Abstract
Objective
To develop a predictive model for sport-related concussion in collegiate athletes and military service academy cadets using baseline data collecting during the pre-participation examination.
Methods
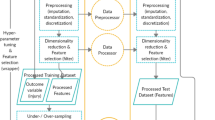
Baseline assessments were performed in 15,682 participants from 21 US academic institutions and military service academies participating in the CARE Consortium Study during the 2015–2016 academic year. Participants were monitored for sport-related concussion during the subsequent season. 176 baseline covariates mapped to 957 binary features were used as input into a support vector machine model with the goal of learning to stratify participants according to their risk for sport-related concussion. Performance was evaluated in terms of area under the receiver operating characteristic curve (AUROC) on a held-out test set. Model inputs significantly associated with either increased or decreased risk were identified.
Results
595 participants (3.79%) sustained a concussion during the study period. The predictive model achieved an AUROC of 0.73 (95% confidence interval 0.70–0.76), with variable performance across sports. Features with significant positive and negative associations with subsequent sport-related concussion were identified.
Conclusion(s)
This predictive model using only baseline data identified athletes and cadets who would go on to sustain sport-related concussion with comparable accuracy to many existing concussion assessment tools for identifying concussion. Furthermore, this study provides insight into potential concussion risk and protective factors.



Similar content being viewed by others
References
Langlois JA, Rutland-Brown W, Wald MM. The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehabil. 2006;21(5):375–8.
National Collegiate Athletic Association. Number of NCAA college athletes reaches all-time high. 2018.
US Department of Defense. Special report—traumatic brain injury. 2015.
BrainLine, How Many Service Members Have Sustained a TBI? Defense Medical Surveillance System, 2018.
Guskiewicz KM, et al. Recurrent concussion and risk of depression in retired professional football players. Med Sci Sports Exerc. 2007;39(6):903–9.
Guskiewicz KM, et al. Association between recurrent concussion and late-life cognitive impairment in retired professional football players. Neurosurgery. 2005;57(4):719–26 (discussion 719–2).
McKee AC, et al. Chronic traumatic encephalopathy in athletes: progressive tauopathy after repetitive head injury. J Neuropathol Exp Neurol. 2009;68(7):709–35.
McKee AC, et al. The spectrum of disease in chronic traumatic encephalopathy. Brain. 2013;136(Pt 1):43–64.
McKee AC, et al. The neuropathology of chronic traumatic encephalopathy. Brain Pathol. 2015;25(3):350–64.
Mez J, et al. Clinicopathological evaluation of chronic traumatic encephalopathy in players of American Football. JAMA. 2017;318(4):360–70.
Caccese JB et al. Does baseline concussion testing aid in identifying future concussion risk? Res Sports Med. 2019:1–6.
Abrahams S, et al. Risk factors for sports concussion: an evidence-based systematic review. Br J Sports Med. 2014;48(2):91–7.
Harmon KG, et al. American Medical Society for Sports Medicine position statement: concussion in sport. Br J Sports Med. 2013;47(1):15–26.
Kerr HA. Concussion risk factors and strategies for prevention. Pediatr Ann. 2014;43(12):e309–15.
Noble JM, Hesdorffer DC. Sport-related concussions: a review of epidemiology, challenges in diagnosis, and potential risk factors. Neuropsychol Rev. 2013;23(4):273–84.
Finnoff JT, Jelsing EJ, Smith J. Biomarkers, genetics, and risk factors for concussion. PM R. 2011;3(10 Suppl 2):S452–9.
Hollis SJ, et al. Incidence, risk, and protective factors of mild traumatic brain injury in a cohort of Australian nonprofessional male rugby players. Am J Sports Med. 2009;37(12):2328–33.
Schneider KJ, et al. Preseason reports of neck pain, dizziness, and headache as risk factors for concussion in male youth ice hockey players. Clin J Sport Med. 2013;23(4):267–72.
Curran-Sills G, Abedin T. Risk factors associated with injury and concussion in sanctioned amateur and professional mixed martial arts bouts in Calgary, Alberta. BMJ Open Sport Exerc Med. 2018;4(1):e000348.
Yeung A, Munjal V, Virji-Babul N. Development of the sports organization concussion risk assessment tool (SOCRAT). Brain Inj. 2017;31(4):542–9.
Baugh CM, et al. Frequency of head-impact-related outcomes by position in NCAA division I collegiate football players. J Neurotrauma. 2015;32(5):314–26.
Black AM, et al. Policy change eliminating body checking in non-elite ice hockey leads to a threefold reduction in injury and concussion risk in 11- and 12-year-old players. Br J Sports Med. 2016;50(1):55–61.
Blumenfeld RS, et al. The epidemiology of sports-related head injury and concussion in water polo. Front Neurol. 2016;7:98.
Hollis SJ, et al. Mild traumatic brain injury among a cohort of rugby union players: predictors of time to injury. Br J Sports Med. 2011;45(12):997–9.
Teramoto M, et al. Style of play and rate of concussions in the national football league. Orthop J Sports Med. 2015;3(12):2325967115620365.
Collins CL, et al. Neck strength: a protective factor reducing risk for concussion in high school sports. J Prim Prev. 2014;35(5):309–19.
Dretsch MN, et al. Evaluating the clinical utility of the Validity-10 for detecting amplified symptom reporting for patients with mild traumatic brain injury and comorbid psychological health conditions. Appl Neuropsychol Adult. 2017;24(4):376–80.
Van Pelt KL, et al. A cohort study to identify and evaluate concussion risk factors across multiple injury settings: findings from the CARE Consortium. Inj Epidemiol. 2019;6(1):1.
Schulz MR, et al. Incidence and risk factors for concussion in high school athletes, North Carolina, 1996–1999. Am J Epidemiol. 2004;160(10):937–44.
Broglio SP, et al. A national study on the effects of concussion in collegiate athletes and US military service academy members: the NCAA-DoD concussion assessment, research and education (CARE) consortium structure and methods. Sports Med. 2017;47(7):1437–51.
Carney N, et al. Concussion guidelines step 1: systematic review of prevalent indicators. Neurosurgery. 2014;75(Suppl 1):S3–15.
Cortes C, Vapnik V. Support-vector networks. Mach Learn. 1995;20(3):273–97.
Ustun B, Traca S, Rudin C. Cynthia supersparse linear integer models for interpretable classification. 2014. arXiv:1306.6677.
Kohavi R. A study of cross-validation and bootstrap for accuracy estimation and model selection. In Proceedings of the 14th international joint conference on Artificial intelligence—Volume 2. 1995, Morgan Kaufmann Publishers Inc.: Montreal, Quebec, Canada. p. 1137–1143.
Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology. 1982;143(1):29–36.
Wasserman EB, et al. Academic dysfunction after a concussion among US High School and College Students. Am J Public Health. 2016;106(7):1247–53.
Manley G, et al. A systematic review of potential long-term effects of sport-related concussion. Br J Sports Med. 2017;51(12):969–77.
Barlow M, et al. Differences in change scores and the predictive validity of three commonly used measures following concussion in the middle school and high school aged population. Int J Sports Phys Ther. 2011;6(3):150–7.
Randolph C, et al. Concussion symptom inventory: an empirically derived scale for monitoring resolution of symptoms following sport-related concussion. Arch Clin Neuropsychol. 2009;24(3):219–29.
Barr WB, McCrea M. Sensitivity and specificity of standardized neurocognitive testing immediately following sports concussion. J Int Neuropsychol Soc. 2001;7(6):693–702.
Mucha A, et al. A Brief Vestibular/Ocular Motor Screening (VOMS) assessment to evaluate concussions: preliminary findings. Am J Sports Med. 2014;42(10):2479–86.
Schmidt JD, et al. Age at first concussion influences the number of subsequent concussions. Pediatr Neurol. 2018;81:19–24.
Stamm JM, et al. Age at first exposure to football is associated with altered corpus callosum white matter microstructure in former professional football players. J Neurotrauma. 2015;32(22):1768–76.
Stamm JM, et al. Age of first exposure to football and later-life cognitive impairment in former NFL players. Neurology. 2015;84(11):1114–20.
Alosco ML, et al. Age of first exposure to American football and long-term neuropsychiatric and cognitive outcomes. Transl Psychiatry. 2017;7(9):e1236.
Schultz V, et al. Age at first exposure to repetitive head impacts is associated with smaller thalamic volumes in former professional american football players. J Neurotrauma. 2018;35(2):278–85.
Caccese JB, et al. Estimated age of first exposure to american football and neurocognitive performance amongst NCAA male student-athletes: a cohort study. Sports Med. 2019;49(3):477–87.
Caccese JB et al. Estimated age of first exposure to contact sports is not associated with greater symptoms or worse cognitive functioning in male U.S. Service Academy Athletes. J Neurotrauma. 2020;37(2):334–9.
Brett BL, et al. Age of first exposure to american football and behavioral, cognitive, psychological, and physical outcomes in high school and collegiate football players. Sports Health. 2019;11(4):332–42.
Koh JO, Cassidy JD, Watkinson EJ. Incidence of concussion in contact sports: a systematic review of the evidence. Brain Inj. 2003;17(10):901–17.
Hootman JM, Dick R, Agel J. Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives. J Athl Train. 2007;42(2):311–9.
Marar M, et al. Epidemiology of concussions among United States high school athletes in 20 sports. Am J Sports Med. 2012;40(4):747–55.
Giza CC, et al. Summary of evidence-based guideline update: evaluation and management of concussion in sports: Report of the Guideline Development Subcommittee of the American Academy of Neurology. Neurology. 2013;80(24):2250–7.
Dick RW. Is there a gender difference in concussion incidence and outcomes? Br J Sports Med. 2009;43(Suppl 1):i46–50.
Lipton RB, et al. A self-administered screener for migraine in primary care: the ID Migraine validation study. Neurology. 2003;61(3):375–82.
Eckner JT, et al. Is migraine headache associated with concussion in athletes? A case-control study. Clin J Sport Med. 2017;27(3):266–70.
Gordon KE, Dooley JM, Wood EP. Is migraine a risk factor for the development of concussion? Br J Sports Med. 2006;40(2):184–5.
Alosco ML, Fedor AF, Gunstad J. Attention deficit hyperactivity disorder as a risk factor for concussions in NCAA division-I athletes. Brain Inj. 2014;28(4):472–4.
Acknowledgements
This project was supported, in part, with support from the Grand Alliance Concussion Assessment, Research, and Education (CARE) Consortium, funded, in part by the National Collegiate Athletic Association (NCAA) and the Department of Defense (DOD). The U.S. Army Medical Research Acquisition Activity, 820 Chandler Street, Fort Detrick MD 21702-5014 is the awarding and administering acquisition office. This work was supported by the Office of the Assistant Secretary of Defense for Health Affairs through the Combat Casualty Care Program, endorsed by the Department of Defense under Award No. W81XWH-BA170608. Opinions, interpretations, conclusions and recommendations are those of the author and are not necessarily endorsed by the Office of the Assistant Secretary of Defense for Health Affairs.
The authors thank Kaitlyn Carter (Azusa Pacific University); Jennifer Brewington Dickerson, Jody Harland, Nicole Johnson, Janetta Matesan, Nicholas Port, Larry Riggen (Indiana University); Margot Putukian (Princeton University); Gerald McGinty (United States Air Force Academy); Patrick G. O’Donnell, Carlos Esteves (United States Coast Guard Academy); Ken Cameron (United States Military Academy); Tom Kaminski (University of Delaware); Julianne Schmidt (University of Georgia); Josh Goldman (University of California Los Angeles); Ashley Rettmann (University of Michigan); Kevin Guskiewicz (University of North Carolina at Chapel Hill); Scott Anderson (University of Oklahoma); Jeffery J Bazarian (University of Rochester); Sara Chrisman (University of Washington); Alison Brooks (University of Wisconsin); Stefan Duma (Virginia Polytechnic Institute and State University); and research and medical staff at each of the CARE participation sites.
Care Consortium Investigators are listed alphabetically by institution: April (Reed) Hoy, Azusa Pacific University; Louise Kelly, California Lutheran University; Jonathan Jackson, United States Air Force Academy; Tim Kelly, United States Military Academy; Thomas Buckley, University of Delaware; James (Jay) R. Clugston, University of Florida; Justus Ortega, Humboldt State University; Anthony Kontos, University of Pittsburgh; Christopher C. Giza, University of California Los Angeles; Jason Mihalik, University of North Carolina at Chapel Hill; Steve Rowson, Virginia Polytechnic Institute and State University.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Funding
This project was supported, in part, with support from the Grand Alliance Concussion Assessment, Research, and Education (CARE) Consortium, funded, in part by the National Collegiate Athletic Association (NCAA) and the Department of Defense (DOD). The U.S. Army Medical Research Acquisition Activity, 820 Chandler Street, Fort Detrick MD 21702-5014 is the awarding and administering acquisition office. This work was supported by the Office of the Assistant Secretary of Defense for Health Affairs through the Combat Casualty Care Program, endorsed by the Department of Defense under Award No. W81XWH-BA170608. Opinions, interpretations, conclusions and recommendations are those of the author and are not necessarily endorsed by the Office of the Assistant Secretary of Defense for Health Affairs.
Conflict of interest
The authors whose names are listed immediately below certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript: Castellanos and Wiens. The authors whose names are listed immediately below certify that grant support for this project was received from the Grand Alliance Concussion Assessment, Research, and Education (CARE) Consortium, funded, in part by the NCAA and the DoD: Phoo, Eckner, Franco, Broglio, McCrea, McAllister. The authors whose names are listed immediately below also certify that travel support was provided by the Grand Alliance Concussion Assessment, Research, and Education (CARE) Consortium, funded, in part by the NCAA and the DoD: Eckner, Franco, Broglio, and McCrea. The authors whose names are listed immediately below certify additional disclosures that do not have financial interest in the subject matter discussed in this manuscript as detailed in their author declaration forms: Eckner (patent, grant funding), Broglio (consultation, expert testimony, grant funding, advisory and editorial boards), and McCrea (grant funding, consultation).
Ethics approval
Institutional Review Board (IRB) approval was obtained at the University of Michigan (lead study site), with US Department of Defense Human Research Protection Office approval as well as local IRB approval at each participating site. This study was performed in accordance with the standards of ethics outlined in the Declaration of Helsinki.
Consent to participate
All participants provided informed written consent.
Consent for publication
Not applicable. No identifiable information or images are included in this publication.
Availability of data
CARE Consortium data are publically available upon request from the Federal Interagency Traumatic Brain Injury Research (FITBIR) Informatics System.
Code availability
The authors are willing to provide the data analysis code upon written request.
Author contributions
Dr. Castellanos contributed to the conception and design of the work; data interpretation; drafting and revision of the manuscript. He approved the final published version and agreed to be accountable for all aspects of the work. Mr. Phoo contributed to the design of the work; data analysis and interpretation; drafting and revision of the manuscript. He approved the final published version and agreed to be accountable for all aspects of the work. Dr. Eckner contributed to the conception and design of the work; data acquisition, analysis, and interpretation; drafting and revision of the manuscript. He approved the final published version and agreed to be accountable for all aspects of the work. Ms. Franco contributed to data acquisition and interpretation; critical revision of the manuscript for intellectual content. She approved the final published version and agreed to be accountable for all aspects of the work. Drs. Broglio, McCrea, and McAllister contributed to the design of the work; data interpretation; critical revision of the manuscript for intellectual content. They approved the final published version and agreed to be accountable for all aspects of the work. Dr. Wiens contributed to the conception and design of the work; data analysis and interpretation; drafting and revision of the manuscript. She approved the final published version and agreed to be accountable for all aspects of the work. The CARE Consortium Investigators (Ms. Hoy, Dr. Kelly, Dr. Jackson, Mr. Kelly, Dr. Buckley, Dr. Clugston, Dr. Ortega, Dr. Kontos, Dr. Giza, Dr. Mihalik, Dr. Rowson) contributed to data acquisition and interpretation and critical revision of the manuscript for intellectual content. They approved the final published version and agreed to be accountable for all aspects of the work.
Additional information
The members of The CARE Consortium Investigators are mentioned in “Acknowledgements” section.
This article is part of a collection on The NCAA-DoD Concussion Assessment, Research and Education (CARE) Consortium.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Castellanos, J., Phoo, C.P., Eckner, J.T. et al. Predicting Risk of Sport-Related Concussion in Collegiate Athletes and Military Cadets: A Machine Learning Approach Using Baseline Data from the CARE Consortium Study. Sports Med 51, 567–579 (2021). https://doi.org/10.1007/s40279-020-01390-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-020-01390-w