Abstract
Pregnant women in sub-Saharan Africa have high rates of maternal morbidity. There is interest in the impact of the vaginal microbiome on maternal health, including HIV and sexually transmitted infection (STI) acquisition. We characterized the vaginal microbiota of South African women ≥ 18 years with and without HIV in a longitudinal cohort over two visits during pregnancy and one visit postpartum. At each visit, we obtained HIV testing and self-collected vaginal swabs for point-of-care testing for STIs and microbiota sequencing. We categorized microbial communities and evaluated changes over pregnancy and associations with HIV status and STI diagnosis. Across 242 women (mean age 29, 44% living with HIV, 33% diagnosed with STIs), we identified four main community state types (CSTs): two lactobacillus-dominant CSTs (dominated by Lactobacillus crispatus and Lactobacillus iners respectively) and two diverse, non-lactobacillus-dominant CSTs (one dominated by Gardnerella vaginalis and one by diverse facultative anaerobes). From the first antenatal visit to the third trimester (24–36 weeks gestation), 60% of women in the Gardnerella-dominant CST shifted to lactobacillus-dominant CSTs. From the third trimester to postpartum (mean 17 days post-delivery), 80% of women in lactobacillus-dominant CSTs shifted to non-lactobacillus-dominant CSTs with a large proportion in the facultative anaerobe-dominant CST. Microbial composition differed by STI diagnosis (PERMANOVA R2 = 0.002, p = 0.004), and women diagnosed with an STI were more likely to be categorized as L. iners-dominant or Gardnerella-dominant CSTs. Overall, we found a shift toward lactobacillus dominance during pregnancy and the emergence of a distinct, highly diverse anaerobe-dominant microbiota profile in the postpartum period.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sub-Saharan Africa faces significant challenges in maternal and infant health. In 2020, 70% of all maternal deaths worldwide occurred in sub-Saharan Africa [1], and there were an estimated 50 infant deaths for every 1000 live births in 2020 [2]. Many of these adverse birth outcomes are caused by preventable or curable infectious diseases. HIV has been estimated to account for 24% of pregnancy-related mortality in sub-Saharan Africa and is a leading cause of death among reproductive-aged cisgender women [3, 4]. The risk of HIV acquisition is increased during pregnancy and postpartum, which then also increases the risk of vertical transmission [5]. HIV incidence remains high in pregnant and breastfeeding women in South Africa; in a recent study in Cape Town, postpartum HIV incidence was 1.86/100 person-years (95% CI 0.88–3.89), and incidence was highest during the first 6 months postpartum (2.71/100 person-years, 95% CI 1.13–6.51) [6]. Sub-Saharan Africa also has the highest incidence rate of bacterial STIs in the world, with 60 million new infections every year [7]. Untreated STIs in pregnancy lead to adverse pregnancy outcomes including preterm birth, stillbirth, and infant death [8]. In South Africa specifically, the prevalence of bacterial STIs during pregnancy ranges from 30 to 40% [9, 10].
There is growing interest in the role of the vaginal microbiome in the health of reproductive-aged women and their infants, particularly with respect to HIV and STI acquisition during pregnancy. Studies from North America and Europe have shown that an optimal vaginal microbiome is dominated by lactobacillus species, including Lactobacillus crispatus, L. gasseri, and L. jensenii [11], which modulate vaginal pH predominantly through the production of D-lactic acid [12]. Conversely, microbiomes dominated by facultative anaerobes including Gardnerella, Prevotella, and Atopobium spp. are linked to bacterial vaginosis (BV). BV and anaerobe-dominant vaginal microbial states may increase the risk of HIV and STI acquisition [13,14,15,16] and have been shown to be associated with adverse pregnancy outcomes including preterm birth [17,18,19].
Subsequent work has demonstrated that the vaginal microbiome varies significantly with geography, ethnicity, and socioeconomic status [11, 20, 21]. Studies have reported that African women have diverse vaginal microbiota with high levels of non-lactobacillus anaerobes, including Gardnerella, Prevotella, and other BV-associated species [13, 22, 23]. They also have a higher relative abundance of Lactobacillus iners which is more likely to coexist with rather than inhibit the growth of anaerobic bacteria [24, 25]. These microbial patterns are not fully understood but may be related to a variety of social, economic, and behavioral factors [26, 27]. Observational studies have shown that differences in microbial composition may increase the risk of acquiring HIV and STIs [15, 25, 28], and some studies have suggested that this may contribute to the disproportionately high burden of HIV and STIs among African women [13, 29, 30]. However, many L. iners and anaerobe-dominant profiles also occur in healthy African women and may represent normal variants that behave differently from lactobacillus-dominant profiles [22, 28, 31]. There is a need to better characterize the vaginal microbiome to understand what constitutes optimal and identify patterns associated with the risk of disease acquisition.
Pregnancy is a normal physiologic state that both influences and is influenced by the composition of the vaginal microbiome. Over the course of pregnancy, there is a gradual increase in lactobacillus species (including L. iners) and decreased microbial diversity, followed by a rapid increase in diversity and growth of anaerobic species in the postpartum period [17, 20, 23, 28, 32,33,34]. This is thought to be mediated by estrogen, which promotes glycogen deposition in the vaginal epithelium and supports lactobacillus proliferation [34, 35]. Given the associations between lactobacillus abundance and an optimal microbiome, studies have suggested that pregnancy induces a favorable change in the microbiome to prevent maternal genital infection and adverse birth outcomes [20]. Conversely, the rapid increase in bacterial diversity in the postpartum period [32, 34] may contribute to increased HIV risk during the postpartum period. Shifts in microbial composition during pregnancy may be particularly pronounced in women with diverse microbiome profiles at baseline [20]. Several cross-sectional studies performed in African countries have shown that pregnant women with HIV have more anaerobe-predominant microbiome profiles [14, 25, 31, 36], and a study from Kenya described species differences in pregnant women with Chlamydia trachomatis (CT) or Trichomonas vaginalis (TV) infection compared to uninfected women. However, there are few longitudinal studies of the vaginal microbiome in pregnant African women, and it is not fully understood whether these microbial transitions during pregnancy and postpartum have any impact on maternal and neonatal outcomes.
This study aims to characterize the vaginal microbiota over the course of pregnancy and in the immediate postpartum period in a cohort of women in Cape Town, South Africa. We also evaluated associations of microbial composition with HIV serostatus and STI diagnosis across the peripartum period.
Methods
Recruitment and Visit Procedures
The STI in pregnancy (STIP) study was conducted at a public sector antenatal clinic (ANC) in Cape Town, South Africa, as described previously [10]. Briefly, from November 2017 to July 2018, we enrolled pregnant women ≥ 18 years of age with and without HIV presenting to the ANC for prenatal care. Gestational age was estimated based on the date of the last menstrual period. Women participated in two visits over the course of their pregnancy and one in early postpartum: first visit to the ANC (Visit A), third-trimester visit (Visit B), and postpartum visit (Visit PPt). Women who presented for Visit A at gestational age > 28 weeks did not have a Visit B.
Data Collection
At each study visit, a trained study counselor collected data from a study survey on demographics, sexual behavior, health data (including HIV status and treatment), and any symptoms of STIs. Each woman then self-collected vulvovaginal swabs using Xpert® CT/NG Vaginal/Endocervical Specimen Collection kits (Cepheid, Sunnyvale, CA). These swabs underwent on-site Xpert nucleic acid amplification testing for Neisseria gonorrhea (NG) and Chlamydia trachomatis (CT) and an Xpert TV assay for Trichomonas vaginalis (Cepheid). Afterwards, swabs were sent to UCLA for microbiome analysis. Women were given same-day results for CT, NG, and TV testing if the results were available before they left the clinic. Women with a positive STI test result based on the Xpert® result or who reported symptoms and did not report previously receiving treatment for their STI at the same visit were given treatment in accordance with South African national guidelines [37]. CT infections were treated with 1 g azithromycin orally via directly observed therapy, NG with an intramuscular injection of 250 mg ceftriaxone plus 1 g azithromycin orally (or 2 g azithromycin in case of significant penicillin allergy), and TV with 400 mg metronidazole orally every 12 h for 7 days. Women who presented with symptoms including dysuria, unusual vaginal discharge, or vaginal itching were given all three antibiotics as syndromic treatment [37]. As per the national STI guidelines, women were given counselling, provided with condoms, and given a partner notification/referral letter [37].
At enrollment, pregnant women with unknown or negative HIV serostatus were tested for HIV according to the South African National testing guidelines [37]. These women received a Toyo® Anti-HIV ½ rapid assay, and those who tested positive received a confirmatory DetermineTM HIV Ag/Ab Combo rapid test (Abbott, Chicago, IL). Women with known HIV reported whether they were taking antiretroviral therapy (ART). Women who tested negative for HIV received repeat rapid HIV testing at each subsequent visit. At the postpartum visit, women were asked about their delivery details and infant outcomes, and this was verified against their antenatal clinical records. World Health Organization guidelines were used to categorize adverse pregnancy and birth outcomes [38].
Microbiota Profiling
Profiling of the bacterial microbiota of the collected vaginal swab samples was performed by sequencing the V4 (515F/806R) region of the 16S rRNA gene, as previously described [39]. Briefly, samples were transferred to Lysing Matrix E tubes (MP Biomedicals, Burlingame, CA, USA) with RLT lysis buffer (Qiagen, Hilden, Germany) and bead-beated on a TissueLyser (Qiagen). Following manufacturer protocol, the AllPrep DNA/RNA/Protein kit (Qiagen) was used to extract DNA. In addition to negative controls from the DNA extraction and PCR steps used to identify contaminant sequences, independent aliquots of a bacterial mock community were processed together with samples to evaluate extraction, amplification, and the expected relative abundance of bacteria [40].
Data Processing and Statistical Analysis
DADA2 was used for exact sequence inference and chimera removal, followed by contaminant sequence removal using the “decontam” R package [41]. Species-level taxonomic labels were assigned using BLASTn against the SILVA database (release 138). We assigned vaginal microbial community state types (CSTs) using the VALENCIA nearest centroid classification method for ease of comparing CSTs across studies [42].
Statistical analyses were performed using the “phyloseq,” “vegan,” “lmerTest,” “glmmTMB,” and “emmeans” packages in the R statistical computing environment (version 4.1.3) [43,44,45,46,47]. Data were stratified by study visit and clinical variables of interest: HIV status, STI diagnosis at any time point, and pregnancy and birth outcomes. The Shannon diversity and Bray-Curtis dissimilarity were used for the analysis of alpha and beta diversity, respectively. Permutational multivariate analysis of variance (PERMANOVA) as implemented in the “adonis2” R function was used to identify drivers of overall microbiota variation. Differences in CST composition and stability were assessed using a chi-squared test or Z-test of equal proportions as appropriate. Alpha diversity was compared using a mixed effects linear model with a subject-level random effect, and data are presented as estimated marginal means. Differential abundance testing at the species level was performed using a zero-inflated negative binomial model. p-values for alpha diversity and species-level differential abundance testing were adjusted for multiple comparisons using the Benjamini-Hochberg false discovery rate (FDR) method. All other p-values were reported without adjustment.
Results
Population Characteristics
We recruited and enrolled 242 women, of which 107 (44%) were living with HIV (Table 1). The mean age was 29.5 years (SD 6.1), and 101 (42%) participants reported to be married or cohabitating. Most participants had completed secondary school (91%), and most were unemployed or students (69%). The mean gestational age at Visit A (first ANC visit) was 18.6 weeks (SD 6.3), with a range of 6–30 weeks (Supplement S1). The gestational age range at Visit B (third trimester visit) was 24–36 weeks. The mean gestational age at the postpartum visit was 17 days after delivery (SD 28 days). The majority of women (98.8%) reported a single partner in the 3 months prior to Visit A.
Of the women living with HIV, 76 (71%) were already on ART at the first ANC visit (Visit A), 12 had previously been on ART but were not taking it at the time of Visit A, and 24 were newly diagnosed and had not yet initiated ART. Of the 76 women taking ART, the majority (75%) reported taking a combination of tenofovir disoproxil, emtricitibine, and efavirenz. Six women who initially tested HIV-negative at Visit A were seroconverted by Visit PPt. A total of 80 participants (33%) tested positive for any STI at any time point, with 52 (22%) positive for CT, 14 (6%) positive for NG, and 38 (16%) positive for TV. The majority of STI diagnoses were made during Visit A (Supplement S2). Overall, 90.9% of participants delivered full-term, and 91.7% had live births without complications.
Bacterial Community Composition
Based on a previously defined set of vaginal community types [42], we identified five CSTs: CST I, dominated by L. crispatus; CST III, dominated by L. iners; CST IV-A, dominated by Candidatus lachnovcurva vaginae and Gardnerella vaginalis with moderate Atopobium vaginae; CST IV-B, with high G. vaginalis and low Ca. l. vaginae and moderate A. vaginae; and CST IVC, low lactobacillus, G. vaginalis, and A. vaginae with high proportions of facultative anaerobes including Prevotella species (Supplement S3). CST IV-A was relatively small and did not appear distinct from CST IV-B on the two major axes of the principal coordinates analysis (PcoA, Supplement S3), so these two were grouped into CST IV-AB for all remaining analyses (Fig. 1). The most prevalent CSTs were CST III (43% of all samples) and CST IV-AB (39% of all samples). Lactobacillus-dominant CSTs were the majority (51%), but only 9% of women were assigned to CST I. There were no samples assigned to CST II (L. jensenii dominant) or CST V (L. gasseri dominant). Approximately 10% of samples were categorized as CST IV-C, which was highly diverse and had large proportions of Prevotella bivia, Prevotella timonensis, and Ureaplasma urealytica.
Heatmap of bacterial taxa identified by 16S sequencing of cervical swabs collected from 242 women across three visits during pregnancy. CSTs determined by the VALENCIA classifier; CST I dominated by L. crispatus; CST III dominated by L. iners; CST IVA dominated by Candidatus lachnovcurva vaginae and Gardnerella vaginalis with moderate Atopobium vaginae; CST IVB with high G. vaginalis and low Ca. l. vaginae and moderate A. vaginae; and CST IVC, low Lactobacillus, G. vaginalis, and A. vaginae with high proportions of facultative anaerobes including Prevotella species. The Shannon diversity index for each sample is depicted across the top
Changes in Vaginal Microbiota During Pregnancy
We next looked at the microbiota across Visits A (6–30 weeks), B (24–36 weeks), and postpartum (mean 17 days after delivery) (Fig. 2). Compared to Visit A, women at Visit B had higher relative abundances of L. crispatus and L. iners and higher proportions of CST I and CST III (Fig. 2a). At the postpartum visit, women were more likely to have CST IV-AB and CST IV-C. Shannon’s diversity was significantly increased at the postpartum visit compared to Visit A (p < 0.001, Fig. 2b). Interestingly, very few samples belonged to CST IV-C at Visit A and Visit B, but a sizable proportion of CST IV-C emerged postpartum. Overall community composition differed significantly by visit or trimester (PERMANOVA R2 = 0.04, p < 0.001, Fig. 2c). Since Visit A varied widely in gestational age, we examined taxa plots from Visit A by week of gestation (Supplement S4), which did not significantly differ. Moderate transitions in CST distribution were observed at an individual level from Visit A to B, with women with CST IV-AB at Visit A predominantly shifting to CST III (Fig. 2d, Table 2, chi-squared p <0.001).
Composition of the vaginal microbiome across three visits during pregnancy. Visit A = initial visit (gestational age ranging from 6 to 30 weeks); Visit B = second-trimester visit (GA 28–36 weeks); Visit PPt = postpartum visit (mean 17 days after delivery). a Relative proportions of bacterial taxa at each visit across pregnancy. CSTs are shown across the bottom. b Shannon’s diversity between visits, presented as box plots with mean and interquartile range for each visit. The Shannon diversity was higher at Visit PPt compared to Visit A (p = 2.0E-11). c PCoA of samples across visits using the Bray-Curtis index (PERMANOVA R2 = 0.04, p < 0.001). Shaded ellipses denote 95% confidence intervals. d Transitions between CSTs across visits. Moderate changes in CST distribution were observed from Visit A to B, with decreased CST IV-AB at Visit B, as a result of shifting to CST I or CST III. CST IV-AB was more likely to transition to CST III than to CST I (chi-squared p < 1E-10). From Visit B to Visit PPt, a majority of CST III samples converted to CST IV-AB, while some members of CST I, CST III, and CST IV-AB all shifted to CST IV-C. CST III was more stable and less likely to transition than CST I (Table 2, chi-squared p = 0.048)
During pregnancy, women with CSTs I and III had a more stable vaginal microbiota than those with IV-AB, whereas CST IV-AB was more stable during the transition period from pregnancy to postpartum (Supplement S5). From Visit B to postpartum, drastic CST transitions were observed, with a majority of CST III samples shifting to CST IV-AB, while a high proportion of women with CST I, CST III, and CST IV-AB all shifted to CST IV-C in similar proportions (Fig. 2d, Table 2). In this transition, very few women in both CST I and CST III remained in the same CST, but women in CST III were more likely than women in CST I to remain in the same CST at the postpartum visit (p = 0.048).
Vaginal Microbial Associations with HIV Serostatus
We next assessed whether HIV infection and any STI diagnosis during pregnancy were associated with differences in vaginal microbiota. CST distribution did not differ by HIV status at any visit (Fig. 3a, Table 3), although community composition differed significantly between women with and without HIV (PERMANOVA R2 = 0.002, p = 0.006, Fig. 3b). Shannon’s diversity was not significantly different between women with and without HIV (Fig. 3c). With respect to individual species, differential abundance testing showed that HIV infection was associated with a lower relative abundance of L. jensenii at Visit B, a lower relative abundance of P. corporis and bergensis at the postpartum visit, and higher Metamycoplasma hominis and A. vaginae at the postpartum visit (Supplement S6, p < 0.01). Transitions in CSTs did not appear to differ by HIV status (Fig. 3d). Specifically, there was no significant difference between women with and without HIV in the likelihood of transitioning from CST IV to CST I or III from Visit A to Visit B, and no significant difference in transition from CST I or III from Visit B to CST IV at Visit PPt, nor any differences in CST stability (Supplement S5).
CST distribution across visits with respect to HIV status. a Relative proportions of CSTs across visits, stratified by HIV status. b Shannon’s diversity at each visit by HIV status. c PCoA by HIV status across all visits using the Bray-Curtis index (PERMANOVA R2 = 0.002, p = 0.006). Shaded ellipses denote 95% confidence intervals. d Transitions between CSTs across visits, stratified by HIV status. No differences in transition probabilities were observed
Overall, 29% of women living with HIV had not yet initiated ART at Visit A. A higher proportion of women living with HIV who had not yet initiated ART had vaginal microbiota characterized by CST IV-AB, though Shannon’s diversity was non-significantly higher in this group (Supplement S7, unadjusted p = 0.06). The six women who seroconverted to HIV-positive over the course of the study were all categorized as CST IV-AB or CST IV-C at Visit PPt (Supplement S8), though this difference was not statistically significant.
Vaginal Microbial Associations with STI Diagnosis During the Peripartum Period
CST distribution differed between women with and without an STI diagnosis (Fig. 4a). At Visit A, women with an STI diagnosis were more likely to be categorized as CST IV-AB or CST III (Fig. 4a, Table 3, Fisher’s exact p = 0.013). This pattern appeared to hold for each individual STI, though it did not reach significance for NG (Supplement S9, Table 3.). Only three women categorized as CST I at Visit A were diagnosed with STIs at any visit. Postpartum, there was a trend for women with an STI diagnosis to be more likely to have vaginal microbiota characterized as CST IV-C compared to any other CSTs (Table 3, p = 0.07).
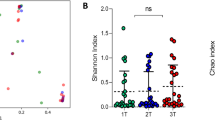
CST distribution across visits with respect to STI diagnosis at any visit. a Relative proportions of CSTs across visits, stratified by STI diagnosis. b Shannon’s diversity by STI diagnosis across all visits. At Visit A, Shannon’s diversity was higher among women who had been diagnosed with an STI (p = 0.004). c PCoA by STI diagnosis across all visits using the Bray-Curtis index (PERMANOVA R2 = 0.002, p = 0.004). Shaded ellipses denote 95% confidence intervals. d Transitions between CSTs across visits, stratified by STI diagnosis. No differences in transition probabilities were observed
Overall microbiota composition also differed between women with and without an STI diagnosis (PERMANOVA R2 = 0.002, p=0.004, Fig. 4b). Shannon’s diversity was increased in women who had an STI diagnosis compared to women who did not at Visit A (Fig. 4c, p=0.004) and at Visit B (Fig. 4c, p=0.05). Individual taxa associated with STI diagnosis included P. bivia, colorons, amnii, and bucallis, Metamycoplasma hominis, and Sneathia amnii at Visit A (Supplement S10, p < 0.05), as well as P. bucallis at Visit B and other Prevotella species at Visit PPt (Supplement S10, p < 0.05). Most of these associations appeared to be driven by C. trachomatis (Supplement S9 and S10). STI diagnosis did not appear to have any impact on CST stability and transition probabilities over the course of pregnancy (Fig. 4d, Supplement S5).
Fifty-nine women reported possible STI-related symptoms at Visit A and 14 at Visit B. Visually, CST distribution showed increased CST IV-C at Visit PPt in women who reported symptoms (and thus received antibiotics) at a prior visit, but PCoA and Shannon’s diversity index showed no significant differences (Supplement S11).
Vaginal Microbial Associations with Adverse Pregnancy and Birth Outcomes
In addition to HIV and STI status, we also examined birth outcomes and other variables for associations with microbiota composition. Overall, 36 participants (15%) reported adverse pregnancy or birth outcomes including miscarriage, neonatal death, stillbirth, or preterm birth. We included these outcomes as a composite adverse birth or pregnancy outcome variable. Visually, women who had adverse pregnancy or birth outcomes were more likely to be categorized in CST IV-A at Visit A or Visit B and less likely to be in CST IV-C at Visit PPt, as compared to women who delivered full-term live infants, but the result was not statistically significant (Supplement S12). We did find a relationship between age and CST, with younger women being more likely to be in CST IV-C at both Visit A (p = 0.044) and Visit PPt (p = 0.035, Table 3).
Discussion
We profiled the vaginal microbiota in a cohort of South African women over three visits during pregnancy and in the immediate postpartum period. We confirmed the transition of diverse microbial signatures toward lactobacillus-dominant signatures during pregnancy and identified the emergence of a facultative-anaerobe-rich, diverse signature in the early postpartum period which appears distinct from the vaginal microbial signatures of women early in pregnancy. We did not find a significant difference in CST distribution in women with and without HIV, but we found that women diagnosed with STIs were more likely to have microbial signatures belonging to CST III or CST IV-A at the first ANC visit. To our knowledge, this is one of the few longitudinal studies of the vaginal microbiota in pregnant South African women.
We categorized vaginal 16S rRNA gene sequences according to the VALENCIA nearest-centroid classification model for ease of comparison across populations. Consistent with prior studies among women of African descent [11, 22], about half of all samples belonged to lactobacillus-dominant CSTs, whereas the other half were dominated by diverse communities. Among the diverse communities, we found distinct and substantial populations of CST IV-AB and CST IV-C. Other studies performed in African populations have also identified distinct anaerobe-dominant CSTs [15, 25, 31, 36], though this may vary with CST clustering methods [48]. It is unclear whether these two non-lactobacillus-dominant CSTs are clinically significant. However, previous studies in non-pregnant women in the FRESH and CAPRISA cohorts also identified a distinct, facultative anaerobe-dominant cervicotype which showed a significantly increased risk of HIV acquisition, in addition to a Gardnerella-dominant cervicotype which did not show this same increased risk [15, 49].
During pregnancy, we noted a significant shift away from CST IV toward lactobacillus-dominant CSTs, which is consistent with prior studies ([20, 28, 33, 34]. Serrano et al. showed that American women of African descent had a decrease in diversity and transition to lactobacillus species early in pregnancy, as early as the second trimester [20]. Our data is limited by the variability of gestational age at the first visit and the absence of a microbiome sample before pregnancy, but there was a clear shift toward lactobacillus species even into the third trimester (Visit B). Like Serrano et al., we noted that vaginal microbial profiles from CST IV were more likely to switch to CST III as compared to CST I [20].
In the postpartum period, we observed an increase in facultative anaerobic taxa and alpha diversity with a significant number of women categorized as CST IV-C, which was not present in high proportions during pregnancy. We noted that both CST I and CST III were similarly likely to transition to CST IV-AB and CST IV-C postpartum. Unlike Goltsman et al., who found that CST I was more stable than CST III from the third trimester into the postpartum period, our data showed the opposite [50]. Previous studies have documented a sharp increase in diversity and anaerobic taxa during the postpartum period [32,33,34, 36], in part from a combination of decreased estrogen and changes in cervical remodeling during delivery [32]. Altogether, these results support a model by which pregnancy acts as a selective pressure toward a more optimal, lactobacillus-dominant vaginal microbiome, possibly mediated by estrogen. Understanding the process by which this occurs may facilitate the development of therapeutics, such as topical hormones, for beneficially altering the vaginal microbiome during or after pregnancy [51, 52].
We found differences in community composition, but not alpha diversity or CST distribution in the vaginal microbiota of women with and without HIV. Prior studies show increased alpha diversity in women living with HIV versus women without HIV [14, 16, 31], though some of these results may be confounded by socioeconomic factors. Price et al. found that compared with women on ART, women not on ART have more diverse vaginal microbiomes with a higher proportion of anaerobes. Chehoud et al. showed no difference in vaginal microbiota by HIV status when all women with HIV women were virally suppressed on ART [53]. In our study, a subset of women who were not on ART at the first ANC visit trended toward more CST IV-AB at Visit A compared to those established on ART, suggesting some of this discrepancy is explained by ART use or degree of immunodeficiency. Unfortunately, our results are limited by the absence of viral load and CD4 data from the time of enrollment.
At the first ANC visit, women who were diagnosed with any STIs (CT, NG, or TV) were more likely to be categorized as CST IV-AB or CST III than CST I. Our findings are consistent with previous studies noting fewer STI diagnoses in L. crispatus-dominant profiles, and more STI diagnoses in both L. iners and anaerobe-dominant profiles [25, 54], and supports the hypothesis that L. crispatus is more protective against pathogens than L. iners and anaerobic species. More research is needed to understand whether and how L. crispatus protects against pathogens, and whether there are distinctions between L. iners and anaerobe-dominant microbiome profiles with respect to STI susceptibility, as STIs are a significant contributor to peripartum morbidity in sub-Saharan Africa. We did not find any significant differences in the microbiota with respect to adverse birth outcomes including preterm birth. However, our study was not powered to detect this difference, and only 36 women in our sample had adverse pregnancy or birth outcomes.
Strengths of our study include its longitudinal design across pregnancy and into the postpartum period. In addition to the limitations already mentioned, others include small numbers of women living with HIV who are not on ART. For STI testing, as all women were treated, it is unclear if any subsequent changes in their microbiota were mediated by antibiotics. We did not collect data on inflammatory markers, metabolomics, or other vaginal biomarkers. Additionally, our study took place among pregnant women at one antenatal clinic in Cape Town, and the results may not be generalizable across other regions or populations. Finally, this study was observational and cannot make any causal inferences regarding pregnancy and vaginal microbiota.
Conclusions
Our study confirms a shift toward lactobacillus dominance during pregnancy and the rapid emergence of distinct, highly diverse anaerobe-dominant vaginal microbial communities in the postpartum period. More work is needed to better understand the impact of the vaginal microbiome on perinatal outcomes and STI, HIV acquisition, and vertical transmission. Researchers have suggested that the shift toward lactobacillus during pregnancy, which is mediated by estrogen and other physiologic changes, might foster a more optimal vaginal environment to prevent infection during pregnancy, which is then lost during the postpartum period. If this is the case, then there may be a role for hormonal and other therapies mimicking the physiologic changes of pregnancy to manipulate the vaginal microbiome toward an optimal state.
Data Availability
The datasets generated and/or analyzed during the current study will be available in the NCBI SRA at https://www.ncbi.nlm.nih.gov/bioproject/PRJNA894713.
Code Availability
Available upon request.
Abbreviations
- ART:
-
Anti-retroviral therapy
- CST:
-
Community state type
- CT:
-
Chlamydia trachomatis
- G:
-
Grams
- HIV:
-
Human immunodeficiency virus
- MG:
-
Milligrams
- NG:
-
Neisseria gonorrhea
- SD:
-
Standard deviation
- STI:
-
Sexually transmitted infection
- TV:
-
Trichomonas vaginalis
References
UNICEF. Trends in estimates of maternal mortality ratio, maternal deaths and lifetime risk of maternal death, 2000-2020. 2003. Available from: https://data.unicef.org/topic/maternal-health/maternal-mortality/. Accessed 25 May 2023
UN Inter-agency Group for Child Mortality Estimation. Child mortality estimates 2020. 2023. Available from: https://childmortality.org/. Accessed 25 May 2023.
Calvert C, Ronsmans C. The contribution of HIV to pregnancy-related mortality: a systematic review and meta-analysis. AIDS. 2013;27(10):1631–9.
Zaba B, Calvert C, Marston M, Isingo R, Nakiyingi-Miiro J, Lutalo T, et al. Effect of HIV infection on pregnancy-related mortality in sub-Saharan Africa: secondary analyses of pooled community-based data from the network for analysing longitudinal population-based HIV/AIDS data on Africa (ALPHA). Lancet. 2013;381(9879):1763–71.
Thomson KA, Hughes J, Baeten JM, John-Stewart G, Celum C, Cohen CR, et al. Increased risk of HIV acquisition among women throughout pregnancy and during the postpartum period: a prospective per-coital-act analysis among women with HIV-infected partners. J Infect Dis. 2018;218(1):16–25.
le Roux SM, Abrams EJ, Nguyen KK, Myer L. HIV incidence during breastfeeding and mother-to-child transmission in Cape Town, South Africa. AIDS. 2019;33(8):1399–401.
World Health Organization. Global health sector strategy on sexually transmitted infections 2016–2021. Geneva, Switzerland; 2016. Available fromhttps://apps.who.int/iris/rest/bitstreams/1032114/retrieve. Accessed 25 May 2023
Warr AJ, Pintye J, Kinuthia J, Drake AL, Unger JA, McClelland RS, et al. Sexually transmitted infections during pregnancy and subsequent risk of stillbirth and infant mortality in Kenya: a prospective study. Sex Transm Inf. 2019;95(1):60–6.
Nyemba DC, Medina-Marino A, Peters RPH, Klausner JD, Ngwepe P, Myer L, et al. Prevalence, incidence and associated risk factors of STIs during pregnancy in South Africa. Sexu Trans Inf. 2021;97(5):375.
Joseph Davey DL, Nyemba DC, Gomba Y, Bekker L-G, Taleghani S, DiTullio DJ, et al. Prevalence and correlates of sexually transmitted infections in pregnancy in HIV-infected and- uninfected women in Cape Town, South Africa. PLoS One. 2019;14(7):e0218349.
Ravel J, Gajer P, Abdo Z, Schneider GM, Koenig SS, McCulle SL, et al. Vaginal microbiome of reproductive-age women. Proc Natl Acad Sci USA. 2011;108(Suppl 1):4680–7.
Tachedjian G, Aldunate M, Bradshaw CS, Cone RA. The role of lactic acid production by probiotic Lactobacillus species in vaginal health. Res Microbiol. 2017;168(9):782–92.
Bayigga L, Kateete DP, Anderson DJ, Sekikubo M, Nakanjako D. Diversity of vaginal microbiota in sub-Saharan Africa and its effects on HIV transmission and prevention. Am J Obstet Gynecol. 2019;220(2):155–66.
Price JT, Vwalika B, Hobbs M, Nelson JAE, Stringer EM, Zou F, et al. Highly diverse anaerobe-predominant vaginal microbiota among HIV-infected pregnant women in Zambia. PLoS One. 2019;14(10):e0223128-e.
Gosmann C, Anahtar MN, Handley SA, Farcasanu M, Abu-Ali G, Bowman BA, et al. Lactobacillus-deficient cervicovaginal bacterial communities are associated with increased HIV acquisition in young South African women. Immunity. 2017;46(1):29–37.
Short C-ES, Brown RG, Quinlan R, Lee YS, Smith A, Marchesi JR, et al. Lactobacillus-depleted vaginal microbiota in pregnant women living with HIV-1 infection are associated with increased local inflammation and preterm birth. Front Cell Infect Microbiol. 2021;10:596917
Stout MJ, Zhou Y, Wylie KM, Tarr PI, Macones GA, Tuuli MG. Early pregnancy vaginal microbiome trends and preterm birth. Am J Obstet Gynecol. 2017;217(3):356.e1–e18.
Fettweis JM, Serrano MG, Brooks JP, Edwards DJ, Girerd PH, Parikh HI, et al. The vaginal microbiome and preterm birth. Nat Med. 2019;25(6):1012–21.
Baud A, Hillion K-H, Plainvert C, Tessier V, Tazi A, Mandelbrot L, et al. Microbial diversity in the vaginal microbiota and its link to pregnancy outcomes. Sci Rep. 2023;13(1):9061.
Serrano MG, Parikh HI, Brooks JP, Edwards DJ, Arodz TJ, Edupuganti L, et al. Racioethnic diversity in the dynamics of the vaginal microbiome during pregnancy. Nat Med. 2019;25(6):1001–11.
Dixon M, Dunlop AL, Corwin EJ, Kramer MR. Joint effects of individual socioeconomic status and residential neighborhood context on vaginal microbiome composition. Front. Public Health. 2023;11:102974.
Anahtar MN, Byrne EH, Doherty KE, Bowman BA, Yamamoto HS, Soumillon M, et al. Cervicovaginal bacteria are a major modulator of host inflammatory responses in the female genital tract. Immunity. 2015;42(5):965–76.
Juliana NCA, Peters RPH, Al-Nasiry S, Budding AE, Morré SA, Ambrosino E. Composition of the vaginal microbiota during pregnancy in women living in sub-Saharan Africa: a PRISMA-compliant review. BMC Pregnancy Childbirth. 2021;21(1):596.
Petrova MI, Reid G, Vaneechoutte M, Lebeer S. Lactobacillus iners: friend or foe? Trends Microbiol. 2017;25(3):182–91.
Borgdorff H, Tsivtsivadze E, Verhelst R, Marzorati M, Jurriaans S, Ndayisaba GF, et al. Lactobacillus-dominated cervicovaginal microbiota associated with reduced HIV/STI prevalence and genital HIV viral load in African women. ISME J. 2014;8(9):1781–93.
Sun S, Serrano Myrna G, Fettweis Jennifer M, Basta P, Rosen E, Ludwig K, et al. Race, the vaginal microbiome, and spontaneous preterm birth. mSystems. 2022;7(3):e00017–22.
Virtanen S, Rantsi T, Virtanen A, Kervinen K, Nieminen P, Kalliala I, et al. Vaginal microbiota composition correlates between pap smear microscopy and next generation sequencing and associates to socioeconomic Status. Sci Rep. 2019;9(1):7750.
McClelland RS, Lingappa JR, Srinivasan S, Kinuthia J, John-Stewart GC, Jaoko W, et al. Evaluation of the association between the concentrations of key vaginal bacteria and the increased risk of HIV acquisition in African women from five cohorts: a nested case-control study. Lancet Infect Dis. 2018;18(5):554–64.
Karim SSA, Baxter C. HIV incidence rates in adolescent girls and young women in sub-Saharan Africa. Lancet Glob Health. 2019;7(11):e1470–e1.
Torrone EA, Morrison CS, Chen P-L, Kwok C, Francis SC, Hayes RJ, et al. Prevalence of sexually transmitted infections and bacterial vaginosis among women in sub-Saharan Africa: an individual participant data meta-analysis of 18 HIV prevention studies. PLoS Med. 2018;15(2):e1002511.
Gudza-Mugabe M, Havyarimana E, Jaumdally S, Garson KL, Lennard K, Tarupiwa A, et al. Human immunodeficiency virus infection is associated with preterm delivery independent of vaginal microbiota in pregnant African women. J Infect Dis. 2020;221(7):1194–203.
Nunn KL, Witkin SS, Schneider GM, Boester A, Nasioudis D, Minis E, et al. Changes in the vaginal microbiome during the pregnancy to postpartum transition. Reprod Sci. 2021;28(7):1996–2005.
DiGiulio DB, Callahan BJ, McMurdie PJ, Costello EK, Lyell DJ, Robaczewska A, et al. Temporal and spatial variation of the human microbiota during pregnancy. Proc Natl Acad Sci U S A. 2015;112(35):11060–5.
MacIntyre DA, Chandiramani M, Lee YS, Kindinger L, Smith A, Angelopoulos N, et al. The vaginal microbiome during pregnancy and the postpartum period in a European population. Sci Rep. 2015;5:8988.
Spear GT, French AL, Gilbert D, Zariffard MR, Mirmonsef P, Sullivan TH, et al. Human α-amylase present in lower-genital-tract mucosal fluid processes glycogen to support vaginal colonization by Lactobacillus. J Infect Dis. 2014;210(7):1019–28.
Doyle R, Gondwe A, Fan Y-M, Maleta K, Ashorn P, Klein N, et al. A Lactobacillus-deficient vaginal microbiota dominates postpartum women in rural Malawi. Appl Environ Microbiol. 2018;84(6):e02150–17.
South African National Department of Health. Sexually transmitted infections management guidelines, SA Health. 2018. https://www.health.gov.za/wp-content/uploads/2020/11/sti-guidelines-27-08-19.pdf. Accessed 25 May 2023.
WHO. Maternal, newborn, child and adolescent health: stillbirths 2020. 2020. Available at: https://www.who.int/maternal_child_adolescent/epidemiology/stillbirth/en/. Accessed June 04 2021.
Birse KD, Kratzer K, Zuend CF, Mutch S, Noël-Romas L, Lamont A, et al. The neovaginal microbiome of transgender women post-gender reassignment surgery. Microbiome. 2020;8(1):61.
Bender JM, Li F, Adisetiyo H, Lee D, Zabih S, Hung L, et al. Quantification of variation and the impact of biomass in targeted 16S rRNA gene sequencing studies. Microbiome. 2018;6(1):155.
Davis NM, Proctor DM, Holmes SP, Relman DA, Callahan BJ. Simple statistical identification and removal of contaminant sequences in marker-gene and metagenomics data. Microbiome. 2018;6:226.
France MT, Ma B, Gajer P, Brown S, Humphrys MS, Holm JB, et al. VALENCIA: a nearest centroid classification method for vaginal microbial communities based on composition. Microbiome. 2020;8(1):166.
McMurdie PJ, Holmes S. phyloseq: An R package for reproducible interactive analysis and graphics of microbiome census data. PLoS One. 2013;8(4):e61217.
Oksanen J. Vegan: community ecology package. R package version 2.6-4. 2022. http://wwwcranr-projectorg. Accessed 25 May 2023
Kuznetsova A, Brockhoff PB, Christensen RHB. lmerTest package: tests in linear mixed effects models. J Stat Soft. 2017;82(13):1–26.
Brooks ME, Kristensen K, Van Benthem KJ, Magnusson A, Berg CW, Nielsen A, Skaug HJ, Maechler M, Bolker BM. glmmTMB balances speed and flexibility among packages for zero-inflated generalized linear mixed modeling. The R J. 2017;9(2):378–400.
Searle SR, Speed FM, Milliken GA. Population marginal means in the linear model: an alternative to least squares means. Am Stat. 1980;34(4):216–21.
Balle C, Konstantinus IN, Jaumdally SZ, Havyarimana E, Lennard K, Esra R, et al. Hormonal contraception alters vaginal microbiota and cytokines in South African adolescents in a randomized trial. NatComm. 2020;11(1):5578.
Wang Y, Noël-Romas L, Perner M, Knodel S, Molatlhegi R, Hoger S, et al. Non-lactobacillus-dominant and polymicrobial vaginal microbiomes are more common in younger South African women and predictive of increased risk of human immunodeficiency virus acquisition. Clin InfectDis. 2023;76(8):1372–81.
Goltsman DSA, Sun CL, Proctor DM, DiGiulio DB, Robaczewska A, Thomas BC, et al. Metagenomic analysis with strain-level resolution reveals fine-scale variation in the human pregnancy microbiome. Genome Res. 2018;28(10):1467–80.
Shen J, Song N, Williams CJ, Brown CJ, Yan Z, Xu C, et al. Effects of low dose estrogen therapy on the vaginal microbiomes of women with atrophic vaginitis. Sci Rep. 2016;6(1):24380.
Srinivasan S, Hua X, Wu MC, Proll S, Valint DJ, Reed SD, et al. Impact of topical interventions on the vaginal microbiota and metabolome in postmenopausal women: a secondary analysis of a randomized clinical trial. JAMA Net Open. 2022;5(3):e225032-e.
Chehoud C, Stieh DJ, Bailey AG, Laughlin AL, Allen SA, McCotter KL, et al. Associations of the vaginal microbiota with HIV infection, bacterial vaginosis, and demographic factors. AIDS. 2017;31(7):895–904.
Ceccarani C, Foschi C, Parolin C, D’Antuono A, Gaspari V, Consolandi C, et al. Diversity of vaginal microbiome and metabolome during genital infections. Sci Rep. 2019;9(1):14095.
Acknowledgements
We received STI test kits from Cepheid (GeneXpert, Sunnyvale, CA, USA). The UCSD Microbiome Core performed sample extractions and library preparation utilizing protocols and primers published on the Earth Microbiome Project website.
Funding
This study was funded by Fogarty International (K01TW011187) and the Global Medicine Program at Massachusetts General Hospital. This publication includes data generated at the UC San Diego IGM Genomics Center utilizing an Illumina NovaSeq 6000 that was purchased with funding from a National Institutes of Health SIG grant (#S10 OD026929).
Author information
Authors and Affiliations
Contributions
DJD, HJ, and KL conceived the study. KL wrote the first version of the manuscript. FL provided statistical support for the design of the manuscript and performed the sequencing and statistical analysis. GA supervised the laboratory analytical procedures and validated the laboratory results. DN, DJD, and LM performed the study design, coordination, and data collection for the study. All authors contributed to the editing and approved the final paper.
Corresponding author
Ethics declarations
Ethics Approval
This study was part of the STIP (STI in pregnancy) study done in Cape Town, South Africa. Ethical approval and oversight were obtained from the Faculty of Health Sciences Human Research Ethics Committee at the University of Cape Town (#454/2017) and the University of California Los Angeles (#19–000237). All experiments were performed in accordance with the Declaration of Helsinki.
Consent to Participate
Written informed consent was obtained from all participants before enrollment. Study data were collected and managed using Research Electronic Data Capture (REDCap). All study data used a unique participant identifier allocated at study enrolment, and all electronic communications were done through password-protected, encrypted files.
Consent for Publication
All participants provided informed consent for the publication of de-identified data.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 1408 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, K.T., Li, F., Jaspan, H. et al. Changes in the Vaginal Microbiome During Pregnancy and the Postpartum Period in South African Women: a Longitudinal Study. Reprod. Sci. 31, 275–287 (2024). https://doi.org/10.1007/s43032-023-01351-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-023-01351-4