Abstract
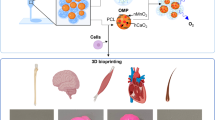
Brain tumors’ severity ranges from benign to highly aggressive and invasive. Bioengineering tools can assist in understanding the pathophysiology of these tumors from outside the body and facilitate development of suitable antitumoral treatments. Here, we first describe the physiology and cellular composition of brain tumors. Then, we discuss the development of three-dimensional tissue models utilizing brain tumor cells. In particular, we highlight the role of hydrogels in providing a biomimetic support for the cells to grow into defined structures. Microscale technologies, such as electrospinning and bioprinting, and advanced cellular models aim to mimic the extracellular matrix and natural cellular localization in engineered tumor tissues. Lastly, we review current applications and prospects of hydrogels for therapeutic purposes, such as drug delivery and co-administration with other therapies. Through further development, hydrogels can serve as a reliable option for in vitro modeling and treatment of brain tumors for translational medicine.

(Adapted from McNeill et al. [37]). b Multiple steps of metastatic colonization including pre-colonization phase, which occurs in minutes to hours, followed by colonization phase, which occurs in years. Pre-colonization steps include intravasation of cancer cells into the tumor vasculature, entry into the circulatory system, and extravasation into the parenchyma of target tissues or organs (Adapted from Massague et al. [40])

(Adapted from Mao et al. [52]). b The glioma perivascular niche. Vascular endothelial cells provide chemotactic signals to migrating glioma cells in order to attract them to blood vessels. GSCs may also migrate to the site and differentiate to multiple cell types due to signals in the PVN (Adapted from Diksin et al. [56])

(Adapted from Langhans et al. [58]). b Incorporation of brain glioblastoma spheroids within a microfluidic 3D culture platform of 96-well plates containing a tapered hole in the center of a rail for brain glioblastoma spheroids to generate angiogenic sprouting patterns (Adapted from Ko et al. [69]). c A 3D model generated by combination of transwell 96-well-plates and 96-well spheroid microplates to simulate penetration of anti-cancer drugs through the BBB (Adapted from Sherman et al. [71]). d Generation of brain organoids on a brain organoid-on-a-chip device to investigate the effect of nicotine on early brain development (Adapted from Wang et al. [74])

(Adapted from Monzo et al. [111]). b Aligned PCL nanofibers promote directional contact guidance to glioma cells seeded on their surface, while randomly oriented fibers produce non-specific cell populations on their surface (Adapted from Agudelo-Garcia et al. [76]). c Microfluidic devices are compartmentalized and consist of wells which allow for GBM cell aggregation as the flow of media provides nutrients as cells proliferate (Adapted from Fan et al. [21]). d Bioprinting extrudes of alginate/gelatin/fibrin gel which encapsulates cells and causes them to grow in distinct arrays (Adapted from Wang et al. [112])

(Adapted from Cha et al. [17])

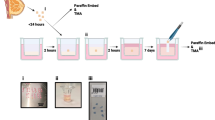
(Adapted from Li et al. [132] and Basso et al. [8]). b Insertion of a PCL/polyurethane carrier conduit containing aligned PCL nanofiber films, and cyclopamine (anti-cancer)-conjugated collagen hydrogel serving as an apoptotic tumor sink in the brain. Migration of tumor cells along the aligned films throughout the cross section of conduit was observed at different distances from the interface of the tumor in the brain (Adapted from Jain et al. [141]. c Stereotactical injection of drug-loaded magnetic hydrogel, and simultaneous magnetic resonance images of treated region over time by degradation of hydrogel and sustained release of drug (Adapted from Kim et al. [144])
Similar content being viewed by others
References
Lu QR, Qian L, Zhou X (2019) Developmental origins and oncogenic pathways in malignant brain tumors. Wiley Interdiscip Rev Dev Biol 8(4):e342
Madhusoodanan S, Opler MG, Moise D, Gordon J, Danan DM, Sinha A, Babu RP (2010) Brain tumor location and psychiatric symptoms: is there any association? A meta-analysis of published case studies. Expert Rev Neurother 10(10):1529–1536
Perkins A, Liu G (2016) Primary brain tumors in adults: diagnosis and treatment. Am Fam Physician 93(3):211–217
Lefranc F, Sadeghi N, Camby I, Metens T, Dewitte O, Kiss R (2006) Present and potential future issues in glioblastoma treatment. Expert Rev Anticancer Ther 6(5):719–732
Puente P, Fettig N, Luderer MJ, Jin A, Shah S, Muz B, Kapoor V, Goddu SM, Salama NN, Tsien C, Thotala D, Shoghi K, Rogers B, Azab AK (2018) Injectable hydrogels for localized chemotherapy and radiotherapy in brain tumors. J Pharm Sci 107(3):922–933
Stupp R, Hegi ME, Mason WP, van den Bent MJ, Taphoorn MJB, Janzer RC, Ludwin SK, Allgeier A, Fisher B, Belanger K, Hau P, Brandes AA, Gijtenbeek J, Marosi C, Vecht CJ, Mokhtari K, Wesseling P, Villa S, Eisenhauer E, Gorlia T, Weller M, Lacombe D, Cairncross JG, Mirimanoff R-O (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10:459–466
Stupp R, Mason WP, van den Bent MJ, Weller M (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996
Basso J, Miranda A, Nunes S, Cova T, Sousa J, Vitorino C, Pais A (2018) Hydrogel-based drug delivery nanosystems for the treatment of brain tumors. Gels. https://doi.org/10.3390/gels4030062
von Eckardstein KL, Reszka R, Kiwit JC (2005) Intracavitary chemotherapy (paclitaxel/carboplatin liquid crystalline cubic phases) for recurrent glioblastoma—clinical observations. J Neurooncol 74(3):305–309
Fourniols T, Randolph LD, Staub A, Vanvarenberg K, Leprince JG, Preat V, des Rieux A, Danhier F (2015) Temozolomide-loaded photopolymerizable PEG-DMA-based hydrogel for the treatment of glioblastoma. J Control Release 210:95–104
Ong BY, Ranganath SH, Lee LY, Lu F, Lee HS, Sahinidis NV, Wang CH (2009) Paclitaxel delivery from PLGA foams for controlled release in post-surgical chemotherapy against glioblastoma multiforme. Biomaterials 30(18):3189–3196
Ranganath SH, Kee I, Krantz WB, Chow PK, Wang CH (2009) Hydrogel matrix entrapping PLGA-paclitaxel microspheres: drug delivery with near zero-order release and implantability advantages for malignant brain tumour chemotherapy. Pharm Res 26(9):2101–2114
Westphal M, Hilt DC, Bortey E, Delavault P, Olivares R, Warnke PC, Whittle IR, Jääskeläinen J, Ram Z (2003) A phase 3 trial of local chemotherapy with biodegradable carmustine (BCNU) wafers (Gliadel wafers) in patients with primary malignant glioma. Neuro Oncol 5(2):79–88
Westphal M, Ram Z, Riddle V, Hilt D, Bortey E, Executive Committee of the Gliadel Study G (2006) Gliadel wafer in initial surgery for malignant glioma: long-term follow-up of a multicenter controlled trial. Acta Neurochir (Wien) 148(3):269–275
Attenello FJ, Mukherjee D, Datoo G, McGirt MJ, Bohan E, Weingart JD, Olivi A, Quinones-Hinojosa A, Brem H (2008) Use of Gliadel (BCNU) wafer in the surgical treatment of malignant glioma: a 10-year institutional experience. Ann Surg Oncol 15(10):2887–2893
Dai X, Ma C, Lan Q, Xu T (2016) 3D bioprinted glioma stem cells for brain tumor model and applications of drug susceptibility. Biofabrication 8:045005
Cha J, Kim P (2017) Biomimetic strategies for the glioblastoma microenvironment. Front Mater 4:45
Caliari SR, Burdick JA (2016) A practical guide to hydrogels for cell culture. Nat Methods 13(5):405–414
Chen JE, Pedron S, Harley BAC (2017) The combined influence of hydrogel stiffness and matrix-bound hyaluronic acid content on glioblastoma invasion. Macromol Biosci 17(8):1700018
Griffith LG, Swartz MA (2006) Capturing complex 3D tissue physiology in vitro. Nat Rev Mol Cell Biol 7(3):211–224
Fan Y, Nguyen DT, Akay Y, Xu F, Akay M (2016) Engineering a brain cancer chip for high-throughput drug screening. Sci Rep 6:25062
Lee JM, Seo HI, Bae JH, Chung BG (2017) Hydrogel microfluidic co-culture device for photothermal therapy and cancer migration. Electrophoresis 38(9–10):1318–1324
Sontheimer-Phelps A, Hassell BA, Ingber DE (2019) Modelling cancer in microfluidic human organs-on-chips. Nat Rev Cancer 19(2):65–81
Pinezich MR, Russell LN, Murphy NP, Lampe KJ (2018) Encapsulated oligodendrocyte precursor cell fate is dependent on PDGF-AA release kinetics in a 3D microparticle-hydrogel drug delivery system. J Biomed Mater Res A 106(9):2402–2411
Saludas L, Pascual-Gil S, Prosper F, Garbayo E, Blanco-Prieto M (2017) Hydrogel based approaches for cardiac tissue engineering. Int J Pharm 523(2):454–475
Wang C, Tong X, Yang F (2014) Bioengineered 3D brain tumor model to elucidate the effects of matrix stiffness on glioblastoma cell behavior using PEG-based hydrogels. Mol Pharm 11(7):2115–2125
Yang J, Sun X, Zhang Y, Chen Y (2020) The application of natural polymer–based hydrogels in tissue engineering. In: Chen Y (ed) Hydrogels based on natural polymers. Elsevier, Amsterdam, pp 273–307
Seliktar D (2012) Designing cell-compatible hydrogels for biomedical applications. Science 336(6085):1124–1128
Ananthanarayanan B, Kim Y, Kumar S (2011) Elucidating the mechanobiology of malignant brain tumors using a brain matrix-mimetic hyaluronic acid hydrogel platform. Biomaterials 32(31):7913–7923
Ulrich TA, Jain A, Tanner K, MacKay JL, Kumar S (2010) Probing cellular mechanobiology in three-dimensional culture with collagen-agarose matrices. Biomaterials 31(7):1875–1884
ter Horst B, Moiemen NS, Grover LM (2019) Natural polymers: biomaterials for skin scaffolds. In: Garcia-Gareta E (ed) Biomaterials for skin repair and regeneration. Elsevier, pp 151–192
Rape A, Ananthanarayanan B, Kumar S (2014) Engineering strategies to mimic the glioblastoma microenvironment. Adv Drug Deliv Rev 79–80:172–183
Xiao W, Ehsanipour A, Sohrabi A, Seidlits SK (2018) Hyaluronic-acid based hydrogels for 3-dimensional culture of patient-derived glioblastoma cells. J Vis Exp 138:58176
Kleihues P, Burger PC, Scheithauer BW (1993) The new WHO classification of brain tumours. Brain Pathol 3(3):255–268
Nayak L, Lee EQ, Wen PY (2012) Epidemiology of brain metastases. Curr Oncol Rep 14(1):48–54
Lukas L, Devos A, Suykens JA, Vanhamme L, Howe FA, Majos C, Moreno-Torres A, Van der Graaf M, Tate AR, Arus C, Van Huffel S (2004) Brain tumor classification based on long echo proton MRS signals. Artif Intell Med 31(1):73–89
McNeill KA (2016) Epidemiology of brain tumors. Neurol Clin 34(4):981–998
Cavalli FMG, Remke M, Rampasek L, Peacock J, Shih DJH, Luu B, Garzia L, Torchia J, Nor C, Morrissy AS, Agnihotri S, Thompson YY, Kuzan-Fischer CM, Farooq H, Isaev K, Daniels C, Cho BK, Kim SK, Wang KC, Lee JY, Grajkowska WA, Perek-Polnik M, Vasiljevic A, Faure-Conter C, Jouvet A, Giannini C, Nageswara Rao AA, Li KKW, Ng HK, Eberhart CG, Pollack IF, Hamilton RL, Gillespie GY, Olson JM, Leary S, Weiss WA, Lach B, Chambless LB, Thompson RC, Cooper MK, Vibhakar R, Hauser P, van Veelen MC, Kros JM, French PJ, Ra YS, Kumabe T, Lopez-Aguilar E, Zitterbart K, Sterba J, Finocchiaro G, Massimino M, Van Meir EG, Osuka S, Shofuda T, Klekner A, Zollo M, Leonard JR, Rubin JB, Jabado N, Albrecht S, Mora J, Van Meter TE, Jung S, Moore AS, Hallahan AR, Chan JA, Tirapelli DPC, Carlotti CG, Fouladi M, Pimentel J, Faria CC, Saad AG, Massimi L, Liau LM, Wheeler H, Nakamura H, Elbabaa SK, Perezpena-Diazconti M, Ponce Chico, de Leon F, Robinson S, Zapotocky M, Lassaletta A, Huang A, Hawkins CE, Tabori U, Bouffet E, Bartels U, Dirks PB, Rutka JT, Bader GD, Reimand J, Goldenberg A, Ramaswamy V, Taylor MD (2017) Intertumoral Heterogeneity within medulloblastoma subgroups. Cancer Cell 31(6):737–754, e736
Taylor MD, Poppleton H, Fuller C, Su X, Liu Y, Jensen P, Magdaleno S, Dalton J, Calabrese C, Board J, Macdonald T, Rutka J, Guha A, Gajjar A, Curran T, Gilbertson RJ (2005) Radial glia cells are candidate stem cells of ependymoma. Cancer Cell 8(4):323–335
Massague J, Obenauf AC (2016) Metastatic colonization by circulating tumour cells. Nature 529(7586):298–306
Bradshaw A, Wickremesekera A, Brasch HD, Chibnall AM, Davis PF, Tan ST, Itinteang T (2016) Cancer stem cells in glioblastoma multiforme. Front Surg 3:48
Rao JS (2003) Molecular mechanisms of glioma invasiveness: the role of proteases. Nat Rev Cancer 3(7):489–501
Gao YF, Zhu T, Chen J, Liu L, Ouyang R (2018) Knockdown of collagen alpha-1(III) inhibits glioma cell proliferation and migration and is regulated by miR128-3p. Oncol Lett 16(2):1917–1923
Mammoto T, Jiang A, Jiang E, Panigrahy D, Kieran MW, Mammoto A (2013) Role of collagen matrix in tumor angiogenesis and glioblastoma multiforme progression. Am J Pathol 183(4):1293–1305
Seano G (2018) Targeting the perivascular niche in brain tumors. Curr Opin Oncol 30(1):54–60
Cao Z, Bao M, Miele L, Sarkar FH, Wang Z, Zhou Q (2013) Tumour vasculogenic mimicry is associated with poor prognosis of human cancer patients: a systemic review and meta-analysis. Eur J Cancer 49(18):3914–3923
Charles N, Holland EC (2010) The perivascular niche microenvironment in brain tumor progression. Cell Cycle 9(15):3012–3021
Calabrese C, Poppleton H, Kocak M, Hogg TL, Fuller C, Hamner B, Oh EY, Gaber MW, Finklestein D, Allen M, Frank A, Bayazitov IT, Zakharenko SS, Gajjar A, Davidoff A, Gilbertson RJ (2007) A perivascular niche for brain tumor stem cells. Cancer Cell 11(1):69–82
Abbott NJ, Ronnback L, Hansson E (2006) Astrocyte-endothelial interactions at the blood-brain barrier. Nat Rev Neurosci 7(1):41–53
Das S, Marsden PA (2013) Angiogenesis in Glioblastoma. N Engl J Med 369(16):1561–1563
Sica G, Lama G, Anile C, Geloso MC, La Torre G, De Bonis P, Maira G, Lauriola L, Jhanwar-Uniyal M, Mangiola A (2010) Assessment of angiogenesis by CD105 and nestin expression in peritumor tissue of glioblastoma. Int J Oncol 38:41–49
Mao Y, Keller ET, Garfield DH, Shen K, Wang J (2013) Stromal cells in tumor microenvironment and breast cancer. Cancer Metastasis Rev 32(1–2):303–315
Chen W, Wang D, Du X, He Y, Chen S, Shao Q, Ma C, Huang B, Chen A, Zhao P, Qu X, Li X (2015) Glioma cells escaped from cytotoxicity of temozolomide and vincristine by communicating with human astrocytes. Med Oncol 32(3):43
Louveau A, Harris TH, Kipnis J (2015) Revisiting the mechanisms of CNS immune privilege. Trends Immunol 36(10):569–577
Louveau A, Smirnov I, Keyes TJ, Eccles JD, Rouhani SJ, Peske JD, Derecki NC, Castle D, Mandell JW, Lee KS, Harris TH, Kipnis J (2015) Structural and functional features of central nervous system lymphatic vessels. Nature 523(7560):337–341
Diksin M, Smith SJ, Rahman R (2017) The molecular and phenotypic basis of the glioma invasive perivascular niche. Int J Mol Sci 18(11):2342
Hopkins AM, DeSimone E, Chwalek K, Kaplan DL (2015) 3D in vitro modeling of the central nervous system. Prog Neurobiol 125:1–25
Langhans SA (2018) Three-dimensional in vitro cell culture models in drug discovery and drug repositioning. Front Pharmacol 9:6
Zhuang P, Sun AX, An J, Chua CK, Chew SY (2018) 3D neural tissue models: from spheroids to bioprinting. Biomaterials 154:113–133
Mansour AA, Goncalves JT, Bloyd CW, Li H, Fernandes S, Quang D, Johnston S, Parylak SL, Jin X, Gage FH (2018) An in vivo model of functional and vascularized human brain organoids. Nat Biotechnol 36(5):432–441
Palama IE, D’Amone S, Cortese B (2018) Microenvironmental rigidity of 3D scaffolds and influence on glioblastoma cells: a biomaterial design perspective. Front Bioeng Biotechnol 6:131
Qian X, Jacob F, Song MM, Nguyen HN, Song H, Ming GL (2018) Generation of human brain region-specific organoids using a miniaturized spinning bioreactor. Nat Protoc 13(3):565–580
Razian G, Yu Y, Ungrin M (2013) Production of large numbers of size-controlled tumor spheroids using microwell plates. J Vis Exp 81:e50665
Nath S, Devi GR (2016) Three-dimensional culture systems in cancer research: focus on tumor spheroid model. Pharmacol Ther 163:94–108
Engebraaten O, Bjerkvig R, Lund-Johansen M, Wester K, Pedersen P-H, Mork S, Backlund E-O, Laerum OD (1990) Interaction between human brain turnout biopsies and fetal rat brain tissue in vitro. Acta Neuropathol 81:130–140
Löhr M, Linsenmann T, Jawork A, Kessler AF, Timmermann N, Homola GA, Ernestus R-I, Hagemann C (2017) Implanting glioblastoma spheroids into rat brains and monitoring tumor growth by MRI volumetry. In: Zhang B (ed) RNAi and small regulatory RNAs in stem cells. Springer, pp 149–159
Jensen SS, Meyer M, Petterson SA, Halle B, Rosager AM, Aaberg-Jessen C, Thomassen M, Burton M, Kruse TA, Kristensen BW (2016) Establishment and characterization of a tumor stem cell-based glioblastoma invasion model. PLoS ONE 11(7):e0159746
Eisemann T, Costa B, Strelau J, Mittelbronn M, Angel P, Peterziel H (2018) An advanced glioma cell invasion assay based on organotypic brain slice cultures. BMC Cancer 18(1):103
Ko J, Ahn J, Kim S, Lee Y, Lee J, Park D, Jeon NL (2019) Tumor spheroid-on-a-chip: a standardized microfluidic culture platform for investigating tumor angiogenesis. Lab Chip 19(17):2822–2833
Quereda V, Hou S, Madoux F, Scampavia L, Spicer TP, Duckett D (2018) A cytotoxic three-dimensional-spheroid, high-throughput assay using patient-derived glioma stem cells. SLAS Discov 23(8):842–849
Sherman H, Rossi AE (2019) A novel three-dimensional glioma blood-brain barrier model for high-throughput testing of tumoricidal capability. Front Oncol 9:351
Linkous A, Balamatsias D, Snuderl M, Edwards L, Miyaguchi K, Milner T, Reich B, Cohen-Gould L, Storaska A, Nakayama Y, Schenkein E, Singhania R, Cirigliano S, Magdeldin T, Lin Y, Nanjangud G, Chadalavada K, Pisapia D, Liston C, Fine HA (2019) Modeling patient-derived glioblastoma with cerebral organoids. Cell Rep 26(12):3203–3211, e3205
Xiang Y, Tanaka Y, Cakir B, Patterson B, Kim K-Y, Sun P, Kang Y-J, Zhong M, Liu X, Patra P (2019) hESC-derived thalamic organoids form reciprocal projections when fused with cortical organoids. Cell Stem Cell 24(3):487–497
Wang Y, Wang L, Zhu Y, Qin J (2018) Human brain organoid-on-a-chip to model prenatal nicotine exposure. Lab Chip 18(6):851–860
Lancaster MA, Renner M, Martin CA, Wenzel D, Bicknell LS, Hurles ME, Homfray T, Penninger JM, Jackson AP, Knoblich JA (2013) Cerebral organoids model human brain development and microcephaly. Nature 501(7467):373–379
Agudelo-Garcia PA, De Jesus JK, Williams SP, Nowicki MO, Chiocca EA, Liyanarachchi S, Li PK, Lannutti JJ, Johnson JK, Lawler SE, Viapiano MS (2011) Glioma cell migration on three-dimensional nanofiber scaffolds is regulated by substrate topography and abolished by inhibition of STAT3 signaling. Neoplasia 13(9):831–840
Liu CJ, Shamsan GA, Akkin T, Odde DJ (2019) Glioma cell migration dynamics in brain tissue assessed by multimodal optical imaging. Biophys J 117(7):1179–1188
Li X, Su X (2018) Multifunctional smart hydrogels: potential in tissue engineering and cancer therapy. J Mater Chem B 6(29):4714–4730
Ostrovidov S, Sakai Y, Fujii T (2011) Integration of a pump and an electrical sensor into a membrane-based PDMS microbioreactor for cell culture and drug testing. Biomed Microdevices 13(5):847–864
Bastiancich C, Bianco J, Vanvarenberg K, Ucakar B, Joudiou N, Gallez B, Bastiat G, Lagarce F, Preat V, Danhier F (2017) Injectable nanomedicine hydrogel for local chemotherapy of glioblastoma after surgical resection. J Control Release 264:45–54
Zhao M, Danhier F, Bastiancich C, Joudiou N, Ganipineni LP, Tsakiris N, Gallez B, Rieux AD, Jankovski A, Bianco J, Preat V (2018) Post-resection treatment of glioblastoma with an injectable nanomedicine-loaded photopolymerizable hydrogel induces long-term survival. Int J Pharm 548(1):522–529
Blatchford DR, Quarrie LH, Tonner E, McCarthy C, Flint DJ, Wilde CJ (1999) Influence of microenvironment on mammary epithelial cell survival in primary culture. J Cell Physiol 181(2):304–311
Vepari C, Kaplan DL (2007) Silk as a biomaterial. Prog Polym Sci 32(8–9):991–1007
Lin C-C, Anseth KS (2009) PEG hydrogels for the controlled release of biomolecules in regenerative medicine. Pharm Res 26(3):631–643
Elliott JE, Macdonald M, Nie J, Bowman CN (2004) Structure and swelling of poly (acrylic acid) hydrogels: effect of pH, ionic strength, and dilution on the crosslinked polymer structure. Polymer 45(5):1503–1510
Noferini D, Faraone A, Rossi M, Mamontov E, Fratini E, Baglioni P (2019) Disentangling polymer network and hydration water dynamics in polyhydroxyethyl methacrylate physical and chemical hydrogels. J Phys Chem 123(31):19183–19194
Zhang YS, Khademhosseini A (2017) Advances in engineering hydrogels. Science 356(6337):eaaf3627
Rao SS, Lannutti JJ, Viapiano MS, Sarkar A, Winter JO (2014) Toward 3D biomimetic models to understand the behavior of glioblastoma multiforme cells. Tissue Eng Part B Rev 20(4):314–327
van Tellingen O, Yetkin-Arik B, de Gooijer MC, Wesseling P, Wurdinger T, de Vries HE (2015) Overcoming the blood-brain tumor barrier for effective glioblastoma treatment. Drug Resist Updat 19:1–12
Inal S, Hama A, Ferro M, Pitsalidis C, Oziat J, Iandolo D, Pappa A-M, Hadida M, Huerta M, Marchat D, Mailley P, Owens RM (2017) Conducting polymer scaffolds for hosting and monitoring 3D Cell culture. Adv Biosyst 1(6):1700052
ter Horst B, Moiemen NS, Grover LM (2019) Natural polymers. In: Garcia-Gareta E (ed) Biomaterials for skin repair and regeneration. pp 151–192
Xiao W, Sohrabi A, Seidlits SK (2017) Integrating the glioblastoma microenvironment into engineered experimental models. Future Sci OA 3(3):FSO189
Vashist A, Vashist A, Gupta Y, Ahmad S (2014) Recent advances in hydrogel based drug delivery systems for the human body. J Mater Chem B 2(2):147–166
Turabee MH, Jeong TH, Ramalingam P, Kang JH, Ko YT (2019) N, N, N-trimethyl chitosan embedded in situ Pluronic F127 hydrogel for the treatment of brain tumor. Carbohydr Polym 203:302–309
Oh Y, Cha J, Kang S-G, Kim P (2016) A polyethylene glycol-based hydrogel as macroporous scaffold for tumorsphere formation of glioblastoma multiforme. J Ind Eng Chem 39:10–15
Umesh V, Rape AD, Ulrich TA, Kumar S (2014) Microenvironmental stiffness enhances glioma cell proliferation by stimulating epidermal growth factor receptor signaling. PLoS ONE 9(7):e101771
Kaufman LJ, Brangwynne CP, Kasza K, Filippidi E, Gordon VD, Deisboeck T, Weitz D (2005) Glioma expansion in collagen I matrices: analyzing collagen concentration-dependent growth and motility patterns. Biophys J 89(1):635–650
Chippada U, Yurke B, Langrana NA (2010) Simultaneous determination of Young’s modulus, shear modulus, and Poisson’s ratio of soft hydrogels. J Mater Res 25(3):545–555
Vichare S, Sen S, Inamdar MM (2014) Cellular mechanoadaptation to substrate mechanical properties: contributions of substrate stiffness and thickness to cell stiffness measurements using AFM. Soft Matter 10(8):1174–1181
Heffernan JM, Overstreet DJ, Le LD, Vernon BL, Sirianni RW (2015) Bioengineered scaffolds for 3D analysis of glioblastoma proliferation and invasion. Ann Biomed Eng 43(8):1965–1977
Sunyer R, Jin AJ, Nossal R, Sackett DL (2012) Fabrication of hydrogels with steep stiffness gradients for studying cell mechanical response. PloS ONE 7(10):e46107
Chu C, Kong H (2012) Interplay of cell adhesion matrix stiffness and cell type for non-viral gene delivery. Acta Biomater 8(7):2612–2619
Kong HJ, Liu J, Riddle K, Matsumoto T, Leach K, Mooney DJ (2005) Non-viral gene delivery regulated by stiffness of cell adhesion substrates. Nat Mater 4(6):460–464
Subramanian A, Lin HY (2005) Crosslinked chitosan: its physical properties and the effects of matrix stiffness on chondrocyte cell morphology and proliferation. J Biomed Mater Res A 75(3):742–753
Park JS, Chu JS, Tsou AD, Diop R, Tang Z, Wang A, Li S (2011) The effect of matrix stiffness on the differentiation of mesenchymal stem cells in response to TGF-beta. Biomaterials 32(16):3921–3930
Paz AC, Soleas J, Poon JC, Trieu D, Waddell TK, McGuigan AP (2014) Challenges and opportunities for tissue-engineering polarized epithelium. Tissue Eng Part B Rev 20(1):56–72
Hughes JH, Ewy JM, Chen J, Wong SY, Tharp KM, Stahl A, Kumar S (2019) Transcriptomic analysis reveals that BMP4 sensitizes glioblastoma tumor-initiating cells to mechanical cues. Matrix Biol 85–86:112–127
Shah S, Sasmal PK, Lee K-B (2014) Photo-triggerable hydrogel–nanoparticle hybrid scaffolds for remotely controlled drug delivery. J Mater Chem B 2(44):7685–7693
Park GK, Kim S-H, Kim K, Das P, Kim B-G, Kashiwagi S, Choi HS, Hwang NSJT (2019) Dual-channel fluorescence imaging of hydrogel degradation and tissue regeneration in the brain. Theranostics 9(15):4255
Kim JI, Chun C, Kim B, Hong JM, Cho JK, Lee SH, Song SC (2012) Thermosensitive/magnetic poly(organophosphazene) hydrogel as a long-term magnetic resonance contrast platform. Biomaterials 33(1):218–224
Monzo P, Chong YK, Guetta-Terrier C, Krishnasamy A, Sathe SR, Yim EK, Ng WH, Ang BT, Tang C, Ladoux B, Gauthier NC, Sheetz MP (2016) Mechanical confinement triggers glioma linear migration dependent on formin FHOD3. Mol Biol Cell 27(8):1246–1261
Wang X, Li X, Dai X, Zhang X, Zhang J, Xu T, Lan Q (2018) Bioprinting of glioma stem cells improves their endotheliogenic potential. Colloids Surf B Biointerfaces 171:629–637
D’Arcangelo E, McGuigan AP (2015) Micropatterning strategies to engineer controlled cell and tissue architecture in vitro. Biotechniques 58(1):13–23
Azioune A, Storch M, Bornens M, Thery M, Piel M (2009) Simple and rapid process for single cell micro-patterning. Lab Chip 9:1640–1642
Thery M (2010) Micropatterning as a tool to decipher cell morphogenesis and functions. J Cell Sci 123(Pt 24):4201–4213
Endler EE, Nealey PF, Yin J (2005) Fidelity of micropatterned cell cultures. J Biomed Mater Res A 74(1):92–103
Guo Z, Hu K, Sun J, Zhang T, Zhang Q, Song L, Zhang X, Gu N (2014) Fabrication of hydrogel with cell adhesive micropatterns for mimicking the oriented tumor-associated extracellular matrix. ACS Appl Mater Interfaces 6(14):10963–10968
Huang Z-M, Zhang YZ, Kotaki M, Ramakrishna S (2003) A review on polymer nanofibers by electrospinning and their applications in nanocomposites. Compos Sci Technol 63(15):2223–2253
Long Y-Z, Yan X, Wang X-X, Zhang J, Yu M (2019) Electrospinning: the setup and procedure. In: Ding B, Wang X, Yu J (eds) Electrospinning: nanofabrication and applications, pp 21–52
Beliveau A, Thomas G, Gong J, Wen Q, Jain A (2016) Aligned nanotopography promotes a migratory state in glioblastoma multiforme tumor cells. Sci Rep 6:26143
Bagó JR, Pegna GJ, Okolie O, Mohiti-Asli M, Loboa EG, Hingtgen SD (2016) Electrospun nanofibrous scaffolds increase the efficacy of stem cell-mediated therapy of surgically resected glioblastoma. Biomaterials 90:116–125
Norouzi M (2018) Recent advances in brain tumor therapy: application of electrospun nanofibers. Drug Discov Today 23(4):912–919
Rao SS, Nelson MT, Xue R, DeJesus JK, Viapiano MS, Lannutti JJ, Sarkar A, Winter JO (2013) Mimicking white matter tract topography using core-shell electrospun nanofibers to examine migration of malignant brain tumors. Biomaterials 34(21):5181–5190
Brown JA, Pensabene V, Markov DA, Allwardt V, Neely MD, Shi M, Britt CM, Hoilett OS, Yang Q, Brewer BM, Samson PC, McCawley LJ, May JM, Webb DJ, Li D, Bowman AB, Reiserer RS, Wikswo JP (2015) Recreating blood-brain barrier physiology and structure on chip: a novel neurovascular microfluidic bioreactor. Biomicrofluidics 9(5):054124
Oddo A, Peng B, Tong Z, Wei Y, Tong WY, Thissen H, Voelcker NH (2019) Advances in microfluidic blood-brain barrier (BBB) models. Trends Biotechnol 37(12):1295–1314
Xu H, Li Z, Yu Y, Sizdahkhani S, Ho WS, Yin F, Wang L, Zhu G, Zhang M, Jiang L, Zhuang Z, Qin J (2016) A dynamic in vivo-like organotypic blood-brain barrier model to probe metastatic brain tumors. Sci Rep 6:36670
Terrell-Hall TB, Ammer AG, Griffith JI, Lockman PR (2017) Permeability across a novel microfluidic blood-tumor barrier model. Fluids Barriers CNS 14(1):3
Knowlton S, Onal S, Yu CH, Zhao JJ, Tasoglu S (2015) Bioprinting for cancer research. Trends Biotechnol 33(9):504–513
Lee VK, Dai G, Zou H, Yoo S-S (2015) Generation of 3-D glioblastoma-vascular niche using 3-D bioprinting. In: Paper presented at the 41st annual northeast biomedical engineering conference (NEBEC), Troy, NY, USA
Ostrom QT, Gittleman H, Xu J, Kromer C, Wolinsky Y, Kruchko C, Barnholtz-Sloan JS (2016) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2009–2013. Neuro Oncol 18(suppl_5):v1–v75
Su J, Hu BH, Lowe WL Jr, Kaufman DB, Messersmith PB (2010) Anti-inflammatory peptide-functionalized hydrogels for insulin-secreting cell encapsulation. Biomaterials 31(2):308–314
Li J, Mooney DJ (2016) Designing hydrogels for controlled drug delivery. Nat Rev Mater 1:16071
Alarcin E, Lee TY, Karuthedom S, Mohammadi M, Brennan MA, Lee DH, Marrella A, Zhang J, Syla D, Zhang YS, Khademhosseini A, Jang HL (2018) Injectable shear-thinning hydrogels for delivering osteogenic and angiogenic cells and growth factors. Biomater Sci 6(6):1604–1615
Avery RK, Albadawi H, Akbari M, Zhang YS, Duggan MJ, Sahani DV, Olsen BD, Khademhosseini A, Oklu R (2016) An injectable shear-thinning biomaterial for endovascular embolization. Sci Transl Med 8:1–12
Gaharwar AK, Avery RK, Assmann A, Paul A, McKinley GH, Khademhosseini A, Olsen BD (2014) Shear-thinning nanocomposite hydrogels for the treatment of hemorrhage. ACS Nano 8(10):9833–9842
Castro Dias M, Mapunda JA, Vladymyrov M, Engelhardt B (2019) Structure and junctional complexes of endothelial, epithelial and glial brain barriers. Int J Mol Sci 20(21):5372
Obermeier B, Daneman R, Ransohoff RM (2013) Development, maintenance and disruption of the blood-brain barrier. Nat Med 19(12):1584–1596
Vishnubhakthula S, Elupula R, Duran-Lara EF (2017) Recent advances in hydrogel-based drug delivery for melanoma cancer therapy: a mini review. J Drug Deliv 2017:7275985
Torres AJ, Zhu C, Shuler ML, Pannullo S (2011) Paclitaxel delivery to brain tumors from hydrogels: a computational study. Biotechnol Prog 27(5):1478–1487
Bastiancich C, Danhier P, Preat V, Danhier F (2016) Anticancer drug-loaded hydrogels as drug delivery systems for the local treatment of glioblastoma. J Control Release 243:29–42
Jain A, Betancur M, Patel GD, Valmikinathan CM, Mukhatyar VJ, Vakharia A, Pai SB, Brahma B, MacDonald TJ, Bellamkonda RV (2014) Guiding intracortical brain tumour cells to an extracortical cytotoxic hydrogel using aligned polymeric nanofibres. Nat Mater 13(3):308–316
Ozeki T, Hashizawa K, Kaneko D, Imai Y, Okada H (2010) Treatment of rat brain tumors using sustained-release of camptothecin from poly(lactic-co-glycolic acid) microspheres in a thermoreversible hydrogel. Chem Pharm Bull 58(9):1142–1147
Tyler B, Wadsworth S, Recinos V, Mehta V, Vellimana A, Li K, Rosenblatt J, Do H, Gallia GL, Siu IM, Wicks RT, Rudek MA, Zhao M, Brem H (2011) Local delivery of rapamycin: a toxicity and efficacy study in an experimental malignant glioma model in rats. Neuro Oncol 13(7):700–709
Kim JI, Kim B, Chun C, Lee SH, Song SC (2012) MRI-monitored long-term therapeutic hydrogel system for brain tumors without surgical resection. Biomaterials 33(19):4836–4842
Akhtar A (2015) The flaws and human harms of animal experimentation. Camb Q Healthc Ethics 24(4):407–419
Ashby LS, Smith KA, Stea B (2016) Gliadel wafer implantation combined with standard radiotherapy and concurrent followed by adjuvant temozolomide for treatment of newly diagnosed high-grade glioma: a systematic literature review. World J Surg Oncol 14(1):225
Menei P, Capelle L, Guyotat J, Fuentes S, Assaker R, Bataille B, Francois P, Dorwling-Carter D, Paquis P, Bauchet L, Parker F, Sabatier J, Faisant N, Benoit JP (2005) Local and sustained delivery of 5-fluorouracil from biodegradable microspheres for the radiosensitization of malignant glioma: a randomized phase II trial. Neurosurgery 56(2):242–248
Menei P, Jadaud E, Faisant N, Boisdron-Celle M, Michalak S, Fournier D, Delhaye M, Benoit JP (2004) Stereotaxic implantation of 5-fluorouracil-releasing microspheres in malignant glioma. Cancer 100(2):405–410
Pereira EAC, Grandidge CA, Nowak VA, Cudlip SA (2017) Cerebrospinal fluid leaks after transsphenoidal surgery—effect of a polyethylene glycol hydrogel dural sealant. J Clin Neurosci 44:6–10
Boogaarts JD, Grotenhuis JA, Bartels RH, Beems T (2005) Use of a novel absorbable hydrogel for augmentation of dural repair: results of a preliminary clinical study. Neurosurgery 57(1 Suppl):146–151
Kinaci A, Algra A, Heuts S, O’Donnell D, van der Zwan A, van Doormaal T (2018) Effectiveness of dural sealants in prevention of cerebrospinal fluid leakage after craniotomy: a systematic review. World Neurosurg 118(368–376):e361
Zanotto-Filho A, Braganhol E, Klafke K, Figueiro F, Terra SR, Paludo FJ, Morrone M, Bristot IJ, Battastini AM, Forcelini CM, Bishop AJR, Gelain DP, Moreira JCF (2015) Autophagy inhibition improves the efficacy of curcumin/temozolomide combination therapy in glioblastomas. Cancer Lett 358(2):220–231
Kotteas EA, Syrigos KN, Saif MW (2016) Profile of capecitabine/temozolomide combination in the treatment of well-differentiated neuroendocrine tumors. Onco Targets Ther 9:699–704
Owen DH, Alexander AJ, Konda B, Wei L, Hemminger JA, Schmidt CR, Abdel-Misih SR, Dillhoff ME, Sipos JA, Kirschner LS (2017) Combination therapy with capecitabine and temozolomide in patients with low and high grade neuroendocrine tumors, with an exploratory analysis of O6-methylguanine DNA methyltransferase as a biomarker for response. Oncotarget 8(61):104046
Ramirez RA, Boudreaux JP, Wang Y-Z, Beyer DT, Woltering E (2015) Combination capecitabine/temozolomide (CAPTEM) in patients with neuroendocrine tumors (NETs): a single institution review. J Clin Oncol 33(156):e15184–e15184
Quinn JA, Jiang SX, Reardon DA, Desjardins A, Vredenburgh JJ, Rich JN, Gururangan S, Friedman AH, Bigner DD, Sampson JH, McLendon RE, Herndon JE 2nd, Walker A, Friedman HS (2009) Phase II trial of temozolomide plus o6-benzylguanine in adults with recurrent, temozolomide-resistant malignant glioma. J Clin Oncol 27(8):1262–1267
Rahman CV, Smith SJ, Morgan PS, Langmack KA, Clarke PA, Ritchie AA, Macarthur DC, Rose FR, Shakesheff KM, Grundy RG, Ruman R (2013) Adjuvant chemotherapy for brain tumors delivered via a novel intra-cavity moldable polymer matrix. PLoS ONE 8(10):e77435
Acknowledgements
The authors have no competing interests. The authors also acknowledge funding from the National Institutes of Health (1U01CA214411-01A1).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
This study does not contain any studies with human or animal subjects performed by any of the authors.
Rights and permissions
About this article
Cite this article
Thakor, J., Ahadian, S., Niakan, A. et al. Engineered hydrogels for brain tumor culture and therapy. Bio-des. Manuf. 3, 203–226 (2020). https://doi.org/10.1007/s42242-020-00084-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42242-020-00084-6