Abstract
Objectives
Autistic individuals and those diagnosed with ADHD are at greater risk for social difficulties, with evidence suggesting that the co-occurrence of these neurodevelopmental disorders may further exacerbate social challenges. Though social skill interventions have strong empirical support in autistic populations, fewer evidence-based social skill interventions for adolescents with ADHD exist. Further, the impact of co-occurring autism and ADHD diagnoses on social skill treatment response is unknown. This study aimed to investigate the comparative efficacy of the evidence-based PEERS® for Adolescents social skills intervention in adolescents with ADHD, autistic adolescents, and adolescents with co-occurring ADHD and autism.
Methods
Adolescents (N = 144; ADHD, n = 43; Autism, n = 60; ADHD + Autism, n = 41) and their parents participated in PEERS® for Adolescents and completed questionnaires on social functioning at pre- and post-intervention. PEERS® for Adolescents is a 16-week, parent-assisted social skills intervention that teaches ecologically valid skills related to making and keeping friends as well as handling conflict and rejection in peer relationships.
Results
At baseline, a MANCOVA revealed significant differences in social behavior by diagnostic group (ADHD, Autism, ADHD + Autism), F(10,218) = 3.60, p < .001. However, in a repeated measures MANCOVA, no significant differences in treatment response following PEERS® for Adolescents across diagnostic groups emerged, F(10,214) = 1.34, p = .209. As a whole, participants significantly improved across all assessed outcomes.
Conclusion
Results suggest that adolescents with ADHD, with or without a co-occurring autism diagnosis, benefit from the novel extension of PEERS® for Adolescents, showing improved social skill proficiency and decreased problem behaviors.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
As neurodevelopmental disorders, attention-deficit/hyperactivity disorder (ADHD) and autism both impact the neurobiological development of an individual and how they interact with the world. Differences are apparent in childhood for both autism and ADHD, though the predominant characteristics, strengths, and challenges are distinct. Neurodiversity does produce strengths for these populations, such that those with ADHD report and display greater cognitive dynamism, creativity, courage, energy, humanity, resilience, and transcendence (Sedgwick et al., 2019; White & Shah, 2006). Per autistic adults,Footnote 1 the ability to hyperfocus, attention to detail, memory, honesty, and loyalty emerge as common autistic traits that can confer advantages (Russell et al., 2019). However, the differences associated with ADHD and autism also often confer challenges for these individuals, with some of these challenges stemming from societal expectations being misaligned with these populations’ neurobehavioral presentations. Youth with ADHD most frequently present with differences in their attention, organization, activity level, and/or impulse control (APA, 2013). In contrast, autistic individuals present with differences in their social communication (e.g., difficulties with nonverbal communication, atypical approach to conversation) and display patterns of restricted, repetitive behaviors (APA, 2013).
Notably, ADHD and autism also share significant transdiagnostic commonalities (Mikami et al., 2019). Studies have shown that ADHD symptoms (e.g., attentional changes, impulsivity, hyperactivity) are common in autism (Mayes et al., 2012). Research has shown increased irritability, sleep difficulties, and executive function differences are present in both children with ADHD and autistic children (APA, 2013; Craig et al., 2016; Eyre et al., 2019; Mayes et al., 2009). Most notably, the differences associated with both diagnoses often impact these populations in their relationships with others (Petrina et al., 2014; Ros & Graziano, 2018). Prior literature has demonstrated that youth diagnosed with ADHD experience higher rates of peer victimization and peer rejection, while also showing a tendency toward deterioration of friendship quality over time that is not observed in peers without ADHD, indicating a difficulty maintaining friendships (Normand et al., 2013; Sciberras et al., 2009; Taylor et al., 2010). Similarly, studies have shown that autistic youth are more likely to have fewer friends, be less actively engaged in social settings, and experience peer rejection and bullying when compared to neurotypical peers (Kasari et al., 2011; Maiano et al., 2016; Taheri et al., 2016).
Theoretically, the barriers to social engagement for those with ADHD may be driven by the presence of culturally inappropriate social behaviors (e.g., interrupting, intrusion on personal space, poor sportsmanship), while autism is more characterized by the absence of culturally normative social behaviors (e.g., less use of social initiations, gestures, facial expressions; Antshel & Russo, 2019; Mikami et al., 2019). Thus, it is plausible that the combined clinical presentation of both ADHD and autism may further compound social challenges. Though it has long been clinically observed that the symptoms of ADHD and autism frequently co-occur, only the most recent edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5; APA, 2013) has allowed for both diagnoses to be assigned. In a recent meta-analysis, the pooled current and lifetime prevalence rates of ADHD in autistic individuals were 38.5% and 40.2%, respectively (Rong et al., 2021). Among a large sample of children with ADHD (n = 2495), 13% were also diagnosed with autism (Zablotsky et al., 2020). These prevalence estimates suggest that the co-occurrence of these conditions is more common than would be expected given general population prevalence. Due to the recency of this change, the field’s knowledge of co-occurring ADHD and autism is still growing, and there is still debate regarding the etiology of the high rates of attentional deficits and differences in autistic populations (Hours et al., 2022).
Despite ongoing scientific study, the current literature suggests that those with both diagnoses may be a uniquely high-risk population in terms of social-emotional difficulty. When comparing the features of children diagnosed with both ADHD and autism to children with ADHD only, youth with both diagnoses had significantly greater treatment needs, were rated as having more severe ADHD symptoms, and were significantly more likely to be diagnosed with additional co-occurring mental health conditions (Zablotsky et al., 2020). Similarly, Sprenger et al. (2013) concluded that compared with those with autism alone, those with co-occurring ADHD and autism had significantly more severe autism-related symptoms, especially in the area of social interaction. Other studies have found similar additive risks and difficulties in populations with both ADHD and autism (Gordon-Lipkin et al., 2018; Jang et al., 2013). With respect to social skill proficiency specifically, the current limited evidence base suggests that autistic individuals, with or without an ADHD diagnosis, have significantly greater social challenges than those with ADHD alone (Dellapiazza et al., 2021; Harkins et al., 2021). However, more research is needed on those with co-occurring ADHD and autism, with particular attention needed for understanding adolescence as a crucial window for symptom constellations (Hartman et al., 2016).
Understanding and addressing the impact of neurodevelopmental disorders on social relationships is essential given the current scientific understanding that suggests friendships and a sense of belonging are especially critical in promoting positive identity development (Ragelienė, 2016). Social difficulties correspond to increased mental health problems in both those with ADHD and those with autism (Becker et al., 2017; Humphreys et al., 2013; Mayes et al., 2011; Ratcliffe et al., 2015). Further, for autistic people, social challenges have also been associated with poor academic performance in adolescence and poor employment outcomes in adulthood (Chen et al., 2015; Chiang et al., 2013; Hsiao et al., 2013). Similarly, in youth with ADHD, poor social acceptance has been linked to poorer quality of life and shown to exacerbate the negative relationship between inattention and academic performance (Dvorsky & Langberg, 2016, Dvorsky et al., 2018). Consequently, beyond understanding, it is also of critical importance to address the social difficulties associated with both neurodevelopmental disorders early in life to enhance long-term quality of life in both populations.
One of the most common approaches for mitigating social challenges in neurodiverse youth is social skills training (SST). SST approaches typically involve direct teaching of social skills (e.g., emotion recognition, body boundaries, nonverbal communication, conversation skills) in a small-group format, through didactic lessons (e.g., structured, educational modules), modeling, skills practice, positive reinforcement, and caregiver training (Moody & Laugeson, 2020). For autistic youth, SST interventions have been classified as an evidence-based practice, with over 40 group design studies in the literature (Hume et al., 2021). Though many studies and programs exist, the Program for the Education and Enrichment of Relational Skills (PEERS®) for Adolescents (Laugeson & Frankel, 2010) is the only evidence-based, publicly available manualized SST for autistic adolescents (Hume et al., 2021). PEERS® for Adolescents has been extensively studied in autistic youth, with a recent meta-analysis showing medium to large pooled effect sizes for multiple outcomes, including adolescent social knowledge and frequency of get-togethers as well as on standardized parent-report measures of social skills and social responsiveness (Zheng et al., 2021). Specific studies have also supported that PEERS® for Adolescents also produces positive changes in observed social behavior (Rabin et al., 2020), well-being (Lordo et al., 2017; McVey et al., 2016; Schiltz et al., 2018), and neurobiological indices (Baker et al., 2020; Van Hecke et al., 2015) in autistic youth.
Despite strong evidence for use in autistic youth, SST interventions in youth with ADHD have demonstrated mixed evidence. A comprehensive systematic review of SST programs for children and adolescents with ADHD including randomized and non-randomized control trial studies concluded that 88% of the SST interventions (n = 16) reviewed improved various social skill outcomes (Willis et al., 2019). Common characteristics of effective SST interventions for youth with ADHD identified in the review were similar to those cited for autistic youth, including similar content (e.g., good sportsmanship, conflict resolution), session length, program duration, small-group format, and some form of parental involvement. However, despite some evidence of benefit, many social improvements were not consistent across informants and did not maintain over time. Similarly, using the primary outcome of teacher-reported behavior, a Cochrane review concluded there was no beneficial effects of SST in youth with ADHD (Storebø et al., 2019). However, most of the identified studies only included children under the age of 12, revealing the SST literature in adolescents to be even weaker. A single meta-analysis of eight studies including but not limited to SST showed no benefit of interventions in improving social skill proficiency more broadly in teens with ADHD (Morris et al., 2021). Indeed, the only included study in this meta-analysis to demonstrate significant effects of SST in youth with ADHD examined PEERS® for Adolescents (Gardner et al, 2019).
In Gardner et al.’s (2019) study (n = 20), PEERS® for Adolescents was tested in teens with a previous diagnosis of ADHD. Results indicated significant increases in adolescents’ reciprocal friendships, get-togethers, and social knowledge. Nonsignificant benefits to friendship quality and social self-efficacy were also observed, and secondary analyses of the sample showed benefits to the family system more broadly (Gonring et al., 2017). Although the PEERS® for Adolescents program is clinically used widely for youth who struggle to make and keep friends regardless of their diagnosis, these promising findings have yet to be replicated in research to further solidify the efficacy of PEERS® for Adolescents in youth with ADHD. Given critical review of the overall mixed evidence for SST in youth with ADHD, researchers have called for inclusion of outcomes that assess ecological success (e.g., sociometric ratings), greater racial/ethnic diversity in samples, and greater empirical study of SST in adolescents (Storebø et al., 2019; Willis et al., 2019). Notably, Mikami et al. (2017) also highlighted increased reinforcement and reminders of culturally appropriate social behavior in real time with peers rather than after the fact with therapists as an important research direction for SST in ADHD. These elements, through practice with peers, live social coaching, and performance feedback, are included in every PEERS® for Adolescents session. Additionally, the PEERS® program’s emphasis on parent involvement and coaching outside of sessions also increases opportunities for in vivo reminders and reinforcement related to social behavior. As suggested by Mikami et al. (2017), these features are particularly well-suited to the needs of youth with ADHD who struggle with consistently performing culturally appropriate social behavior in the moment, despite having knowledge of such behavior, likely due to difficulties with impulse control and emotion regulation (Aduen et al., 2018). Further, the program directly addresses certain behaviors often present in ADHD (e.g., poor sportsmanship, interrupting).
SST research must also evaluate interventions specifically for individuals with co-occurring ADHD and autism — an area where empirical guidance is lacking beyond showing efficacy in ADHD alone. One study found that the effect of parent training in autistic children is moderated by the presence of ADHD with effects observed more readily in autistic children without ADHD (Lecavalier et al., 2017). This could suggest that co-occurring ADHD and autism may make it more difficult for children to benefit from parent training interventions. This study illustrates the need to rigorously examine psychosocial interventions to confirm benefits and understand risks in diagnostically complex individuals. To our knowledge, no research to date has examined how the co-occurrence of ADHD and autism may impact the efficacy of established social skills training approaches.
The current study’s objective was to examine the comparative treatment outcomes of adolescents with ADHD, autistic adolescents, and adolescents with co-occurring ADHD and autism following the PEERS® for Adolescents social skills intervention, delivered in an outpatient clinic setting. In doing so, we aimed to (1) replicate previous findings that produce benefits to social outcomes in youth with ADHD (e.g., Gardner et al., 2019) and (2) investigate program efficacy in adolescents with co-occurring autism and ADHD, which has yet to be established. It was hypothesized that all three groups would benefit significantly from the program, with the ADHD groups, regardless of the presence of autism, showing a less robust effect. This was posited given mixed findings from previous studies examining SST in this population, particularly for adolescents with ADHD, as discussed above (Storebø et al., 2019; Willis et al., 2019).
Method
Participants
Participants included families seeking social skills treatment through the UCLA PEERS® Clinic, an outpatient clinical setting, and data were drawn from a larger archival clinical database with approval from the university Institutional Review Board. Adolescent participants presented with a history of social difficulties and included 144 adolescents in middle school and high school with ADHD and/or autism ranging from 10 to 18 years of age. Adolescents and their parents engaged in a phone screening followed by an intake appointment with a postdoctoral psychology fellow or licensed clinical psychologist to determine eligibility. Eligibility criteria for entry into treatment included the following: (1) adolescent and parent were both fluent in English; (2) adolescent did not have a major mental illness (e.g., active psychosis); (3) adolescent was willing to be coached by their caregiver outside of the treatment setting; (4) adolescent was motivated to participate in the program and learn the skills taught in PEERS®; and (5) adolescent was able to comprehend session content and meaningfully participate in group format, as determined by clinician judgement. In determining an adolescent’s ability to meaningfully participate in the group format, intake clinicians attended to the adolescent’s expressive and receptive language (e.g., contingent responding, use of full sentences) during the intake when asking about hobbies, peer interactions, and mood. Adolescents who may need more support or a slower pace were provided referrals for certified PEERS® providers who could provide the content in an individualized, one-on-one setting. After determining eligibility and interest, participants were enrolled in PEERS® for Adolescents in cohorts of 10-12 persons. Cohorts were diagnostically heterogeneous with considerations based on age, developmental level, and social communication support needs of adolescents, as determined by clinician judgement, to ensure an ecologically valid social context for within-group practice.
Diagnostic information was gathered from parents and adolescents during the intake process. Given the changes in the DSM-5 (APA, 2013) that allowed both diagnoses to co-occur, we limited the sample to participants who participated between 2014 and 2020, in person prior to the COVID-19 pandemic. Adolescents were classified into one of three groups (ADHD, n = 43; Autism, n = 60; ADHD + Autism, n = 41). Twenty-five percent of enrolled participants with the eligible diagnoses during the selected time period discontinued prior to completion of the PEERS® for Adolescents program. This attrition rate is lower than what is typically seen in youth outpatient mental health care (de Haan et al., 2013). No significant differences in attrition by diagnosis were present, χ2(2) = 1.15, p = 0.563. Anecdotally, the most common reasons for discontinuing treatment were scheduling conflicts and logistical challenges (e.g., travel time). Only participants who had completed pre- and post-treatment assessments on at least one primary outcome measure were included in the current sample of 144 adolescents.
Adolescent participants in the ADHD group (n = 43) were previously diagnosed with ADHD, inclusive of inattentive, hyperactive-impulsive, and combined presentations, without a diagnosis of autism. Those in the Autism group (n = 60) were previously diagnosed with autism and did not have a diagnosis of ADHD. Though not formally assessed in a comprehensive diagnostic evaluation due to the nature of outpatient services, adolescent participants generally presented with lower support needs (majority “Level 1; Requiring Support,” with some “Level 2; Requiring Substantial Support” in both the social communication and restricted, repetitive behaviors domains per the DSM-5; APA, 2013) given eligibility criteria. Participants in the ADHD + Autism group (n = 41) reported both previous diagnoses. Of note, some participants in all three groups had other co-occurring conditions (e.g., anxiety, depression).
Across the entire sample, the average age of participating adolescents was 13.9 years old (SD = 1.9). With respect to gender, 75.0% (n = 108) of the adolescent participants identified as male and 25.0% (n = 36) identified as female. Sixty percent (n = 87) of adolescent participants identified as White; 8.3% (n = 12) as Hispanic/Latinx; 6.9% (n = 10) as Asian; 2.1% (n = 3) as Black; and 22.3% (n = 32) as being from other/unspecified ethnic groups, including multiracial identities. Participating parent social coaches remained consistent throughout the 16-week intervention; parents were mostly mothers (81%) and highly educated (85% having a bachelor’s degree or higher). See Table 1 for more information on demographic and clinical characteristics of the sample by the three diagnostic groups (i.e., ADHD, Autism, ADHD + Autism). There were no significant differences by diagnostic group in adolescent gender, χ2(2) = 1.38, p = .501, or race/ethnicity (considered as a binary variable: White, BIPOC), χ2(2) = 2.30, p = .317. An ANOVA indicated significant differences by diagnostic group in age, F(2,140) = 3.46, p = .034. Post hoc comparisons with a Bonferroni adjustment indicated that adolescents in the Autism group (Mage = 14.3, SD = 2.0) were significantly older than those in the ADHD only group (Mage = 13.4, SD = 1.8), p = .045.
Procedures
Following the phone screening and initial intake appointments, adolescents and their parents completed measures assessing participants’ social functioning. Following the 16-week intervention, adolescents and parents completed outcome measures again to assess change over course of treatment. Social functioning outcome measures are described in the Measures section.
PEERS® for Adolescents (Laugeson & Frankel, 2010) is a 90-minute 16-week intervention that utilizes a small-group format (e.g., 10-12 adolescents) with a concurrent parent social coach group. The groups consist of didactic lessons with concrete rules and steps of targeted social skills, role-play demonstrations, behavioral rehearsal exercises, and weekly ecologically valid socialization assignments. The structure of the group utilizes tenets of cognitive behavioral therapy (CBT), such as psychoeducation, Socratic questioning, skills building and practice, cognitive strategies, and homework assignments, through a social skill-focused lens. Topics discussed include conversational skills, sources of friends, electronic communication, use of humor, good sportsmanship, conversation entry and exiting strategies, organizing get-togethers with peers, handling conflict (i.e., disagreements), and navigating rejection (i.e., various types of bullying, bad reputations). See Table 2 for a list of session content by week. The rules and steps of social skills are demonstrated through content exemplars representative of developmentally normative adolescent social situations (e.g., high school, school clubs). Each session is dedicated to ecologically valid content related to making and keeping friends and developing more meaningful friendships, while social coaches simultaneously learn how to coach and maintain skill generalization beyond sessions.
Parent social coaching sessions were led by a licensed clinical psychologist and adolescent sessions were led by either a licensed clinical psychologist or postdoctoral psychology fellow, under the supervision of the developer of PEERS®. As a training clinic, the archival data from 2014 to 2020 included in this study spans approximately 13 group leaders across the social coaching and adolescent sessions; 85% of group leaders identified as female (15% male) and 69% identified as White (31% as BIPOC, including Asian and Hispanic/Latinx). The sessions were also supported by a team of 4-7 psychology undergraduate students, postbaccalaureate clinic coordinator staff, and allied health graduate students and pre-doctoral psychology interns who served as behavioral coaches. Throughout the 16 weeks, behavioral coaches assisted in tracking treatment fidelity, homework compliance, conducting role-play demonstrations, and providing performance feedback to participants during small-group behavioral rehearsals. Prior to leading and assisting in the groups, all group facilitators and behavioral coaches attended trainings in PEERS®. All members of the treatment team followed published treatment manual guidelines during groups (Laugeson, 2014; Laugeson & Frankel, 2010) and were supervised by the developer of the PEERS® intervention to maintain fidelity. Given that data were drawn from archival clinical database, no formal measures of fidelity are available. However, behavioral coaches informally monitored treatment fidelity throughout every session and notified group leaders if a rule or step from the lesson was missed. Of note, the clinical groups in the current study used a weekly 90-minute parent-assisted model as described in Laugeson and Frankel (2010); however, groups followed the school-based 16-week curriculum (Laugeson, 2014), which adds two additional sessions from the original parent-assisted model.
Measures
Demographic Questionnaire
Prior to the initial intake appointment, a questionnaire gathering general information regarding age, gender, ethnic background, diagnoses, education, and medication history was administered. Parents of participating adolescents completed the demographic questionnaire at baseline.
Social Skills Improvement System Rating Scales
The Social Skills Improvement System (SSIS; Gresham & Elliott, 2008) Rating Scales are norm-referenced rating forms completed by caregivers on behalf of children and adolescents ages 3 to 18. The SSIS parent form yields standard scores (M = 100, SD = 15) in two distinct domains: the Social Skills Domain, which contains subscales of Communication, Cooperation, Assertion, Responsibility, Empathy, Engagement, and Self-Control, and the Problem Behaviors Domain, which is made up of items from the Externalizing Problems, Internalizing Problems, Hyperactivity/Inattention, Autism Spectrum, and Bullying subscales. Items are rated by frequency (e.g., never, seldom, often, almost always) through Likert-scale response options and provide information specific to behaviors that may adversely affect the child or adolescent’s ability to develop relationships or utilize specific social skills. This measure is commonly used to measure treatment outcome in SST interventions and has been shown to be sensitive to differences in social skill proficiency among autistic adolescents (Moody et al., 2022). Social skill proficiency and positive behavioral functioning is indicated by higher scores on the Social Skills Domain and lower scores on the Problem Behaviors Domain, respectively. In the current study, both domains showed strong internal consistency: SSIS Social Skills α = 0.906 and SSIS Problem Behaviors α = 0.863. The SSIS was administered to parents at pre- and post-intervention to assess treatment outcomes related to social skills and problem behaviors.
Social Responsiveness Scale, 2nd Edition
The Social Responsiveness Scale (SRS-2; Constantino & Gruber, 2012) is a 65-item rating scale completed by caregivers that measures social behavior generally indicative of autism and distinguishes those behavior patterns from other disorders. The validity and reliability of the SRS-2 as a quantitative measure of core autism features related to social responsiveness in general have been supported through various studies (Bruni, 2014; Cholemkery et al., 2014). Each question on the measure is rated from 1 (“not true”) to 4 (“almost always true”). The SRS-2 yields a total T-score (M = 50, SD = 10) and five subscales: Social Awareness, Social Cognition, Social Communication, Social Motivation, and Restricted, Repetitive Behaviors. Higher scores on this measure indicate greater autism features and social challenges (T-scores ≥ 60 are considered within the clinical range). In the current study, items contributing to the SRS-2 Total score demonstrated strong internal consistency, α = 0.923. The SRS-2 was completed by parents at pre- and post-intervention to assess treatment-related outcomes in social responsiveness.
Test of Adolescent Social Skills Knowledge
The Test of Adolescent Social Skills Knowledge (TASSK; Laugeson, 2014) is a 30-item criterion-based assessment of adolescents’ knowledge of the skills taught in the PEERS® for Adolescents intervention. Items include sentence stems and two response options. There are two items for each of the 15 skill-based lessons, excluding the graduation session. Higher scores on this measure suggest greater adolescent social skill knowledge. Similar to previous research (Laugeson et al., 2009; Moody et al., 2022), the TASSK displayed poor internal consistency, α = 0.422, in the current study. This is likely influenced by a number of factors, including the binary nature of the data, its assessment of multiple very distinct social skills, and its focus on social skills knowledge, which may be more uneven than measures of social behavior (e.g., some teens may exhibit appropriate social behavior without being able to identify or articulate the purpose or rules of social behavior). The TASSK was administered to adolescents at pre- and post-intervention to assess treatment response in social skills knowledge.
Quality of Socialization Questionnaire
The Quality of Socialization Questionnaire (QSQ; Laugeson, 2014) is a self-report measure adapted from the Quality of Play Questionnaire (QPQ; Frankel & Mintz, 2011) to better capture adolescent social engagement. The QSQ includes 12 items, which assess frequency of hosted and invited get-togethers with peers in the past month, as well as conflict during get-togethers. For the current study, total number of get-togethers at pre- and post-intervention was calculated by summing the number of hosted and invited get-togethers. In children, the QPQ number of playdates successfully discriminates clinical populations from community controls (Frankel & Mintz, 2011). The QSQ has been used as an outcome measure in previous studies of the PEERS® for Adolescents social skills intervention (Laugeson et al., 2009, 2012) and represents an ecologically valid, real-world outcome of social engagement. The QSQ was administered to adolescents at pre- and post-intervention to assess changes in adolescent social engagement.
Data Analyses
MANCOVAs were utilized given the use of multiple measures intended to capture social skills proficiency and functioning. To analyze baseline differences in social skills proficiency across diagnostic groups, a MANCOVA was conducted including all outcomes of interest at baseline, with post hoc tests to explore specific differences between the three diagnostic groups of ADHD, Autism, and ADHD + Autism. To assess differences in treatment response from pre- to post-intervention, a repeated measures MANCOVA was utilized, again including all outcomes of social functioning. If significant group by time interaction emerged, follow-up univariate repeated measures ANCOVAs were planned to probe diagnostic differences in change over the course of treatment. In all analyses, age (centered on the sample mean) was included as a covariate given the significant differences by diagnostic group.
Results
Baseline Comparison
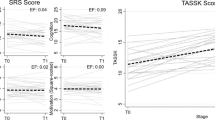
At baseline, the initial MANCOVA controlling for age revealed significant differences in social skill proficiency across the three diagnostic groupings (ADHD, Autism, ADHD + Autism), F(10,218) = 3.60, p < .001, with a large effect size, ηp2 = 1.42. Follow-up univariate ANCOVAs indicated that significant diagnostic differences emerged only on the SRS-2 Total score, F(2,138) = 12.68, p < .001, ηp2 = 1.55, and SSIS Social Skills Domain score, F(2,138) = 6.05, p = .003, ηp2 = 0.08. No significant differences at baseline emerged on adolescent problem behaviors, social skills knowledge, or get-togethers. On the SRS-2 specifically (see Fig. 1), post hoc comparisons with a Bonferroni correction indicated that those with ADHD (M = 67.1, SD = 9.8) were reported to have significantly fewer autism features and related social challenges than both the Autism group (M = 75.1, SD = 9.8), p < .001, and the ADHD + Autsim group (M = 77.2, SD = 9.7), p < .001. In contrast, on the SSIS Social Skills domain (see Fig. 2), adolescents in the ADHD + Autism group (M = 74.0, SD = 11.8) were rated as having significantly less well-developed social skill proficiency than either adolescents in the ADHD group (M = 82.5, SD = 11.9), p = .004, or the Autism group (M = 80.8, SD = 12.0), p = .019.
Treatment Response
A repeated measures MANCOVA, with age as a covariate and including all treatment outcomes, further revealed a nonsignificant diagnostic group by time interaction, F(10,214) = 1.34, p = .209, with a moderate effect size, ηp2 = 0.060. Given equivalence across diagnostic groups, repeated measures ANOVAs collapsed across the entire sample revealed significant differences over time from pre- to post-intervention on all measured outcomes with large effect sizes, in the expected directions, indicating improved social skill proficiency and reduced problem behaviors. Specifically, results indicated a significant reduction in impairments in social responsiveness on the SRS-2 from pre-intervention (M = 73.5, SD = 10.5) to post-intervention, (M = 66.1, SD = 10.1), F(1,138) = 82.95, p < .001, ηp2 = 0.37. Overall, parents also reported a significant improvement in social skills (Mpre = 79.3, SD = 12.3; Mpost = 87.1, SD = 12.0), F(1,139) = 68.81, p < .001, ηp2 = 0.33, and reduced problem behaviors on the SSIS (Mpre = 125.3, SD = 14.0; Mpost = 117.2, SD = 13.9), F(1,138) = 64.57, p < .001, ηp2 = 0.32. Adolescents themselves demonstrated that they learned the skills taught in PEERS®, as measured by the TASSK, with a 10 point increase on this measure (Mpre = 14.7, SD = 3.4; Mpost = 24.6, SD = 4.3), F(1,126) = 609.74, p < .001, ηp2 = 0.83. Lastly, adolescents also reported a significant increase in the number of get-togethers they had in the previous month from pre- to post-intervention, F(1,123) = 31.54, p < .001, ηp2 = 0.20. Prior to PEERS®, adolescents had 2.8 get-togethers (SD = 4.0) in the previous month. In contrast, after the program, they reported having 5.8 get-togethers (SD = 5.1) in the previous month. See Table 3 for estimated marginal means, controlling for age, for each diagnostic group and corresponding ANOVA results for the full sample on pre- and post- outcome measures.
Discussion
We aimed to examine SST treatment response in various diagnostic presentations of neurodevelopmental disorders in adolescents, specifically extending the PEERS® for Adolescents evidence base beyond autistic adolescents to include both adolescents with ADHD and autistic adolescents with ADHD. The overall findings indicated that PEERS® for Adolescents is effective in improving social and behavioral functioning among all three diagnostic groups.
Although all groups benefited similarly, there were significant differences across diagnostic groups at baseline on certain measures of social skill proficiency. Both groups of autistic teens (Autism, ADHD + Autism) had significantly higher levels of core autism features on the SRS-2 than those teens with ADHD only. These findings would be expected given that the SRS-2 is designed to capture autism-related social challenges and features — which would be less prevalent in an ADHD sample without autism. Interestingly, the co-occurring diagnostic group of autistic adolescents with ADHD presented with significantly lower social skill proficiency on the SSIS Social Skills Domain as compared to the other groups. This is consistent with previous findings that the co-occurrence of both these neurodevelopmental disorders results in more treatment needs (Zablotsky et al., 2020), though is incongruent with other findings that autistic adolescents with ADHD do not differ from autistic adolescents without ADHD with respect to social challenges (Dellapiazza et al., 2021; Harkins et al., 2021).
The current results suggest that all three groups significantly improved, and to a similar degree, across all outcomes following PEERS® for Adolescents. The relative consistency in treatment response across diagnostic groups is especially interesting given baseline differences in social responsiveness and social skills. It is possible that the curriculum, which covers both foundational and complex skills, creates a context in which adolescents across a wide range of starting skills were able to benefit. Additionally, the equivalence in treatment gains may also reflect a consistent dose (16 weeks) of individualized social skills support via social coaching and homework review. Teens and parents may also have been susceptible to bias given their participation in the intervention and lack of blinding. Though additional study is needed, these results are especially encouraging given that previous research has only produced mixed or weak support for SST in ADHD (Morris et al., 2021; Storebø et al., 2019; Willis et al., 2019). In contrast, the present findings suggest that PEERS® for Adolescents may enhance the social skills and social functioning of youth with ADHD.
The pervasive gains across adolescent-reported outcomes of social skills knowledge and frequency of get-togethers, as well as parent-reported outcomes of social skills (SSIS), behavioral functioning (SSIS), and social responsivness (SRS-2) further bolster confidence in the efficacy of PEERS® for Adolescents for both non-autistic youth with ADHD and autistic youth with ADHD. Effect size estimates in the current study, which were considered large on all outcomes, were generally greater than the pooled effect sizes reported in meta-analytic results of the PEERS® for Adolescents program in autistic adolescents for the TASSK (large effects), SRS-2 (moderate to large effects), SSIS-SS (moderate to large effects), and QSQ report of get-togethers (moderate effects; Zheng et al., 2021). This may be expected given that the current study was conducted at UCLA, where PEERS® was developed, under the supervision of the developer, and in North America, the original cultural context. These factors are consistent with findings from the meta-analysis, which showed greater effects under these circumstances (Zheng et al., 2021). Of note, the magnitude of the effects showed a similar pattern as in the meta-analysis, such that the greatest effect size emerged on the TASSK and relatively smaller effects on the QSQ.
Across these neurodivergent youth, the increased frequency of get-togethers (QSQ) with peers suggests that social skills improvements being reported on standardized measures are indeed generalizing to contexts outside of treatment, resulting in more interactions with peers. Furthermore, the use of a real-world sample in an operating outpatient treatment setting also serves as a strength of this study. By including clinical complexity, such as the presence of other co-occurring mental health disorders like anxiety, the findings suggest the successful translation of PEERS® for Adolescents from closely controlled research samples to outpatient community settings.
Given that youth with ADHD may be more likely to experience significant peer rejection and social challenges, which may in turn negatively impact other areas of functioning (e.g., academics, mental health), PEERS® for Adolescents may be a powerful tool to ameliorate negative outcomes and provide support for teens with ADHD. The extension of PEERS® for Adolescents for use with this population has several advantages given the existing infrastructure to support rapid widespread dissemination and access, through the PEERS® global network of certified providers, publicly available manuals, translated and culturally validated protocols, and existing adaptations to be delivered in school-based settings. In summary, these findings suggest that participation in PEERS® for Adolescents may produce meaningful improvements in social engagement and relationship development for adolescents diagnosed with ADHD, autism, and/or co-occurring ADHD and autism.
Limitations and Future Directions
Although promising, the results of the current study are limited primarily in sample demographics and methodological rigor. We recognize there are many factors involved in social behavior variance including but not limited to individual experience (e.g., trauma history, emotional state), co-occurring diagnoses, local community culture, and generational/cohort effects. With lower representation of diverse racial and ethnic identities, particularly of Black youth, we are unable to confidently generalize these findings to all racial and ethnic groups. Additionally, as is often typical in autism research, the majority male sample warrants future investigation to confirm benefits in female-identifying participants as well as nonbinary participants, using oversampling to ensure adequate power. Although we limited our sample to clinical participants who completed the program in 2014 or later, it is possible that some participants with co-occurring autism and ADHD had not yet received both diagnoses given the recency of the DSM-5 change in 2013.
With regard to methodological rigor, analyses were conducted on archival clinical data from an outpatient treatment setting and were not collected in the context of a research study. Due to this methodological limitation, thorough and strict characterization of the sample (e.g., independent confirmation of diagnosis, assessment of ADHD symptom severity), random assignment, and blinded informants were not possible. Additionally, precise data on treatment fidelity were not collected in this clinical context; however, given the manualized and didactic nature of the PEERS® for Adolescents curriculum, weekly supervision and case conference meetings, and team monitoring throughout each group, the risk of significant deviations from treatment protocol is low. Outcomes measured at pre- and post-intervention intervals did not account for long-term follow-up after intervention, limiting our knowledge regarding persistence of social skill gains across the diagnostic groups assessed. Additionally, these outcomes did not include observational measures or school-based informants, such as teachers, to assess the full extent of skills generalization and external validity.
In addition to outcome measurement, it is also essential that social validity data be collected from youth with ADHD and their families who participate in PEERS® for Adolescents to enhance knowledge of the acceptability and feasibility of this intervention in this population, as well as their overall satisfaction. Systematic exploration into barriers in treatment and reasons for discontinuing the program before completion would also be critical to inform future clinical practice. Anecdotally, we have experienced families and youth with neurodevelopmental disorders (i.e., autism, ADHD) to be very satisfied with the program, including its teaching methods and feasibility, though concrete data would increase confidence in relation to broader dissemination and recommendations.
Future research might also replicate the current findings using a randomized control trial design with additional outcome measures (e.g., teacher reports, observational assessments, follow-up timepoints) to ensure benefits are attributable to the intervention, are generalizable, and maintain over time. Additional recruitment of more diverse samples representative of the USA and beyond will also enhance confidence in using PEERS® for Adolescents in community clinical practice with marginalized communities. As this study is the second to directly test and provide evidence for the use of PEERS® for Adolescents in youth with ADHD, it would also be beneficial to examine moderators of treatment response for this population, as they may be distinct from moderators for autistic adolescents.
Notes
We acknowledge that language is dynamic and that individual preferences related to describing disabilities may differ. Due to the preferences of the autistic self-advocate community (Bury et al., 2023; Taboas et al., 2023), we have chosen to utilize identity-first language when referring to autistic people. As there is no identity-first construction for ADHD, person-first language (“adolescents with ADHD”) is utilized.
References
Aduen, P. A., Day, T. N., Kofler, M. J., Harmon, S. L., Wells, E. L., & Sarver, D. E. (2018). Social problems in ADHD: Is it a skills acquisition or performance problem? Journal of Psychopathology and Behavioral Assessment, 40, 440–451. https://doi.org/10.1007/s10862-018-9649-7
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.). American Psychiatric Publishing. https://doi.org/10.1176/appi.books.9780890425596
Antshel, K. M., & Russo, N. (2019). Autism spectrum disorders and ADHD: Overlapping phenomenology, diagnostic issues, and treatment considerations. Current Psychiatry Reports, 21(5), 1–11. https://doi.org/10.1007/s11920-019-1020-5
Baker, E., Veytsman, E., Martin, A. M., Blacher, J., & Stavropoulos, K. K. (2020). Increased neural reward responsivity in adolescents with ASD after social skills intervention. Brain Sciences, 10(6), 402. https://doi.org/10.3390/brainsci10060402
Becker, S. P., Mehari, K. R., Langberg, J. M., & Evans, S. W. (2017). Rates of peer victimization in young adolescents with ADHD and associations with internalizing symptoms and self-esteem. European Child & Adolescent Psychiatry, 26(2), 201–214. https://doi.org/10.1007/s00787-016-0881-y
Bruni, T. P. (2014). Test review: Social responsiveness scale–Second edition (SRS-2). Journal of Psychoeducational Assessment, 32(4), 365–369. https://doi.org/10.1177/0734282913517525
Bury, S. M., Jellett, R., Spoor, J. R., & Hedley, D. (2023). “It defines who I am” or “It’s something I have”: What language do [autistic] Australian adults [on the autism spectrum] prefer? Journal of Autism and Developmental Disorders, 53(2), 677–687. https://doi.org/10.1007/s10803-020-04425-3
Chen, J. L., Leader, G., Sung, C., & Leahy, M. (2015). Trends in employment for individuals with autism spectrum disorder: A review of the research literature. Review Journal of Autism and Developmental Disorders, 2(2), 115–127. https://doi.org/10.1007/s40489-014-0041-6
Chiang, H. M., Cheung, Y. K., Li, H., & Tsai, L. Y. (2013). Factors associated with participation in employment for high school leavers with autism. Journal of Autism and Developmental Disorders, 43(8), 1832–1842. https://doi.org/10.1007/s10803-012-1734-2
Cholemkery, H., Mojica, L., Rohrmann, S., Gensthaler, A., & Freitag, C. M. (2014). Can autism spectrum disorders and social anxiety disorders be differentiated by the social responsiveness scale in children and adolescents? Journal of Autism and Developmental Disorders, 44(5), 1168–1182. https://doi.org/10.1007/s10803-013-1979-4
Constantino, J. N., & Gruber, C. P. (2012). Social responsiveness scale: SRS-2. Western Psychological Services.
Craig, F., Margari, F., Legrottaglie, A. R., Palumbi, R., De Giambattista, C., & Margari, L. (2016). A review of executive function deficits in autism spectrum disorder and attention-deficit/hyperactivity disorder. Neuropsychiatric Disease and Treatment, 1191–1202. https://doi.org/10.2147/NDT.S104620
De Haan, A. M., Boon, A. E., De Jong, J. T., Hoeve, M., & Vermeiren, R. R. (2013). A meta-analytic review on treatment dropout in child and adolescent outpatient mental health care. Clinical Psychology Review, 33(5), 698–711. https://doi.org/10.1016/j.cpr.2013.04.005
Dellapiazza, F., Audras-Torrent, L., Michelon, C., & Baghdadli, A. (2021). Clinical characteristics of children with ASD and comorbid ADHD: Association with social impairment and externalizing and internalizing behaviours. Research in Developmental Disabilities, 113, 103930. https://doi.org/10.1016/j.ridd.2021.103930
Dvorsky, M. R., & Langberg, J. M. (2016). A review of factors that promote resilience in youth with ADHD and ADHD symptoms. Clinical Child and Family Psychology Review, 19(4), 368–391. https://doi.org/10.1007/s10567-016-0216-z
Dvorsky, M. R., Langberg, J. M., Evans, S. W., & Becker, S. P. (2018). The protective effects of social factors on the academic functioning of adolescents with ADHD. Journal of Clinical Child & Adolescent Psychology, 47(5), 713–726. https://doi.org/10.1080/15374416.2016.1138406
Eyre, O., Hughes, R. A., Thapar, A. K., Leibenluft, E., Stringaris, A., Davey Smith, G., … & Thapar, A. (2019). Childhood neurodevelopmental difficulties and risk of adolescent depression: the role of irritability. Journal of Child Psychology and Psychiatry, 60(8), 866–874. https://doi.org/10.1111/jcpp.13053
Frankel, F., & Mintz, J. (2011). Maternal reports of play dates of clinic referred and community children. Journal of Child and Family Studies, 20(5), 623–630. https://doi.org/10.1007/s10826-010-9437-9
Gardner, D. M., Gerdes, A. C., & Weinberger, K. (2019). Examination of a parent-assisted, friendship-building program for adolescents with ADHD. Journal of Attention Disorders, 23(4), 363–373. https://doi.org/10.1177/1087054715588188
Gonring, K., Gerdes, A., & Gardner, D. (2017). Program for the education and enrichment of relational skills: Parental outcomes with an ADHD sample. Child & Family Behavior Therapy, 39(1), 19–42. https://doi.org/10.1080/07317107.2016.1268003
Gordon-Lipkin, E., Marvin, A. R., Law, J. K., & Lipkin, P. H. (2018). Anxiety and mood disorder in children with autism spectrum disorder and ADHD. Pediatrics, 141(4), e20171377. https://doi.org/10.1542/peds.2017-1377
Gresham, F., & Elliott, S. N. (2008). Social skills improvement system (SSIS) rating scales. SSIS Rating Scales. Pearson.
Harkins, C. M., Handen, B. L., & Mazurek, M. O. (2021). The Impact of the Comorbidity of ASD and ADHD on Social Impairment. Journal of Autism and Developmental Disorders, 1–11. https://doi.org/10.1007/s10803-021-05150-1
Hartman, C. A., Geurts, H. M., Franke, B., Buitelaar, J. K., & Rommelse, N. N. (2016). Changing ASD-ADHD symptom co-occurrence across the lifespan with adolescence as crucial time window: Illustrating the need to go beyond childhood. Neuroscience & Biobehavioral Reviews, 71, 529–541. https://doi.org/10.1016/j.neubiorev.2016.09.003
Hours, C., Recasens, C., & Baleyte, J. M. (2022). ASD and ADHD comorbidity: What are we talking about? Frontiers in Psychiatry, 13, 154. https://doi.org/10.3389/fpsyt.2022.837424
Hsiao, M. N., Tseng, W. L., Huang, H. Y., & Gau, S. S. F. (2013). Effects of autistic traits on social and school adjustment in children and adolescents: The moderating roles of age and gender. Research in Developmental Disabilities, 34(1), 254–265. https://doi.org/10.1016/j.ridd.2012.08.001
Hume, K., Steinbrenner, J. R., Odom, S. L., Morin, K. L., Nowell, S. W., Tomaszewski, B., ... & Savage, M. N. (2021). Evidence-based practices for children, youth, and young adults with autism: Third generation review. Journal of Autism and Developmental Disorders, 51(11), 4013–4032. https://doi.org/10.1007/s10803-020-04844-2
Humphreys, K. L., Katz, S. J., Lee, S. S., Hammen, C., Brennan, P. A., & Najman, J. M. (2013). The association of ADHD and depression: Mediation by peer problems and parent–child difficulties in two complementary samples. Journal of Abnormal Psychology, 122(3), 854. https://doi.org/10.1037/a0033895
Jang, J., Matson, J. L., Williams, L. W., Tureck, K., Goldin, R. L., & Cervantes, P. E. (2013). Rates of comorbid symptoms in children with ASD, ADHD, and comorbid ASD and ADHD. Research in Developmental Disabilities, 34(8), 2369–2378. https://doi.org/10.1016/j.ridd.2013.04.021
Kasari, C., Locke, J., Gulsrud, A., & Rotheram-Fuller, E. (2011). Social networks and friendships at school: Comparing children with and without ASD. Journal of Autism and Developmental Disorders, 41(5), 533–544. https://doi.org/10.1007/s10803-010-1076-x
Laugeson, E. A. (2014). The PEERS® curriculum for school based professionals: Social skills training for adolescents with autism spectrum disorder. Routledge. https://doi.org/10.4324/9780203102374
Laugeson, E. A., & Frankel, F. (2010). Social skills for teenagers with developmental and autism spectrum disorders: The PEERS treatment manual. Routledge. https://doi.org/10.4324/9780203867686
Laugeson, E. A., Frankel, F., Mogil, C., & Dillon, A. R. (2009). Parent-assisted social skills training to improve friendships in teens with autism spectrum disorders. Journal of Autism and Developmental Disorders, 39(4), 596–606. https://doi.org/10.1007/s10803-008-0664-5
Laugeson, E. A., Frankel, F., Gantman, A., Dillon, A. R., & Mogil, C. (2012). Evidence-based social skills training for adolescents with autism spectrum disorders: The UCLA PEERS program. Journal of Autism and Developmental Disorders, 42(6), 1025–1036. https://doi.org/10.1007/s10803-011-1339-1
Lecavalier, L., Smith, T., Johnson, C., Bearss, K., Swiezy, N., Aman, M. G., Sukhodolsky, D. G., Deng, Y., Dziura, J., & Scahill, L. (2017). Moderators of parent training for disruptive behaviors in young children with autism spectrum disorder. Journal of Abnormal Child Psychology, 45(6), 1235–1245. https://doi.org/10.1007/s10802-016-0233-x
Lordo, D. N., Bertolin, M., Sudikoff, E. L., Keith, C., Braddock, B., & Kaufman, D. A. (2017). Parents perceive improvements in socio-emotional functioning in adolescents with ASD following social skills treatment. Journal of Autism and Developmental Disorders, 47(1), 203–214. https://doi.org/10.1007/s10803-016-2969-0
Maiano, C., Normand, C. L., Salvas, M. C., Moullec, G., & Aimé, A. (2016). Prevalence of school bullying among youth with autism spectrum disorders: A systematic review and meta-analysis. Autism Research, 9(6), 601–615. https://doi.org/10.1002/aur.1568
Mayes, S. D., Calhoun, S., Bixler, E. O., & Vgontzas, A. N. (2009). Sleep problems in children with autism, ADHD, anxiety, depression, acquired brain injury, and typical development. Sleep Medicine Clinics, 4(1), 19–25. https://doi.org/10.1016/j.jsmc.2008.12.004
Mayes, S. D., Calhoun, S. L., Murray, M. J., & Zahid, J. (2011). Variables associated with anxiety and depression in children with autism. Journal of Developmental and Physical Disabilities, 23(4), 325–337. https://doi.org/10.1007/s10882-011-9231-7
Mayes, S. D., Calhoun, S. L., Mayes, R. D., & Molitoris, S. (2012). Autism and ADHD: Overlapping and discriminating symptoms. Research in Autism Spectrum Disorders, 6(1), 277–285. https://doi.org/10.1016/j.rasd.2011.05.009
McVey, A. J., Dolan, B. K., Willar, K. S., Pleiss, S., Karst, J. S., Casnar, C. L., Caiozzo, C., Vogt, E. M., Gordon, N. S., & Van Hecke, A. V. (2016). A replication and extension of the PEERS® for young adults social skills intervention: Examining effects on social skills and social anxiety in young adults with autism spectrum disorder. Journal of Autism and Developmental Disorders, 46(12), 3739–3754. https://doi.org/10.1007/s10803-016-2911-5
Mikami, A. Y., Smit, S., & Khalis, A. (2017). Social skills training and ADHD—What works? Current Psychiatry Reports, 19(12), 1–9. https://doi.org/10.1007/s11920-017-0850-2
Mikami, A. Y., Miller, M., & Lerner, M. D. (2019). Social functioning in youth with attention-deficit/hyperactivity disorder and autism spectrum disorder: Transdiagnostic commonalities and differences. Clinical Psychology Review, 68, 54–70. https://doi.org/10.1016/j.cpr.2018.12.005
Moody, C. T., & Laugeson, E. A. (2020). Social skills training in autism spectrum disorder across the lifespan. The Psychiatric Clinics of North America, 43(4), 687–699. https://doi.org/10.1016/j.psc.2020.08.006
Moody, C. T., Schiltz, H. K., Ratto, A. B., Gulsrud, A. C., & Laugeson, E. A. (2022). Measurement of social skills treatment outcome in autism: Moving beyond informant report and considering diversity. International Review of Research in Developmental Disabilities, 62, 265–312.
Morris, S., Sheen, J., Ling, M., Foley, D., & Sciberras, E. (2021). Interventions for adolescents with ADHD to improve peer social functioning: A systematic review and meta-analysis. Journal of Attention Disorders, 25(10), 1479–1496. https://doi.org/10.1177/1087054720906514
Normand, S., Schneider, B. H., Lee, M. D., Maisonneuve, M. F., Chupetlovska-Anastasova, A., Kuehn, S. M., & Robaey, P. (2013). Continuities and changes in the friendships of children with and without ADHD: A longitudinal, observational study. Journal of Abnormal Child Psychology, 41(7), 1161–1175. https://doi.org/10.1007/s10802-013-9753-9
Petrina, N., Carter, M., & Stephenson, J. (2014). The nature of friendship in children with autism spectrum disorders: A systematic review. Research in Autism Spectrum Disorders, 8(2), 111–126. https://doi.org/10.1016/j.rasd.2013.10.016
Rabin, S. J., Laugeson, E. A., Mor-Snir, I., & Golan, O. (2020). An Israeli RCT of PEERS®: Intervention effectiveness and the predictive value of parental sensitivity. Journal of Clinical Child and Adolescent Psychology, 50(6), 933–949. https://doi.org/10.1080/15374416.2020.1796681
Ragelienė, T. (2016). Links of adolescents identity development and relationship with peers: A systematic literature review. Journal of the Canadian Academy of Child and Adolescent Psychiatry, 25(2), 97–105.
Ratcliffe, B., Wong, M., Dossetor, D., & Hayes, S. (2015). The association between social skills and mental health in school-aged children with autism spectrum disorder, with and without intellectual disability. Journal of Autism and Developmental Disorders, 45(8), 2487–2496. https://doi.org/10.1007/s10803-015-2411-z
Rong, Y., Yang, C. J., Jin, Y., & Wang, Y. (2021). Prevalence of attention-deficit/hyperactivity disorder in individuals with autism spectrum disorder: A meta-analysis. Research in Autism Spectrum Disorders, 83, 101759. https://doi.org/10.1016/j.rasd.2021.101759
Ros, R., & Graziano, P. A. (2018). Social functioning in children with or at risk for attention deficit/hyperactivity disorder: A meta-analytic review. Journal of Clinical Child & Adolescent Psychology, 47(2), 213–235. https://doi.org/10.1080/15374416.2016.1266644
Russell, G., Kapp, S. K., Elliott, D., Elphick, C., Gwernan-Jones, R., & Owens, C. (2019). Mapping the Autistic Advantage from the Accounts of Adults Diagnosed with Autism: A Qualitative Study. Autism in Adulthood: Challenges and Management, 1(2), 124–133. https://doi.org/10.1089/aut.2018.0035
Schiltz, H. K., McVey, A. J., Dolan, B. K., Willar, K. S., Pleiss, S., Karst, J. S., ... & Van Hecke, A. V. (2018). Changes in depressive symptoms among adolescents with ASD completing the PEERS® social skills intervention. Journal of Autism and Developmental Disorders, 48(3), 834–843. https://doi.org/10.1007/s10803-017-3396-6
Sciberras, E., Roos, L. E., & Efron, D. (2009). Review of prospective longitudinal studies of children with ADHD: Mental health, educational, and social outcomes. Current Attention Disorders Reports, 1(4), 171–177. https://doi.org/10.1007/s12618-009-0024-1
Sedgwick, J. A., Merwood, A., & Asherson, P. (2019). The positive aspects of attention deficit hyperactivity disorder: A qualitative investigation of successful adults with ADHD. Attention Deficit and Hyperactivity Disorders, 11(3), 241–253. https://doi.org/10.1007/s12402-018-0277-6
Sprenger, L., Bühler, E., Poustka, L., Bach, C., Heinzel-Gutenbrunner, M., Kamp-Becker, I., & Bachmann, C. (2013). Impact of ADHD symptoms on autism spectrum disorder symptom severity. Research in Developmental Disabilities, 34(10), 3545–3552. https://doi.org/10.1016/j.ridd.2013.07.028
Storebø, O. J., Andersen, M. E., Skoog, M., Hansen, S. J., Simonsen, E., Pedersen, N., ... & Gluud, C. (2019). Social skills training for attention deficit hyperactivity disorder (ADHD) in children aged 5 to 18 years. Cochrane Database of Systematic Reviews, 6(6), CD008223. https://doi.org/10.1002/14651858.CD008223.pub3
Taboas, A., Doepke, K., & Zimmerman, C. (2023). Preferences for identity-first versus person-first language in a US sample of autism stakeholders. Autism, 27(2), 565–570. https://doi.org/10.1177/13623613221130845
Taheri, A., Perry, A., & Minnes, P. (2016). Examining the social participation of children and adolescents with intellectual disabilities and autism spectrum disorder in relation to peers. Journal of Intellectual Disability Research, 60(5), 435–443. https://doi.org/10.1111/jir.12289
Taylor, L. A., Saylor, C., Twyman, K., & Macias, M. (2010). Adding insult to injury: Bullying experiences of youth with attention deficit hyperactivity disorder. Children’s Health Care, 39(1), 59–72. https://doi.org/10.1080/02739610903455152
Van Hecke, A. V., Stevens, S., Carson, A. M., Karst, J. S., Dolan, B., Schohl, K., ... & Brockman, S. (2015). Measuring the plasticity of social approach: A randomized controlled trial of the effects of the PEERS intervention on EEG asymmetry in adolescents with autism spectrum disorders. Journal of Autism and Developmental Disorders, 45(2), 316–335. https://doi.org/10.1007/s10803-013-1883-y
White, H. A., & Shah, P. (2006). Uninhibited imaginations: Creativity in adults with attention-deficit/hyperactivity disorder. Personality and Individual Differences, 40(6), 1121–1131. https://doi.org/10.1016/j.paid.2005.11.007
Willis, D., Siceloff, E. R., Morse, M., Neger, E., & Flory, K. (2019). Stand-alone social skills training for youth with ADHD: A systematic review. Clinical Child and Family Psychology Review, 22(3), 348–366. https://doi.org/10.1007/s10567-019-00291-3
Zablotsky, B., Bramlett, M. D., & Blumberg, S. J. (2020). The co-occurrence of autism spectrum disorder in children with ADHD. Journal of Attention Disorders, 24(1), 94–103. https://doi.org/10.1177/1087054717713638
Zheng, S., Kim, H., Salzman, E., Ankenman, K., & Bent, S. (2021). Improving social knowledge and skills among adolescents with autism: Systematic review and meta-analysis of UCLA PEERS® for adolescents. Journal of Autism and Developmental Disorders, 51(12), 4488–4503. https://doi.org/10.1007/s10803-021-04885-1
Acknowledgements
The authors would like to acknowledge the UCLA PEERS® Clinic team including staff and research assistants who assisted with running groups and scoring and entering data. We would also like to thank the adolescents and families who participated in our clinical groups over many years and made this research possible.
Author information
Authors and Affiliations
Contributions
ZFG and EAL contributed to the study conception, generation of research question, and design. EAL, HAM, DB, and SB led and coordinated PEERS®® for Adolescents group and facilitated collection of data used in the current study. CTM oversaw data management, conducted the data analysis, and interpreted results. ZFG, CTM, and HAM collaboratively co-authored first draft of manuscript. All authors contributed to editing and approval of final manuscript.
Corresponding author
Ethics declarations
EAL receives royalties from Routledge for sales of the PEERS® treatment manuals. All other authors have no financial conflicts of interest or non-financial conflicts of interests to disclose. This article utilizes data originally collected through a clinical outcome database for purposes of program evaluation. The Institutional Review Board at University of California, Los Angeles approved the use of this data for secondary analysis for the purpose of this research. Data supporting this study are not publicly available given specifications of IRB approval for data usage. No financial support or funding was received to assist with data collection or preparation of this manuscript.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Geannopoulos, Z.F., Moody, C.T., McGregor, H.A. et al. Outcomes in PEERS® for Adolescents Across Neurodevelopmental Disorders: ADHD, Autism, and Their Co-occurrence. Adv Neurodev Disord (2024). https://doi.org/10.1007/s41252-023-00380-z
Accepted:
Published:
DOI: https://doi.org/10.1007/s41252-023-00380-z