Abstract
Purpose
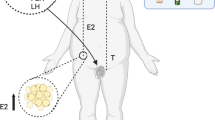
Hypercholesterolemia due to a high-cholesterol diet is linked to numerous diseases and may lead to male infertility. However, the underlying mechanism remains unknown. The maintenance of male fertility requires intact testicular structures (including seminiferous tubules and mesenchyme) and functioning cells (Leydig cells, Sertoli cells and germ cells, etc.), production of appropriate concentrations of sex hormones, and cooperation among testicular cells. Thus, we considered whether male fertility declined as the structure and function of testicular cells were altered in rats on a high-cholesterol diet.
Methods
Male Sprague Dawley rats were fed either a standard or a high-cholesterol diet for 16 weeks. Serum sex hormones, lipid components, semen quality, and fertility rate were assayed in the rats. The 3β-hydroxysteroid dehydrogenase (3β-HSD), Wilms tumor 1 (WT-1), and deleted in azoospermia-like (DAZL) were regarded as specific markers of Leydig, Sertoli, and germ cells in rats. In addition, the ultrastructure of the testis and expression levels of particular marker molecules of testicular cells were further investigated.
Results
Compared to rats fed on a regular diet, the serum testosterone levels and sperm progressive motility decreased in rats fed high cholesterol. Moreover, we observed a deformed nucleus, dilated smooth endoplasmic reticulum, and swollen mitochondria of Leydig cells and a schizolytic nucleus of Sertoli cells in rats on a high-cholesterol diet. The 3β-HSD, WT-1, and DAZL protein expression levels were significantly reduced in rats on a high-cholesterol diet.
Conclusions
Our results showed that a high-cholesterol diet adversely affected testosterone production and sperm progressive motility, possibly due to Leydig, Sertoli, and germ cell abnormalities.




Similar content being viewed by others
Data Availability
The datasets generated and analyzed during the current study are not publicly available but are available from the corresponding author on reasonable request.
Abbreviations
- StAR:
-
steroidogenic acute regulatory protein
- 3β-HSD:
-
3β-hydroxysteroid dehydrogenase
- WT-1:
-
Wilms tumor gene
- DAZL:
-
deleted in azoospermia-like
- ND:
-
normal diet
- HC:
-
high-cholesterol diet
- SSA:
-
surplus semen analysis
- PR:
-
progressive motility
- NP:
-
non-progressive motility
- IM:
-
immobility
- TG:
-
triacylglycerol
- TC:
-
total cholesterol
- LDL-C:
-
low-density lipoprotein cholesterol
- HDL-C:
-
high-density lipoprotein cholesterol
- LH:
-
luteinizing hormone
- FSH:
-
follicle stimulating hormone
- ELISA:
-
enzyme-linked immunosorbent assay
- TBST:
-
Tris-buffered saline containing 0.1% Tween 20
- SEM:
-
standard error of mean
- HPG:
-
hypothalamic–pituitary–gonadal
References
Sharlip ID, Jarow JP, Belker AM, Lipshultz LI, Sigman M, Thomas AJ, Schlegel PN, Howards SS, Nehra A, Damewood MD, Overstreet JW, Sadovsky R (2002) Best practice policies for male infertility. Fertil Steril 77(5):873–882. https://doi.org/10.1016/s0015-0282(02)03105-9
Eslamian G, Amirjannati N, Rashidkhani B, Sadeghi MR, Hekmatdoost A (2012) Intake of food groups and idiopathic asthenozoospermia: a case-control study. Hum Reprod 27(11):3328–3336. https://doi.org/10.1093/humrep/des311
Giahi L, Mohammadmoradi S, Javidan A, Sadeghi MR (2016) Nutritional modifications in male infertility: a systematic review covering 2 decades. Nutr Rev 74(2):118–130. https://doi.org/10.1093/nutrit/nuv059
Hayden RP, Flannigan R, Schlegel PN (2018) The role of lifestyle in male infertility: diet, physical activity, and body habitus. Curr Urol Rep 19(7):56. https://doi.org/10.1007/s11934-018-0805-0
Lecerf JM, de Lorgeril M (2011) Dietary cholesterol: from physiology to cardiovascular risk. Br J Nutr 106(1):6–14. https://doi.org/10.1017/S0007114511000237
Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Blaha MJ, Dai S, Ford ES, Fox CS, Franco S, Fullerton HJ (2014) Heart disease and stroke statistics--2014 update: a report from the American Heart Association. Circulation 129(3):e28–e292. https://doi.org/10.1161/01.cir.0000441139.02102.80
Kleemann R, Verschuren L, van Erk MJ, Nikolsky Y, Cnubben NH, Verheij ER, Smilde AK, Hendriks HF, Zadelaar S, Smith GJ, Kaznacheev V, Nikolskaya T, Melnikov A, Hurt-Camejo E, van der Greef J, van Ommen B, Kooistra T (2007) Atherosclerosis and liver inflammation induced by increased dietary cholesterol intake: a combined transcriptomics and metabolomics analysis. Genome Biol 8(9):R200. https://doi.org/10.1186/gb-2007-8-9-r200
Tous M, Ferré N, Camps J, Riu F, Joven J (2005) Feeding apolipoprotein E-knockout mice with cholesterol and fat enriched diets may be a model of non-alcoholic steatohepatitis. Mol Cell Biochem 268(1-2):53–58. https://doi.org/10.1007/s11010-005-2997-0
Hu J, La Vecchia C, de Groh M, Negri E, Morrison H, Mery L, Canadian Cancer Registries Epidemiology Research Group (2012) Dietary cholesterol intake and cancer. Ann Oncol 23(2):491–500. https://doi.org/10.1093/annonc/mdr155
Fernández-Cabada T, Ramos-Gómez M (2019) A novel contrast agent based on magnetic nanoparticles for cholesterol detection as Alzheimer’s disease biomarker. Nanoscale Res Lett 14(1):36. https://doi.org/10.1186/s11671-019-2863-8
Yu C, Jiang F, Zhang M, Luo D, Shao S, Zhao J, Gao L, Zuo C, Guan Q (2019) HC diet inhibited testosterone synthesis by activating endoplasmic reticulum stress in testicular Leydig cells. J Cell Mol Med 23(5):3140–3150. https://doi.org/10.1111/jcmm.14143
Morgan DH, Ghribi O, Hui L, Geiger JD, Chen X (2014) Cholesterol-enriched diet disrupts the blood-testis barrier in rabbits. Am J Physiol Endocrinol Metab 307(12):E1125–E1130. https://doi.org/10.1152/ajpendo.00416.2014
Saez Lancellotti TE, Boarelli PV, Monclus MA, Cabrillana ME, Clementi MA, Espínola LS, Cid Barría JL, Vincenti AE, Santi AG, Fornés MW (2010) Hypercholesterolemia impaired sperm functionality in rabbits. PloS One 5(10):e13457. https://doi.org/10.1371/journal.pone.0013457
Oduwole OO, Huhtaniemi IT, Misrahi M (2021) The roles of luteinizing hormone, follicle-stimulating hormone and testosterone in spermatogenesis and folliculogenesis revisited. Int J Mol Sci 22(23):12735. https://doi.org/10.3390/ijms222312735
Neto FT, Bach PV, Najari BB, Li PS, Goldstein M (2016) Spermatogenesis in humans and its affecting factors. Semin Cell Dev Biol 59:10–26. https://doi.org/10.1016/j.semcdb.2016.04.009
Juul A, Skakkebaek NE (2002) Testosterone treatment of elderly men. The so called andropause doesn’t exist. Ugeskr Laeger 164(42):4941–4942
Sharpe RM, McKinnell C, Kivlin C, Fisher JS (2003) Proliferation and functional maturation of Sertoli cells, and their relevance to disorders of testis function in adulthood. Reproduction (Cambridge, England) 125(6):769–784. https://doi.org/10.1530/rep.0.1250769
Zirkin BR, Papadopoulos V (2018) Leydig cells: formation, function, and regulation. Biol Reprod 99(1):101–111. https://doi.org/10.1093/biolre/ioy059
Wang XN, Li ZS, Ren Y, Jiang T, Wang YQ, Chen M, Zhang J, Hao JX, Wang YB, Sha RN, Huang Y (2013) The Wilms tumor gene, Wt1, is critical for mouse spermatogenesis via regulation of Sertoli cell polarity and is associated with non-obstructive azoospermia in humans. PLoS Genet 9(8):e1003645. https://doi.org/10.1371/journal.pgen.1003645
Collier B, Gorgoni B, Loveridge C, Cooke HJ, Gray NK (2005) The DAZL family proteins are PABP-binding proteins that regulate translation in germ cells. EMBO J 24(14):2656–2666. https://doi.org/10.1038/sj.emboj.7600738
Jung HJ, Song H, Yoon MJ (2014) Stage-dependent DAZL localization in stallion germ cells. Anim Reprod Sci 147(1-2):32–38. https://doi.org/10.1016/j.anireprosci.2014.03.011
Lin YM, Chen CW, Sun HS, Tsai SJ, Hsu CC, Teng YN, Lin JS, Kuo PL (2001) Expression patterns and transcript concentrations of the autosomal DAZL gene in testes of azoospermic men. Mol Hum Reprod 7(11):1015–1022. https://doi.org/10.1093/molehr/7.11.1015
Kuo PL, Wang ST, Lin YM, Lin YH, Teng YN, Hsu CC (2004) Expression profiles of the DAZ gene family in human testis with and without spermatogenic failure. Fertil Steril 81(4):1034–1040. https://doi.org/10.1016/j.fertnstert.2003.08.047
Saunders PT, Turner JM, Ruggiu M, Taggart M, Burgoyne PS, Elliott D, Cooke HJ (2003) Absence of mDazl produces a final block on germ cell development at meiosis. Reproduction (Cambridge, England) 126(5):589–597. https://doi.org/10.1530/rep.0.1260589
Bataineh HN, Nusier MK (2005) Effect of cholesterol diet on reproductive function in male albino rats. Saudi Med J 26(3):398–404
Ibrahim HA, Zhu Y, Wu C, Lu C, Ezekwe MO, Liao SF, Huang K (2012) Selenium-enriched probiotics improves murine male fertility compromised by high fat diet. Biol Trace Elem Res 147(1-3):251–260. https://doi.org/10.1007/s12011-011-9308-2
Ouvrier A, Alves G, Damon-Soubeyrand C, Marceau G, Cadet R, Janny L, Brugnon F, Kocer A, Pommier A, Lobaccaro JM, Drevet JR, Saez F (2011) Dietary cholesterol-induced post-testicular infertility. PloS one 6(11):e26966. https://doi.org/10.1371/journal.pone.0026966
Sharma RK, Agarwal A (1996) Role of reactive oxygen species in male infertility. Urology 48(6):835–850. https://doi.org/10.1016/s0090-4295(96)00313-5
Rao B, Soufir JC, Martin M, David G (1989) Lipid peroxidation in human spermatozoa as related to midpiece abnormalities and motility. Gamete Res 24(2):127–134. https://doi.org/10.1002/mrd.1120240202
Kumanov P, Nandipati K, Tomova A, Agarwal A (2006) Inhibin B is a better marker of spermatogenesis than other hormones in the evaluation of male factor infertility. Fertil Steril 86(2):332–338. https://doi.org/10.1016/j.fertnstert.2006.01.022
Fijak M, Bhushan S, Meinhardt A (2011) Immunoprivileged sites: the testis. Methods Mol Biol 677:459–470. https://doi.org/10.1007/978-1-60761-869-0_29
Zhang J, Li K, Yuan M, Zhang J, Huang G, Ao J, Tan H, Li Y, Gong D, Li J, Kang L, An N, Li F, Lin P, Huang L (2017) A high-fat diet impairs reproduction by decreasing the IL1β level in mice treated at immature stage. Sci Rep 7(1):567. https://doi.org/10.1038/s41598-017-00505-0
Steinfeld K, Beyer D, Mühlfeld C, Mietens A, Eichner G, Altinkilic B, Kampschulte M, Jiang Q, Krombach GA, Linn T, Weidner W, Middendorff R (2018) Low testosterone in ApoE/LDL receptor double-knockout mice is associated with rarefied testicular capillaries together with fewer and smaller Leydig cells. Sci Rep 8(1):5424. https://doi.org/10.1038/s41598-018-23631-9
Hasanein P, Fazeli F, Parviz M, Roghani M (2018) Ferulic acid prevents lead-induced testicular oxidative stress and suppressed spermatogenesis in rats. Andrologia 50(1):e12798. https://doi.org/10.1111/and.12798
Lee KH, Lee S, Kim B, Chang S, Kim SW, Paick JS, Rhee K (2006) Dazl can bind to dynein motor complex and may play a role in transport of specific mRNAs. EMBO J 25(18):4263–4270. https://doi.org/10.1038/sj.emboj.7601304
Funding
This work was supported by the National Natural Science Foundation of China (82270839 and 81770860) and Key Research and Development Plan of Shandong Province (2017CXGC1214).
Author information
Authors and Affiliations
Contributions
Luna Liu was involved in the writing of the manuscript, performed part of the experiments, and contributed to the revision of the manuscript. Meijie Zhang and Fangjie Jiang conducted part of the experiments. Dandan Luo, Shuang Liu, Yu Su, and Qingbo Guan contributed to feeding the rats and analyzing the data. Chunxiao Yu designed the study and directed the project. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All animal protocols and procedures were approved by the Animal Ethics Committee of Shandong Provincial Hospital and performed according to the Shandong Provincial Hospital Animal Care and Use Committee.
Consent for publication
All authors read and approved the final manuscript.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, L., Zhang, M., Jiang, F. et al. High cholesterol diet–induced testicular dysfunction in rats. Hormones 22, 685–694 (2023). https://doi.org/10.1007/s42000-023-00472-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42000-023-00472-4