Abstract
Background
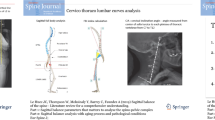
Scoliosis causes abnormal spinal curvature and torsional rotation of the vertebrae and has implications for human suffering and societal cost. In differential geometry, Writhe describes three-dimensional curvature. Differential geometric quantities can inform better diagnostic metrics of scoliotic deformity. This evaluation could help physicians and researchers study scoliosis and determine treatments.
Methods
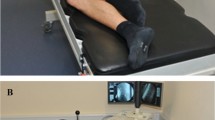
Eight adult lumbar spine CT scans were analyzed in custom MATLAB programs to estimate Writhe and Cobb angle. Five patients exhibited scoliotic curvature, and three controls were asymptomatic. Vertebral centroids in three-dimensional space were determined, and Writhe was approximated. A T-test determined whether the affected spines had greater Writhe than the controls. Cohen’s D test was used to determine effect size.
Results
Writhe of scoliotic spines (5.4E-4 ± 2.7E-4) was significantly higher than non-scoliotic spines (8.2E-5 ± 1.1E-4; p = 0.008).
Conclusion
Writhe, a measure of curvature derived from 3D imaging, is significantly greater in scoliotic than in non-scoliotic spines. Future directions must include more subjects and examine writhe as a marker of scoliosis severity, progression, and response to treatment.



Similar content being viewed by others
Data availability
The data and custom MATLAB scripts used to segment vertebrae, determine the spine centerline, and evaluate Writheare available upon reasonable request to the corresponding author.
References
Levitt M (1983) Protein folding by restrained energy minimization and molecular dynamics. J Mol Biol 170(3):723–764
Dennis MR, Hannay JH (2005) Geometry of Călugăreanu’s theorem. Proceedings: Math Phys Eng 461(2062):3245–3254
Gstoettner M, Sekyra K, Walochnik N et al (2007) Inter- and intraobserver reliability assessment of the Cobb angle: manual versus digital measurement tools. Eur Spine J 16(10):1587–1592
Klenin K, Langowski J (2000) Computation of writhe in modeling of supercoiled DNA. Biopolymers: Original Res Biomol. 54(5):307–317
Lenke LG, Betz RR, Harms J et al (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg 83(8):1169–1181
Pasha S, Cahill PJ, Dormans JP et al (2016) Characterizing the differences between the 2D and 3D measurements of spine in adolescent idiopathic scoliosis. Eur Spine J 25(10):3137–3145
Pasha S, Aubin C-E, Sangole A et al (2014) Three-dimensional spinopelvic relative alignment in adolescent idiopathic scoliosis. Spine 39(7):564–570
Schwab F, Farcy J-P, Bridwell K et al (2006) A clinical impact classification of scoliosis in the adult. Spine 31(18):2109–2114
Kadoury S, Shen J, Parent S (2014) Global geometric torsion estimation in adolescent idiopathic scoliosis. Med Biol Eng Compu 52(4):309–319
Shakil H, Iqbal ZA, Al-Ghadir AH (2014) Scoliosis: review of types of curves, etiological theories and conservative treatment. J Back Musculoskelet Rehabil 27(2):111–115
Poncet P, Dansereau J, Labelle H (2001) Geometric torsion in idiopathic scoliosis: three-dimensional analysis and proposal for a new classification. Spine 26(20):2235–2243
Tribus CB (2003) Degenerative lumbar scoliosis: evaluation and management. J Am Acad Orthop Surg 11(3):174–183
Weber MH, Mathew JE, Takemoto SK et al (2014) Postoperative recovery outcomes in adult scoliosis: a prospective multicenter database with 5-year follow-up. Spine Deformity 2(3):226–232
Sabou S, Carrasco R, Verma R et al (2019) The clinical and radiological outcomes of multilevel posterior lumbar interbody fusion in the treatment of degenerative scoliosis: a consecutive case series with minimum 2 years follow up. J Spine Surg 5(4):520–528
Addai D, Zarkos J, Bowey AJ (2020) Current concepts in the diagnosis and management of adolescent idiopathic scoliosis. Childs Nerv Syst. https://doi.org/10.1007/s00381-020-04608-4
Pasha S, Baldwin K (2019) Surgical outcome differences between the 3D subtypes of right thoracic adolescent idiopathic scoliosis. Eur Spine J. https://doi.org/10.1007/s00586-019-06145-4
Acknowledgements
The National Institutes of Health, the Catherine D. Sharpe Foundation, the Kevin and Bernadette McKenna Family Research Fund, and the EpiLog Project.
Funding
Funding for this work was received from the National Institutes of Health (R01AR071975), the Catherine D. Sharpe Foundation, and the Kevin and Bernadette McKenna Family Research Fund.
Author information
Authors and Affiliations
Contributions
TA: Design, conception, data collection, analysis, figure and table creation, writing-original draft preparation, writing-critical revision, approval of final version, and accountable for work. RSG: Data analysis, figure and table creation, writing-original draft preparation, writing-critical revision, approval of final version, and accountable for work. AJB: Data analysis, figure and table creation, writing-original draft preparation, writing-critical revision, approval of final version, and accountable for work. GG: Data analysis, figure and table creation, writing-original draft preparation, writing-critical revision, approval of final version and accountable for work. LS: Data collection and analysis, writing- critical revision, approval of final version, and accountable for work. SP: Conception, data analysis, writing—critical revision, approval of final version, and accountable for work. DT: Design, conception, writing-critical revision, approval of final version, and accountable for work. NRM: Design, conception, data collection and analysis, writing–original draft preparation, writing – critical revision, approval of final version, and accountable for work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no personal or institutional interest with regards to the authorship and/or publication of this manuscript. The manuscript submitted does not contain information about medical devices/drugs.
Ethical approval
This study was approved by the IRB at the Hospital of the University of Pennsylvania. IRB number for this study is: 830260. A waiver of informed consent was granted by the University of Pennsylvania IRB as this study was considered to be minimal risk to patients. All ethical guidelines and rules were followed to protect patient privacy.
Consent to participate
A waiver of informed consent was granted by the University of Pennsylvania IRB as this study was considered to be minimal risk to patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arginteanu, T., Gallagher, R.S., Borja, A.J. et al. Quantifying a novel three-dimensional marker of scoliosis. Spine Deform 12, 231–237 (2024). https://doi.org/10.1007/s43390-023-00752-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-023-00752-4