Abstract
Background
With medical education shifting towards competency-based models, medical students are expected to be self-directed lifelong learners. There is an urgent need to understand what technology students adopt for self-directed learning and what factors contributed to students’ self-initiated technology use.
Method
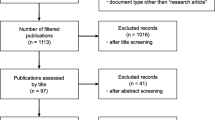
This study took place in a midwestern university medical school, which implements a flipped classroom model where students are required to learn all the course materials independently before class. Twenty-six first- and second-year medical students participated in a semi-structured interview about their self-directed learning with technology, and contributing factors towards technology use. A qualitative description methodology using thematic analysis was used to identify key themes from the interview data.
Results
Medical students reported using four types of technologies for learning video resources, self-assessment tools, management tools, and social media. Three key determinants of students’ self-directed technology use were identified, including perceived usefulness, subjective norms, and educational compatibility.
Conclusions
By probing medical students’ self-initiated technology use and its determinants, this study suggested that in a self-directed learning environment, medical students used a variety of third-party resources to facilitate learning and develop self-directed learning skills. This study also provided important practical implications to better support students’ productive use of technologies for self-directed learning.

Similar content being viewed by others
References
Hawkins RE, Welcher CM, Holmboe ES, Kirk LM, Norcini JJ, Simons KB, et al. Implementation of competency-based medical education: are we addressing the concerns and challenges? Med Educ. 2015;49(11):1086–102.
Lucey CR, Thibault GE, Ten Cate O. Competency-based, time-variable education in the health professions: crossroads. Acad Med. 2018;93(3S):S1-5.
Liaison Committee on Medical Education. Functions and Structure of a Medical School Standards for Accreditation of Medical Education Programs Leading to the MD Degree. [Internet]. 2020. Available from: https://lcme.org/publications/#Standard
Hill M, Peters M, Salvaggio M, Vinnedge J, Darden A. Implementation and evaluation of a self-directed learning activity for first-year medical students. Med Educ Online. 2020;25(1):1717780.
Scott K, Morris A, Marais B. Medical student use of digital learning resources. Clin Teach. 2018;15(1):29–33.
Jones N. Social networking sites and medical education. Clin Teach. 2017;14(6):456–7.
Curran V, Matthews L, Fleet L, Simmons K, Gustafson DL, Wetsch L. A review of digital, social, and mobile technologies in health professional education. J Contin Educ Health Prof. 2017;37(3):195–206.
Ajzen I. From intentions to actions: a theory of planned behavior. In: Kuhl J, Beckmann J, editors. Action control: from cognition to behavior [Internet]. Berlin, Heidelberg: Springer; 1985 [cited 2020 Aug 17]. p. 11–39. (SSSP Springer Series in Social Psychology). Available from: https://doi.org/10.1007/978-3-642-69746-3_2.
Davis FD. Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q. 1989;13(3):319–40.
Lai C. A framework for developing self-directed technology use for language learning. Lang Learn Technol. 2013;17(2):100–22.
Lai C, Wang Q, Lei J. What factors predict undergraduate students’ use of technology for learning? A case from Hong Kong. Comput Educ. 2012;59(2):569–79.
Fishbein M, Ajzen I. Belief, attitude, intention, and behavior: an introduction to theory and research. Addison-Wesley Publishing Company; 1975. 600 p.
Chen J-L. The effects of education compatibility and technological expectancy on e-learning acceptance. Comput Educ. 2011;57(2):1501–11.
Guest G, Bunce A, Johnson L. How many interviews are enough?: an experiment with data saturation and variability. Field Methods. 2006;18(1):59–82.
Guest G, Namey E, Chen M. A simple method to assess and report thematic saturation in qualitative research. PLoS One. 2020;15(5):e0232076.
Gale NK, Heath G, Cameron E, Rashid S, Redwood S. Using the framework method for the analysis of qualitative data in multi-disciplinary health research. BMC Med Res Methodol. 2013;13(1):1–8.
Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology. 2006 1;3(2):77–101.
Yot-Domínguez C, Marcelo C. University students’ self-regulated learning using digital technologies. Int J Educ Technol High Educ. 2017;14(1):38.
Echenique EEG, Molías LM, Bullen M. Students in higher education: social and academic uses of digital technology. RUSC Univ Knowl Soc J. 2015;12(1):25–37.
Burk-Rafel J, Santen SA, Purkiss J. Study behaviors and USMLE Step 1 performance: implications of a student self-directed parallel curriculum. Acad Med. 2017;92(11S):S67-74.
Chen DR, Priest KC, Batten JN, Fragoso LE, Reinfeld BI, Laitman BM. Student perspectives on the “Step 1 Climate” in preclinical medical education. Acad Med. 2019;94(3):302–4.
Dabbagh N, Kitsantas A. Personal learning environments, social media, and self-regulated learning: a natural formula for connecting formal and informal learning. Internet High Educ. 2012;15(1):3–8.
Brydges R, Butler D. A reflective analysis of medical education research on self-regulation in learning and practice. Med Educ. 2012;46(1):71–9.
White CB, Gruppen LD, Fantone JC. Self-regulated learning in medical education. In: Tim S, editor. Understanding medical education [Internet]. John Wiley & Sons, Ltd; 2013 [cited 2018 Mar 6]. p. 201–11. Available from: https://doi.org/10.1002/9781118472361.ch15/summary.
Durning SJ, Cleary TJ, Sandars J, Hemmer P, Kokotailo P, Artino AR. Perspective: viewing “strugglers” through a different lens: how a self-regulated learning perspective can help medical educators with assessment and remediation. Acad Med J Assoc Am Med Coll. 2011;86(4):488–95.
Zheng B, Ward A, Stanulis R. Self-regulated learning in a competency-based and flipped learning environment: learning strategies across achievement levels and years. Med Educ Online. 2020;25(1):1686949.
Delen E, Liew J, Willson V. Effects of interactivity and instructional scaffolding on learning: self-regulation in online video-based environments. Comput Educ. 2014;1(78):312–20.
Schwan S, Riempp R. The cognitive benefits of interactive videos: learning to tie nautical knots. Learn Instr. 2004;14(3):293–305.
Hadwin AF, Winne PH. CoNoteS2: a software tool for promoting self-regulation. Educ Res Eval. 2001;7(2–3):313–34.
Bransen D, Govaerts MJB, Sluijsmans DMA, Driessen EW. Beyond the self: the role of co-regulation in medical students’ self-regulated learning. Med Educ. 2020;54(3):234–41.
Yousafzai SY, Foxall GR, Pallister JG. Technology acceptance: a meta-analysis of the TAM: part 1. J Model Manag. 2007;2(3):251–80.
Khalil MK, Wright WS, Spearman KA, Gaspard AC. Relationship between students’ perceptions of the adequacy of M1 and M2 curricula and their performance on USMLE Step 1 examination. BMC Med Educ. 2019;19(1):358.
Sawang S, Sun Y, Salim SA. It’s not only what I think but what they think! The moderating effect of social norms. Comput Educ. 2014;1(76):182–9.
Werner LS, Bull BS. The effect of three commercial coaching courses on Step One USMLE performance. Med Educ. 2003;37(6):527–31.
Hoi VN, Mu GM. Perceived teacher support and students’ acceptance of mobile-assisted language learning: evidence from Vietnamese higher education context. Br J Educ Technol. 2021;52(2):879–98.
Lai C, Yeung Y, Hu J. University student and teacher perceptions of teacher roles in promoting autonomous language learning with technology outside the classroom. Comput Assist Lang Learn. 2016;29(4):703–23.
Lai C. Modeling teachers’ influence on learners’ self-directed use of technology for language learning outside the classroom. Comput Educ. 2015;1(82):74–83.
van Woezik T, Koksma J, Reuzel R, Jaarsma D, Jan van der Wilt G. How to encourage a lifelong learner? The complex relation between learning strategies and assessment in a medical curriculum. Assess Eval High Educ. 2020;45(4):513–26.
Kogan JR, Hauer KE. Sparking change: how a shift to Step 1 pass/fail scoring could promote the educational and catalytic effects of assessment in medical education. Acad Med J Assoc Am Med Coll. 2020;95(9):1315–7.
Acknowledgements
I would like to express my great appreciation to Dr. Chin-Hsi Lin for his valuable and constructive suggestion and contribution during the study design and manuscript revision stages of this research work. My grateful thanks are also extended to Dr. Brian Mavis for his comments and suggestions for the manuscript revision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
This study was approved by the designated school’s institutional review board. Informed consent was obtained during the interview from students who agreed to participate in this study.
Conflict of Interest
The author declares no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zheng, B. Medical Students’ Technology Use for Self-Directed Learning: Contributing and Constraining Factors. Med.Sci.Educ. 32, 149–156 (2022). https://doi.org/10.1007/s40670-021-01497-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40670-021-01497-3