Abstract
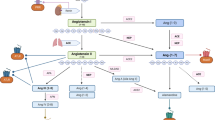
Pseudohyperaldosteronism is characterized by a clinical picture of hyperaldosteronism with suppression of renin and aldosterone. It can be due to endogenous or exogenous substances that mimic the effector mechanisms of aldosterone, leading not only to alterations of electrolytes and hypertension, but also to an increased inflammatory reaction in several tissues. Enzymatic defects of adrenal steroidogenesis (deficiency of 17α-hydroxylase and 11β-hydroxylase), mutations of mineralocorticoid receptor (MR) and alterations of expression or saturation of 11-hydroxysteroid dehydrogenase type 2 (apparent mineralocorticoid excess syndrome, Cushing’s syndrome, excessive intake of licorice, grapefruits or carbenoxolone) are the main causes of pseudohyperaldosteronism. In these cases treatment with dexamethasone and/or MR-blockers is useful not only to normalize blood pressure and electrolytes, but also to prevent the deleterious effects of prolonged over-activation of MR in epithelial and non-epithelial tissues. Genetic alterations of the sodium channel (Liddle’s syndrome) or of the sodium-chloride co-transporter (Gordon’s syndrome) cause abnormal sodium and water reabsorption in the distal renal tubules and hypertension. Treatment with amiloride and thiazide diuretics can respectively reverse the clinical picture and the renin aldosterone system. Finally, many other more common situations can lead to an acquired pseudohyperaldosteronism, like the expansion of volume due to exaggerated water and/or sodium intake, and the use of drugs, as contraceptives, corticosteroids, β-adrenergic agonists and FANS. In conclusion, syndromes or situations that mimic aldosterone excess are not rare and an accurate personal and pharmacological history is mandatory for a correct diagnosis and avoiding unnecessary tests and mistreatments.

Similar content being viewed by others
References
Armanini D, Strasser T, Weber PC. Characterization of aldosterone binding sites in circulating human mononuclear leukocytes. Am J Physiol. 1985;248:E388–90.
Bordin L, Donà G, Sabbadin C, Ragazzi E, Andrisani A, Ambrosini G, Brunati AM, Clari G, Armanini D. Human red blood cells alterations in primary aldosteronism. J Clin Endocrinol Metab. 2013;98:2494–501.
Armanini D, Calò L, Semplicini A. Pseudohyperaldosteronism: pathogenetic mechanisms. Crit Rev Clin Lab Sci. 2003;40:295–335.
Scaroni C, Opocher G, Mantero F. Renin-angiotensin-aldosterone system: a long-term follow-up study in 17 alpha-hydroxylase deficiency syndrome (17OHSD). Clin Exp Hypertens A. 1986;8:773–80.
Zhao LQ, Han S, Tian HM. Progress in molecular-genetic studies on congenital adrenal hyperplasia due to 11beta-hydroxylase deficiency. World J Pediatr. 2008;4:85–90.
Osmond JM, Dorrance AM. 11β-Hydroxysteroid dehydrogenase type II inhibition causes cerebrovascular remodeling and increases infarct size after cerebral ischemia. Endocrinology. 2009;150:713–9.
Calò LA, Zaghetto F, Pagnin E, Davis PA, De Mozzi P, Sartorato P, Martire G, Fiore C, Armanini D. Effect of aldosterone and glycyrrhetinic acid on the protein expression of PAI-1 and p22(phox) in human mononuclear leukocytes. J Clin Endocrinol Metab. 2004;89:1973–6.
Pizzolo F, Friso S, Morandini F, Antoniazzi F, Zaltron C, Udali S, Gandini A, Cavarzere P, Salvagno G, Giorgetti A, Speziali G, Choi SW, Olivieri O. Apparent mineralocorticoid excess by a novel mutation and epigenetic modulation by HSD11B2 promoter methylation. J Clin Endocrinol Metab. 2015;100:E1234–41.
Ronzaud C, Staub O. Ubiquitylation and control of renal Na+ balance and blood pressure. Physiology (Bethesda). 2014;29:16–26.
Ferraù F, Korbonits M. Metabolic comorbidities in Cushing’s syndrome. Eur J Endocrinol. 2015;173:M133–57.
Charmandari E, Lino T, Chrousos GP. Primary generalized familial and sporadic glucocorticoid resistance (Chrousos syndrome) and hypersensitivity. Endocr Dev. 2013;24:67–85.
Geller DS, Farhi A, Pinkerton N, Fradley M, Moritz M, Spitzer A, Meinke G, Tsai FT, Sigler PB, Lifton RP. Activating mineralocorticoid receptor mutation in hypertension exacerbated by pregnancy. Science. 2000;289:119–23.
Glover M, Ware JS, Henry A, Wolley M, Walsh R, Wain LV, Xu S, Van’t Hoff WG, Tobin MD, Hall IP, Cook S, Gordon RD, Stowasser M, O’Shaughnessy KM. Detection of mutations in KLHL3 and CUL3 in families with FHHt (familial hyperkalaemic hypertension or Gordon’s syndrome). Clin Sci (Lond). 2014;126:721–6.
Armanini D, Lewicka S, Pratesi C, Scali M, Zennaro MC, Zovato S, Gottardo C, Simoncini M, Spigariol A, Zampollo V. Further studies on the mechanism of the mineralocorticoid action of licorice in humans. J Endocrinol Invest. 1996;19:624–9.
Scali M, Pratesi C, Zennaro MC, Zampollo V, Armanini D. Pseudohyperaldosteronism from liquorice-containing laxatives. J Endocrinol Invest. 1990;13:847–8.
Palermo M, Armanini D, Delitala G. Grapefruit juice inhibits 11beta-hydroxysteroid dehydrogenase in vivo, in man. Clin Endocrinol (Oxf). 2003;59:143–4.
Armanini D, Karbowiak I, Krozowski Z, Funder JW, Adam WR. The mechanism of mineralocorticoid action of carbenoxolone. Endocrinology. 1982;111:1683–6.
Stowasser M, Ahmed AH, Pimenta E, Taylor PJ, Gordon RD. Factors affecting the aldosterone/renin ratio. Horm Metab Res. 2012;44:170–6.
Armanini D, Fiore C, Pellati D. Spontaneous resolution of idiopathic aldosteronism after long-term treatment with potassium canrenoate. Hypertension. 2007;50:e69–70.
Armanini D, Fiore C. Some considerations about evolution of idiopathic primary aldosteronism. J Endocrinol Invest. 2009;32:623–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflict of interest and no financial disclosure to disclose.
Rights and permissions
About this article
Cite this article
Sabbadin, C., Armanini, D. Syndromes that Mimic an Excess of Mineralocorticoids. High Blood Press Cardiovasc Prev 23, 231–235 (2016). https://doi.org/10.1007/s40292-016-0160-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-016-0160-5