doi.org/10.1155/2019/4569614.
Acknowledgements
We would like to acknowledge Prof. Jędrzej Antosiewicz from the Medical University of Gdańsk (Gdańsk, Poland) for providing the PNT1A cell line. We also thank Dr. Ewa Augustin from Gdańsk University of Technology (Gdańsk, Poland) for the possibility of performing experiments in the laboratory.
Funding
This research was funded by the Polish National Science Center, Grant no. 2020/37/N/NZ7/01979.
Author information
Authors and Affiliations
Contributions
Joanna Pilch - original draft, review, and editing of the manuscript, project administration, funding acquisition, resources, conceptualization, methodology, investigation, data curation, formal analysis, and supervision. Agnieszka Potęga - original draft, review, and editing of the manuscript, methodology, and investigation. Patrycja Kowalik - review and editing of the manuscript. Agata Kowalczyk - review and editing of the manuscript, methodology, and investigation. Piotr Bujak - review and editing of the manuscript, and methodology. Artur Kasprzyk - methodology. Ewa Paluszkiewicz - methodology. Anna M. Nowicka - review and editing of the manuscript, methodology, investigation, and supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pilch, J., Potęga, A., Kowalik, P. et al. In vitro biological evaluation of a novel folic acid-targeted receptor quantum dot−β−cyclodextrin carrier for C−2028 unsymmetrical bisacridine in the treatment of human lung and prostate cancers. Pharmacol. Rep (2024). https://doi.org/10.1007/s43440-024-00606-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43440-024-00606-4