Abstract
Purpose
While the C-EOS system helps organize and classify Early Onset Scoliosis (EOS) pathology, it is not data-driven and does not help achieve consensus for surgical treatment. The current study aims to create an automated method to cluster EOS patients based on pre-operative clinical indices.
Methods
A total of 1114 EOS patients were used for the study, with the following distribution by etiology: congenital (240), idiopathic (217), neuromuscular (417), syndromic (240). Pre-operative clinical indices used for clustering were age, major curve (Cobb) angle, kyphosis, number of levels involved in a major curve (Cobb angle) and kyphosis along with deformity index (defined as the ratio of major Cobb angle and kyphosis). Fuzzy C-means clustering was performed for each etiology individually, with one-way ANOVA performed to assess statistical significance (p < 0.05).
Results
The automated clustering method resulted in three clusters per etiology as the optimal number based on the highest average membership values. Statistical analyses showed that the clusters were significantly different for all the clinical indices within and between etiologies. Link to the ACT-EOS web application: https://biomed.drexel.edu/labs/obl/toolkits/act-eos-application.
Conclusion
An automated method to cluster EOS patients based on pre-operative clinical indices was developed identifying three unique, data-driven subgroups for each C-EOS etiology category. Adoption of such an automated clustering framework can help improve the standardization of clinical decision-making for EOS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Early onset scoliosis (EOS) is a progressive spine deformity defined by an onset of spinal curvature greater than 10 degrees in children under 10 years of age [1, 2]. EOS is believed to account for nearly 10% of all pediatric scoliosis cases, with the true prevalence unknown [3, 4]. While EOS encompasses different etiologies with a variable natural history, the resulting progressive spine and rib cage deformity that can very likely lead to thoracic insufficiency syndrome which is characterized by reduced lung development and growth [4,5,6,7]. To help better understand clinical presentations in the heterogeneous EOS patient population, the Classification of EOS (C-EOS) was developed by an expert committee of spine surgeons to group patients using pre-operative clinical indices such as age, etiology (congenital, idiopathic, neuromuscular, syndromic), major curve (Cobb) angle (< 20°, 20–50°, > 50- < 90°, > 90°) and kyphosis (< 20°, 20–50°, > 50°) [8]. The C-EOS system helps assign a patient to 1 of 48 subgroups based on the aforementioned clinical indices. In 12 of these subgroups, patients have < 20° of major curve (Cobb) angle group and rarely need surgical intervention due to the low extent of the deformity.
C-EOS is the only available classification system to group EOS patients based on the pre-operative clinical indices. While the system is both reliable and accurate, the cut-offs for major curve (Cobb) angle and kyphosis are not based on a data-driven approach [9]. In addition, the 48 subgroups in C-EOS limit meaningful analysis due to a small number of patients in each subgroup, thereby making it difficult to correlate interventions with outcomes [10]. While C-EOS has helped establish a standardized method to communicate different aspects of EOS deformity, it is not widely used like the Lenke classification system for Adolescent Idiopathic Scoliosis (AIS) to help guide surgical treatment [11, 12].
Currently, there is limited consensus among surgeons on treatment selection with variations in the timing of surgery, selection of treatment modality, and levels involved in the instrumentation [13,14,15,16]. Management decisions are guided more by a clinician’s experience and training, complicating outcome comparisons between institutions. This is in part due to C-EOS system not providing guidance on treatment decision-making. Clustering methods have been used to detect clinically relevant curve patterns for the AIS population using pre-operative clinical indices and a few studies have even used a data-driven approach to cluster such patients [17,18,19,20,21]. Such automated clustering methods and analysis have yet to be attempted for EOS.
Due to the need for data-driven grouping of the heterogenous EOS patient population, the objective of this study is to use machine learning-based clustering methods to generate a limited number of automated, meaningful subgroups based on pre-operative clinical indices of EOS patients. Such a framework can be used along with the existing C-EOS system as the foundation to build a novel automated classification system informed by patient data to provide standardized guidance for surgical interventions for EOS.
Methods
Patient data
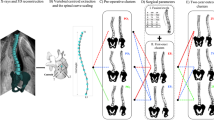
After institutional review board approval, EOS patients were retrospectively selected from the prospectively maintained database of the Pediatric Spine Study Group (PSSG) over a 20-year period (1995–2015). For all subjects, pre-operative PA, and lateral radiographs along with measurement of pre-operative clinical indices were obtained. For patients with multiple clinical visits, only the clinical indices from the first visit were considered. Subjects with missing clinical indices were excluded, which resulted in a total of 1170 subjects (congenital (n = 259), idiopathic (n = 224), neuromuscular (n = 440), and syndromic (n = 247)) being included for the automated clustering analyses.
Clinical indices measurement and automated clustering method
Pre-operative clinical indices used for clustering were age, major curve (Cobb) angle, kyphosis, number of levels involved in a major curve (Cobb angle) and kyphosis along with deformity index (defined as the ratio of major Cobb angle and kyphosis.
Fuzzy C-means clustering algorithm is an automated method to group data into a specific number of clusters provided by the user. The algorithm works by initially finding cluster centroids based on the data, after which every datapoint is assigned a membership value that denotes how close it is to the cluster centroid. Based on these membership values, datapoints are clustered together [22]. In the current study, a Fuzzy C-means clustering algorithm was used to cluster EOS patients for each etiology based on age, major curve (Cobb) angle, kyphosis, number of levels involved in the major curve, number of levels involved in kyphosis and deformity index. Hence, four cluster analyses were performed for each of the four EOS etiologies namely congenital, idiopathic, neuromuscular, and syndromic. One of the advantages of the fuzzy c-means clustering algorithm is that it considers the heterogeneity of the dataset and is able to identify outliers using the membership values.
For this study, the optimal number of clusters for each etiology was decided based on the average membership values of the clusters. Different number of clusters were used to perform the clustering analysis, and the one that resulted in the highest average membership value was selected as the optimal number.
Clustering evaluation metric
The membership values calculated during the fuzzy C-means analyses describe how close a datapoint is to the calculated cluster centroid, hence offering the basis to detect outliers. These membership values help quantify the certainty (i.e. accuracy) of a data point belonging to a particular cluster. Since these values provide accuracy on a data point and its cluster center, these can also be used a metric to determine outliers by defining a lower bound. For the current study, a membership value of 0.6 was used as the lower bound with values below this deemed as outliers. Hence, subjects who had clinical indices with membership values lower than 0.6 were considered as not belonging to a cluster and were excluded from the clustering analyses.
Statistical analysis
MATLAB (v2020b, The MathWorks Inc, Natick, MA) was used to perform statistical analyses. Average and standard deviation values for each cluster within an etiology were computed and compared with each other using a one-way ANOVA (< 0.01), to detect differences between the clusters. Furthermore, Tukey’s post-hoc analysis was performed to detect differences between the clusters of all the etiologies.
Results
For fuzzy-C-means, based on the average membership values, three clusters per etiology resulted in the highest membership values. Out of 1170 eligible subjects, a total of 56 subjects (congenital (n = 19 out of 259), idiopathic (n = 7 out of 224), neuromuscular (n = 23 out of 440), and syndromic (n = 7 out of 247)) were excluded from the analyses due to their low membership values (i.e. < 0.6), resulting in a total of 1114 subjects being included for the final analyses.
Tables 1, 2, 3, 4 show the average and standard deviation values of clinical indices for each etiology along with exemplar radiographic images. In each table, clusters 1–3 are arranged in ascending order of average magnitude of major curve (Cobb) angle. To best visualize the clusters, scatter plots of kyphosis versus major curve (Cobb) for each etiology are shown in Figs. 1, 2, 3, 4, respectively. For each etiology, one-way ANOVA showed that the clinical indices for any cluster were significantly different (p < 0.01) from other clusters. Link to the ACT-EOS web application: https://biomed.drexel.edu/labs/obl/toolkits/act-eos-application.
Discussion
This is the first study to perform automated fuzzy C-means clustering of EOS subjects based on pre-operative clinical indices, complementing the existing C-EOS classification system. While the C-EOS system uses Cobb angle and kyphosis, which were based on expert review informed by normative values derived from the literature, the current clustering method uses a data-driven approach, by using the highest average membership values to determine subject assignments to respective clusters, to create the subgroups. The smaller number (3) of subgroups per etiology generated by this clustering analysis could better focus research initiatives for the rare and heterogenous population of EOS patients to improve and standardize clinical decision-making. In contrast, as shown in Tables 1, 2, 3, 4, subjects in each cluster would be classified under multiple C-EOS groups which would not be conducive to clinical decision making [23]. This is supported by previous studies that have reported limitations of large EOS subgroups to aid in clinical outcome determination [10].
In this study, we identified unique clusters within each EOS etiology that were significantly different from each other based on all the clinical indices. Although one cluster in the idiopathic and congenital groups, respectively, had severe kyphotic deformities, these clusters still had a deformity index greater than one (i.e. greater major curve Cobb angle as compared to kyphosis). In contrast, both neuromuscular and syndromic groups had one cluster each with a deformity index less than one indicative of greater kyphosis as compared to the major curve Cobb angle. Although further validation is required for these methods to be widely adopted, the novel preliminary findings reported in the current study may point to differences in general deformity patterns observed between EOS etiologies, which are not immediately discernible with the C-EOS system. Additionally, while post-hoc testing showed significant differences across all clusters for all etiologies, we may not fully capture the heterogeneity as these are solely based on radiographic measurements.
Limited previous studies for automated clustering of patients with spine deformity have used techniques such as ISOData and K-means + + [20, 24]. While these methods were able to create clusters based on patient deformity characteristics, they do not provide a quantitative basis to assign a patient to a particular cluster, and also lack the ability to assess whether or not a patient is an outlier. On the other hand, Fuzzy C-means, which is an automated unsupervised clustering algorithm that performs well on heterogenous datasets, uses membership values to provide a probabilistic estimate of a patient belonging to a particular cluster. Higher membership values (> 0.6) would indicate a greater probability of a patient’s assignment to a cluster, and thereby also help identify and exclude any outliers.
The current study is not without limitations. First, to better address the heterogeneity of EOS subjects, the current clustering method can be further improved. For example, a small number of subjects (n = 56 out of 1170), were excluded in any cluster due to low membership values (i.e. < 0.6) of the limited radiographic measurements. Inclusion of additional structural (such as thoracic deformity parameters), functional (such as pulmonary functional parameters) and time-based measures (Annual Progression Modifier (APM)) may help better address the variable presentations of EOS deformity. Secondly, we used a multi-institutional and multi-modal dataset with clinical indices measured made by multiple observers. Variations associated with such datasets would impact any classification method equally. However, the fuzzy C-means algorithm would be less affected by such variations due to the automated selection that is unbiased by preset cut-offs for clinical indices.
Conclusion
An automated framework to cluster EOS patients based on pre-operative clinical indices was developed identifying three unique, data-driven subgroups for each C-EOS etiology category. Adoption of this clustering framework with further validation may assist with clinical applications such as surgical planning, optimization of intervention type and timing to improve clinical outcomes and reduce complications.
Link to the ACT-EOS web application: https://biomed.drexel.edu/labs/obl/toolkits/act-eos-application.
Data availability
All data are available with the Pediatric Spine Study Group.
References
Skaggs D, Akbarnia B, Flynn J et al (2014) Chest wall and spine deformity study group; growing spine study group; pediatric orthopaedic society of North America; scoliosis research society growing spine study committee. A classification of growth friendly spine implants. J Pediatr Orthop 34(3):260–274
El-Hawary R, Akbarnia BA (2015) Early onset scoliosis - time for consensus. Spine Deform 3(2):105–106
Riseborough EJ, Wynne-Davies R (1973) A genetic survey of idiopathic scoliosis in Boston, Massachusetts. JBJS 55(5):974–982
Yang S, Andras LM, Redding GJ et al (2016) Early-onset scoliosis: a review of history, current treatment, and future directions. Pediatrics 137(1):e20150709
Akbarnia BA, Yazici M, Thompson GH (2010) The growing spine: management of spinal disorders in young children. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-540-85207-0
Skaggs DL, Akbarnia BA, Flynn JM et al (2014) A classification of growth friendly spine implants. J Pediatr Orthop 34(3):260–274
Campbell RM Jr, Smith MD, Mayes TC et al (2003) The characteristics of thoracic insufficiency syndrome associated with fused ribs and congenital scoliosis. JBJS 85(3):399–408
Williams BA, Matsumoto H, McCalla DJ et al (2014) Development and initial validation of the classification of early-onset scoliosis (C-EOS). J Bone Joint Surg Am 96(16):1359–1367
Dragsted C, Ohrt-Nissen S, Hallager DW et al (2020) Reproducibility of the classification of early onset scoliosis (C-EOS). Spine Deform 8(2):285–293
Russo C, Trupia E, Campbell M et al (2019) The association between the classification of early-onset scoliosis and smith complications after initiation of growth-friendly spine surgery: a preliminary study. J Pediatr Orthop 39(10):e737–e741
Lenke LG, Betz RR, Harms J et al (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. JBJS 83(8):1169–1181
Garbuz DS, Masri BA, Esdaile J et al (2002) Classification systems in orthopaedics. JAAOS - J Am Acad Orthop Surg 10(4):290–297
Vitale MG, Gomez JA, Matsumoto H et al (2011) Variability of expert opinion in treatment of early-onset scoliosis. Clin Orthop Relat Res 469(5):1317–1322
Corona J, Miller DJ, Downs J et al (2013) Evaluating the extent of clinical uncertainty among treatment options for patients with early-onset scoliosis. JBJS 95(10):e67
Hughes MS, Swarup I, Makarewich CA et al (2020) Expert consensus for early onset scoliosis surgery. J Pediatr Orthop 40(7):e621–e628
Williams BA, Asghar J, Matsumoto H et al (2013) More experienced surgeons less likely to fuse: a focus group review of 315 hypothetical EOS cases. J Pediatr Orthop 33(1):68–74
Sangole AP, Aubin C-E, Labelle H et al (2009) Three-dimensional classification of thoracic scoliotic curves. Spine 34(1):91–99
Stokes IA, Sangole AP, Aubin C-E (2009) Classification of scoliosis deformity 3-D spinal shape by cluster analysis. Spine 34(6):584
Donzelli S, Poma S, Balzarini L et al (2015) State of the art of current 3-D scoliosis classifications: a systematic review from a clinical perspective. J Neuroeng Rehabil 12(1):1–11
Thong W, Parent S, Wu J et al (2016) Three-dimensional morphology study of surgical adolescent idiopathic scoliosis patient from encoded geometric models. Eur Spine J 25(10):3104–3113
Kadoury S, Labelle H (2012) Classification of three-dimensional thoracic deformities in adolescent idiopathic scoliosis from a multivariate analysis. Eur Spine J 21(1):40–49
Bezdek J (1981) Pattern recognition with fuzzy objective function algorithms. Plenum, New York
Shen J, Parent S, Wu J et al (2020) Towards a new 3D classification for adolescent idiopathic scoliosis. Spine Deform 8(3):387–396
Ball GH (1965) Isodata-An iterative method of multivariate analysis and pattern classification. Proc IFIPS Congr
Acknowledgements
This project was partly supported by funding from Drexel University, and the Wyss-Campbell Center for Thoracic Insufficiency Syndrome at the Children’s Hospital of Philadelphia.
Funding
Wyss-Campbell Center for Thoracic Insufficiency Syndrome.
Author information
Authors and Affiliations
Consortia
Contributions
GV: Conception, data collection, data curation and analysis, methodology, data visualization, data analysis and interpretation, data visualization, writing—original draft and editing, agree to be accountable for the work, approval of the final version of the manuscript. PJC: Methodology, data curation and analysis, resources, formal analysis, writing-critical review and editing, approval of the final version of the manuscript, agree to be accountable for the work. MGV: Methodology, data curation and analysis, resources, formal analysis, writing -critical review and editing, approval of the final version of the manuscript, agree to be accountable for the work. BAW: Formal analysis, data curation and analysis, writing—critical review and editing, approval of the final version of the manuscript, agree to be accountable for the work. Pediatric Spine Study Group: Data curation and analysis, formal analysis, writing—critical review and editing, approval of the final version of the manuscript, agree to be accountable for the work. SB: Conceptualization, methodology, formal analysis, resources, data collection, data curation and analysis, writing—original draft, visualization, supervision, project administration, funding acquisition, approval of the final version of the manuscript, agree to be accountable for the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This study was given Ethical Approval by the Institutional Review Board prior to the conduct of this study. Informed consent and/or a waiver of consent was obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Viraraghavan, G., Cahill, P.J., Vitale, M.G. et al. Automated Clustering Technique (ACT) for Early Onset Scoliosis: A preliminary report. Spine Deform 11, 723–731 (2023). https://doi.org/10.1007/s43390-022-00634-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-022-00634-1