Abstract
Purpose of Review
We discuss how epidemiologic studies have used observational data to estimate the effects of potential interventions on early-life environmental exposures. We summarize the value of posing questions about interventions, how a group of techniques known as “g-methods” can provide advantages for estimating intervention effects, and how investigators have grappled with the strong assumptions required for causal inference.
Recent Findings
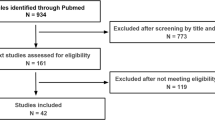
We identified nine studies that estimated health effects of hypothetical interventions on early-life environmental exposures. Of these, six examined air pollution. Interventions evaluated by these studies included setting exposure levels at a specific value, shifting exposure distributions, and limiting exposure levels to less than a threshold value. Only one study linked exposure contrasts to a specific intervention on an exposure source, however.
Summary
There is growing interest in estimating intervention effects of early-life environmental exposures, in part because intervention effects are directly related to possible public health actions. Future studies can build on existing work by linking research questions to specific hypothetical interventions that could reduce exposure levels. We discuss how framing questions around interventions can help overcome some of the barriers to causal inference and how advances related to machine learning may strengthen studies by sidestepping the overly restrictive assumptions of parametric regression models. By leveraging advancements in causal inference and exposure science, an intervention framework for environmental epidemiology can guide actionable solutions to improve children’s environmental health.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Landrigan P, Baloh R, Barthel W, et al. Neuropsychological dysfunction in children with chronic low-level lead absorption. Lancet. 1975;305:708–12. https://doi.org/10.1016/S0140-6736(75)91627-X.
Buckley JP, Hamra GB, Braun JM. Statistical approaches for investigating periods of susceptibility in children’s environmental health research. Curr Environ Health Rep. 2019;6:1–7. https://doi.org/10.1007/s40572-019-0224-5.
Selevan SG, Kimmel CA, Mendola P. Identifying critical windows of exposure for children’s health. Environ Health Perspect. 2000;108:451–5. https://doi.org/10.1289/ehp.00108s3451.
Galea S. An argument for a consequentialist epidemiology. Am J Epidemiol. 2013;178:1185–91. https://doi.org/10.1093/aje/kwt172.
Westreich D, Edwards JK, Rogawski ET, et al. Causal impact: epidemiological approaches for a public health of consequence. Am J Public Health. 2016;106:1011. https://doi.org/10.2105/AJPH.2016.303226.
Hernán MA, Robins JM. Estimating causal effects from epidemiological data. J Epidemiol Community Health. 2006;60:578–86. https://doi.org/10.1136/jech.2004.029496.
Rubin DB. Estimating causal effects of treatment in randomized and nonrandomized studies. J Educ Psychol. 1974;66:688–701. https://doi.org/10.1037/h0037350.
Robins J. A new approach to causal inference in mortality studies with a sustained exposure period - application to control of the healthy worker survivor effect. Math Model. 1986;7:1393–512. https://doi.org/10.1016/0270-0255(86)90088-6.
Naimi AI, Cole SR, Kennedy EH. An introduction to g methods. Int J Epidemiol. 2017;46:756–62. https://doi.org/10.1093/ije/dyw323.
Hernán MA, Taubman SL. Does obesity shorten life? The importance of well-defined interventions to answer causal questions. Int J Obes (Lond). 2008;32:S8-14. https://doi.org/10.1038/ijo.2008.82.
•• Garcia E, Urman R, Berhane K, et al. Effects of policy-driven hypothetical air pollutant interventions on childhood asthma incidence in southern California. Proc Natl Acad Sci U S A. 2019;116:15883–8. https://doi.org/10.1073/pnas.1815678116. Demonstrates use of g-computation for several types of interventions and assesses causal assumptions.
Zigler CM, Dominici F. Point: clarifying policy evidence with potential-outcomes thinking—beyond exposure-response estimation in air pollution epidemiology. Am J Epidemiol. 2014;180:1133–40. https://doi.org/10.1093/aje/kwu263.
Casey JA, Gemmill A, Karasek D, et al. Increase in fertility following coal and oil power plant retirements in California. Environ Health. 2018;17:1–10. https://doi.org/10.1186/s12940-018-0388-8.
Casey JA, Karasek D, Ogburn EL, et al. Retirements of coal and oil power plants in California: association with reduced preterm birth among populations nearby. Am J Epidemiol. 2018;187:1586–94. https://doi.org/10.1093/aje/kwy110.
Westreich D, Cole SR, Young JG, et al. The parametric g-formula to estimate the effect of highly active antiretroviral therapy on incident AIDS or death. Stat Med. 2012;31:2000–9. https://doi.org/10.1002/sim.5316.
Writing Committee for the CASCADE Collaboration. Timing of HAART initiation and clinical outcomes in human immunodeficiency virus type 1 seroconverters. Arch Intern Med. 2011;171:1560–9. https://doi.org/10.1001/archinternmed.2011.401.
Rudolph JE, Cartus A, Bodnar LM, et al. The role of the natural course in causal analysis. Am J Epidemiol. 2022;191:341–8. https://doi.org/10.1093/aje/kwab248.
Urman R, Garcia E, Berhane K, et al. The potential effects of policy-driven air pollution interventions on childhood lung development. Am J Respir Crit Care Med. 2020;201:438–44. https://doi.org/10.1164/rccm.201903-0670OC.
Snowden JM, Mortimer KM, Kang Dufour MS, et al. Population intervention models to estimate ambient NO2 health effects in children with asthma. J Expo Sci Environ Epidemiol. 2015;25:567–73. https://doi.org/10.1038/jes.2014.60.
Goin DE, Sudat S, Riddell C, et al. Hyperlocalized measures of air pollution and preeclampsia in Oakland. California Environ Sci Technol. 2021;55:14710–9. https://doi.org/10.1021/acs.est.1c02151.
Riddell CA, Goin DE, Morello-Frosch R, et al. Hyper-localized measures of air pollution and risk of preterm birth in Oakland and San Jose. California Int J Epidemiol. 2021;50:1875–85. https://doi.org/10.1093/ije/dyab097.
•• Oulhote Y, Coull B, Bind M-A, et al. Joint and independent neurotoxic effects of early life exposures to a chemical mixture: a multi-pollutant approach combining ensemble learning and g-computation. Environ Epidemiol 2019;3. https://doi.org/10.1097/ee9.0000000000000063. Demonstrates g-computation with biomarkers of exposure, using Super Learner.
Kponee-Shovein KZ, Weisskopf MG, Grashow R, et al. Estimating the causal effect of prenatal lead exposure on prepulse inhibition deficits in children and adolescents. Neurotoxicology. 2020;78:116–26. https://doi.org/10.1016/j.neuro.2020.02.013.
•• Keil AP, Buckley JP, Kalkbrenner AE. Bayesian g-computation to estimate impacts of interventions on exposure mixtures: demonstration with metals from coal-fired power plants and birthweight. Am J Epidemiol. 2021;190:2647–57. https://doi.org/10.1093/aje/kwab053. Links exposure levels to intervention on a source and discusses tradeoffs between causal assumptions.
Snowden JM, Rose S, Mortimer KM. Implementation of G-computation on a simulated data set: demonstration of a causal inference technique. Am J Epidemiol. 2011;173:731–8. https://doi.org/10.1093/aje/kwq472.
Ahern J, Hubbard A, Galea S. Estimating the effects of potential public health interventions on population disease burden: a step-by-step illustration of causal inference methods. Am J Epidemiol. 2009;169:1140–7. https://doi.org/10.1093/aje/kwp015.
Naimi AI, Moodie EEM, Auger N, et al. Constructing inverse probability weights for continuous exposures: a comparison of methods. Epidemiology. 2014;25:292–9. https://doi.org/10.1097/EDE.0000000000000053.
Keil AP, Richardson DB. Quantifying cancer risk from radiation. Risk Anal. 2018;38:1474–89. https://doi.org/10.1111/risa.12947.
Moore K, Neugebauer R, Lurmann F, et al. Ambient ozone concentrations and cardiac mortality in Southern California 1983–2000: application of a new marginal structural model approach. Am J Epidemiol. 2010;171:1233–43. https://doi.org/10.1093/aje/kwq064.
• Carone M, Dominici F, Sheppard L. In pursuit of evidence in air pollution epidemiology: the role of causally driven data science. Epidemiology. 2020;31:1–6. https://doi.org/10.1097/EDE.0000000000001090. Discusses the advantages of causal estimators over traditional regression-based approaches.
Ahern J, Hubbard AE. A Roadmap for estimating and interpreting population intervention parameters. In: Oakes JM, Kaufman JS, eds. Methods in Social Epidemiology. San Francisco, CA: Jossey-Bass 2017. 432–57.
• Mooney SJ, Keil AP, Westreich DJ. Thirteen questions about using machine learning in causal research (you won’t believe the answer to number 10!). Am J Epidemiol. 2021;190:1476–82. https://doi.org/10.1093/aje/kwab047. Provides an overview of machine learning for causal inference.
Naimi AI, Balzer LB. Stacked generalization: an introduction to super learning. Eur J Epidemiol. 2018;33:459–64. https://doi.org/10.1007/s10654-018-0390-z.
van der Laan MJ, Polley EC, Hubbard AE. Super learner. Stat Appl Genet Mol Biol 2007;6. https://doi.org/10.2202/1544-6115.1309
Keil AP, Daza EJ, Engel SM, et al. A Bayesian approach to the g-formula. Stat Methods Med Res. 2018;27:3183–204. https://doi.org/10.1177/0962280217694665.
Edwards JK, Cole SR, Westreich D. All your data are always missing: incorporating bias due to measurement error into the potential outcomes framework. Int J Epidemiol. 2015;44:1452–9. https://doi.org/10.1093/ije/dyu272.
Díaz I, van der Laan MJ. Assessing the causal effect of policies: an example using stochastic interventions. Int J Biostat. 2013;9:161–74. https://doi.org/10.1515/ijb-2013-0014.
Huang W, Igusa T, Wang G, et al. In-utero co-exposure to toxic metals and micronutrients on childhood risk of overweight or obesity: new insight on micronutrients counteracting toxic metals. Int J Obes (Lond) Published Online First: 2022. https://doi.org/10.1038/s41366-022-01127-x
Hamra GB, Buckley JP. Environmental exposure mixtures: questions and methods to address them. Curr Epidemiol Rep. 2018;5:160–5. https://doi.org/10.1007/s40471-018-0145-0.
Weisskopf MG, Seals RM, Webster TF. Bias amplification in epidemiologic analysis of exposure to mixtures. Environ Health Perspect. 2018;126:047003. https://doi.org/10.1289/EHP2450.
Webster TF, Weisskopf MG. Epidemiology of exposure to mixtures: we can’t be casual about causality when using or testing methods [Preprint]. arXiv Published Online First: 2020. https://doi.org/10.48550/arXiv.2007.01370
Keil AP, Buckley JP, O’Brien KM, et al. A quantile-based g-computation approach to addressing the effects of exposure mixtures. Environ Health Perspect. 2020;128:1–10. https://doi.org/10.1289/EHP5838.
Petersen ML, Porter KE, Gruber S, et al. Diagnosing and responding to violations in the positivity assumption. Stat Methods Med Res. 2012;21:31–54. https://doi.org/10.1177/0962280210386207.
Zigler CM. Invited commentary: the promise and pitfalls of causal inference with multivariate environmental exposures. Am J Epidemiol. 2021;190:2658–61. https://doi.org/10.1093/aje/kwab142.
Keil AP, Buckley JP, Kalkbrenner AE. Keil et al. Respond to “Causal Inference for Environmental Mixtures.” Am J Epidemiol. 2021;190:2662–3. https://doi.org/10.1093/aje/kwab143.
Zivich PN, Breskin A. Machine learning for causal inference: on the use of cross-fit estimators. Epidemiology. 2021;32:393–401. https://doi.org/10.1097/EDE.0000000000001332.
Harvard CAUSALab. Software. https://causalab.sph.harvard.edu/software/ (accessed 23 May 2022).
Funding
TJSS was supported by the National Institute for Environmental Health Sciences (NIEHS; T32ES007141). APK and JPB were supported by NIEHS (R01ES029531).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Early Life Environmental Health
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Smith, T.J.S., Keil, A.P. & Buckley, J.P. Estimating Causal Effects of Interventions on Early-life Environmental Exposures Using Observational Data. Curr Envir Health Rpt 10, 12–21 (2023). https://doi.org/10.1007/s40572-022-00388-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-022-00388-y