Abstract
Introduction
This article evaluates the efficacy and safety of baricitinib 4 mg versus placebo in United States including Puerto Rico (US) and rest of the world (ROW) subpopulations using data pooled from RA-BEAM and RA-BUILD, which enrolled patients with moderate-to-severe adult-onset rheumatoid arthritis (RA).
Methods
In RA-BEAM, patients with an inadequate response (IR) to methotrexate, at least one X-ray erosion, and high sensitivity C-reactive protein (hsCRP) ≥ 6 mg/L were randomized to placebo or orally administered baricitinib 4 mg daily or subcutaneously administered adalimumab 40 mg every other week. In RA-BUILD, patients with an IR to at least one conventional synthetic disease-modifying antirheumatic drug (csDMARD) and with hsCRP ≥ 3.6 mg/L were randomized to placebo or baricitinib 2 or 4 mg daily. Patients in both trials were biologic naive. In this post hoc analysis, data from both studies were pooled (714 baricitinib 4 mg-treated, 716 placebo-treated patients).
Results
Overall, 188 US and 1242 ROW patients were included. Subgroups differed in baseline characteristics including race, weight, age, time since RA diagnosis, current corticosteroid use, and previous csDMARD use. At weeks 12 and 24, baricitinib-treated patients had larger responses compared to placebo-treated patients for multiple efficacy outcomes: American College of Rheumatology 20/50/70 response, low disease activity, remission, Disease Activity Score 28-C-reactive protein, and Health Assessment Questionnaire-Disability Index. Overall, similar efficacy was observed in US and ROW subgroups with no notable safety differences between subgroups at weeks 12 or 24.
Conclusion
Baricitinib 4 mg was efficacious compared to placebo in US and ROW subpopulations. Safety was similar between subgroups.
Funding
Eli Lilly & Company and Incyte Corporation.
Trial Registration
ClinicalTrials.gov identifiers, NCT01721057; NCT01710358.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is a systemic inflammatory autoimmune disease with heterogeneous disease courses that may be associated with progressive joint destruction, reduced quality of life, and even reduced survival [1, 2]. Management of RA has improved substantially in recent years with improved patient outcomes and clinical remission becoming more achievable. Because persistent joint inflammation can lead to progressive joint destruction and functional impairment, current guidelines recommend clinical remission as the primary treatment goal [3, 4]. Joint damage can occur within months of disease onset, and early aggressive treatment provides increased probability of disease control and minimizes the long-term impact of RA [1, 5].
Conventional synthetic disease-modifying antirheumatic drugs (csDMARDs) such as methotrexate are generally used as initial treatment of RA [3, 4]. However, many patients have active disease despite the use of these agents or are intolerant to them. Hence, there is a need for improved RA treatments.
Baricitinib is an orally administered, selective, reversible inhibitor of Janus kinase (JAK)1 and JAK2 [6], which are endogenous signal transducers of proinflammatory cytokines involved in inflammatory diseases such as RA [7]. In two global, double-blind phase 3 studies in patients with active RA and either inadequate response (IR) to csDMARDs (RA-BUILD) [8] or IR to methotrexate (RA-BEAM) [9], once daily (QD) baricitinib was associated with clinical improvements through 24 weeks, with an acceptable safety profile. Geographic differences in RA presentation and its management may affect patient outcomes. The objective was to perform a subgroup analysis evaluating the efficacy and safety of baricitinib 4 mg compared to placebo in patients from the United States including Puerto Rico (US) and the “rest of the world” (ROW) using pooled data sets to identify possible demographic and clinical characteristics that may contribute to patient response to therapy. Understanding these characteristics can provide additional information for the clinician that is relevant to their patient population and assessment of response. The dose of baricitinib 4 mg was chosen because it was common to both RA-BEAM and RA-BUILD [8, 9].
Methods
Patients
This is a post hoc pooled analysis from RA-BUILD (NCT01721057) [8] and RA-BEAM (NCT01710358) [9]. In both trials, key inclusion criteria included ≥ 6 out of 68 tender joints, ≥ 6 out of 66 swollen joints, and IR to at least one csDMARD (stable background csDMARD permitted). In RA-BUILD, inclusion criteria included high-sensitivity C-reactive protein (hsCRP) ≥ 3.6 mg/L [8] and in RA-BEAM inclusion criteria included hsCRP ≥ 6 mg/L [9]. Additionally, inclusion in RA-BEAM required either ≥ 1 joint erosion in the hand, wrist, or foot with rheumatoid factor (RF) or anti-citrullinated peptide antibody (ACPA) positive status or ≥ 3 joint erosions regardless of RF or ACPA status [9]. Exclusion criteria in both studies included previous biologic DMARD use [8, 9]. Both studies were conducted in accordance with ethical principles of the Declaration of Helsinki and Good Clinical Practice guidelines and approved by ethical review boards for each center. All patients provided written informed consent before enrollment.
Treatment Regimens
In RA-BUILD, patients were randomly assigned 1:1:1 to placebo or orally administered baricitinib (2 or 4 mg QD) and treated for 24 weeks [8]. In RA-BEAM, patients were randomized 3:3:2 to placebo, orally administered baricitinib 4 mg QD, or subcutaneously administered adalimumab 40 mg every other week, respectively, and treated for 52 weeks [9]. In both trials, randomization was stratified by region and baseline joint erosion status, and the primary endpoint was American College of Rheumatology 20% response (ACR20) at week 12 [8, 9]. At week 16 or subsequent visits, inadequate responders received baricitinib 4 mg QD as rescue therapy. Inadequate response was defined as lack of improvement of at least 20% in both tender joint count and swollen joint count at both week 14 and week 16 compared to baseline. The pooled data set presented focuses on baricitinib 4 mg and placebo. Geographically defined subpopulations were US and ROW.
Efficacy Evaluations
The efficacy endpoints were the proportion of patients achieving ACR20, ACR 50% response (ACR50), and ACR 70% response (ACR70) [10], and the proportions of patients achieving low disease activity as measured by a Clinical Disease Activity Index (CDAI) [11, 12] score of ≤ 10, a Simplified Disease Activity Index (SDAI) [12, 13] score of ≤ 11, and clinical remission as measured by an SDAI score of ≤ 3.3 or a CDAI score of ≤ 2.8 [4, 12, 14]. Change from baseline in physical function was assessed by the Health Assessment Questionnaire-Disability Index (HAQ-DI) score [15, 16] and change from baseline in disease activity was assessed by the Disease Activity Score using 28 joint counts and hsCRP (DAS28-hsCRP) [17].
Safety
For the safety analyses, all randomized patients who received at least one dose of the study drug and who did not discontinue from the study for the reason “lost to follow-up” at the first postbaseline visit were included. An overview of adverse events from both trials is reported.
Statistical Analyses
Patient demographics and baseline characteristics, including sample size and percentages by treatment group, are presented using summary statistics. In the current subgroup analyses, comparisons between each baricitinib 4 mg group and placebo group were performed across subgroups (US and ROW) at weeks 12 and 24 on the modified intent-to-treat (mITT) population using summary statistics. The mITT population was defined as all randomized patients who received at least one dose of study drug.
For the categorical outcomes, nonresponder imputation was used in the analysis for patients who received either rescue therapy or discontinued from the study or study treatment. To detect significant interactions between treatment and subgroups at week 12, the following logistic regression model was used for each efficacy endpoint: treatment group + subgroup + treatment-by-subgroup interaction + study.
An interaction p value ≤ 0.10 was considered statistically significant for this analysis. When the sample size requirements were not met (if any of the treatment groups in the US or ROW subgroups had less than 30 patients in a stratum within a subgroup or less than five responders in any level of the factors in the model), the interaction p value was not calculated. Within a subgroup, the odds ratio and 95% CI are from a logistic regression model: treatment group + study. When the aforementioned sample size requirements were not met, the p value from the Cochran–Mantel–Haenszel test was used instead of the odds ratio and 95% CI.
Interpretation of subgroup interaction analyses that had a p value of ≤ 0.10 began with an examination of the direction (same as or opposite to overall treatment effect) followed by the magnitude of the treatment effect across the geographic subgroup.
Results
Baseline Characteristics
The pooled data set consisted of 714 (96 US; 618 ROW) and 716 (92 US; 624 ROW) patients in the baricitinib 4 mg and placebo groups, respectively. The proportions of patients who were White or Black/African-American were higher in US, whereas Asians were more represented in ROW (Table 1).
Patients in the US subgroup were slightly older with higher mean weight and body mass index (BMI), fewer years of RA from time of diagnosis, and a lower percentage was RF/ACPA-positive and/or used corticosteroids. Mean modified total Sharp score (mTSS) and hsCRP were higher in the ROW than the US subgroup. More patients in the US subgroup had previously used only one csDMARD whereas more patients in the ROW subgroup had previously used at least two csDMARDs.
Efficacy
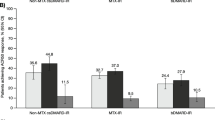
At week 12, the proportions of patients achieving ACR20, ACR50, and ACR70 responses were higher in the baricitinib group compared to the placebo group within both the US and ROW subgroups (Fig. 1a). The odds ratios for multiple efficacy measures for the baricitinib versus placebo comparisons were between 2- to 3-fold among the US subgroup and 3- to 6-fold among the ROW subgroup (Fig. 1b) favoring a positive baricitinib treatment effect compared to placebo. At week 12, the interaction p values were not significant (ACR20, p = 0.852; ACR50, p = 0.424; ACR70, p value not calculated because of small sample size). Similarly, a higher proportion of baricitinib-treated patients compared to placebo-treated patients responded at 24 weeks (Fig. 1c, d).
Efficacy at 12 and 24 weeks: baricitinib 4 mg versus placebo. Percentage (95% CI) of patients achieving ACR20, ACR50, and ACR70 at 12 weeks (a) and 24 weeks (c) using nonresponder imputation. The numbers within the bars are the actual percentages. Odds ratios (95% CI) for the baricitinib versus placebo comparisons at 12 weeks (b) and 24 weeks (d) for ACR20, ACR50, and ACR70. The values within the bars are the odds ratios. ACR20, 20% improvement using American College of Rheumatology criteria; ACR50, 50% improvement using American College of Rheumatology criteria; ACR70, 70% improvement using American College of Rheumatology criteria; BARI, baricitinib 4 mg; CI, confidence interval; N, population size; PBO, placebo; ROW, rest of the world; US, United States including Puerto Rico
At week 12 and week 24, baricitinib-treated patients experienced greater improvements in their DAS28-hsCRP and HAQ-DI scores relative to placebo-treated patients within both the US and ROW subgroups (Fig. 2). At weeks 12 and 24, a greater proportion of baricitinib-treated patients achieved low disease activity (CDAI ≤ 10 and SDAI ≤ 11) and remission (CDAI ≤ 2.8 and SDAI ≤ 3.3) compared to placebo-treated patients in both the US and ROW subgroups (Figs. 3, 4). In summary, the baricitinib treatment effect versus placebo was similar in the US and ROW subgroups for multiple efficacy endpoints.
Change from baseline in DAS28-CRP and HAQ-DI at 12 and 24 weeks: baricitinib 4 mg versus placebo. Least squares mean (95% CI) using mLOCF are shown for DAS28-hsCRP at 12 (a) and 24 weeks (b) and for HAQ-DI at 12 (c) and 24 weeks (d). The numbers within the bars are the actual values. BARI, baricitinib 4 mg; CI, confidence interval; DAS28-CRP, Disease Activity Score 28 joints high sensitivity C-reactive protein; HAQ-DI, Health Assessment Questionnaire-Disability Index; mLOCF, modified last observation carried forward; LSM, least squares mean; N, population size; PBO, placebo; ROW, rest of the world; US, United States including Puerto Rico
CDAI at 12 and 24 weeks: baricitinib 4 mg versus placebo. The percentage (95% CI) of patients achieving low disease activity defined as CDAI ≤ 10 at 12 weeks (a) and 24 weeks (b) and remission defined as CDAI ≤ 2.8 at 12 weeks (c) and 24 weeks (d) using NRI are shown. The numbers within the bars are the actual percentages. BARI, baricitinib 4 mg; CI, confidence interval; CDAI, Clinical Disease Activity Index; N, population size; NRI nonresponder imputation; PBO, placebo; ROW, rest of the world; US, United States including Puerto Rico
SDAI at 12 and 24 weeks: baricitinib 4 mg versus placebo. The percentage (95% CI) of patients achieving low disease activity defined as SDAI ≤ 11 at 12 weeks (a) and 24 weeks (b) and remission defined as SDAI ≤ 3.3 at 12 weeks (c) and 24 weeks (d) using NRI are shown. The numbers within the bars are the actual percentages. BARI, baricitinib 4 mg; CI, confidence interval; N, population size; NRI, nonresponder imputation; PBO, placebo; ROW, rest of the world; SDAI, Simplified Disease Activity Index; US, United States including Puerto Rico
Safety
Full adverse event and safety information was previously reported in the RA-BUILD and RA-BEAM manuscripts [8, 9]. As a result of the small number of patients in the US subgroup, limited analyses were conducted in this subpopulation to evaluate the incidence of adverse events in US compared to the ROW. Safety through 12 and 24 weeks is summarized in Table 2. At both 12 and 24 weeks, there were no notable differences between the US and ROW subgroups. Herpes zoster events were more frequently observed with baricitinib treatment. There were few malignancies and deaths, with no notable differences between groups.
Discussion
In this post hoc, pooled subset analysis of two phase 3 studies in patients with an IR to csDMARDs, baricitinib 4 mg was efficacious compared to placebo in both the US and the ROW subgroups. There were no notable between-subgroup differences in safety.
The geo-epidemiology of RA and other inflammatory autoimmune diseases has been discussed in the literature [18, 19]. The development of RA is complex and multifactorial with the development and severity of RA being linked to both environmental and genetic factors, such as exposure to tobacco smoke and pollutants and/or the presence of specific genetic markers, respectively. At least among women in the United States, there is geographic variation in the incidence of RA even after controlling for confounders, suggesting that regional differences in behavior, climate, environmental exposures, genetic factors, or diagnosis may exist [20].
Despite numerous geo-epidemiological studies, little is known about treatment differences between the US and the ROW and whether geographic subpopulations of RA patients respond differently to specific treatments. Within the racially and ethnically diverse US population, it is unknown whether there are differences in efficacy and safety of therapeutic agents among the various racial and ethnic subgroups. Although it is known that race-related patient preferences and access play a role in the types of RA drugs taken by Black/African-Americans [21, 22], these issues should not affect results in a clinical trial setting. Unfortunately, these studies enrolled a very small number of Black/African-Americans across the two trials (14 placebo; 11 baricitinib) (Table 1), so it is difficult to make meaningful comparisons between this subgroup and other races in this study. Similarly, the sample sizes were too small to perform additional subgroup analyses such as by age, ethnicity, or disease characteristics.
The predominant limitation of this post hoc pooled analysis was the small sample size of the US subgroup (n = 188) compared to the ROW subgroup (n = 1242), as well as differences in the baseline demographics between the US and ROW subpopulations, which included time since RA diagnosis, weight, BMI, proportion of RF/ACPA-positive patients, hsCRP, number of csDMARDs previously used, corticosteroid use, and evidence of damage (mean mTSS), all of which were greater in the ROW subpopulation with the exception of weight and BMI, which were greater in the US. However, baseline disease activity scores were similar in the US and ROW subgroups. It is possible that RA patients in the US may not have progressed as far as patients from some other countries because of earlier treatment and access to care, including earlier use of csDMARDs; this is reflected in the higher percentage of US patients that had previously used only one csDMARD before enrolling in the clinical trials.
Published literature has demonstrated that high BMI/obesity may negatively impact the response to TNF inhibitors [23,24,25] and that the presence of baseline autoantibodies and autoantibody levels have been correlated with clinical responses. In the AMPLE trial, baseline ACPA positivity (versus ACPA negativity) as measured by an anti-CCP2 ELISA was associated with better responses to abatacept or adalimumab; patients with the highest baseline ACPA antibody concentrations had better clinical response to abatacept than patients with lower concentrations, which was not observed with adalimumab [26]. These analyses were not possible here because of the limited sample sizes in this subpopulation analyses.
Additionally, we previously performed an integrated subgroup analysis through 12 weeks for an all-phase csDMARD-IR analysis set to evaluate potential subgroup interactions for baricitinib 4 mg QD versus placebo (data on file). This analysis set includes data from placebo- and active-controlled phase 2 and phase 3 studies that evaluated baricitinib on a background of csDMARD treatment in patients with active RA. Consistent with results in the overall patient samples from these studies, there was no evidence suggesting an absent or unfavorable baricitinib treatment effect (i.e., a qualitative interaction) in any subgroup based on demographic or disease-related characteristics (including age, RF/ACPA- positivity, or disease state at baseline).
Conclusions
Baricitinib 4 mg demonstrated higher clinical responses compared to placebo in RA patients with IR to methotrexate and/or csDMARD within both the US and ROW subpopulations despite some differences in baseline patient characteristics. As more targeted synthetic agents are developed to treat various rheumatic diseases, it is crucial to establish that such therapies maintain their efficacy and safety profile in wide, heterogeneous patient populations.
References
Colmegna I, Ohata BR, Menard HA. Current understanding of rheumatoid arthritis therapy. Clin Pharmacol Ther. 2012;91:607–20.
Smolen JS, Steiner G. Therapeutic strategies for rheumatoid arthritis. Nat Rev Drug Discov. 2003;2:473–88.
Smolen JS, Landewé R, Breedveld FC, et al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2013 update. Ann Rheum Dis. 2014;73:492–509.
Singh JA, Saag KG, Bridges SL Jr, et al. 2015 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68:1–26.
Klareskog L, Catrina AI, Paget S. Rheumatoid arthritis. Lancet. 2009;373:659–72.
Fridman JS, Scherle PA, Collins R, et al. Selective inhibition of JAK1 and JAK2 is efficacious in rodent models of arthritis: preclinical characterization of INCB028050. J Immunol. 2010;184:5298–307.
O’Shea JJ, Kontzias A, Yamaoka K, et al. Janus kinase inhibitors in autoimmune diseases. Ann Rheum Dis 2013;72(Suppl 2):ii111–ii115.
Dougados M, van der Heijde D, Chen YC, et al. Baricitinib in patients with inadequate response or intolerance to conventional synthetic DMARDs: results from the RA-BUILD study. Ann Rheum Dis. 2017;76:88–95.
Taylor PC, Keystone EC, van der Heijde D, et al. Baricitinib versus placebo or adalimumab in rheumatoid arthritis. N Engl J Med. 2017;376:652–62.
Felson DT, Anderson JJ, Boers M, et al. American College of Rheumatology preliminary definition of improvement in rheumatoid arthritis. Arthritis Rheum. 1995;38:727–35.
Aletaha D, Nell VP, Stamm T, et al. Acute phase reactants add little to composite disease activity indices for rheumatoid arthritis: validation of a clinical activity score. Arthritis Res Ther. 2005;7:R796–806.
Aletaha D, Smolen J. The Simplified Disease Activity Index (SDAI) and the Clinical Disease Activity Index (CDAI): a review of their usefulness and validity in rheumatoid arthritis. Clin Exp Rheumatol. 2005;23:S100–8.
Smolen JS, Breedveld FC, Schiff MH, et al. A simplified disease activity index for rheumatoid arthritis for use in clinical practice. Rheumatology. 2003;42:244–57.
Felson DT, Smolen JS, Wells G, et al. American College of Rheumatology/European League against Rheumatism provisional definition of remission in rheumatoid arthritis for clinical trials. Ann Rheum Dis. 2011;70:404–13.
Fries JF, Spitz P, Kraines RG, et al. Measurement of patient outcome in arthritis. Arthritis Rheum. 1980;23:137–45.
Fries JF, Spitz PW, Young DY. The dimensions of health outcomes: the health assessment questionnaire, disability and pain scales. J Rheumatol. 1982;9:789–93.
DAS-28. Disease Activity Score in rheumatoid arthritis. Nijmegen, the Netherlands: University Medical Center. http://www.das-score.nl/das28/. Accessed 16 Nov 2016.
Shapira Y, Agmon-Levin N, Shoenfeld Y. Geoepidemiology of autoimmune rheumatic diseases. Nat Rev Rheumatol. 2010;6:468–76.
Tobón GJ, Youinou P, Saraux A. The environment, geo-epidemiology, and autoimmune disease: rheumatoid arthritis. J Autoimmun. 2010;35:10–4.
Costenbader KH, Chang SC, Laden F, et al. Geographic variation in rheumatoid arthritis incidence among women in the United States. Arch Intern Med. 2008;168:1664–70.
Constantinescu F, Goucher S, Weinstein A, et al. Racial disparities in treatment preferences for rheumatoid arthritis. Med Care. 2009;47:350–5.
Solomon DH, Ayanian JZ, Yelin E, et al. Use of disease-modifying medications for rheumatoid arthritis by race and ethnicity in the National Ambulatory Medical Care Survey. Arthritis Care Res (Hoboken). 2012;64:184–9.
Klaasen R, Wijbrandts CA, Gerlag DM, et al. Body mass index and clinical response to infliximab in rheumatoid arthritis. Arthritis Rheum. 2011;63:359–64.
Micheroli R, Hebeisen M, Wildi LM, et al. Impact of obesity on the response to tumor necrosis factor inhibitors in axial spondyloarthritis. Arthritis Res Ther. 2017;19:164.
Ibáñez Vodnizza SE, Nurmohamed MT, Visman IM, et al. Fat mass lowers the response to tumor necrosis factor-α blockers in patients with ankylosing spondylitis. J Rheumatol. 2017;44:1355–61.
Sokolove J, Schiff M, Fleischmann R, et al. Impact of baseline anti-cyclic citrullinated peptide-2 antibody concentration on efficacy outcomes following treatment with subcutaneous abatacept or adalimumab: 2-year results from the AMPLE trial. Ann Rheum Dis. 2016;75:709–14.
Acknowledgements
The authors wish to thank the patients and their families and study personnel who participated in these clinical trials.
Funding
This work was supported by Eli Lilly and Company and Incyte Corporation. The article processing charges were funded by Eli Lilly and Company. All authors had full access to all of the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis.
Medical Writing and/or Editorial Assistance and Statistical Assistance
Lori Kornberg, PhD and Meredith Fraser, MFA, who are full-time employees of Syneos Health (Raleigh, NC), provided writing support and editorial support. Jinglin Zhong, MS (IQVIA, Morrisville, NC) assisted with the statistical analyses.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
AF Wells reports research support and consulting fees from Eli Lilly and Company. M Greenwald reports that her institution has ongoing research grants from Eli Lilly and Company. JD Bradley is an employee of Eli Lilly and Company and owns stock. V Arora is an employee of Eli Lilly and Company and owns stock. CE Kartman is an employee of Eli Lilly and Company and owns stock. J Alam was an employee of Eli Lilly and Company at the time that this work was conducted.
Compliance with Ethics Guidelines
Both studies were conducted in accordance with ethical principles of the Declaration of Helsinki and Good Clinical Practice guidelines and approved by ethical review boards for each center. All patients provided written informed consent before enrolment.
Data Availability
Lilly provides access to relevant anonymized patient level data from studies on approved medicines and indications as defined by the sponsor specific information on clinicalstudydatarequest.com. For details on submitting a request see the instructions provided at clinicalstudydatarequest.com.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced digital features
To view enhanced digital features for this article go to https://doi.org/10.6084/m9.figshare.6127052.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Wells, A.F., Greenwald, M., Bradley, J.D. et al. Baricitinib in Patients with Rheumatoid Arthritis and an Inadequate Response to Conventional Disease-Modifying Antirheumatic Drugs in United States and Rest of World: A Subset Analysis. Rheumatol Ther 5, 43–55 (2018). https://doi.org/10.1007/s40744-018-0110-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40744-018-0110-x