Abstract
Background
Finerenone, a selective non-steroidal mineralocorticoid receptor antagonist, improves kidney and cardiovascular outcomes in patients with chronic kidney disease (CKD) associated with type 2 diabetes (T2D). The FINE-REAL study (NCT05348733) aims to evaluate the characteristics and treatment patterns of participants treated with finerenone in clinical practice.
Methods
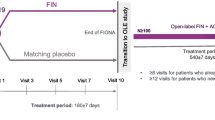
FINE-REAL is a prospective, single-arm, non-interventional study of patients initiated on finerenone as part of their routine care in accordance with country-approved labels. The study, initiated in June 2022, is expected to be completed by January 2028. The cutoff for this pre-specified interim analysis was June 13, 2023.
Results
Participants were recruited across nephrology, endocrinology, cardiology, and primary care settings. Of 556 participants enrolled in the study by the cut-off date, 504 were included in this analysis (median follow-up duration of 7 months [finerenone treatment initiation to last recorded observation]). At baseline, 76.1% of participants were in the high or very high (KDIGO) CKD risk categories. Angiotensin converting enzyme inhibitors/angiotensin receptor blockers and sodium–glucose cotransporter 2 inhibitors were prescribed to 71.8% and 46.6% of participants, respectively. Based on prescribing information, 87.9% and 12.1% of participants initiated finerenone at doses of 10 and 20 mg, respectively. Finerenone treatment was uninterrupted in 92.3% of participants after 7 months’ median follow-up. Treatment-emergent adverse events occurred in 110 (21.8%) participants. Hyperkalemia occurred in 25 (5.0%) participants, with no cases leading to death, dialysis, or hospitalization.
Conclusion
At this interim analysis, finerenone was initiated in patients with CKD and T2D across various clinical practices participating in the study. Treatment discontinuation and hyperkalemia occurred infrequently.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes (T2D) and chronic kidney disease (CKD) are rapidly growing public health burdens with high global prevalence [1,2,3]. Patients with CKD and T2D are at risk of developing other comorbidities such as cardiovascular disease, including heart failure, ischemic heart disease, cerebrovascular complications, and diabetic retinopathy [4,5,6,7,8].
Treatment guidelines recommend that patients with CKD and T2D be treated with renin–angiotensin-aldosterone system inhibitors (angiotensin-converting enzyme inhibitors [ACEis] or angiotensin receptor blockers [ARBs]) alongside sodium–glucose cotransporter 2 (SGLT2) inhibitors, and/or glucagon-like peptide-1 (GLP-1) receptor agonists (to achieve adequate glycemic control) [9, 10]. Guidance from the European Society of Cardiology (ESC) also recommends administering SGLT2 inhibitors in people with CKD and T2D to reduce cardiovascular and kidney failure risk [11]. Despite the use of ACEis, ARBs, SGLT2 inhibitors, and GLP-1 receptor agonists, the residual risk of kidney failure and cardiovascular events remains high [12,13,14].
Finerenone is a non-steroidal, selective mineralocorticoid receptor antagonist (nsMRA). It is approved for the treatment of CKD associated with T2D worldwide, including in the European Union, North, South, and Central America, and Asia [15, 16], based on demonstrated efficacy in randomized phase 3 studies (FIDELIO-DKD [NCT02540993] and FIGARO-DKD [NCT02545049]) [17,18,19]. In FIDELITY, a pre-specified pooled analysis of the FIDELIO-DKD and FIGARO-DKD studies, finerenone reduced the risk of adverse kidney and cardiovascular outcomes compared with placebo in patients treated with maximum renin–angiotensin-aldosterone system inhibition [17,18,19]. While there was a similar incidence of treatment-emergent adverse events (TEAEs), hyperkalemia occurred more frequently with finerenone than placebo; however, most occurrences were of mild-to-moderate severity with few treatment discontinuations [17,18,19]. Finerenone is also included as a recommended treatment for CKD associated with T2D by the American Diabetes Association, American Association of Clinical Endocrinologists, European Society of Cardiology, and the Kidney Disease Improving Global Outcomes (KDIGO) work group [9,10,11, 20]; and is recommended as a treatment to reduce the risk of hospitalization for heart failure in people with CKD and T2D [21].
Patients enrolled in randomized clinical trials may differ from those encountered in routine clinical practice. A retrospective, observational, cross-sectional study in the United States (US) has shown that during the initial months after receipt of marketing authorization, finerenone has been used across a broad range of people with CKD and T2D and clinical or demographic characteristics, prescribed in alignment with international clinical guidance [22]. However, the need to provide prospective real-world data (treatment patterns and patient characteristics) on the use of finerenone in routine clinical care across different geographies remains.
The FINE-REAL study aims to evaluate the characteristics, treatment patterns, and safety of finerenone in participants with CKD associated with T2D who have been enrolled across many countries and treated with finerenone in routine clinical practice [23]. In this article, a pre-specified interim analysis of FINE-REAL following participants 1 year after study initiation, with a median follow-up duration of 7 months (finerenone treatment initiation to last recorded observation), is presented.
Methods
Study participants
Eligible participants were aged ≥ 18 years, with a diagnosis of CKD (and with albuminuria in European countries in accordance with the local label) associated with T2D based on physician assessment. Participants were receiving finerenone (10 or 20 mg) in accordance with the local marketing authorization. Participants were excluded if they were involved in an investigational trial during the study and/or had a contraindication per the finerenone label [15, 16].
Study design and conduct
The study design for FINE-REAL (NCT05348733) has been described previously [23]. In brief, FINE-REAL is an ongoing, prospective, non-interventional, multi-center study aiming to enroll participants from several countries across Asia, the European Union, North, South, and Central America.
The study, initiated in June 2022, is expected to be completed by January 2028. Annual interim analyses are planned to start a year from the date of the first participant’s first visit (June 13, 2022), as pre-specified in the protocol. The data cutoff for this pre-specified interim analysis (first patient first visit + 1 year) was June 13, 2023. FINE-REAL is being conducted in compliance with the principles of the Declaration of Helsinki.
Study follow-up
All follow-up visits are being documented, but given the observational nature of the study, there is no fixed schedule for follow-up visits. Due to their underlying disease, it is expected that participants will generally have routine follow-up visits to their physician approximately every 3 months. The observation period will regularly end 12 months after the start of treatment in cases where finerenone therapy is still ongoing. In cases where the duration of finerenone therapy is less than 12 months, or after death, withdrawal of informed consent, or loss to follow-up (whichever occurs first), the last observation will be documented approximately 30 days after the end of treatment.
Assessments
Demographic characteristics and disease history were recorded at baseline, defined as ≤ 1 month prior to the first dose of finerenone [23]. Concomitant medications, laboratory parameters (estimated glomerular filtration rate [eGFR] and urine albumin:creatinine ratio [UACR]), adverse events (AE), hyperkalemia, and diabetic retinopathy assessments were recorded at baseline and follow-up visits [23]. The Chronic Kidney Disease Epidemiology Collaboration 2009 formula (CKD-EPI) without adjustment for race was used to calculate eGFR [24].
Endpoints
The primary endpoint was to describe clinical characteristics and treatment patterns in participants with CKD and T2D treated with finerenone. Outcomes included duration and dose of finerenone treatment, and use of concomitant therapies. Secondary endpoints were the occurrence of TEAEs, serious TEAEs, and hyperkalemia. Hyperkalemia outcomes included the occurrence of hyperkalemia leading to permanent discontinuation of finerenone, dialysis, hospitalization, or death. As a post-hoc analysis of FIDELIO-DKD and FIGARO-DKD suggested that finerenone may delay the progression of non-proliferative diabetic retinopathy (NPDR) [25], the incidence of diabetic retinopathy was assessed as an additional endpoint in the FINE-REAL study. The presence of diabetic retinopathy was assessed through a questionnaire at the time of consent to participate in the study, and its progression is being surveyed at later study visits.
Statistical analysis
Statistical analyses were of an exploratory and descriptive nature. Participant demographics and other baseline characteristics, prior and concomitant medication, safety, and outcomes of interest (including hyperkalemia-related events and diabetic retinopathy) were described by frequency tables and summary statistics.
TEAEs were classified according to Medical Dictionary for Regulatory Activities (MedDRA) preferred terms (PTs) and summarized by primary System Organ Class and MedDRA PT. Hyperkalemia-related events were reported as TEAEs at the investigator’s discretion. Hyperkalemia was defined according to the combined MedDRA PTs “hyperkalemia” and “blood potassium increased.” Cumulative incidence of hyperkalemia TEAEs was calculated using Aalen–Johansen estimates, with 95% confidence intervals (CIs).
All data are presented for the full analysis set, defined as all participants who signed the informed consent form and received at least one dose of finerenone during the observation period.
Results
Participant characteristics
Of 556 participants enrolled in the study at the cutoff date, 504 were included in the full analysis set. Seventeen individuals were unable to participate due to inclusion and/or exclusion criteria violation, participant decision, physician decision, or other reasons. Another 35 participants had not yet started their finerenone treatment by the cutoff date (Supplementary Fig. 1). This interim analysis included participants from the US (n = 390), China (n = 64), Belgium (n = 10), Germany (n = 23), the Netherlands (n = 11), Denmark (n = 5), and Switzerland (n = 1).
At baseline, the mean (standard deviation [SD]) age was 66.1 years (11.0) and 306 participants (60.7%) were male (Table 1). The median (interquartile range [IQR]) duration of T2D at baseline was 14.0 years (8.0–22.0). At baseline, eGFR and UACR measurements were documented for 490 (97.4%) and 359 (71.8%) participants, respectively. UACR measurements were not done in 141 (28.2%) participants. A total of 459 (93.7%) participants had an eGFR ≥ 25 mL/min/1.73 m2. Specifically, eGFR was < 15 mL/min/1.73 m2 in 3 (0.6%) participants, 15–< 30 mL/min/1.73 m2 in 72 (14.7%) participants, 30–< 45 mL/min/1.73 m2 in 154 (31.4%) participants, 45–< 60 mL/min/1.73 m2 in 119 (24.3%) participants, 60–< 90 mL/min/1.73 m2 in 93 (19.0%) participants, and ≥ 90 mL/min/1.73 m2 in 49 (10.0%) participants. The median (IQR) UACR was 295.0 mg/g (85.9–897.0), with most participants having UACR ≥ 30 mg/g (319 participants; 63.8%). There were 2.0%, 22.0%, 27.9%, and 48.2% of patients in the low, moderate, high, and very high KDIGO risk categories, respectively (Fig. 1). A total of 463 (95%) participants had a normal serum potassium range at baseline.
Proportion according to KDIGO heatmap CKD risk categories in FINE-REAL and FIDELITYa[19] at baseline. aPooled analysis of patients with CKD and T2D from the phase 3 FIDELIO-DKD and FIGARO-DKD studies. bOnly participants with a UACR with an upper limit of ≤ 5000 mg/g were permitted into the FIDELIO-DKD or FIGARO-DKD studies. CKD chronic kidney disease, eGFR estimated glomerular filtration rate, G group, KDIGO Kidney Disease Improving Global Outcomes, T2D type 2 diabetes, UACR urine albumin:creatinine ratio
At baseline, 362 participants (71.8%) were receiving ACEis or ARBs. A total of 387 (76.8%) participants were receiving statins, 241 (47.8%) were receiving insulin, 235 (46.6%) were receiving SGLT2 inhibitors, and 168 (33.3%) were receiving GLP-1 receptor agonists. Ten participants (2.0%) had documented steroidal MRA use prior to initiation of finerenone. Concomitant therapies were used in 444 (88.1%) participants for T2D treatment, 379 (75.2%) participants for comorbidity treatment, 70 (13.9%) participants for CKD treatment, and 11 (2.2%) participants for AE treatment. In addition, 225 (44.6%) participants received concomitant therapies for a reason other than T2D, CKD, comorbidity, or AE treatment.
Treatment patterns
At the cutoff date (June 13, 2023), participants in the full analysis set had been followed for a median (IQR) of 7.0 (3.4–10.0) months. A total of 443 (87.9%) and 61 (12.1%) participants initiated finerenone at doses of 10 mg and 20 mg, respectively. After initiation of finerenone, treatment was continued and uninterrupted in 465 participants (92.3%) for the entire observation period.
Finerenone treatment was interrupted (i.e. stopped and restarted) in 27 (5.4%) participants. The mean (SD) duration of treatment pause was 47.0 days. The most frequent reason for a pause in treatment administration was an AE (nine [1.8%] participants). Following a pause in treatment, finerenone was restarted without simultaneous addition of any other new co-medications in 23 (4.6%) participants, and in combination with other medications in four (0.8%) participants. Finerenone was administered concomitantly with patiromer in the first participant; dapagliflozin and sodium bicarbonate in the second participant; furosemide in the third participant (this co-medication was paused and restarted with finerenone); and allopurinol, candesartan, and empagliflozin in the fourth participant (these three co-medications were also paused and restarted with finerenone).
Finerenone was permanently discontinued in five participants. Two participants permanently discontinued finerenone due to hyperkalemia. One patient made the decision to discontinue finerenone, and treatment was discontinued in another patient due to physician decision. One patient permanently discontinued finerenone and switched to another therapy. The median (IQR) duration of finerenone administration was 112 days (104–152) among the five patients who discontinued treatment.
Safety
TEAEs were reported in 110 participants (21.8%). The most frequently reported TEAEs (≥ 1%) were hyperkalemia/blood potassium increase (25 participants; 5.0%), urinary tract infection (six participants; 1.2%, three of whom were documented to be on an SGLT2 inhibitor at the time of the event), vitamin D deficiency (six participants; 1.2%), acute kidney injury (five participants; 1%), and coronavirus disease 2019 (five participants; 1%) (Table 2). Serious TEAEs were reported for 27 participants (5.4%). The three most frequently reported serious TEAEs (≥ 0.4%) were acute kidney injury (five participants; 1.0%), coronary artery disease (two participants; 0.4%), and urinary tract infections (two participants; 0.4%) (Table 2). One participant with concomitant hepatic cancer died during the study period study because of hepatic failure. Concomitant medications to manage AEs were administered to 11 (2.2%) participants.
Hyperkalemia was reported in 25 (5.0%) participants (Table 3), with symptomatic hyperkalemia (paresthesia) only being identified in one of these participants. There were no cases of hyperkalemia leading to dialysis, hospitalization, or death. Two participants discontinued the study due to hyperkalemia. The cumulative incidence of hyperkalemia (Aalen–Johansen estimate [95% CI]) was 1.2% (0.5–2.5), 1.2% (1.3–4.1%), and 4.1% (2.5–6.4%) at months 1, 3, and 6, respectively (Supplementary Table 1).
Incidence of diabetic retinopathy
In total, diabetic retinopathy was reported in 62 participants (12.3%) at baseline. Among participants with NPDR (32 participants, 6.4%), 13 (2.6%), six (1.2%), and six (1.2%) were diagnosed with mild, moderate, or severe disease, respectively. Information on NPDR was unknown or missing in seven (1.4%) patients.
Discussion
In this prospective study of individuals with CKD and T2D receiving finerenone treatment in routine clinical practice, at baseline most participants were classified as high or very high risk per the KDIGO risk categories [9]. Relative to FIDELITY [19], FINE-REAL included a greater proportion of participants in the moderate KDIGO risk category, fewer participants in the high-risk category, and a similar number of participants in the very high-risk category at baseline at the time of this pre-specified interim analysis. This trend suggests that in routine clinical practice, physicians are increasingly treating patients with earlier stage CKD compared with participants in the randomized clinical trials.
UACR is a sensitive and early indicator of kidney damage and can be routinely used to accurately assess CKD stage and monitor kidney health [26]. The American Diabetes Association and KDIGO work group recommend that all patients with T2D be screened for CKD at least annually through the measurement of UACR and eGFR [9, 20, 27]. In FINE-REAL, a total of 71.8% of participants had UACR measurements, suggesting that patients are often screened for CKD in accordance with guideline recommendations [9, 20, 27]. Whilst guidelines recommend that patients undergo annual UACR screening [9, 20, 27], it is not a requirement, according to the prescribing information, for starting treatment with finerenone [15, 16]. Nevertheless, the prevalence of UACR screening in FINE-REAL is much higher than currently available real-world data suggest; one retrospective study reported that urine protein assessment (including UACR) was only conducted in approximately 30% of patients with CKD and T2D in the US in 2019 [28]. Early detection of CKD enables the timely administration of appropriate treatment, which is essential for preventing disease progression in patients. Treatment guidelines recommend UACR should be reduced by ≥ 30% in patients with CKD and UACR ≥ 300 mg/g [20]. Moreover, the availability of SGLT2 inhibitors and GLP-1 receptor agonists, medications in addition to ACEis and ARBs that reduce UACR [29, 30][Supplementary reference 31], may contribute to clinicians being more inclined to assess UACR.
While UACR screening is always relevant, it is clearly very important in patients treated with finerenone. A recent mediation analysis demonstrated that UACR reduction in the FIDELIO-DKD and FIGARO-DKD studies accounted for 84% of the effect of finerenone in reducing the risk of the composite kidney endpoint (onset of kidney failure, a sustained decrease in eGFR ≥ 57% over at least 4 weeks or kidney-related death) [Supplementary reference 32]. These results provide evidence supporting measuring UACR for the identification of patients eligible for finerenone therapy (both in high-risk patients and in moderate-risk patients with relatively preserved eGFRs) and the monitoring of subsequent response to treatment. The use of agents that act on the renin–angiotensin–aldosterone system, SGLT2 inhibitors, GLP-1 receptor agonists, and a nsMRA (finerenone) are described as the four pillars of treatment to reduce cardiorenal outcomes in people with T2D and CKD [Supplementary reference 33]. These agents have distinct mechanisms of action from each other, providing further evidence supporting their combinability, yet research confirming their potentially additive benefits is lacking. The FINE-REAL study will provide supporting evidence from a real-word perspective on the utilization of these pharmacological pillars for disease management.
Finerenone was continuously administered in most (92.3%) participants. Following a pause in treatment, finerenone was restarted in 27 patients. Furthermore, only five participants permanently discontinued treatment. These data suggest good tolerance as well as adherence to finerenone treatment in the study cohort. Serious TEAEs were reported in 27 (5.4%) participants, while concomitant medications to manage AEs were only administered to 11 (2.2%) participants. Moreover, this interim analysis, at a median follow-up duration of 7 months, showed that the occurrence of hyperkalemia in the real-world setting was low (5.0%), with no hyperkalemia leading to dialysis, hospitalization or death. In FIDELITY, finerenone was associated with an increase from baseline in serum potassium of 0.21 mmol/L at 4 months; thereafter, mean serum potassium levels remained stable for the remaining duration of the follow-up period [19]. Pre-specified annual analyses from FINE-REAL will provide insight on TEAE and hyperkalemia occurrences when more study participants have completed the full follow-up period.
In contrast, results from a retrospective observational study of 224,100 individuals who were documented to have initiated a steroidal MRA in the Healthcare Integrated Research Database (identified comorbidities were categorized by heart failure, CKD, or other) suggest that discontinuation of steroidal MRAs occurs more frequently in clinical practice, with 73% of individuals discontinuing treatment after a median of 90 days [Supplementary reference 34]. Steroidal MRAs are associated with a risk of hyperkalemia and do not have a label indication for reducing kidney disease progression in people with CKD and T2D [Supplementary references 35–38]. The KDIGO 2024 clinical practice guideline for the management of CKD states that a steroidal MRA may be used for heart failure, hyperaldosteronism, or refractory hypertension, but may cause hyperkalemia or a reversible decline in eGFR, especially in people with a low eGFR [Supplementary reference 39]. A systematic review and meta-analysis of 33,048 patients with diabetic kidney disease across 31 randomized controlled trials reported that hyperkalemia occurred more frequently with steroidal MRAs than finerenone when added to ACEis/ARBs; the pooled risk ratio for steroidal MRA + ACEi/ARB vs ACEi/ARB was 5.42 (95% CI 2.15–13.67) and for finerenone + ACEi/ARB vs ACEi/ARB was 2.05 (95% CI 1.84–2.28) [Supplementary reference 40]. In the phase 2 ARTS trial (NCT01807221), people with heart failure with reduced ejection fraction and mild or moderate CKD were randomized to multiple doses of finerenone or spironolactone. In this study, hyperkalemia occurred less frequently in those randomized to finerenone compared with those randomized to spironolactone (pooled finerenone vs spironolactone; 5.3 vs 12.7%, respectively) [Supplementary reference 41]. Similarly, in an indirect comparison study of finerenone and spironolactone using data from FIDELITY and the AMBER study (NCT03071263), there were fewer treatment discontinuations due to hyperkalemia with finerenone (0.3%) compared to spironolactone + patiromer (6.8%), and spironolactone + placebo (23.0%) [Supplementary reference 42].
ACEis or ARBs were prescribed to 71.8% of participants at baseline in FINE-REAL, and despite guideline recommendations, 28.2% of participants did not receive a concomitant ACEi or ARB. This may be due to multiple factors such as clinical inertia (failure to initiate or intensify treatment) and a lack of patient compliance. A recent retrospective analysis indicated that the use of concomitant medications is somewhat similar in finerenone users across two US databases; including use of concomitant ACEis/ARBs (70.5% vs 70.4%), SGLT2 inhibitors (42.5% vs 53.3%), and GLP-1 receptor agonists (35.1% vs 42.1%) [22]. However, these results must be interpreted cautiously and considered in the context of additional real-world studies of finerenone. FINE-REAL is the first global, prospective, observational study investigating the use of a nsMRA in routine clinical care in patients with CKD and T2D. These findings, and future data from this ongoing study, will help to inform decision-making with respect to initiation of finerenone in patients with CKD and T2D. As more participants are enrolled in FINE-REAL, it may be possible to analyze how finerenone initiation varies across different nations, particularly when more low- and middle-income countries are included. Moreover, FINE-REAL will likely provide information on the treatment of patients with multimorbidity, including cardiovascular comorbidities, both in terms of the multidisciplinary management (i.e. cardiologists, endocrinologists, and nephrologists) involved in their care as well as the different classes of treatments prescribed (i.e. ACEis/ARBs, SGLT2 inhibitors, GLP-1 receptor agonists, and MRAs). The American Diabetes Association/KDIGO consensus guidelines advocate for comprehensive, multidisciplinary care for patients in recognition of the need for primary and secondary prevention of diabetes-related heart and kidney complications [9].
The FINE-REAL study has several strengths. Firstly, the findings can be generalized due to the global nature of the study. Secondly, FINE-REAL enrolls a more heterogeneous patient population than the randomized clinical trials of finerenone, particularly as patients were recruited across nephrology, endocrinology, cardiology, and primary care settings. Thirdly, the study provides insights into clinical practice following the approval of finerenone. The limitations of this interim analysis of FINE-REAL include the short follow-up time and the observational nature of the study, meaning the findings cannot be used to demonstrate causality. Some analyses could not be reported/performed due to short follow-up time and/or small sample sizes, including longitudinal data on eGFR or UACR and the association of participant characteristics with TEAEs.
In conclusion, finerenone was initiated across various clinical settings and populations with CKD and T2D in routine clinical practice; treatment discontinuation and occurrence of hyperkalemia in this finerenone-prescribed cohort were low, consistent with clinical trial data.
Data availability
Availability of the data underlying this publication will be determined according to Bayer’s commitment to the EFPIA/PhRMA “Principles for responsible clinical trial data sharing”. This pertains to scope, timepoint and process of data access. As such, Bayer commits to sharing upon request from qualified scientific and medical researchers patient-level clinical trial data, study-level clinical trial data, and protocols from clinical trials in patients for medicines and indications approved in the United States (US) and European Union (EU) as necessary for conducting legitimate research. This applies to data on new medicines and indications that have been approved by the EU and US regulatory agencies on or after January 01, 2014. Interested researchers can use www.vivli.org to request access to anonymized patient-level data and supporting documents from clinical studies to conduct further research that can help advance medical science or improve patient care. Information on the Bayer criteria for listing studies and other relevant information is provided in the member section of the portal. Data access will be granted to anonymized patient-level data, protocols and clinical study reports after approval by an independent scientific review panel. Bayer is not involved in the decisions made by the independent review panel. Bayer will take all necessary measures to ensure that patient privacy is safeguarded.
References
IDF. IDF diabetes atlas. 2021. https://diabetesatlas.org/. Accessed 3 May 2022.
Wu B, Bell K, Stanford A, Kern DM, Tunceli O, Vupputuri S et al (2016) Understanding CKD among patients with T2DM: prevalence, temporal trends, and treatment patterns-NHANES 2007–2012. BMJ Open Diabetes Res Care 4(1):e000154. https://doi.org/10.1136/bmjdrc-2015-000154
ISN. ISN global kidney health atlas. 2023. https://www.theisn.org/wp-content/uploads/media/ISN%20Atlas_2023%20Digital_REV_2023_10_03.pdf. Accessed 23 November 2023.
Hong J, Surapaneni A, Daya N, Selvin E, Coresh J, Grams ME et al (2021) Retinopathy and risk of kidney disease in persons with diabetes. Kidney Med 3(5):808-15e1. https://doi.org/10.1016/j.xkme.2021.04.018
Lawson CA, Seidu S, Zaccardi F, McCann G, Kadam UT, Davies MJ et al (2021) Outcome trends in people with heart failure, type 2 diabetes mellitus and chronic kidney disease in the UK over twenty years. EClinicalMedicine 32:100739. https://doi.org/10.1016/j.eclinm.2021.100739
Folkerts K, Kelly AMB, Petruski-Ivleva N, Fried L, Blankenburg M, Gay A et al (2021) Cardiovascular and renal outcomes in patients with Type-2 diabetes and chronic kidney disease identified in a United States administrative claims database: a population cohort study. Nephron 145(4):342–352. https://doi.org/10.1159/000513782
Tanaka Y, Joki N, Hase H (2015) Ischemic heart disease in patients with end-stage kidney disease. Blood Purif 40(4):332–336. https://doi.org/10.1159/000441582
Lau WL, Huisa BN, Fisher M (2017) The cerebrovascular-chronic kidney disease connection: perspectives and mechanisms. Transl Stroke Res 8(1):67–76. https://doi.org/10.1007/s12975-016-0499-x
de Boer IH, Khunti K, Sadusky T, Tuttle KR, Neumiller JJ, Rhee CM et al (2022) Diabetes management in chronic kidney disease: a consensus report by the American diabetes association (ADA) and kidney disease: improving global outcomes (KDIGO). Kidney Int 102(5):974–989
Blonde L, Umpierrez GE, Reddy SS, McGill JB, Berga SL, Bush M et al (2022) American Association of clinical endocrinology clinical practice guideline: developing a diabetes mellitus comprehensive care plan-2022 update. Endocr Pract 28(10):923–1049. https://doi.org/10.1016/j.eprac.2022.08.002
Marx N, Federici M, Schutt K, Muller-Wieland D, Ajjan RA, Antunes MJ et al (2023) 2023 ESC guidelines for the management of cardiovascular disease in patients with diabetes. Eur Heart J 44(39):4043–4140. https://doi.org/10.1093/eurheartj/ehad192
Nuffield Department of Population Health Renal Studies Group, SGLT2 inhibitor Meta-Analysis Cardio-Renal Trialists Consortium (2022) Impact of diabetes on the effects of sodium glucose co-transporter-2 inhibitors on kidney outcomes: collaborative meta-analysis of large placebo-controlled trials. Lancet 400(10365):1788–1801. https://doi.org/10.1016/S0140-6736(22)02074-8
Sattar N, Lee MMY, Kristensen SL, Branch KRH, Del Prato S, Khurmi NS et al (2021) Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of randomised trials. Lancet Diabetes Endocrinol 9(10):653–662. https://doi.org/10.1016/s2213-8587(21)00203-5
Alicic RZ, Rooney MT, Tuttle KR (2017) Diabetic kidney disease: challenges, progress, and possibilities. Clin J Am Soc Nephrol 12(12):2032–2045. https://doi.org/10.2215/CJN.11491116
Bayer HealthCare Pharmaceuticals Inc. KERENDIA (finerenone) tablets, for oral use: US prescribing information. 2021. https://labeling.bayerhealthcare.com/html/products/pi/Kerendia_PI.pdf. Accessed 26 June 2023.
Bayer HealthCare Pharmaceuticals Inc. Kerendia summary of product characteristics. 2022. https://www.ema.europa.eu/en/documents/product-information/kerendia-epar-product-information_en.pdf. Accessed 26 June 2023.
Bakris GL, Agarwal R, Anker SD, Pitt B, Ruilope LM, Rossing P et al (2020) Effect of finerenone on chronic kidney disease outcomes in type 2 diabetes. N Engl J Med 383(23):2219–2229. https://doi.org/10.1056/NEJMoa2025845
Pitt B, Filippatos G, Agarwal R, Anker SD, Bakris GL, Rossing P et al (2021) Cardiovascular events with finerenone in kidney disease and type 2 diabetes. N Engl J Med 385:2252–2263. https://doi.org/10.1056/NEJMoa2110956
Agarwal R, Filippatos G, Pitt B, Anker SD, Rossing P, Joseph A et al (2022) Cardiovascular and kidney outcomes with finerenone in patients with type 2 diabetes and chronic kidney disease: the FIDELITY pooled analysis. Eur Heart J 43(6):474–484. https://doi.org/10.1093/eurheartj/ehab777
Draznin B, Aroda VR, Bakris G, Benson G, Brown FM, Freeman R et al (2022) 11 Chronic kidney disease and risk management: standards of medical care in diabetes-2022. Diabetes Care 45(Supplement_1):S175–S184. https://doi.org/10.2337/dc22-S011
McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M et al (2023) 2023 Focused update of the 2021 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J 44(37):3627–3639. https://doi.org/10.1093/eurheartj/ehad195
Vizcaya D, Kovesdy CP, Reyes A, Pessina E, Pujol P, James G et al (2023) Characteristics of patients with chronic kidney disease and type 2 diabetes initiating finerenone in the USA: a multi-database, cross-sectional study. J Comp Eff Res. https://doi.org/10.57264/cer-2023-0076
Desai NR, Navaneethan SD, Nicholas SB, Pantalone KM, Wanner C, Hamacher S et al (2023) Design and rationale of FINE-REAL: a prospective study of finerenone in clinical practice. J Diabetes Complicat 37(4):108411. https://doi.org/10.1016/j.jdiacomp.2023.108411
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Rossing P, Garweg JG, Anker SD, Osonoi T, Pitt B, Rosas SE et al (2023) Effect of finerenone on the occurrence of vision-threatening complications in patients with non-proliferative diabetic retinopathy: Pooled analysis of two studies using routine ophthalmological examinations from clinical trial participants (ReFineDR/DeFineDR). Diabetes Obes Metab 25(3):894–898. https://doi.org/10.1111/dom.14915
Christofides EA, Desai N (2021) Optimal early diagnosis and monitoring of diabetic kidney disease in type 2 diabetes mellitus: addressing the barriers to albuminuria testing. J Prim Care Community Health 12:21501327211003684. https://doi.org/10.1177/21501327211003683
Shlipak MG, Tummalapalli SL, Boulware LE, Grams ME, Ix JH, Jha V et al (2021) The case for early identification and intervention of chronic kidney disease: conclusions from a kidney disease: improving global outcomes (KDIGO) controversies conference. Kidney Int 99(1):34–47. https://doi.org/10.1016/j.kint.2020.10.012
Pantalone KM, Ji X, Kong SX, Elliott JC, Milinovich A, Misra-Hebert AD et al (2023) Unmet needs and opportunities for optimal management of patients with type 2 diabetes and chronic kidney disease. J Diabetes Complicat 37(4):108418. https://doi.org/10.1016/j.jdiacomp.2023.108418
Yu B, Dong C, Hu Z, Liu B (2021) Effects of sodium-glucose co-transporter 2 (SGLT2) inhibitors on renal outcomes in patients with type 2 diabetes mellitus and chronic kidney disease: a protocol for systematic review and meta-analysis. Medicine (Baltimore) 100(8):e24655. https://doi.org/10.1097/md.0000000000024655
Shaman AM, Bain SC, Bakris GL, Buse JB, Idorn T, Mahaffey KW et al (2022) Effect of the glucagon-like peptide-1 receptor agonists semaglutide and liraglutide on kidney outcomes in patients with Type 2 diabetes: pooled analysis of SUSTAIN 6 and LEADER. Circulation 145(8):575–585. https://doi.org/10.1161/circulationaha.121.055459
Acknowledgments
The authors would like to thank the participants, their families, and all investigators involved in this study. The authors would like to acknowledge Marcel Schulz, PhD, of Bayer AG, Berlin, Germany, for his support with the study design and setup. Medical writing support was provided by Charlotte Simpson, PhD, and Rachel Wright, PhD, and editorial support, including formatting, proofreading, and submission, was provided by Melissa Ward, BA, all of Orion (a division of Prime), London, UK, supported by Bayer according to Good Publication Practice guidelines (https://www.acpjournals.org/doi/https://doi.org/10.7326/M22-1460).
Funding
The FINE-REAL study is sponsored by Bayer AG, Berlin, Germany.
Author information
Authors and Affiliations
Contributions
All authors substantially contributed to the conception, design, or planning of the study. All authors substantially contributed to critically reviewing or revising the manuscript for important intellectual content.
Corresponding author
Ethics declarations
Conflict of interest
This study is sponsored by Bayer AG. The authors wrote the article with the assistance of a medical writer funded by the sponsor. The sponsor was involved in the study design and the writing of the report. Susanne B. Nicholas is supported by NIH research grants R01MD014712, RF00250-2022-0038, U2CDK129496, P50MD017366, and CDC project number 75D301-21-P-12254; received research support from Bayer AG for the submitted work, as well as research support from Goldfinch Bio, Travere, and Terasaki Institute of Biomedical Innovation; and personal fees and other support from AstraZeneca, Bayer AG, Gilead, Novo Nordisk, and Boehringer Ingelheim/Lilly. Ricardo Correa-Rotter has received consulting and/or speaker and/or advisory board fees and/or research support from AbbVie, AstraZeneca, Bayer, Boehringer Ingelheim, Chinook, Novo Nordisk and Roche. Nihar Desai works under contract with the Centers for Medicare and Medicaid Services to develop and maintain performance measures used for public reporting and pay for performance programs. He reports research grants and consulting for Amgen, AstraZeneca, Bayer, Boehringer Ingelheim, Bristol Myers Squibb, Cytokinetics, Merck, Novartis, SCPharmaceuticals, and Vifor. Lixin Guo has nothing to disclose. Sankar D. Navaneethan reports receipt of personal fees from AstraZeneca (Data and Safety Monitoring Board), ACI clinical (Clinical Event Committee), Bayer, Boehringer Ingelheim/Lilly, GSK, Intercept, Vifor, and Vertex; and grants from Keryx outside the submitted work. Kevin M. Pantalone discloses speaker bureau fees from AstraZeneca, Corcept Therapeutics, Merck, and Novo Nordisk; consulting fees from AstraZeneca, Bayer, Corcept Therapeutics, Diasome, Eli Lilly, Novo Nordisk, Merck, Sanofi, and Twinhealth; and research support from Bayer, Novo Nordisk, Merck, and Twinhealth. Christoph Wanner reports steering committee and advisory board participation as well as lecturing honoraria from AstraZeneca, Bayer, Boehringer Ingelheim, Eli Lilly, FMC, Gilead, GSK, MSD, Sanofi, and Vifor. Stefanie Hamacher was an employee of ClinStat GmbH at the time of the study and reports consulting or advisory roles of her former CRO with Bayer AG. Samuel Fatoba is an employee of Bayer U.S. LLC, Pharmaceuticals. Andrea Horvat-Broecker is an employee of Bayer AG, Germany. Antonio Garreta-Rufas is an employee of Bayer AG, Germany. Alain Gay was an employee of Bayer AG, Germany at the time the interim analysis was performed. Martin Merz is an employee of Bayer AG, Germany. David C. Wheeler has received honoraria from Astellas, AstraZeneca (ongoing consultancy agreement), Amgen, Bayer, Boehringer Ingelheim, GSK, Gilead, Janssen, Mundipharma, Merck Sharp and Dohme, Tricida, Vifor, and Zydus.
Ethical approval
Documented approval from appropriate independent ethics committees/institutional review boards was obtained for all participating centers in applicable countries prior to study start. The study is being conducted within an approved drug indication in accordance with guidelines and regulations of the European Medicines Agency, the U.S. Food and Drug Administration [15, 16], and applicable local laws and regulations.
Human and animal rights
Documented approval from appropriate independent ethics committees/institutional review boards was obtained for all participating centers in applicable countries prior to study start. The study is being conducted within an approved drug indication in accordance with guidelines and regulations of the European Medicines Agency, the U.S. Food and Drug Administration, and applicable local laws and regulations. All participants provided written informed consent. This article does not contain any studies with animals performed by any of the authors.
Informed consent to participate
All participants provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nicholas, S.B., Correa-Rotter, R., Desai, N.R. et al. First interim results from FINE-REAL: a prospective, non-interventional, phase 4 study providing insights into the use and safety of finerenone in a routine clinical setting. J Nephrol (2024). https://doi.org/10.1007/s40620-024-02070-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40620-024-02070-y