Abstract
Purpose
Pneumonia is the third leading cause of death in children under 5 years of age worldwide. In pediatrics, both the accuracy and safety of diagnostic tools are important. Lung ultrasound (LUS) could be a safe diagnostic tool for this reason. We searched in the literature for diagnostic studies about LUS to predict pneumonia in pediatric patients using systematic review and meta-analysis.
Methods
The Medline, CINAHL, Cochrane Library, Embase, SPORTDiscus, ScienceDirect, and Web of Science databases from inception to September 2017 were searched. All studies that evaluated the diagnostic accuracy of LUS in determining the presence of pneumonia in patients under 18 years of age were included.
Results
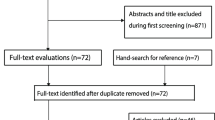
1042 articles were found by systematic search. 76 articles were assessed for eligibility. Seventeen studies were included in the systematic review. We included 2612 pooled cases. The age of the pooled sample population ranged from 0 to about 21 years old. Summary sensitivity, specificity, and AUC were 0.94 (IQR: 0.89–0.97), 0.93 (IQR: 0.86–0.98), and 0.98 (IQR: 0.94–0.99), respectively. No agreement on reference standard was detected: nine studies used chest X-rays, while four studies considered the clinical diagnosis. Only one study used computed tomography.
Conclusions
LUS seems to be a promise tool for diagnosing pneumonia in children. However, the high heterogeneity found across the individual studies, and the absence of a reliable reference standard, make the finding questionable. More methodologically rigorous studies are needed.
Sommario
Obiettivo
La polmonite è la terza causa di morte nel mondo al di sotto dei 5 anni. In campo pediatrico, sia l’accuratezza che la sicurezza degli strumenti diagnostici sono importanti. In questo senso l’ecografia polmonare (LUS) potrebbe essere uno strumento diagnostico sicuro. Abbiamo analizzato la letteratura sull’accuratezza della LUS nel diagnosticare la polmonite nei pazienti pediatrici attraverso una revisione sistematica e una meta-analisi.
Metodi
Sono stati consultati i database Medline, CINAHL, Cochrane Library, Embase, SPORTDiscus, ScienceDirect e Web of Science dal loro avvio alla fine di settembre 2017. Sono stati inclusi tutti gli studi che hanno valutato l’accuratezza diagnostica della LUS nel determinare la presenza di polmonite nei pazienti di età inferiore ai 18 anni. 1.042 articoli sono stati trovati dalla ricerca sistematica. 76 articoli sono stati valutati per l’ammissibilità. 17 studi sono stati inclusi nella revisione sistematica.
Risultati
Abbiamo incluso 2.612 casi raggruppati. L’età della popolazione campione raggruppata varia da 0 a circa 21 anni. Sensibilità, specificità e AUC sono rispettivamente 0,94 (IQR: 0,89–0,97); 0,93 (IQR: 0,86–0,98) e 0,98 (IQR: 0,94–0,99). Non è stato rilevato accordo sullo standard di riferimento: 9 studi hanno usato la radiografia del torace; 4 studi hanno considerato la diagnosi clinica. Solo uno studio ha utilizzato la tomografia computerizzata.
Conclusioni
La LUS sembra essere uno strumento promettente per diagnosticare la polmonite nei bambini. Tuttavia l’elevata eterogeneità riscontrata nei singoli studi e l’assenza di uno standard di riferimento affidabile rendono discutibile il risultato. Sono necessari studi metodologicamente più rigorosi.







Similar content being viewed by others
References
Liu L, Oza S, Hogan D, Perin J, Rudan I, Lawn JE, Cousens S, Mathers C, Black RE (2015) Global, regional, and national causes of child mortality in 2000-13, with projections to inform post-2015 priorities: an updated systematic analysis. Lancet 385:430–440
Walker CL, Rudan I, Liu L, Nair H, Theodoratou E, Bhutta ZA, O’Brien KL, Campbell H, Black RE (2013) Global burden of childhood pneumonia and diarrhoea. Lancet 381:1405–1416
Shah SN, Bachur RG, Simel DL, Neuman MI (2017) Does this child have pneumonia? The rational clinical examination systematic review. JAMA 318:461–471
Lynch T, Bialy L, Kellner JD, Osmond MH, Klassen TP, Durec T, Leicht R, Johnson DW (2010) A systematic review on the diagnosis of pediatric bacterial pneumonia: when gold is bronze. PLoS One 5:e11989
Ben Shimol S, Dagan R, Givon-Lavi N, Tal A, Aviram M, Bar-Ziv J, Zodicov V, Greenberg D (2012) Evaluation of the World Health Organization criteria for chest radiographs for pneumonia diagnosis in children. Eur J Pediatr 171:369–374
Williams GJ, Macaskill P, Kerr M, Fitzgerald DA, Isaacs D, Codarini M, McCaskill M, Prelog K, Craig JC (2013) Variability and accuracy in interpretation of consolidation on chest radiography for diagnosing pneumonia in children under 5 years of age. Pediatr Pulmonol 48:1195–1200
Levinsky Y, Mimouni FB, Fisher D, Ehrlichman M (2013) Chest radiography of acute paediatric lower respiratory infections: experience versus interobserver variation. Acta Paediatr 102:e310–e314
Johnson J, Kline JA (2010) Intraobserver and interobserver agreement of the interpretation of pediatric chest radiographs. Emerg Radiol 17:285–290
Llamas-Álvarez AM, Tenza-Lozano EM, Latour-Pérez J (2017) Accuracy of lung ultrasound in the diagnosis of pneumonia in adults: systematic review and meta-analysis. Chest 151:374–382
Alzahrani SA, Al-Salamah MA, Al-Madani WH, Elbarbary MA (2017) Systematic review and meta-analysis for the use of ultrasound versus radiology in diagnosing of pneumonia. Crit Ultrasound J 9:6
Testa A, Soldati G, Copetti R, Giannuzzi R, Portale G, Gentiloni-Silveri N (2012) Early recognition of the 2009 pandemic influenza A (H1N1) pneumonia by chest ultrasound. Crit Care 16:R30
Reissig A, Copetti R (2014) Lung ultrasound in community-acquired pneumonia and in interstitial lung diseases. Respiration 87:179–189
Asano M, Watanabe H, Sato K, Okuda Y, Sakamoto S, Hasegawa Y, Sudo K, Takeda M, Sano M, Kibira S, Ito H (2017) Validity of ultrasound lung comets for assessment of the severity of interstitial pneumonia. J Ultrasound Med. https://doi.org/10.1002/jum.14497 (Epub ahead of print)
Perrone T, Quaglia F (2017) Lung US features of severe interstitial pneumonia: case report and review of the literature. J Ultrasound 20:247–249
Whiting PF, Rutjes AW, Westwood ME, Mallett S, Deeks JJ, Reitsma JB, Leeflang MM, Sterne JA, Boosuyt PM, Quadas-2 Group (2011) QUADAS-2: a revised tool for the qualify assessment of diagnostic accuracy studies. Ann Intern Med 155:529–536
Boursiani C, Tsolia M, Koumanidou C, Malagari A, Vakaki M, Karapostolakis G, Mazioti A, Alexopoulou E (2017) Lung ultrasound as first-line examination for the diagnosis of community-acquired pneumonia in children. Pediatr Emer Care 33:62–66
Ellington LE, Gilman RH, Chavez MA, Pervaiz F, Marin-Concha J, Compen-Chang P, Riedel S, Rodriguez SJ, Gaydos C, Hardick J, Tielsch JM, Steinhoff M, Benson J, May EA, Figueroa-Quintanilla D, Checkley W, Lung Ultrasound for Pneumonia Assessment (LUPA) Study Investigators (2017) Lung ultrasound as a diagnostic tool for radiographically-confirmed pneumonia in low resource settings. Respir Med 128:57–64
Man SC, Fufezan O, Sas V, Schnell C (2017) Performance of lung ultrasonography for the diagnosis of community-acquired pneumonia in hospitalized children. Med Ultrason 19:276–281
Yadav KK, Awasthi S, Parihar A (2017) Lung ultrasound is comparable with chest roentgenogram for diagnosis of community-acquired pneumonia in hospitalised children. Indian J Pediatr 84:499–504
Yilmaz HL, Özkaya AK, Gökay SS, Kendir ÖT, Şenol H (2017) Point-of-care lung ultrasound in children with community acquired pneumonia. Am J Emer Med 35:964–969
Ambroggio L, Sucharew H, Rattan MS, O’Hara SM, Babcock DS, Clohessy C, Steinhoff MC, Macaluso M, Shah SS, Coley BD (2016) Lung ultrasonography: a viable alternative to chest radiography in children with suspected pneumonia? J Pediatr 176:93–98
Claes AS, Clapuyt P, Menten R, Michoux N, Dumitriu D (2017) Performance of chest ultrasound in pediatric pneumonia. Eur J Radiol 88:82–87
Samson F, Gorostiza I, Gonzalez A, Landa M, Ruiz L, Grau M (2018) Prospective evaluation of clinical lung ultrasonography in the diagnosis of community-acquired pneumonia in a pediatric emergency department. Eur J Emer Med 25:65–70
Zhan C, Grundtvig N, Klug BH (2016) Performance of bedside lung ultrasound by a pediatric resident: a useful diagnostic tool in children with suspected pneumonia. Pediatr Emer Care. https://doi.org/10.1097/pec.0000000000000888 (Epub ahead of print)
Iorio G, Capasso M, De Luca G, Prisco S, Mancusi C, Laganà B, Comune V (2015) Lung ultrasound in the diagnosis of pneumonia in children: proposal for a new diagnostic algorithm. Peer J 3:e1374
Urbankowska E, Krenke K, Drobczyński L, Korczyński P, Urbankowski T, Krawiec M, Kraj G, Brzewski M, Kulus M (2015) Lung ultrasound in the diagnosis and monitoring of community acquired pneumonia in children. Respir Med 109:1207–1212
Esposito S, Sferrazza Papa S, Borzani I, Pinzani R, Giannitto C, Consonni D, Principi N (2014) Performance of lung ultrasonography in children with community-acquired pneumonia. Ital J Pediatr 40:37
Liu J, Liu F, Liu Y, Wang HW, Feng ZC (2014) Lung ultrasonography for the diagnosis of severe neonatal pneumonia. Chest 146:383–388
Reali F, Sferrazza Papa GF, Carlucci P, Fracasso P, Di Marco F, Mandelli M, Soldi S, Riva E, Centanni S (2014) Can lung ultrasound replace chest radiography for the diagnosis of pneumonia in hospitalized children? Respiration 88:112–115
Shah VP, Tunik MG, Tsung JW (2013) Prospective evaluation of point-of-care ultrasonography for the diagnosis of pneumonia in children and young adults. JAMA Pediatr 167:119–125
Caiulo VA, Gargani L, Caiulo S, Fisicaro A, Moramarco F, Latini G, Picano E, Mele G (2013) Lung ultrasound characteristics of community-acquired pneumonia in hospitalized children. Pediatr Pulmonol 48:280–287
Copetti R, Cattarossi L (2008) Ultrasound diagnosis of pneumonia in children. Radiol Med 113:190–198
Bradley JS, Byngton CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL, Mace SE, McCracken GH jr, Moore MR, St Peter SD, Stockwell Ja, Swanson JT; Pediatric Infectious Diseases Society and the Infectious Diseases Society of America (2011) The management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin Infect Dis 53:e25–e76
Harris M, Clark J, Coote N, Fletcher P, Harnden A, McKean M, Thomson A; British Thoracic Society Standard of Care Committee (2011) British Thoracic Society guidelines for the management of community acquired pneumonia in children: update 2011. Thorax 66 Suppl 6: ii1-23
Nascimento-Carvalho CM, Araùio-Neto CA, Ruuskanen O (2015) Association between bacterial infection and radiologically confirmed pneumonia among children. Pediatr Infect Dis J 34:490–493
Self WH, Courtney DM, McNaughton CD, Wunderink RG, Kline JA (2014) High discordance of chest x-ray and computed tomography for detection of pulmonary opacities in ED patients: implications for diagnosing pneumonia. Am J Emerg Med 31:401–405
Maughan BC, Asseling N, Carey JL, Sucov A, Valente JH (2013) False-negative chest radiographs in emergency department diagnosis of pneumonia. R I Med J 97:20–23
Simbalista R, Andrade DC, Borges IC, Araùjo M, Nascimento-Carvalho CM (2015) Diferrences upon admission and in hospital course of children hospitalized with community-acquired pneumonia with or without radiologically-confirmed pneumonia: a retrospective color study. BMC Pediatr 15:166
Pereda MA, Chavez MA, Hooper-Miele CC, Gilman RH, Steinhoff MC, Ellington LE, Gross M, Price C, Tielsch JM, Checkley W (2015) Lung ultrasound for the diagnosis of pneumonia in children: a meta-analysis. Pediatrics 135:714–722
Blackstock U, Munson J, Szyld D (2015) Bedside ultrasound curriculum for medical students: report a blended learning curriculum implementation and validation. J Clin Ultrasound 43:139–144
Xin H, Li J, Hu HY (2017) Is lung ultrasound useful for diagnosing pneumonia in children?: a meta-analysis and systemic review. Ultrasound Q https://doi.org/10.1097/ruq.0000000000000330 (Epub ahead of print)
Wingerter SL, Bachur RG, Monuetaux MC, Neuman MI (2012) Application of the World Health Organization criteria to predict radiograph pneumonia in a US-based pediatric emergency department. Pediatr Infect Dis J 31:561–564
O’Grady KAF, Torzillo PJ, Ruben AR, Taylor-Thomson D, Valery PC, Chang AB (2012) Identification of radiological alveolar pneumonia in children with high rates of hospitalized respiratory infections: comparison of WHO-defined and pediatric pulmonologist diagnosis in the clinical context. Pediatr Pulmonol 47:386–392
Mearelli F, Orso D, Fiotti N, Altamura N, Breglia A, De Nardo M, Paoli I, Zanetti M, Casarsa C, Biolo G (2015) Sepsis outside intensive care unit: the other side of the coin. Infection 43:1–11
Bedford Russell AR, Kumar R (2015) Early onset neonatal sepsis: diagnostic dilemmas and practical management. Arch Dis Child Fetal Neonatal Ed 100:F350–F354
Neuman MI, Monuteaux MC, Scully KJ, Bachur RG (2011) Prediction of pneumonia in a pediatric emergency department. Pediatrics 128:246–253
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.

40477_2018_306_MOESM1_ESM.jpg
Figure 8 Comparison of the sensitivity for individual studies for every sampling method. On the left column are the individual studies. On the right column is the sensitivity (95%CI). Prospective = prospective enrolment; Retrospective = retrospective enrolment; TP = true positives; FP = false positives; TN = true negatives; FN = false negatives. The dashed area represents the 95% confidence interval (JPEG 224 kb)

40477_2018_306_MOESM2_ESM.jpg
Figure 9 Comparison of the specificity for individual studies for every sampling method. On the left column are the individual studies. On the right column is the specificity (95%CI). Prospective prospective enrolment; Retrospective retrospective enrolment; TP true positives; FP false positives; TN true negatives; FN false negatives. The dashed area represents the 95% confidence interval (JPEG 220 kb)
Rights and permissions
About this article
Cite this article
Orso, D., Ban, A. & Guglielmo, N. Lung ultrasound in diagnosing pneumonia in childhood: a systematic review and meta-analysis. J Ultrasound 21, 183–195 (2018). https://doi.org/10.1007/s40477-018-0306-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-018-0306-5