Abstract
Passive exercise/movement has a long history in both medicine and physiology. Early clinical applications of passive exercise/movement utilized pneumatic and direct limb compression to stimulate the vasculature and evoke changes in blood flow to avoid complications brought about by stasis and vascular disease. Over the last 50 years, passive exercise/movement has continued to progress and has provided physiologists with a reductionist approach to mechanistically examine the cardiorespiratory, hyperemic, and afferent responses to movement without the confounding influence of metabolism that accompanies active exercise. This review, in addition to providing an historical perspective, focuses on the recent advancements utilizing passive leg movement, and how the hyperemic response at the onset of this passive movement has evolved from a method to evaluate the central and peripheral regulation of blood flow during exercise to an innovative and promising tool to assess vascular function. As an assessment of vascular function, passive leg movement is relatively simple to perform and provides a nitric oxide-dependent evaluation of endothelial function across the lifespan that is sensitive to changes in activity/fitness and disease state (heart failure, peripheral artery disease, sepsis). The continual refinement and characterization of passive leg movement are aimed at improving our understanding of blood flow regulation and the development of a clinically ready approach to predict and monitor the progression of cardiovascular disease.

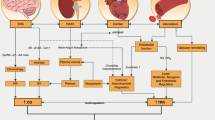
Modified from Nobrega et al. [29]

Modified from Radegran and Saltin [46]

Modified from McDaniel et al. [33]

Modified from Groot et al. [52]

Modified from Trinity et al. [40]

Modified from Rossman et al. [54]


Similar content being viewed by others
References
Murray J. Nature and treatment of cholera: new method proposed. Lond Med Surg J. 1832;1:749–52.
Clanny WR. Apparatus for removing the pressure of the atmosphere from the body or limbs. Lancet. 1835;23(601):804–5.
Junod V-T. Recherches physiologiques et thérapeutiques sur les effets de la compression et de la raréfaction de l’air, tant sur le corps que sur les membres isolés. Rev Med Franc Estrange. 1834;3:350–68.
Bluck E. Improved means or appliances for promoting or modifying the circulation of the blood in a living body. London: Darling and Sons; 1888.
Sinkowitz S, Gottlieb I. Thrombo-angiitis obliterans: the conservative treatment by Bier’s ilyperemia suction apparatus. JAMA. 1917;68(13):961–3.
Herrmann LG, Reid MR. The conservative treatment of arteriosclerotic peripheral vascular diseases: passive vascular exercises (Pavaex therapy). Ann Surg. 1934;100(4):750–60.
Herrmann LG, Reid MR. Passive vascular exercises: treatment of peripheral obliterative arterial diseases by rhythmic alternation of environmental pressure. Arch Surg. 1934;29(5):697–704.
Reid MR, Herrmann LG. Treatment of obliterative vascular diseases by means of an intermittent negative pressure environment. J Med. 1933;14(June):200.
Roberts V, Sabri S, Pietroni M, Gurewich V, Cotton L. Passive flexion and femoral vein flow: a study using a motorized foot mover. Br Med J. 1971;3(5766):78–81.
Sabri S, Roberts V, Cotton L. Prevention of early postoperative deep vein thrombosis by intermittent compression of the leg during surgery. Br Med J. 1971;4(5784):394–6.
Chen A, Frangos S, Kilaru S, Sumpio B. Intermittent pneumatic compression devices: physiological mechanisms of action. Eur J Vasc Endovasc Surg. 2001;21(5):383–92.
Morgan RH, Carolan G, Psaila JV, Gardner AMN, Fox RH, Woodcock JP. Arterial flow enhancement by impulse compression. Vascular Surg. 1991;25(1):8–16. https://doi.org/10.1177/153857449102500102.
Nicolaides AN, Fernandes e Fernandes J, Pollock AV. Intermittent sequential pneumatic compression of the legs in the prevention of venous stasis and postoperative deep venous thrombosis. Surgery. 1980;87(1):69–76.
van Bemmelen PS, Mattos MA, Faught WE, Mansour MA, Barkmeier LD, Hodgson KJ, et al. Augmentation of blood flow in limbs with occlusive arterial disease by intermittent calf compression. J Vasc Surg. 1994;19(6):1052–8. https://doi.org/10.1016/S0741-5214(94)70217-9.
Geppert J, Zuntz N. Ueber die Regulation der Athmung. Archiv für die gesamte Physiologie des Menschen und der Tiere. 1888;42(1):189–245. https://doi.org/10.1007/bf01669357.
Dixon ME, Stewart PB, Mills FC, Varvis CJ, Bates DV. Respiratory consequences of passive body movement. J Appl Physiol. 1961;16(1):30–4. https://doi.org/10.1152/jappl.1961.16.1.30.
Flandrois R, Lacour JR, Islas-Maroquin J, Charlot J. Limbs mechanoreceptors inducing the reflex hyperpnea of exercise. Respir Physiol. 1967;2(3):335–43. https://doi.org/10.1016/0034-5687(67)90038-2.
Nobrega AC, Williamson JW, Friedman DB, Araujo CG, Mitchell JH. Cardiovascular responses to active and passive cycling movements. Med Sci Sports Exerc. 1994;26(6):709–14.
Asmussen E, Johansen SH, Jorgensen M, Nielsen M. On the nervous factors controlling respiration and circulation during exercise: experiments with curarization. Acta Physiol (Oxf). 1965;63(3):343–50. https://doi.org/10.1111/j.1748-1716.1965.tb04073.x.
Asmussen E, Nielsen M, Wieth-Federsen G. On the regulation of circulation during muscular work. Acta Physiol (Oxf). 1943;6(4):353–8. https://doi.org/10.1111/j.1748-1716.1943.tb02861.x.
Galbo H, Kjaer M, Secher NH. Cardiovascular, ventilatory and catecholamine responses to maximal dynamic exercise in partially curarized man. J Physiol. 1987;389(1):557–68. https://doi.org/10.1113/jphysiol.1987.sp016672.
Hollander AP, Bouman LN. Cardiac acceleration in man elicited by a muscle-heart reflex. J Appl Physiol. 1975;38(2):272–8.
Hornbein TF, Sorensen SC, Parks CR. Role of muscle spindles in lower extremities in breathing during bicycle exercise. J Appl Physiol. 1969;27(4):476–9. https://doi.org/10.1152/jappl.1969.27.4.476.
Iwamoto GA, Mitchell JH, Mizuno M, Secher NH. Cardiovascular-responses at the onset of exercise with partial neuromuscular blockade in cat and man. J Physiol. 1987;384(1):39–47. https://doi.org/10.1113/jphysiol.1987.sp016442.
Kjaer M, Hanel B, Worm L, Perko G, Lewis SF, Sahlin K, et al. Cardiovascular and neuroendocrine responses to exercise in hypoxia during impaired neural feedback from muscle. Am J Physiol. 1999;277(1):R76–85. https://doi.org/10.1152/ajpregu.1999.277.1.R76.
Kjaer M, Perko G, Secher NH, Boushel R, Beyer N, Pollack S, et al. Cardiovascular and ventilatory responses to electrically induced cycling with complete epidural anaesthesia in humans. Acta Physiol (Oxf). 1994;151(2):199–207. https://doi.org/10.1111/j.1748-1716.1994.tb09738.x.
Strange S, Secher NH, Pawelczyk JA, Karpakka J, Christensen NJ, Mitchell JH, et al. Neural control of cardiovascular responses and of ventilation during dynamic exercise in man. J Physiol. 1993;470(1):693–704. https://doi.org/10.1113/jphysiol.1993.sp019883.
Waisbren SJ, Whiting CS, Nadel ER. Effects of passive limb movement on pulmonary ventilation. Yale J Biol Med. 1990;63(6):549–56.
Nobrega AC, Araujo CG. Heart rate transient at the onset of active and passive dynamic exercise. Med Sci Sports Exerc. 1993;25(1):37–41.
Radegran G, Saltin B. Muscle blood flow at onset of dynamic exercise in humans. Am J Physiol Heart Circ Physiol. 1998;274(1):H314–22.
Wray DW, Donato AJ, Uberoi A, Merlone JP, Richardson RS. Onset exercise hyperaemia in humans: partitioning the contributors. J Physiol. 2005;565(3):1053–60. https://doi.org/10.1113/jphysiol.2005.084327.
Gonzalez-Alonso J, Mortensen SP, Jeppesen TD, Ali L, Barker H, Damsgaard R, et al. Haemodynamic responses to exercise, ATP infusion and thigh compression in humans: insight into the role of muscle mechanisms on cardiovascular function. J Physiol. 2008;586(9):2405–17. https://doi.org/10.1113/jphysiol.2008.152058.
McDaniel J, Fjeldstad AS, Ives S, Hayman M, Kithas P, Richardson RS. Central and peripheral contributors to skeletal muscle hyperemia: response to passive limb movement. J Appl Physiol. 2010;108(1):76–84. https://doi.org/10.1152/japplphysiol.00895.2009.
Ter Woerds W, De Groot PCE, van Kuppevelt DHJM, Hopman MTE. Passive leg movements and passive cycling do not alter arterial leg blood flow in subjects with spinal cord injury. Phys Ther. 2006;86(5):636–45.
Fernandes A, Galbo H, Kjaer M, Mitchell JH, Secher NH, Thomas SN. Cardiovascular and ventilatory responses to dynamic exercise during epidural anaesthesia in man. J Physiol. 1990;420(1):281–93. https://doi.org/10.1113/jphysiol.1990.sp017912.
Trinity JD, Amann M, McDaniel J, Fjeldstad AS, Barret-O’Keefe Z, Runnels S, et al. Limb movement-induced hyperemia has a central hemodynamic component; eidence from a neural blockade study. Am J Physiol Heart Circ Physiol. 2010;299(5):H1693–700. https://doi.org/10.1152/ajpheart.00482.2010.
Venturelli M, Amann M, Layec G, McDaniel J, Trinity JD, Fjeldstad AS, et al. Passive leg movement-induced hyperaemia with a spinal cord lesion: evidence of preserved vascular function. Acta Physiol (Oxf). 2014;210(2):429–39. https://doi.org/10.1111/apha.12173.
Ives SJ, McDaniel J, Witman MA, Richardson RS. Passive limb movement: evidence of mechanoreflex sex specificity. Am J Physiol Heart Circ Physiol. 2013;304(1):H154–61. https://doi.org/10.1152/ajpheart.00532.2012.
Ives SJ, Amann M, Venturelli M, Witman MA, Groot HJ, Wray DW, et al. The mechanoreflex and hemodynamic response to passive leg movement in heart failure. Med Sci Sports Exerc. 2016;48(3):368–76. https://doi.org/10.1249/MSS.0000000000000782.
Trinity JD, Groot HJ, Layec G, Rossman MJ, Ives SJ, Runnels S, et al. Nitric oxide and passive limb movement: a new approach to assess vascular function. J Physiol. 2012;590(6):1413–25. https://doi.org/10.1113/jphysiol.2011.224741.
Lawrenson L, Poole JG, Kim J, Brown C, Patel P, Richardson RS. Vascular and metabolic response to isolated small muscle mass exercise: effect of age. Am J Physiol Heart Circ Physiol. 2003;285(3):H1023–31. https://doi.org/10.1152/ajpheart.00135.2003.
Poole JG, Lawrenson L, Kim J, Brown C, Richardson RS. Vascular and metabolic response to cycle exercise in sedentary humans: effect of age. Am J Physiol Heart Circ Physiol. 2003;284(4):H1251–9. https://doi.org/10.1152/ajpheart.00790.2002.
McDaniel J, Hayman MA, Ives SJ, Fjeldstad AS, Trinity JD, Wray DW, et al. Attenuated exercise induced hyperemia with age: mechanistic insight from passive limb movement. J Physiol. 2010. https://doi.org/10.1113/jphysiol.2010.198770.
Bada AA, Svendsen JH, Secher NH, Saltin B, Mortensen SP. Peripheral vasodilatation determines cardiac output in exercising humans: insight from atrial pacing. J Physiol. 2012;590(8):2051–60. https://doi.org/10.1113/jphysiol.2011.225334.
Mortensen SP, Askew CD, Walker M, Nyberg M, Hellsten Y. The hyperaemic response to passive leg movement is dependent on nitric oxide: a new tool to evaluate endothelial nitric oxide function. J Physiol. 2012;590(17):4391–400. https://doi.org/10.1113/jphysiol.2012.235952.
Radegran G, Saltin B. Nitric oxide in the regulation of vasomotor tone in human skeletal muscle. Am J Physiol. 1999;276(6):H1951–60. https://doi.org/10.1152/ajpheart.1999.276.6.H1951.
Celermajer DS, Sorensen KE, Spiegelhalter DJ, Georgakopoulos D, Robinson J, Deanfield JE. Aging is associated with endothelial dysfunction in healthy-men years before the age-related decline in women. J Am Coll Cardiol. 1994;24(2):471–6. https://doi.org/10.1016/0735-1097(94)90305-0.
Taddei S, Galetta F, Virdis A, Ghiadoni L, Salvetti G, Franzoni F, et al. Physical activity prevents age-related impairment in nitric oxide availability in elderly athletes. Circulation. 2000;101(25):2896–901. https://doi.org/10.1161/01.cir.101.25.2896.
DeSouza CA, Shapiro LF, Clevenger CM, Dinenno FA, Monahan KD, Tanaka H, et al. Regular aerobic exercise prevents and restores age-related declines in endothelium-dependent vasodilation in healthy men. Circulation. 2000;102(12):1351–7.
Celermajer DS, Sorensen KE, Gooch VM, Spiegelhalter DJ, Miller OI, Sullivan ID, et al. Non-invasive detection of endothelial dysfunction in children and adults at risk of atherosclerosis. Lancet. 1992;340(8828):1111–5.
Trinity JD, Groot HJ, Layec G, Rossman MJ, Ives SJ, Morgan DE, et al. Passive leg movement and nitric oxide-mediated vascular function: the impact of age. Am J Physiol Heart Circ Physiol. 2015;308(6):H672–9. https://doi.org/10.1152/ajpheart.00806.2014.
Groot HJ, Trinity JD, Layec G, Rossman MJ, Ives SJ, Morgan DE, et al. The role of nitric oxide in passive leg movement-induced vasodilatation with age: insight from alterations in femoral perfusion pressure. J Physiol. 2015;593(17):3917–28. https://doi.org/10.1113/jp270195.
Groot HJ, Rossman MJ, Trinity JD, Layec G, Ives SJ, Richardson RS. Passive leg movement-induced vasodilation in women: the impact of age. Am J Physiol Heart Circ Physiol. 2015;309(5):H995–1002. https://doi.org/10.1152/ajpheart.00422.2015.
Rossman MJ, Groot HJ, Garten RS, Witman MA, Richardson RS. Vascular function assessed by passive leg movement and flow-mediated dilation: initial evidence of construct validity. Am J Physiol Heart Circ Physiol. 2016;311(5):H1277–86. https://doi.org/10.1152/ajpheart.00421.2016.
Walker MA, Hoier B, Walker PJ, Schulze K, Bangsbo J, Hellsten Y, et al. Vasoactive enzymes and blood flow responses to passive and active exercise in peripheral arterial disease. Atherosclerosis. 2016;246:98–105. https://doi.org/10.1016/j.atherosclerosis.2015.12.029.
Gokce N, Keaney JF, Hunter LM, Watkins MT, Nedeljkovic ZS, Menzoian JO, et al. Predictive value of noninvasivelydetermined endothelial dysfunction for long-term cardiovascular events inpatients with peripheral vascular disease. J Am Coll Cardiol. 2003;41(10):1769–75. https://doi.org/10.1016/s0735-1097(03)00333-4.
Hirsch L, Shechter A, Feinberg MS, Koren-Morag N, Shechter M. The impact of early compared to late morning hours on brachial endothelial function and long-term cardiovascular events in healthy subjects with no apparent coronary heart disease. Int J Cardiol. 2011;151(3):342–7. https://doi.org/10.1016/j.ijcard.2010.08.069.
Yeboah J, Crouse JR, Hsu FC, Burke GL, Herrington DM. Brachial flow-mediated dilation predicts incident cardiovascular events in older adults: the Cardiovascular Health Study. Circulation. 2007;115(18):2390–7. https://doi.org/10.1161/CIRCULATIONAHA.106.678276.
Yeboah J, Folsom AR, Burke GL, Johnson C, Polak JF, Post W, et al. Predictive value of brachial flow-mediated dilation for incident cardiovascular events in a population-based study: the multi-ethnic study of atherosclerosis. Circulation. 2009;120(6):502–9. https://doi.org/10.1161/CIRCULATIONAHA.109.864801.
Burns KJ, Pollock BS, McDaniel J. The cardiovascular response to passive movement is joint dependent. Physiol Rep. 2016. https://doi.org/10.14814/phy2.12721.
Nishiyama SK, Wray DW, Richardson RS. Aging affects vascular structure and function in a limb-specific manner. J Appl Physiol. 2008;105(5):1661–70. https://doi.org/10.1152/japplphysiol.90612.2008.
Richardson RS, Secher NH, Tschakovsky ME, Proctor DN, Wray DW. Metabolic and vascular limb differences affected by exercise, gender, age, and disease. Med Sci Sports Exerc. 2006;38(10):1792–6. https://doi.org/10.1249/01.mss.0000229568.17284.ab.
Bellien J, Iacob M, Gutierrez L, Isabelle M, Lahary A, Thuillez C, et al. Crucial role of NO and endothelium-derived hyperpolarizing factor in human sustained conduit artery flow-mediated dilatation. Hypertension. 2006;48(6):1088–94. https://doi.org/10.1161/01.HYP.0000246672.72188.bd.
Bellien J, Iacob M, Remy-Jouet I, Lucas D, Monteil C, Gutierrez L, et al. Epoxyeicosatrienoic acids contribute with altered nitric oxide and endothelin-1 pathways to conduit artery endothelial dysfunction in essential hypertension. Circulation. 2012;125(10):1266–75. https://doi.org/10.1161/CIRCULATIONAHA.111.070680.
Busse R, Edwards G, Feletou M, Fleming I, Vanhoutte PM, Weston AH. EDHF: bringing the concepts together. Trends Pharmacol Sci. 2002;23(8):374–80.
Joannides R, Haefeli WE, Linder L, Richard V, Bakkali EH, Thuillez C, et al. Nitric-oxide is responsible for flow-dependent dilatation of human peripheral conduit arteries in-vivo. Circulation. 1995;91(5):1314–9. https://doi.org/10.1161/01.Cir.91.5.1314.
Okahara K, Sun B, Kambayashi J. Upregulation of prostacyclin synthesis-related gene expression by shear stress in vascular endothelial cells. Arterioscler Thromb Vasc Biol. 1998;18(12):1922–6.
Parker BA, Tschakovsky ME, Augeri AL, Polk DM, Thompson PD, Kiernan FJ. Heterogenous vasodilator pathways underlie flow-mediated dilation in men and women. Am J Physiol Heart Circ Physiol. 2011;301(3):H1118–26. https://doi.org/10.1152/ajpheart.00400.2011.
Casey DP, Walker BG, Ranadive SM, Taylor JL, Joyner MJ. Contribution of nitric oxide in the contraction-induced rapid vasodilation in young and older adults. J Appl Physiol. 2013;115(4):446–55. https://doi.org/10.1152/japplphysiol.00446.2013.
Brock RW, Tschakovsky ME, Shoemaker JK, Halliwill JR, Joyner MJ, Hughson RL. Effects of acetylcholine and nitric oxide on forearm blood flow at rest and after a single muscle contraction. J Appl Physiol. 1998;85(6):2249–54. https://doi.org/10.1152/jappl.1998.85.6.2249.
Buckwalter JB, Clifford PS. Autonomic control of skeletal muscle blood flow at the onset of exercise. Am J Physiol Heart Circ Physiol. 1999;277(5):H1872–7. https://doi.org/10.1152/ajpheart.1999.277.5.H1872.
Corcondilas A, Koroxenidis GT, Shepherd JT. Effect of a brief contraction of forearm muscles on forearm blood flow. J Appl Physiol. 1964;19(1):142–6. https://doi.org/10.1152/jappl.1964.19.1.142.
Dyke CK, Dietz NM, Lennon RL, Warner DO, Joyner MJ. Forearm blood flow responses to handgripping after local neuromuscular blockade. J Appl Physiol. 1998;84(2):754–8. https://doi.org/10.1152/jappl.1998.84.2.754.
Naik JS, Valic Z, Buckwalter JB, Clifford PS. Rapid vasodilation in response to a brief tetanic muscle contraction. J Appl Physiol. 1999;87(5):1741–6. https://doi.org/10.1152/jappl.1999.87.5.1741.
Wunsch SA, Muller-Delp J, Delp MD. Time course of vasodilatory responses in skeletal muscle arterioles: role in hyperemia at onset of exercise. Am J Physiol Heart Circ Physiol. 2000;279(4):H1715–23. https://doi.org/10.1152/ajpheart.2000.279.4.H1715.
Hamann JJ, Buckwalter JB, Clifford PS. Vasodilatation is obligatory for contraction-induced hyperaemia in canine skeletal muscle. J Physiol. 2004;557(Pt 3):1013–20. https://doi.org/10.1113/jphysiol.2004.062836.
Kiens B, Saltin B, WallØSe L, Wesche J. Temporal relationship between blood flow changes and release of ions and metabolites from muscles upon single weak contractions. Acta Physiol (Oxf). 1989;136(4):551–9. https://doi.org/10.1111/j.1748-1716.1989.tb08701.x.
Mohrman DE, Sparks HV. Myogenic hyperemia following brief tetanus of canine skeletal muscle. Am J Physiol. 1974;227(3):531–5. https://doi.org/10.1152/ajplegacy.1974.227.3.531.
Clifford PS, Kluess HA, Hamann JJ, Buckwalter JB, Jasperse JL. Mechanical compression elicits vasodilatation in rat skeletal muscle feed arteries. J Physiol. 2006;572(Pt 2):561–7. https://doi.org/10.1113/jphysiol.2005.099507.
Juel C, Olsen S, Rentsch RL, González-Alonso J, Rosenmeier JB. K+ as a vasodilator in resting human muscle: implications for exercise hyperaemia. Acta Physiol (Oxf). 2007;190(4):311–8. https://doi.org/10.1111/j.1748-1716.2007.01678.x.
Armstrong ML, Dua AK, Murrant CL. Potassium initiates vasodilatation induced by a single skeletal muscle contraction in hamster cremaster muscle. J Physiol. 2007;581(Pt 2):841–52. https://doi.org/10.1113/jphysiol.2007.130013.
Crecelius AR, Kirby BS, Luckasen GJ, Larson DG, Dinenno FA. Mechanisms of rapid vasodilation after a brief contraction in human skeletal muscle. Am J Physiol Heart Circ Physiol. 2013;305(1):H29–40. https://doi.org/10.1152/ajpheart.00298.2013.
Crecelius AR, Richards JC, Luckasen GJ, Larson DG, Dinenno FA. Reactive hyperemia occurs via activation of inwardly rectifying potassium channels and Na+/K+-ATPase in humans. Circ Res. 2013;113(8):1023–32. https://doi.org/10.1161/CIRCRESAHA.113.301675.
Kirby BS, Carlson RE, Markwald RR, Voyles WF, Dinenno FA. Mechanical influences on skeletal muscle vascular tone in humans: insight into contraction-induced rapid vasodilatation. J Physiol. 2007;583(3):861–74.
Crecelius AR, Kirby BS, Richards JC, Dinenno FA. Mechanical effects of muscle contraction increase intravascular ATP draining quiescent and active skeletal muscle in humans. J Appl Physiol. 2013;114(8):1085–93. https://doi.org/10.1152/japplphysiol.01465.2012.
Mortensen SP, Thaning P, Nyberg M, Saltin B, Hellsten Y. Local release of ATP into the arterial inflow and venous drainage of human skeletal muscle: insight from ATP determination with the intravascular microdialysis technique. J Physiol. 2011;589(Pt 7):1847–57. https://doi.org/10.1113/jphysiol.2010.203034.
Gifford JR, Richardson RS. CORP: ultrasound assessment of vascular function with the passive leg movement technique. J Appl Physiol. 2017;123(6):1708–20. https://doi.org/10.1152/japplphysiol.00557.2017.
Groot HJ, Rossman MJ, Garten RS, Wang E, Hoff J, Helgerud J, et al. The effect of physical activity on passive leg movement-induced vasodilation with age. Med Sci Sports Exerc. 2016;48(8):1548–57. https://doi.org/10.1249/MSS.0000000000000936.
Hayman MA, Nativi JN, Stehlik J, McDaniel J, Fjeldstad AS, Ives SJ, et al. Understanding exercise-induced hyperemia: central and peripheral hemodynamic responses to passive limb movement in heart transplant recipients. Am J Physiol Heart Circ Physiol. 2010;299(5):H1653–9. https://doi.org/10.1152/ajpheart.00580.2010.
Nelson AD, Rossman MJ, Witman MA, Barrett-O’Keefe Z, Groot HJ, Garten RS, et al. Nitric oxide-mediated vascular function in sepsis using passive leg movement as a novel assessment: a cross-sectional study. J Appl Physiol. 2016;120(9):991–9. https://doi.org/10.1152/japplphysiol.00961.2015.
Venturelli M, Layec G, Trinity J, Hart CR, Broxterman RM, Richardson RS. Single passive leg movement-induced hyperemia: a simple vascular function assessment without a chronotropic response. J Appl Physiol. 2017;122(1):28–37. https://doi.org/10.1152/japplphysiol.00806.2016.
Witman MA, Ives SJ, Trinity JD, Groot HJ, Stehlik J, Richardson RS. Heart failure and movement-induced hemodynamics: partitioning the impact of central and peripheral dysfunction. Int J Cardiol. 2015;178:232–8. https://doi.org/10.1016/j.ijcard.2014.10.044.
Burns KJ, Pollock BS, Stavres J, Kilbane M, Brochetti A, McDaniel J. Passive limb movement intervals results in repeated hyperemic responses in those with paraplegia. Spinal Cord. 2018;56(10):940–8. https://doi.org/10.1038/s41393-018-0099-6.
Böger RH, Bode-Böger SM, Thiele W, Junker W, Alexander K, Frölich JC. Biochemical evidence for impaired nitric oxide synthesis in patients with peripheral arterial occlusive disease. Circulation. 1997;95(8):2068–74. https://doi.org/10.1161/01.cir.95.8.2068.
Hoier B, Rufener N, Bojsen-Moller J, Bangsbo J, Hellsten Y. The effect of passive movement training on angiogenic factors and capillary growth in human skeletal muscle. J Physiol. 2010;588(Pt 19):3833–45. https://doi.org/10.1113/jphysiol.2010.190439.
Hellsten Y, Rufener N, Nielsen JJ, Hoier B, Krustrup P, Bangsbo J. Passive leg movement enhances interstitial VEGF protein, endothelial cell proliferation, and eNOS mRNA content in human skeletal muscle. Am J Physiol Regul Integr Comp Physiol. 2008;294(3):R975–82. https://doi.org/10.1152/ajpregu.00677.2007.
Hoier B, Walker M, Passos M, Walker PJ, Green A, Bangsbo J, et al. Angiogenic response to passive movement and active exercise in individuals with peripheral arterial disease. J Appl Physiol. 2013;115(12):1777–87. https://doi.org/10.1152/japplphysiol.00979.2013.
Iepsen UW, Munch GD, Rugbjerg M, Rinnov AR, Zacho M, Mortensen SP, et al. Effect of endurance versus resistance training on quadriceps muscle dysfunction in COPD: a pilot study. Int J Chron Obstruct Pulmon Dis. 2016;11:2659–69. https://doi.org/10.2147/COPD.S114351.
Inaba Y, Chen JA, Bergmann SR. Prediction of future cardiovascular outcomes by flow-mediated vasodilatation of brachial artery: a meta-analysis. Int J Cardiovasc Imaging. 2010;26(6):631–40. https://doi.org/10.1007/s10554-010-9616-1.
Taddei S, Virdis A, Mattei P, Salvetti A. Vasodilation to acetylcholine in primary and secondary forms of human hypertension. Hypertension. 1993;21(6):929–33. https://doi.org/10.1161/01.hyp.21.6.929.
Furchgott RF, Zawadzki JV. The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature. 1980;288:373–6. https://doi.org/10.1038/288373a0.
Kuvin JT, Patel AR, Sliney KA, Pandian NG, Sheffy J, Schnall RP, et al. Assessment of peripheral vascular endothelial function with finger arterial pulse wave amplitude. Am Heart J. 2003;146(1):168–74. https://doi.org/10.1016/s0002-8703(03)00094-2.
Rubinshtein R, Kuvin JT, Soffler M, Lennon RJ, Lavi S, Nelson RE, et al. Assessment of endothelial function by non-invasive peripheral arterial tonometry predicts late cardiovascular adverse events. Eur Heart J. 2010;31(9):1142–8. https://doi.org/10.1093/eurheartj/ehq010.
Flammer AJ, Anderson T, Celermajer DS, Creager MA, Deanfield J, Ganz P, et al. The assessment of endothelial function: from research into clinical practice. Circulation. 2012;126(6):753–67. https://doi.org/10.1161/CIRCULATIONAHA.112.093245.
Deanfield JE, Halcox JP, Rabelink TJ. Endothelial function and dysfunction: testing and clinical relevance. Circulation. 2007;115(10):1285–95.
Joannides R, Bellien J, Thuillez C. Clinical methods for the evaluation of endothelial function: a focus on resistance arteries. Fundam Clin Pharmacol. 2006;20(3):311–20. https://doi.org/10.1111/j.1472-8206.2006.00406.x.
Ludmer PL, Selwyn AP, Shook TL, Wayne RR, Mudge GH, Alexander RW, et al. Paradoxical vasoconstriction induced by acetylcholine in atherosclerotic coronary arteries. N Engl J Med. 1986;315(17):1046–51. https://doi.org/10.1056/NEJM198610233151702.
Linder L, Kiowski W, Bühler FR, Lüscher TF. Indirect evidence for release of endothelium-derived relaxing factor in human forearm circulation in vivo: blunted response in essential hypertension. Circulation. 1990;81(6):1762–7. https://doi.org/10.1161/01.cir.81.6.1762.
Harris RA, Nishiyama SK, Wray DW, Richardson RS. Ultrasound assessment of flow-mediated dilation. Hypertension. 2010;55(5):1075–85. https://doi.org/10.1161/hypertensionaha.110.150821.
Thijssen DH, Black MA, Pyke KE, Padilla J, Atkinson G, Harris RA, et al. Assessment of flow-mediated dilation in humans: a methodological and physiological guideline. Am J Physiol Heart Circ Physiol. 2011;300(1):H2–12. https://doi.org/10.1152/ajpheart.00471.2010.
Green DJ, Jones H, Thijssen D, Cable N, Atkinson GJH. Flow-mediated dilation and cardiovascular event prediction: does nitric oxide matter? Hypertension. 2011;57(3):363–9.
Anderson TJ, Uehata A, Gerhard MD, Meredith IT, Knab S, Delagrange D, et al. Close relation of endothelial function in the human coronary and peripheral circulations. J Am Coll Cardiol. 1995;26(5):1235–41.
Broxterman RM, Witman MA, Trinity JD, Groot HJ, Rossman MJ, Park S-Y, et al. Strong relationship between vascular function in the coronary and brachial arteries. Hypertension. 2019;74(1):208–15. https://doi.org/10.1161/HYPERTENSIONAHA.119.12881.
Nohria A, Gerhard-Herman M, Creager MA, Hurley S, Mitra D, Ganz P. Role of nitric oxide in the regulation of digital pulse volume amplitude in humans. J Appl Physiol. 2006;101(2):545–8. https://doi.org/10.1152/japplphysiol.01285.2005.
Moerland M, Kales AJ, Schrier L, van Dongen MG, Bradnock D, Burggraaf J. Evaluation of the EndoPAT as a tool to assess endothelial function. Int J Vasc Med. 2012;2012:904141. https://doi.org/10.1155/2012/904141.
Hamburg NM, Keyes MJ, Larson MG, Vasan RS, Schnabel R, Pryde MM, et al. Cross-sectional relations of digital vascular function to cardiovascular risk factors in the Framingham Heart Study. Circulation. 2008;117(19):2467–74. https://doi.org/10.1161/circulationaha.107.748574.
Hamburg NM, Palmisano J, Larson MG, Sullivan LM, Lehman BT, Vasan RS, et al. Relation of brachial and digital measures of vascular function in the community: the Framingham heart study. Hypertension. 2011;57(3):390–6. https://doi.org/10.1161/HYPERTENSIONAHA.110.160812.
Bonetti PO, Pumper GM, Higano ST, Holmes DR Jr, Kuvin JT, Lerman A. Noninvasive identification of patients with early coronary atherosclerosis by assessment of digital reactive hyperemia. J Am Coll Cardiol. 2004;44(11):2137–41. https://doi.org/10.1016/j.jacc.2004.08.062.
Broxterman RM, Trinity JD, Gifford JR, Kwon OS, Kithas AC, Hydren JR, et al. Single passive leg movement assessment of vascular function: contribution of nitric oxide. J Appl Physiol. 2017;123(6):1468–76. https://doi.org/10.1152/japplphysiol.00533.2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was supported by Veterans Affairs Rehabilitation Research and Development Career Development (IK2RX001215), Merit (E6910-R and E1697-R), Spire (E1433-P), Senior Research Career Scientist (E9275-L) awards, American Heart Association (14SDG18850039), and a National Heart, Lung, and Blood Institute grant (HL-091830).
Conflict of interest
Joel D. Trinity and Russell S. Richardson have no conflicts of interest that are directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Trinity, J.D., Richardson, R.S. Physiological Impact and Clinical Relevance of Passive Exercise/Movement. Sports Med 49, 1365–1381 (2019). https://doi.org/10.1007/s40279-019-01146-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-019-01146-1