Abstract
Background
Past studies examining the cognitive empathy of medical school graduates grouped the various residency selections vs. parsing them out. This study examines both affective and cognitive empathy scores of osteopathic medical school graduates entering eleven different residency specialties.
Methods
Participants from the Campbell University Jerry M. Wallace School of Osteopathic Medicine (CUSOM) classes of 2017–2019 completed the Balanced Emotional Empathy Scale (BEES; measuring affective empathy) and the Jefferson Scale of Empathy, Student version (JSE-S; measuring cognitive empathy). Empathy scores were compared to residency choice upon graduation. The specialty choices were broken into two groups: Core specialties (i.e., people-oriented) that include Family Medicine, Internal Medicine, Obstetrics and Gynecology (OB/Gyn), Pediatrics, and Psychiatry. The remaining specialties are considered Non-Core specialties (i.e., technical/procedure-oriented) and included Anesthesiology, Diagnostic Radiology, Emergency Medicine, General Surgery, Neurology, and Orthopedics. Results are compared to data from the nationwide Project in Osteopathic Medical Education and Empathy (POMEE).
Results
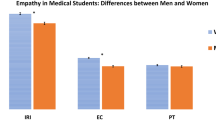
Women graduates tended to have larger BEES and JSE-S scores than men. Affective empathy scores were the largest for students selecting Core specialties. Four of these Core specialties were in the top four positions out of the eleven specialties selected by eight or more graduates. None of the eleven specialties was ranked higher than the 50th percentile compared to BEES score norms. Cognitive empathy scores were also the largest for students selecting Core specialties. All five of the Core specialties were in the top six positions out of the eleven specialties. None of the eleven specialties ranked greater than the 39th percentile when compared to OMS-III and OMS-IV POMEE data. Only women entering Psychiatry had a JSE-S score that was greater than the 50th percentile.
Conclusions
Osteopathic graduates selecting the five Core specialties have BEES and JSE-S scores that are, usually, larger than students entering Non-Core specialties. For either survey instrument, both Pediatrics and Family Medicine were first and second out of a possible 11 positions, respectively. Most CUSOM graduates had JSE-S scores lower than their peers in other osteopathic medical schools that participated in the POMEE study. When the CUSOM data are compared to allopathic data, there is no clear evidence that osteopathic students have substantially higher affective or cognitive empathy scores than their allopathic peers. Therefore, it appears that medical students who select osteopathy for its tenant of a more holistic approach to patient care are no more empathetic than students studying allopathic medicine. Several suggestions are made on how to potentially increase student empathy during undergraduate medical education.
Similar content being viewed by others
References
Chaitoff A, Sun B, Windover A, Bokar D, Featherall J, Rothberg MB, Misra-Hebert AD. Associations between physician empathy, physician characteristics, and standardized measures of patient experience. Acad Med. 2017;92(10):1464–71. https://doi.org/10.1097/ACM.0000000000001671.
Del Canale S, Louis DZ, Maio V, Wang X, Rossie G, Hojat M, Gonnella JS. The relationship between physician empathy and disease complications: an empirical study of primary care physicians and their diabetic patients in Parma. Italy Acad Med. 2012;87(9):1243–9. https://doi.org/10.1097/ACM.0b013e3182628fbf.
Hojat M, Louis DZ, Markham FW, Wender R, Rabinowitz C, Gonnella JS. Physicians’ empathy and clinical outcomes in diabetic patients. Acad Med. 2011;86:359–64. https://doi.org/10.1097/ACM.0b013e3182086fe1.
Stewart MA. Effective physician-patient communication and health outcomes: a review. Canadian Med Assoc J. 1996;152:1423–33.
Rakel D, Barrett B, Zhang Z, Hoeft T, Chewning B, Marchand L, Scheder J. Perception of empathy in the therapeutic encounter: effects on the common cold. Patient Educ Couns. 2011;84(3):390–7. https://doi.org/10.1016/j.pec.2011.01.009.
Levinson W, Roter D, Mullooly JP, Dull VT, Frankel R. Physician-patient communication: the relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;277:553–9. https://doi.org/10.1001/jama.277.7.553.
Colliver JA, Willis MS, Robbs RS, Cohen DS, Swartz MH. Assessment of empathy in a standardized-patient examination. Teach Learn Med. 1998;10:8–11. https://doi.org/10.1207/S15328015TLM1001_2.
LaNoue MD, Roter DL. Exploring patient-centeredness: the relationship between self-reported empathy and patient-centered communication in medical trainees. Patient Educ Couns. 2018;101(6):1143–6. https://doi.org/10.1016/j.pec.2018.01.016.
Mehrabian A, Young AL, Sato S. Emotional empathy and associated individual differences. Curr Psychol Res Rev. 1988;8:221–40.
Mehrabian A. Manual for the Balanced Emotional Empathy Scale (BEES). 1996 (Note: As of 2014, the BEES is no longer available for distribution by Dr. Mehrabian).
Newton, BW. Walking a fine line: is it possible to remain an empathic physician and have a hardened heart?. In: The neural underpinnings of vicarious empathy, Peter Enticott, ed., Front Hum Neurosci. 2013;11(7):233. https://doi.org/10.3389/fnhum.2013.00233.
Davis MH. A multidimensional approach to individual differences in empathy. JSAJ Catalog of Selected Docs Psychol. 1980;10(4):85.
Hogan R. Development of an empathy scale. J Consult Clin Psychol. 1969;33(3):307–16. https://doi.org/10.1037/h0027580.
Hojat M, Mangione S, Nasca TJ, Cohen MJ, Gonnella JS, Erdmann JB, et al. The Jefferson Scale of Physician Empathy: development and preliminary psychometric data. Educ Psychol Measure. 2001;61(2):349–65. https://doi.org/10.1177/00131640121971158.
Hojat M, Gonnella JS, Nasca TJ, Mangione S, Vergare M, Magee M. Physician empathy: definition, components, measurement, and relationship to gender and specialty. Am J Psychiatry. 2002;159(9):1563–9. https://doi.org/10.1176/appi.ajp.159.9.1563.
Foreback J, Kusz H, Lepisto BL, Pawlaczyk B. Empathy in internal medicine residents at community-based hospitals: a cross-sectional study. J Med Educ Curric Devl. 2018;5:1–4. https://doi.org/10.1177/2382120518771352.
Stratta EC, Riding DM, Baker P. Ethical erosion in newly qualified doctors: perceptions of empathy decline. Int J Med Educ. 2016;7:286–92. https://doi.org/10.5116/ijme.57b8.48e4.
Neumann M, Edelhäuser F, Tauschel D, Fischer MR, Wirtz M, Woopen C, et al. Empathy decline and its reasons: a systematic review of studies with medical students and residents. Acad Med. 2011;86(8):996–1009. https://doi.org/10.1097/ACM.0b013e318221e615.
Mangione S, Kane GC, Caruso JW, Gonnella JS, Nasca TJ, Hojat M. Assessment of empathy in different years of internal medicine training. Med Teach. 2002;24(4):370–3. https://doi.org/10.1080/01421590220145725.
Hojat M, Mangione S, Nasca TJ, Gonnella JS. Empathy scores in medical school and ratings of empathic behavior in residency training 3 years later. J Soc Psychol. 2005;145(6):663–72. https://doi.org/10.3200/SOCP.145.6.663-672.
Newton BW, Clardy J, Barber L, Cleveland E. Who has heart? Vicarious empathy vs. residency match. Med Sci Educ. 2014;24(1):45–50. https://doi.org/10.1007/s40670-014-0021-6.
Calabrese LH, Bianco JA, Mann D, Massello D, Hojat M. Correlates and changes in empathy and attitudes toward interprofessional collaboration in osteopathic medical students. J Am Osteopath Assoc. 2013;113(2):898–907. https://doi.org/10.7556/jaoa.2013.068.
Magalhães E, Salgueria AP, Costa P, Costa MJ. Empathy in senior and first year medical students: a cross-sectional study. BMC Med Educ. 2011;11:52. https://doi.org/10.1186/1472-6920-11-52.
Hojat M, Zuckerman M, Magee M, Mangione S, Nasca T, Vergare M, Gonnella JS. Empathy in medical students as related to specialty interest, personality, and perceptions of mother and father. Person Individ Diff. 2005;39(7):1205–15. https://doi.org/10.1016/j.paid.2005.04.007.
Santos MA, Grosseman S, Morelli TC, Giuliano ICB, Erdmann TR. Empathy differences by gender and specialty preference in medical students: a study in Brazil. Int J Med Educ. 2016;7:149–53. https://doi.org/10.5116/ijme.572f.115f.
Hojat M, Shannon SC, DeSantis J, Speicher MR, Bragan L, Calabrese LH. Empathy in medicine national norms for the Jefferson Scale of Empathy: a nationwide project in osteopathic medical education and empathy (POMEE). J Am Osteopath Assoc. 2019;119(8):520–32. https://doi.org/10.7556/jaoa.2019.091.
Newton BW, Barber L, Clardy J, Cleveland E, O’Sullivan P. Is there hardening of the heart during medical school? Acad Med. 2008;83(3):244–9. https://doi.org/10.1097/ACM.0b013e3181637837.
Hojat M, DeSantis J, Shannon SC, Speicher MR, Bragan L, Calabrese LH. Empathy as related to gender, age, race, ethnicity, academic background and career interest: a nationwide study of osteopathic medical students in the United States. Med Educ. 2020;54:571–81. https://doi.org/10.1111/medu.14138.
Newton BW, Vaskalis Z. A cross-sectional study of affective and cognitive empathy of the osteopathic classes of 2017–2020. Med Sci Educ. 2017;27(suppl. 1):S22.
Christov-Moore L, Simpson EA, Coudé G, Grigaityte K, Iacoboni M, Ferrari PF. Empathy: gender effects in brain and behavior. Neurosci Biobehav Rev. 2014;46(4):604–27. https://doi.org/10.1016/j.neubiorev.2014.09.001.
Decety J. The neurodevelopment of empathy in humans. Dev Neurosci. 2010;32(4):257–67. https://doi.org/10.1159/000317771.
Singer T, Seymour B, O’Doherty J, Kaube H, Dolan RJ, Frith CD. Empathy for pain involves the affective but not sensory components of pain. Science. 2004;303:1157–62. https://doi.org/10.1126/science.1093535.
Singer T, Lamm C. The social neuroscience of empathy. Ann NY Acad Sci. 2009;1156:81–96. https://doi.org/10.1111/j.1749-6632.2009.04418.x.
Berkley KJ. Sex differences in pain. Behav Brain Sci. 1997;20(3):371–80. https://doi.org/10.1017/s0140525x97221485.
Fillingim RB. Sex, gender, and pain: women and men are really different. Curr Rev Pain. 2000;4(1):24–30. https://doi.org/10.1007/s11916-000-0006-6.
Chen C, Martinez RM, Chen Y. The developmental origins of the social brain: empathy, morality, and justice. Front Psychol. 2018;9:2584. https://doi.org/10.3389/fpsyg.2018.02584.
Eisenberg N. Empathy-related responding and prosocial behavior. Novartis Found Symp. 2007;278:71–80. PMID 17214311.
Eisenberg N, Morris, AS, McDaniel B, Spinrad TL. Moral cognitions and prosocial responding in adolescence. In Lerner RM, Steinberg L (Eds.). Handbook of adolescent psychology (pp. 229–265). 2009. New York, NY: John Wiley & Sons.
Hojat M, DeSantis J, Shannon SC, Mortensen LH, Speicher MR, Bragan L, et al. The Jefferson Scale of Empathy: a nationwide study of measurement properties, underlying components, latent variable structure, and national norms in medical students. Adv Health Sci Educ Theory Pract. 2018;23(5):899–920. https://doi.org/10.1007/s10459-018-9839-9.
Hojat M. Empathy in health professions education and patient care. 2016. New York, NY: Springer. ISBN: 978-3-319-27624-3.
Thompson BM, Hearn GN, Collins MJ. Patient perceptions of health professional interpersonal skills. Australian Psychol. 1992;27(2):91–5. https://doi.org/10.1080/00050069208257586.
Decety J, Yang CY, Cheng Y. Physicians down-regulate their pain empathy response: an event-related brain potential study. Neuroimage. 2010;50(4):1676–82. https://doi.org/10.1016/j.neuroimage.2010.01.025.
Stefanello E. Your pain is not mine: a critique of clinical empathy. Bioethics. 2021;1–8. https://doi.org/10.1111/bioe.12980.
Backović DV, Zivojinović JI, Maksimović J, Maksimović M. Gender differences in academic stress and burnout among medical students in final years of education. Psychiatr Danub. 2012;24(2):175–81. PMID: 22706416.
Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med. 2006;81(4):354–73. https://doi.org/10.1097/00001888-200604000-00009.
Riess H, Kraft-Todd G. EMPATHY: a tool to enhance nonverbal communication between clinicians and their patients. Acad Med. 2014;89:1108–12. https://doi.org/10.1097/ACM.0000000000000287.
Hojat M. Ten approaches for enhancing empathy in health and human services cultures. J Health Hum Serv Adm Spring. 2009;31(4):412–50. https://doi.org/10.2307/25790741.
Harden RM. Twelve tips on teaching and learning how to break bad news. Med Teach. 1996;18(4):275–8. https://doi.org/10.3109/01421599609034177.
Hojat M, DeSantis J, Cain RA, Speicher MR, Bragan L, Shannon SC, Calabrese LH. Attitudes toward osteopathic medicine scale: development and psychometrics. Int J Med Educ. 2021;12:222–32. https://doi.org/10.5116/ijme.615c2cf.
Acknowledgements
The author is grateful to those members of the CUSOM graduating classes of 2017–2019 who participated in the longitudinal empathy study. Various aspects of these data were presented in abstract form at the 2007, 2008, and 2015–2019 meetings of the International Association for Medical Science Educators (IAMSE).
Author information
Authors and Affiliations
Contributions
The author designed the study, collected the data, and wrote the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
N/A. Informed consent was obtained from all participants in this study via Campbell University IRB #030.
Consent for Publication
N/A.
Conflict of Interest
The author has no conflicts of interest to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Newton, B.W. Having Heart: Affective and Cognitive Empathy Scores vs. Residency Specialty Match at an Osteopathic Medical School. Med.Sci.Educ. 32, 423–436 (2022). https://doi.org/10.1007/s40670-022-01526-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-022-01526-9