Abstract
Background
Many trials of human epidermal growth factor receptor 2 (HER2)-positive metastatic breast cancer treatment with trastuzumab have provided evidence of improved clinical outcomes. This systematic review examined how a regimen that includes trastuzumab affects patients’ health-related quality of life (HRQoL) during and after treatment.
Methods
A systematic search for articles published up to February 2023 without restrictions of language or publication year was performed using the Pubmed, Embase, and Scopus databases. We included studies of women aged > 18 years with metastatic HER2-positive breast cancer treated with a trastuzumab-containing regimen. We assessed the quality of the studies using the Cochrane Risk of Bias (RoB) tool (2.0) for randomized controlled trials (RCTs) and the Risk Of Bias In Non-randomised Studies—of Interventions (ROBINS-I) tool for cross-sectional studies. We used Microsoft Excel to extract and synthesize data, and documented the review procedure following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines.
Results
In total, eight studies compared 1104 trastuzumab-treated patients and 1003 non-trastuzumab-treated patients. Most studies were RCTs (n = 7) and one was a prospective observational study. All the included studies used the EORTC-QLQ-C30, EORTC-QLQ-BR23, FACT-B, or FACT-G questionnaires. During treatment, patients taking regimens that included trastuzumab showed clinical improvement in HRQoL, social functioning, and role functioning. After the treatment, patients’ HRQoL profiles in the trastuzumab and chemotherapy arms were similar. However, trastuzumab (versus chemotherapy) treatment led to clinically improved functional status, role and physical functioning, and fatigue. The quality assessment revealed some concerns in most RCTs, with the risk of bias being high in two studies, low in one study, and moderate in the cross-sectional study.
Conclusions
Trastuzumab-containing regimens administered to HER2-positive breast cancer patients at the metastatic stage evidenced beneficial effects on total HRQoL during and after treatment. Upon therapy cessation, patients’ HRQoL scores for both interventions improved. Nevertheless, HRQoL profiles of patients treated with trastuzumab were more favorable, particularly for functional status, role functioning, physical well-being, and fatigue.
Clinical Trials Registration
This review was registered in PROSPERO (registration number: CRD42021259826).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The addition of trastuzumab in human epidermal growth factor receptor 2 (HER2)-positive metastatic breast cancer treatment regimens improved treatment outcomes and did not cause a deterioration in health-related quality of life (HRQoL). |
While being treated with trastuzumab-containing regimens, HER2-positive breast cancer patients showed more favorable HRQoL profiles than those treated solely with chemotherapy. |
Although metastatic breast cancer patients undergo prolonged treatment, incorporating trastuzumab into their treatment reportedly has a positive impact on their complete HRQoL profile, including their physical functioning, fatigue, emotional and role functioning, pain, insomnia, and financial constraints. |
1 Introduction
Overexpression of human epidermal growth factor receptor 2 (HER2) is associated with an increased incidence of metastasis in approximately 20% of breast cancer survivors [1,2,3]. Patients with metastatic breast cancer and overexpression of HER2 typically have advanced disease with a poor prognosis as well as shorter overall survival and disease-free survival periods [2]. Trastuzumab, a HER2-targeted therapy, has shown improved clinical outcomes and is recommended for patients with metastatic breast cancer with overexpression of HER2 [4]. Numerous trials have demonstrated the advantageous survival-related effects of trastuzumab, either when used alone or in conjunction with chemotherapy [5,6,7,8]. According to the findings of several studies, the addition of trastuzumab to a chemotherapy regimen significantly increases overall survival as well as progression-free survival compared with these survival outcomes associated with a chemotherapy regimen alone [9, 10].
The objective of metastatic breast cancer treatment is to extend survival and improve health-related quality of life (HRQoL) [11, 12]. In particular, treatment is aimed at supporting patients in overcoming challenging obstacles throughout their illness, including severe medical conditions, emotional suffering, and decreased everyday functioning [13, 14]. The physical and psychological impacts of breast cancer can be captured using HRQoL measurements. They reflect an increasingly widely acknowledged crucial endpoint of cancer therapy [15, 16], offering essential details on treatment effects from patients’ perspectives [17]. Therefore, assessing the HRQoL of breast cancer patients to contextualize the results of treatment is important [18, 19]. Notably, HRQoL measurements should include both disease symptoms and the potential adverse effects of treatments [20].
This systematic review was aimed at summarizing findings on how trastuzumab affects the HRQoL of patients with HER2-positive metastatic breast cancer. Although previous studies have explored the overall HRQoL of women with metastatic stage breast cancer [21,22,23], none have specifically investigated the influence of trastuzumab on HRQoL. Therefore, this review examined how a regimen that includes trastuzumab affects a patient’s HRQoL both during and after treatment.
2 Materials and Methods
2.1 Protocol and Registration
The protocol for this systematic review, which follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [24], was recorded in PROSPERO (registration number: CRD42021259826).
2.2 Systematic Literature Search and Study Selection
We performed a systematic search of the literature published up to February 2023 across three databases (Pubmed, Embase, and Scopus); the search terms were based on three key thematic focus areas, i.e. breast cancer, trastuzumab, and HRQoL. The search terms are presented in the Online Resource (Table A). We manually searched the included articles’ reference lists to identify any other potentially relevant articles for inclusion in the review.
This review included articles published in any language and in any year. All of the selected articles focused on women with HER2-positive metastatic breast cancer, with the intervention groups comprising regimens with and without trastuzumab. Review articles, articles that had not been peer reviewed, and posters and abstracts for which full-text articles were not available were excluded from the review. We included women aged ≥ 18 years, with no age limit, as breast cancer mostly affects adults and its incidence increases with age [25].
Applying the study’s inclusion criteria, two reviewers (SMK and FDAS) independently screened the titles and abstracts of papers to select those for inclusion in the full-text review. The full text of the articles was reviewed to select studies for inclusion in the final analysis. Disagreements arising during the review process were discussed and resolved by the reviewers. Data extraction was conducted using Microsoft Excel (Microsoft Corporation, Redmond, WA, USA), and the review procedure was documented as a PRISMA flow diagram, which helped to clarify reasons for excluding studies.
The data in all the studies were extracted by SMK and subsequently verified by FDAS. The data items comprised the author(s), year of publication, study methods, patients’ ages, instrument type, participant criteria, interventions, HRQoL outcomes, and conclusions.
2.3 Health-Related Quality of Life (HRQoL) Assessment
Changes in the significance of the minimal important difference (MID) reported in the included studies were used to summarize the HRQoL measures. The MID scores in the Functional Assessment of Cancer Therapy—Breast (FACT-B) were 7–8, whereas those for the Functional Assessment of Cancer Therapy—General (FACT-G) and Trial Outcome Index (TOI) were 5–6 points [26]. For the European Organization for the Research and Treatment of Cancer Quality of Life Questionnaire (EORTC-QLQ-C30), differences of ≥ 10 points were deemed clinically significant for all domains [27].
2.4 Quality Assessment
Quality assessments of randomized controlled trials (RCTs) were conducted using the Cochrane Risk of Bias (RoB) tool 2.0 [28], and the cross-sectional study was evaluated using the Risk Of Bias In Non-randomised Studies—of Interventions (ROBINS-I) tool [29]. The evaluation was independently performed by two authors (SMK and FDAS).
3 Results
3.1 Study Selection
The database search yielded 5752 articles, which were subsequently reduced to 257 records after eliminating duplicates and screening titles and abstracts. Following the application of eligibility criteria, this number was further reduced to 89 full-text articles, which were subsequently assessed. Ultimately, only eight records matched the inclusion characteristics and were included in this review. The selection process is outlined in detail in Fig. 1.
3.2 Characteristics of the Included Studies
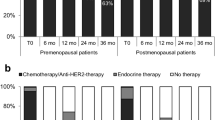
The majority of the studies included recruited patients aged >18 years [30,31,32,33,34,35,36], with one study limiting participants to those aged 18–80 years [37]. Five studies [30, 33,34,35, 37] focused on patients who had received hormonal treatment but not chemotherapy [30, 32], and one study [31] included patients who had received anthracycline, taxane, and trastuzumab in the neoadjuvant and adjuvant settings. Another study [32] included postmenopausal women who had undergone hormonal and trastuzumab treatments. Some studies [32, 34,35,36] only recruited patients with adequate organ function and excluded those with untreated or symptomatic bone and brain metastasis [33, 35, 36]. In addition, five studies [30, 32, 34, 35, 37] recruited participants with an Eastern Cooperative Oncology Group (ECOG) performance status of 0 or 1, while two studies [33, 36] only enrolled patients with a Karnofsky Index value ≥ 60%. Table 1 presents the characteristics of the included studies.
Of the eight studies, seven were RCTs [30,31,32,33,34,35,36] and one was a prospective observational study [37]. The duration of all the studies ranged between 8 and 52 months. The median treatment durations for the treatment arms in the RCTs were 48 weeks [36], 54 months [32], 32 weeks [33], 56 weeks [36], and 18 weeks [34]. The median follow-up times were 35 months [30] and 14 months [35]. In addition, one study was conducted over a 1-year period [37].
The interventions were as follows: five studies [30, 33, 35,36,37] assessed trastuzumab combined with chemotherapy versus chemotherapy alone, and the remaining studies examined the effects of trastuzumab combined with targeted therapy [31], hormone therapy [32], and eribulin mesylate [34]. Specifically, patients in three studies [33, 36, 37] were administered anthracycline plus cyclophosphamide combined with trastuzumab, while trastuzumab emtansine (T-DM1) and docetaxel, considered a comparator group, were evaluated in two other studies [30, 35]. In one study [31], a combination of trastuzumab and lapatinib versus lapatinib monotherapy was administered until either disease progression or withdrawal due to the occurrence of toxicity. In another study, trastuzumab and lapatinib were administered after treatment with aromatase inhibitors [32]. A combination of trastuzumab with eribulin mesylate was assessed in one study [34].
The EORTC-QLQ-C30 questionnaire was administered in three studies [33, 36, 37] and the FACT-B questionnaire was administered in four studies [30,31,32, 35]. In one trial [31], the FACT-B questionnaire was used along with the FACT-G questionnaire and the TOI. The EORTC-QLQ-C30 and QLQ-BR23 questionnaires were implemented together in one study [34], and the FACT-B and FACT-G questionnaires were administered together in another study [32]. Most studies [31, 33,34,35,36] showed a response rate for questionnaire completion that exceeded 50% (Table 1); however, in one study [32], the response rate was 24%, while two studies did not report the response rate.
3.3 HRQoL Evaluation
3.3.1 HRQoL During Treatment
In all studies that reported HRQoL during patients’ treatment [30,31,32,33,34, 36], on the whole the HRQoL scores significantly favored patients treated with trastuzumab combined with chemotherapy compared with other intervention groups. A significant difference was observed between the assessments performed at baseline and those performed in Week 12 [31], using the FACT-B questionnaire. Patients in a trastuzumab-treated group showed a clinically significant improvement in their HRQoL, which corresponded to stabilization regarding the progression of the disease [31]. In other domains, such as physical, functional, and social well-being, the HRQoL profile was slightly lower than at baseline but the difference was not significant [31, 32]. However, patients treated solely with trastuzumab maintained the baseline HRQoL for a shorter period than patients in the T-DM1 treatment group [30].
One study [34] that used the EORTC-QLQ-C30 questionnaire showed a clinically non-significant decrease in the total HRQoL score from baseline [33, 36], and an improvement compared with chemotherapy, T-DM1, and eribulin mesylate. A worsening score relative to the baseline was obtained for role, physical, and social functioning [33], whereas two studies [34, 36] reported improvements for fatigue, emotional functioning, pain, insomnia, and financial hardships. Furthermore, one study reported an improvement in social and role functioning in Week 12 [33]. The results of the HRQoL measurements are presented in Table 2, and the HRQoL scores for the included studies are shown in the Online Resource (Table B).
3.3.2 HRQoL After Treatment
In general, the post-treatment HRQoL profile increased in four studies [31,32,33, 36], and the mean change improved in all the intervention groups. Two studies using the FACT-B instrument showed that while the post-treatment HRQoL profiles for the trastuzumab and non-trastuzumab arms were similar, the total HRQoL scores, as well as the scores for all domains, were still more favorable in patients who received trastuzumab combined with chemotherapy than those who received chemotherapy alone [31, 35]. A similar profile was obtained using the EORTC-QLQ-C30 instrument—the overall HRQoL score and scores for all domains improved [33, 34, 36, 37]. Notably, the proportion of patients with improved HRQoL scores was considerably higher among women treated with trastuzumab plus chemotherapy than among those who only received chemotherapy [33, 34, 36]. In addition, more patients in a trastuzumab arm experienced an improvement relative to the baseline in terms of global health, physical functioning, fatigue, role functioning, emotional functioning, pain, insomnia, and financial difficulties compared with those in a non-trastuzumab arm [34]. The fatigue domain showed significant improvement in trastuzumab-treated patients [33, 36]. Notably, following the cessation of chemotherapy, patients treated with trastuzumab and chemotherapy who continued to receive trastuzumab beyond Week 20 up to the onset of disease progression showed a trend of overall improvement in quality of life, role functioning, and social functioning, and there was a clinically significant improvement in fatigue [33].
3.4 Quality Assessment
The quality assessment showed that for most of the RCTs [31, 32, 35, 36], the risk of bias was a concern to varying degrees. Two studies [33, 36] were found to have a high risk of bias (Fig. 2 and Online Resource Table C). One study was deemed to be of high quality [30]. Three studies [32, 33, 36] had some issues relating to the randomization process domain (D1) because of insufficient reporting of the strategy applied to allocate interventions to participants. There were some issues in the domain of deviation from the intended intervention (D2) in three trials [33, 35, 36] because of the lack of reporting adherence by trial subjects regarding their assigned intervention. In addition, some concerns were raised about the selection of the reported result in three studies [31, 34, 36].
Quality assessment using the Cochrane Risk of Bias (RoB) tool, version 2.0 [28]
The risk of bias in the observational study assessed using the ROBINS-I tool is shown in Online Resource Table D. This study was deemed to have a moderate risk of bias and adequate reporting quality. All confounding variables in the study [37] were evaluated and controlled, and critical domains were appropriately monitored and measured for both reliability and validity. Nevertheless, there may have been issues relating to selection bias, lack of information on adjustment techniques, an inadequate explanation of the sample size calculation, and insufficient reporting on missing data.
4 Discussion
This systematic review highlighted the effect of trastuzumab, administered as a targeted therapy, on HRQoL of HER2-positive metastatic breast cancer patients. All studies included in the review showed that treatment with trastuzumab had a more beneficial effect on HRQoL than treatment without trastuzumab. Patients undergoing a treatment regimen that included trastuzumab generally had better HRQoL profiles than those on a regimen that excluded trastuzumab. After the therapy was stopped, the HRQoL scores of the trastuzumab and non-trastuzumab groups were comparable. However, a more favorable profile was observed for the domains of functional status, role functioning, physical functioning, and fatigue in patients on a regimen containing trastuzumab.
Both groups of patients (with and without inclusion of trastuzumab in their treatment) generally experienced a decline in their HRQoL scores between the commencement and midpoint of their treatment. However, those in the trastuzumab arm evidenced better HRQoL than those in the chemotherapy arm up to follow-up. Two studies [31, 32] that used the FACT-B questionnaire also reported a favorable HQoL profile. They indicated an improved pattern of HRQoL and physical, social, and functional well-being during treatment with trastuzumab. Measurements obtained using the EORTC-QLQ-C30 instrument were similar, indicating that the deterioration in patients’ HRQoL in the trastuzumab group was less than that of patients in the non-trastuzumab group, which was also the case for the specific domains of fatigue, physical functioning, role functioning, and social functioning [33, 36]. In addition, one of the studies demonstrated an improvement in physical functioning, pain, insomnia, and financial constraints of the trastuzumab group relative to baseline [34].
The less favorable mean change from the baseline HRQoL in the chemotherapy group was probably due to the unfavorable adverse effects of chemotherapy. Patients treated with chemotherapy were associated with poorer HRQoL [38]. In addition, patients who had a worse prognosis or who were receiving chemotherapy were more likely to experience pain, fatigue, and other negative experiences [22, 39]. Trastuzumab presented a more favorable profile of adverse effect symptoms, with a lower prevalence of gastrointestinal problems, nausea, vomiting, and skin rash [40].
After treatment, and following the initial decline at baseline, all the intervention groups showed an improvement in HRQoL for all domains. There was no meaningful difference in HRQoL scores between the two intervention arms, although the HRQoL profile was slightly higher for trastuzumab-treated patients, more of whom had a better total HRQoL score than those in the chemotherapy group. At the same time, some domains, measured using both the FACT-B and EORTC-QLQ-C30 questionnaires, demonstrated a significant improvement. These domains included functional status, role functioning, physical functioning, and fatigue [33, 34, 36]. In addition, diarrhea and cognitive adverse effects were experienced less by patients undergoing trastuzumab treatment.
The findings of the current review suggest that the addition of trastuzumab to the breast cancer treatment regimen results in faster recovery from fatigue. Breast cancer patients frequently experience fatigue both during and after treatment. Thus, fatigue has significant consequences for patients’ overall quality of life [41, 42]. Moreover, one study [43] suggested that fatigue is a crucial predictor of survival.
It is necessary to consider the impact of a novel medicine introduced within a treatment regimen on a patient’s quality of life when assessing its benefits [27, 44]. Ideally, the new drug should enhance treatment effectiveness without negatively affecting the HRQoL. The findings of this systematic review suggest that incorporating trastuzumab into the treatment regimen will improve treatment outcomes without causing a decline in HRQoL. Enhanced HRQoL is likely associated with a decrease in tumor size [36]. Research has shown that a significant number of patients who receive trastuzumab along with chemotherapy experience a decrease in tumor size, resulting in a prolonged duration of disease control and survival compared with individuals who receive only chemotherapy [9].
Treatment duration is not only limited to the adjuvant phase but it also extends to the stage of disease progression in metastatic patients, who are expected to undergo a more prolonged treatment course, which can increase their susceptibility to adverse effects. Patients with late-stage disease most frequently reported a higher burden of symptoms, including pain and fatigue [21]. Those at the metastatic stage of the disease had significantly lower scores on the functional scale than those without metastasis [23]. One study found that HRQoL of metastatic breast cancer patients treated with chemotherapy, who were assessed using the FACT-B questionnaire, had lower scores (103.64 ± 22.57) compared with those at an early stage of the disease (115.84 ± 20.91) [22]. However, the addition of trastuzumab to the treatment induced a beneficial effect on patients’ HRQoL profiles; their physical, emotional, and role functioning; fatigue; pain; insomnia; and financial constraints [33, 34, 36]. Additionally, when incorporated into a breast cancer treatment regimen, trastuzumab reportedly reduces disease progression, improves the objective response rate, and extends the survival time [9, 45, 46]. Patients with metastasis on a regimen that included trastuzumab tolerated it well and had a significantly longer progression-free survival than those treated with chemotherapy alone [47].
This study had several strengths. It is the first systematic review of studies on HRQoL of patients during and after receiving trastuzumab for HER2-positive metastatic breast cancer treatment, which highlights the total HRQoL score as well as scores for specific domains. Its findings have significant clinical and economic implications. An understanding of how various treatments impact HRQoL has important clinical implications for customizing therapies to optimize patient well-being alongside disease management, thereby fostering more patient-centered care. Additionally, the identification of specific areas of marked decline in patients’ HRQoL enables targeted allocation of psychosocial support resources and coping strategies during and after treatment. From an economic standpoint, integrating HRQoL evaluations into economic analyses aids in comprehensive evaluations of treatment cost effectiveness, potentially favoring therapies offering better HRQoL outcomes relative to costs. Ultimately, comprehensive assessments of HRQoL in breast cancer patients can potentially enhance clinical decision making, optimize resource allocation, and improve patients’ well-being, while also considering the economic implications of various treatment strategies. Our search strategy for identifying articles did not have any language or time limitations, thereby ensuring that all relevant publications were covered. However, we acknowledge the limitations of this review. The targeted studies entailed different treatment regimens, which may have led to discrepancies in the results for HRQoL profiles. Moreover, the instruments utilized in these studies varied. It is also important to note that because this review did not elaborate on the factors influencing HRQoL scores, its findings are only based on each study’s HRQoL values.
In future studies aimed at assessing the HRQoL outcomes for breast cancer patients, several critical considerations should guide the research approach. Comparative analyses covering diverse treatment modalities would offer nuanced perspectives on the differential impacts of various treatments on HRQoL outcomes. Additionally, it is essential to encompass diverse patient demographics and breast cancer stages to ensure comprehensive representation. Moreover, evaluations of psychosocial factors and their impacts on HRQoL outcomes, for example, within supportive care programs, conducted alongside interventions can provide valuable insights. Incorporating multiple HRQoL measurement tools and emphasizing the importance of patient-reported outcomes within clinical trials would provide a holistic perspective. The validation of instruments for diverse populations is critical to ensure accuracy and applicability. Future studies that incorporate these elements would provide a more holistic understanding of HRQoL among breast cancer patients, fostering tailored interventions and improved patient-centered care approaches.
5 Conclusions
Treatment regimens for HER2-positive, metastatic breast cancer patients that include trastuzumab showed beneficial effects both during and after treatment. Upon cessation of therapy, HRQoL scores of patients undergoing both regimens (with and without trastuzumab) improved; however, patients treated with trastuzumab had more favorable HRQoL profiles, particularly in the domains of functional status, role functioning, physical well-being, and fatigue. These findings suggest that while overall HRQoL improved after the completion of treatment, trastuzumab conferred additional benefits for patients during and after their therapy.
References
Dawood S, Broglio K, Buzdar AU, Hortobagyi GN, Giordano SH. Prognosis of women with metastatic breast cancer by her2 status and trastuzumab treatment: an institutional-based review. J Clin Oncol. 2010;28:92.
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL. Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science. 1979;1987(235):182–91.
Ross JS, Slodkowska EA, Symmans WF, Pusztai L, Ravdin PM, Hortobagyi GN. The HER-2 receptor and breast cancer: ten years of targeted anti-HER-2 therapy and personalized medicine. Oncologist. 2009;14:320–68.
McKeage K, Perry CM. Trastuzumab: a review of its use in the treatment of metastatic breast cancer overexpressing HER2. Drugs. 2002;62:209–43. https://doi.org/10.2165/00003495-200262010-00008. (cited 23 Jan 2023).
Jackisch C, Schoenegg W, Reichert D, Welslau M, Selbach J, Harich H-D, et al. Trastuzumab in advanced breast cancer—a decade of experience in Germany. BMC Cancer. 2014;14:924.
De Mattos-Arruda L, Cortes J, De M-A, Cortes J. Advances in first-line treatment for patients with HER-2+ metastatic breast cancer. Oncologist. 2012;17:631–44.
Mendes D, Alves C, Afonso N, Cardoso F, Passos-Coelho JL, Costa L, et al. The benefit of HER2-targeted therapies on overall survival of patients with metastatic HER2-positive breast cancer—a systematic review. Breast Cancer Res. 2015;17:140.
Robert N, Leyland-Jones B, Asmar L, Belt R, Ilegbodu D, Loesch D, et al. Randomized phase III study of trastuzumab, paclitaxel, and carboplatin compared with trastuzumab and paclitaxel in women with HER-2-overexpressing metastatic breast cancer. J Clin Oncol. 2006;24:2786–92.
Slamon DJ, Leyland-Jones B, Shak S, Fuchs H, Paton V, Bajamonde A, et al. Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N Engl J Med. 2001;344:783–92.
Marty M, Cognetti F, Maraninchi D, Snyder R, Mauriac L, Tubiana-Hulin M, et al. Randomized phase II trial of the efficacy and safety of trastuzumab combined with docetaxel in patients with human epidermal growth factor receptor 2-positive metastatic breast cancer administered as first-line treatment: the M77001 study group. J Clin Oncol. 2005;23:4265–74.
Ahmed S, Sami A, Xiang J. HER2-directed therapy: current treatment options for HER2-positive breast cancer. Breast Cancer. 2015;22:101–16.
Cardoso F, Costa A, Senkus E, Aapro M, André F, Barrios CH, et al. 3rd ESO-ESMO International Consensus guidelines for advanced breast cancer (ABC 3). Ann Oncol. 2017;28:16–33 (cited 23 Jan 2023).
Michael YLD, Kawachi I, Berkman LF, Holmes MD, Colditz GA, Corsano K, et al. The persistent impact of breast carcinoma on functional health status: prospective evidence from the Nurses’ Health Study. Cancer. 2000;89(11):2176–86.
Stein KD, Syrjala KL, Andrykowski MA. Physical and psychological long-term and late effects of cancer. Cancer. 2008;112:2577–92.
Snyder CF, Aaronson NK. Use of patient-reported outcomes in clinical practice. Lancet. 2009;374:369–70.
Marshall S, Haywood K, Fitzpatrick R. Impact of patient-reported outcome measures on routine practice: a structured review. J Eval Clin Pract. 2006;12:559–68.
Frank L, Basch E, Selby JV. The PCORI perspective on patient-centered outcomes research. JAMA. 2014;312:1513–4.
Riis CL, Bechmann T, Jensen PT, Coulter A, Steffensen KD, Lundgaard Riis C, et al. Are patient-reported outcomes useful in post-treatment follow-up care for women with early breast cancer? A scoping review. Patient Relat Outcome Meas. 2019;10:117–27.
Stefanovic S, Wallwiener M, Karic U, Domschke C, Katic L, Taran FA, et al. Patient-reported outcomes (PRO) focused on adverse events (PRO-AEs) in adjuvant and metastatic breast cancer: clinical and translational implications. Support Care Cancer. 2017;25:549–58.
Cardoso F, Spence D, Mertz S, Corneliussen-James D, Sabelko K, Gralow J, et al. Global analysis of advanced/metastatic breast cancer: decade report (2005–2015). Breast. 2018;39:131–8.
Rautalin M, Färkkilä N, Sintonen H, Saarto T, Taari K, Jahkola T, et al. Health-related quality of life in different states of breast cancer—comparing different instruments. Acta Oncol. 2018;57:622–8.
Hamer J, McDonald R, Zhang L, Verma S, Leahey A, Ecclestone C, et al. Quality of life (QOL) and symptom burden (SB) in patients with breast cancer. Support Care Cancer. 2017;25:409–19.
El Fakir S, El Rhazi K, Zidouh A, Bennani M, Benider A, Errihani H, et al. Health-related quality of life among breast cancer patients and influencing factors in Morocco. Asian Pac J Cancer Prev. 2016;17:5063.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. J Clin Epidemiol. 2021;134:178–89 (cited 7 Dec 2023).
Ilic L, Haidinger G, Simon J, Hackl M, Schernhammer E, Papantoniou K. Trends in female breast cancer incidence, mortality, and survival in Austria, with focus on age, stage, and birth cohorts (1983–2017). Sci Rep. 2022;12. Available at: https://www.nature.com/articles/s41598-022-10560-x. [cited 9 Dec 2023].
Eton DT, Cella D, Yost KJ, Yount SE, Peterman AH, Neuberg DS, et al. A combination of distribution- and anchor-based approaches determined minimally important differences (MIDs) for four endpoints in a breast cancer scale. J Clin Epidemiol. 2004;57:898–910.
Osoba D, Rodrigues G, Myles J, Zee B, Pater J. Interpreting the significance of changes in health-related quality-of-life scores. J Clin Oncol. 2016;16:139–44.
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ. 2019;366:I4898. Available at: https://www.bmj.com/content/366/bmj.l4898. [cited 19 Feb 2023].
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016;355:I4919. Available at: https://www.bmj.com/content/355/bmj.i4919. [cited 19 Feb 2023]
Perez EA, Barrios C, Eiermann W, Toi M, Im Y-H, Conte P, et al. Trastuzumab emtansine with or without pertuzumab versus trastuzumab plus taxane for human epidermal growth factor receptor 2-positive, advanced breast cancer: primary results from the phase III MARIANNE study. J Clin Oncol. 2017;35:141–8.
Wu Y, Amonkar MM, Sherrill BH, O’Shaughnessy J, Ellis C, Baselga J, et al. Impact of lapatinib plus trastuzumab versus single-agent lapatinib on quality of life of patients with trastuzumab-refractory HER2+ metastatic breast cancer. Ann Oncol. 2011;22:2582–90.
Johnston SRD, Hegg R, Im SA, Park IH, Burdaeva O, Kurteva G, et al. Phase III, randomized study of dual human epidermal growth factor receptor 2 (HER2) blockade with lapatinib plus trastuzumab in combination with an aromatase inhibitor in postmenopausal women with HER2-positive, hormone receptor–positive metastatic breast cancer: updated results of alternative. J Clin Oncol. 2021;39:79–89.
Rugo H, Brammer M, Zhang F, Lalla D. Effect of trastuzumab on health-related quality of life in patients with HER2-positive metastatic breast cancer: data from three clinical trials. Clin Breast Cancer. 2010;10:288–93.
Schwartzberg L, McIntyre K, Wilks S, Puhalla S, O’Shaughnessy J, Berrak E, et al. Health-related quality of life in patients receiving first-line eribulin mesylate with or without trastuzumab for locally recurrent or metastatic breast cancer. BMC Cancer. 2019;19:578 (cited 25 May 2022).
Hurvitz SA, Dirix L, Kocsis J, Bianchi GV, Lu J, Vinholes J, et al. Phase II randomized study of trastuzumab emtansine versus trastuzumab plus docetaxel in patients with human epidermal growth factor receptor 2-positive metastatic breast cancer. J Clin Oncol. 2013;31:1157–63.
Osoba D, Slamon DJ, Burchmore M, Murphy M. Effects on quality of life of combined trastuzumab and chemotherapy in women with metastatic breast cancer. J Clin Oncol. 2002;20:3106–13.
Syrios J, Pappa E, Volakakis N, Grivas A, Alafis J, Manioudaki S, et al. Real-world data on health-related quality of life assessment in patients with breast cancer receiving subcutaneous trastuzumab. Breast Cancer (Auckl). 2018;12:1178223418758031 (cited 12 Sep 2021).
Wöckel A, Schwentner L, Krockenberger M, Kreienberg R, Janni W, Wischnewsky M, et al. Predictors of the course of quality of life during therapy in women with primary breast cancer. Qual Life Res. 2017;26:2201–8.
Hsu HT, Lin KC, Wu LM, Juan CH, Hou MF, Hwang SL, et al. Symptom cluster trajectories during chemotherapy in breast cancer outpatients. J Pain Symptom Manag. 2017;53:1017–25.
Sodergren SC, Copson E, White A, Efficace F, Sprangers M, Fitzsimmons D, et al. Systematic review of the side effects associated with anti-HER2-targeted therapies used in the treatment of breast cancer, on behalf of the EORTC Quality of Life Group. Target Oncol. 2016;11:277–92.
Bower JE, Ganz PA, Desmond KA, Rowland JH, Meyerowitz BE, Belin TR. Fatigue in breast cancer survivors: occurrence, correlates, and impact on quality of life. J Clin Oncol. 2000;18:743–53.
Smets EMA, Garssen B, Schuster-Uitterhoeve ALJ, de Haes JCJM. Fatigue in cancer patients. Br J Cancer. 1993;68:220–4.
Groenvold M, Petersen MA, Idler E, Bjorner JB, Fayers PM, Mouridsen HT. Psychological distress and fatigue predicted recurrence and survival in primary breast cancer patients. Breast Cancer Res Treat. 2007;105:209–19.
Johansson B, Brandberg Y, Hellbom M, Persson C, Petersson LM, Berglund G, et al. Health-related quality of life and distress in cancer patients: results from a large randomised study. Br J Cancer. 2008;99:1975–83 (cited 2 Feb 2022).
Extra J-M, Antoine EC, Vincent-Salomon A, Delozier T, Kerbrat P, Bethune-Volters A, et al. Efficacy of trastuzumab in routine clinical practice and after progression for metastatic breast cancer patients: the observational Hermine study. Oncologist. 2010;15:799–809.
Vogel CL, Cobleigh MA, Tripathy D, Gutheil JC, Harris LN, Fehrenbacher L, et al. Efficacy and safety of trastuzumab as a single agent in first-line treatment of HER2-overexpressing metastatic breast cancer. J Clin Oncol. 2002;20:719–26.
Li H, Shao B, Yan Y, Song G, Liu X, Wang J, et al. Efficacy and safety of trastuzumab combined with chemotherapy for first-line treatment and beyond progression of HER2-overexpressing advanced breast cancer. Chin J Cancer Res. 2016;28:330.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded through the Indonesia Endowment Funds for Education (LPDP) under grant number 0005479/PHA/D/BUDI-2019, and by the University of Groningen/University Medical Center Groningen.
Availability of data and material
All data generated and/or analyzed for this review are included in this published article.
Conflict of interest
Sudewi Mukaromah Khoirunnisa, Fithria Dyah Ayu Suryanegara, Lisa Aniek de Jong, Didik Setiawan, and Maarten Jacobus Postma declare they have no competing interests in relation to this work.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Code availability
Not applicable.
Author contributions
Conceptualization: SMK. Methodology and investigation: SMK and FDAS. Writing—original draft preparation: SMK. Writing—review and editing: SMK, FDAS, LAdJ, DS, and MJ. Supervision: LAdJ, DS, and MJP. All authors approved the final version of the manuscript.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Khoirunnisa, S.M., Suryanegara, F.D.A., de Jong, L.A. et al. A Systematic Review of Health-Related Quality of Life in Women with HER2-Positive Metastatic Breast Cancer Treated with Trastuzumab. PharmacoEconomics Open (2024). https://doi.org/10.1007/s41669-024-00478-7
Accepted:
Published:
DOI: https://doi.org/10.1007/s41669-024-00478-7