Abstract
Purpose
The effect of combined lifestyle interventions (LSI) including dietary and physical activity on metabolic health, energy metabolism and VO2max in diabetic patients has provided mixed results. We evaluated the impact of 1-year caloric restriction (CR), and 12-week supervised structured exercise training (SSET) on metabolic health, RMR and VO2max in obese adults with type 2 diabetes.
Methods
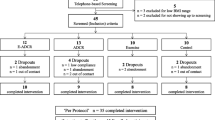
After 1-month education for LSI, 33 participants had anthropometric, biochemical and metabolic assessments. They then started CR based on RMR, and 3-month SSET during the months 1–3 (Early-SSET) or 4–6 (Late-SSET). Reassessments were planned after 3, 6 and 12 months. Using a per-protocol analysis, we evaluated parameter changes from baseline and their associations for the 23 participants (11 Early-SSET, 12 Late-SSET) who completed the study. RMR was adjusted (adjRMR) for age, sex, fat-free mass (FFM) and fat mass (FM).
Results
Compared with baseline, after 6 months we found significant increases in VO2max (+ 14%) and HDL-cholesterol (+ 13%), and reduction in body mass index (− 3%), FM (− 8%) and glycated hemoglobin (HbA1c, − 7%). Training-related caloric expenditure negatively correlated with changes in body weight (p < 0.001), FM (p < 0.001) and HbA1c (p = 0.006). These results were confirmed at the 12-month follow-up. Pooling together all follow-up data, adjRMR changes correlated with changes in glycemia (r = 0.29, p = 0.02), total-cholesterol (r = 0.29, p = 0.02) and VO2max (r = − 0.26,p = 0.02). No significant differences emerged between the Early- and Late-SSET groups.
Conclusions
Combined intervention with SSET and CR improved metabolic control. Changes in metabolic health and fitness correlated with changes of adjRMR, which was reduced improving fitness, glycemia and cholesterolemia.
Clinical trial registry
Trial registration number: NCT03785379. URL of registration: http://clinicaltrials.gov.


Similar content being viewed by others
References
Tobias DK, Pan A, Jackson CL, O’Reilly EJ, Ding EL, Willett WC, Manson JE, Hu FB (2014) Body-mass index and mortality among adults with incident type 2 diabetes. N Engl J Med. 370:233–244. https://doi.org/10.1056/NEJMoa1304501
American Diabetes Association (2017) Standards of medical care in diabetes-2017: summary of revisions. Diabetes Care 40:S4–S5
Yu AP, Wu EQ, Birnbaum HG, Emani S, Fay M, Pohl G, Wintle M, Yang E, Oglesby A (2007) Short-term economic impact of body weight change among patients with type 2 diabetes treated with antidiabetic agents: analysis using claims, laboratory, and medical record data. Curr Med Res Opin 23:2157–2169. https://doi.org/10.1185/0300799007X219544
Lau DCW, Teoh H (2013) Benefits of modest weight loss on the management of type 2 diabetes mellitus. Can J diabetes. 37:128–134 (Pii/S1499267113001895)
Church TS, Blair SN, Cocreham S, Johannsen N, Johnson W, Kramer K, Mikus CR, Myers V, Nauta M, Rodarte RQ et al (2010) Effects of aerobic and resistance training on hemoglobin A1c levels in patients with type 2 diabetes: a randomized controlled trial. JAMA. 304:2253–2262. https://doi.org/10.1001/jama.2010.1710
Zheng J, Wang H, Ren M (2017) Influence of exercise intervention on gestational diabetes mellitus: a systematic review and meta-analysis. J Endocrinol Invest 40:1027–1033
Daousi C, Casson IF, Gill GV, MacFarlane IA, Wilding JPH, Pinkney JH (2006) Prevalence of obesity in type 2 diabetes in secondary care: association with cardiovascular risk factors. Postgrad Med J. 82:280–284. https://doi.org/10.1136/pmj.2005.039032
Ross SA, Dzida G, Vora J, Khunti K, Kaiser M, Ligthelm RJ (2011) Impact of weight gain on outcomes in type 2 diabetes. Curr Med Res Opin. 27:1431–1438. https://doi.org/10.1185/03007995.2011.585396
ADVANCE Collaborative Group, Patel A, MacMahon S, Chalmers J, Neal B, Billot L, Woodward M, Marre M, Cooper M, Glasziou P et al (2008) Intensive Blood Glucose Control and Vascular Outcomes in Patients with Type 2 Diabetes. N Engl J Med. 358:2560–2572
Wolf AM, Conaway MR, Crowther JQ, Hazen KY, Nadler JL, Oneida B, Bovbjerg VE, Improving Control with Activity and Nutrition (ICAN) Study (2004) Translating lifestyle intervention to practice in obese patients with type 2 diabetes: improving Control with Activity and Nutrition (ICAN) study. Diabetes Care. 27:1570–1576
Brehm BJ, Lattin BL, Summer SS, Boback JA, Gilchrist GM, Jandacek RJ, D’Alessio DA (2009) One-year comparison of a high-monounsaturated fat diet with a high-carbohydrate diet in type 2 diabetes. Diabetes Care. 32:215–220. https://doi.org/10.2337/dc08-0687
Look AHEAD Research Group, Wing RR, Bolin P, Brancati FL, Bray GA, Clark JM, Coday M, Crow RS, Curtis JM, Egan CM et al (2013) Cardiovascular Effects of Intensive Lifestyle Intervention in Type 2 Diabetes. N Engl J Med. 369:145–154
Look AHEAD Research Group, Pi-Sunyer X, Blackburn G, Brancati FL, Bray GA, Bright R, Clark JM, Curtis JM, Espeland MA, Foreyt JP et al (2007) Reduction in weight and cardiovascular disease risk factors in individuals with type 2 diabetes: one-year results of the look AHEAD trial. Diabetes Care 30:1374–1383. https://doi.org/10.2337/dc07-0048
Estruch R, Ros E, Salas-Salvadó J, Covas M-I, Corella D, Arós F, Gómez-Gracia E, Ruiz-Gutiérrez V, Fiol M, Lapetra J et al (2013) Primary prevention of cardiovascular disease with a mediterranean diet. N Engl J Med. 368:1279–1290
Haddad E, Wells GA, Sigal RJ, Boulé NG, Kenny GP (2003) Meta-analysis of the effect of structured exercise training on cardiorespiratory fitness in type 2 diabetes mellitus. Diabetologia 46:1071–1081
Galgani J, Ravussin E (2008) Energy metabolism, fuel selection and body weight regulation. Int J Obes (Lond) 32(Suppl 7):S109–S119
Ravussin E, Lillioja S, Knowler WC, Christin L, Freymond D, Abbott WG, Boyce V, Howard BV, Bogardus C (1988) Reduced rate of energy expenditure as a risk factor for body-weight gain. N Engl J Med. 318:467–472. https://doi.org/10.1056/NEJM198802253180802
Piaggi P, Thearle MS, Bogardus C, Krakoff J (2013) Lower energy expenditure predicts long-term increases in weight and fat mass. J Clin Endocrinol Metab. 98:E703–E707. https://doi.org/10.1210/jc.2012-3529
Reynolds CM, Gray C, Li M, Segovia SA, Vickers MH. Early life nutrition and energy balance disorders in offspring in later life. Nutrients. 2015;7:8090–8111. http://www.mdpi.com/2072-6643/7/9/5384/. Accessed 31 Jul 2017
Alawad AO, Merghani TH, Ballal MA (2013) Resting metabolic rate in obese diabetic and obese non-diabetic subjects and its relation to glycaemic control. BMC Res Notes 6:382
Stevenson RW, Parsons JA, Alberti KG (1983) Effect of intraportal and peripheral insulin on glucose turnover and recycling in diabetic dogs. Am J Physiol 244:E190–E195
Zawadzki JK, Wolfe RR, Mott DM, Lillioja S, Howard BV, Bogardus C (1988) Increased rate of Cori cycle in obese subjects with NIDDM and effect of weight reduction. Diabetes 37:154–159
Piaggi P, Thearle MS, Bogardus C, Krakoff J (2015) Fasting hyperglycemia predicts lower rates of weight gain by increased energy expenditure and fat oxidation rate. J Clin Endocrinol Metab 100:1078–1087. https://doi.org/10.1210/jc.2014-3582
Araiza P, Hewes H, Gashetewa C, Vella CA, Burge MR (2006) Efficacy of a pedometer-based physical activity program on parameters of diabetes control in type 2 diabetes mellitus. Metabolism 55:1382–1387
Jennings AE, Alberga A, Sigal RJ, Jay O, Boulé NG, Kenny GP (2009) The effect of exercise training on resting metabolic rate in type 2 diabetes mellitus. Med Sci Sport Exerc. 41:1558–1565
Mourier A, Gautier JF, De Kerviler E, Bigard AX, Villette JM, Garnier JP, Duvallet A, Guezennec CY, Cathelineau G (1997) Mobilization of visceral adipose tissue related to the improvement in insulin sensitivity in response to physical training in NIDDM. Effects of branched-chain amino acid supplements. Diabetes Care 20:385–391
Karstoft K, Brinkløv CF, Thorsen IK, Nielsen JS, Ried-Larsen M (2017) Resting metabolic rate does not change in response to different types of training in subjects with type 2 diabetes. Front Endocrinol (Lausanne) 8:132
Mikus CR, Oberlin DJ, Libla J, Boyle LJ, Thyfault JP (2012) Glycaemic control is improved by 7 days of aerobic exercise training in patients with type 2 diabetes. Diabetologia 55:1417–1423. https://doi.org/10.1007/s00125-012-2490-8
Sergi G, Coin A, Sarti S, Perissinotto E, Peloso M, Mulone S, Trolese M, Inelmen EM, Enzi G, Manzato E (2010) Resting VO2, maximal VO2 and metabolic equivalents in free-living healthy elderly women. Clin Nutr. Elsevier 29:84–88
Zurlo F, Larson K, Bogardus C, Ravussin E (1990) Skeletal muscle metabolism is a major determinant of resting energy expenditure. J Clin Invest. 86:1423–1427
Galgani JE, Santos JL (2016) Insights about weight loss-induced metabolic adaptation. Obesity (Silver Spring) 24:277–278. https://doi.org/10.1002/oby.21408
Janicki J, Weber K (1986) Equipment to protocols to evaluate the s-exercise response. In: Weber K, Janicki J (eds) Cardiopulmonary s-exercise testing. WB Saunders, Philadelphia, pp 138–150
Colberg SR, Sigal RJ, Fernhall B, Regensteiner JG, Blissmer BJ, Rubin RR, Chasan-Taber L, Albright AL, Braun B, American College of Sports Medicine et al (2010) Exercise and type 2 diabetes: the American College of Sports Medicine and the American Diabetes Association: joint position statement. Diabetes Care 33:e147–e167
American Diabetes Association (2017) 7. Obesity management for the treatment of type 2 diabetes. Diabetes Care 40:S57–S63
Bacchi E, Negri C, Zanolin ME, Milanese C, Faccioli N, Trombetta M, Zoppini G, Cevese A, Bonadonna RC, Schena F et al (2012) Metabolic effects of aerobic training and resistance training in type 2 diabetic subjects: a randomized controlled trial (the RAED2 study). Diabetes Care 35:676–682
Fothergill E, Guo J, Howard L, Kerns JC, Knuth ND, Brychta R, Chen KY, Skarulis MC, Walter M, Walter PJ et al (2016) Persistent metabolic adaptation 6 years after “The Biggest Loser” competition. Obesity 24:1612–1619. https://doi.org/10.1002/oby.21538
Bartelt A, John C, Schaltenberg N, Berbée JFP, Worthmann A, Cherradi ML, Schlein C, Piepenburg J, Boon MR, Rinninger F et al (2017) Thermogenic adipocytes promote HDL turnover and reverse cholesterol transport. Nat Commun 8:15010. https://doi.org/10.1038/ncomms15010
Borsheim E, Bahr R (2003) Effect of exercise intensity, duration and mode on post-exercise oxygen consumption. Sport Med 33:1037–1060. https://doi.org/10.2165/00007256-200333140-00002
Ballor DL, Poehlman ET (1995) A meta-analysis of the effects of exercise and/or dietary restriction on resting metabolic rate. Eur J Appl Physiol Occup Physiol 71:535–542. https://doi.org/10.1007/BF00238557
Donnelly JE, Pronk NP, Jacobsen DJ, Pronk SJ, Jakicic JM (1991) Effects of a very-low-calorie diet and physical-training regimens on body composition and resting metabolic rate in obese females. Am J Clin Nutr 54:56–61
Connolly J, Romano T, Patruno M (1999) Effects of dieting and exercise on resting metabolic rate and implications for weight management. Fam Pract 16:196–201. https://doi.org/10.1093/fampra/16.2.196
Geliebter A, Maher MM, Gerace L, Gutin B, Heymsfield SB, Hashim SA (1997) Effects of strength or aerobic training on body composition, resting metabolic rate, and peak oxygen consumption in obese dieting subjects. Am J Clin Nutr 66:557–563
Svendsen OL, Hassager C, Christiansen C (1993) Effect of an energy-restrictive diet, with or without exercise, on lean tissue mass, resting metabolic rate, cardiovascular risk factors, and bone in overweight postmenopausal women. Am J Med. 95:131–140 (pii/000293439390253L)
Acknowledgments
The authors are indebted to the nursing staff and physicians of the Diabetes Clinic, and to the laboratory staff of the Department of Medicine, Metabolic Unit for their assistance; to Prof. E. Manzato, chief of the Department of Medicine, Geriatrics Division, for the use of the calorimetric and body composition equipment; to Mrs. E. Rampazzo and the staff of Forum Wellness Club; to Mr. P. Servidei for the computer assistance; to Ms. M. Adams for editing the manuscript; and to Prof. Egle Perissinotto for the statistical support. Finally, we are especially grateful to all of the volunteer participants whose commitment made this study possible.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
FZ, AA, ER, and GS contributed to the study concept and design. FZ and CT contributed to the statistical analysis. FZ, CT, MS, CS, NV, SC, II, AS, LP, SdK, and AM, contributed to the data collection. FZ, CT, ER, NV, and GS contributed to the drafting of the manuscript. All authors contributed to the interpretation of the results and approved the final version of the manuscript. FZ is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors disclose no potential conflicts of interest.
Ethical approval
The research conforms to the principles of the Declaration of Helsinki, revised in 2000. The Ethics Committee of the University Hospital of Padua approved the protocol (Prot. n. 2718P).
Informed consent
Written informed consent was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zurlo, F., Trevisan, C., Vitturi, N. et al. One-year caloric restriction and 12-week exercise training intervention in obese adults with type 2 diabetes: emphasis on metabolic control and resting metabolic rate. J Endocrinol Invest 42, 1497–1507 (2019). https://doi.org/10.1007/s40618-019-01090-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-019-01090-x