Abstract
Purpose of Review
Cannabis exposure during critical windows of development may have intergenerational physiological consequences disrupting epigenetic programming and marks. This review examines the literature relating to pre-gestational and prenatal cannabinoid exposure and its effect on genes and molecular pathways related to the development of psychiatric disease.
Recent Findings
Developmental cannabis exposure alters epigenetic processes with functional gene consequences. These include potentially heritable alterations in genes and molecular pathways critical for brain development and associated with autism spectrum disorder (ASD), attention deficit hyperactivity disorder (ADHD), schizophrenia, addiction, and other psychiatric diseases.
Summary
Cannabis consumption and mental health illness in adolescents and young adults are increasing in the United States (U.S.), and recent studies suggest that cannabis consumption during critical periods of brain development could contribute to mental health illness through epigenetic mechanisms. These findings warrant future studies and consideration by regulators and health communicators.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cannabis (marijuana) is the most commonly used illicit psychoactive drug in the United States (U.S.) with an estimated 9.6% of the population aged 12 and older reporting use in the past month [1]. States are increasingly legalizing both recreational and medicinal cannabis use [2]. The majority of new users are under 18 years of age [3], and cannabis use has increased among youth and teens since 2007 [4]. In addition, pregnant women are increasingly using it to mitigate morning sickness. In the U.S., between 2002–2003 and 2016–2017, the adjusted prevalence of past-month cannabis use increased from 3.4 to 7.0% among pregnant women overall and from 5.7 to 12.1% among pregnant women during the first trimester [5]. A recent national survey suggested that the public perception of “great risk” from weekly cannabis use has dropped from 50.4% in 2002 to 33.3% in 2014 [6]. Another recent survey found that 81% of U.S. adults believe that cannabis has at least one health benefit, such as use in pain management, disease treatment, or relief of anxiety, stress, or depression. While 91% of U.S. adults also believe cannabis use has at least one risk, including those associated with legal issues, 9% believe it has no risks, and the American public has an overall favorable view of cannabis [7].
Cannabis is composed of over 400 chemicals, of which over 60 are cannabinoid compounds. The four major compounds include Δ9-tetrahydrocannabinol (THC), cannabidiol (CBD), Δ8-tetrahydrocannabinol, and cannabinol [8]. The major psychoactive cannabinoid in cannabis, THC, targets the endocannabinoid (eCB) system, which regulates biological processes involved in development and neuroplasticity [9]. It mimics eCB action, exerting most of its effects via cannabinoid receptors (CBR)s 1 and 2. CBR1 is one of the most abundant G protein-coupled receptors in the adult brain, and it is localized in regions important in movement, cognition, attention, emotion, and memory [10]. In animals, expression begins early in the central nervous system (CNS) during embryonic development [11,12,13]. One study found CBR1 expressed in the human fetal brain at 20 weeks, with high expression in the hippocampus and amygdala [14]. In contrast, CBR2 is mainly expressed in immune cells. Male mitotic germ cells also express a high level of CBR2, whose activation promotes their differentiation and progresses spermatogenesis [15••]. During adolescence, the eCB system continues to facilitate neurodevelopment through its involvement in neuroplasticity and synaptic function. Levels of CBRs fluctuate during adolescence and depend on the brain region. For instance, there is a rapid, sustained increase in CBR binding sites in the striatum that is reduced by half in early adulthood [16], as well as high levels in limbic related regions that gradually decrease by adulthood [17]. Tightly regulated biosynthetic pathways ensure proper signaling throughout development, and correct brain function depends heavily on the temporal and spatial layout of the eCB system [18]. Thus, exposure to THC, especially during critical windows of brain development, has the potential to disrupt the tightly regulated system.
Parallel to the increase in adolescent cannabis use, the percentage of adolescents and young adults experiencing certain types of psychiatric disorders has risen in the United States over the past decade, despite the lack of increase in adults [19]. In human studies, THC has been shown to disrupt the development and function of the brain [20, 21], and in animals, THC has been experimentally shown to lead to molecular impairments that are heritable and extend into subsequent generations [22], thus increasing the risk of offspring developing a psychiatric disease [23,24,25,26]. Three different routes of multigenerational transmission have been summarized in a prior review [27]; they include fetal programming (direct effect), germline transmission (direct effect), and behavioral or social transfer (indirect effect). The first route is typical for prenatal exposure, the second route is typical for pre-gestational exposure, while the third route is typical for both.
In a recent commentary, which was published in response to a study examining the epigenetic impact of cannabis use on rat and human sperm [28••], the authors highlighted that the epigenomic toxicology of cannabinoids should have priority on the research agenda, especially considering the potential transgenerational health implications [29]. A review published in 2016 focused on the epigenetic effects of cannabis exposure [22]. The authors noted that the majority of addiction-related epigenetic neurobiological studies had targeted the adult brain, while there was a dearth of literature on the potential intergenerational impacts of cannabis [22]. Another article published in 2018 provided an overview of the current data regarding vulnerabilities of the developing brain to cannabinoid exposure during sensitive windows of development, especially with regard to epigenetic changes associated with cannabis use [27]. Since that time, additional studies were published that address research gaps and have the potential to better inform clinical guidelines, preventative policy, and public opinion related to cannabis use during specific time points of the life course.
Heritable molecular impairments include epigenetic modifications, such as DNA methylation, histone modifications, and changes in non-coding RNA (ncRNA), which regulate patterns of gene expression by altering DNA accessibility and chromatin structure [30]. DNA methylation occurs when a methyl group is added at a cytosine nucleotide that precede guanines (CpG dinucleotides), influencing DNA function by activating or repressing transcriptional activity of a gene and by altering chromatin accessibility and remodeling [30]. DNA methylation in the promoter region of a gene usually downregulates its expression, while higher DNA methylation in a gene body may promote expression of a gene. In most instances, DNA methylation represses gene expression by preventing the binding of transcription factors, or recruiting proteins that bind to methylated DNA [31]. Histones are large groups of protein complexes that help DNA condense into chromatin. Histone modifications include methylation and acetylation of lysine residues on histone tails, which affect gene expression by altering chromatin structure and accessibility [31]. In addition, ncRNA, such as micro (mi)RNA and long non-coding (lnc)RNA, control DNA availability and transcription, regulate RNA processing and splicing, and form a scaffold upon which layers of DNA regulation are built [29, 32].
Some epigenetic modifications are passed down to offspring through genomic imprinting (1% of mammalian genes), in which offspring only inherit one working copy of a gene. Imprinted genes are silenced via DNA methylation in either the egg or sperm [33]. Other modifications are passed down when genes escape epigenetic reprogramming, a process that occurs during the formation of primordial germ cells and in the early embryo soon after fertilization [34], in which genomic potential resets and epigenetic memory is erased [35].
In this review, we provide an analysis of the recent literature relating to pre-gestational and prenatal cannabinoid exposure and its effect on genes and molecular pathways. Along with the studies discussed in the review, additional animal studies are summarized in Tables 1 and 2, in which molecular changes are observed in the F0 generation of adolescent brain tissue [36,37,38,39, 40•, 41••, 42•].
Prenatal Exposure to Cannabis: Epigenetic and Functional Alterations in Offspring Brain Tissue
Since 2002, there has been an increase in pregnant women in the U.S. reporting daily cannabis use, use in the past-month, as well as an increase in the number of days during pregnancy that they report using cannabis [5]. Pregnant women report using cannabis most frequently during the first trimester [5], in order to mitigate morning sickness [43]. Studies have confirmed that THC readily crosses the placenta, distributes into the fetal compartment, and crosses the fetal blood-brain barrier [44]. A handful of studies in both human subjects and animal models have indicated that the embryonic nervous system patterning is particularly susceptible to maternal cannabis use [45,46,47,48,49,50]. Its use during pregnancy has been associated with an increased risk of various cognitive, behavioral, and neuropsychiatric defects [51, 52]. Use during pregnancy has also been associated with an increased risk of preterm birth in some studies [49, 50], as well as decreased birth weight [53, 54]. This section highlights recent studies that have examined the epigenetic mechanisms by which prenatal cannabis exposure increases the risk of postnatal psychiatric disease.
Human Evidence
Considering that maternal cannabis use during pregnancy is associated with long-term adverse behavioral outcomes and addiction vulnerability in offspring [44], it is possible that epigenetic changes established in utero that affect dopaminergic reward signaling are involved. The striatal dopamine system, composed of medium spiny neurons enriched in cannabinoid receptors, is implicated in the pathogenesis of neuropsychiatric disorders [55]. One study tested the neurobiology underlying the risk of addiction vulnerability in humans by examining mRNA expression in fetal brain specimens of the putamen and nucleus accumbens (NAc), from mothers who underwent elective abortions between 18 and 22 weeks of gestation [55] (Table 1). Half of the fetal brain specimens were those from mothers who had positive maternal self-report and/or maternal urine that tested positive for THC and/or fetal meconium positive for THC, while the other half had no cannabis exposure. Not only did fetuses exposed prenatally to cannabis have decreased dopamine receptor D2 (DRD2) mRNA levels in the NAc, compared to controls, but there was also a dose response observed in which greater maternal use was correlated with decreased DRD2 mRNA levels. In contrast, there was no difference in DRD2 mRNA levels in the putamen. There was also no difference in DRD1 mRNA levels, or mRNA levels of the opioid neuropeptides proenkephalin (PENK) and prodynorphin (PDYN) in the putamen or NAc, between the exposed and unexposed groups. The NAc core and shell are important components of motor and reward circuits, respectively [56], and disruptions in these signaling pathways could lead to adverse psychiatric outcomes [57].
Additional studies were conducted on the same fetal brain specimens used in the study discussed above [55]. In these analyses, decreased DRD2 mRNA levels were observed in the amygdala basal nucleus of fetuses exposed prenatally to cannabis compared to controls [58], which was consistent with the reduced levels observed in the NAc [55]. In addition, fetal brain specimens with maternal cannabis exposure had reduced PENK expression in the caudal putamen, and PENK mRNA levels were inversely correlated with amount of maternal cannabis intake during pregnancy [59]. Disruptions in the opioid system during development contribute to the development of psychiatric disorders [59, 60] and persist into adulthood, increasing vulnerability to opiate-seeking behavior [61]. Dysregulation of DRD2 is implicated in addiction risk and other psychiatric disorders, and its alteration was a consistent finding in the animal studies, as well as the human studies.
Another recent study evaluated whether prenatal cannabis exposure is associated with DNA methylation of dopamine receptor D4 (DRD4) promoter in buccal cells from the neonates of maternal subjects with either cannabis or no cannabis use anytime during pregnancy [62•] (Table 1). Buccal epithelial cells have the same developmental origins as neuronal cells, and prior studies provide support for buccal cells as a proxy for neurodevelopmental phenotypes [63]. There was no association between DNA methylation at individual CpG sites in DRD4 after correction for multiple testing. It is unclear if the null findings were due to the relatively small sample size (n = 804 maternal subjects), the tissue specificity, or a lack of biological relevance [62•]. Certain genetic polymorphisms of DRD4 increase risk of drug use and severity of ADHD symptoms in children, both of which have been associated with cannabis exposure [64]. Future candidate gene studies should examine the association between prenatal cannabis exposure and epigenetic changes in DRD4 in brain or other target cells, instead of the buccal cell proxy, as well as account for genetic polymorphisms.
Animal Evidence
The study discussed above [55] that reported decreased DRD2 mRNA levels in the NAc of cannabis-exposed gestation week 18–22 human fetuses also explored the mechanisms underlying this decrease in studies in rats (Table 2). Pregnant rats were exposed to THC and changes in NAc Drd2 gene expression in offspring were evaluated at postnatal day 2 (PND2), a comparable point in brain development as that occurring in humans during gestation weeks 18–22 [55, 58, 59]. A separate cohort of male offspring was studied in adulthood (PND62), in order to evaluate any long-term impairments induced by prenatal THC exposure. Consistent with the cannabis-exposed human fetuses, rats exposed to THC had about a 40% reduction in NAc Drd2 mRNA levels at PND2, compared to unexposed control rats. This decrease persisted into adulthood, with about a 30% reduction in NAc Drd2 mRNA levels observed at PND62 in prenatally exposed rats, compared to unexposed controls. There was no difference in Drd2 mRNA levels, between the exposed and unexposed groups, in the dorsal striatum [55].
In this study [55], the epigenetic mechanisms by which Drd2 mRNA transcript expression was altered were evaluated. THC exposure significantly increased the repressive dimethylated lysine 9 (2meH3K9) mark on histone H3 between − 1.8 kb (69% increase vs control) and − 3 kb (83% increase vs control) upstream of the transcription start site (TSS) in the Drd2 gene. It also decreased trimethylated lysine 4 (3meH3K4) on histone H3 across the analyzed genomic fragment in the NAc of adult rats. Consistent with 3meH3K4 acting as a mark of transcriptional activity, its reduction was associated with decreased RNA polymerase II (Pol II) at the TSS (+ 0.3 kb) and within the coding region(+ 40 kb). Although no change in 2meH3K9 was observed at the dopamine receptor D1 (Drd1) gene, there was reduced 3meH3K4 and decreased Pol II association at this locus, despite the lack of alteration of Drd1 transcripts in the NAc during adulthood. Decreased dopamine receptor binding sites were also observed in the adult NAc in the THC-exposed rats, compared to controls.
Pre-gestational Exposure to Cannabis: Epigenetic and Functional Alterations in Offspring Brain Tissue
There is some evidence in model animal studies that pre-gestational exposure to cannabis also causes alterations that can be passed down to offspring, even after years of cannabis cessation. It is possible that epigenetic modifications mediate the relationship between pre-gestational exposure to cannabis and adverse psychiatric outcomes in offspring, especially when cannabis exposure occurs during adolescence or early adulthood.
Animal Evidence
A recent study evaluated the association between male rat exposure to synthetic CBR1 agonist WIN 55212-2 (WIN) during adolescence (compared to pre-gestational vehicle [VEH] exposure) and global DNA methylation in the prefrontal cortex (PFC) of their offspring. The offspring were also subjected to unpredictable stress, variable stress, or no stress, in order to examine the interaction between pre-gestational WIN exposure and stress response [65•] (Table 2). Increased global DNA methylation was observed in offspring with pre-gestational WIN exposure, compared to controls, regardless of presence or absence of stress exposure. In addition, increased DNA methyltransferase (Dnmt)1 mRNA levels were observed in offspring with pre-gestational WIN exposure, compared to unexposed controls in non-stressed animals only, while increased Dnmt3 mRNA levels were observed in offspring with pre-gestational WIN exposure, compared to unexposed controls, regardless of presence or absence of stress exposure. It is plausible that the increased global PFC DNA methylation observed in animals with pre-gestational WIN exposure, as well as in stressed animals, was mediated by the upregulation of DNMT enzymes, since these are responsible for epigenetic maintenance. The molecular alterations were consistent with the observed phenotypes, as stress exposure induced anxiety-like behavior in offspring with pre-gestational WIN exposure, compared to controls without pre-gestational WIN exposure. The epigenetic changes in the offspring could have been due to direct epigenetic modifications on the sperm or testes, as well as related to disruptions in the paternal endocannabinoid system. This animal model supports a transgenerational epigenetic effect of cannabinoid exposure potentially altering stress response in the offspring. However, global DNA methylation measurements lack gene specificity and therefore provide limited biological insights.
Another study in rats examined the association between exposure to THC in male and female rats during adolescence and differentially methylated regions (DMRs) in the NAc of offspring using Enhanced Reduced Representation Bisulfite Sequencing (ERRBS) [25] (Table 2). A total of 1027 DMRs, including 406 hypermethylated and 621 hypomethylated regions, were observed in exposed offspring, compared to unexposed controls with genes enriched for cell membrane function, synaptic organization, and receptor activity. The hypomethylated DMR in the first coding exon of glutamate ionotropic receptor NMDA type subunit 2A (Grin2a) was consistent with Grin2a mRNA transcript expression differences observed in another rat study by the same research group [24] (Table 2). This is in line with the hypothesis that hypomethylation in gene bodies may lead to decreased gene expression [66]. The Grin2a gene is involved in calcium channel activity and ionotropic glutamate receptor activity and mediates synaptic plasticity and transmission, with impacts on addictive behavior [24, 67].
The same authors that observed reduced Grin2a mRNA levels in the NAc also observed differential mRNA gene expression in different areas of the brain, depending on the time of evaluation (adolescence versus adulthood) in rats pre-gestationally exposed to THC [24] (Table 2). There was increased Cbr1, Grin2a, and Gria2 mRNA expression in pre-gestationally exposed rats, compared to controls at the adolescent time point, while there was a decrease in mRNA expression of Cbr1, Drd2, Grin1, Grin2a, Gria1, and Gria2 in the dorsal striatum in pre-gestationally exposed rats, compared to controls, at the adult time point. The shift in mRNA expression from the adolescent to adult time point is consistent with the transition from reward-oriented to habitual, compulsive drug-taking that typifies progression from recreational drug use to addiction disorder. The same study authors further evaluated potential sex-specific effects and observed that sex-specific mRNA expression patterns were present in both the adolescent and adult brains [23] (Table 2). Overall, the findings contribute to evidence that parental history of germline THC exposure could possibly confer enhanced risk for psychiatric disorders in the subsequent generation, as a result of impaired epigenetic regulatory processes in relevant genes and pathways.
One other study observed no changes in Drd2 mRNA levels in the NAc of adult rats exposed pre-gestationally to WIN and postnatally to morphine [68] (Table 2). The latter study, however, found higher opioid receptor mu (Oprm)1 mRNA levels in WIN-exposed animals, compared to unexposed animals, following a morphine challenge. On the day of the morphine challenge, animals pre-gestationally exposed to WIN had an enhanced response to morphine, compared to controls. The Oprm1 gene encodes at least three opioid receptors in humans, and it is involved in dependence to drugs such as nicotine, cocaine, and alcohol via its modulation of the dopamine system. The study contributed to evidence that pre-gestational cannabis could induce addiction vulnerability in F1 offspring.
Pre-gestational Exposure to Cannabis: Epigenetic and Functional Alterations in Parental Sperm
Not only are epigenetic and functional alterations observed in brain tissue of offspring with pre-gestational exposure to cannabis, but there is also evidence of epigenetic and functional alterations in sperm of exposed individuals in the F0 generation, which could promote germline epigenetic inheritance in future generations.
Human Evidence
In order to evaluate the impact of cannabis exposure during adulthood on the sperm methylome, one study examined DNA methylation in adult male subjects that had either cannabis or no cannabis use [28••] (Table 1). Over 6000 CpG sites differed between cannabis and non-cannabis users. Specifically, prostaglandin I2 receptor (PTGIR) methylation was inversely correlated with THC level, while casein kinase 1 epsilon (CSNK1E) methylation was associated with increased THC. The PTGIR gene is associated with reduced sperm fecundity, while CSNK1E phosphorylates period circadian regulator (PER)2 and is implicated in sensitivity to opioids [67]. Discs-Large Associated Protein (DGLAP)2 was also hypomethylated in the sperm of cannabis-exposed men, compared to controls [28••]. The DGLAP2 gene encodes a membrane-associated protein that is involved in synapse organization and signaling in neuronal cells [67] and is linked to psychological and neurological disorders, such as schizophrenia [69]. It has also been identified as an autism candidate gene [70, 71]. While it is biallelically expressed in the brain, only the paternal allele is expressed in the testes due to imprinting [67].
Another recent study by Schrott et al. 2019 [72••] further evaluated DNA methylation and mRNA transcript expression using the same study population as the study discussed above [28••] (Table 1). They first validated the findings related to DLGAP2 in the study discussed above using quantitative bisulfite pyrosequencing, instead of reduced representation bisulfite sequencing (RRBS) [28••], which showed good agreement. The authors noted that it was one of 46 genes with more than 10 CpG sites showing altered DNA methylation in the sperm of cannabis users, compared to controls. They observed sperm hypomethylation of DLGAP2 at 17 CpGs in exposed adult men, compared to controls, in the RRBS assay. The differential DNA methylation was validated in DLGAP2 for nine CpG sites, plus an additional site, in intron 7 in the pyrosequencing assay. They further determined the functional association between DNA methylation and mRNA transcript expression in human brain tissue from terminated pregnancies, a relevant target tissue for the expression of DLGAP2. In these human brain samples, methylation of DLGAP2 intron 7 was inversely correlated with DLGAP2 mRNA expression and significant only in females.
Animal Evidence
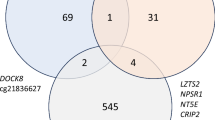
The same two studies in human sperm highlighted in the preceding section also validated their findings using male, sexually mature adult rat sperm from animals exposed to THC, compared to unexposed controls. In the first study, 627 genes had altered DNA methylation associated with THC exposure [28••] (Table 2). There were six overlapping genes among the rat and human-exposed sperm, suggesting that these two pathways may be targets of THC exposure across species. Although the study focused on the F0 generation, some DNA methylation changes of non-imprinted genes in gametes can resist post-fertilization reprogramming and persist in the somatic cells of offspring [73]. Supporting this hypothesis, the authors compared the 627 genes exhibiting DMRs in the rat sperm [28••] to the 473 DMR genes identified in the NAc of adult rats exposed to THC pre-gestationally (compared to unexposed controls) in a study discussed earlier in this review [25] (Table 2). They found 55 overlapping DMR genes between these two datasets with significant enrichment, suggesting that THC-induced epigenetic modifications in sperm cells could persist in somatic cells. Important strengths of this study include some validation from similar observations in human sperm and in adult rat brain tissue.
The same authors pooled data from a new set of sexually mature rats that were given intravenous THC, with the set of rats from Murphy et al. 2018 [28••] given oral THC, and identified a region of Dlgap2 that showed differential methylation in eight CpG sites in sperm between exposed and control groups. Hypomethylation at CpG site 2 was detected in the NAc of pre-gestationally exposed offspring (F1 generation), compared to controls, as well as in the sperm of the THC exposed fathers, compared to controls [72••] (Table 2). The study provided evidence of potential intergenerational inheritance of epigenetic marks in Dlgap2, despite evidence from the same study that it is not an imprint control region.
Finally, a recent study examined epigenetic and functional alterations in sperm of sexually mature mice exposed to the synthetic CBR2 agonist JWH-133. Not only did exposed males have decreased sperm count, but their offspring demonstrated impaired placental development and reduced growth, compared to unexposed controls. This was accompanied by increased DNA methylation at the paternally expressed imprinted genes Peg 10 and Plagl1 in sperm, which was retained in the offspring placenta [15••]. Although the study highlights that overactivation of CBR2 can promote altered DNA methylation in sperm, which is retained in embryonic tissue and may cause altered offspring phenotypes, it could not confirm the precise effect that the epigenetic alterations may have on offspring. However, considering that cannabis is made up of numerous cannabinoids that could bind with CBR2, it adds to the body of evidence that pre-gestational cannabis may promote epigenetic changes in sperm cells that are functionally relevant in offspring.
Conclusion
Together, these findings suggest that pre-gestational and developmental cannabis exposure alters epigenetic processes like DNA methylation and histone modifications with functional consequences for gene expression. Fetal epigenetic programming of genes and some molecular pathways are suggestive of alterations in regions involved in the development of autism spectrum disorder (ASD), attention deficit hyperactivity disorder (ADHD), schizophrenia, addiction, and other psychiatric diseases.
The overall body of evidence is of high public health relevance, as attitudes about cannabis use are changing in favor of its use, especially in adolescents and young adults. In the 2018 National Survey on Drug Use and Health, the majority of people aged 12 or older perceived great risk of harm from weekly use of cocaine or heroin (86.5% and 95.3%, respectively), while less than one third of people (30.6%) aged 12 or older perceived great risk of harm from weekly cannabis use [74]. The legal cannabis market is capitalizing on its popularity by implementing selective growing methods to boost psychoactive potency and to increase profits [75]. In fact, over the last two decades, the average THC content of cannabis has increased from four to 12% [75]. Levels as high as 30% have recently been documented in legal cannabis grown for recreational use [76]. Additionally, ease of delivery methods such as cannabis vaping can increase its reach to younger groups.
According to the 2018 National Survey on Drug Use and Health, more than a third of young adults aged 18 to 25 (34.8%) were past year users of cannabis, or about 11.8 million young adults. A lower percentage of adults ages 26 years or older reported using cannabis in the past year (13.3%), compared to the young adult age group. However, the percentage of adults reporting use of cannabis in the past year was higher than had been reported in surveys conducted between 2002 and 2016. About 3.1 million people aged 12 or older used cannabis for the first time in the past 12 months, translating to about 8400 new cannabis users each day [74].
The main gaps in the literature are the lack of human studies on pre-gestational exposure to cannabis, as well as the lack of studies examining the transgenerational effect of cannabis exposure. Limitations in the body of literature examined in this review include limited statistical power from low sample sizes, limitations in exposure quantification in human studies, and differences in dosage, timing of exposure, and tissue and cell types analyzed for epigenetic endpoints. Human exposure to cannabis is complex due to different delivery methods, THC/CBD ratios, and timing of exposure during critical developmental periods (e.g., adolescence, pre-gestational, and prenatal). However, studies that incorporated mixed study designs that examined the effects of developmental cannabis exposure on both animals and humans, or that compared findings to other studies, found consistent epigenetic and functional gene changes between species and between studies [23,24,25, 28••, 55, 72••], which is rare in epigenetic studies. In addition, significant effects were observed in cannabis-exposed subjects in the majority of studies, despite low sample sizes. Yet, publication bias could be an important driver. The field would benefit from a large meta-analysis to increase power, particularly from human studies to uncover novel epigenetic biomarkers. The majority of experimental and epidemiological studies have examined differences in DNA methylation. Future studies should also incorporate the measurement of histone modifications, changes in ncRNA, and persistence over time in sperm, which could yield valuable information in transgenerational studies [77].
Cannabis consumption and mental health illness in young adults is increasing in the United States. Developmental cannabinoid exposure may increase the intergenerational risk of psychiatric disease through epigenetic mechanisms. These findings could be used by regulators and health communicators to inform consumers of potential risks associated with cannabis use during specific time points in the life course.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Bose J Key Substance Use and Mental Health Indicators in the United States: Results from the 2017 National Survey on Drug Use and Health. 2017:124.
Smart R, Caulkins JP, Kilmer B, Davenport S, Midgette G. Variation in cannabis potency and prices in a newly legal market: evidence from 30 million cannabis sales in Washington state: legal cannabis potency and price variation. Addiction. 2017;112(12):2167–77. https://doi.org/10.1111/add.13886.
DrugFacts: Nationwide Trends | National Institute on Drug Abuse (NIDA).
Marijuana Use in Adolescence. HHSgov. 2018.
Volkow ND, Han B, Compton WM, McCance-Katz EF. Self-reported medical and nonmedical cannabis use among pregnant women in the United States. JAMA. 2019;322(2):167–9. https://doi.org/10.1001/jama.2019.7982.
Compton WM, Han B, Jones CM, Blanco C, Hughes A. Marijuana use and use disorders in adults in the USA, 2002–14: analysis of annual cross-sectional surveys. Lancet Psychiatry. 2016;3(10):954–64. https://doi.org/10.1016/S2215-0366(16)30208-5.
Keyhani S, Steigerwald S, Ishida J, Vali M, Cerdá M, Hasin D, et al. Risks and benefits of marijuana Use: A National Survey of U.S. Adults. Ann Intern Med. 2018;169(5):282. https://doi.org/10.7326/M18-0810.
Atakan Z. Cannabis, a complex plant: different compounds and different effects on individuals. Ther Adv Psychopharmacol. 2012;2(6):241–54. https://doi.org/10.1177/2045125312457586.
Sharma P, Murthy P, Bharath MMS. Chemistry, metabolism, and toxicology of cannabis: clinical implications. Iran J Psychiatry. 2012;7(4):149–56.
Jutras-Aswad D, DiNieri JA, Harkany T, Hurd YL. Neurobiological consequences of maternal cannabis on human fetal development and its neuropsychiatric outcome. Eur Arch Psychiatry Clin Neurosci. 2009;259(7):395–412. https://doi.org/10.1007/s00406-009-0027-z.
Buckley NE, Hansson S, Harta G, Mezey E. Expression of the CB1 and CB2 receptor messenger RNAs during embryonic development in the rat. Neuroscience. 1998;82(4):1131–49. https://doi.org/10.1016/s0306-4522(97)00348-5.
Begbie J, Doherty P, Graham A. Cannabinoid receptor, CB1, expression follows neuronal differentiation in the early chick embryo. J Anat. 2004;205(3):213–8. https://doi.org/10.1111/j.0021-8782.2004.00325.x.
Psychoyos D, Vinod KY, Cao J, Hyson RL, Wlodarczyk B, He W, et al. Cannabinoid receptor 1 signaling in embryo neurodevelopment. Birth Defects Res B Dev Reprod Toxicol. 2012;95(2):137–50. https://doi.org/10.1002/bdrb.20348.
Wang X, Dow-Edwards D, Keller E, Hurd YL. Preferential limbic expression of the cannabinoid receptor mRNA in the human fetal brain. Neuroscience. 2003;118(3):681–94. https://doi.org/10.1016/S0306-4522(03)00020-4.
•• Innocenzi E, De Domenico E, Ciccarone F, Zampieri M, Rossi G, Cicconi R, et al. Paternal activation of CB 2 cannabinoid receptor impairs placental and embryonic growth via an epigenetic mechanism. Sci Rep. 2019;9(1):1–13. https://doi.org/10.1038/s41598-019-53579-3Demonstrated role of CBR2 agonist in inducing epigenetic alterations in male gametes that are retained in the placenta.
Rodríguez de Fonseca F, Ramos JA, Bonnin A, Fernández-Ruiz JJ. Presence of cannabinoid binding sites in the brain from early postnatal ages. Neuroreport. 1993;4(2):135–8. https://doi.org/10.1097/00001756-199302000-00005.
Heng L, Beverley JA, Steiner H, Tseng KY. Differential developmental trajectories for CB1 cannabinoid receptor expression in limbic/associative and sensorimotor cortical areas. Synapse. 2011;65(4):278–86. https://doi.org/10.1002/syn.20844.
Keimpema E, Mackie K, Harkany T. Molecular model of cannabis sensitivity in developing neuronal circuits. Trends Pharmacol Sci. 2011;32(9):551–61. https://doi.org/10.1016/j.tips.2011.05.004.
Twenge JM, Cooper AB, Joiner TE, Duffy ME, Binau SG. Age, period, and cohort trends in mood disorder indicators and suicide-related outcomes in a nationally representative dataset, 2005-2017. J Abnorm Psychol. 2019;128(3):185–99. https://doi.org/10.1037/abn0000410.
Morris CV, DiNieri JA, Szutorisz H, Hurd YL. Molecular mechanisms of maternal cannabis and cigarette use on human neurodevelopment: prenatal cannabis and cigarette molecular mechanisms. Eur J Neurosci. 2011;34(10):1574–83. https://doi.org/10.1111/j.1460-9568.2011.07884.x.
Chadwick B, Miller ML, Hurd YL. Cannabis use during adolescent development: susceptibility to psychiatric illness. Front Psychiatry. 2013;4. https://doi.org/10.3389/fpsyt.2013.00129.
Szutorisz H, Hurd YL. Epigenetic effects of cannabis exposure. Biol Psychiatry. 2016;79(7):586–94. https://doi.org/10.1016/j.biopsych.2015.09.014.
Szutorisz H, Egervári G, Sperry J, Carter JM, Hurd YL. Cross-generational THC exposure alters the developmental sensitivity of ventral and dorsal striatal gene expression in male and female offspring. Neurotoxicol Teratol. 2016;58:107–14. https://doi.org/10.1016/j.ntt.2016.05.005.
Szutorisz H, DiNieri JA, Sweet E, Egervari G, Michaelides M, Carter JM, et al. Parental THC exposure leads to compulsive heroin-seeking and altered striatal synaptic plasticity in the subsequent generation. Neuropsychopharmacol. 2014;39(6):1315–23. https://doi.org/10.1038/npp.2013.352.
Watson CT, Szutorisz H, Garg P, Martin Q, Landry JA, Sharp AJ, et al. Genome-wide DNA methylation profiling reveals epigenetic changes in the rat nucleus accumbens associated with cross-generational effects of adolescent THC exposure. Neuropsychopharmacol. 2015;40(13):2993–3005. https://doi.org/10.1038/npp.2015.155.
Levin ED, Hawkey AB, Hall BJ, Cauley M, Slade S, Yazdani E, et al. Paternal THC exposure in rats causes long-lasting neurobehavioral effects in the offspring. Neurotoxicol Teratol. 2019;74:106806. https://doi.org/10.1016/j.ntt.2019.04.003.
Szutorisz H, Hurd YL. High times for cannabis: epigenetic imprint and its legacy on brain and behavior. Neurosci Biobehav Rev. 2018;85:93–101. https://doi.org/10.1016/j.neubiorev.2017.05.011.
•• Murphy SK, Itchon-Ramos N, Visco Z, Huang Z, Grenier C, Schrott R, et al. Cannabinoid exposure and altered DNA methylation in rat and human sperm. Epigenetics. 2018;13(12):1208–21. https://doi.org/10.1080/15592294.2018.1554521Found correlations between THC exposure levels in human sperm and methylation of 177 genes, as well as substantial overlap in THC target genes in rat sperm and genes reported as having altered methylation in the brains of pre-gestationally exposed rats.
Reece AS, Hulse GK. Impacts of cannabinoid epigenetics on human development: reflections on Murphy et. al. ‘cannabinoid exposure and altered DNA methylation in rat and human sperm’ epigenetics 2018; 13: 1208–1221. Epigenetics. 2019;14(11):1041–56. https://doi.org/10.1080/15592294.2019.1633868.
Handy DE, Castro R, Loscalzo J. Epigenetic modifications: basic mechanisms and role in cardiovascular disease. Circulation. 2011;123(19):2145–56. https://doi.org/10.1161/CIRCULATIONAHA.110.956839.
Wen K-X, Miliç J, El-Khodor B, Dhana K, Nano J, Pulido T, et al. The role of DNA methylation and histone modifications in neurodegenerative diseases: a systematic review. PLoS One. 2016;11(12). https://doi.org/10.1371/journal.pone.0167201.
Paraskevopoulou MD, Hatzigeorgiou AG. Analyzing MiRNA–LncRNA Interactions. In: Feng Y, Zhang L, editors. Long Non-Coding RNAs: Methods and Protocols. Methods in Molecular Biology. New York: Springer; 2016. p. 271–86.
Reference GH. What are genomic imprinting and uniparental disomy? Genetics Home Reference.
O'Neill C. The epigenetics of embryo development. Anim Front. 2015;5(1):42–9. https://doi.org/10.2527/af.2015-0007.
von Meyenn F, Reik W. Forget the parents: epigenetic reprogramming in human germ cells. Cell. 2015;161(6):1248–51. https://doi.org/10.1016/j.cell.2015.05.039.
Gleason KA, Birnbaum SG, Shukla A, Ghose S. Susceptibility of the adolescent brain to cannabinoids: long-term hippocampal effects and relevance to schizophrenia. Transl Psychiatry. 2012;2(11):e199-e. https://doi.org/10.1038/tp.2012.122.
Tomasiewicz HC, Jacobs MM, Wilkinson MB, Wilson SP, Nestler EJ, Hurd YL. Proenkephalin mediates the enduring effects of adolescent cannabis exposure associated with adult opiate vulnerability. Biol Psychiatry. 2012;72(10):803–10. https://doi.org/10.1016/j.biopsych.2012.04.026.
Hollins SL, Zavitsanou K, Walker FR, Cairns MJ. Alteration of transcriptional networks in the entorhinal cortex after maternal immune activation and adolescent cannabinoid exposure. Brain Behav Immun. 2016;56:187–96. https://doi.org/10.1016/j.bbi.2016.02.021.
Hollins SL, Zavitsanou K, Walker FR, Cairns MJ. Alteration of imprinted Dlk1-Dio3 miRNA cluster expression in the entorhinal cortex induced by maternal immune activation and adolescent cannabinoid exposure. Transl Psychiatry. 2014;4(9):e452-e. https://doi.org/10.1038/tp.2014.99.
• Miller ML, Chadwick B, Dickstein DL, Purushothaman I, Egervari G, Rahman T, et al. Adolescent exposure to Δ9-tetrahydrocannabinol alters the transcriptional trajectory and dendritic architecture of prefrontal pyramidal neurons. Mol Psychiatry. 2019;24(4):588–600. https://doi.org/10.1038/s41380-018-0243-xFound differential expression of genes in brain tissue, which were implicated in neurodevelopment and psychiatric disorders, in rat adolescents exposed to THC.
•• Gerra MC, Jayanthi S, Manfredini M, Walther D, Schroeder J, Phillips KA, et al. Gene variants and educational attainment in cannabis use: mediating role of DNA methylation. Transl Psychiatry. 2018;8. https://doi.org/10.1038/s41398-017-0087-1DNA methylation higher in cannabis users, compared to controls, in exon 8 of DRD2 gene in peripheral whole blood of human subjects, which could underly reward deficit condition.
• Tomas-Roig J, Benito E, Agis-Balboa R, Piscitelli F, Hoyer-Fender S, Di Marzo V, et al. Chronic exposure to cannabinoids during adolescence causes long-lasting behavioral deficits in adult mice: Long-lasting WIN55212.2 effect. Addict Biol. 2017;22(6):1778–89. https://doi.org/10.1111/adb.12446Mice exposed to CBR1 agonist had hypermethylation of Rgs7 in the hippocampus, compared to controls, which could have implications for memory, motor control, vision, and reward behavior.
Dickson B, Mansfield C, Guiahi M, Allshouse AA, Borgelt LM, Sheeder J, et al. Recommendations from cannabis dispensaries about first-trimester Cannabis use. Obstet Gynecol. 2018;131(6):1031–8. https://doi.org/10.1097/AOG.0000000000002619.
Jaques SC, Kingsbury A, Henshcke P, Chomchai C, Clews S, Falconer J, et al. Cannabis, the pregnant woman and her child: weeding out the myths. J Perinatol. 2014;34(6):417–24. https://doi.org/10.1038/jp.2013.180.
Goldschmidt L, Day NL, Richardson GA. Effects of prenatal marijuana exposure on child behavior problems at age 10. Neurotoxicol Teratol. 2000;22(3):325–36. https://doi.org/10.1016/S0892-0362(00)00066-0.
Goldschmidt L, Richardson GA, Willford JA, Severtson SG, Day NL. School achievement in 14-year-old youths prenatally exposed to marijuana. Neurotoxicol Teratol. 2012;34(1):161–7. https://doi.org/10.1016/j.ntt.2011.08.009.
Noland JS, Singer LT, Short EJ, Minnes S, Arendt RE, Lester Kirchner H, et al. Prenatal drug exposure and selective attention in preschoolers. Neurotoxicol Teratol. 2005;27(3):429–38. https://doi.org/10.1016/j.ntt.2005.02.001.
Leech SL, Larkby CA, Day R, Day NL. Predictors and correlates of high levels of depression and anxiety symptoms among children at age 10. J Am Acad Child Adolesc Psychiatry. 2006;45(2):223–30. https://doi.org/10.1097/01.chi.0000184930.18552.4d.
Conner SN, Bedell V, Lipsey K, Macones GA, Cahill AG, Tuuli MG. Maternal marijuana use and adverse neonatal outcomes: a systematic review and meta-analysis. Obstet Gynecol. 2016;128(4):713–23. https://doi.org/10.1097/AOG.0000000000001649.
Leemaqz SY, Dekker GA, McCowan LM, Kenny LC, Myers JE, Simpson NAB, et al. Maternal marijuana use has independent effects on risk for spontaneous preterm birth but not other common late pregnancy complications. Reprod Toxicol. 2016;62:77–86. https://doi.org/10.1016/j.reprotox.2016.04.021.
Vargish GA, Pelkey KA, Yuan X, Chittajallu R, Collins D, Fang C, et al. Persistent inhibitory circuit defects and disrupted social behaviour following in utero exogenous cannabinoid exposure. Mol Psychiatry. 2017;22(1):56–67. https://doi.org/10.1038/mp.2016.17.
Ryan SA, Ammerman SD, O’Connor ME. Prevention CoSUA, Breastfeeding SO. Marijuana use during pregnancy and breastfeeding: implications for neonatal and childhood outcomes. Pediatrics. 2018;142(3). https://doi.org/10.1542/peds.2018-1889.
El Marroun H, Tiemeier H, Steegers EAP, Jaddoe VWV, Hofman A, Verhulst FC, et al. Intrauterine Cannabis exposure affects fetal growth trajectories: the generation R study. J Am Acad Child Adolesc Psychiatry. 2009;48(12):1173–81. https://doi.org/10.1097/CHI.0b013e3181bfa8ee.
Gray TR, Eiden RD, Leonard KE, Connors GJ, Shisler S, Huestis MA. Identifying prenatal Cannabis exposure and effects of concurrent tobacco exposure on neonatal growth. Clin Chem. 2010;56(9):1442–50. https://doi.org/10.1373/clinchem.2010.147876.
DiNieri JA, Wang X, Szutorisz H, Spano SM, Kaur J, Casaccia P, et al. Maternal Cannabis use alters ventral striatal dopamine D2 gene regulation in the offspring. Biol Psychiatry. 2011;70(8):763–9. https://doi.org/10.1016/j.biopsych.2011.06.027.
Zahm DS. An integrative neuroanatomical perspective on some subcortical substrates of adaptive responding with emphasis on the nucleus accumbens. Neurosci Biobehav Rev. 2000;24(1):85–105. https://doi.org/10.1016/S0149-7634(99)00065-2.
Zhu Z, Wang G, Ma K, Cui S, Wang J-H. GABAergic neurons in nucleus accumbens are correlated to resilience and vulnerability to chronic stress for major depression. Oncotarget. 2017;8(22):35933–45. https://doi.org/10.18632/oncotarget.16411.
Wang X, Dow-Edwards D, Anderson V, Minkoff H, Hurd YL. In utero marijuana exposure associated with abnormal amygdala dopamine D2 gene expression in the human fetus. Biol Psychiatry. 2004;56(12):909–15. https://doi.org/10.1016/j.biopsych.2004.10.015.
Wang X, Dow-Edwards D, Anderson V, Minkoff H, Hurd YL. Discrete opioid gene expression impairment in the human fetal brain associated with maternal marijuana use. Pharmacogenomics J. 2006;6(4):255–64. https://doi.org/10.1038/sj.tpj.6500375.
Ross EJ, Graham DL, Money KM, Stanwood GD. Developmental consequences of fetal exposure to drugs: what we know and what we still must learn. Neuropsychopharmacol. 2015;40(1):61–87. https://doi.org/10.1038/npp.2014.147.
Spano MS, Ellgren M, Wang X, Hurd YL. Prenatal cannabis exposure increases heroin seeking with allostatic changes in limbic enkephalin systems in adulthood. Biol Psychiatry. 2007;61(4):554–63. https://doi.org/10.1016/j.biopsych.2006.03.073.
• Fransquet PD, Hutchinson D, Olsson CA, Allsop S, Elliott EJ, Burns L, et al. Cannabis use by women during pregnancy does not influence infant DNA methylation of the dopamine receptor DRD4. Am J Drug Alcohol Abuse. 2017;43(6):671–7. https://doi.org/10.1080/00952990.2017.1314488DNA methylation of DRD4 was not influenced by human gestational cannabis use, but null findings could be due to use of buccal cells and not neuronal cells.
Wong CCY, Caspi A, Williams B, Craig IW, Houts R, Ambler A, et al. A longitudinal study of epigenetic variation in twins. Epigenetics. 2010;5(6):516–26. https://doi.org/10.4161/epi.5.6.12226.
Mallard TT, Doorley J, Esposito-Smythers CL, McGeary JE. Dopamine D4 receptor VNTR polymorphism associated with greater risk for substance abuse among adolescents with disruptive behavior disorders: preliminary results. Am J Addict. 2016;25(1):56–61. https://doi.org/10.1111/ajad.12320.
• Ibn Lahmar Andaloussi Z, Taghzouti K, Abboussi O. Behavioural and epigenetic effects of paternal exposure to cannabinoids during adolescence on offspring vulnerability to stress. Int J Dev Neurosci. 2019;72:48–54. https://doi.org/10.1016/j.ijdevneu.2018.11.007Pre-gestational exposure to cannbinoids during adolescence can promote stress-induced anxiety and alter the epigenetic programming of offspring in rats.
Jjingo D, Conley AB, Yi SV, Lunyak VV, Jordan IK. On the presence and role of human gene-body DNA methylation. Oncotarget. 2012;3(4):462–74. https://doi.org/10.18632/oncotarget.497.
GeneCards - Human Genes | Gene Database | Gene Search.
Vassoler FM, Johnson NL, Byrnes EM. Female adolescent exposure to cannabinoids causes transgenerational effects on morphine sensitization in female offspring in the absence of in utero exposure. J Psychopharmacol. 2013;27(11):1015–22. https://doi.org/10.1177/0269881113503504.
Rasmussen AH, Rasmussen HB, Silahtaroglu A. The DLGAP family: neuronal expression, function and role in brain disorders. Mol Brain. 2017;10:43. https://doi.org/10.1186/s13041-017-0324-9.
Chien W-H, Gau SS-F, Liao H-M, Chiu Y-N, Wu Y-Y, Huang Y-S, et al. Deep exon resequencing of DLGAP2 as a candidate gene of autism spectrum disorders. Mol Autism. 2013;4:26. https://doi.org/10.1186/2040-2392-4-26.
Soler J, Fañanás L, Parellada M, Krebs M-O, Rouleau GA, Fatjó-Vilas M. Genetic variability in scaffolding proteins and risk for schizophrenia and autism-spectrum disorders: a systematic review. J Psychiatry Neurosci. 2018;43(4):170066–244. https://doi.org/10.1503/jpn.170066.
•• Schrott R, Acharya K, Itchon-Ramos N, Hawkey AB, Pippen E, Mitchell JT, et al. Cannabis use is associated with potentially heritable widespread changes in autism candidate gene DLGAP2 DNA methylation in sperm. Epigenetics. 2019;0(0):1–13. https://doi.org/10.1080/15592294.2019.1656158Identified region of Dlgap2, which is strongly implicated in the development of autism, with differential methylation in eight CpG sites in THC exposed rat sperm, which was consistent in human sperm.
Tang Walfred WC, Dietmann S, Irie N, Leitch Harry G, Floros Vasileios I, Bradshaw Charles R, et al. A unique gene regulatory network resets the human germline epigenome for development. Cell. 2015;161(6):1453–67. https://doi.org/10.1016/j.cell.2015.04.053.
Lipari RN. Key Substance Use and Mental Health Indicators in the United States: Results from the 2018 National Survey on Drug Use and Health. 2018:82.
ElSohly MA, Mehmedic Z, Foster S, Gon C, Chandra S, Church JC. Changes in Cannabis potency over the last 2 decades (1995–2014): analysis of current data in the United States. Biol Psychiatry. 2016;79(7):613–9. https://doi.org/10.1016/j.biopsych.2016.01.004.
Grant KS, Petroff R, Isoherranen N, Stella N, Burbacher TM. Cannabis use during pregnancy: pharmacokinetics and effects on child development. Pharmacol Ther. 2018;182:133–51. https://doi.org/10.1016/j.pharmthera.2017.08.014.
Maamar MB, Sadler-Riggleman I, Beck D, Skinner MK. Epigenetic Transgenerational inheritance of altered sperm histone retention sites. Sci Rep. 2018;8(1):1–10. https://doi.org/10.1038/s41598-018-23612-y.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
AS and AC report grants and non-financial support from Office of Environmental Health Hazard Assessment (OEHHA) of the California Environmental Protection Agency, during the conduct of the study. MS and FK report no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Disclaimer
The views expressed are those of the authors and do not necessarily represent those of the Office of Environmental Health Hazard Assessment (OEHHA), the California Environmental Protection Agency, or the State of California.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Topical Collection on Environmental Epigenetics
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Smith, A., Kaufman, F., Sandy, M.S. et al. Cannabis Exposure During Critical Windows of Development: Epigenetic and Molecular Pathways Implicated in Neuropsychiatric Disease. Curr Envir Health Rpt 7, 325–342 (2020). https://doi.org/10.1007/s40572-020-00275-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-020-00275-4