Abstract
Background
Discriminatory policies, attitudes, and practices have had deleterious impacts on the health of Black, Indigenous, and other racialized groups. The aim of this study was to investigate racism as barrier to access to medicines in Canada. The study investigated the characteristics of structural racism and implicit biases that affect medicines access.
Methods
A scoping review using the STARLITE literature retrieval approach and analysis of census tract data in Toronto, Ontario, Canada, were undertaken. Government documents, peer-reviewed articles from public policy, health, pharmacy, social sciences, and gray literature were reviewed.
Results
Structural racism that created barriers to access to medicines and vaccines was identified in policy, law, resource allocation, and jurisdictional governance. Institutional barriers included health care providers’ implicit biases about racialized groups, immigration status, and language. Pharmacy deserts in racialized communities represented a geographic barrier to access.
Conclusion
Racism corrupts and impedes equitable allocation and access to medicine in Canada. Redefining racism as a form of corruption would obligate societal institutions to investigate and address racism within the context of the law as opposed to normative policy. Public health policy, health systems, and governance reform would remove identified barriers to medicines, vaccines, and pharmaceutical services by racialized groups.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
“Racism is a public health issue,” headlined a report submitted to the chair and members of the Wellington-Dufferin-Guelph Board of Health [1]. Discriminatory policies, attitudes, and practices have negatively impacted the health of Black, Indigenous, and other racialized groups in Canada and globally [2, 3]. Racism is defined as “racist ideologies, prejudiced attitudes, discriminatory behavior, structural arrangements, and institutionalized practices resulting in racial inequality, as well as the fallacious notion that discriminatory relations between groups are morally and scientifically justifiable; it is reflected in discriminatory provisions in legislation or regulations and discriminatory practices, as well as in anti-social beliefs and acts” [The United Nations Declaration on Race and Racial Prejudice (1978)]. The aim of this scoping review was to investigate racism as a barrier to accessing medicines in the Canadian setting. The study investigated the manifestations of structural racism and impact of implicit bias on accessing medicines. “Structural racism is defined as the totality of ways in which societies foster racial discrimination through mutually reinforcing systems” [4]. Study findings reveal racism corrupts and impedes equitable access to medicines.
A scoping review of peer-reviewed and gray literature was undertaken in this study. Scoping reviews are conducted to map the literature to identify characteristics related to a key concept or to clarify a key concept [5]. In this scoping review, the concept of racism as corruption was explored. Corruption is defined as the unethical and/or illegal allocation of resources, opportunities, or the intentional mis-performance or neglect of a recognized duty or entrusted power for private gain [6-8].
Key manifestations of the relationship between racism, corruption, and access to medicines, as described in the literature, were investigated. The primary focus of the scoping review was Ontario, Canada’s most populous province. The a priori assumption was that a greater volume of literature would be found written about Ontario than other provinces, which was borne out by the literature retrieved by the search of databases. No assumptions were made regarding the prevalence of racism in accessing medicines in Ontario as compared to other provinces. The scoping review also examined the extra-provincial Canada-Indigenous relationship with respect to access to medicines. Findings from this scoping review will inform future studies on racism and access to medicine across Canada.
Pharmacogovernance and Access to Medicines
Pharmacogovernance is defined as the manner in which governing structures, policy instruments, and institutional authority are managed to promote societal interests for access to medicines and safety due to medication use [9, 10]. In 1978, the Alma-Ata Declaration stated that health was a fundamental human right, and although not explicitly stated at Alma-Ata, access to pharmaceuticals directly impacts health. Inequity in access to antivirals used to treat HIV/AIDS in low- and middle-income countries was raised in debates about the TRIPS agreement at the 2001 DOHA convention. The challenge to World Trade Organization intellectual property rights, led by Brazil, resulted in a recognition that patents should not impede public health. The TRIPS agreement enabled the production of lower-cost generic antivirals by pharmaceutical industries in Brazil and India. Yet, access to common therapies to treat asthma, infections, and more remains elusive for many. The 65th World Health Assembly called for the WHO to focus on increasing affordability of medicines and “strengthening health system that includes national medical policies” [11]. This scoping review reveals that access to medicines is not limited to low- and middle-income countries. Structural, institutional, and interpersonal aspects of racism are identified as barriers to access in high-income countries, such as Canada.
How national, state/provincial, and municipal governments establish priorities, make policy, and allocate resources is shaped by governance. The Canada Health Act states that the primary objective of Canadian health care policy is to protect, promote, and restore the physical and mental well-being of residents of Canada and to facilitate reasonable access to health services without financial or other barriers [12]. The performance of federal, provincial, and territorial governments and healthcare institutions in meeting their obligation to equitable access to pharmaceuticals has not been adequately measured in Canada. The Anti-Racism Act (2017) created a legal mechanism to assure collection of data to identify and monitor racial disparities. however, norms have discouraged the collection of demographic data about racial identity.
International Covenants and Access to Medicines
International covenants signed by Canada provide the groundwork for abolishing structural racism thereby assuring the right to equitable access to medicines. The International Covenant on Economic, Social, and Cultural Rights (ICESCR) broadly addresses the Right to Health and the Right to Benefit from Scientific Progress. The covenant states that signatories have “a duty to the equitable distribution of scientific advances, especially for vulnerable and marginalized populations,” thereby abiding by their duty to “ensure a nondiscriminatory approach to access.” Access to essential medicines is codified in the International Covenant on Civil and Political Rights (ICCPR, Article 6), Right to Life. United Nations declarations that are relevant to racism and access to medicines are the 2006 UN Declaration on the Rights of Indigenous Peoples, Article 24(2), that stated Indigenous individuals have an equal right to the enjoyment of the highest attainable standard of physical and mental health, and the UN Declaration for the International Decade for People of African Descent 2015–2024, which declared that nation-states should take measures to improve access to quality health services to people of African descent, and the collection of data should be undertaken as a measure of accountability.
Theoretical Framework
The theoretical framework underpinning this research is critical race theory (CRT). CRT explains that racism is structural. “Race” is a social construction rather than biological, and racial categories are social inventions [13]. Critical race scholars posit that settler-colonists “universally demonize their subjects to feel better about exploiting them” [13]. Systemic racism is a social determinant of health and a public health issue because it contributes to health inequities in Canada [1, 14]. The United Nations Declaration on Race and Racial Prejudice (1978) defined racism as “racist ideologies, prejudiced attitudes, discriminatory behavior, structural arrangements, and institutionalized practices resulting in racial inequality, as well as the fallacious notion that discriminatory relations between groups are morally and scientifically justifiable; it is reflected in discriminatory provisions in legislation or regulations and discriminatory practices, as well as in anti-social beliefs and acts.”
In this study, the a priori assumption is that racism is normative in Canada. Members of racialized groups may be further marginalized by additional self-identities such as women, immigrants, 2SLGBTQ + , or disabled. Healthcare providers’ implicit biases about racial and ethnic groups create barriers to treatment [15, 16] and affect assessment, diagnoses, treatment recommendations, and prescribing of medicines [3, 15, 17]. CRT has not previously been employed to explain inequities in medicines and pharmacy services.
Research Aims
The aim of this study was to investigate racism as barrier to access to medicines in Canada, including identifying (1) the manifestations of racism in accessing to medicines; (2) impacts of structural racism on access to medicines, including resource allocation; (3) how institutional and provider bias is manifested and affects access to medicines.
Methods
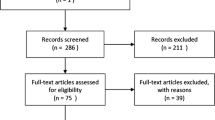
The STARLITE approach was used in the literature retrieval process (Table 1). The sampling strategy included articles from public policy, health, pharmacy, social sciences, government documents, and provincial formularies. Peer-reviewed and non-peer-reviewed policy papers, dissertations, and qualitative studies were screened. Academic One File, Canadian Electronic Library, Canadian Periodicals Index Quarterly, Indigenous Studies Portal, Scholars Portal, Canadian Public Documents Collection, Directory of Open Access Journals, Google Scholar, JSTOR, Project MUSE, PubMed, Theses Canada, CBC Digital Archives, Cochrane Database of Systematic Reviews, Conference Board of Canada e-Library, Index to Canadian Legal Literature, LEGISinfo, Journals@OVID, LabourSource, Omni, Ontario Government Documents Collection, Open Dissertations, PLOS, PAIS Index, Policy File Index, Politics Collection, Semantic Scholar, and SSRN databases were screened. A date range between 2010 and 2021 was selected to capture earliest discussions about Pharmacare in Canada and equitable access to medicine. A total of 6237 articles were retrieved. Search terms were: [COVID-19 OR coronavirus OR “SARS-CoV-2” OR “2019-nCoV”] OR [pharmaceutical OR medicine OR medication OR vaccine] AND [“access to medicines” OR “allocation of vaccines” OR procurement OR distribution] AND [government OR governance OR pharmacogovernance OR ministry OR administration OR “federal government” OR “provincial government” OR state] AND [racism OR racist OR race OR marginalized OR racialized] AND [Black OR Indigenous OR Aboriginal OR First Nations OR Métis OR BIPOC OR “people of color”] AND [Ontario OR Toronto]. Articles were retrieved between July 12, 2021, and July 25, 2021. Of the 6237 articles retrieved, a total of 27 articles met the inclusion criteria for the scoping review. Ontario studies describing regulatory governance (policy, law, and legislation) and racism; pharmacogovernance and access to medicines or vaccines; racism and access to medicines or vaccines; equity and access to medicines or vaccines; or GIS studies of pharmacies or COVID-19 vaccination sites and access were included. The Prisma flow chart (Fig. 1) details the number of articles screened, excluded, and included in this study. City of Toronto neighborhoods census tract maps showing population density of racialized communities and Google maps were analyzed to identify the location of City of Toronto neighborhood community pharmacies in relation to the neighborhood demographics.
Results
Study results revealed that racism is barrier to accessing healthcare and medicines. Our analysis showed barriers occurred at structural, organizational, and interpersonal levels (Fig. 2). Primary barriers directly impacted access to medicines whereas secondary barriers impeded access to healthcare services in general, affecting access to prescription medicines.
Structural Barriers
Pharmacogovernance and Access to Medicines
Access to medicines was influenced by governance with respect to policy, regulation, jurisdictional disputes, and resource allocation. The promise of reasonable access to health services, as stated in the Health Act, has been unfulfilled with respect to Black, Indigenous, and other racialized groups [3, 15, 18, 19].
The Indian Act
The Indian Act (c. 1876), a legacy of Canada’s settler colonial history, governs healthcare for First Nations Peoples. In Canada, “the Governor in Council may make regulations to (h) provide medical treatment and health services to Indians” [20]. Indigenous health services, including medicines, are provided under the Non-Insured Health Benefits (NIHB) program. Eligibility for NIHB medical and pharmaceutical coverage is limited to status Indians registered under the Indian Act, Inuk recognized by an Inuit land claim organization, and child of an NIHB-eligible individual [21].
Racism is associated with power and privilege of the dominant group over others [13, 22]. Racial inequities are entrenched in the Indian Act. The Final Report to Parliament on the Review of Bill S-3 (December 2020) highlighted that up to 450,000 Indigenous people that had been denied status by exclusionary policies would become eligible for status with passage of the amendment to the Indian Act. Bill S-3 rescinded the policy that removed the Indian status of a woman and denied her children’s status upon marriage to a non-Indigenous person. Up to 57,000 individuals would be able to pass their entitlement onto their dependent children. In 2017, the Government of Canada signed an accord that formerly recognized the Métis Nation and established improvement of health and wellness as a priority area. Whereas Bill S-3 increased access to NIHB coverage to previously ineligible First Nations individuals, NIHB eligibility was not expanded to include Métis people, thereby continuing to limit their access to medicines. Power and privilege imbued by Canada’s settler, colonial history have also impeded access to Indigenous traditional medicines and healing practices. The Truth and Reconciliation Call to Action #22 calls upon those in power “to recognize the value of Aboriginal healing practices and use them in the treatment of Aboriginal patients” under the guidance of Indigenous Elders and healers [23].
Drug Policy
Little has been written about the intersection of anti-Black and anti-Indigenous structural racism, implicit bias, and drug policy (Table 2). Four studies described the disproportionate effect of drug policy, criminalizing drug use, on racialized individuals [24]. Black and Indigenous individuals were more likely than their white counterparts to receive jail time for drug-related crimes [25, 26]. Access to opioid agonist therapy (OAT) and harm reduction services by incarcerated individuals was limited pursuant to many provincial policies. Nova Scotia’s policy limited access to OAT to prisoners receiving therapy prior to incarceration. OAT has been denied to incarcerated individuals or inaccessible upon release [27].
Review of municipal policy in the Greater Toronto Area (GTA) showed that access to harm reduction services and pharmaceutical interventions was affected by bylaws and land use policies restricting the location of methadone clinics and safe drug use sites [2]. The City of Oshawa Zoning By-law 60–94 D. 4.24.1 explicitly states that “Notwithstanding any provision of this By-law to the contrary, the use of land, buildings, or structures on all lands set out in Schedule “E,” save and except for 32 Simcoe Street South, for the purposes of a methadone clinic is prohibited” [28]. Municipal bylaws limit access to methadone maintenance therapy to a narrow corridor within Oshawa.
Resource Allocation
Structural racism coupled with provider bias contributed to disparate allocation of resources, health services, and access to medications for racialized individuals. In one study, GTA community health center leaders reported that disparities in the allocation of resources for COVID-19 vaccination and testing “points to systemic discrimination, neglect, and a lack of prioritization of racialized communities, which are in need the most” [17, 29]. Despite calls to consider racism as a criterion to achieve an equitable allocation of COVID-19 vaccines [30], racialized communities have yet to be prioritized [29]. Two studies showed that public expenditures for opioid addiction treatment were influenced by racialized framing of opioid users and criminalization of opioid possession [25, 26].
Jurisdictional Issues
Decentralized governance has created provincial variation in medication access [3, 18]. Moreover, First Nations peoples have been caught in jurisdictional disputes between federal and provincial governments stemming from the Indian Act. One study reported that Federal Non-insured Health Benefits “repeatedly asserted their intention to assume the role of ‘payer of last resort” [3]. Jurisdictional barriers have impeded Indigenous access to provincial/territorial subsidies to cover the cost of medications that non-Indigenous individuals might be eligible for.
In response to findings by the Canadian Human Rights Tribunal (2016) that the Government of Canada’s approach to services for First Nations children was discriminatory, Jordan’s Principle was passed in 2020 and upheld in 2021. The passage of Jordan’s Principle aimed to end jurisdictional infighting over claims for reimbursement [18]. Jordan’s Principle was named after a Cree child that had complex special needs and died in hospital while the federal government and Manitoba provincial government fought over who should be responsible for paying for in-home care. Jordan’s Principle mandates the Government of Canada “to provide First Nations children on-reserve or off-reserve, and Indigenous children ordinarily living on reserve with publicly funded benefits, supports, programs, goods, and services in a manner and according to a standard that meets their particular needs… on a substantially equal basis with non-First Nations children.” Medical supplies not covered by NIHB or difficult to access, such as insulin pumps, may be considered for funding by Jordan’s Principle [14].
Geographic Dimensions of Access to Medicines and Racism
Access to prescription and non-prescription medicines is directly related to access to a pharmacy and pharmacy services such as COVID-19 vaccination and other immunizations. Medication monitoring services for chronic diseases such as diabetes and hypertension by pharmacists can affect access to medication refills or initiation of new therapies. Few studies in Canada have investigated the relationship between geographic access to pharmacies and access to medicines, despite pharmaceutical care being an essential health service that is principally accessed through community pharmacies [31,32,33].
Geographic accessibility is defined as the “relative ease with which individuals from one location can reach other specified zones or point locations, and can be measured by geographical models” [34]. Geographic models measure distance and time to reach a specified location or service in determining accessibility. Although one study of community pharmacy locations found that nearly three-quarters of urban residents (73.3%) live within 5 km of a pharmacy [31], the census data used in the study lacked demographic data (race, income, etc.), thus neighborhood characteristics as a determinant of pharmacy access in Ontario was not undertaken. In this study, the City of Toronto neighborhoods census tract maps, showing the population density of racialized communities, were overlaid on Google Maps, identifying the location of City of Toronto neighborhood community pharmacies. Five Toronto neighborhoods with low-density visible minorities (16.8–22.9%) were compared with five neighborhoods with high-density visible minorities (51.8–96.2%). Our analysis of the census tract maps and Google Maps pharmacies in the corresponding locations reveals that the number of pharmacies per population in low-density visible minority neighborhoods was higher than in high-density visible minority areas (Table 3). The low-density visible minority neighborhoods studied were Mount Pleasant E, Forest Hills S, Lawrence Park S, Rosedale-Moore Park, and Yonge-St. Clair. In the low-density visible minority neighborhoods studied, the ratio of community pharmacies per population ranged between 1:1783 and 1:2612. In the neighborhood of Forest Hills S, visible minorities accounted for 16.8% of the population, and the ratio of pharmacies per population was 1:1783. The Lawrence Park S neighborhood was an outlier with a ratio of 1: 3040. The ratio of community pharmacies per population in the high-density visible minority neighborhoods studied ranged between 1:2355 and 0 per 25,700. The high-density visible minority neighborhoods studied were Malvern East, Malvern West, Mount Olive-Silverstone-Jamestown, Rexdale-Kipling, and Morningside Heights.
Racialized groups, low-income families with young children, newcomers, and older immigrant women often live where housing is affordable, yet transportation is inadequate [32, 33]. Although driving time has been studied as a measure of geospatial access, a more realistic measure for individuals reliant on public transportation is the number of subway/bus stops, number of fare zones, and distance to walk from home or to the pharmacy from the bus/subway stop. Inadequate transportation to get to the clinic or healthcare provider was cited as a barrier to accessing childhood vaccinations in surveys conducted by an Ontario Health unit and Simcoe Muskoka District Health [35]. British Columbia provincial health officer Dr. Bonnie Henry cautioned against conflating low levels of vaccination with anti-vaccination beliefs; recognizing that “issues were often around access” [35]. Policies requiring prescriptions for OAT or methadone to be filled at a specific pharmacy also pose geospatial barriers if access to transportation is inadequate.
Financial Barriers
Out-of-pocket expenditures for medicines, vaccines, and health services were cited as a barrier to access by low-income [15, 36], unemployed, underemployed, or precariously employed [15], immigrants [37], or Indigenous people [3] in several studies. The Parliamentary Budget Office reported that in 2016, 21% of prescriptions were paid for out of pocket [38]. Nearly 8% of Canadians failed to fill prescriptions because they could not afford the cost, they did not have insurance coverage, or had inadequate coverage [38]. Racialized workers in Ontario were found to have lower prescription drug coverage in a study of racism in Toronto’s healthcare system [15]. They were also more likely to be precariously employed or underemployed [1]. Uninsured and undocumented residents faced greater financial barriers accessing prescription drugs than other Canadians [15, 39]. A 2013 report of the medically uninsured in Toronto found that lack of health insurance was a factor in children not receiving vaccinations [39]. One study found a positive correlation between employment status, income, and HIV vaccine acceptability, important given the lifetime cost of HIV therapy can exceed $400,000 [36]. Out-of-pocket costs, stigma, and discrimination were concerns reported by Black Canadian and African American women in the same study. Ontario First Nations adults faced barriers to accessing medications that were not covered by NIHB and Métis people are ineligible for non-insured health benefits [3, 40].
Institutional Barriers
An institutional barrier is defined as an impediment to accessing medicines resulting from institutional policy, practices, or healthcare provider biases. Institutional barriers identified in this scoping review included: racism [3, 14, 17], language [41], immigration status [37, 42], and care without consideration for cultural practices [17, 19] (Fig. 3).
Four studies described examples of Black and Indigenous patients that reported racism in healthcare settings as a deterrent to accessing medicines and needed care because the healthcare settings were alienating and unwelcoming [3, 14, 17, 19]. Monchalin (2020) quoted a nurse and a midwife who reported their healthcare environment was not accepting of Indigenous people after overhearing racist comments from healthcare workers. In a 2013 study of racialization and health inequities in Toronto, Black, South/West Asian, Arab, and East/Southeast Asian women reported difficulty scheduling routine healthcare appointments. South/West Asian, Arab men and women, and east/southeast Asian women reported barriers to accessing their doctors for emergent health problems [17]. Delays in accessing care delayed access to medication.
Immigration Status
A literature review of immigrant patients’ experiences in accessing primary healthcare in Canada identified two studies highlighting racism as a barrier [37, 42]. Immigrant clients reported that they encountered racism in accessing healthcare services, and African immigrants reported more negative experiences than other immigrants [37].
Linguistic Barriers
A study of the Malton neighborhood of Mississauga found that French and English primary language speakers had higher access to primary care than individuals whose primary language was Arabic or Urdu [41]. Linguistic barriers to primary care can affect access to prescribed medicines. Addressing barriers to entry of foreign-trained pharmacists and doctors in Canada would mitigate linguistic barriers.
Interpersonal Barriers: Provider Bias
“Othering” is based on a belief that the dominant culture is superior and all others should be excluded from the circle of belonging. This study found that “othered” groups included Black, Indigenous, racialized peoples, racialized newcomers, and the incarcerated. Implicit bias was central to othering. Implicit bias is defined as “a system of beliefs or stereotypes that influence our attitudes, behaviors, and decisions unconsciously” [3]. Provider bias, whether conscious or unconscious, can result in misinterpretation of symptoms, inappropriate prescribing, and denial of medication [3]. In one study a healthcare worker reported that they had to advocate on behalf of Indigenous patients to receive pain medications because “physicians or the medical staff seem reluctant to give it to them” [16]. Stereotypes that Indigenous people have an alcohol or substance use problem persist despite statistics to the contrary [2, 3, 16]. One study cited a case in which a patient was sent away in tears because doctors were reluctant to prescribe pain medication stronger than Advil because she was Métis [19].
Implicit bias is rooted in racism and encoded in theories of biological essentialism, upon which pharmacogenetic research, drug development, and marketing of “race”-based medications are grounded [43]. Biogenetic fallacies, such as Black people have less sensitive nerve endings and thus greater pain tolerance than White people, have thicker skin (25%), denser bones (29%), and are less likely to contract spinal cord disease (57%), were found to be prevalent amongst medical residents surveyed in 2021 [15, 44] deleteriously impacting patient health [19, 43].
Navigating Racism in the Healthcare System
Trust is essential to the doctor-patient relationship. Patients are more willing to talk about health problems, leading to better diagnoses, more appropriate prescribing, and access to more effective medical treatments and pharmaceuticals. Lived experience of racism and discrimination has created mistrust, whereby some Black, Indigenous, and other racialized individuals avoid seeking care [3, 14, 16]. Three studies reported that mistrust was the reason for reduced utilization of health services, including screening for infectious diseases and managing chronic disease [3, 14, 36]. Two studies found that Regional Health Authority services were underutilized by Indigenous patients that reported interactions with healthcare providers triggered trauma of their residential school experience [3, 14]. The Inner-City Health Strategy Working Group study of racialization and health inequity found that patients who reported feeling anxiety and stress prior to doctor visits delayed seeking care [22]. One study cited examples of Métis women who chose to not self-disclose their Métis identity to avoid stigmatization and provider bias [19]. This practice was described by study participants as a mechanism to navigate mainstream health and social services without a fear that they may be treated in a racist manner or receive a lower standard of care [19]. More research is needed to understand this response to racism and its potential effects on mental and emotional health.
Discussion
This paper establishes that “promises” were made to achieve the right to quality health care and wellbeing for all, as affirmed in the Alma Ata Declaration. Healthcare policy and legislation, including the Canada Health Act, the Anti-Racism Act, the International Covenant on Economic, Social and Cultural Rights (ICESCR), the International Covenant on Economic, Social, and Cultural Rights (ICCPR), the UN Declaration on the Rights of Indigenous Peoples, and the UN Declaration for the International Decade for People of African Descent, establish a framework by which the promise and right to quality healthcare and wellbeing might be achieved. The study also shows that racism corrupts and has broken promises of equitable access to medicines. The concept of racism as corruption was clarified in this scoping review and revealed to act as an impediment to the right to health when medicines are needed.
Racism as Corruption
One of the earliest definitions of corruption comes from Samuel Johnson’s Dictionary of the English Language, Vol. 1 Johnson (1756), in which corruption is defined as: “Wickedness; a perversion of principles; loss of integrity” [8]. Corruption was later defined as “the intentional mis-performance or neglect of a recognized duty, or the unwarranted excise of power, with the motive of gaining some advantage” [8]. Transparency International (2020) defines corruption as “the abuse of entrusted power for private gain.” Corruption is defined in the urban dictionary as “the unethical and/or illegal allocation of resources and/or opportunities” [6].
Based on the above definitions of corruption, this paper uniquely proposes racism as a form of corruption. Racism is the abusive exercise of power privilege of a dominant racial group over other racial groups [13, 22]. Critical Race Theory asserts that “racism is a means by which society allocates privilege and status” [13]. In Canada, the state is entrusted with the power to deliver on healthcare for all, yet structural racism in the public and private health sectors has led to inequitable access to medicines for many racialized individuals [3, 15, 19]. The literature revealed structural racism was codified in pharmaceutical policies and regulations that determined eligibility for and funding of pharmaceuticals [15]. Provincial and federal governments use their “entrusted power for private gain” by shifting financial responsibility for payment of pharmacy and medical services rendered to Indigenous peoples. In doing so, governments achieve economic gain. As such, structural racism is a form of corruption. The study reveals structural racism as also impacting access to community pharmacies. The data showed an inverse relationship between population density in racialized communities (high-density visible minorities) and the number of pharmacies. More research is needed to investigate the rationale for the dearth of community pharmacies in neighborhoods with a high density of racialized groups. Possible reasons range from implicit biases of pharmacy owners to structural racism of lending institutions that refuse to finance businesses in racialized neighborhoods.
The primary institutional barrier to access described in the literature was implicit bias. Implicit biases are situated within a system of ideas that interprets and defines the underpinnings of racial differences, real or imagined, within the context of cultural values. Critical Race Theory asserts that societal allocation of privilege is linked to ideology that ranks racialized differences as “better or worse, superior or inferior, desirable or undesirable” [45]. Ideological, relational, and structural aspects of racism describe this abuse of power privilege that collectively contributes to the loss of integrity in the public and private health sectors and lead racialized individuals to adopt strategies for navigating racism in the healthcare system that exacerbate inequitable access to medicines for many.
Provider bias influenced prescribing decisions. Failure to prescribe specific medications such as opioids was found to relate to false stereotypes and biogenetic fallacies. The ascribing of cultural characteristics to health outcomes is rooted in racism [43]. Yet race, ethnicity, and culture have been intertwined in health lexicon as codes for biologic characteristics. Pathologizing racialized individuals is reinforced in health professional program curricula, thereby reinforcing implicit biases rather that shifting the narrative to focus on health inequities resulting from structural racism. The scoping review identified studies describing the effects of implicit biases on eroding trust in the healthcare system by racialized individuals that was manifested in their choices to not seek healthcare or not to disclose their racialized identity. Findings from this scoping review will inform further studies on racism and access to medicines.
Policy Recommendations
The Canadian healthcare system is touted as a model of public, universal, and comprehensive care in international comparisons however, this study found that the ideal deviates materially from the actual lived experience of racialized individuals. The policy recommendations emerging from this research will benefit Canadians and may have transferability to other countries where racism is prevalent. Policy recommendations are:
-
Address diversity in pharmaceutical care provision planning. National and provincial investments should be made to reduce pharmacy deserts in racialized communities.
-
Collect data to measure and monitor improvements in access to medicines by racialized and marginalized individuals and help promote evidence-based solutions, actions, and policies.
-
Update policy and law to remove jurisdictional barriers to access to medicines by First Nations, Métis, and Inuit peoples.
-
Implement Universal Pharmacare to mitigate the impact of racism in employment practices that effect medicines coverage.
-
Include cultural competency training emphasizing decolonial perspectives to reduce implicit bias in health care provider education.
-
Design policies to foster access to medicines, vaccines, and pharmaceutical services.
Conclusions
This study contributes to the literature on racism and access to medicines. The study informs healthcare policy debates in Canada and internationally regarding how to assure equitable access to affordable, quality, safe, and efficacious medicines. Understanding how racism is manifested in pharmaceutical and health systems can contribute to system redesign to increase access for Black, Indigenous, and other racialized communities. World Health Assembly Declaration (2012) calls for “strengthening national regulatory authorities and health systems that include national medicine policies” to achieve universal access to essential medicines. International covenants provide the groundwork for abolishing structural racism to assure the right to equitable access to medicines. Racism corrupts and impedes the equitable allocation of and access to medicines in Canada. Redefining racism as a form of corruption would obligate societal institutions to investigate and address racism within the context of the law as opposed to normative policy.
Data Availability
Upon request.
Code Availability
MAXQDA2022.
References
Robson L, Ackford R. Racism and a public health issue. BH.01.DEC0220.R21, Wellington-Dufferin-Guelph Public Health, 2020. https://wdgpublichealth.ca/sites/default/files/file-attachments/BOH/bh.01.dec0220.r21_-_racism_as_a_public_health_issue.pdf. Accessed 23 Dec 2021.
Carter C, McPherson D. Getting to tomorrow: a report on canadian drug policy. Vancouver: Canadian Drug Policy Coalition, 2013. www.drugpolicy.ca. Accessed 1 Nov 2022.
Phillips-Beck W, Eni R, Lavoie JG, et al. Confronting racism within the Canadian healthcare system: systemic exclusion of first nations from quality and consistent care. Int J Environ Res Public Health. 17. Epub ahead of print 2020. https://doi.org/10.3390/ijerph17228343.
AMA. What is structural racism? AMA: Health Equity, https://www.ama-assn.org/delivering-care/health-equity/what-structural-racism (2021, accessed 14 September 2022).
Munn Z, Peters MDJ, Stern C, et al. Systematic review or scoping review? Guidance for authors when choosing between a systematic or scoping review approach. BMC Med Res Methodol. 2018;18:143.
Corruption. Urban dictionary, https://www.urbandictionary.com/define.php?term=Corruption. Accessed 10 Mar 2023.
Transparency International. What is corruption, (nd). https://www.transparency.org/en/what-is-corruption. Accessed 10 Mar 2023.
Rose J. The meaning of corruption: testing the coherence and adequacy of corruption definitions. Public Integr. 2018;20:220–33.
Moscou K, Kohler JC, MaGahan A. Governance and pharmacovigilance in Brazil: a scoping review. J Pharm Policy Pract. 9. Epub ahead of print 2016. https://doi.org/10.1186/s40545-016-0053-y.
Moscou K. Pharmacogovernance in Kenya. In: Leadership in pharmaceutical systems. Ouidah, Benin, (2018). https://globalmed.sciencesconf.org/data/pages/EN_programme_220318_Light.pdf. Accessed 2 Nov 2022.
World Health Assembly. Substandard/spurious/falsely-labelled/falsified/counterfeit medical products. WHA65.19 Sixty-fifth World Health Assembly. Tenth Plenary Meeting A65/VR/10 (Vol. Agenda item 13.13). 26 May 2012.
Canada Health Act. Canada Health Act R.S.C., 1985, https://laws-lois.justice.gc.ca/eng/acts/C-6/page-1.html#h-151484. Accessed 10 Mar 2023
Delgado R, Stefanic J. Critical race theory: an introduction. Third. New York University Press, http://ebookcentral.proquest.com (2017).
Jacklin KM, Henderson RI, Green ME, et al. Health care experiences of indigenous people living with type 2 diabetes in Canada. CMAJ. 2017;189:E106–12.
Mahabir DF, O’Campo P, Lofters A, et al. Experiences of everyday racism in Toronto’s health care system: a concept mapping study. Int J Equity Health. 2021;20:74.
Wylie L, McConkey S. Insiders’ insight: discrimination against Indigenous peoples through the eyes of health care professionals. J Racial Ethn Health Disparities. 2019;6:37–45.
Levy J, Ansara D, Stover A. Racialization and health inequities in Toronto. Toronto: Toronto Public Health, https://www.deslibris.ca/ID/240398 (2013).
Chambers L, Burnett K. Jordan’s Principle: the struggle to access on-reserve health care for high-needs indigenous children in Canada. Am Indian Q. 2017;41:101–24.
Monchalin R, Smylie J, Nowgesic E. “I guess I shouldn’t come back here”: racism and discrimination as a barrier to accessing health and social services for urban Métis women in Toronto, Canada. J Racial Ethn Health Disparities. 2020;7:251–61.
Indian Act, R.S.C., https://laws-lois.justice.gc.ca/eng/acts/i-5/ (1985).
Government of Canada. Guide for pharmacy benefits: non-insured health benefits. Government of Canada, 2021. https://www.sac-isc.gc.ca/eng/1576430557687/1576430636766#chp5_1. Accessed 2 Nov 2022.
The Inner City Health Strategy Working Group. Inner city health: experiences of racialization and health inequity. Toronto: Wellesley Institute, 2010. https://www.deslibris.ca/ID/225229. Accessed 2 Nov 2022.
Truth and Reconciliation Commission of Canada. Truth and reconciliation commission of Canada: calls to action, 2015. www.trc.ca. Accessed 15 Sept 2022.
Khenti A. The Canadian war on drugs: structural violence and unequal treatment of Black Canadians. Int J Drug Policy. 2013;25:190–5.
McKelvie S. “Smack in the middle”: urban governance and the spatialization of overdose epidemics. City Community 19:704–725. https://doi.org/10.1111/cico.12456
Dollar CB. Criminalization and drug “wars” or medicalization and health “epidemics”: how race, class, and neoliberal politics influence drug laws. Crit Criminol. 2019;27:305–27.
Bodkin C, Bonn M, Wildeman S. Fuelling-a-crisis-lack-of-treatment-for-opioid-use-in-canadas-prisons-and-jails. The conversation, 2020. https://theconversation.com/fuelling-a-crisis-lack-of-treatment-for-opioid-use-in-canadas-prisons-and-jails-130779.
City of Oshawa Zoning By-law 60–94. n.d.
Ahmed R, Jamal O, Ishak W, et al. Racial equity in the fight against COVID-19: a qualitative study examining the importance of collecting race-based data in the Canadian context. Trop Dis Travel Med Vaccines. 2021;7:15.
May T. The role of race in pandemic vaccine allocation. Am J Bioeth. 2021;21:89–91.
Law MR, Dijkstra A, Douillard JA, et al. Geographic accessibility of community pharmacies in Ontario. Healthcare Policy. 2011;6:36–45.
Shah TI, Bell S, Wilson K. Spatial accessibility to health care services: identifying under-serviced neighbourhoods in Canadian urban areas. PLoS ONE. 2016;11:e0168208.
Wang L, Ramroop S. Geographic disparities in accessing community pharmacies among vulnerable populations in the Greater Toronto Area. Can J Public Health. 2018;109:821–32.
Glazier RH, Yeritsyan N, Gozdyra P. Geographic access to primary care and hospital services for rural and northern communities : report to the Ontario Ministry of Health and Long-Term Care. Toronto, Ont: Institute for Clinical Evaluative Sciences, 2011. Retrived 30 April 2023 from https://www.ices.on.ca/Publications/Atlases-and-Reports/2011/Geographic-Access-to-Primary-Care
Hapuhennedige S. Vaccination debates may obscure access issues. 2020; E935+.
Weaver J, Newman PA, Williams CC, et al. ‘Sisters, mothers, daughters and aunties’: HIV vaccine acceptability among African, Caribbean and other Black women in Toronto. Canadian J Public Health. 2013;104:e413+.
Bajgain BB, Bajgain KT, Badal S, et al. Patient-reported experiences in accessing primary healthcare among immigrant population in Canada: a rapid literature review. Int J Environ Res Public Health. 2020;17:8724.
Grignon M, Longo C, Marchildon G, et al. The 2018 decision to establish an advisory council on adding pharmaceuticals to universal health coverage in Canada. Health Policy. 2020;124:7.
Medical Officer of Health. Medically uninsured residents in Toronto: staff report. Toronto: Toronto Public Health, https://www.deslibris.ca/ID/239282 (2013).
Chiefs of Ontario. First Nations Regional Health Survey (RHS) Ontario region phase 2 (2008/10): people’s report. Toronto: Chiefs of Ontario, https://www.deslibris.ca/ID/247162 (2015).
Bell S, Wilson K, Bissonnette L, et al. Access to primary health care: does neighborhood of residence matter. Ann Assoc Am Geogr. 2013;103:85–105.
Chen YYB. Migrant health in a time of pandemic: fallacies of us-versus-them. In: Vulnerable The Law, Policy and Ethics of COVID-19. University of Ottawa Press, 2020, pp 407–418.
Benjamin R. Cultura obscura: race, power, and “culture talk” in the health sciences. Am J Law Med. 2017;43:225–38.
Hoffman KM, Trawalter S, Axt JR, et al. Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites. Proc Natl Acad Sci USA. 2016;113:4296.
Nash M. Race and the ideology of race. Curr Anthropol. 1962;3:285–8.
Acknowledgements
The authors would like to acknowledge Sadie Red Wing, Lakatoa from the Spirit Lake Nation and Assistant Professor at OCAD University for her review of this manuscript.
Funding
The research was supported by a SEED grant provided by OCAD University.
Author information
Authors and Affiliations
Contributions
The corresponding author conceived and designed the study. All authors contributed to literature retrieval and screening for exclusion and inclusion in the study. All authors contributed to data analysis to identify key themes. KM, YO, and AB contributed to drafting the manuscript, and KM, YO, AB, AS, and IZ revised the manuscript. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Moscou, K., Bhagaloo, A., Onilude, Y. et al. Broken Promises: Racism and Access to Medicines in Canada. J. Racial and Ethnic Health Disparities 11, 1182–1198 (2024). https://doi.org/10.1007/s40615-023-01598-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-023-01598-2