Abstract
Objectives
Whole-body vibration training (WBVT) has been emerging as a promising therapeutic modality for cerebral palsy (CP); however, reported efficacy is inconsistent and methodological approaches differ substantially. This study aimed to review the methodological protocols adopted by randomised controlled trials reporting on the efficacy of WBVT for people with CP.
Methods
Electronic databases were searched for randomised controlled trials reporting on the efficacy of WBVT for people with CP. Data were extracted from included studies related to study and participant characteristics and WBVT protocols including training programmes, patient positioning, and machine and vibration specifications.
Results
Eighteen randomised controlled trials were identified. Training programmes varied considerably, including duration, number of sessions per week, session length, and whether static, dynamic, or combination exercises were performed. Positioning of participants on the vibration platform also varied, including foot, knee, hip, and hand positioning. The machine specifications were poorly reported, with variations in frequency, amplitude, and peak acceleration settings.
Conclusions
This review highlights the inconsistency in the use and reporting of training protocols, machine specifications, and patient positioning when investigating the efficacy of WBVT for people with CP. Current clinical trials continue to poorly acknowledge WBVT research recommendations, which may contribute to ongoing misunderstanding of basic WBVT principals and safety considerations, as well as contribute to the inconclusive results with regard to treatment efficacy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Cerebral palsy (CP) describes an array of disorders that result from static lesions of the developing and neonate brain, causing deficits in movement and postural control (Rosenbaum et al., 2007). With an estimated prevalence of 2 per 1000 live births (Oskoui et al., 2013), CP is the most common childhood physical disability. People with CP experience difficulty in walking and performing other functional activities due to impairments in muscle strength and coordination, as well as muscle spasticity (Nelson & Boyer, 2021). These impairments adversely affect daily activities, social interactions, and overall quality of life (Makris et al., 2021; Pirpiris et al., 2006).
In recent years, the evidence base for CP management has grown considerably, with over one hundred different therapeutic interventions reported in the literature (Novak et al., 2020). The primary goals for management of people with CP are aimed at improving mobility and function. Common conservative treatments include physical therapy, occupational therapy, orthoses and oral medications, neurodevelopmental treatment, and exercise (passive stretching, static weight-bearing, strength training, and cardiovascular fitness). Although several systematic reviews and meta-analyses have illustrated the potential role of these interventions for people with CP, results on functional improvements are inconsistent (Bania et al., 2019; Booth et al., 2018; Liang et al., 2021; Morgan et al., 2014, 2016; Papavasiliou, 2009; Ryan et al., 2017), and alternative treatment modalities are being increasingly discussed and sought by families of children with CP.
In the past two decades, whole-body vibration training (WBVT) has been emerging as a promising therapeutic modality for CP and has been shown to improve gross motor function, reduce spasticity and contracture, and improve passive range of motion (Novak et al., 2020). WBVT involves the use of energy produced from an oscillating mechanical vibration platform which is transferred through a person, thereby producing vibration of the whole body (Lorenzen et al., 2009; Rittweger, 2010). WBVT has several advantages over other therapeutic interventions, including reduced strain and risk of injury, providing a more passive training activity, and a shorter time to complete training sessions (Ruhde & Hulla, 2022).
The overall effectiveness of WBVT is determined by the combined effect of the machine vibrations/force and the correct biomechanical position of the patient. Recommendations have been published in regard to undertaking and reporting research using WBVT (Rauch et al., 2010; van Heuvelen et al., 2021; Wuestefeld et al., 2020). However, the methodological approaches differ substantially across studies, with heterogeneity in almost all methodological aspects, including WBVT protocols, vibration platform settings, and patient positioning on the platform (Duquette et al., 2015; Khan et al., 2021; Ritzmann et al., 2018), suggesting that the proposed recommendations have not been adhered to. In conjunction with the lack of standardised terminology (Lorenzen et al., 2009), there is a “replication crisis” evident in current WBVT research, which may also contribute to the inconsistency in reported WBVT efficacy. Inappropriate training techniques and vibration intensities may also promote injury and concerns have been raised about the use of WBVT for children with disabilities (Leite et al., 2019).
This systematic review aims to evaluate the methodological protocols adopted by randomised controlled trials reporting on the efficacy of WBVT for people with CP, and to provide recommendations to improve the quality, standardisation, and safety of WBVT research for this population.
Method
This review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement (Moher et al., 2009).
Pragmatic (Lived Experience) Collaborative Research Partners
The work arose through discussion between DP, LS, and KO. KO has lived experience of CP and regular use of different types of vibration machines. LS is a Royal New Zealand navy-trained engineer who has advised key design improvements for at least four commercial vibration plate companies. LS also runs a studio in New Zealand using five types of vibration machines, and since 2004 has offered free advice and use of the machines for many people with disabilities, including CP. The programme of work and study protocol was developed through discussion between LS, KO, DP, and SS. Contributions to the extraction of data, study interpretation, and, in particular, recommendations were developed in partnership with the collaborative research partners.
Search Strategy
Using relevant search terms ((“whole body vibration” OR “whole-body vibration” OR wbv OR wbvt) AND “cerebral palsy”), the following electronic databases were searched in April 2022 and updated in November 2022: Allied and Complementary Medicine (AMED), Web of Science, Scopus, MEDLINE, The Cumulative Index to Nursing and Allied Health Literature (CINAHL), and Sport Discus. Reference lists of retrieved studies and reviews were also hand-searched to identify additional studies. No time restrictions were placed on the search.
Studies were included if they were randomised controlled trials which involved human participants with a diagnosis of cerebral palsy and reported using whole body vibration training or therapy as an intervention. Only papers published in English were included and there were no restrictions based on the age or gender of participants, or the vibration device used. Studies which reported using segmental or local vibration training (i.e. not whole body) were excluded, as they do not involve vibration of the whole body which the term WBVT infers (Bosco et al., 1998; Cronin et al., 2007). Review articles, conference proceedings, protocols, editorials, and letters to the editor were also excluded.
All identified studies were exported into Rayyan (http://rayyan.qcri.org), an online systematic review application (Johnson & Phillips, 2018), and duplicates removed. Two independent reviewers (DP, KO) screened titles and abstracts against the above criteria and studies not relevant were excluded. Full texts of the remaining studies were then reviewed by two independent reviewers (DP, KO) to confirm eligibility. Any disagreements were discussed by consensus with a third reviewer (SS).
Quality Assessment
The quality of included studies was assessed independently by two reviewers (DP, SS) using the 6-item modified Jadad scale which assesses randomisation, blinding, withdrawals, dropouts, inclusion/exclusion criteria, adverse events, and statistical analysis (Oremus et al., 2001). The scale has a maximum score of 8 points, with low-quality studies yielding scores of 0 to 3 and high-quality studies yielding scores of 4 to 8. Any disagreements in the quality assessment were resolved by discussion between the two reviewers.
Data Extraction
Two independent reviewers (DP, KO) extracted data from each included study into a standardised data extraction sheet in Microsoft Excel. Extracted data included study characteristics (first author surname, publication year, country of first author, and study design) and participant characteristics for each group (sample size, gender, age, inclusion/exclusion criteria, and description of interventions). Data relating to the WBVT programmes were extracted, including the total duration of the training (weeks), total session length (minutes), exercise and rest times (minutes), and exercise type (static/dynamic/combination). Patient position data related to foot, knee, hip, trunk, elbow, and hand positioning was extracted, as were data related to machine and vibration specifications: brand and model of machine, year of machine, type of vibration (i.e. lineal (vertical or synchronous) or pivotal (side-alternating)), frequency (hertz), amplitude (mm), peak acceleration (g), peak-to-peak displacement (mm), force (kN), and whether or not the machine (via accelerometer and force transducer) was independently tested by an engineer prior to the training (to ensure the machines are complying with a number of specifications related to engineering requirements and principles (Larbi et al., 2020)). Finally, data reporting any adverse events were extracted.
Data Synthesis
Data relating to the study and participant characteristics, training programme protocols, patient positioning, and machine specifications were summarised in tables using descriptive statistics.
Results
Study and Participant Characteristics
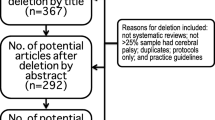
A total of 196 studies were identified across the database searches (Fig. 1). After removal of duplicates, 98 studies were screened based on title and abstract, of which 29 were included in the full-text screening stage. Of these, 11 were excluded (reasons are described in Fig. 1), and a total of 18 studies are included in the current review.
Figure 2 displays the quality assessment scores for the 18 included studies according to the Jadad scale. Although all studies were randomised, only seven (39%) described an appropriate method of randomisation. No studies were described as double-blind. Six (33%) studies provided a description of withdrawals and dropouts, and all but one study (94%) provided a clear description of the inclusion and exclusion criteria. Only one study (6%) described the method used to assess adverse effects and 17 (94%) studies described the methods of statistical analysis used. The total Jadad score ranged from 1 to 5 (mean (SD): 2.5 (0.9)).
Study and participant characteristics of the included studies are presented in Supplementary Table 1. Fourteen (78%) studies were randomised controlled trials, and four (22%) were randomised cross-over trials. The experimental groups all received WBVT with or without interventions also received by the control groups (including resistance training, physical therapy, passive stretching, suit therapy, hippotherapy (utilisation of the natural gait and movement of a horse to provide motor and sensory input), and core stability). Total sample sizes across the included studies ranged from 12 to 60 participants with CP. Seventeen studies included paediatric populations (age range 4–18 years) with one study including adult participants with CP (mean age 31 years) (Ahlborg et al., 2006).
Training Programme Protocols
Table 1 presents details of the WBVT programme protocols used, which varied considerably across the included studies. Duration of the training programme ranged from 3 to 24 weeks, with number of sessions per week ranging from 2 to 10. The total session length ranged from 9 to 60 min with exercise times ranging from 30 to 600 s, and rest periods ranging from 15 to 180 s. Static exercises were the most commonly performed (n = 12, 67% studies), with the remaining studies using combinations of static and dynamic exercises (n = 6, 33% studies).
Patient Positioning
The majority of studies undertook WBVT with the participants in a static standing position (n = 8, 44%), followed by a squat position (n = 3, 17%), or a combination of standing and dynamic exercises (n = 7, 39%) (Table 2). Foot positioning was described in 13 (72%) studies, with the majority instructing participants to stand with equal weight on both legs at an equal distance from the centre line on the vibrating platform. Two (11%) studies performed the vibration exercises with shoes on, four (22%) with participants barefoot, and the remaining 12 (67%) did not specify the footwear condition used. Twelve (67%) studies described the knee position which was flexed anywhere between 10 and 100° from full extension. Hip positioning was described by four (22%) studies in which hip flexion ranged from 10 to 50°. The trunk position was described by only three (17%) studies which reported using a belt or support to stabilise the trunk. No studies reported elbow positioning. Four (22%) studies instructed participants to hold on to handles for support, three (17%) studies told participants to avoid holding onto the handles, and 10 (56%) studies did not specify the hand position.
Machine Specifications
A range of vibrating machine models were used with no study reporting the manufacturing year of the machine (Table 3). Seven (39%) studies reported using pivotal (side-alternating) vibration with the remaining 11 (61%) studies not indicating the type of vibration used. Machine frequencies were reported by all 18 (100%) studies and ranged from 5 to 40 Hz. Amplitude was reported by 11 (61%) studies, ranging from 1 to 3 mm. Peak acceleration was reported by only five (28%) studies, ranging from 0.3 to 2.6 g (g-force). No studies reported force (kilonewtons (kN)) or whether accelerometers or force transducers were used for loaded and unloaded testing of the machine by an independent engineer.
Adverse Events
Three (17%) studies described adverse events reported by participants in the WBVT groups. Eighty percent of participants in each of two studies reported redness of the feet or ankles following the first few training sessions (Ibrahim et al., 2014; Ruck et al., 2010). Ruck et al. (2010) also reported that 0.6% of total treatment sessions were interrupted due to complaints of fatigue and 0.5% due to pain; however, it was not clear whether this was directly due to the WBVT. One participant also reported leg stiffness in the evening following training (Ahlborg et al., 2006).
Discussion
This systematic review evaluated the protocols adopted by randomised controlled trials reporting on the efficacy of WBVT for people with CP. Although the purpose of this review was not to comment on the efficacy of this intervention (which is notoriously inconsistent across published work Leite et al., 2019; Novak et al., 2013, 2020; Ritzmann et al., 2018; Sá-Caputo et al., 2016), an understanding of WBVT protocols (including machine parameters and patient positioning) is central to the delivery, and therefore effectiveness of this intervention, with respect to safety and reproducibility. The results from this review have revealed considerable variation in the WBVT programmes, protocols, machine settings, and patient positions adopted by clinical trials involving people with CP.
Despite the influence of patient positioning on the level of vibration transmitted through the axial skeleton and head (Muir et al., 2013; Pel et al., 2009; Rittweger, 2010; Tankisheva et al., 2014), patient positioning was inconsistently described across the included studies. Foot position, and more specifically forefoot loading, has been reported to dampen the vibration through the trunk and to the head (Rittweger, 2010), which should be considered in the presence of contractures of the gastrocnemius-soleus complex in people with CP. Furthermore, although most included trials required participants to be positioned on the vibrating platform in a squat or with their knees flexed, the majority of studies provided no specific angular measurements. A study comparing the impact of three knee angles (130°, 110°, and 0°, where 180° is full extension) on vibration transmission demonstrated that the most effective position was achieved with the knee at 110° (deep squat) (Tankisheva et al., 2014). In fact, straight-legged standing positions have been abandoned due to transmission of force to the head exceeding that measured at the foot (Muir et al., 2013). Detailed descriptions of the participants’ ability to hold positions, and the safety measures that are in place, such as handrails, and whether the handrail is attached directly to the platform, or not, as well as whether residual vibration was being transferred to the participant were all poorly considered in the included studies, despite their relevance in terms of positioning and safety (Wuestefeld et al., 2020).
Although it has been acknowledged that there is little evidence on the safety of machine specifications, specifically with children (Unger et al., 2013), none of the included studies in the current review reported independently validated specifications, and few reported the machine type and peak acceleration. Reporting a brand name without clear specifications, or focusing on the Hz or peak-to-peak acceleration without disclosing the type of machine (Jordan et al., 2005; Lorenzen et al., 2009; Rauch et al., 2010), has implications for safety in terms of adverse events and contraindications when considering an intervention for people with CP. It is difficult to comment on the two lineal machine types or pivotal machine type in the current review, without information about the loaded and unloaded specifications, and therefore whether the stated frequencies are correct. Only one out of eighteen included clinical trials considered reporting adverse events resulting from the WBVT (including acute leg pain, sore feet, and headache). Adverse events resulting from WBVT are closely related to machine settings and participant positioning and have an important influence on overall therapeutic efficacy (Alizadeh-Meghrazi et al., 2012).
The engineering specifications for every vibrating platform are almost identical to the Earthquake Simulators used at the University of Tokyo since 1893 to categorise building construction types and how multidirectional vibrations affect man-made structures (Reitherman, 2012). Using engineering requirements and principles (Larbi et al., 2020), the vibrating machines must comply with a number of specifications that relate to four factors: frequency, amplitude, direction, and force. Although the recommendations include reporting the specifications of the vibrating platform, such as frequency (vibration speed) and direction and amplitude (displacement) along the X, Y, and Z axes (Rauch et al., 2010; Wuestefeld et al., 2020), they do not recommend calculating the kN force (multiplying a mass of “A” kilogrammes on a platform that vibrates at a peak acceleration of “B” g-forces equals the kN force), which will enable other researchers to determine the maximum payload (mass) the plate can withstand. Should the maximum load be exceeded, it is possible that vibration performance, control, and frequency are diminished, which emphasises the importance of ensuring the vibration machine specifications are met whilst operating under load, specifically when used in clinical trials (Kaeding, 2015, 2017).
Also absent from the protocols implemented in the included studies was the use of an accelerometer and force transducer; specifically, to measure and report how the vibration parameters were verified, which change over the lifetime of the device (Kaeding et al., 2018; van Heuvelen et al., 2021). The authors recommend the use of three-dimensional tri-axial accelerometers that report X, Y, and Z percentages and a force transducer to allow more accurate between-study comparisons and indication of vibration stability and control.
Limitations and Future Research
The findings from this review should be considered in light of some limitations. Firstly, although the inclusion criteria were limited to randomised controlled trials in attempt to include research reflecting the highest level of evidence, methodology quality was poor across the included studies. Secondly, the review included only studies involving people with CP which limits our ability to comment on WBVT adopted by authors investigating other conditions. Thirdly, the purpose of this review was to investigate the methodological protocols adopted by research using WBVT for people with CP, rather than comment on treatment efficacy; however, future studies may explore how various machine settings and patient positioning may influence efficacy of WBVT in this population.
Based on the insights gained from this review, we suggest a number of recommendations for future clinical trials of WBVT for people with CP. Firstly, researchers should measure and report machine specifications, particularly the force of the machine(s), which should be verified by an independent engineer: using accelerometers (multiple locations on the platform if possible; disclosing the placement on the machine) and the use of a force transducer prior to a study being undertaken. Secondly, researchers should report a measurement of loaded (with a range of weights) and unloaded, and whether this range is appropriate for the CP population being studied. The year of manufacture of the machine should also be reported along with the service as key parameters change as device componentry ages. Additionally, reporting of any modifications or alterations made to the plate should be included. The authors also recommended including clear photographs of the machine, accelerometers, and transducer placement, as well as the positioning of the participant with joint angles clearly marked. Finally, we recommend that distinct intervention parameters be developed for the different machine types, especially for safety and effectiveness. A key factor to consider is the context of the protocol in conjunction with the machine and its original reason for development (Signorile, 2011).
References
Ahlborg, L., Andersson, C., & Julin, P. (2006). Whole-body vibration training compared with resistance training: Effect on spasticity, muscle strength and motor performance in adults with cerebral palsy. Journal of Rehabilitation Medicine, 38(5), 302–308. https://doi.org/10.1080/16501970600680262
Ahmadizadeh, Z., Khalili, M. A., Ghalam, M. S., & Mokhlesin, M. (2019). Effect of whole body vibration with stretching exercise on active and passive range of motion in lower extremities in children with cerebral palsy: A randomized clinical trial. Iranian Journal of Pediatrics, 29(5), Article e84436. https://doi.org/10.5812/ijp.84436
Ali, M. S., & Abd el-aziz, H. G. (2021). Effect of whole-body vibration on abdominal thickness and sitting ability in children with spastic diplegia. Journal of Taibah University Medical Sciences, 16(3), 379–386. https://doi.org/10.1016/j.jtumed.2020.11.006
Ali, M. S., & Awad, A. S. (2022). Comparison of the efficacy of two interventions in ameliorating abdominal thickness and sitting function in children with diplegia. Journal of Taibah University Medical Sciences, 17(4), 548–555. https://doi.org/10.1016/j.jtumed.2022.01.011
Ali, M. S., Awad, A. S., & Elassal, M. I. (2019). The effect of two therapeutic interventions on balance in children with spastic cerebral palsy: A comparative study. Journal of Taibah University Medical Sciences, 14(4), 350–356. https://doi.org/10.1016/j.jtumed.2019.05.005
Alizadeh-Meghrazi, M., Masani, K., Popovic, M. R., & Craven, B. C. (2012). Whole-body vibration during passive standing in individuals with spinal cord injury: Effects of plate choice, frequency, amplitude, and subject’s posture on vibration propagation. The Journal of Injury, Function and Rehabilitation, 4(12), 963–975. https://doi.org/10.1016/j.pmrj.2012.08.012
Bania, T., Chiu, H. C., & Billis, E. (2019). Activity training on the ground in children with cerebral palsy: Systematic review and meta-analysis. Physiotherapy Theory and Practice, 35(9), 810–821. https://doi.org/10.1080/09593985.2018.1460647
Booth, A. T. C., Buizer, A. I., Meyns, P., Oude Lansink, I. L. B., Steenbrink, F., & van der Krogt, M. M. (2018). The efficacy of functional gait training in children and young adults with cerebral palsy: A systematic review and meta-analysis. Developmental Medicine and Child Neurology, 60(9), 866–883. https://doi.org/10.1111/dmcn.13708
Bosco, C., Cardinale, M., & Tsarpela, O. (1998). The influence on whole body vibration on jumping performance. Biology of Sport, 15, 157–164.
Cheng, H. Y. K., Yu, Y. C., Wong, A. M. K., Tsai, Y. S., & Ju, Y. Y. (2015). Effects of an eight-week whole body vibration on lower extremity muscle tone and function in children with cerebral palsy. Research in Developmental Disabilities, 38, 256–261. https://doi.org/10.1016/j.ridd.2014.12.017
Cronin, J., Nash, M., & Whatman, C. (2007). The effect of four different vibratory stimuli on dynamic range of motion of the hamstrings. Physical Therapy in Sport, 8(1), 30–36. https://doi.org/10.1016/j.ptsp.2006.11.003
Duquette, S. A., Guiliano, A. M., & Starmer, D. J. (2015). Whole body vibration and cerebral palsy: A systematic review. Journal of the Canadian Chiropractic Association, 59(3), 245–252.
El-Bagalaty, A. E., & Ismaeel, M. M. I. (2021). Suit therapy versus whole-body vibration on bone mineral density in children with spastic diplegia. Journal of Musculoskeletal Neuronal Interactions, 21(1), 79–84. https://www.scopus.com/inward/record.uri?eid=2-s2.0-85102482252&partnerID=40&md5=093b79f8da3816e12c0ac7fcc3bafcf8
El-Shamy, S. M. (2014). Effect of whole-body vibration on muscle strength and balance in diplegic cerebral palsy: A randomized controlled trial. American Journal of Physical Medicine and Rehabilitation, 93(2), 114–121. https://doi.org/10.1097/PHM.0b013e3182a541a4
El-Shamy, S. M., & Mohamed, M. S. E. (2012). Effect of whole body vibration training on bone mineral density in cerebral palsy children. Indian Journal of Physiotherapy and Occupational Therapy, 6(1), 139–141.
Ibrahim, M. M., Eid, M. A., & Moawd, S. A. (2014). Effect of whole-body vibration on muscle strength, spasticity, and motor performance in spastic diplegic cerebral palsy children. Egyptian Journal of Medical Human Genetics, 15(2), 173–179. https://doi.org/10.1016/j.ejmhg.2014.02.007
Johnson, N., & Phillips, M. (2018). Rayyan for systematic reviews. Journal of Electronic Resouces Librianship, 30(1), 46–48.
Jordan, M. J., Norris, S. R., Smith, D. J., & Herzog, W. (2005). Vibration training: An overview of the area, training consequences, and future considerations. Journal of Strength and Conditioning Research, 19(2), 459–466. https://doi.org/10.1519/13293.1
Jung, M., & Dammerer, J. (2020). Movement therapy in chemotherapy-induced polyneuropathy (CIPN) in pediatric oncology – A Delphi study. Neurologie und Rehabilitation, 25(3), 177–187. https://doi.org/10.14624/NR1902004
Kaeding, T. S. (2015). Deviations of frequency and the mode of vibration of commercially available whole-body vibration training devices. The Journal of Sports Medicine and Physical Fitness, 55(6), 569–577.
Kaeding, D. T. S. (2017). Deviations in whole-body vibration training devices: A narrative review. Journal of Yoga and Physical Therapy, 7, 275. https://doi.org/10.4172/2157-7595.1000275
Kaeding, T. S., Moghaddamnia, S., Kück, M., & Stein, L. (2018). Deviations in frequency and mode of vibration in whole-body vibration training devices with long-term and regular use. Medical Engineering and Physics, 51, 84–90.
Khan, A. A., Akram, M. U., Khalid, M., & Zeb, J. (2021). The effect of vibration therapy on spasticity of children suffering from cerebral palsy: A systematic review. 2021 International Conference on Robotics and Automation in Industry (ICRAI),
Ko, M. C., Wu, L. S., Lee, S., Wang, C. C., Lee, P. F., Tseng, C. Y., & Ho, C. C. (2017). Whole-body vibration training improves balance control and sit-to-stand performance among middle-aged and older adults: A pilot randomized controlled trial. European Review of Aging and Physical Activity, 14(1), Article 11. https://doi.org/10.1186/s11556-017-0180-8
Larbi, S. H., Bourahla, N., Benchoubane, H., Choutri, K., & Badaoui, M. (2020). Earthquake ground motion matching on a small electric shaking table using a combined NN-PDFF controller. Shock and Vibration, 2020, 7260590. https://doi.org/10.1155/2020/7260590
Lee, B. K., & Chon, S. C. (2013). Effect of whole body vibration training on mobility in children with cerebral palsy: A randomized controlled experimenter-blinded study. Clinical Rehabilitation, 27(7), 599–607. https://doi.org/10.1177/0269215512470673
Leite, H. R., Camargos, A. C. R., Mendonça, V. A., Lacerda, A. C. R., Soares, B. A., & Oliveira, V. C. (2019). Current evidence does not support whole body vibration in clinical practice in children and adolescents with disabilities: A systematic review of randomized controlled trial. Brazilian Journal of Physical Therapy, 23(3), 196–211. https://doi.org/10.1016/j.bjpt.2018.09.005
Liang, X., Tan, Z., Yun, G., Cao, J., Wang, J., Liu, Q., & Chen, T. (2021). Effectiveness of exercise interventions for children with cerebral palsy: A systematic review and meta-analysis of randomized controlled trials. Journal of Rehabilitation Medicine, 53(4), jrm00176–jrm00176. https://doi.org/10.2340/16501977-2772
Lorenzen, C., Maschette, W., Koh, M., & Wilson, C. (2009). Inconsistent use of terminology in whole body vibration exercise research. Journal of Science and Medicine in Sport, 12(6), 676–678. https://doi.org/10.1016/j.jsams.2008.06.008
Makris, T., Dorstyn, D., & Crettenden, A. (2021). Quality of life in children and adolescents with cerebral palsy: A systematic review with meta-analysis. Disability and Rehabilitation, 43(3), 299–308. https://doi.org/10.1080/09638288.2019.1623852
Moher, D., Liberati, A., Tetzlaff, J., & Altman, D. G. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. British Medical Journal, 339, b2535. https://doi.org/10.1136/bmj.b2535
Morgan, P. E., Dobson, F. L., & McGinley, J. L. (2014). A systematic review of the efficacy of conservative interventions on the gait of ambulant adults with cerebral palsy. Journal of Developmental and Physical Disabilities, 26(5), 633–654. https://doi.org/10.1007/s10882-014-9385-1
Morgan, C., Darrah, J., Gordon, A. M., Harbourne, R., Spittle, A., Johnson, R., & Fetters, L. (2016). Effectiveness of motor interventions in infants with cerebral palsy: A systematic review. Developmental Medicine and Child Neurology, 58(9), 900–909. https://doi.org/10.1111/dmcn.13105
Muir, J., Kiel, D. P., & Rubin, C. T. (2013). Safety and severity of accelerations delivered from whole body vibration exercise devices to standing adults. Journal of Science and Medicine in Sport, 16(6), 526–531. https://doi.org/10.1016/j.jsams.2013.01.004
Nelson, J. A., & Boyer, E. R. (2021). Perceived limitations of walking in individuals with cerebral palsy. Physical Therapy, 101(7). https://doi.org/10.1093/ptj/pzab102
Novak, I., McIntyre, S., Morgan, C., Campbell, L., Dark, L., Morton, N., Stumbles, E., Wilson, S. A., & Goldsmith, S. (2013). A systematic review of interventions for children with cerebral palsy: State of the evidence. Developmental Medicine and Child Neurology, 55(10), 885–910. https://doi.org/10.1111/dmcn.12246
Novak, I., Morgan, C., Fahey, M., Finch-Edmondson, M., Galea, C., Hines, A., Langdon, K., Namara, M. M., Paton, M. C., Popat, H., Shore, B., Khamis, A., Stanton, E., Finemore, O. P., Tricks, A., Te Velde, A., Dark, L., Morton, N., & Badawi, N. (2020). State of the evidence traffic lights 2019: Systematic review of interventions for preventing and treating children with cerebral palsy. Current Neurology and Neuroscience Reports, 20(2), 3. https://doi.org/10.1007/s11910-020-1022-z
Oremus, M., Wolfson, C., Perrault, A., Demers, L., Momoli, F., & Moride, Y. (2001). Interrater reliability of the modified Jadad quality scale for systematic reviews of Alzheimer’s disease drug trials. Dementia and Geriatric Cognitive Disorders, 12(3), 232–236. https://doi.org/10.1159/000051263
Oskoui, M., Coutinho, F., Dykeman, J., Jetté, N., & Pringsheim, T. (2013). An update on the prevalence of cerebral palsy: A systematic review and meta-analysis. Developmental Medicine and Child Neurology, 55(6), 509–519. https://doi.org/10.1111/dmcn.12080
Papavasiliou, A. S. (2009). Management of motor problems in cerebral palsy: A critical update for the clinician. European Journal of Paediatric Neurology, 13(5), 387–396. https://doi.org/10.1016/j.ejpn.2008.07.009
Pel, J. J., Bagheri, J., van Dam, L. M., van den Berg-Emons, H. J., Horemans, H. L., Stam, H. J., & van der Steen, J. (2009). Platform accelerations of three different whole-body vibration devices and the transmission of vertical vibrations to the lower limbs. Medical Engineering and Physics, 31(8), 937–944. https://doi.org/10.1016/j.medengphy.2009.05.005
Pirpiris, M., Gates, P. E., McCarthy, J. J., D’Astous, J., Tylkowksi, C., Sanders, J. O., Dorey, F. J., Ostendorff, S., Robles, G., Caron, C., & Otsuka, N. Y. (2006). Function and well-being in ambulatory children with cerebral palsy. Journal of Pediatric Orthopedics, 26(1), 119–124. https://doi.org/10.1097/01.bpo.0000191553.26574.27
Rauch, F., Sievanen, H., Boonen, S., Cardinale, M., Degens, H., Felsenberg, D., Roth, J., Schoenau, E., Verschueren, S., & Rittweger, J. (2010). Reporting whole-body vibration intervention studies: Recommendations of the International Society of Musculoskeletal and Neuronal Interactions. Journal of Musculoskeletal Neuronal Interactions, 10(3), 193–198. https://www.scopus.com/inward/record.uri?eid=2-s2.0-77957377791&partnerID=40&md5=310a663795ee1434a80b16fe4bc93ef7
Reitherman, R. (2012). Earthquakes and engineers: An international history. https://doi.org/10.1061/9780784410714
Rittweger, J. (2010). Vibration as an exercise modality: How it may work, and what its potential might be. European Journal of Applied Physiology, 108(5), 877–904.
Ritzmann, R., Stark, C., & Krause, A. (2018). Vibration therapy in patients with cerebral palsy: A systematic review. Neuropsychiatric Disease and Treatment, 14, 1607–1625. https://doi.org/10.2147/NDT.S152543
Rosenbaum, P., Paneth, N., Leviton, A., Goldstein, M., Bax, M., Damiano, D., Dan, B., & Jacobsson, B. (2007). A report: The definition and classification of cerebral palsy. Developmental Medicine and Child Neurology, 109, 8–14.
Ruck, J., Chabot, G., & Rauch, F. (2010). Vibration treatment in cerebral palsy: A randomized controlled pilot study. Journal of Musculoskeletal Neuronal Interactions, 10(1), 77–83.
Ruhde, L., & Hulla, R. (2022). An overview of the effects of whole-body vibration on individuals with cerebral palsy. Journal of Pediatric Rehabilitation Medicine, 15, 193–210. https://doi.org/10.3233/PRM-201508
Ryan, J. M., Cassidy, E. E., Noorduyn, S. G., & O’Connell, N. E. (2017). Exercise interventions for cerebral palsy. Cochrane Database Systematic Reviews, 6(6), Cd011660. https://doi.org/10.1002/14651858.CD011660.pub2
Sá-Caputo, D., Gonçalves, C. R., Morel, D. S., Marconi, E. M., Fróes, P., Rufino, R., Costa, C. H., Lopes, A. J., Arnóbio, A., Asad, N. R., Marin, P. J., Furness, T., & Bernardo-Filho, M. (2016). Benefits of whole-body vibration, as a component of the pulmonary rehabilitation, in patients with chronic obstructive pulmonary disease: A narrative review with a suitable approach. Evidence-based Complementary and Alternative Medicine, 2016, Article 2560710. https://doi.org/10.1155/2016/2560710
Signorile, J. (2011). Whole body vibration: What’s shakin’ now? Journal of Active Aging, 10, 46–59.
Stark, C., Herkenrath, P., Hollmann, H., Waltz, S., Becker, I., Hoebing, L., Semler, O., Hoyer-Kuhn, H., Duran, I., Hero, B., Hadders-Algra, M., & Schoenau, E. (2016). Early vibration assisted physiotherapy in toddlers with cerebral palsy – A randomized controlled pilot trial. Journal of Musculoskeletal Neuronal Interactions, 16(3), 183–192.
Tankisheva, E., Bogaerts, A., Boonen, S., Feys, H., & Verschueren, S. (2014). Effects of intensive whole-body vibration training on muscle strength and balance in adults with chronic stroke: A randomized controlled pilot study. Archives of Physical Medicine and Rehabilitation, 95(3), 439–446. https://doi.org/10.1016/j.apmr.2013.09.009
Tekin, F., & Kavlak, E. (2021). Short and long-term effects of whole-body vibration on spasticity and motor performance in children with hemiparetic cerebral palsy. Perceptual and Motor Skills, 128(3), 1107–1129. https://doi.org/10.1177/0031512521991095
Tupimai, T., Peungsuwan, P., Prasertnoo, J., & Yamauchi, J. (2016). Effect of combining passive muscle stretching and whole body vibration on spasticity and physical performance of children and adolescents with cerebral palsy. Journal of Physical Therapy Science, 28(1), 7–13. https://doi.org/10.1589/jpts.28.7
Unger, M., Jelsma, J., & Stark, C. (2013). Effect of a trunk-targeted intervention using vibration on posture and gait in children with spastic type cerebral palsy: A randomized control trial [Article]. Developmental Neurorehabilitation, 16(2), 79–88. https://doi.org/10.3109/17518423.2012.715313
van Heuvelen, M. J. G., Rittweger, J., Judex, S., Sañudo, B., Seixas, A., Fuermaier, A. B. M., Tucha, O., Nyakas, C., Marín, P. J., Taiar, R., Stark, C., Schoenau, E., Sá-Caputo, D. C., Bernardo-Filho, M., & van der Zee, E. A. (2021). Reporting guidelines for whole-body vibration studies in humans, animals and cell cultures: A consensus statement from an international group of experts. Biology, 10(10), 965. https://www.mdpi.com/2079-7737/10/10/965
Wuestefeld, A., Fuermaier, A. B. M., Bernardo-Filhoda Cunha de Sá-Caputo, M. D., Rittweger, J., Schoenau, E., Stark, C., Marin, P. J., Seixas, A., Judex, S., Taiar, R., Nyakas, C., van der Zee, E. A., van Heuvelen, M. J. G., & Tucha, O. (2020). Towards reporting guidelines of research using whole-body vibration as training or treatment regimen in human subjects-A Delphi consensus study. PLoS One, 15(7), e0235905–e0235905. https://doi.org/10.1371/journal.pone.0235905
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Contributions
LS, KO, SS, and DP were involved in conceptualisation, investigation, and visualisation. LS, KO, and DP were also involved in validation and SS was involved in methodology and project administration. All authors were involved in the writing of the manuscript, including critical review and editing. All authors approved the final version for publication.
Corresponding author
Ethics declarations
Conflict of Interest
KO has lived experience of CP and regular use of different types of vibration machines. LS runs Vibration Training Limited in Auckland, New Zealand, which had no financial or other role in the design, conduct, and interpretation of this study. The other authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Shaw, L., O’Leary, K., Stewart, S. et al. Whole-Body Vibration Training Protocols for People with Cerebral Palsy: a Systematic Review of Randomised Controlled Trials. Adv Neurodev Disord 8, 222–234 (2024). https://doi.org/10.1007/s41252-023-00331-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41252-023-00331-8