Abstract
Purpose
To radiographically evaluate if vertebral body tethering (VBT) can maintain differential peri-apical vertebral growth at medium-term follow-up of 4 years.
Methods
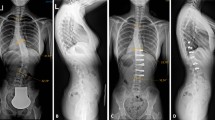
A prospective, international, multicenter database was queried to identify idiopathic scoliosis patients treated with thoracic VBT. Concave vs. convex vertebral body height, vertebral wedging, and disc wedging of the 3 peri-apical vertebrae were measured by two independent observers at 5 timepoints (pre-operative to 4-year follow-up).
Results
65 skeletally immature patients (60 female, mean 12.8 years old, 21 with open triradiate cartilages) met inclusion criteria. Mean pre-operative maximum scoliosis of 50 ± 8° decreased significantly post-operatively to 27 ± 9° (p < 0.001), which remained stable at 4-year follow-up 30 ± 17° (p = 0.38 vs. post-operative). Mean instrumented scoliosis was 21 ± 14° at 4-year follow-up, which was significantly different than 4-year maximum scoliosis (p < 0.001). Mean pre-operative kyphosis of 30 ± 12° did not significantly change post-operatively (p = 1.0) and remained stable at 4-year follow-up (35 ± 18°; p = 0.05).
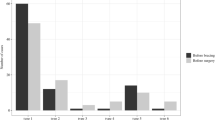
Mean individual convex vertebral height increased from 17.7 ± 1.9 mm to 19.8 ± 1.5 mm (p < 0.001), while mean individual concave height increased from 14.8 ± 1.9 mm to 17.6 ± 1.6 mm (p < 0.001). Summing the peri-apical heights, the difference in height from pre-operative to 4-year follow-up was greater on the concave (8.3 ± 4.7 mm) than on the convex side (6.2 ± 4.7 mm) (p < 0.001). Mean individual vertebral wedging decreased from 6 ± 2° at pre-operative to 4 ± 2° at 4-year follow-up (p < 0.001). Mean total vertebral and disc wedging started at 29 ± 7° pre-operatively, decreased to 16 ± 6° at post-operative (p < 0.001), then further decreased to 14 ± 8° at 4-year follow-up (p < 0.001). Patients with open triradiate cartilages at the time of surgery had a larger height change over the 4 years compared to those with closed triradiate cartilages (p < 0.001).
Conclusion
Patients with idiopathic scoliosis treated with VBT demonstrated differential vertebral growth which was maintained at minimum 4-year follow-up. This effect was more pronounced in patients whose triradiate cartilages were open at the time of surgery.
Level of Evidence
III.






Similar content being viewed by others
Data availability
Registry data are available to member institutions. Measurements and analysis done at the IWK Health Centre are on a password protected server. Access may be arranged through application to the REB.
Code availability
Statistical analysis was conducted using Excel version 2002 (Microsoft Corporation, Redmond, Washington, USA) and SPSS version 27.0 (IBM Corp, Armonk, NY, USA).
References
El-Hawary R, Chukwunyerenwa C (2014) Update on evaluation and treatment of scoliosis. Pediatr Clin N Am 61(6):1223–1241. https://doi.org/10.1016/j.pcl.2014.08.007
Hoernschemeyer DG, Boeyer ME, Robertson ME et al (2020) Anterior vertebral body tethering for adolescent scoliosis with growth remaining: a retrospective review of 2 to 5-year postoperative results. J Bone Joint Surg Am 102(13):1169–1176. https://doi.org/10.2106/JBJS.19.00980
Parent S, Shen J (2020) Anterior vertebral body growth-modulation tethering in idiopathic scoliosis: surgical technique. J Am Acad Orthop Surg 28(17):693–699. https://doi.org/10.5435/JAAOS-D-19-00849
Kepler C, Meredith D, Green D, Widmann R (2012) Long-term outcomes after posterior spine fusion for adolescent idiopathic scoliosis. Curr Opin Pediatr 24(1):68–75. https://doi.org/10.1097/MOP.0b013e32834ec982
Pehlivanoglu T, Oltulu I, Erdag Y et al (2021) Comparison of clinical and functional outcomes of vertebral body tethering to posterior spinal fusion in patients with adolescent idiopathic scoliosis and evaluation of quality of life: preliminary results. Spine Deform 9:1175–1182. https://doi.org/10.1007/s43390-021-00323-5
Crawford CH 3rd, Lenke LG (2010) Growth modulation by means of anterior tethering resulting in progressive correction of juvenile idiopathic scoliosis: a case report. J Bone Joint Surg Am 92(1):202–209. https://doi.org/10.2106/JBJS.H.01728
Miyanji F, Pawelek J, Nasto LA, Rushton P, Simmonds A, Parent S (2020) Safety and efficacy of anterior vertebral body tethering in the treatment of idiopathic scoliosis. J Bone Joint Surg Br 102-B(12):1703–1708. https://doi.org/10.1302/0301-620X.102B12.BJJ-2020-0426.R1
Newton PO, Takahashi Y, Yang Y et al (2022) Anterior vertebral body tethering for thoracic idiopathic scoliosis leads to asymmetric growth of the periapical vertebrae. Spine Deform 10(3):553–561. https://doi.org/10.1007/s43390-021-00464-7
McDonald T, Shah S, Hargiss J et al (2022) When successful, anterior vertebral body tethering (VBT) induces differential segmental growth of vertebrae: an in vivo study of 51 patients and 764 vertebrae. Spine Deform 10(4):791–797. https://doi.org/10.1007/s43390-022-00471-2
Shin M, Arguelles GR, Cahill PJ, Flynn JM, Baldwin KD, Anari JB (2021) Complications, reoperations, and mid-term outcomes following anterior vertebral body tethering versus posterior spinal fusion: a meta-analysis. JB JS Open Access. https://doi.org/10.2106/JBJS.OA.21.00002
Zhu F, Qiu X, Liu S, Man CheeCheung K (2022) Minimum 3-year experience with vertebral body tethering for treating scoliosis: a systematic review and single-arm meta-analysis. J Orthop Surg (Hong Kong). https://doi.org/10.1177/10225536221137753
Raitio A, Syvänen J, Helenius I (2022) Vertebral body tethering: indications, surgical technique, and a systematic review of published results. J Clin Med 11(9):2576. https://doi.org/10.3390/jcm11092576
Bizzoca D, Piazzolla A, Moretti L, Vicenti G, Moretti B, Solarino G (2022) Anterior vertebral body tethering for idiopathic scoliosis in growing children: a systematic review. World J Orthop 13(5):481–493. https://doi.org/10.5312/wjo.v13.i5.481
Labrom FR, Izatt MT, Contractor P et al (2020) Sequential MRI reveals vertebral body wedging significantly contributes to coronal plane deformity progression in adolescent idiopathic scoliosis during growth. Spine Deform 8(5):901–910. https://doi.org/10.1007/s43390-020-00138-w
Newton PO (2020) Spinal growth tethering: indications and limits. Ann Transl Med 8(2):27. https://doi.org/10.21037/atm.2019.12.159
Manring M, Calhoun J (2010) Joseph C. Risser Sr., 1892–1982. Clin Orthop Relat Res 468(3):643–645
Sanders JO, Khoury JG, Kishan S et al (2008) Predicting scoliosis progression from skeletal maturity: a simplified classification during adolescence. J Bone Joint Surg Am 90(3):540–553. https://doi.org/10.2106/JBJS.G.00004
Photopoulos G, Hurry J, Murphy J et al (2022) Reliability of radiographic assessment of growth modulation from anterior vertebral body tethering surgery in pediatric scoliosis. Spine Deform. https://doi.org/10.1007/s43390-022-00570-0
Villemure I, Aubin CE, Dansereau J, Labelle H (2002) Simulation of progressive deformities in adolescent idiopathic scoliosis using a biomechanical model integrating vertebral growth modulation. J Biomech Eng 124(6):784–790. https://doi.org/10.1115/1.1516198
Floman Y, El-Hawary R, Lonner BS, Betz RR, Arnin U (2021) Vertebral growth modulation by posterior dynamic deformity correction device in skeletally immature patients with moderate adolescent idiopathic scoliosis. Spine Deform 9(1):149–153. https://doi.org/10.1007/s43390-020-00189-z
Welborn MC, Coghlan R, Sienko S, Horton W (2021) Correlation of collagen X biomarker (CXM) with peak height velocity and radiographic measures of growth in idiopathic scoliosis. Spine Deform 9(3):645–653. https://doi.org/10.1007/s43390-020-00262-7
von Elm E, Altman DG, Egger M et al (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61(4):344–349. https://doi.org/10.1016/j.jclinepi.2007.11.008
Newton PO, Parent S, Miyanji F, Alanay A, Lonner BS, Neal KM, Hoernschemeyer DG, Yaszay B, Blakemore LC, Shah SA, Bastrom TP, Harms Study Group (2022) Anterior vertebral body tethering compared with posterior spinal fusion for major thoracic curves: a retrospective comparison by the Harms Study Group. J Bone Joint Surg Am 104(24):2170–2177. https://doi.org/10.2106/JBJS.22.00127. (Epub 2022 Oct 20. PMID: 37010479)
Farivar D, Parent S, Miyanji F, Heffernan MJ, El-Hawary R, Larson AN, Andras LM, Skaggs DL, Pediatric Spine Study Group (2023) Concave and convex growth do not differ over tethered vertebral segments, even with open tri-radiate cartilage. Spine Deform 11(4):881–886. https://doi.org/10.1007/s43390-023-00683-0. (Epub 2023 Apr 1. PMID: 37004694; PMCID: PMC10261211)
Murray E, Tung R, Sherman A, Schwend RM (2020) Continued vertebral body growth in patients with juvenile idiopathic scoliosis following vertebral body stapling. Spine Deform 8(2):221–226. https://doi.org/10.1007/s43390-019-00019-x. (Epub 2020 Feb 5 PMID: 32026438)
Acknowledgements
The authors acknowledge the contribution of the Pediatric Spine Study Group.
Funding
Funding was received for this study from the Dalhousie Medical Research Foundation W. Alan Curry Studentship and Dalhousie Faculty of Medicine Gladys Osman Estate.
Author information
Authors and Affiliations
Consortia
Contributions
Design or the acquisition, analysis, or interpretation of data, Drafted the work or revised it critically, Approved, Accountable: Gregory Photopoulos, Jennifer Hurry, Ankita Bansal, Firoz Miyanji, Stefan Parent, Joshua Murphy, Pediatric Spine Study Group, Ron El-Hawary.
Corresponding author
Ethics declarations
Conflict of interest
-
1.
Gregory Photopoulos—received two studentships from Dalhousie University during the conduct of the study.
-
2.
Jennifer Hurry—reports a fellowship from Depuy Synthes Spine outside the submitted work.
-
3.
Ankita Bansal—nothing to disclose.
-
4.
Firoz Miyanji—DePuy, A Johnson & Johnson Company: paid consultant; research support. OrthoPediatrics: paid consultant. Pediatric Orthopaedic Society of North America: board or committee member. Stryker: paid consultant. Zimmer: IP royalties; paid consultant. All disclosures are outside the submitted work.
-
5.
Stefan Parent—EOS-imaging: paid consultant, research grant, Royalties. K2M: paid consultant. DePuy Synthes Spine: paid consultant, research grant, fellowship support. Spinologics/Spino-Modulation: stock/shareholder, employee. Academic Research chair in spine deformities of the CHU Sainte-Justine (DePuy): endowment. Pediatric Orthopaedic Society of North America: research grant. Scoliosis Research Society: research grant. Canadian Foundation for Innovation: research grant. Setting Scoliosis Straight Foundation: research grant. Natural Sciences and Engineering Council of Canada: research grant. Fonds de recherche Québec—Santé: research grant, committee member. Orthopaedic Research and Education Foundation: research grant. Medtronic: research grant. OrthoPediatrics: speaker’s bureau. All disclosures are outside the submitted work.
-
6.
Joshua Murphy—reports personal fees from Depuy Synthes Spine, personal fees from OrthoPediatrics, personal fees from Alphatec Spine, outside the submitted work.
-
7.
Pediatric Spine Study Group—reports grants from DePuy Synthes Spine, grants from Medtronic, grants from NuVasive, grants from Globus Medical Inc., grants from OrthoPediatrics, grants from Zimmer Biomet, grants from Pediatric Spine Foundation, grants from Stryker. All disclosures are outside the submitted work.
-
8.
Ron El-Hawary—reports personal fees from Depuy Synthes Spine, personal fees from Medtronic Spine, grants from Depuy Synthes Spine, grants from Medtronic Spine, personal fees from OrthoPediatrics, other from Pediatric Spine Foundation, other from Scoliosis Research Society. All disclosures are outside the submitted work.
Ethical approval
This work is a sub-study of the Pediatric Spine Study Group Registry which was approved by the Research Ethics Board at the IWK Health Centre (#1002256) in accordance with the ethical standards outlined in the Tri-Council Policy Statement and the 1964 Declaration of Helsinki and its later amendments.
Consent to participate
All research participants or their legal guardians provided written consent to be a part of the registry and have the data collected be used in ongoing research on scoliosis.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Photopoulos, G., Hurry, J., Bansal, A. et al. Differential vertebral body growth is maintained after vertebral body tethering surgery for idiopathic scoliosis: 4-year follow-up on 888 peri-apical vertebrae and 592 intervertebral discs. Spine Deform (2024). https://doi.org/10.1007/s43390-024-00874-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s43390-024-00874-3