Abstract
Background
The extent of concussion injury in the rugby codes for women is unclear.
Objective
Our aim was to review all published studies reporting concussion injuries from match and training participation in rugby codes and report the pooled data estimates for rugby league and union concussion injury epidemiology.
Methods
We conducted a systematic literature analysis of concussion in rugby league and rugby union for published studies from January 1990 to July 2021. Data from 16 studies meeting the inclusion criteria were extracted for women’s concussion injuries and were subsequently pooled. Costs from Accident Compensation Corporation (ACC) data were attributed to the results to provide cost estimates.
Results
The pooled analysis match injury incidence of women’s concussion was higher for rugby league (10.3 per 1000 match hours) than rugby 15 s (2.8 per 1000 match hours) or rugby 7 s (8.9 per 1000 match hours). There was a fourfold difference in the pooled incidence of concussion in women’s rugby league (risk ratio [RR] 4.53, 95% confidence interval [CI] 1.8–11.3]; p = 0.0001) when compared with rugby 15 s. There was also a ninefold higher risk of a concussion during match participation compared with training participation for women’s rugby 15 s (RR 9.3, 95% CI 1.29–66.78; p = 0.0070). The total estimated costs for the concussions reported were NZ$1,235,101. For rugby 7 s, the pooled concussive injury burden was 33.2 days.
Conclusions
Our pooled analysis clarified the extent of concussion injury and the possible associated costs at several levels of the game for women’s rugby codes. The pooled mean days lost because of concussions was 33 days. As this was considerably longer than the 7- to 10-day expected timeframe outlined in the Concussion in Sport Consensus statement, these guidelines need to be updated to include sex-specific differences.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Rugby league had higher concussion rates than rugby union for women. |
Rugby 7 s had higher concussion rates than rugby 15 s for women. |
The higher risk of concussion during matches compared with training varied with participation level. |
1 Introduction
Rugby union and rugby league are international collision sports played by junior, amateur, semi-professional and professional players worldwide [1,2,3,4]. Both have similar characteristics, with forwards and backs players in possession of the ball advancing into the opposition’s territory to score a try by passing the ball backwards or kicking the ball forward in the opposition’s territory. The key differences between league and union are that league has 13 not 15 players on the field; it does not have line outs, rucks or mauls; and players can only hold possession of the ball for a maximum of six tackles before handing the opposition the ball [2]. Rugby league and union, at the senior level of participation, are played on the same size fields, for two 40 min halves with a 10 min break in the middle, although this can vary by age or competition [1, 5]. Although rugby league is typically played with 13 players, rugby union has two versions of participation on the same size field. These are rugby 15 s and the popular shortened version of rugby union, termed rugby 7 s, where seven players compete on a full size rugby field over two 7-min halves [6]. Rugby 7 s matches are typically held during tournaments via a multi-team or multi-game structure over a shortened period (typically 2–3 days) [6].
Female involvement in rugby 15 s and rugby 7 s has increased in popularity, with over 2 million women participating under the same rules as their male counterparts at the community and elite levels of participation [7]. This has been similar in women’s rugby league, with a reported 29% increase in participation numbers reported in Australia and an increased competition pathway in both Australia and England [8]. Despite the increases in participation for both rugby union and rugby league, there are a paucity of studies reporting on match injuries. It has been recently identified [9] that only seven papers have been available since 1990 reporting on women’s rugby match injuries [10,11,12,13,14,15,16], compared with more than 113 studies [1, 17, 18] reporting on men’s rugby. One paper has reported on female rugby league [19] participation compared with more than 25 [20,21,22] studies reporting on male rugby league. This is similar across a variety of sports research, with one study reporting an under-representation of female participant research across three leading sports medicine research journals [23].
Although females participate in match activities under the same rules as males, females reportedly have higher injury risks, even though they have lower physiological indices (e.g. reduced speed and less agility, lower muscular power, lower estimated maximal aerobic power) compared with men [24]. Interestingly, injury patterns also differ between males and females in other sports such as basketball [25], football [26], and handball [27].
In New Zealand, most rugby union and league participants are amateur (i.e., they derive income from another source). This is similar to other league-playing nations. Therefore, the majority of injuries occur at that level of play. Of those papers published reporting on women’s rugby union and league, there is a paucity of studies at the amateur and junior levels of participation in both codes. There is also an assumption that the findings of the epidemiological studies on professional participants translate to other cohorts of participants in other countries but this is yet to be tested [28].
There is a growing body of evidence [29,30,31,32] identifying that following sports-related concussion, female athletes experience greater symptom severity and take longer to recover when compared with male athletes. There is likely a combination of intrinsic and extrinsic factors that contribute to this observed sex difference. It has been suggested that it could be due to more reporting of symptoms in females [33, 34], lower neck strength in females [35], sex differences in white matter volume [36, 37], hormonal influence [38, 39], and differences in neural networks utilisation [40]. It has also been reported [41] that the smaller axons in females have a greater probability of microtubule damage compared with males when exposed to equivalent acceleration/deceleration forces. Importantly, data also show that earlier access to medical care can improve time to symptom recovery, especially in females [42]. These factors highlight further opportunity to tailor and improve prevention, care, and recovery of female athletes to ensure a safe and sustained return to sport.
1.1 Objective
The purpose of this pooled analysis was to provide estimates for rugby league and rugby union training and match concussion injury epidemiology for women.
2 Methods
The methodology utilised in this pooled analysis was similar to previous pooled analysis studies reporting rugby league injuries [43, 44] and followed the steps as described by Friedenreich [45, 46]. An additional advantage to utilising a pooled analysis approach is that the same statistical model can be utilised with data from methodologically diverse studies [47]. The review was registered with the International Prospective Register of Systematic Reviews (PROSPERO) on 27 January 2020 (Registration No. CRD42020166833). Guidelines for the reporting of systematic reviews (Preferred Reporting Items for Systematic Reviews and Meta-Analyses [PRISMA] [48]) and observational studies (Meta-analysis Of Observational Studies in Epidemiology [MOOSE] [49]) were followed. The PRISMA and MOOSE guidelines contain checklists that were utilised for conducting and reviewing the included studies.
2.1 Search Strategy for Identification of Databases
Articles were identified from an initial search of the online databases from January 1990 to July 2021. The search was undertaken using the key search terms of ‘Rugby Union’, Rugby League’, ‘rugby’, ‘union’, ‘league’ and ‘football’ AND ‘women’, ‘female’, ‘woman’, ‘females’, AND ‘match’ OR ‘training’ as well as the injury terms ‘athletic injuries’, ‘concussion’, ‘sports concussion’, ‘sports-related concussion’, ‘brain concussion’, ‘brain injury’, ‘brain injuries’, ‘mild traumatic brain injury’, ‘mild TBI’, ‘mTBI’, ‘traumatic brain injury’, ‘TBI’, ‘craniocerebral trauma’, ‘head injury’, and ‘brain damage’. The reference lists of those articles retrieved for inclusion in this review were also hand searched to identify any other relevant articles. Key articles were retrieved via online databases and through hand searching reference lists, and these were also used for further searches using the Web of Science Cited Reference function. During the second stage of the literature search, the titles and abstracts of articles were reviewed to assess eligibility for inclusion in this review.
2.2 Inclusion/Exclusion Criteria
To establish some control over the heterogeneity of the different studies [49], inclusion criteria were established. Published studies that reported the incidence of injury in rugby league and rugby union match and training activities were collated and included in the pooled analysis if they:
-
(1)
were available in English; and
-
(2)
were published in a peer reviewed journal or book; and
-
(3)
were prospective cohort studies; and
-
(4)
reported the match or training time exposure enabling the calculation of women’s rugby 15 s, rugby 7 s, rugby league player time injury rates; and
-
(5)
reported concussions as a result of match or training injuries.
Studies were excluded from this review if it was identified that the publication:
-
(1)
was unavailable in English; or
-
(2)
did not provide match or training exposure enabling the calculation of player time rates; or
-
(3)
did not report on concussions that occurred because of match or training activities; or
-
(4)
combined male and female sex match or training exposure and did not differentiate; or
-
(5)
was a case study; or
-
(6)
utilised previously published data on concussions; or
-
(7)
was a meta-analysis or systematic review of rugby league and rugby union injuries.
All references were downloaded into a dedicated EndNote library (Endnote, X9). The library was reviewed, and duplicate records were identified and removed. All publications identified were initially screened by publication title and abstract to identify eligibility. The full-text versions of the remaining articles were then retrieved and evaluated against the inclusion criteria. Those studies meeting the inclusion criteria were included in the review. Searches were limited to ‘English language’ only. The references of all relevant articles were searched for further articles. In cases of discrepancies of eligibility, another author assessed the publication to screen for eligibility.
2.3 Procedures
All the studies included in the pooled analysis were observational in design. Two authors extracted the study characteristics and numerical data and assessed the quality by adhering to the protocol for systematic review of observational studies (MOOSE) [49] [see electronic supplementary Table S1]. This approach enabled a more precise estimate of the effects of influential factors and took into account confounding factors (participation level and age) and the heterogeneity of the studies [47].
2.4 Assessment of Publication Quality
All included studies were independently assessed by two authors reporting on the article quality utilising the STrengthening the Reporting of OBservational studies in Epidemiology (STROBE) statement [50]. The statement provides a 22-item checklist guidance on the reporting of observational studies in order to facilitate a critical appraisal of the study and for the interpretation of the results. Following the appraisal, the included studies were categorised as either poor, moderate or good quality based on the percentage of fulfilled items on the STROBE checklist, with cut-off values of < 50, 50–80 and > 80%, respectively [51].
2.5 Data Extraction
Those studies meeting the inclusion criteria underwent data extraction for information pertaining to level of participation, concussion and injury definition utilised, reported concussions and player position/group. Not all studies reported the same information in relationship to injury incidence or number of concussive injuries recorded.
2.6 Reconciliation of Incidence Data and Injury Costs
Not all studies included in the systematic review and pooled analysis utilised the standardised method for injury reporting (i.e., per 1000 h of exposure). As a result, calculations were required to convert some study data to the standardised method for injury reporting to enable pooled analysis to be conducted. The mean costs per concussion injury have been reported in several studies [52,53,54,55,56]. Only two of these studies have specifically reported on the associated costs of women participants [52, 53] but these were from two different reporting periods and had a wide variance in mean costs per concussion injury. More recently, a study reported 10 years of sports-related concussion costs and included female costs per concussion for moderate-to-severe claims (MSCs). This study was utilised to calculate the approximate associated costs for concussion across all the studies included in this review. The reported mean costs for concussions from this study were adjusted for inflation (Reserve Bank inflation adjustor; https://www.rbnz.govt.nz/monetary-policy/inflation-calculator) to 2021 values (rugby union: $10,741; rugby league: $12,002) and calculated per reported concussion.
2.7 Injury Definitions
To enable meaningful comparisons, the sports injury definitions of the included studies were categorised into broad groups [57]. The definition of an injury is a contentious issue [58, 59] and there have been many variations on what constitutes a recordable injury. Although there are two broadly accepted definitions (medical treatment and loss-of-time-fully-inclusive) there are advantages and disadvantages to these definitions [57]. The definitions utilised are dependent on what the authors are reporting, such as injuries that result in missed match participation only (semi-inclusive time loss), missed match and training (full-inclusive) or an all-inclusive injury definition [57]. The results of these different definitions is that some papers will report some injuries (time loss in match and training activities) or eliminate them if they did not result on time loss from matches [57, 60]. For the purpose of this review, these groups consisted of: (1) medical attention/treatment injury (any injury that requires the assistance of sports medicine personnel with or without time loss from training or completion); (2) full-inclusive time-loss injury (any injury that results in time lost from competition and/or training); (3) semi-inclusive time-loss injury (any injury that results in time lost from competition only); and (4) all-inclusive injury (an injury that requires the assistance of sports medicine personnel and/or that results in time loss from competition and/or training) [60]. All included studies were reviewed to identify any concussion definitions utilised.
2.8 Pooled Analysis of Concussion Incidence
A pooled analysis of the included studies was undertaken where homogeneity occurred in terms of the injury definition utilised and the reporting of injury incidence was per 1000 match or training hours. This strategy has been previously utilised in rugby 15 s [9, 18, 61] and rugby league [22, 43, 44] epidemiological studies to combine the information provided into a single estimate [46, 62]. By pooling the data, the information provided can then be statistically reanalysed, providing more precise injury data [46].
2.9 Statistical Analyses
A combined estimate of injuries within a specific sport through pooled analysis [63] provides more precise evidence and meaningful information about the sport, while controlling for between-study variation due to individual subcohort characteristics [46]. Data from the individual studies were combined. Incidence rates and 95% confidence intervals (CIs) were calculated [64] where data were available and were reported according to the methodology utilised in the individual studies. Reviewer inter-rater reliability was assessed utilising the Cohen’s Kappa (κ) statistic. The level of agreement was categorised as none, minimal, weak, moderate, strong and almost perfect, with cut-offs of < 0.20, 0.21–0.39, 0.40–0.59, 0.60–0.79, 0.80–0.90, and > 0.90, respectively [65]. The pooled calculation of the incidence of concussion was undertaken to report the incidence per 1000 h and the 95% CIs. To compare between injury rates, risk ratios (RRs) were used. To test for significant differences between studies and player positions, Chi-square goodness-of-fit tests were utilised. All statistics were carried out using the SPSS statistical software packages (IBM SPSS Statistics for Windows, Version 22.0, Armonk, NY: IBM Corp).
3 Results
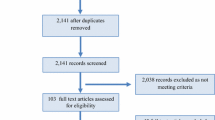
Sixteen studies [10, 11, 13,14,15,16, 19, 66,67,68,69,70,71,72,73,74] met the inclusion criteria for this review (see Fig. 1). Nine of the included studies [10, 11, 13,14,15,16, 70, 73, 74] reported on women’s rugby 15 s match injuries, four studies [66,67,68, 72] reported on women’s rugby 7 s, two studies [19, 69] reported on women’s rugby league, and two studies [14, 71] reported on women’s rugby 15 s training injuries. Although included in the review, some studies were excluded from the pooled analysis. One of these studies [15] combined both rugby 15 s and rugby 7 s, while another study [16] only reported the number of concussions. Three studies [14, 15, 73] utilised the athlete exposures (AEs) rate and two of these three studies [15, 73] reported on match injuries. Other studies were reviewed but were excluded as they were not peer reviewed [75,76,77], reported on a specific injury [67, 78,79,80,81,82,83,84,85], did not stratify the results by sex [86,87,88,89,90], did not report concussions [12] or exposure rates [91], assessed injuries as a result of foul play [92], utilised a self-reporting survey [87, 92, 93], reported on the costs [52,53,54,55, 94, 95], reported previously included data [6, 67, 68, 96,97,98,99], or were reviews [1, 3, 4, 9, 100,101,102]. Reviewer inter-rater reliability was assessed as strong (κ = 0.84; p < 0.0001) between two of the reviewers. All the studies included in this review were considered to be of moderate quality [51].
PRISMA 2020 [48] flow diagram for the identification, screening, eligibility, and inclusion of studies for the pooled analysis of match and training women’s rugby league and rugby union concussion injuries. PRISMA Preferred Reporting Items for Systematic Reviews and Meta-Analyses
More than half of the studies (62.6%) utilised either an all-inclusive [10, 13,14,15, 68] or fully-inclusive [11, 66, 67, 70, 71] injury definition. Upon pooling the data, the all-inclusive injury definition resulted in a concussion incidence of 1.0 (95% CI 0.7–1.4) per 1000 match hours for rugby 15 s, whereas the fully-inclusive injury definition resulted in a concussion incidence of 3.6 (95% CI 1.4–9.7) per 1000 match hours. For rugby 7 s, the all-inclusive injury definition resulted in a concussion incidence of 7.7 (95% CI 6.0–9.8) per 1000 match hours, whereas the fully inclusive concussion incidence was 12.7 (95% CI 8.4–19.3) per 1000 match hours. Less than one-fifth (18.8%) of the studies [16, 72, 74] utilised a semi-inclusive injury definition but they did not provide exposure hours and could not be pooled. Two studies [69, 73] did not report an injury definition and one study [19] utilised a medical attention/treatment injury definition. Although all the studies did report on concussion, only two studies [15, 70] provided a definition for the identification of a concussive injury.
The studies reporting rugby 15 s match injury concussion data were drawn from 23,772 match exposure hours (professional: 2300 match hours; amateur/national/collegiate: 21,472 match hours), 7440 player game hours, 76,073 AEs and studies reporting rugby 15 s. Training injury concussion data were drawn from 3339.5 training exposure hours and 23,746 AEs (see Table 1). Studies reporting rugby 7 s match injury concussion data were drawn from 10,705 match hours, and studies reporting on women’s rugby league match injuries were drawn from 484.8 match exposure hours.
The pooled analysis concussion injury incidence for womens rugby 15 s match injuries was 2.8 (95% CI 2.1–3.4) per 1000 match hours (see Table 1). Although women’s World Cup rugby 15 s recorded a higher pooled concussion incidence rate than amateur rugby 15 s (RR 1.3, 95% CI 0.6–2.7; p = 0.5015), this was not significant. Amateur women’s rugby 15 s reported a higher incidence of concussion (16.1 [95% CI 8.4–31.0] per 1000 match hours) than World Cup (RR 4.8, 95% CI 1.5–15.6; p = 0.0037), national (RR 6.1, 95% CI 1.9–19.7; p = 0.0006) and collegiate (RR 10.2, 95% CI 4.8–21.7; p < 0.0001) rugby 15 s levels of participation.
The pooled concussion incidence of rugby 7 s was 8.9 (95% CI 7.1–10.7) per 1000 match hours. Participants at the elite level of women’s rugby 7 s participation recorded a higher concussion incidence (16.5 [95% CI 12.5–20.5] per 1000 match hours) than the amateur/elite candidate (RR 2.0, 95% CI 1.3–3.3; p = 0.0038) level of participation. There was a fourfold difference in the pooled incidence of concussion in women’s rugby league (RR 4.53, 95% CI 1.8–11.3; p = 0.0001) when compared with women’s rugby 15 s, and a ninefold increase in the risk of concussion in women’s rugby 15 s match activities (RR 9.3, 95% CI 1.29–66.78; p = 0.0070) when compared with women’s rugby 15 s training activities. The total estimated costs for the concussions reported was New Zealand dollars (NZ$) $2,358,584. More than one-third (39.4%; NZ$1,020,395) of the estimated total costs were attributed to women’s rugby 7 s, while women’s rugby 15 s total estimated costs were slightly less (27.4%; NZ$708,906).
Only four studies [11, 66,67,68] reported player position for concussion (see Table 2). Although backs recorded more concussions than forwards in women’s World Cup (RR 0.9, 95% CI 0.1–6.2; p = 0.8927) and rugby 7 s (RR 1.0, 95% CI 0.7–1.5; p = 0.9279), these differences were not significant. Elite rugby 7 s forwards recorded more concussions (17.2 [95% CI 11.9–24.7] per 1000 match hours) than forwards at the women’s World Cup (RR 5.0, 95% CI 1.2–21.1; p = 0.0138) and amateur/elite candidate rugby 7 s participants (RR 2.8, 95% CI 1.2–6.3; p = 0.0130). Elite backs at the rugby 7 s level of participation (12.8 [95% CI 9.7–16.8] per 1000 match hours) recorded more concussions than backs at the amateur/elite candidates (RR 4.1, 95% CI 1.0–17.0; p = 0.0349) level of participation but this was not significant. Of the studies that reported player positions, backs recorded higher pooled estimated costs for women’s rugby union concussions (NZ$271,572 vs. NZ$210,084).
Five studies [67, 68, 70,71,72] reported injury burden (see Table 3). At the amateur level of rugby 15 s match participation [70], the concussive injury burden was 28.9 ± 3.7 days. For rugby 7 s, the concussive injury burden ranged from 36.7 (20.8–52.6) days [67] to 37.0 (19.7–54.3) days [68] and 9 days per 1000 player hours [72]. For amateur women’s rugby 15 s training [71], the concussive injury burden was 30 days.
4 Discussion
The aim of this review was to examine the incidence of concussion in rugby union and rugby league match play and training, across all levels of play for women. While recent reviews [3, 103] have reported concussion incidence in rugby league for men, no pooled analysis for women has previously been undertaken. The current pooled analysis incorporates both match and training concussion injuries at levels of participation from collegiate to world championships.
On review of the studies for inclusion, three studies [67, 68, 99] reporting on rugby 7 s were identified as reporting similar data, and some values could not be calculated given the data provided. The lead author was contacted for clarification of the results provided in the articles. As a result of the replies from the author, only one study [68] was included in the analysis as this study covered the other two previously published studies [67, 99]. The number of concussions reported were differentiated into time loss (n = 15) and medical attention (n = 6) concussion injuries, with a definition of > 1 day absent for any concussion, not just seen by medical staff for medical attention (personal email dated 7 August 2020). It is not clear whether the six concussions that were assessed and did not result in time loss were suspected concussions that did not go on to have a medically confirmed diagnosis or if these were confirmed concussions that returned to full participation on the same day of injury.
4.1 Injury-Related Costs for Concussion
In a review of the associated costs of sport-related concussion in five sports in New Zealand over a 10-year period (2001–2011) [55], there were 1330 Accident Compensation Corporation (ACC) moderate-to-severe injury claims (MSCs) costing a total of $13,039,416, or $9804 per claim. The costs for the concussions recorded in this study [55] were classified as MSCs, meaning the injury required additional financial support for treatment, loss of earnings and related medical costs [104, 105]. This is not an indication of the injury severity but gives an indication of the impact that the injury has on the person’s life. The costs do not include presentations to a hospital as these are covered by bulk payments made by ACC to the hospitals. Rugby union recorded the highest total costs ($6,252,870) but rugby league recorded the highest mean cost per claim ($25,545). When female claims and costs were separated, female rugby union concussion cost a total of $608,215, with a mean cost of $9078, while female rugby league cost less at $121,732 but had a higher mean cost per claim ($10,144). When adjusted for inflation (Reserve Bank inflation adjustor; https://www.rbnz.govt.nz/monetary-policy/inflation-calculator), the costs were $719,645 ($10,741 per claim) for rugby union and $114,034 ($12,002 per claim) for rugby league. However, these costs were only for those concussive injuries that were seen more than once for further management and included additional financial support for treatment, loss of earnings and related medical costs [104, 105]. Given these average costs, the concussions reported in this review would equate to approximately $2,358,584 (rugby union: $2,298,574; rugby league $60,010), with concussions to backs costing more ($569,273 vs. $440,381) when compared with forwards.
The differences in the costs between rugby league and rugby union may be related to the period when the study was conducted and how concussion was identified and managed. With the increased awareness of the effects of concussion, players may be seeking medical assistance earlier and this may be reflected in the costs reported. Ongoing research reporting on the costs of concussions in rugby union and rugby league is warranted to identify the costs of these injuries.
4.2 Concussion Injury Burden
The finding that the mean injury burden (days lost) varied by participation level may be more reflective of the level of medical support provided, with female participation having minimal or no medical support available at the sideline, at all participation levels. Of the studies included in this review, the mean injury burden (days lost) for concussions, when pooled together, was 33 days, which was similar to a previous study [30] where the majority (77%) of concussions (male and female) took 28 days to recover and females had a 43–48% longer recovery time when compared with males. This is considerably longer than the 7- to 10-day expected timeframe outlined in the Concussion in Sport Consensus (CISC) statement for 80–90% of all concussions [106,107,108]. These longer recovery times indicate that the CISC guidance may need to be updated, include a breadth of sport-related concussion studies, and consider sex-specific recommendations. Further research is warranted to better understand concussion recovery in female athletes and the identification of tailored treatments for female concussions [40].
4.3 Male Versus Female Differences in Concussion
In a recent study [109] reporting on differences between male and female student athletes, the incidence of concussion was notably higher in female participants in sex-comparable sports (i.e., male and female teams play under the same rules and with the same equipment) and these concussions were more severe when compared with male participants. However, there is a paucity of studies reporting women’s rugby 15 s, rugby 7 s and rugby league when compared with male participation in these sporting codes. In examining symptom cluster discrepancies between male and female athletes, both at baseline and post-concussive event [34, 110, 111], it was reported that female athletes experienced more symptoms than male athletes. In a recent study [109], it was identified that females had notably higher scores in three of the concussion symptom clusters (migraine, cognitive and neuropsychiatric) in the acute concussion phase and at follow-up when compared with males. The cognitive and migraine clusters are classic symptoms of concussion [112], whereas the neuropsychiatric symptom cluster (irritability, nervousness, sadness, feeling more emotional) is less traditional and has a reported insidious effect on daily living and recovery [113]. Females have been reported to have a higher risk of mood disturbances after a concussive injury [109]. It has been recommended that sex-based considerations for managing concussion risk may be necessary to prevent further widening of the gap in concussion incidence between male and female sports participants [109].
4.4 Cause of Injury
In a study reporting on male and female athletes between the ages of 5 and 19 years [91], rugby union accounted for 5.6% (n = 721) of brain injuries. The primary mechanisms for a concussion occurring in females in rugby union were being tackled or tackling another player (51.7%), head-to-head collisions (7.3%) and head-to-knee collisions (5.1%). This was similar to another study reporting on women’s amateur rugby 15 s [96], where the majority (88%) of concussions occurred in the tackle (tackler: 11%; ball carrier: 77%) and only 11% of the concussions occurred in the ruck situation, and the exact mechanism of injury was not reported. One study [14] comparing both male and female rugby 15 s participants reported an incidence of 2.2 per 1000 match hours and 1.6 per 1000 match hours for males and females, respectively. The results of this study were consistent with another study reporting on the injury risk associated with tackling in rugby 15 s [114].
4.5 Injury Definition
As previously identified, what constitutes a reliable and accurate injury definition remains a contentious issue [58, 59] and this can be seen by the different types of injury definitions reported in this review. Injury definition and exposure heterogeneity can limit interstudy comparability, and this was evident with three studies not reporting exposure rates and three studies reporting a different exposure rate (AE). Although more than half of the included studies [10, 11, 13,14,15, 66,67,68, 70, 71] utilised an inclusive-type injury definition, this was evenly split, with five studies reporting an all-inclusive [10, 13,14,15, 68] injury definition and five studies reporting a fully-inclusive [11, 66, 67, 70, 71] injury definition. The use of these definitions is similar; however the fully-inclusive definition reports on missed match and training time and excludes injuries that require assistance from medical personnel [57, 60]. This is problematic as any injury that does not result in a missed match and occurs in a limited training session may be declared recovered and not recorded as an injury [115]. Missed-match definitions also depend on the duration between matches [115], with some studies reporting on tournaments where matches may occur more than once in a 7-day period or more than one match a day for consecutive days.
4.6 Limitations
As identified, there is a paucity of published literature reporting on female participation in both rugby union and rugby league injury epidemiology. Areas such as interstudy comparisons are limited by the different methodological approaches and definitions utilised as identified in this study. The publication of the consensus for data collection in rugby union studies [116] and the more recent community-based injury surveillance in rugby union [117] provides for a standardised approach that should be considered for future rugby union and rugby league studies. This will assist with the identification of the injury site, type, location, severity and mechanism of injury that occurs within female rugby union and rugby league.
Typically, most of the studies included in this review were undertaken over a single season or competition, limiting the identification of concussion injury trends, and future longitudinal studies should be encouraged in female rugby union and rugby league activities. There is an increasing awareness of the issue of concussion in rugby union and rugby league and a standardised approach to the assessment of this injury in women participants is necessary in terms of assessment tools, concussion definition and recovery management. Although the data collection methods appear to be similar for males and females, there are differences in terms of injury risk and recovery when comparing the sexes [118, 119]. As such, some aspects unique to females may be important for future research being undertaken, such as the relationship between the phase of the menstrual cycle and the incidence of concussive injuries [38, 120,121,122,123]. This information would be beneficial towards the development of tailored injury management for female participants [40].
Other limitation considerations identified in conducting this review were that the included studies ranged from 1999 to 2021, and much has occurred in regard to the definition, recognition, and medical management of concussions, including return to play, over that period of time. This may be reflected in the differences in the injury severity and injury burden recorded for concussions over the duration of the analysis. In addition, the included studies also span different levels of competition (amateur to professional) as well as national populations and may have different periods between match events. These factors may impact how concussion care is delivered, particularly when one considers a professional athlete versus an amateur/community athlete. The differences in medical care availability when comparing amateur and professional athletes or across nations and their healthcare systems are factors to be considered and these are difficult to control for. In addition, the differences in access to medical care across the different healthcare systems may impact upon the return-to-sport duration after a concussion has occurred.
5 Conclusions
Our pooled analysis provided combined estimates of concussion injuries for training and games within rugby league and rugby union and showed differences in concussion injury rates and possible associated costs at several levels in the game for women. It has been recommended that sex-based considerations for managing concussion risk may be necessary to prevent further widening of the gap in concussion incidence between male and female sports participants. The pooled mean days lost because of concussions was 33 days. As this was considerably longer than the 7- to 10-day expected timeframe outlined in the CISC statement, these guidelines need to be updated to include sex-specific differences.
References
Brooks J, Kemp S. Recent trends in rugby union injuries. Clin J Sport Med. 2008;27(1):51–73.
King D, Hume P, Milburn P, Guttenbeil D. Match and training injuries in rugby league: a review of published studies. Sports Med. 2010;40(2):163–78.
Gardner A, Iverson G, Levi C, Schofield P, Kay-Lambkin F, Kohler R, et al. A systematic review of concussion in rugby league. Br J Sports Med. 2015;49(8):495–8.
Gardner AJ, Iverson GL, Williams WH, Baker S, Stanwell P. A systematic review and meta-analysis of concussion in rugby union. Sports Med. 2014;44(12):1717–31.
Gissane C, Jennings D, Standing P. Incidence of injury in rugby league football. Physio. 1993;79:305–10.
Fuller CW, Taylor A, Raftery M. 2016 Rio Olympics: an epidemiological study of the men’s and women’s rugby-7s tournaments. Br J Sports Med. 2017;51(17):1272–8.
Gabb N, Trewartha G, Stokes K. Injury epidemiology in rugby. In: Twist C, Worsfold P, editors. The science of rugby. New York: Routledge; 2015. p. 219–36.
Cummins C, Melinz J, King D, Sanctuary C, Murphy A. Call to action: a collaborative framework to better support female rugby league players. Br J Sports Med. 2020;54(9):501–2. https://doi.org/10.1136/bjsports-2019-101403.
King D, Hume P, Cummins C, Pearce A, Clark T, Foskett A, et al. Match and training injuries in women’s rugby union: a systematic review of published studies. Sports Med. 2019;49(10):1559–74.
Schick D, Molloy M, Wiley J. Injuries during the 2006 women’s rugby world cup. Br J Sports Med. 2008;42(6):447–51.
Taylor A, Fuller C, Molloy M. Injury surveillance during the 2010 IRB women’s rugby world cup. Br J Sports Med. 2011;45(15):1243–5.
Doyle C, George K. Injuries associated with elite participation in women’s rugby over a competitive season: an initial investigation. Phys Ther Sport. 2004;5:44–50.
Carson J, Roberts M, White A. The epidemiology of women’s rugby injuries. Clin J Sport Med. 1999;9(2):75–8.
Kerr H, Micheli L, Kocher M, Curtis C, Kemp S, Brooks J. Collegiate rugby union injury patterns in New England: a prospective cohort study. Br J Sports Med. 2008;42(7):598–603.
Peck KY, Johnston DA, Owens BD, Cameron KL. The incidence of injury among male and female intercollegiate rugby players. Sports Health. 2013;5(4):327–33.
Collins C, Micheli L, Yard E, Comstock R. Injuries sustained by high school rugby players in the United States, 2005–2006. Arch Pediatr Adolesc Med. 2008;162(1):49–54.
Yeomans C, Kenny IC, Cahalan R, Warrington GD, Harrison AJ, Hayes K, et al. The incidence of injury in amateur male rugby union: a systematic review and meta-analysis. Sports Med. 2018;48(4):837–48.
Williams S, Trewartha G, Kemp S, Stokes K. A meta-analysis of injuries in senior men’s professional rugby union. Sports Med. 2013;43(10):1043–55.
King D, Gabbett T. Injuries in a national women’s rugby league tournament: an initial investigation. NZ J Sports Med. 2007;34(2):18–22.
Gabbett T. Science of rugby league football: a review. J Sports Sci. 2005;23(9):961–76.
Gabbett T, King T, Jenkins D. Applied physiology of rugby league. Sports Med. 2008;38(2):119–38.
King D, Hume P, Gissane C, Clark T. Semi-professional rugby league players have higher concussion risk than professional or amateur participants: a pooled analysis. Sports Med. 2017;47(2):197–205.
Costello JT, Bieuzen F, Bleakley CM. Where are all the female participants in Sports and Exercise Medicine research? Eur J Sport Sci. 2014;14(8):847–51.
King D, Hume P, Milburn P, Guttenbeil D. A review of the physiological and anthropometrical characteristics of rugby league players. S Afr J Res Sport Phys Ed Recr. 2009;31(2):49–67.
Deitch J, Starkey C, Walters S, Moseley J. Injury risk in professional basketball players: a comparison of women’s National Basketball Association and National Basketball Association athletes. Am J Sports Med. 2006;34:1077–83.
Waldén M, Hägglund M, Magnusson H, Ekstrand J. Anterior cruciate ligament injury in elite football: a prospective three-cohort study. Knee Surg Sports Traumatol Arthrosc. 2011;19(1):11–9.
Langevoort G, Myklebust G, Dvorak J, Junge A. Handball injuries during major international tournaments. Scand J Med Sci Sports. 2007;17(4):400–7.
Brooks JHM, Kemp SPT. Recent trends in rugby union injuries. Clin Sports Med. 2008;27(1):51–73.
Thibeault CM, Thorpe S, Canac N, Wilk SJ, Hamilton RB. Sex-based differences in transcranial Doppler ultrasound and self-reported symptoms after mild traumatic brain injury. Front Neurol. 2019;10:590.
Kara S, Crosswell H, Forch K, Cavadino A, McGeown J, Fulcher M. Less than half of patients recover within 2 weeks of injury after a sports-related mild traumatic brain injury: a 2-year prospective study. Clin J Sport Med. 2020;30(2):96–101.
McGeown JP, Kara S, Fulcher M, Crosswell H, Borotkanics R, Hume PA, et al. Predicting sport-related mTBI symptom resolution trajectory using initial clinical assessment findings: a retrospective cohort study. Sports Med. 2020;50(6):1191–202.
Bauman S, Ray M, Joseph PP. Gender differences in clinical presentation and recovery of sports related concussion. Br J Sports Med. 2017;51(11):A35-A.
Broshek D, Kaushik T, Freeman J, Erlanger D, Webbe F, Barth J. Sex differences in outcome following sports-related concussion. J Neurosurg. 2005;102(5):856–63.
Covassin T, Swanik C, Sachs M, Kendrick Z, Schatz P, Zillmer E, et al. Sex differences in baseline neuropsychological function and concussion symptoms of collegiate athletes. Br J Sports Med. 2006;40(11):923–7.
Tierney R, Sitler M, Swanik C, Swaink K, Higgins M, Torg J. Gender differences in head-neck segment dynamic stabilization during head acceleration. Med Sci Sports Exerc. 2005;37(2):272–9.
Sollmann N, Echlin PS, Schultz V, Viher PV, Lyall AE, Tripodis Y, et al. Sex differences in white matter alterations following repetitive subconcussive head impacts in collegiate ice hockey players. Neuroimage Clin. 2017;17:642–9.
Kanaan RA, Allin M, Picchioni M, Barker GJ, Daly E, Shergill SS, et al. Gender differences in white matter microstructure. PLoS ONE. 2012;7(6):e38272-e.
Wunderle K, Hoeger K, Wasserman E, Bazarian J. Menstrual phase as predictor of outcome after mild traumatic brain injury in women. J Head Trauma Rehabil. 2014;29:E1–8.
Duffy D, Elliott-Sale KJ, Gardner H, Goldenstein S, Wideman L. Endocrine responses to sport-related brain injury in female athletes: a narrative review and a call for action. Endocrines. 2021;2(2):99–108.
Solomito M, Reuman H, Wang D. Sex differences in concussion: a review of brain anatomy, function, and biomechanical response to impact. Brain Inj. 2019;33(2):105–10.
Dollé JP, Jaye A, Anderson SA, Ahmadzadeh H, Shenoy VB, Smith DH. Newfound sex differences in axonal structure underlie differential outcomes from in vitro traumatic axonal injury. Exp Neurol. 2018;300(Feb 2018):121–34.
Desai N, Wiebe DJ, Corwin DJ, Lockyer JE, Grady MF, Master CL. Factors affecting recovery trajectories in pediatric female concussion. Clin J Sport Med. 2019;29(5):361–7.
Gissane C, Jennings D, Kerr K, White J. A pooled data analysis of injury incidence in rugby league football. Sports Med. 2002;32(3):211–6.
King D, Gissane C, Clark T, Marshall S. The incidence of match and training injuries in rugby league: a pooled analysis of published studies. Int J Sport Sci Coach. 2014;9(2):417–31.
Friedenreich C. Methods for pooled analyses of epidemiologic studies. Epidemiology. 1993;4(4):295–302.
Blettner M, Sauerbrei W, Schlehofer B, Scheuchenpflug T, Friedenreich C. Traditional reviews, meta-analyses and pooled analyses in epidemiology. Int J Epidemiol. 1999;28(1):1–9.
Giacco D, McCabe R, Kallert T, Hansson L, Fiorillo A, Priebe S. Friends and symptom dimensions in patients with psychosis: a pooled analysis. PLoS ONE. 2012;7(11): e50119.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. J Clin Epidemiol. 2021;134:178–89.
Stroup D, Berlin J, Morton S, Olkin I, Williamson G, Rennie D, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. JAMA. 2000;283(15):2008–12.
von Elm E, Altman D, Egger M, Pocock S, Gøtzsche P, Vandenbroucke J. The strengthening the reporting of observational studies in epidemiology (STROBE) statement. Guidelines for reporting observational studies. Epidemiology. 2007;18(6):800–4.
Olmos M, Antelo M, Vazquez H, Smecuol E, Mauriño E, Bai JC. Systematic review and meta-analysis of observational studies on the prevalence of fractures in coeliac disease. Dig Liver Dis. 2008;40(1):46–53.
King D, Hume P, Milburn P, Gianotti S. Women’s rugby league injury claims and costs in New Zealand. Br J Sports Med. 2010;44(14):1016–23.
King D, Hume PA, Hardaker N, Cummins C, Clark T, Pearce AJ, et al. Female rugby union injuries in New Zealand: a review of five years (2013–2017) of Accident Compensation Corporation moderate to severe claims and costs. J Sci Med Sport. 2019;22(5):532–7.
King D, Gissane C, Brughelli M, Hume P, Harawira J. Sport-related concussions in New Zealand: a review of 10 years of Accident Compensation Corporation moderate to severe claims and costs. J Sci Med Sport. 2014;17(3):250–5.
King D, Hume PA, Hardaker N, Cummins C, Gissane C, Clark T. Sports-related injuries in New Zealand: National Insurance (Accident Compensation Corporation) claims for five sporting codes from 2012 to 2016. Br J Sports Med. 2019;53(16):1026–33.
King D, Hume PA, Hardaker N, Pearce A, Cummins C, Clark T. Traumatic brain injuries in New Zealand: National Insurance (Accident Compensation Corporation) claims from 2012 to 2016. J Neurol Sci. 2019;2019(399):61–8.
Brooks J, Fuller C. The influence of methodological issues on the results and conclusions from epidemiological studies of sports injuries: illustrative examples. Sports Med. 2006;36(6):459–72.
Orchard J, Hoskins W. For debate: consensus injury definitions in team sports should focus on missed match playing time. Clin J Sport Med. 2007;17(3):192–6.
Hodgson L, Gissane C, Gabbett T, King D. For debate: consensus injury definitions in team sports should focus on encompassing all injuries. Clin J Sport Med. 2007;17(3):188–91.
Swain M, Lystad R, Pollard H, Bonello R. Incidence and severity of neck injury in rugby union: a systematic review. J Sci Med Sport. 2011;14(5):383–9. https://doi.org/10.1016/j.jsams.2010.10.460.
Freitag A, Kirkwood G, Scharer S, Ofori-Asenso R, Pollock AM. Systematic review of rugby injuries in children and adolescents under 21 years. Br J Sports Med. 2015;49(8):511–9.
McElvenny D, Armstrong B, Järup L, Higgins J. Meta-analysis in occupational epidemiology: a review of practice. Occup Med (Lond). 2004;54(5):336–44.
Checkoway H. Data pooling in occupational studies. J Occup Med. 1991;33(12):1257–60.
Twellaar M, Verstappen F, Huson A. Is prevention of sports injuries a realistic goal? A four-year prospective investigation of sports injuries among physical education students. Am J Sports Med. 1996;24(4):528–34.
McHugh M. Lessons in biostatistics. Interrater reliability: the kappa statistic. Biochem Med. 2012;22(3):276–82.
Fuller CW, Taylor A. Eight-season epidemiological study of match injuries in women’s international rugby sevens. J Sports Sci. 2021;39(8):865–74.
Lopez V, Ma R, Weinstein M, Cantu R, Myers L, Nadkar N, et al. Concussive injuries in rugby 7s: an American experience and current review. Med Sci Sports Exerc. 2016;48(7):1320–30.
Lopez V, Ma R, Weinstein MG, Hume PA, Cantu RC, Victoria C, et al. United States under-19 rugby-7s: Incidence and nature of match injuries during a 5-year epidemiological study. Sports Med Open. 2020;6(1):41.
King DA, Hume PA, Gissane C, Kieser DC, Clark TN. Head impact exposure from match participation in women’s rugby league over one season of domestic competition. J Sci Med Sport. 2018;21(2):139–46.
King D, Hume P, Clark T, Foskett A, Barnes M. Incidence of match injuries in an amateur women’s rugby union team in New Zealand over two consecutive seasons. Adv Ortho Sports Med. 2020;2020(4):AOASM-129.
King D, Hume PA, Clark T, Foskett A, Barnes MJ. Training injury incidence in an amateur women’s rugby union team in New Zealand over two consecutive seasons. J Sci Med Sport. 2021;24(6):544–8.
Toohey LA, Drew MK, Finch CF, Cook JL, Fortington LV. A 2-year prospective study of injury epidemiology in elite Australian rugby sevens: exploration of incidence rates, severity, injury type, and subsequent injury in men and women. Am J Sports Med. 2019;47(6):1302–11. https://doi.org/10.1177/0363546518825380(0).
Langevin TL, Antonoff D, Renodin C, Shellene E, Spahr L, Marsh WA, et al. Head impact exposures in women’s collegiate rugby. Phys Sports Med. 2021;49(1):68–73.
Yeomans C, Kenny IC, Cahalan R, Warrington GD, Harrison AJ, Purtill H, et al. Injury trends in Irish amateur rugby: an epidemiological comparison of men and women. Sports Health. 2021;13(6):540–7. https://doi.org/10.1177/1941738121997145:1941738121997145.
Fuller C, Taylor A. World rugby surveillance studies: Women's rugby world cup 2017 review. World Rugby; 2017. https://playerwelfare.worldrugby.org/?documentid=181. Accessed 16 Jan 2018.
Fuller C, Taylor A. World rugby surveillance studies: Sevens world series (women). World Rugby; 2017. https://playerwelfare.worldrugby.org/?documentid=183. Accessed 12 Sep 2017.
Schick DM, Wiley J. 2006 RWC—women injury surveillance. World Rugby; 2006. https://playerwelfare.worldrugby.org/?documentid=31. Accessed 13 Mar 2020.
Havkins S. Head, neck, face and shoulder injuries in female and male rugby players. Phys Sports Med. 1986;14(7):111–8.
Gwinn D, Wilckens J, McDevitt E, Ross G, Kao T-C. The relative incidence of anterior cruciate ligament injury in men and women at the United States Naval Academy. Am J Sports Med. 2000;28(1):98–102.
Wetzler M, Akpata T, Laughlin W, Levy A. Occurrence of cervical spine injuries during the rugby scrum. Am J Sports Med. 1998;26(2):177–80.
Wetzler M, Akpata T, Albert T, Foster T, Levy A. A retrospective study of cervical spine injuries in American rugby, 1970 to 1994. Am J Sports Med. 1996;24(4):454–8.
Levy A, Wetzler M, Lewars M, Laughlin W. Knee injuries in women collegiate rugby players. Am J Sports Med. 1997;25(3):360–2.
Browne G. Cervical spinal injury in children’s community rugby football. Br J Sports Med. 2006;40(1):68–71.
Quarrie K, Cantu R, Chalmers D. Rugby union injuries to the cervical spine and spinal cord. Sports Med. 2002;32(10):633–53.
Bohu Y, Klouche S, Lefevre N, Peyrin J-C, Dusfour B, Hager J-P, et al. The epidemiology of 1345 shoulder dislocations and subluxations in French rugby union players: a five-season prospective study from 2008 to 2013. Br J Sports Med. 2015;49(23):1535–40.
Gerrard D, Waller A, Bird Y. The New Zealand rugby injury and performance project: II. Previous injury experience of a rugby-playing cohort. Br J Sports Med. 1994;28(4):229–33.
Comstock R, Knox C. Rugby RIO (Reporting Information Online) high school: Internet-based surveillance of injuries sustained by US high school players. California: US Rugby Foundation; 2005.
Richman P, Brogan G, Lechowicz M. Rugby injuries. Am J Emerg Med. 1998;16(3):327–8.
Pfister T, Pfister K, Hagel B, Ghali WA, Ronksley PE. The incidence of concussion in youth sports: a systematic review and meta-analysis. Br J Sports Med. 2016;50(5):292–7.
Teahan C, O’Connor S, Whyte EF. Injuries in Irish male and female collegiate athletes. Phys Ther Sport. 2021;51:1–7.
Cusimano M, Cho N, Amin K, Shirazi M, McFaull S, Do M, et al. Mechanisms of team-sport-related brain injuries in children 5 to 19 years old: opportunities for prevention. PLoS ONE. 2013;8(3): e58868. https://doi.org/10.1371/journal.pone.0058868.
Comstock R, Fields S. The fair sex? Foul play among female rugby players. J Sci Sport Med. 2005;8(1):101–10.
Comstock R. Patterns of injury among female rugby players. San Diego: University of California; 2002.
King D, Hume P, Gianotti S, Clark T. Neck back and spine injuries in amateur rugby league: a review of nine years of Accident Compensation Corporation injury entitlement claims and costs. J Sci Med Sport. 2011;14(2):126–9.
King D, Hume P, Milburn P, Gianotti S. Rugby league injuries in New Zealand: a review of 8 years of Accident Compensation Corporation injury entitlement claims and costs. Br J Sports Med. 2009;43(8):595–602.
King D, Hume P, Clark T, Hind K. Use of the Recovery-Stress Questionnaire—Sport (RESTQ-Sport) and King-Devick Test to monitor changes during recovery of concussion in an amateur women’s rugby union team. JSM Physical Med Rehabil. 2021;5(1):1014.
Lopez V Jr, Ma R, Weinstein MG, Chen JL, Black CM, Gupta AT, et al. An American experience with a new Olympic collision sport: Rugby sevens. Orthop J Sports Med. 2014;2(7): 2325967114S0005.
King D, Hume PA, Clark TN, Pearce AJ. Use of the King-Devick test for the identification of concussion in an amateur domestic women’s rugby union team over two competition seasons in New Zealand. J Neurol Sci. 2020;418:117162.
Ma R, Lopez VJ, Weinstein MG, Chen JL, Black CM, Gupta AT, et al. Injury profile of American women’s rugby-7s. Med Sci Sport Exerc. 2016;48(10):1957–66.
Prien A, Grafe A, Rössler R, Junge A, Verhagen E. Epidemiology of head injuries focusing on concussions in team contact sports: a systematic review. Sports Med. 2018;48(4):953–69.
Clay M, Glover K, Lowe D. Epidemiology of concussion in sport: a literature review. J Chiropr Med. 2013;12(4):230–51.
McGroarty N, Brown S, Mulcahey M. Sport-related concussion in female athletes: a systematic review. Orthop J Sports Med. 2020;8(7):2325967120932306.
Kirkwood G, Parekh N, Ofori-Asenso R, Pollock A. Concussion in youth rugby union and rugby league: a systematic review. Br J Sports Med. 2015;49(8):506–10.
Gianotti S, Hume P. A cost-outcome approach to pre and post-implementation of national sports injury prevention programmes. J Sci Med Sport. 2007;10(6):436–46.
Gianotti S, Hume P. Concussion sideline management intervention for rugby union leads to reduced concussion entitlement claims. NeuroRehabalitation. 2007;22(3):181–9.
McCrory P, Meeuwisse W, Dvořák J, Aubry M, Bailes J, Broglio S, et al. Consensus statement on concussion in sport—the 5th international conference on concussion in sport held in Berlin, October 2016. Br J Sports Med. 2017;51(11):838–47.
Harmon KG, Clugston JR, Dec K, Hainline B, Herring S, Kane SF, et al. American Medical Society for Sports Medicine position statement on concussion in sport. Br J Sports Med. 2019;53(4):213–25.
McCrea M, Guskiewicz K, Randolph C, Barr WB, Hammeke TA, Marshall SW, et al. Incidence, clinical course, and predictors of prolonged recovery time following sport-related concussion in high school and college athletes. J Int Neuropsychol Soc. 2013;19(1):22–33.
Hannah TC, Li AY, Spiera Z, Kuohn L, Dai J, McAuley F, et al. Sex-related differences in the incidence, severity, and recovery of concussion in adolescent student-athletes between 2009 and 2019. Am J Sports Med. 2021;49(7):1929–37.
Covassin T, Elbin R, Bleecker A, Lipchik A, Kontos A. Are there differences in neurocognitive function and symptoms between male and female soccer players after concussions? Am J Sports Med. 2013;41(12):2890–5.
Covassin T, Elbin R, Larson E, Kontos A. Sex and age differences in depression and baseline sport-related concussion neurocognitive performance and symptoms. Clin J Sport Med. 2012;22(2):98–104.
Lau B, Lovell M, Collins M, Pardini J. Neurocognitive and symptom predictors of recovery in high school athletes. Clin J Sport Med. 2009;19(3):216–21.
Sandel N, Reynolds E, Cohen PE, Gillie BL, Kontos AP. Anxiety and mood clinical profile following sport-related concussion: from risk factors to treatment. Sport Exerc Perform Psychol. 2017;6(3):304–23.
Fuller CW, Ashton T, Brooks JHM, Cancea RJ, Hall J, Kemp SPT. Injury risks associated with tackling in rugby union. Br J Sports Med. 2010;44(3):159–67.
Hammond LE, Lilley JM, Ribbans WJ. Defining recovery: an overlooked criterion in sports injury surveillance. Clin J Sport Med. 2013;23(3):157–9.
Fuller C, Molloy M, Bagate C, Bahr R, Brooks J, Donson H, et al. Consensus statement on injury definitions and data collection procedures for studies of injuries in rugby union. Clin J Sport Med. 2007;17(3):177–81.
Brown JC, Cross M, England M, Finch CF, Fuller GW, Kemp SPT, et al. Guidelines for community-based injury surveillance in rugby union. J Sci Med Sport. 2019;22(12):1314–8.
Gifford RM, Todisco T, Stacey M, Fujisawa T, Allerhand M, Woods DR, et al. Risk of heat illness in men and women: a systematic review and meta-analysis. Environ Res. 2019;171:24–35.
Sung E, Kim J. The influence of ovulation on postural stability (Biodex Balance System) in young female. J Exerc Rehabil. 2018;14(4):638–42.
dos Santos Andrade M, Mascarin N, Foster R, Jármy di Bella Z, Vincini R, Barbosa de Lira C. Is muscular strength balance influenced by menstrual cycle in female soccer players? J Sports Med Phys Fit. 2016;57(6):859–64.
Fouladi R, Rajabi R, Naseri N, Pourkazemi F, Geranmayeh M. Menstrual cycle and knee joint position sense in healthy female athletes. Knee Surg Sports Traumatol Arthrosc. 2012;20(8):1647–52.
Mihalik JP, Ondrak KS, Guskiewicz KM, McMurray RG. The effects of menstrual cycle phase on clinical measures of concussion in healthy college-aged females. J Sci Med Sport. 2009;12(3):383–7.
Wojtys EM, Huston LJ, Lindenfeld TN, Hewett TE, Greenfield MLVH. Association between the menstrual cycle and anterior cruciate ligament injuries in female athletes. Am J Sports Med. 1998;26(5):614–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions.
Conflicts of interest
Doug King, Patria Hume, Karen Hind, Trevor Clark and Natalie Hardaker declare that they have no conflicts of interest relevant to the contents of this review.
Author contributions
Contributor statement: According to the definition given by the International Committee of Medical Journal Editors (ICMJE), the authors listed qualify for authorship based on making one or more of the substantial contributions to the intellectual content of: conception and design (DK, TC); and/or acquisition of data (DK); and/or analysis and interpretation of data (DK, PH, TC); and/or participated in drafting of the manuscript (DK, PH, TC, NH); and/or critical revision of the manuscript for important intellectual content (DK, PH, TC, NH); and all authors read and approved the final manuscript.
Data availability
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
King, D.A., Hume, P.A., Hind, K. et al. The Incidence, Cost, and Burden of Concussion in Women’s Rugby League and Rugby Union: A Systematic Review and Pooled Analysis. Sports Med 52, 1751–1764 (2022). https://doi.org/10.1007/s40279-022-01645-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-022-01645-8