Abstract
Introduction
The aim of the present study was to conduct a review of major publications on the use of Colobreathe® [colistimethate sodium dry powder for inhalation (CDPI) via Turbospin®] for the treatment of cystic fibrosis-associated pulmonary infections.
Methods
Data for this research were extracted from original articles and reviews obtained through a search of the MEDLINE, MEDLINE in-Process, EMBASE, Cochrane Library, CINAHL, Web of Science, Conference Proceedings Citation Index and BIOSIS Previews databases through July 2015, using the key words "Colobreathe," "colistimethate sodium dry powder inhalation" and "cystic fibrosis." Published data on Colobreathe® from international congresses were also included.
Results
One clinical trial, the phase III FREEDOM study, found that the use of Colobreathe® inhalation of 125 mg twice daily via Turbospin® was non-inferior to inhaled tobramycin solution. Two reviews of colistimethate sodium focused on its use and its efficacy. The relevant outcomes observed included forced expiratory volume in 1 s (FEV1% predicted), tolerability, health-related quality of life (HRQL), ease of use of the inhalation device, and pharmacokinetics. The results showed no inferiority for CDPI compared to inhaled tobramycin solution. Most of the HRQL scores tended to be in favour of the dry powder intervention, although none of the differences were statistically significant, but good treatment satisfaction was measured. One study focused on cost. Five conference abstracts on CDPI reported good implementation in a “real world setting,” significant high lung deposition, and good compliance and tolerability data for patients who continued to inhale CDPI for 4 weeks.
Conclusions
Studies demonstrated no inferiority of CDPI to tobramycin inhalation solution (TIS) in FEV1% predicted, and reported a preference of patients for the dry powder inhalation of colistimethate sodium because it was well tolerated, easier to use, less inconvenient and associated with improved adherence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cystic fibrosis (CF) is the most common lethal genetic disease among white populations, affecting approximately 70,000 persons worldwide. The leading cause of death is progressive lung disease, driven by a complex and diverse inflammatory immune syndrome induced by acute and chronic recurrent bacterial infections of the lung [1–3].
The positive development of life expectancy in CF in recent years has led to a new discussion on evidence-based medicine, usefulness of therapy, burden of treatment and health-related quality of life. In this discussion, dry powder antibiotic inhalation interventions such as the Colobreathe® inhaler play an important role and will be elucidated in this review.
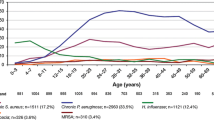
Pulmonary exacerbations occur often in CF and are related to a decline in lung function [4] Therefore, controlling these exacerbations is a major target in CF treatment. Because of the high susceptibility of patients with CF to respiratory tract bacterial infections, oral, inhaled and intravenous antibiotic treatments are needed, and evidence-based treatments for Pseudomonas aeruginosa are already well established. In addition to P. aeruginosa, the bacteria most commonly believed to be pathogenic in CF include Staphylococcus aureus, Haemophilus influenzae, Stenotrophomonas maltophilia, Achromobacter xylosoxidans, and Burkholderia species, although evidence is low or does not exist [5].
The treatment of the most common bacteria P. aeruginosa can be deviated into eradication therapy and suppression therapy. In the case of first-time cultivation of P. aeruginosa from a patient’s throat swab or sputum, eradication of the pathogen is indicated. If a mucoid phenotype, a consequence of overproduction of exopolysaccharides alginate, is found in P. aeruginosa isolates from chronically infected patients with CF, eradication can no longer be the target of therapy [6]. The indications for eradication therapy of P. aeruginosa and the treatment of chronic pseudomonas infection are the major focus of inhaled antibiotic therapy. Currently approved drugs for inhalation therapy in patients with CF are tobramycin, colistimethate sodium, and aztreonam lysine [7].
Eradication Therapy
In terms of eradication therapy, proof of P. aeruginosa colonization should be determined as early as possible in order to quickly begin inhaled antibiotic therapy to prevent the development of mucus-forming (mucoid) pseudomonas. The results for eradication of the non-mucoid P. aeruginosa are 81.2% on average, with a range of 63% to 100% [5]. For inhalation with tobramycin and colistin, data for eradication therapy are available in the literature.
The ELITE study [8] obtained similar results for the inhalation of tobramycin solution 300 mg twice daily for eradication therapy of 28 and 56 days. In both groups, the cultures were negative for P. aeruginosa 1 month after treatment in over 90% of the patients examined.
The addition of oral ciprofloxacin to nebulized tobramycin did not increase the eradication rate, as evidenced in the EPIC study [9]. Inhaled colistin in combination with ciprofloxacin also showed successful eradication results at a treatment duration of 3 months [10]. The comparison of inhaled therapy with colistin and oral ciprofloxacin for 3 months showed equal effectiveness of eradication therapy and therapy for 1 month with nebulized tobramycin [11]. Several different eradication treatment forms. therefore, appear promising. Most eradication treatments take place during childhood. Suppressive therapy in chronically colonized patients with CF seems to be a topic in adult patients.
Available Inhaled Antibiotics
Aminoglycosides
Aminoglycoside tobramycin was the first approved aerosol for inhaled antibiotic therapy (TOBI® tobramycin inhalation solution [TIS], Novartis), and has therefore been used successfully for many years in patients with CF. The dose is 300 mg twice daily and is prescribed in so-called 4-week on/off cycles. Patients inhale the drug for 4 weeks, followed by a 4-week break [12, 13, 14]. Another tobramycin inhalation solution is offered by the company Chiesi (Bramitob®). With Bramitob®, similar to TOBI®, significant improvements in FEV1(%) were shown in the active treatment group compared to the placebo group [15].
In addition, a recent US study showed reduced mortality in patients receiving inhaled tobramycin compared to the group without tobramycin inhalation (1.3% versus 2.1% at 2 years, 5.2% versus 8.0% at 5 years and 9.9% versus 15.0% after 10 years). In this study, 12,740 patients with CF were examined, of which 2538 had died. This once again underscores the importance of antibiotic inhalation as a major treatment option in CF [16].
Monobactams
Aztreonam lysine is another inhaled antibiotic. With aztreonam lysine (Cayston®), a drug within a new class of inhaled antibiotics, the monobactams, (a monocyclic beta-lactam antibiotic), was approved in 2010. Because of its half-life, the antibiotic must be inhaled three times a day at a dose of 75 mg, with an interval of 4 h between inhalations being sufficient. For best bronchopulmonary deposition of aztreonam lysine, especially for this drug, an optimized inhalation device—the Altera® Nebulizer system—was developed by the company PARI Pharma GmbH.
The efficacy of this device, with a significant improvement in FEV1, was shown in a study comparing Cayston® and tobramycin inhalation solution, with a difference of 7.8% on day 28 and 2.7% after a total of 24 weeks of treatment for Cayston. In addition, fewer exacerbations occurred after 28 days, and an increase in weight after a 12-month observation period was observed [17].
Colistimethate Sodium
The efficacy and safety of inhaled colistin was also demonstrated in several studies among patients with CF [18, 19, 20]. The efficacy and safety of the dry powder is discussed in this manuscript.
Dry Powder Inhalation
In recent years, researchers have focused on developing new formulations of inhaled antibiotics and drug-delivery devices. The TOBI® Podhaler™® and the Colobreathe® inhaler are the first dry-powder inhaled antibiotics.
TOBI Podhaler
Tobramycin was developed as a dry powder by the company Novartis for the use in patients with CF and chronic P. aeruginosa colonization. The dose of the TOBI® Podhaler™® was addressed in development according to the pharmacokinetics of tobramycin inhalation solution, and is inhaled twice daily via a passive dry powder inhaler T-326 (Podhaler®), each with 4 capsules containing 28 mg. This corresponds to a dry powder dose of 128 mg [21].
The efficacy and safety of tobramycin dry powder was proven in two studies. In the EAGER and EVOLVE trials, comparable tolerability and effectiveness was achieved with dry powder and an inhalation solution of tobramycin. The FEV1 improved significantly during treatment with the TOBI® Podhaler™® compared to the placebo group [22, 23]. A great benefit for patients with the novel dry powder is the significantly shorter inhalation time, with a mean 5.6 min inhalation time for the TOBI® dry powder compared to 19.7 min on average for the TOBI® solution inhalation (p < 0.0001). In this calculation, the time for cleaning and sterilization of the inhalation device, which is also significantly lower for the Podhaler™®, was not taken into account [22]. The second dry powder antibiotic inhalation drug, Colobreathe®, which is approved in the EU but not in the US for chronic P. aeruginosa infections for patients with CF aged >6 years, will be discussed in this review.
The aim of this review is to discuss the efficacy, tolerability, pharmacokinetics and ease of use of the inhalation device and lung deposition of Colobreathe.
Methods
A systematic literature review was conducted regarding the clinical effectiveness, pharmacokinetics and ease of use of colistimethate sodium DPI within its licensed indications for the treatment of chronic P. aeruginosa lung infection in CF.
Data for this research were extracted from original articles and reviews obtained through a search of the MEDLINE, MEDLINE in-Process, EMBASE, Cochrane Library, CINAHL, Web of Science, Conference Proceedings Citation Index and BIOSIS Previews databases through July 2015, using the key words "Colobreathe," "colistimethate sodium dry powder inhalation" and "cystic fibrosis." Published data on Colobreathe® from international congresses were also included. This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors (Table 1).
Mechanism of Action of the Colistimethate Sodium Inhalation Powder
Colistimethate sodium is an antibiotic drug from the polymyxins, a group of cationic polypeptide antibiotics consisting of five chemically different compounds (polymyxins A–E), which were discovered in 1947 [24]. Only polymyxin B and polymyxin E (colistin) have been used in clinical practice. The colistin base is a cationic, multicomponent lipopeptide consisting of a cyclic heptapeptide with a tripeptide side chain acylated at the N terminus by a fatty acid. The two major components of colistin are colistin A (polymyxin E1) and colistin B (polymyxin E2) [25]. Different pharmaceutical preparations of colistin may contain different amounts of these two components. Colistimethate sodium (also called polymyxin E) has long been established as an established inhaled antibiotic in the treatment of chronic colonization of the airways by P. aeruginosa in patients with CF [26].
Antimicrobial activity in colistin and polymyxin B is mainly directed against the bacterial cell membrane. The cationic polypeptides of colistin and polymyxin B interact with anionic lipopolysaccharide (LPS) molecules in the outer membrane of gram-negative bacteria, leading to displacement of calcium (Ca2+) and magnesium (Mg2+), which stabilizes the LPS membrane, thus causing derangement of the cell membrane. This results in an increase in cell membrane permeability, leakage of cell contents, and ultimately cell death [27–29].
Dose and Administration of the Colistimethate Sodium Inhalation Powder
The Colobreathe® (Forest Laboratories) contains a dose of 125 mg colistimethate sodium (equivalent to 1,662,500 IU) and is inhaled through the so-called Turbospin® inhaler. Since the total dose is contained in a 125-mg capsule, the patient has to inhale only one capsule in the morning and one in the evening. Average deposition of one inhaled capsule is at least the average deposition of a nebulized dose (not less than 2 MU) [30].
According to the literature, this is currently the fastest way to administer an inhaled antibiotic, with inhalation time measured at 60 s [30]. With regard to effectiveness, the pivotal FREEDOM study showed non-inferiority of Colobreathe® 125-mg twice daily inhalation via the Turbospin® device compared to inhaled tobramycin solution [31].
The lung deposition of inhaled colistimethate sodium was analyzed in a randomized open-label three-way crossover study [32]. Adults with CF (7 males and 3 females) received a total of three randomly assigned treatments, each administered on separate study days (72 h apart): 125 mg radiolabeled colistimethate sodium DPI via the Turbospin® device, 125 mg radiolabeled colistimethate sodium DPI via Turbospin®, preceded by 220 μg salbutamol via a pressurized metered-dose inhaler and 1 mega unit (80 mg) of radiolabeled Colomycin® injection via a MedicAid Ventstream® nebulizer. The whole lung deposition of nebulized antibiotic (5.9 ± 3.4) was nearly half the amount deposited with the dry powder either with (11.9 ± 4.9) or without (11.6 ± 4.3) salbutamol pretreatment (see Fig. 1). This study showed a clear advantage of colistimethate sodium deposition delivered by the Turbospin® inhaler compared with the nebulizer.
Systemic Absorption of Colistimethate Sodium Dry Powder Inhalation
A multicenter, multiple-dose, open-label PK study in 34 patients with CF chronically infected with P. aeruginosa investigated the systemic absorption of inhaled colistimethate sodium dry powder in three age groups [33]. The maximum plasma concentration (C max) for total colistimethate sodium was achieved between 0.5 and 1 h post-dose, with less than 350 ng/ml for the mean of the three age groups (children, adolescents, and adults; see also Fig. 2). The mean plasma C max for total colistimethate sodium and free colistin was significantly below the minimum inhibitory concentration (MIC)90 against P. aeruginosa (4.0 μg/ml). The C max and AUC0–6 for total colistimethate sodium and total free colistin were comparable between children and adolescents, while higher values were observed in the adult group. High PK variability (CV% ranged from 50.8% to 81.8% for the area under the curve [AUC] 0–6 and from 41.3% to 76.1% for C max) was observed in all three age groups. The sputum results revealed a C max for total free colistin at least tenfold higher than the MIC90 breakpoint for P. aeruginosa. Plasma levels of colistin were ~500 times lower than documented levels following intravenous injection of colistimethate sodium [19], suggesting a low risk of systemic toxicity and interactions with other drugs. The high levels of colistimethate sodium and colistin in sputum are consistent with the intended mechanism of the drug acting as a topical antibiotic for patients with chronic pseudomonas lung infection.
Antifungal Activity of Colomycin
Recent in vitro data suggest that colistin may have fungicidal properties [34], although the effect of colistin against Aspergillus in vivo is not known. In a retrospective comparison study of 76 patients with nebulized colistin, 30 patients with nebulized tobramycin and 28 patients without nebulized antibiotic therapy, results revealed that patients who did not receive inhaled antibiotics had significantly lower Aspergillus-positive cultures in sputum samples (p = 0.003) and lower Aspergillus-specific IgE levels (p = 0.001) than patients inhaling an antibiotic drug. No significant difference was seen between the colistin and tobramycin groups aside from the colomycin group, which received less anti-fungal treatment (p = 0.03) [35]. The hypothesis that colistin has anti-fungal activity was prospectively analyzed by Schemuth et al. [36]. Their study demonstrated that in addition to its bactericidal activity, the antibiotic colistin also showed antifungal activity against Scedosporium/Pseudallescheria spp., E. dermatitidis and G. argillacea. In addition, combining colistin with antifungal substances demonstrated species-specific reduction in the MIC values of antifungal agents. Based on these findings, colistin may be considered as a novel agent for antifungal therapy in combination with an antifungal compound.
Clinical Data on Colobreathe
Colobreathe dry powder for inhalation (CDPI) uses a new encapsulated dry-powder formulation of micronized colistimethate sodium administered via a convenient hand-held inhaler (Turbospin; PH&T, Milan, Italy). The aim was to increase patient convenience, which may improve treatment adherence and clinical outcomes. To this end, the FREEDOM study—a prospective, centrally randomized phase III open-label study—was started.
FREEDOM Study
Patients aged ≥6 years with stable CF with chronic P. aeruginosa lung infection were included. Patients were randomized to CDPI (one capsule containing colistimethate sodium 1,662,500 IU, twice daily) or three 28-day cycles with a twice-daily 300-mg/5-ml tobramycin inhaler solution (TIS). The study duration was 24 weeks, and 380 patients were randomized. After logarithmic transformation of data due to non-normal distribution, the adjusted mean difference between treatment groups (CDPI vs TIS) in FEV1 change (% predicted) at week 24 was −0.98% (95% CI −2.74% to 0.86%) in the intention-to-treat population (n = 373) and −0.56% (95% CI −2.71% to 1.70%) in the per-protocol population (n = 261). The proportion of colistin-resistant isolates was ≤1.1% in both groups. A significantly greater number of patients receiving CDPI rated their device as "very easy or easy to use" (90.7% vs 53.9% respectively; p < 0.001). However, clear and comparable data on acute exacerbations, a highly relevant outcome, are missing [37]. A similar range of adverse events was seen in both groups, except for cough, abnormal taste, and throat irritation, which were more frequent in the DPI group. Interestingly, these adverse events were observed only during the first 4 weeks of treatment, after which no difference in tolerability between formulations was seen [31, 38]. This observation is very important for the prescription of colistimethate sodium DPI and the expected adherence to the drug. Prescribers should focus their communication with patients not only on efficacy but also on side effects such as cough and on inhalation techniques. As economic strategies are becoming more important, this topic has been discussed in a review, although the authors conclude that thus far, there have been no data showing either a cost benefit or cost deficit for dry powder inhalation [39].
Recommended CDPI Inhalation Techniques
The importance of communication to patients was mentioned in the previous chapter, but additional aspects must be added, as CF therapeutics now include a growing number of other dry powders (mannitol, TOBI Podhaler). Therefore, education is crucial. Flume et al. [40] previously discussed this topic with regard to mannitol dry powder inhalation. Similar to their recommendations, we provide the most important points for colistimethate sodium dry powder inhalation via the Turbospin inhaler as follows:
-
1.
The capsule should be inserted gently into the chamber with the widest end first, and should then be pierced by pushing the piston upwards until the visible line is reached.
-
2.
Patients should inhale with the head tilted slightly upward, breathing in deeply at an even, steady rate sufficient to make the capsule spin.
-
3.
The rotating capsule will make an audible “rattle,” indicating satisfactory inspiratory flow.
-
4.
Rapid inhalation may result in cough, in which case the patient should slow their inhalation rate.
-
5.
The capsule should be checked after inspiration, and if powder is still present, the patient should inhale a second time.
-
6.
After taking in the dose, the patient should hold their breath for 10 s or for as long as it is comfortable, before breathing out slowly.
Dry Powder in the “Real World“
The FREEDOM study showed the efficacy of colistimethate sodium DPI in a phase III trial. Observational studies representing real-world scenarios were presented recently in European and North American CF congresses. The study group from Liverpool [41] looked at lung function and adherence during a 3-month period before and after the introduction of Colobreathe following a test dose in 17 patients who had previously taken other forms of colistin, and patient-related outcomes (PROMs) were measured in nine. There was no change in FEV1, but eight patients reported improved adherence due to a marked reduction in administration time. Similar results were generated by the study group from Birmingham [42]. In a prospective observational cohort study, patients with CF who were clinically intolerant (INTOL group) of or demonstrated poor adherence to (ADH group) nebulized colistimethate sodium were included. At the 1-month review, 7/10 patients in the INTOL group and 12/13 in the ADH group successfully tolerated a full month of dry powder and planned to continue. The reported adherence at 1 month was significantly higher (p = 0.002) with the dry powder colistimethate sodium (median 100% of doses, interquartile range [IQR] 80.5–100%) compared with the nebulized drug (median 50% of doses, IQR 50–86%). Both studies demonstrated patient preference for dry powder inhalation of colistimethate sodium, as it was well tolerated, easier to use, less inconvenient and associated with improved adherence. Results comparable to those with colistimethate sodium dry powder inhalation had previously been obtained in a real-world study comparing the safety, effectiveness and tolerability of tobramycin inhaled powder (TIP) versus tobramycin inhaled solution (TIS) [43]. Adult patients with CF commencing TIP (n = 78) completed a questionnaire assessing safety, efficacy, tolerability, patient satisfaction and self-reported adherence to TIS at baseline and during 12 months of TIP therapy. There was a significant improvement in adherence scores, with a significant decrease in the number of intravenous antibiotic courses received during the 12 months of TIP compared with the preceding 12 months using TIS. Ninety-four percent of patients who had previously used TIS preferred TIP therapy over TIS. This study demonstrated the important association of dry powder inhalation with improved adherence and tolerability, resulting in a reduced exacerbation rate compared to nebulized treatment in real-life practice. The advantages and disadvantages of dry powder inhalation and inhaled solution are summarized in Table 2.
The Future of Cystic Fibrosis Treatment
Newborn screening, animal models, biomarkers, innovative drugs (prototypical cystic fibrosis transmembrane conductance regulator [CFTR] modulators), and advances in lung transplantation have moved the field forward, probably faster than for any other lung disease in recent years [44–48]. As a consequence, the mean survival of patients with CF is steadily increasing and now exceeds 40 years of age in most European countries [49, 50] and beyond [51]. In this context, the burden of disease and especially the burden of treatment are of high interest because the aims in CF should include therapies, which are feasible in a growing CF population. Although new therapies targeting the CFTR defect will be implemented in the future, basic therapies such as vitamin and enzyme supplementation, anti-infective and anti-inflammatory therapies, physiotherapy, and bronchial clearance therapies will have to be continued. As inhalation therapy with antibiotics is usually a lifelong therapy, convenience and satisfaction with the therapy plays a major role. The ageing CF population and the high number of drugs, as well as time needed for CF therapy, will be positive factors supporting the use of dry powder inhalation such as colistimethate sodium or others. A longer duration of prospective randomized observation studies is needed to confirm the results, and studies should also focus on side effects of dry powders that can lead to non-adherence.
Conclusions
In this review, studies demonstrated no inferiority of CDPI to tobramycin inhalation solution in FEV1% predicted, and showed patient preference for the dry-powder inhalation of colistimethate sodium, as it is well tolerated, easier to use, less inconvenient and associated with improved adherence.
References
Kallet RH, Volsko TA, Hess DR. Respiratory care year in review 2012: invasive mechanical ventilation, noninvasive ventilation, and cystic fibrosis. Respir Care. 2013;58(4):702–11.
Cutting GR. Cystic fibrosis genetics: from molecular understanding to clinical application. Nat Rev Genet. 2014;16(1):45–56.
Döring G, Flume P, Heijerman H, Elborn JS. Treatment of lung infection in patients with cystic fibrosis: current and future strategies. J Cyst Fibros. 2012;11(6):461–79.
Westerman EM, Heijerman H, Frijlink HW. Dry powder inhalation versus wet nebulisation delivery of antibiotics in cystic fibrosis patients. Expert Opin Drug Deliv. 2007;4(2):91–4.
Döring G, Flume P, Heijerman H, Elborn JS, Consensus Study Group. Treatment of lung infection in patients with cystic fibrosis: current and future strategies. J Cyst Fibros. 2012;11(6):461–79.
Henry RL, Mellis CM, Petrovic L. Mucoid Pseudomonas aeruginosa is a marker of poor survival in cystic fibrosis. Pediatr Pulmonol. 1992;12(3):158–61.
Schwarz C, Staab D. Cystic fibrosis and associated complications. Internist (Berl). 2015;20:1–12.
Ratjen F, Munck A, Kho P, Angyalosi G, ELITE Study Group. Treatment of early Pseudomonas aeruginosa infection in patients with cystic fibrosis: the ELITE trial. Thorax. 2010;65(4):286–91.
Treggiari MM, Retsch-Bogart G, Mayer-Hamblett N, Khan U, Kulich M, Kronmal R, et al. Comparative efficacy and safety of 4 randomized regimens to treat early Pseudomonas aeruginosa infection in children with cystic fibrosis. Arch Pediatr Adolesc Med. 2011;165(9):847–56.
Høiby N, Frederiksen B, Pressler T. Eradication of early Pseudomonas aeruginosa infection. J Cyst Fibros. 2005;4 Suppl 2:49–54.
Proesmans M, Vermeulen F, Boulanger L, Verhaegen J, De Boeck K. Comparison of two treatment regimens for eradication of Pseudomonas aeruginosa infection in children with cystic fibrosis. J Cyst Fibros. 2013;12(1):29–34.
Flume PA, Mogayzel PJ, Robinson KA, Goss CH, Rosenblatt RL, Kuhn RJ, et al. Cystic fibrosis pulmonary guidelines: treatment of pulmonary exacerbations. Am J Respir Crit Care Med. 2009;180(9):802–8.
Flume PA, O’Sullivan BP, Robinson KA, Goss CH, Mogayzel PJ, Willey-Courand D-B, et al. Cystic fibrosis pulmonary guidelines: chronic medications for maintenance of lung health. Am J Respir Crit Care Med. 2007;176(10):957–69.
Ryan G, Singh M, Dwan K. Inhaled antibiotics for long-term therapy in cystic fibrosis. Cochrane Database Syst Rev. 2011;(3):CD001021.
Chuchalin A, Csiszér E, Gyurkovics K, Bartnicka MT, Sands D, Kapranov N, et al. A formulation of aerosolized tobramycin (Bramitob) in the treatment of patients with cystic fibrosis and Pseudomonas aeruginosa infection: a double-blind, placebo-controlled, multicenter study. Paediatr Drugs. 2007;9 Suppl 1:21–31.
Sawicki GS, Signorovitch JE, Zhang J, Latremouille-Viau D, von Wartburg M, Wu EQ, et al. Reduced mortality in cystic fibrosis patients treated with tobramycin inhalation solution. Pediatr Pulmonol. 2012;47(1):44–52.
Assael BM, Pressler T, Bilton D, Fayon M, Fischer R, Chiron R, et al. Inhaled aztreonam lysine vs. inhaled tobramycin in cystic fibrosis: a comparative efficacy trial. J Cyst Fibros. 2013;12(2):130–40.
Quintana-Gallego E, Lopez-Campos JL, Calero C, Dapena FJ. Nebulized colistin versus tobramycin in the treatment of chronic Pseudomonas colonization in cystic fibrosis patients. Med Clin (Barc). 2014;142(2):59–63.
Yapa WS, Li J, Patel K, Wilson JW, Dooley MJ, George J, et al. Pulmonary and systemic pharmacokinetics of inhaled and intravenous colistin methanesulfonate in cystic fibrosis patients: targeting advantage of inhalational administration. Antimicrob Agents Chemother. 2014;58(5):2570–9.
Ratjen F, Rietschel E, Kasel D, Schwiertz R, Starke K, Beier H, et al. Pharmacokinetics of inhaled colistin in patients with cystic fibrosis. J Antimicrob Chemother. 2006;57(2):306–11.
Geller DE, Konstan MW, Smith J, Noonberg SB, Conrad C. Novel tobramycin inhalation powder in cystic fibrosis subjects: pharmacokinetics and safety. Pediatr Pulmonol. 2007;42(4):307–13.
Konstan MW, Flume PA, Kappler M, Chiron R, Higgins M, Brockhaus F, et al. Safety, efficacy and convenience of tobramycin inhalation powder in cystic fibrosis patients: the EAGER trial. J Cyst Fibros. 2011;10(1):54–61.
Konstan MW, Geller DE, Minić P, Brockhaus F, Zhang J, Angyalosi G. Tobramycin inhalation powder for P. aeruginosa infection in cystic fibrosis: the EVOLVE trial. Pediatr Pulmonol. 2011;46(3):230–8.
Storm DR, Rosenthal KS, Swanson PE. Polymyxin and related peptide antibiotics. Annu Rev Biochem. 1977;46(1):723–63.
Orwa JA, Govaerts C, Busson R, Roets E, Van Schepdael A, Hoogmartens J. Isolation and structural characterization of colistin components. J Antibiot. 2001;54(7):595–9.
Döring G, Høiby N, Consensus Study Group. Early intervention and prevention of lung disease in cystic fibrosis: a European consensus. J Cyst Fibros. 2004;3:67–91. doi:10.1016/j.jcf.2004.03.008.
Newton BA. The properties and mode of action of the polymyxins. Bacteriol Rev. 1956;20(1):14–27.
Davis SD, Iannetta A, Wedgwood RJ. Activity of colistin against Pseudomonas aeruginosa: inhibition by calcium. J Infect Dis. 1971;124(6):610–2.
Schindler M, Osborn MJ. Interaction of divalent cations and polymyxin B with lipopolysaccharide. Biochemistry. 1979;18(20):4425–30.
Conole D, Keating GM. Colistimethate sodium dry powder for inhalation: a review of its use in the treatment of chronic Pseudomonas aeruginosa infection in patients with cystic fibrosis. Drugs. 2014;74(3):377–87.
Schuster A, Haliburn C, Döring G, Goldman MH, Freedom Study Group. Safety, efficacy and convenience of colistimethate sodium dry powder for inhalation (Colobreathe DPI) in patients with cystic fibrosis: a randomised study. Thorax. 2013;68(4):344–50.
Su S, Riccobene T, Scott C. Lung deposition of inhaled colistimethate sodium in cystic fibrosis patients. Eur Respir J. 2014;44 Suppl 58:P1975.
Goldman MH, Riethmuller J, Turay P. A 7-day open-label PK study to investigate the systemic absorption of a dry powder formulation of inhaled colistimethate sodium (CDPI) [Colobreathe® 1,662,500 IU] in adult, adolescent and paediatric cystic fibrosis subjects with chronic Pseudomonas aeruginosa lung infection. J Cyst Fibros. 2013;11 (Supp l) 1:12.
Ben-Ami R, Lewis RE, Tarrand J, Leventakos K, Kontoyiannis DP. Antifungal activity of colistin against mucorales species in vitro and in a murine model of Rhizopus oryzae pulmonary infection. Antimicrob Agents Chemother. 2010;54(1):484–90.
Lumb C, Whitaker P, Williams K, Pollard K. 116 Effect of nebulised antibiotics on Aspergillus colonisation and complications. J Cyst Fibros. 2011;10:S30.
Schemuth H, Dittmer S, Lackner M, Sedlacek L, Hamprecht A, Steinmann E, et al. In vitro activity of colistin as single agent and in combination with antifungals against filamentous fungi occurring in patients with cystic fibrosis. Mycoses. 2013;56(3):297–303.
Uttley L, Harnan S, Cantrell A, Taylor C, Walshaw M, Brownlee K, et al. Systematic review of the dry powder inhalers colistimethate sodium and tobramycin in cystic fibrosis. Eur Respir Rev. 2013;22(130):476–86.
Goldman MH, Werner T, Schuster A. Does persistence with inhaled dry powder antibiotic treatment improve tolerability? Pediatr Pulmonol. 2013;48:347.
Tappenden P, Harnan S, Uttley L, Mildred M, Carroll C, Cantrell A. Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of chronic Pseudomonas aeruginosa lung infection in cystic fibrosis: systematic review and economic model. Health Technol Assess. 2013;17(56):v–xvii–1–181.
Flume PA, Aitken ML, Bilton D, Agent P, Charlton B, Forster E, et al. Optimising inhaled mannitol for cystic fibrosis in an adult population. Breathe (Sheff). 2015;11(1):39–48.
Sapina-Vivo R, Lloyd EA, Mujtaba H, Spencer-Clegg E, Walshaw M. 40 Experience with Colobreathe® in a large adult cystic fibrosis unit. J Cyst Fibros. 2014;13:S57.
Cameron S, Choyce J, Ahitan B, Brown C, Rashid R, Whitehouse JL, et al. 39 “Real world” tolerability, ease of use, patient satisfaction and reported adherence in CF adults commencing Colobreathe®. J Cyst Fibros. 2014;13(1):S56–62.
Harrison MJ, McCarthy M, Fleming C, Hickey C, Shortt C, Eustace JA, et al. Inhaled versus nebulised tobramycin: a real world comparison in adult cystic fibrosis (CF). J Cyst Fibros. 2014;13(6):692–8.
Stoltz DA, Meyerholz DK, Welsh MJ. Origins of cystic fibrosis lung disease. N Engl J Med. 2015;372(4):351–62.
Mall MA, Hartl D. CFTR: cystic fibrosis and beyond. Eur Respir J. 2014;44(4):1042–54.
Pittman JE, Cutting G, Davis SD, Ferkol T, Boucher R. Cystic fibrosis: NHLBI workshop on the primary prevention of chronic lung diseases. Ann Am Thorac Soc. 2014;11 Suppl 3:S161–8.
De Boeck K, Kent L, Davies J, Derichs N, Amaral M, Rowe SM, et al. CFTR biomarkers: time for promotion to surrogate end-point. Eur Respir J. 2013;41(1):203–16.
Amin R, Ratjen F. Emerging drugs for cystic fibrosis. Expert Opin Emerg Drugs. 2014;19(1):143–55.
MacKenzie T, Gifford AH, Sabadosa KA, Quinton HB, Knapp EA, Goss CH, et al. Longevity of patients with cystic fibrosis in 2000 to 2010 and beyond: survival analysis of the cystic fibrosis foundation patient registry. Ann Intern Med. 2014;161(4):233–41.
Kerem E, Viviani L, Zolin A, MacNeill S, Hatziagorou E, Ellemunter H, et al. Factors associated with FEV1 decline in cystic fibrosis: analysis of the ECFS patient registry. Eur Respir J. 2014;43(1):125–33.
Stephenson AL, Tom M, Berthiaume Y, Singer LG, Aaron SD, Whitmore GA, et al. A contemporary survival analysis of individuals with cystic fibrosis: a cohort study. Eur Respir J. 2015;45(3):670–9.
Acknowledgments
No funding or sponsorship was received for this study or publication of this article. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published. During the peer review process, the manufacturer of the agent under review was offered an opportunity to comment on the article. Changes resulting from comments received were made by the author based on their scientific and editorial merit.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures.
Carsten Schwarz received honoraria from Forest Laboratories for advisory board membership.
Compliance with ethics guidelines.
This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Schwarz, C. Colobreathe® for the Treatment of Cystic Fibrosis-Associated Pulmonary Infections. Pulm Ther 1, 19–30 (2015). https://doi.org/10.1007/s41030-015-0007-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41030-015-0007-6