Abstract
Research on active smoking and secondhand smoke exposure has led to policy changes to protect individuals from the adverse health impacts of tobacco smoke. Despite the extensive literature on tobacco, only recently has there been recognition that long-lived tobacco smoke components (known as “thirdhand smoke” or THS) in indoor environments where smoking has taken place may have adverse health consequences. This paper describes THS and addresses the challenges of limiting exposure to THS in vulnerable populations (e.g., nonsmokers and young children). We conducted a limited survey of key stakeholders in the Los Angeles area to better understand approaches to address THS in the real estate and automobile industries. Most respondents indicated concerns about past smoking for property value and reported using various techniques to eliminate THS. We consider examples of other pollutants as case studies, including radon, asbestos, and lead, to help frame policy directions for THS. Based on the information collected from stakeholders and the case studies, we offer policy approaches to managing THS.
Similar content being viewed by others
Introduction
The year 2014 marked the 50th Anniversary of the 1964 Report of the Advisory Committee to the Surgeon General, which reached the powerful conclusion that active smoking causes lung cancer in men. Since this initial report, thousands of studies have provided evidence documenting that smoking causes various cancers, heart disease, lung disease, and other diseases throughout the body and characterizing the mechanisms by which tobacco smoke causes these adverse effects [1]. Nearly three decades have also passed since the US Surgeon General and other scientific authorities concluded that exposure to secondhand tobacco smoke (SHS) causes disease in nonsmokers, including lung cancer in adults [2–4]. These scientific conclusions have led to a broad range of policy actions and public health programs in the USA and worldwide aimed at reducing smoking prevalence and exposure to SHS in public places. Consequently, the tobacco-related disease burden has begun to decrease in some countries, including the USA, with effective tobacco control policies in place [1].
Despite the plethora of data on the toxic contaminants contained in tobacco smoke and their impact on health, only recently has there been recognition that exposure to long-lived tobacco smoke components in indoor environments where smoking has taken place may result in possible adverse health consequences. The mixture of chemicals and their metabolic by-products that remain on surfaces after smoking has taken place is now referred to as thirdhand smoke (THS). In a 2011 review, Matt and colleagues described THS as: “THS consists of residual tobacco smoke pollutants that remain on surfaces and in dust after tobacco has been smoked, are reemitted into the gas phase, or react with oxidants and other compounds in the environment to yield secondary pollutants” [5•]. In places where there is active smoking, THS exposure is an inescapable consequence of the generation of SHS. The initial research evidence on THS shows that it is present in environments where smoking no longer takes place, persisting in materials and on surfaces. Thus, nonsmokers, both adults and children, may be unknowingly and involuntarily exposed to THS in environments where there was smoking in the past, such as rental cars, hotel rooms, and rental properties.
In an increasingly smoke-free era, there is a societal expectation that nonsmokers should not be involuntarily exposed to tobacco smoke and its components. This paper addresses the challenge of limiting exposure to long-lived tobacco components, or THS, in indoor environments. We begin by describing THS and its exposure pathways and provide findings from limited surveys of key stakeholder groups and their approaches to addressing THS. We then consider other case studies of controlling indoor environmental exposures—asbestos, lead, and radon—that provide “lessons learned” for THS. We conclude by offering a policy framework for developing a broad strategy for limiting exposure to THS.
Exposure to THS and the Risks of Exposure
Similar to SHS, THS is composed of numerous chemicals, many of which are known carcinogens, irritants, and mutagens [5•, 6]. Over time after smoking has taken place, THS components evolve through various reactions and can interact with other chemicals and compounds in the environment resulting in changes to chemical structure and in generation of secondary toxicants [7••, 8–11]. The result is off-gassing of different and potentially more toxic compounds. The sorption-desorption mechanism of THS provides more opportunities for nonsmokers to be exposed to toxicants and known carcinogens. Unlike active smoking and exposure to SHS for which the route of exposure is inhalation, there are several exposure pathways for THS as discussed in more detail below. THS is present on surfaces (e.g., walls, counters, tables, and desks), on upholstery (e.g., couches, bedding, and curtains), and on smokers themselves (e.g., their clothes, hair, and hands). THS is able to penetrate surfaces and remain in the environment for extended periods of time and can also be aerosolized and dispersed through air ventilation systems, wall and floor cracks, and plumbing or electrical routes in multi-house units [5•].
In their 2011 review, Matt and colleagues addressed the composition of THS and its relationship to SHS [5•]. Immediately after there has been smoking within a space, SHS and THS are both present, but without further smoking, THS becomes predominant. Tobacco smoke components are present, but as implied by the THS definition, THS is a dynamic mixture with toxic components that may contribute to disease risk through several mechanisms. Chemical transformations for some compounds have been described; for example, there are ozone-driven reactions with volatile organic compounds of THS, including nicotine [7••].
The THS mixture does include compounds that are considered as contributing to the health risks associated with active smoking and exposure to SHS. Various carcinogens have been identified in THS, as have nicotine and nicotine metabolites. Tobacco-specific nitrosamines, known carcinogens, have also been identified in house dust samples [12]. Nicotine absorbed on surfaces has been shown to react with other compounds in the environment to form secondary toxicants such as 1-(N-methyl-N-nitrosamino)-1-(2-pyridinyl)-4-butanal (NNA), 4-(methylnitrosamino-1-(3-pyridinyl)-1-butanone (NNK), and N-nitrosonornicotine (NNN) [6, 7••]. Not surprisingly, given its composition, THS has been shown to damage DNA. An in vitro system with human HepG2 cells and THS, generated both acutely and chronically, showed significant DNA strand breaks compared to controls [10]. The exposure to chronic THS resulted in more DNA damage than the acutely generated exposure material [10].
Determining individual exposure to THS, and consequent relative risks, is scientifically challenging. This is, in part, due to the difficulty in separating THS exposure from potential SHS exposure. Scientists are currently carrying out research to develop a THS-specific biological marker—i.e., a compound present in THS, but not SHS. Moreover, it has been challenging to establish protocols to measure exposure within individuals without exposing study participants to known carcinogens.
Pathways of Exposure and Vulnerable Populations
Three pathways of exposure exist for THS: dermal, ingestion, and/or inhalation. Individuals may incur exposures through these pathways in their homes, in public areas, at hotels, and if they rent or purchase property owned previously by smokers (e.g., homes or used cars).
Dermal
Individuals may be exposed via dermal contact with surfaces contaminated by THS. Toxicants in THS deposit in upholstery, walls, countertops, and other surfaces where smoking has taken place, including the clothing of smokers. In a study published in 2013, Quintana and colleagues reviewed multiple studies where surface wipe samples were taken from various environments including homes of smokers with and without bans, homes of nonsmokers, hotel rooms, and used cars. The wipe samples were collected from surfaces such as doors, tables, window panels, kitchen cabinets, and bed frames to understand deposition of toxicant in different areas of the environment [13••]. Findings from this study indicate that nicotine levels in the surface wipes differed significantly between the various environments, the highest levels reported in homes of smokers and hotels where smoking was permitted (Fig. 1). Renters and used car owners are also at risk of dermal exposure if homes and cars have been occupied or owned previously by smokers. Dermal exposure may or may not be detectable. While the smell of cigarette smoke is apparent in homes and cars of heavy smokers or soon after smoking, over time, the smell may be masked or no longer apparent, leaving those in the environment unaware that surfaces harbor toxicants. This may be especially true for renters and those purchasing used cars. Research has not yet established which THS components will be absorbed through the skin; nicotine, of course, can be absorbed through the skin.
Levels of surface wipe nicotine between varying environments and smoking behaviors. Source: Quintana et al., Wipe Sampling for Nicotine as a Marker of Thirdhand Tobacco Smoke Contamination on Surfaces in Homes, Cars, and Hotels, Nicotine and Tobacco Research: Official Journal of the Society for Research on Nicotine and Tobacco, 2013, 15 (9), p 1555–1563, by permission of Oxford University Press [13••]
Ingestion
One potential pathway of THS exposure is through ingestion, particularly for infants and young children exposed to contaminated surfaces. Infants are at a higher risk for THS exposure through ingestion because of hand-to-mouth behavior, involving touching contaminated surfaces and then putting their hands or other contaminated objects in their mouth (e.g., pacifiers, toys, and blankets). The Environmental Protection Agency (EPA) reported ingestion of indoor dust as a pathway of exposure to pollutants such as lead, nicotine, pesticides, brominated flame retardants, phthalates, and perfluorinated chemicals for young children [14]. Therefore, house dust containing THS components and secondary toxicants is a concern for children living in homes where past smoking or current smoking has taken place.
Inhalation
Individuals are also at risk for THS exposure through inhalation of volatile components. In addition to being deposited on surfaces, THS may be trapped in air ventilation systems and travel through ducts or cracks and openings in homes. Additionally, through surface sorption and desorption, THS components enter and leave the air and can be inhaled. Additionally, while in the air, reactions, e.g., with ozone, may create gas-phase by-products [7••]. A chamber experiment examined the interaction of nicotine with atmospheric ozone and found that gas-phase oxidation by-products were produced (e.g., N-methyl formamide, nicotinaldehyde or 3-pyridinecar-bxaldehyde, cotinine, and formaldehyde) [9]. Volatile by-products and other secondary toxicants produced well after smoking has taken place and present in the air can irritate the eyes, skin, and upper respiratory system [5•].
Vulnerable Populations
Due to widespread success in eliminating smoking in workplaces and other public places, exposure to THS has decreased among the general population [1]. However, key locations remain where the public is exposed to significant levels of THS. Clearly, locations where smoking is permitted contain THS. Such locations of concern may include private homes, multi-unit housing, hotels, and casinos. THS is also a potential issue resulting from the transfer of occupancy or ownership of THS-exposed property, including real estate (rented and purchased) and automobiles (rented and pre-owned).
Given the present smoking patterns, those with lower household incomes are the most likely to be exposed to higher levels of THS over longer periods of time. This exposure profile reflects not only the demographics of smoking but also the disproportionate residence in shared housing as well as greater ownership of pre-owned cars among those with lower incomes.
Infants and small children are also likely to be more exposed and possibly at greater risk for health effects than older children and adults because they are more likely to spend extended periods of time on exposed surfaces (e.g., carpets and blankets) than older children and adults and are prone to place exposed items in their mouths (e.g., pacifiers, their hands, and blankets) [14].
Stakeholder Concerns About THS
The emergence of THS as an exposure with potential risks to the population has broad health implications for the population in general and economic implications for several sectors. As described above, THS is a potential issue related to property transfer, including home sales, property rentals, and the purchase of a used vehicle. To gain an understanding of the current level of concern about THS in these sectors, we conducted a survey of a small number of professionals engaged within each of these sectors. The methods largely drew on convenience sampling from Craig’s list and other sources to acquire a sufficient number of respondents to gain a preliminary picture of concerns about THS and approaches to address them. Questions were developed for this purpose, and after a pilot test, responses were collected by phone or in-person interview. The data were collected in 2013.
Realtors were asked about their business, level of involvement in selling homes previously owned by smokers, beliefs about the impact of smoking on home sales, disclosure issues, and cleaning practices. Table 1 shows the findings for realtors and car dealers. Figure 2 presents findings for disclosure practices of previous smoking habits in the properties (homes and used cars). Over half of realtors surveyed (58 %) serve the San Gabriel/San Fernando Valley areas in Los Angeles. Seventy-four percent (74 %) of respondents estimated that up to 20 % of their business involved homes of previous smokers. A majority of realtors (73 %) agreed that past smoking was a concern for buyers, and more than half concur that smoking has an impact on both home value and sale price.
While half of the realtor respondents considered past smoking an issue that discouraged purchasing a contaminated home, they noted that buyers with children were especially discouraged (67 %). Most responded that buyers having children and buyers’ personal smoking habits played a role in how the buyers think about homes for sale. Realtors infrequently ask sellers about smoking in the home, and most feel that sellers never or rarely voluntarily disclose this information (85 and 74 %, respectively). Our data show that from the realtors’ perspective, previous smoking in a home has an impact on real estate transactions. Realtors are aware of the negative effect that past smoking in a home has on property value. When asked about support for a mandatory disclosure of smoking habits in home sales, the majority (59 %) were supportive of this idea; however, most were reluctant to support a mandatory cleaning for smoke smell or residue as a condition for home sales (70 %). While most did not support the idea of a mandatory cleaning, all realtors surveyed recommend carpet cleaning and painting as part of the preparation of a home for sale. Other methods usually recommended include new carpet installation (85 % of respondents), surface cleaning (85 % of respondents), and HEPA vacuuming (74 % of respondents).
As with realtors, car dealers also viewed past smoking in used cars as a problem. All dealers surveyed expressed some level of concern about past smoking, agreeing that smoking in a car affects its value and the time it takes to sell the car (90 %). According to the dealers, buyers are reluctant to buy a car owned by a smoker, whether or not they have children (83 and 85 %, respectively). Unlike realtors, the majority of car dealers (60 %) reported buyers as sometimes or often demanding to know the smoking habits of former owners. The majority (68 %) of dealers reported that evidence of smoking is masked by the seller or dealer, and cars are purchased without knowledge of the smoking status of previous owners (75 %). While all respondents felt that past smoking had an impact on used car sales, less than half of respondents support mandatory disclosure of past smoking in cars and mandatory cleaning of smoke smell or residue as a condition of car sales (45 and 47 %, respectively). Most dealers have cleaning methods that they recommend to prepare cars for sale. Eighty percent or more of respondents recommended vacuuming, upholstery cleaning, surface cleaning (e.g., dashboard and console), and ozone treatment.
Potential Models for Control: Lessons from Radon, Lead, and Asbestos
While the health risks of THS are yet to be characterized, there exist multiple potential models for its management based on experiences with other environmental contaminants, including radon, lead, and asbestos. The EPA and other agencies provide guidance and regulations for these agents that are relevant to THS.
Radon
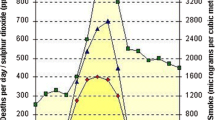
Radon is a colorless, odorless, naturally occurring gas that results from the decay of naturally occurring uranium in the soil and is a known cause of lung cancer. It is present in soil gas and enters homes and other structures through foundations, crawl spaces, and openings in basements. Studies of radon-exposed underground miners show a clear excess of lung cancer and a risk that increases with cumulative exposure [15]. Epidemiological studies in the general population confirm that exposures in homes also increase lung cancer risk [15]. Evidence indicates that the risk relationship for lung cancer and radon exposure is linear and without a threshold [15]. Thus, any exposure conveys some risk.
Radon is ubiquitous in homes and some have levels as high as those in mines [15]. Because exposure to radon is unavoidable and it causes lung cancer at any level, the EPA estimates that indoor radon is the second leading cause of lung cancer in the USA [16]. The skewed shape of the distribution of indoor radon concentrations makes clear the challenge of control of indoor radon exposure (Fig. 3); there is a need to identify those homes in the tail of the distribution with extremely high levels and to also shift the whole distribution to the left as much as feasible, since most population exposure takes place at the lower concentrations, as measured in most homes.
Distribution of radon in US homes. Source: National Research Council, Health Effects of Exposure to Radon, BEIR VI, 1999 [15]. Reprinted with permission from the National Academies Press, Copyright 1999, National Academy of Sciences
The problem of indoor radon was first recognized in the 1950s in Europe but did not receive wide recognition in the USA until 1984 when a few homes were found to have concentrations as high as those in underground uranium mines, and surveys showed that radon was universally present in homes [15]. Lacking direct regulatory authority, the EPA has followed a strategy of public education concerning the risks of radon, voluntary testing of homes to determine the concentration of indoor radon using certified contractors, promulgation of an action guideline value above which mitigation should be considered, and development of mitigation strategies for existing and new homes. This overall strategy is embodied in its “A Citizen’s Guide to Radon” and guidance for specific sectors [17]. At the state level, particularly in those states with documentation that indoor radon is a concern, more proactive policies have been implemented, including requiring radon testing at the time of real estate transactions and mitigation if needed. Many states also require disclosure of any radon problem as part of a real estate transaction.
With reference to THS, there are several applicable “lessons learned” from the radon story related to the need for public education, the ability to measure the specific contaminant of concern, and the availability of approaches for mitigation. Additionally, real estate transactions have become a critical element of the radon control strategy. While strong guidelines are in place by the EPA regarding indoor radon, there are no federal laws that require testing or disclosure of radon hazards. With help from the EPA, many states have required disclosure of radon hazards as part of real estate transactions. States such as Illinois require sellers to provide the purchaser with a pamphlet on radon hazards and a written disclosure form, much as is done for lead. The EPA’s “A Citizen’s Guide to Radon” promotes the testing of homes (i.e., using either a short-term or long-term test) for indoor radon and following simple and inexpensive mitigation techniques if levels greater than the guideline value are present in the home. In a 2005 Health Advisory, the US Surgeon General urged the public to test their homes and follow recommendations to lower the risks. Public awareness has been successfully used to encourage homeowners to test and mitigate when needed. Radon concentrations can be drastically reduced using ventilation techniques for basements and below foundations. The Indoor Radon Abatement Act, passed in 1988, supported states in encouraging homeowners to test their homes, fix the problem, and build or renovate with new radon-resistant materials [18]. It was through this act that the EPA’s “A Citizen’s Guide to Radon” was developed as well as establishing state programs, model construction standards, and creating training centers. Since the 1980s, radon has been included in other federal policies to regulate radon emissions in air and water. Most recently, in 2011 the federal government published the “Federal Radon Action Plan” with the intent to reduce radon levels in homes and buildings by using awareness campaigns and allotting funding to test/fix homes and use radon-resistant materials for new building and remodeling [19].
Lead
Lead is a long-studied metal that harms workers and the general population, particularly infants and children. Its hazards for children have been well documented through epidemiological studies showing that lead exposure adversely affects neuropsychological development [20]. Over time, adverse effects on children have been demonstrated at progressively lower levels, and recommendations for acceptable blood lead levels by the Centers for Disease Control and Prevention have dropped, parallel with the emerging findings (Table 2) [21–23]. Children may be exposed to lead through atmospheric emissions from smelters and other industrial sources, from lead-containing paints, from secondhand smoke, and previously from use of leaded gasoline [24, 25].
A major use prior to the 1980s was in lead-based paint, now one of the predominant sources most easily accessible to children. Exposure to deteriorated and flaking lead-based paint and dust during renovations poses a major risk for children, particularly those in poorly maintained urban housing. Children are particularly vulnerable because they tend to put their hands in their mouth more often and may eat the flaking paint off the walls. Additionally, pica, a disorder where individuals eat substances that are not food (e.g., paint, paper, soil, sand, and clay), is especially problematic if there is lead-based paint in the home. Pica is commonly diagnosed in young children. Ingestion of flaking paint can lead to high levels of lead in the body and lead poisoning [26].
There is also evidence suggesting that SHS is a source of lead exposure among children [24, 25]. This is not a surprise as lead is one of the metals contained in tobacco and smokers are known to have higher lead levels than nonsmokers. In children, lead levels increase with the number of smokers living in the home, and there is also a relatively strong positive relationship between lead and serum cotinine concentrations [24]. Little is known, however, about the potential contribution of THS to lead exposure through children’s hand-to-mouth behavior. It is, however, well established that lead concentrations in house dust are markedly higher in houses with one or more smokers, even after adjustment for markers of socioeconomic status [24].
With regard to addressing THS, federal and state policy pertaining to lead has been successful in reducing lead exposure and childhood lead poisoning, and these policies offer a well-established model for addressing an environmental toxicant. Laws have accomplished a large drop in lead poisoning cases and have increased the public’s awareness, making it possible for people to know the risks and mitigate when needed. As with THS, children are most at risk for exposure by the ingestion pathway. Many laws have been enacted to protect people from the effects of lead. Among those is the 1992 Residential Lead-Based Paint Hazard Reduction Act, known as Title X, which required all states to have a disclosure of lead hazards in homes built before 1978 [27]. While the law does not require testing for lead in private homes, the disclosure in real estate requires sellers to give the purchaser a 10-day grace period to perform his/her own lead testing. The seller or real estate agent is required to provide the brochure “Protect Your Family from Lead in Your Home” along with the disclosure to the purchaser before a contract is signed. This law applies to lessors as well, where disclosure and the brochure information are required prior to signing a lease.
There has been substantial litigation against the manufacturers of lead paint, but with little success. In the 1990s states such as Rhode Island, Wisconsin, Ohio, Missouri, New Jersey, and California filed lawsuits against lead manufacturers and the Lead Industries Association (Rhode Island vs. Lead Industries, City of Milwaukee vs. NL Industries, City of Toledo vs. Sherwin-Williams, City of St. Louis vs. Benjamin Moore & Co., In re: Lead Paint Litigation, and California vs. Atlantic Richfield Co., respectively) [28–33]. States sought monetary compensation to provide abatement programs and care for children affected by lead poisoning. Most courts ruled against the states; however, a recent ruling by Judge James Kleinberg in 2013 in the California vs. Atlantic Richfield Co. case upheld the plaintiffs’ case and ordered three lead manufacturers to pay $1.1 billion for abatement programs.
For lead, like radon, there is a specific compound that can be measured in the environment, reference measurement methods exist, and exposure biomarkers are available. National laws exist and housing sales offer a time point for measurement and mitigation. There are also educational materials.
Asbestos
Asbestos refers to a group of fibrous silicate minerals that occur naturally in the soil [34]. The fibers are heat resistant and flexible and consequently have been used widely in numerous products including insulation, cement, and other construction materials. Epidemiological and experimental research shows that asbestos causes cancer, most notably mesothelioma and lung cancer, and nonmalignant respiratory diseases [35, 36]. Mesothelioma is a rare form of cancer (developing in the lining of the lung or lining of other organs where mesothelial cells are found) that is almost exclusively caused by asbestos exposure. While the majority of lung cancer is caused by tobacco use, exposure to asbestos has been linked to lung cancer. Studies have shown that there is a dose-response relationship, such that longer exposure to asbestos increases the risk of lung cancer [36].
Laws are in place to regulate—at both federal and state levels—the use of asbestos in products. As early as 1973, the government enacted national emission standards for asbestos through the Clean Air Act (section 112) [37]. The asbestos national emission standards were followed by regulation of asbestos in drinking water. In 1974 the EPA was asked to set a maximum contamination level goal (MCGL) for asbestos in drinking water, where no adverse health effects were likely to occur. The MCGL for asbestos was set at seven million fibers per liter (MFL) by the Safe Drinking Water Act [38]. Regulation regarding asbestos exposure in the workplace is set by the Occupational Safety and Health Administration (OSHA) and the Mine Safety and Health Administration (MSHA) with policies that set limits for exposure as well as regulations on proper respirator equipment and protective wear, reporting and monitoring standards, and rules on disclosure to employees concerning exposure levels. Occupational exposure places individuals at higher risk for inhalation and disease; however, building occupants exposed to lower levels of asbestos are also at risk for disease. Compared to health risks due to radon or SHS, asbestos poses a low risk to the general building occupant, yet federal and state actions have been taken to ensure the safety of the population.
In the 1980s asbestos abatement began in schools under the Asbestos Hazard Emergency Response Act (AHERA) of 1986 (Title II of the Toxic Substances Control Act). AHERA requires elementary and secondary schools (both private and public) to inspect all school buildings for asbestos and asbestos-containing materials (ACM) and prepare management plans to reduce or prevent asbestos exposure and risks [39]. Since inspection and abatement procedures can only be done by professionals, the act also required training to accredit asbestos inspectors. To promulgate this regulation, the EPA enforced the Asbestos-Containing Materials in Schools Rule (1987), which outlined the requirements to meet the AHERA policy [40]. To support and encourage asbestos abatement, the Asbestos School Hazard Abatement and Reauthorization Act of 1990 was set in place [41]. This act extended the funding for asbestos abatement in schools (loans and grant to carry out mitigation) and expanded requirements to include all public and commercial buildings in addition to schools. At the state level, multiple states such as California and Maine have adopted statutes that require the disclosure of the presence and/or removal of asbestos [42, 43]. Testing for asbestos is not required in residential property; however, at the national level, the Asbestos National Emission Standards for Hazardous Air Pollutants (NESHAP) requires workers to follow specific work practices for asbestos removal during demolition and renovation of all buildings excluding residential property that have four or less units, and at the state level, regulations on proper removal and waste management are in place (e.g., CA asbestos waste is regulated by local, state, and federal agencies).
Conclusions and the Way Forward
Policy approaches for lead, asbestos, and radon provide a potential foundation for models to address THS. Each of the case studies above incorporated measurement activities to clearly identify and quantify the relevant toxicants, as well as to establish risk profiles, emphasized information dissemination to the public, and initiated policy action at multiple levels of governance to abate exposure, ranging from voluntary testing (radon) to mandatory disclosures (lead).
The feasibility of moving forward with similar policies and regulations to reduce THS will require additional research and policy innovation. The concept of THS is relatively new, although the surface deposition of tobacco smoke components has long been recognized. For educating the public about the potential importance of THS and motivating mitigation, better understanding of the health consequences is needed, along with the development of markers that can support intervention strategies. Proven mitigation methods are also needed. Thus, we call for further research while acknowledging that there is already an enormous body of evidence on active smoking and SHS that is relevant to THS.
The 2011 commentary by Matt and colleagues offered a broad, interdisciplinary research agenda [5•]. It covered all facets of the THS issue, including the chemistry of THS; exposure assessment; toxicology and health effects; knowledge, attitudes, and behavior; and tobacco control policies. To this comprehensive list, we add the development and evaluation of proper cleaning methods that remove smoke residue without reemission and new chemical reactions for the key exposure microenvironments, such as homes and automobiles. In terms of motivating policy action and awareness, we suggest that exposure assessment research would have immediate utility as a way to motivate action and to target the most critical pathways and populations. We anticipate, for example, that exposures of infants and young children through contaminated furnishings and carpet may be significant. As for lead, the demonstration of childhood exposure to a potentially hazardous agent may prompt action.
The three case studies each involved an agent that can be measured and its presence confirmed. Mitigation strategies have been initiated with the confirmation that the agent was present (lead and asbestos) or at a sufficiently high concentration (radon). Various tobacco smoke components can be measured in house dust from the homes of smokers and even of users of smokeless tobacco [44]; wipe sampling for nicotine is also a sensitive marker of THS [13••]. Jacob and colleagues (2013) have proposed nicotelline, which is present in tobacco smoke, as a potentially useful marker of particulate matter from tobacco smoking [45]. Thus, there are a number of potential markers that might be used in protocols for THS identification and mitigation. Research is needed to further explore the sensitivity and specificity of the various compounds.
Further research on perceptions, knowledge, attitudes, and beliefs would also be helpful, particularly if data were obtained for groups most likely to be heavily exposed to THS. Our preliminary research also indicates a need for further information gathering from key stakeholder groups, including the real estate and vehicle sales industries. When an appropriate suite of markers is available, pragmatic investigation will be needed on mitigation approaches. While our research did not show strong support for mandatory disclosure or mitigation, other models outlined above using public education and voluntary testing seem potentially feasible.
While more scientific research is needed to determine the relative risk of THS exposure in various environments and among different populations, allowing for further targeting of policy interventions, there are sufficient existing data to observe the precautionary principle in public health and immediately undertake efforts to limit exposures. As has been the case for SHS policy, THS smoke policy is likely to be initiated at the state and local levels. One key lesson is the importance of public awareness campaigns such as those in place for radon to help individuals understand the risks of THS. Requirements such as informational brochures to buyers involved in real estate transactions could be adopted and expanded to other relevant transactions, including used cars.
Consumers should have the right to be made aware of their potential exposure to THS when renting or purchasing property. Measures could include adding disclosures to real estate transactions, hotel stays, car rentals, and car sales. In addition to increased public awareness campaigns and information dissemination, various forms of disclosure regulations (voluntary or mandated) in real estate and vehicle ownership transactions could increase awareness and allow the public to identify the presence of THS and demand mitigation of the problem.
The most effective way to stop exposure to THS is through the extension of indoor smoking bans to those remaining outposts, including multi-unit housing, hotels, and casinos. In places where smoking has previously taken place, appropriate cleanup efforts should be made. Cleaners need to be trained in appropriate techniques to remove as much THS from the environment as possible. Above all, the public needs to be informed of their rights to know whether or not they are potentially being exposed to THS and have the ability to protect themselves and their family.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
U.S. Department of Health and Human Services. The health consequences of smoking–50 years of progress: a report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health. 2014.
International Agency for Research on Cancer. IARC monographs on the evaluation of the carcinogenic risk of chemicals to humans: tobacco smoking. Report No.: 38. 1986-32676. Lyon, France: World Health Organization, IARC.
National Research Council, Committee on Passive Smoking. Environmental tobacco smoke: measuring exposures and assessing health effects. Washington, D.C: National Academy Press; 1986.
U.S. Department of Health and Human Services. The health consequences of involuntary smoking. A report of the Surgeon General. 1986-32676. Report No.: DHHS Publication No. (CDC) 87-8398. Washington, D.C.: U.S. Department of Health and Human Services, Public Health Service, Office on Smoking and Health..
Matt GE, Quintana PJ, Destaillats H, Gundel LA, Sleiman M, Singer BC, et al. Thirdhand tobacco smoke: emerging evidence and arguments for a multidisciplinary research agenda. Environ Health Perspect. 2011;119(9):1218–26. doi:10.1289/ehp.1103500. This paper is an early review on THS and summarizes the literature up to 2011. The paper still provides useful information on the topic.
Schick SF, Farraro KF, Perrino C, Sleiman M, van de Vossenberg G, Trinh MP, et al. Thirdhand cigarette smoke in an experimental chamber: evidence of surface deposition of nicotine, nitrosamines and polycyclic aromatic hydrocarbons and de novo formation of NNK. Tob Control. 2014;23(2):152–9. doi:10.1136/tobaccocontrol-2012-050915.
Sleiman M, Gundel LA, Pankow JF, Jacob 3rd P, Singer BC, Destaillats H. Formation of carcinogens indoors by surface-mediated reactions of nicotine with nitrous acid, leading to potential thirdhand smoke hazards. Proc Natl Acad Sci U S A. 2010;107(15):6576–81. doi:10.1073/pnas.0912820107. This paper provides results from elegant experimental studies on the chemistry of THS.
Hoh E, Hunt RN, Quintana PJ, Zakarian JM, Chatfield DA, Wittry BC, et al. Environmental tobacco smoke as a source of polycyclic aromatic hydrocarbons in settled household dust. Environ Sci Technol. 2012;46(7):4174–83. doi:10.1021/es300267g.
Destaillats H, Singer BC, Lee SK, Gundel LA. Effect of ozone on nicotine desorption from model surfaces: evidence for heterogeneous chemistry. Environ Sci Technol. 2006;40(6):1799–805.
Hang B, Sarker AH, Havel C, Saha S, Hazra TK, Schick S, et al. Thirdhand smoke causes DNA damage in human cells. Mutagenesis. 2013;28(4):381–91. doi:10.1093/mutage/get013.
Petrick LM, Svidovsky A, Dubowski Y. Thirdhand smoke: heterogeneous oxidation of nicotine and secondary aerosol formation in the indoor environment. Environ Sci Technol. 2011;45(1):328–33. doi:10.1021/es102060v.
Ramirez N, Ozel MZ, Lewis AC, Marce RM, Borrull F, Hamilton JF. Exposure to nitrosamines in thirdhand tobacco smoke increases cancer risk in non-smokers. Environ Int. 2014;71:139–47. doi:10.1016/j.envint.2014.06.012.
Quintana PJ, Matt GE, Chatfield D, Zakarian JM, Fortmann AL, Hoh E. Wipe sampling for nicotine as a marker of thirdhand tobacco smoke contamination on surfaces in homes, cars, and hotels. Nicotin Tob Res. 2013;15(9):1555–63. doi:10.1093/ntr/ntt014. This paper documents the presence of THS in environments that are critical for the public.
U.S. Environmental Protection Agency. America’s children and the environment. EPA 240-R-13-001. Washington, D.C.: US Environmental Protection Agency; 2008.
National Research Council. Health effects of exposure to radon: BEIR VI. Washington, DC: The National Academies Press; 1999. p. 516.
U.S. Environmental Protection Agency, U.S. Department of Health and Human Services, U.S. Department of Agriculture, U.S. Department of Defense, U.S. Department of Energy, U.S. Department of Housing and Urban Development, U.S. Department of Interior, U.S. Department of Veterans Affairs, U.S. General Services Administration. Protecting people and families from radon: a federal action plan for saving lives. Washington, D.C.: U.S. Environmental Protection Agency; 2011. p. 10.
U.S. Environmental Protection Agency. A citizen’s guide to radon: the guide to protecting yourself and your family from radon. Washington, DC: U.S. Environmental Protection Agency; 2012.
Indoor Radon Abatement Act of 1988. 15 USC Sect 53 Subchapter III. 1988.
U.S. Environmental Protection Agency, U.S. Department of Health and Human Services, U.S. Department of Agriculture, U.S. Department of Defense, U.S. Department of Energy, U.S. Department of Housing and Urban Development, U.S. Department of Interior, U.S. Department Veterans Affairs, U.S. General Services Administration. Protecting people and families from radon: a federal action plan for saving lives. Washington, DC: U.S. Environmental Protection Agency; 2011.
Lanphear BP, Hornung R, Khoury J, Yolton K, Baghurst P, Bellinger DC, et al. Low-level environmental lead exposure and children’s intellectual function: an international pooled analysis. Environ Health Perspect. 2005;113(7):894–9.
Advisory Committee on Childhood Lead Poisoning Prevention of the CDC. Low level lead exposure harms children: a renewed call for primary prevention. Atlanta, GA: CDC; 2012 January 4.
Centers for Disease Control and Prevention. Preventing lead poisoning in young children. Report No.: 0149-2195 Contract No.: 99-2230. Atlanta, GA: Centers for Disease Control and Prevention, Division CfDC-CfEH-CD; 1985.
Centers for Disease Control and Prevention. Preventing lead poisoning in young children. 1991 [cited 2015 April 20]. Available from http://www.cdc.gov/nceh/lead/publications/books/plpyc/contents.htm#contents.
Apostolou A, Garcia-Esquinas E, Fadrowski JJ, McLain P, Weaver VM, Navas-Acien A. Secondhand tobacco smoke: a source of lead exposure in US children and adolescents. Am J Public Health. 2012;102(4):714–22. doi:10.2105/ajph.2011.300161.
Mannino DM, Albalak R, Grosse S, Repace J. Second-hand smoke exposure and blood lead levels in U.S. children. Epidemiol (Cambridge, Mass). 2003;14(6):719–27. doi:10.1097/01.ede.0000081998.02432.53.
MedlinePlus. Pica. Bethesda, MD: U.S. National Library of Medicine, NIH; 2015 [updated March 16; cited 2015 March 31]. Available from: http://www.nlm.nih.gov/medlineplus/ency/article/001538.htm.
Disclosure of known lead-based paint and/or lead-based paint hazards upon sale or lease of residential property. 24 US CFR Title 24 Subtitle A Part 35 Subpart A(1992).
City of Milwaukee v. NL Industries, 762 N.W.2d 757 (Wis. Ct. App. 2008).
State of Rhode Island v. Lead Industries Association, Inc., 951 A.2d 428 (R.I. 2008).
City of Toledo v. Sherwin-Williams Company, Case No. CI 200606040 slip op. (Court of Common Pleas of Lucas County, Ohio 2007).
In Re: Lead Paint Litigation, 924 A.2d 484 (N.J. 2007).
City of St. Luis v. Benjamin Moore & Co., 226 S.W. 3d 110 (MO, 2007).
County of Santa Clara v. Atlantic Richfield Co., 137 Cal. App. 4th 292, 40 Cal.Rptr.3d 313 (6th District, 2006).
U.S. Environmental Protection Agency. Learn about asbestos Washington, DC: EPA; 2015 [updated February 19; cited 2015 March 31]. Available from: http://www2.epa.gov/asbestos/learn-about-asbestos#asbestos.
Agency for Toxic Substances and Disease Registry (ATSDR). Fact sheet: asbestos (case# 1332-21-4). Atlanta, GA: U.S. Department of Health and Human Services; 2001.
National Research Council. Asbestos: selected cancers. Washington, DC: The National Academies Press; 2006. p. 340.
Clean Air Act. 42 USC Sect 7412(1990).
Safe Drinking Water Act 42 USC Sect 1400(1974).
Asbestos Hazard Emergency Response Act. 15 USC Chapter 53 Subchapter II(1986).
Asbestos-Containing Materials in Schools. 40 CFR Chapter 1 Subchapter R Part 763 Subpart E(1987).
Asbestos School Hazard Abatement Reauthorization Act of 1990. 104 Stat 4589(1990).
Maine Department of Environmental Protection—Waste Management. Information that realty agents should know about asbestos regulations Maine: Maine DEP; 2004 [updated 2013; cited 2015 March 31]. Available from http://www.maine.gov/dep/waste/asbestos/realtors.html.
State of California Department of Real Estate. Disclosures in real property transactions: California Department of Real Estate. 2005. Available from http://www.dre.ca.gov/files/pdf/re6.pdf. Accessed 2 July 2015.
Whitehead TP, Havel C, Metayer C, Benowitz NL, Jacob P. Tobacco alkaloids and tobacco-specific nitrosamines in dust from homes of smokeless tobacco users, active smokers, and non-tobacco users. Chem Res Toxicol. 2015. doi:10.1021/acs.chemrestox.5b00040.
Jacob 3rd P, Goniewicz ML, Havel CM, Schick SF, Benowitz NL. Nicotelline: a proposed biomarker and environmental tracer for particulate matter derived from tobacco smoke. Chem Res Toxicol. 2013;26(11):1615–31. doi:10.1021/tx400094y.
Acknowledgments
The authors were supported by a grant from the UC Berkeley (UCSF) California Tobacco-Related Disease Research Program (grant number 20PT-0184).
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
Jonathan M. Samet, Dayana Chanson, and Heather Wipfli declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors. Because the content of the survey was not related to human health, it was not considered human subject research requiring IRB approval or informed consent.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Global Environmental Health and Sustainability
Rights and permissions
About this article
Cite this article
Samet, J.M., Chanson, D. & Wipfli, H. The Challenges of Limiting Exposure to THS in Vulnerable Populations. Curr Envir Health Rpt 2, 215–225 (2015). https://doi.org/10.1007/s40572-015-0060-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40572-015-0060-1