Abstract
Currently, only a few theoretical support systems exist for the treatment of hyperthyroidism. They are typically not practically applicable and solely focus on Graves’ disease. The recently developed DigiThy software framework can be used to assist physicians for methimazole dose titration during the treatment of Graves’ disease. In this study, a pool of 60 virtual patients was created to compare physicians’ individual treatment approaches by 8 different physicians and students (including three colleagues, unexperienced with care of Graves’ disease) with the decision support system DigiThy in terms of already defined performance indices. These indices are used to assess the deviation of FT4 from the reference range throughout the treatment. The computer aided treatment algorithms outperformed the usual care approach according to different prespecified criteria for treatment success. Two out of the three unexperienced colleagues improved their treatment success over time, i.e. with more patients treated. In conclusion, our findings suggest that the DigiThy software may be a useful tool for use as a decision support system in routine care of patients with Graves’ disease, while also serving as an effective training tool for the education of physicians. Randomized controlled studies are required before implementation of DigiThy in daily clinical practice.
Zusammenfassung
Derzeit gibt es nur wenige theoretische Decision-Support-Systeme für die Behandlung der Hyperthyreose. Sie sind in der Regel nicht praktisch anwendbar und konzentrieren sich ausschließlich auf Morbus Basedow. Das kürzlich entwickelte DigiThy-Software-Framework kann Ärzte bei der Festlegung der Methimazol-Dosis während der Behandlung von Morbus Basedow unterstützen. In dieser Studie wurde ein Pool von 60 virtuellen Patienten erstellt, um die individuellen Behandlungsansätze von 8 verschiedenen Ärzten und Studenten (darunter drei Kollegen, die keine Erfahrung mit der Behandlung von Morbus Basedow haben) mit dem Recommender System DigiThy im Hinblick auf bereits definierte Performance-Indizes zu vergleichen. Diese Indizes werden verwendet, um die Abweichung von FT4 vom Referenzbereich während der Behandlung zu bewerten. Die computergestützten Behandlungsalgorithmen übertrafen die Usual-Care Behandlung nach verschiedenen vordefinierten Kriterien für den Behandlungserfolg. Zwei der drei unerfahrenen Kollegen verbesserten ihren Behandlungserfolg im Laufe der Zeit, d. h. mit zunehmender Zahl der behandelten Patienten. Unsere Ergebnisse deuten darauf hin, dass die DigiThy-Software ein nützliches Instrument für den Einsatz als Decision-Support-System in der Routineversorgung von Patienten mit Morbus Basedow sein kann und gleichzeitig als wirksames Schulungsinstrument für die Ausbildung von Ärzten dient. Vor dem Einsatz von DigiThy in der täglichen klinischen Praxis sind randomisierte kontrollierte Studien erforderlich.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Relevance
About 20 to 30 persons out of 100,000 of the population suffer annually from Graves’ disease, an autoimmune disease affecting the thyroid gland [1, p. 430]. Women are usually more frequently affected and have a lifetime risk of 3%, while men have a lifetime risk of 0.5%. Graves’ disease is also the main cause of hyperthyroidism [2].
This study will therefore focus on support systems made for the treatment of Graves’ disease.
Introduction to Graves’ Disease
In the case of Graves’ disease thyroid-stimulating antibodies produce an overactive thyroid behavior. The antibodies bind to the thyrotropin (TSH) receptor and activate it [3, p. 1236]. Due to this stimulation by TSH receptor antibodies (TRAb), hyperthyroidism often develops as the main consequence [4, p. 373]. The majority of studies on Graves’ disease only determine TRAb antibodies in general, without further distinguishing between stimulating and blocking ones. However, “antibodies against the thyroid-stimulating hormone receptor (TSHR) can activate or block the function of the receptor directly causing hyper- or hypothyroidism, respectively” [1, p. 58]. In patients with Graves’ disease, the stimulating antibodies (TSAb) are detected with a probability of over 95% [1, p. 438]. Given that Graves’ disease is the primary cause of hyperthyroidism, it can generally be assumed that the stimulating antibodies are significantly more prevalent, and thus the blocking antibodies (TSBAb) can usually be neglected.
Difficulties due to antibody measurement and lack of data
In everyday clinical practice, no distinction is typically made between the two types of antibodies, and their quantities are measured collectively. This introduces an element of uncertainty in the development and validation of mathematical models [5]. Such mathematical models typically serve as the foundation for the development of support systems, as will be demonstrated later in this article. Studies that explicitly deal with the distinction between antibodies are scarce, but would be very helpful for many approaches. In this context, [6], it was confirmed that most patients have stimulating antibodies and only few have blocking ones. However, it was also shown that two out of 98 patients underwent a complete transition from TSAb-positive hyperthyroidism to TSBAb-positive hypothyroidism. It is likely that the quality of recommendation systems for hyperthyroidism therapy could be improved if it would become standard practice to measure antibodies at each visit and distinguish between their characteristics, since support systems heavily rely on measured blood values and estimate their influence on the further development of the disease. In general, the data quality often complicates the utilization and development of support systems. Based on the experience with data from the Graz Endocrinology Registry Study, as well as data from publications by others [7, 8], it can be stated that the available evidence on this issue is limited, which makes the verification and development of models challenging. In one registry study, for example, antibodies were often not measured, but TSH, FT3 and FT4 were measured each time, while in another investigation [7], units were mixed up, extreme time intervals between treatments occurred, and the appointments were not recorded precisely by date. Additionally, it was sometimes only noted in which month a patient visited the clinic. Furthermore in another study [8], only data restricted to the FT4 values were published.
Difficulties in treatment due to high individuality of patients
One of the reasons why the treatment of thyroid diseases is challenging is that the HPT-axis has a highly individual “healthy setpoint” varying significantly from patient to patient [9]. In one study [9], sixteen healthy patients were investigated to demonstrate how much the normal concentrations of FT3, T4, FT4 and TSH differ between individuals. Moreover, these values change over time, even for the individuals themselves, albeit to a lesser extent [9]. Due to the strong inter-individuals variability, the ultimate goal proposed [9] is to determine the individual setpoint of a person on the basis of genetic analyses and thus aim for personalized medicine. Support systems based on control engineering methods, as in [5] and [10], can also allow individualization of the treatment by setting the targeted hormone concentration setpoint via the control variable. In summary, the individual variability of the disease process represents the greatest challenge not only for standard care treatment but also for decision support systems.
State of the art of support systems
Guidelines
Recommendations from professional medical organizations can be interpreted as a simple form of support system. However, few are available and doctors mostly have to rely on their personal experiences regarding dose titration. Among the limited specific recommendations for the treatment of Graves’ disease, one is provided by the American Thyroid Association, suggesting
”5–10 mg if free T4 is 1–1.5 times the upper limit of normal; 10–20 mg for free T4 1.5–2 times the upper limit of normal; and 30–40 mg for free T4 2–3 times the upper limit of normal” [11, p. 1355].
This recommendation assigns suggested dosages to different FT4 intervals and is shown graphically in Fig. 1. This plot highlights that the suggested dosing at 48.0 pmol L\({}^{-1}\) may be non-practicable. If one were to adhere strictly to the recommendation, a patient with 47.9 pmol L\({}^{-1}\) would be prescribed 20 mg MMI, while a patient with 48.1 pmol L\({}^{-1}\) would receive a prescription for 30 mg. The measurement of FT4 is strongly dependent on the measurement method. For instance, in one study [12] the FT4 values of the same patients, measured by using two different methods, correlated only with a Spearman correlation coefficient of \(r=0.75\). If the underlying measurement of FT4 is subject to such uncertainty, the discontinuity in dosage at 48.0 pmol L\({}^{-1}\) seems unjustified and inconsistent.
Computer aided support systems
For more advanced computer-aided support systems, a mathematical model is usually required. In order to be able to assess what support systems for hyperthyroidism therapy can already achieve, it is important to assess how well the disease can be described mathematically.
Dietrich et al provides a detailed overview of methods for the mathematical description of the HPT-axis [14]. However, it is mentioned that only a few mathematical models are actually used in clinics [14]. Many of the models do not consider the antibodies that lead to Graves’ disease [15, 16]. Both models showed in [15, 16] are highly sophisticated, using a large number of differential equations and patient specific parameters to model thyroid behavior. Due to the high number of parameters, these models are primarily evaluated qualitatively rather than quantitatively, since tuning numerous parameters present challenges in validation with real patient data. If the number of observations, i.e., blood measurements at a single appointment, is smaller than the number of model parameters, generally one encounters many possible solutions for patient-specific model parameters [17]. This, in turn, renders support systems unable to accurately predict future hormone development. Given the significant intra-individual variability among patients and the sporadic measurement of blood parameters—usually performed every few weeks—it is impractical to employ models with dozens of internal patient parameters as clinical support systems.
Nevertheless, it must be noted that these complex models provide an important insight into the disease process and can reflect various disease patterns. For instance, one study [10] demonstrates a possible treatment for Graves’ disease using the drug methimazole, administered by a model predictive controller (MPC). The disease process could be modelled using the model shown in the supplementary material of [18], which builds upon the preliminary work of [15, 19, 20]. Although the antibodies that cause Graves’ disease are not directly present in the model, the disease process can still be simulated by adjusting parameters such as secretion capacity and introducing a relationship between methimazole and the activity of TPO [10]. This makes that study [10] one of the few sources proposing a support system for treating Graves’ disease. Unfortunately, it is stated in [10] that this support system can only be used if the hormone concentrations can be measured daily, if the results of the measurements are available immediately and if all states of the model can be measured. Moreover, for this type of MPC, the individual patient parameters would also need to be known. Consequently, the practical application of this support system currently remains not feasible for use in clinical routine.
Another model describing the progression of Graves’ disease is provided by Pandiyan et al. [21]. This model has 13 patient-specific parameters and has been validated with patient data. Although this model in principle allows for its use as a predictor and thus as a support system, the paper [21] does not explicitly carry out this application. In [22] it was demonstrated that certain inconsistencies in the used input function render it unfit for use as a support system.
Meng published an approach to determine the dose amount for Graves’ patient in 2019 [8]. This approach does not take into account the antibody concentration. Moreover, the model’s structure can lead to drastic changes in FT4 levels in very short periods of time. Such rapid changes would not be possible in real life, considering that the known half life of FT4 is approximately seven days [4]. Meng mentions that half-life can shorten to 3‑4 days in the hyperthyroid state, but even then the decreases obtained from the model are too rapid.
In conclusion, only the publications [5, 8, 10, 21] provide a foundation for support systems in treating Graves’ disease, as indicated by the literature search. Among these, [5] is the only approach that is explicitly designed for a practical use, as it is able to make a decision based solely on FT4 measurement despite long time intervals between follow-up measurements.
In summary, there are currently very few support systems available and none of them is feasible for clinical use.
Initial dose recommendations according to the American Thyroid Association. Please note that the upper limit of the reference interval must be known for the presentation of the recommendation. Reference ranges refer to the population, which was the basis for the determination, and laboratory methods [23]. Accordingly, the exact value for the upper and lower limit of free T4 in a healthy person may vary slightly from clinic to clinic. For this work, a reference interval for free T4 from 9.5 pmol L\({}^{-1}\) to 24.0 pmol L\({}^{-1}\) was assumed
Methods
Test framework
The DigiThy framework, introduced in [5] can be used in several ways as a support system in the treatment of Graves’ disease and is available, after registration, as free web application under https://thyroid.tugraz.at/. In total it can serve the following use purposes:
-
1.
It can serve as a database, allowing for the entry of patient blood values and scheduling of control appointments.
-
2.
It can serve as a support system by recommending Methimazole (MMI) dosage suggestions after the patient’s blood values have been entered.
-
3.
It can serve as a learning tool, allowing users to create virtual patients, manually prescribe methimazole (MMI) dosages, and simulate the resultant course of time.
-
4.
The learning tool can also be used alongside the recommender system, enabling trainees to learn from the algorithm’s suggestions while working with virtual patients.
The mathematical model employed within DigiThy assigns values to each virtual patient, determining characteristics such as the patient’s response to the drug and the secretion capacity of their thyroid gland. Additionally, the course of antibodies in each patient is subject to random fluctuations. In some patients, these antibodies may completely disappear over time, while in others, they may persist. This allows the DigiThy framework to virtually mimic a variety of individual patients and courses of disease [5]. This framework enables investigations that would otherwise be unfeasible. For instance, it allows for the repeated treatment of the same patient and testing of new treatment strategies. Doctors can safely try various recommendations, like those from Fig. 1, within this digital test framework, instead of testing them on the actual patient. It also allows for multiple physicians to treat the same patient independently. The same applies to support systems, as different dosage-calculating algorithms can be applied to the same virtual patients, enabling a comparison of their performance. Of course, this also allows for comparing support systems with usual care, as was done in [5], where physicians’ treatment was compared with a specific algorithm. In [5], the treatment intervals were fixed, which limited a significant degree of freedom.
Study design
The aim of the present study is to compare the treatment quality of an existing support system, DigiThy, with the treatment of physicians at different experience and education levels.
Patients, study participants and support systems
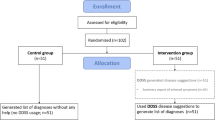
Within the DigiThy framework 60 virtual patients were created and assigned to 8 doctors, each with different levels of experience in treating Graves’ disease, see Table 1. The 60 patients were randomly generated by DigiThy, resulting in a wide range of patient-specific parameters. The progression of antibodies also varied among these virtual patients. For some patients, the disease disappeared over time. In these cases, only a few antibodies remained present, leading to such low thyroid stimulation that the FT4 concentration returned to the normal range, even without medication. In such treatments, also a “healthy” TSH concentration is restored. In other patients, the antibodies remained permanently too high, which means that they needed a permanent inhibitor, i.e. MMI, to keep the FT4 concentration within the reference interval.
In addition, there are two computer-aided support systems that can treat the virtual patients. The characteristics of these algorithms are summarized in Table 2.
The algorithms operate on the same level of information that would be available in a real-world treatment setting, specifically:
-
The real patient-specific model parameters are not transferred to the algorithms for the treatment process and must be estimated.
-
The algorithms only receive the blood values taken during control appointments and not the in-between hormonal fluctuations.
Indeed, doctors utilizing the DigiThy framework with virtual patients can view the blood concentration from the simulation between treatments, providing them with more information than the computer-aided support systems have. It should also be noted that the implemented algorithms can treat patients based solely on FT4 values, rendering them independent from TSH and TRAb measurements. Therefore, these additional measurements could potentially be omitted when utilizing support systems in the treatment of real patients.
Procedure
Each of the 8 study participants treated all 60 virtual patients. As mentioned earlier, some patients can recover and others cannot. The study participants therefore have the opportunity to decide when to finalize the treatments. This can happen under two circumstances:
-
1.
The patient’s thyroid hormone levels have stabilized within the healthy reference interval and the patient no longer requires treatment. The physician can then mark the treatment as completed.
-
2.
The patient still requires MMI after several months or years of treatment. The doctor can mark the treatment as completed and refer the patient for e.g. thyroidectomy.
Each doctor, therefore, will have a different treatment duration for each patient, depending on their assessment and the patient’s response to treatment. The algorithms then treat the 60 patients using the treatment duration of the physician with the best performance, according to the performance indices.
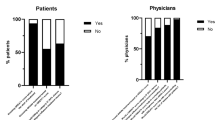
The participants without experience were also surveyed to rate the usefulness of the simulation framework as a learning platform. They were asked to choose from the following options:
-
very helpful
-
helpful
-
little helpful
-
not helpful
In the simulation framework, participants could theoretically set any number of follow-up, thereby conducting virtual blood tests for patients at any desired frequency. Accordingly, a participant could also choose an interval of 1 day between each treatment. However, participants were instructed to select intervals in DigiThy that they would realistically employ in clinical practice. Therefore, while the intervals were not strictly determined by the study design, they were implicitly constrained by the intention to reflect real-world clinical practices. This was done to ensure that the study provides a practical and realistic representation of medical practice while still giving doctors some freedom. Participants without experience could find out from guidelines which intervals are common.
Comparison
In principle, there are various possibilities to compare the quality of treatment over several weeks and months. In order to obtain a suitable comparison, three different performance indices were introduced in [5]. All these indices assess in different ways how much the FT4 concentration deviates from the center of the reference interval. In general, these indices are designed such that “smaller” values reflect “better” treatments. The used dosage can also be considered, as in performance index 2. This index not only assesses the FT4 deviation, but also takes into account the use of the drug and favours treatment approaches that require a lower dosage. The meanings of the individual ratings are summarized in Table 3.
Results
Table 4 shows the comparison between the computer aided support systems and the study participants, using the performance indices previously defined. In this context, the mean values and standard deviations for all 60 patients are presented. In addition, the mean and median values of the selected treatment intervals are given.
The interpretation of the results is discussed in Sect. 4.
Results of inexperienced physicians
The results of the three study participants without any treatment experience are illustrated in Fig. 2 using the performance index \(J_{1}\). The participants approached the task in a very structured way by first reading through the medical guidelines. As previously discussed in Sect. 1.5.1, however, these guidelines are often vague. As shown in the figure, two of the three inexperienced users (Study Users 1 and 5) visibly gained experience, as the performance index decreased over time (indicating “better” treatments), reflecting their adoption of more advanced dosing strategies contrary to the somewhat “simplistic” medical recommendations. Especially after the particularly difficult treatment of patient 21, both appeared to have gained enough experience to manage such complex disease trajectories appropriately. For Study User 5 in particular, the quality of treatment stabilizes considerably after this case. Overall, the results demonstrate that the DigiThy framework can serve as a training platform for inexperienced doctors.
Qualitative feedback from the participants
The endocrinology experts stated that they found the tool valuable due to its high potential to assist inexperienced doctors in their learning process. It was noted that it is often very difficult to familiarize young doctors with the treatment of Graves’ in everyday clinical practice because the feedback from patient follow-up visit is often received only after weeks or months. According to the participating thyroid experts, support systems that have the ability to simulate diseases can have great potential in teaching. Participants without prior practical experience were asked to evaluate the platform as a learning tool. The results of this evaluation are listed in Table 5. The evaluation ranges from little to very helpful. One of the participants noted that an exclusive focus on blood values does not eliminate the necessity of clinic visits, since this approach seems to be too simple, as it fails to consider the impact of concurrent medications, as well as patient compliance. The simulation framework presently assumes perfect adherence, with patients invariably taking their prescribed medications, which is not always the case in real-life scenarios.
As mentioned earlier, it is crucial for the development of support systems that the underlying mathematical model approximates the course of the disease sufficiently well. This has already been demonstrated in [5] using clinical data. Nevertheless, some of the qualitative feedback from the participants noted that some of the digital cases had characteristics that would not or rarely occur in everyday clinical practice. The participants themselves often emphasized that these observations are very subjective. Nevertheless, some of the statements are mentioned below, as they can open up further research questions, which in turn can lead to improved simulations and subsequent support systems.
The following effects were mentioned:
-
More frequently than in everyday clinical practice, patients are already within the reference range for FT4, even though the antibody concentration is still elevated.
-
Maximum dose of 40 mg MMI sometimes show too strong and harsh effects.
-
It was also observed that dose reduction can frequently result in larger FT4 increases than what is typically seen in clinical practice.
Overall, the expert feedback indicated that the framework can simulate patients very realistically. While one expert reported no unexpected occurrences at all, another noted minor surprises for 11 out of 60 patients. Worth noting is that the expert who did not note any unrealistic effects scored best in all 3 indices among all study participants. Since this participant never had the subjective feeling that the simulation showed unexpected effects, fewer “mistakes” happened.
Study participant 8 was the participant who chose the longest intervals. The participant pointed out that intervals longer than 8 weeks can lead to difficulties both in simulation and in reality. Accordingly, the participant considered the DigiThy framework an excellent learning opportunity to ascertain the most effective intervals.
Conclusion
The DigiThy system can be operated using two different automatic dosing algorithms. Based on 60 patients, both algorithm perform better, in terms of all 3 performance indices, than any of the study participants. This can even be achieved with those versions that use treatment intervals of 5 weeks for indices \(J_{1}\) and \(J_{3}\), see CATT-V1-35D and CATT-V2-35D in Table 4. For \(J_{2}\) only one expert performs better than CATT-V1-35D and only two experts perform better than CATT-V2-35D.
Table 6 illustrates how doctors with no previous experience and the experts perform on average according to the performance indices. The experts perform better and have slightly more variation in their treatments.
Nevertheless, all algorithms, even those that apply a 5-week interval, perform better than the best participant. Based on the feedback from the doctors, the simulation framework, while not flawless, is perceived to be realistic and of high quality. Since the algorithms performed noticeably better than the experts, this can be taken as a strong indication that they would also perform very well in everyday clinical practice.
The experts’ comments about surprising effects within the simulation mainly concern effects in edge cases. As stated in [5], the patients are determined by 8 patient-specific parameters, which must lie within previously defined limits. By refining these boundaries, a closer alignment between the computer simulation and reality can be achieved, subsequently optimizing the foundation for support systems.
Discussion
A thorough review of the literature has revealed only a sparse number of available treating support systems for hyperthyroidism. Since Graves’ disease is the main cause of hyperthyroidism, the focus was placed on support systems for this disease. Among the few theoretical approaches, there are almost no support systems that are practically applicable.
This study using 60 identical virtual patients could show that the support system DigiThy is able to treat the patients “better” based on predefined performance criteria compared to study participants, which included endocrinology experts with years of experience. The outcome suggests that support systems could offer significant advantages in routine clinical settings.
However, such support systems are usually based on mathematical descriptions and some study participants have sometimes perceived the digital descriptions of treatments as insufficiently reflecting real-life experiences in the clinics. While support systems show immense promise, future work must focus on rendering digital simulations even more realistic. This primarily necessitates the availability of real patient data.
In conclusion, the present support systems, as demonstrated in this study, appear to be very suitable for use in daily clinical routine. Validation through a clinical study is planned as a next step within this project.
References
Vitti P, Hegedüs L (2018) Thyroid Diseases – Pathogenesis, Diagnosis, and Treatment, 1st edn. Springer, Cham, Heidelberg, New York, Dordrecht, London
Smith TJ, Hegedus L (2016) Graves’ disease. N Engl J Med 375(16):1552–1565. https://doi.org/10.1056/NEJMra1510030
Weetman AP (2000) Graves’ disease. N Engl J Med 343(17):1236–1248. https://doi.org/10.1056/nejm200010263431707
Melmed S, Polonsky KS, Larsen PR, Kronenberg HM (2015) Williams Textbook of Endocrinology, 13th edn. Elsevier, Edinburgh, New York
Theiler-Schwetz V, Benninger T, Trummer C, Pilz S, Reichhartinger M (2022) Mathematical modeling of free thyroxine concentrations during methimazole treatment for graves’ disease: Development and validation of a computer-aided thyroid treatment method. Front Endocrinol (lausanne) 13:841888
Takasu N, Matsushita M (2012) Changes of TSH-stimulation blocking antibody (TSBAb) and thyroid stimulating antibody (TSAb) over 10 years in 34 TSBab-positive patients with hypothyroidism and in 98 TSAb-positive graves’ patients with hyperthyroidism: Reevaluation of TSBAb and TSAb in TSH-receptor-antibody (TRAb)-positive patients. J Thyroid Res. https://doi.org/10.1155/2012/182176
Pandiyan B (2011) Mathematical modeling and dynamical analysis of the operation of the hypothalamus–pituitary–thyroid (HPT) axis in autoimmune (Hashimoto’s) thyroiditis. PhD thesis. Marquette University
Meng F, Li E, Yen PM, Leow MKS (2019) Hyperthyroidism in the personalized medicine era: the rise of mathematical optimization. J Royal Soc Interface. https://doi.org/10.1098/rsif.2019.0083
Medici M, Visser WE, Visser TJ, Peeters RP (2015) Genetic determination of the hypothalamic-pituitary-thyroid axis: Where do we stand? Endocr Rev 36(2):214–244. https://doi.org/10.1210/er.2014-1081
Wolff TM, Menzel M, Dietrich JW, Müller MA (2022) Treating Hyperthyroidism: Model Predictive Control for the Prescription of Antithyroid Agents https://doi.org/10.48550/arXiv.2212.10096
Ross DS (1994) Hyperthyroidism, thyroid hormone therapy, and bone. Thyroid 4(3):319–326. https://doi.org/10.1089/thy.1994.4.319
Jonklaas J, Sathasivam A, Wang H, Gu J, Burman KD, Soldin SJ (2014) Total and free thyroxine and triiodothyronine: measurement discrepancies, particularly in inpatients. Clin Biochem 47(13-14):1272–1278
Schober P, Boer C, Schwarte LA (2018) Correlation coefficients. Anesth Analg 126(5):1763–1768
Dietrich JW, Midgley JEM, Hoermann R (eds) (2018) Homeostasis and Allostasis of Thyroid Function. Frontiers Media SA https://doi.org/10.3389/978-2-88945-570-6
Dietrich JW (2001) Der hypophysen-schilddrüsen-regelkreis: Entwicklung und klinische anwendung eines nichtlinearen modells. PhD thesis. Ludwig-Maximilians-Universität München
Lamooki GRR, Shirazi AH, Mani AR (2015) Dynamical model for thyroid. Commun Nonlinear Sci Numer Simul 22(1-3):297–313. https://doi.org/10.1016/j.cnsns.2014.09.013
Polyak B, Tremba A (2017) Solving underdetermined nonlinear equations by newton-like method
Wolff TM, Veil C, Dietrich JW, Müller MA (2022) Mathematical modeling and simulation of thyroid homeostasis: Implications for the allan-herndon-dudley syndrome. Front Endocrinol. https://doi.org/10.3389/fendo.2022.882788
Dietrich JW, Tesche A, Pickardt CR, Mitzdorf U (2004) Thyrotropic feedback control: Evidence for an additional ultrashort feedback loop from fractal analysis. Cybern Syst 35(4):315–331. https://doi.org/10.1080/01969720490443354
Berberich J, Dietrich JW, Hoermann R, Müller MA (2018) Mathematical modeling of the pituitary–thyroid feedback loop: Role of a TSH-t3-shunt and sensitivity analysis. Front Endocrinol. https://doi.org/10.3389/fendo.2018.00091
Pandiyan B, Merrill SJ, Bari FD, Antonelli A, Benvenga S (2018) A patient-specific treatment model for graves’ hyperthyroidism. Theor Biol Med Model. https://doi.org/10.1186/s12976-017-0073-6
Benninger T (2020) Modelling, simulation and control of graves’ hyperthyroidism. Master’s thesis. Graz University of Technology
Kratz A, Ferraro M, Sluss PM, Lewandrowski KB (2004) Case records of the massachusetts general hospital. weekly clinicopathological exercises. laboratory reference values. N Engl J Med 351(15):1548–1563
Acknowledgments
We’d like to thank all study participants for investing their time in treating the virtual patients. Feedback from medical professionals as well as inexperienced doctors is extremely important for the improvement of the project.
Funding
Open access funding provided by Graz University of Technology.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.

Scan QR code & read article online
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Benninger, T., Theiler-Schwetz, V., Pilz, S. et al. Hyperthyroidism therapy: What can decision support systems already achieve?. J. Klin. Endokrinol. Stoffw. 16, 122–131 (2023). https://doi.org/10.1007/s41969-023-00216-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41969-023-00216-0